Abstract
Objectives
Schizophrenia spectrum disorders and bipolar spectrum disorders are the product of both heritable and non-heritable factors, the impact of which converges at different biological levels. Recent evidence from molecular approaches has provided new insights about how environmental exposures cause persistent alterations in the regulation of gene expression, particularly by so-called epigenetic mechanisms. The aim of this review is to provide an overview of findings of epigenetic studies in psychotic disorders, summarizing findings of human and animal studies on epigenetic alterations due to postnatal environmental exposures associated with psychotic disorders.
Methods
Electronic and manual literature search of MEDLINE, EMBASE and PSYCHINFO, using a range of search terms around epigenetics, DNA methylation, histone modifications, psychoses, schizophrenia, bipolar disorder and environmental risks associated with psychotic disorders as observed in human and experimental animal studies, complemented by review articles and cross-references.
Results
Despite several promising findings of differential epigenetic profiles in individuals with psychotic disorders in the studies published to date, the knowledge of the role of epigenetic processes in psychotic disorder remains very limited, and should be interpreted cautiously given various challenges in this rapidly evolving field of research.
Conclusions
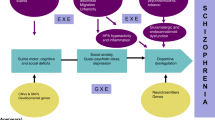
Integration of epigenetic findings into biopsychosocial models of the etiology of psychotic disorders eventually may yield important insights into the biological underpinnings of the onset and course of psychotic disorders.

Similar content being viewed by others
References
Lichtenstein P, Yip BH, Bjork C, Pawitan Y, Cannon TD, Sullivan PF, Hultman CM (2009) Common genetic determinants of schizophrenia and bipolar disorder in Swedish families: a population-based study. Lancet 373(9659):234–239. doi:10.1016/S0140-6736(09)60072-6
Lee SH, Ripke S, Neale BM et al (2013) Genetic relationship between five psychiatric disorders estimated from genome-wide SNPs. Nat Genet 45(9):984–994. doi:10.1038/ng.2711
Leboyer M, Meyer-Lindenberg A, Stetanis N, Rutten BPF, Arango C, Jones P, Kapur S, Lewis S, Murray R, Owen MJ, Schizophrenia EN (2008) Schizophrenia aetiology: do gene–environment interactions hold the key? Schizophr Res 102(1–3):21–26. doi:10.1016/J.Schres.04.003
van Os J, Rutten BP (2009) Gene–environment-wide interaction studies in psychiatry. Am J Psychiatry 166(9):964–966. doi:10.1176/appi.ajp.2008.09060904
van Os J, Kenis G, Rutten BP (2010) The environment and schizophrenia. Nature 468(7321):203–212. doi:10.1038/nature09563
Harrison PJ, Weinberger DR (2005) Schizophrenia genes, gene expression, and neuropathology: on the matter of their convergence. Mol Psychiatry 10(1):40–68. doi:10.1038/Sj.Mp.4001558
de Jong S, Boks MP, Fuller TF, Strengman E, Janson E, de Kovel CG, Ori AP, Vi N, Mulder F, Blom JD, Glenthoj B, Schubart CD, Cahn W, Kahn RS, Horvath S, Ophoff RA (2012) A gene co-expression network in whole blood of schizophrenia patients is independent of antipsychotic-use and enriched for brain-expressed genes. PLoS One 7(6):e39498. doi:10.1371/journal.pone.0039498
Kofink D, Boks MP, Timmers HT, Kas MJ (2013) Epigenetic dynamics in psychiatric disorders: environmental programming of neurodevelopmental processes. Neurosci Biobehav Rev 37(5):831–845. doi:10.1016/j.neubiorev.2013.03.020
Chuang JC, Jones PA (2007) Epigenetics and microRNAs. Pediatr Res 61(5 Pt 2):24R–29R. doi:10.1203/pdr.0b013e3180457684
van Rooij E, Sutherland LB, Qi X, Richardson JA, Hill J, Olson EN (2007) Control of stress-dependent cardiac growth and gene expression by a microRNA. Science 316(5824):575–579. doi:10.1126/science.1139089
Moore LD, Le T, Fan G (2013) DNA methylation and its basic function. Neuropsychopharmacology 38(1):23–38. doi:10.1038/npp.2012.112
Yu M, Hon GC, Szulwach KE, Song CX, Zhang L, Kim A, Li X, Dai Q, Shen Y, Park B, Min JH, Jin P, Ren B, He C (2012) Base-resolution analysis of 5-hydroxymethylcytosine in the mammalian genome. Cell 149(6):1368–1380. doi:10.1016/j.cell.2012.04.027
Akbarian S, Huang HS (2008) Epigenetic regulation in human brain-focus on histone lysine methylation. Biol Psychiatry 65(3):198–203. doi:10.1016/J.Biopsych.08.015
Peerbooms OL, Wichers M, Jacobs N, Kenis G, Derom C, Vlietinck R, Thiery E, van Os J, Rutten BP (2010) No major role for X-inactivation in variations of intelligence and behavioral problems at middle childhood. Am J Med Genet B Neuropsychiatr Genet 153B(7):1311–1317. doi:10.1002/ajmg.b.31111
Smits L, Pedersen C, Mortensen P, van Os J (2004) Association between short birth intervals and schizophrenia in the offspring. Schizophr Res 70(1):49–56. doi:10.1016/J.Schres.10.002
Mill J, Tang T, Kaminsky Z, Khare T, Yazdanpanah S, Bouchard L, Jia P, Assadzadeh A, Flanagan J, Schumacher A, Wang SC, Petronis A (2008) Epigenomic profiling reveals DNA-methylation changes associated with major psychosis. Am J Hum Genet 82(3):696–711. doi:10.1016/j.ajhg.2008.01.008
Melas PA, Rogdaki M, Osby U, Schalling M, Lavebratt C, Ekstrom TJ (2012) Epigenetic aberrations in leukocytes of patients with schizophrenia: association of global DNA methylation with antipsychotic drug treatment and disease onset. FASEB J 26(6):2712–2718. doi:10.1096/Fj.11-202069
Shimabukuro M, Sasaki T, Imamura A, Tsujita T, Fuke C, Umekage T, Tochigi M, Hiramatsu K, Miyazaki T, Oda T, Sugimoto J, Jinno Y, Okazaki Y (2007) Global hypomethylation of peripheral leukocyte DNA in male patients with schizophrenia: a potential link between epigenetics and schizophrenia. J Psychiatr Res 41(12):1042–1046. doi:10.1016/J.Jpsychires.08.006
Dempster EL, Pidsley R, Schalkwyk LC, Owens S, Georgiades A, Kane F, Kalidindi S, Picchioni M, Kravariti E, Toulopoulou T, Murray RM, Mill J (2011) Disease-associated epigenetic changes in monozygotic twins discordant for schizophrenia and bipolar disorder. Hum Mol Genet 20(24):4786–4796. doi:10.1093/hmg/ddr416
Bromberg A, Levine J, Nemetz B, Belmaker RH, Agam G (2008) No association between global leukocyte DNA methylation and homocysteine levels in schizophrenia patients. Schizophr Res 101(1–3):50–57. doi:10.1016/J.Schres.01.009
Bromberg A, Bersudsky Y, Levine J, Agam G (2009) Global leukocyte DNA methylation is not altered in euthymic bipolar patients. J Affect Disord 118(1–3):234–239. doi:10.1016/J.Jad.01.031
Rosa A, Picchioni MM, Kalidindi S, Loat CS, Knight J, Toulopoulou T, Vonk R, van der Schot AC, Nolen W, Kahn RS, McGuffin P, Murray RM, Craig IW (2008) Differential methylation of the X-chromosome is a possible source of discordance for bipolar disorder female monozygotic twins. Am J Med Genet B 147B(4):459–462. doi:10.1002/Ajmg.B.30616
Gavin DP, Rosen C, Chase K, Grayson DR, Tun N, Sharma RP (2009) Dimethylated lysine 9 of histone 3 is elevated in schizophrenia and exhibits a divergent response to histone deacetylase inhibitors in lymphocyte cultures. J Psychiatry Neurosci 34(3):232–237
Akbarian S, Ruehl MG, Bliven E, Luiz LA, Peranelli AC, Baker SP, Roberts RC, Bunney WE Jr, Conley RC, Jones EG, Tamminga CA, Guo Y (2005) Chromatin alterations associated with down-regulated metabolic gene expression in the prefrontal cortex of subjects with schizophrenia. Arch Gen Psychiatry 62(8):829–840. doi:10.1001/archpsyc.62.8.829
Howes OD, Murray RM (2013) Schizophrenia: an integrated sociodevelopmental-cognitive model. Lancet. doi:10.1016/S0140-6736(13)62036-X
Abdolmaleky HM, Cheng KH, Faraone SV, Wilcox M, Glatt SJ, Gao F, Smith CL, Shafa R, Aeali B, Carnevale J, Pan H, Papageorgis P, Ponte JF, Sivaraman V, Tsuang MT, Thiagalingam S (2006) Hypomethylation of MB-COMT promoter is a major risk factor for schizophrenia and bipolar disorder. Hum Mol Genet 15(21):3132–3145. doi:10.1093/hmg/ddl253
Nohesara S, Ghadirivasfi M, Mostafavi S, Eskandari MR, Ahmadkhaniha H, Thiagalingam S, Abdolmaleky HM (2011) DNA hypomethylation of MB-COMT promoter in the DNA derived from saliva in schizophrenia and bipolar disorder. J Psychiatr Res 45(11):1432–1438. doi:10.1016/j.jpsychires.2011.06.013
Dempster EL, Mill J, Craig IW, Collier DA (2006) The quantification of COMT mRNA in post mortem cerebellum tissue: diagnosis, genotype, methylation and expression. BMC Med Genet 7:10
Petronis A, Gottesman II, Kan P, Kennedy JL, Basile VS, Paterson AD, Popendikyte V (2003) Monozygotic twins exhibit numerous epigenetic differences: clues to twin discordance? Schizophr Bull 29(1):169–178
Kordi-Tamandani DM, Sahranavard R, Torkamanzehi A (2013) Analysis of association between dopamine receptor genes’ methylation and their expression profile with the risk of schizophrenia. Psychiatr Genet 23(5):183–187. doi:10.1097/Ypg.0b013e328363d6e1
Zhang AP, Yu J, Liu JX, Zhang HY, Du YY, Zhu JD, He G, Li XW, Gu NF, Feng GY, He L (2007) The DNA methylation profile within the 5’-regulatory region of DRD2 in discordant sib pairs with schizophrenia. Schizophr Res 90(1–3):97–103. doi:10.1016/J.Schres.11.007
Kordi-Tamandani DM, Dahmardeh N, Torkamanzehi A (2013) Evaluation of hypermethylation and expression pattern of GMR2, GMR5, GMR8, and GRIA3 in patients with schizophrenia. Gene 515(1):163–166. doi:10.1016/j.gene.2012.10.075
Benes FM, Lim B, Matzilevich D, Walsh JP, Subburaju S, Minns M (2007) Regulation of the GABA cell phenotype in hippocampus of schizophrenics and bipolars. Proc Natl Acad Sci U S A 104(24):10164–10169. doi:10.1073/pnas.0703806104
Guidotti A, Auta J, Davis JM, Di-Giorgi-Gerevini V, Dwivedi Y, Grayson DR, Impagnatiello F, Pandey G, Pesold C, Sharma R, Uzunov D, Costa E (2000) Decrease in reelin and glutamic acid decarboxylase67 (GAD67) expression in schizophrenia and bipolar disorder: a postmortem brain study. Arch Gen Psychiat 57(11):1061–1069
Huang HS, Matevossian A, Whittle C, Kim SY, Schumacher A, Baker SP, Akbarian S (2007) Prefrontal dysfunction in schizophrenia involves mixed-lineage leukemia 1-regulated histone methylation at GABAergic gene promoters. J Neurosci 27(42):11254–11262. doi:10.1523/Jneurosci.3272-07
Veldic M, Guidotti A, Maloku E, Davis JM, Costa E (2005) In psychosis, cortical interneurons overexpress DNA-methyltransferase 1. Proc Natl Acad Sci U S A 102(6):2152–2157. doi:10.1073/pnas.0409665102
Boulle F, van den Hove DL, Jakob SB, Rutten BP, Hamon M, van Os J, Lesch KP, Lanfumey L, Steinbusch HW, Kenis G (2012) Epigenetic regulation of the BDNF gene: implications for psychiatric disorders. Mol Psychiatry 17(6):584–596. doi:10.1038/mp.2011.107
Ikegame T, Bundo M, Sunaga F, Asai T, Nishimura F, Yoshikawa A, Kawamura Y, Hibino H, Tochigi M, Kakiuchi C, Sasaki T, Kato T, Kasai K, Iwamoto K (2013) DNA methylation analysis of BDNF gene promoters in peripheral blood cells of schizophrenia patients. Neurosci Res. doi:10.1016/j.neures.2013.08.004
dell’Osso B, d’Addario C, Palazzo M, Cattaneo E, Galimberti D, Scarpini E, Bresolin N, Arosio B, Bergamaschini L, Candeletti S, Romualdi P, Altamura AC (2011) Selective DNA Methylation of Bdnf promoter and nociceptin gene in bipolar disorder. Eur Psychiat 26
Ziller MJ, Gu H, Muller F, Donaghey J, Tsai LT, Kohlbacher O, De Jager PL, Rosen ED, Bennett DA, Bernstein BE, Gnirke A, Meissner A (2013) Charting a dynamic DNA methylation landscape of the human genome. Nature 500(7463):477–481. doi:10.1038/nature12433
Kinoshita M, Numata S, Tajima A, Shimodera S, Ono S, Imamura A, Iga J, Watanabe S, Kikuchi K, Kubo H, Nakataki M, Sumitani S, Imoto I, Okazaki Y, Ohmori T (2013) DNA methylation signatures of peripheral leukocytes in schizophrenia. Neuromolecular Med 15(1):95–101. doi:10.1007/S12017-012-8198-6
Aberg KA, McClay JL, Nerella S, Clark S, Kumar G, Chen W, Khachane AN, Xie L, Hudson A, Gao G, Harada A, Hultman CM, Sullivan PF, Magnusson PK, van den Oord EJ (2014) Methylome-wide association study of Schizophrenia: identifying blood biomarker signatures of environmental insults. JAMA Psychiatry. doi:10.1001/jamapsychiatry.2013.3730
Zhubi A, Veldic M, Puri NV, Kadriu B, Caruncho H, Loza I, Sershen H, Lajtha A, Smith RC, Guidotti A, Davis JM, Costa E (2009) An upregulation of DNA-methyltransferase 1 and 3a expressed in telencephalic GABAergic neurons of schizophrenia patients is also detected in peripheral blood lymphocytes. Schizophr Res 111(1–3):115–122. doi:10.1016/J.Schres.03.020
Veldic M, Caruncho HJ, Liu WS, Davis J, Satta R, Grayson DR, Guidotti A, Costa E (2004) DNA-methyltransferase 1 mRNA is selectively overexpressed in telencephalic GABAergic interneurons of schizophrenia brains. Proc Natl Acad Sci U S A 101(1):348–353. doi:10.1073/pnas.2637013100
Zhang C, Fang Y, Xie B, Cheng W, Du Y, Wang D, Yu S (2009) DNA methyltransferase 3B gene increases risk of early onset schizophrenia. Neurosci Lett 462(3):308–311. doi:10.1016/j.neulet.2009.06.085
Kale A, Naphade N, Sapkale S, Kamaraju M, Pillai A, Joshi S, Mahadik S (2010) Reduced folic acid, vitamin B12 and docosahexaenoic acid and increased homocysteine and cortisol in never-medicated schizophrenia patients: implications for altered one-carbon metabolism. Psychiatry Res 175(1–2):47–53. doi:10.1016/j.psychres.2009.01.013
Guidotti A, Ruzicka W, Grayson DR, Veldic M, Pinna G, Davis JM, Costa E (2007) S-adenosyl methionine and DNA methyltransferase-1 mRNA overexpression in psychosis. NeuroReport 18(1):57–60. doi:10.1097/WNR.0b013e32800fefd7
Peerbooms OL, van Os J, Drukker M, Kenis G, Hoogveld L, de Hert M, Delespaul P, van Winkel R, Rutten BP (2011) Meta-analysis of MTHFR gene variants in schizophrenia, bipolar disorder and unipolar depressive disorder: evidence for a common genetic vulnerability? Brain Behav Immun 25(8):1530–1543. doi:10.1016/j.bbi.2010.12.006
Roffman JL, Brohawn DG, Nitenson AZ, Macklin EA, Smoller JW, Goff DC (2013) Genetic variation throughout the folate metabolic pathway influences negative symptom severity in schizophrenia. Schizophr Bull 39(2):330–338. doi:10.1093/schbul/sbr150
Roffman JL, Lamberti JS, Achtyes E, Macklin EA, Galendez GC, Raeke LH, Silverstein NJ, Smoller JW, Hill M, Goff DC (2013) Randomized multicenter investigation of folate plus vitamin B12 supplementation in schizophrenia. JAMA Psychiatry 70(5):481–489. doi:10.1001/jamapsychiatry.2013.900
Liu Y, Chen G, Norton N, Liu W, Zhu H, Zhou P, Luan M, Yang S, Chen X, Carroll L, Williams NM, O’Donovan MC, Kirov G, Owen MJ (2009) Whole genome association study in a homogenous population in Shandong peninsula of China reveals JARID2 as a susceptibility gene for schizophrenia. J Biomed Biotechnol 2009:536918. doi:10.1155/2009/536918
Kirov G, Pocklington AJ, Holmans P, Ivanov D, Ikeda M, Ruderfer D, Moran J, Chambert K, Toncheva D, Georgieva L, Grozeva D, Fjodorova M, Wollerton R, Rees E, Nikolov I, van de Lagemaat LN, Bayes A, Fernandez E, Olason PI, Bottcher Y, Komiyama NH, Collins MO, Choudhary J, Stefansson K, Stefansson H, Grant SG, Purcell S, Sklar P, O’Donovan MC, Owen MJ (2012) De novo CNV analysis implicates specific abnormalities of postsynaptic signalling complexes in the pathogenesis of schizophrenia. Mol Psychiatry 17(2):142–153. doi:10.1038/mp.2011.154
Han H, Yu Y, Shi J, Yao Y, Li W, Kong N, Wu Y, Wang C, Wang S, Meng X, Kou C (2013) Associations of histone deacetylase-2 and histone deacetylase-3 genes with schizophrenia in a Chinese population. Asia Pac Psychiatry 5(1):11–16. doi:10.1111/j.1758-5872.2012.00205.x
Kim T, Park JK, Kim HJ, Chung JH, Kim JW (2010) Association of histone deacetylase genes with schizophrenia in Korean population. Psychiatry Res 178(2):266–269. doi:10.1016/j.psychres.2009.05.007
Sharma RP, Grayson DR, Gavin DP (2008) Histone deactylase 1 expression is increased in the prefrontal cortex of schizophrenia subjects: analysis of the National Brain Databank microarray collection. Schizophr Res 98(1–3):111–117. doi:10.1016/j.schres.2007.09.020
Hobara T, Uchida S, Otsuki K, Matsubara T, Funato H, Matsuo K, Suetsugi M, Watanabe Y (2010) Altered gene expression of histone deacetylases in mood disorder patients. J Psychiatr Res 44(5):263–270. doi:10.1016/j.jpsychires.2009.08.015
Bartel DP (2004) MicroRNAs: genomics, biogenesis, mechanism, and function. Cell 116(2):281–297
(2011) Genome-wide association study identifies five new schizophrenia loci. Nat Genet 43(10):969–976. doi:10.1038/ng.940
Green MJ, Cairns MJ, Wu J, Dragovic M, Jablensky A, Tooney PA, Scott RJ, Carr VJ (2013) Genome-wide supported variant MIR137 and severe negative symptoms predict membership of an impaired cognitive subtype of schizophrenia. Mol Psychiatry 18(7):774–780. doi:10.1038/mp.2012.84
Lett TA, Chakavarty MM, Felsky D, Brandl EJ, Tiwari AK, Goncalves VF, Rajji TK, Daskalakis ZJ, Meltzer HY, Lieberman JA, Lerch JP, Mulsant BH, Kennedy JL, Voineskos AN (2013) The genome-wide supported microRNA-137 variant predicts phenotypic heterogeneity within schizophrenia. Mol Psychiatry 18(4):443–450. doi:10.1038/mp.2013.17
Whalley HC, Papmeyer M, Romaniuk L, Sprooten E, Johnstone EC, Hall J, Lawrie SM, Evans KL, Blumberg HP, Sussmann JE, McIntosh AM (2012) Impact of a microRNA MIR137 susceptibility variant on brain function in people at high genetic risk of schizophrenia or bipolar disorder. Neuropsychopharmacology 37(12):2720–2729. doi:10.1038/npp.2012.137
Labrie V, Pai S, Petronis A (2012) Epigenetics of major psychosis: progress, problems and perspectives. Trends Genet 28(9):427–435. doi:10.1016/j.tig.2012.04.002
Szulwach KE, Li X, Li Y, Song CX, Wu H, Dai Q, Irier H, Upadhyay AK, Gearing M, Levey AI, Vasanthakumar A, Godley LA, Chang Q, Cheng X, He C, Jin P (2011) 5-hmC-mediated epigenetic dynamics during postnatal neurodevelopment and aging. Nat Neurosci 14(12):1607–1616. doi:10.1038/nn.2959
Rutten BP, Hammels C, Geschwind N, Menne-Lothmann C, Pishva E, Schruers K, van den Hove D, Kenis G, van Os J, Wichers M (2013) Resilience in mental health: linking psychological and neurobiological perspectives. Acta Psychiatr Scand 128(1):3–20. doi:10.1111/acps.12095
Rutten BP, Mill J (2009) Epigenetic mediation of environmental influences in major psychotic disorders. Schizophr Bull 35(6):1045–1056. doi:10.1093/schbul/sbp104
Weaver IC, Cervoni N, Champagne FA, D’Alessio AC, Sharma S, Seckl JR, Dymov S, Szyf M, Meaney MJ (2004) Epigenetic programming by maternal behavior. Nat Neurosci 7(8):847–854. doi:10.1038/nn1276
Wand GS, Oswald LM, McCaul ME, Wong DF, Johnson E, Zhou Y, Kuwabara H, Kumar A (2007) Association of amphetamine-induced striatal dopamine release and cortisol responses to psychological stress. Neuropsychopharmacology 32(11):2310–2320. doi:10.1038/sj.npp.1301373
Webster MJ, Knable MB, O’Grady J, Orthmann J, Weickert CS (2002) Regional specificity of brain glucocorticoid receptor mRNA alterations in subjects with schizophrenia and mood disorders. Mol Psychiatry 7(9):985–994, 924. doi:10.1038/sj.mp.4001139
Ouellet-Morin I, Odgers CL, Danese A, Bowes L, Shakoor S, Papadopoulos AS, Caspi A, Moffitt TE, Arseneault L (2011) Blunted cortisol responses to stress signal social and behavioral problems among maltreated/bullied 12-year-old children. Biol Psychiatry 70(11):1016–1023. doi:10.1016/j.biopsych.2011.06.017
Weaver IC, Champagne FA, Brown SE, Dymov S, Sharma S, Meaney MJ, Szyf M (2005) Reversal of maternal programming of stress responses in adult offspring through methyl supplementation: altering epigenetic marking later in life. J Neurosci Off J Socr Neurosci 25(47):11045–11054. doi:10.1523/JNEUROSCI.3652-05.2005
Weaver ICG, Meaney MJ, Szyf M (2006) Maternal care effects on the hippocampal transcriptome and anxiety-mediated behaviors in the offspring that are reversible in adulthood. Proc Natl Acad Sci U S A 103(9):3480–3485. doi:10.1073/Pnas.0507526103
Perroud N, Dayer A, Piguet C, Nallet A, Favre S, Malafosse A, Aubry JM (2013) Childhood maltreatment and methylation of the glucocorticoid receptor gene NR3C1 in bipolar disorder. Br J Psychiatry. doi:10.1192/bjp.bp.112.120055
Tyrka AR, Price LH, Marsit C, Walters OC, Carpenter LL (2012) Childhood adversity and epigenetic modulation of the leukocyte glucocorticoid receptor: preliminary findings in healthy adults. PLoS One 7(1):e30148. doi:10.1371/journal.pone.0030148
Yang BZ, Zhang H, Ge W, Weder N, Douglas-Palumberi H, Perepletchikova F, Gelernter J, Kaufman J (2013) Child abuse and epigenetic mechanisms of disease risk. Am J Prev Med 44(2):101–107. doi:10.1016/j.amepre.2012.10.012
McGowan PO, Sasaki A, D’Alessio AC, Dymov S, Labonte B, Szyf M, Turecki G, Meaney MJ (2009) Epigenetic regulation of the glucocorticoid receptor in human brain associates with childhood abuse. Nat Neurosci 12(3):342–348. doi:10.1038/nn.2270
Naumova OY, Lee M, Koposov R, Szyf M, Dozier M, Grigorenko EL (2012) Differential patterns of whole-genome DNA methylation in institutionalized children and children raised by their biological parents. Dev Psychopathol 24(1):143–155. doi:10.1017/S0954579411000605
Koenen KC, Uddin M (2010) FKBP5 polymorphisms modify the effects of childhood trauma. Neuropsychopharmacology 35(8):1623–1624. doi:10.1038/npp.2010.60
Klengel T, Mehta D, Anacker C, Rex-Haffner M, Pruessner JC, Pariante CM, Pace TW, Mercer KB, Mayberg HS, Bradley B, Nemeroff CB, Holsboer F, Heim CM, Ressler KJ, Rein T, Binder EB (2013) Allele-specific FKBP5 DNA demethylation mediates gene–childhood trauma interactions. Nat Neurosci 16(1):33–41. doi:10.1038/nn.3275
Meaburn EL, Schalkwyk LC, Mill J (2010) Allele-specific methylation in the human genome: implications for genetic studies of complex disease. Epigenetics 5(7):578–582. doi:10.4161/epi.5.7.12960
Collip D, Myin-Germeys I, Wichers M, Jacobs N, Derom C, Thiery E, Lataster T, Simons C, Delespaul P, Marcelis M, van Os J, van Winkel R (2013) FKBP5 as a possible moderator of the psychosis-inducing effects of childhood trauma. Br J Psychiatry 202(4):261–268. doi:10.1192/bjp.bp.112.115972
Murgatroyd C, Patchev AV, Wu Y, Micale V, Bockmuhl Y, Fischer D, Holsboer F, Wotjak CT, Almeida OF, Spengler D (2009) Dynamic DNA methylation programs persistent adverse effects of early-life stress. Nat Neurosci 12(12):1559–1566. doi:10.1038/nn.2436
Selten JP, van der Ven E, Rutten BP, Cantor-Graae E (2013) The social defeat hypothesis of schizophrenia: an update. Schizophr Bull 39(6):1180–1186. doi:10.1093/schbul/sbt134
Tsankova NM, Berton O, Renthal W, Kumar A, Neve RL, Nestler EJ (2006) Sustained hippocampal chromatin regulation in a mouse model of depression and antidepressant action. Nat Neurosci 9(4):519–525. doi:10.1038/nn1659
Renthal W, Maze I, Krishnan V, Covington HE III, Xiao G, Kumar A, Russo SJ, Graham A, Tsankova N, Kippin TE, Kerstetter KA, Neve RL, Haggarty SJ, McKinsey TA, Bassel-Duby R, Olson EN, Nestler EJ (2007) Histone deacetylase 5 epigenetically controls behavioral adaptations to chronic emotional stimuli. Neuron 56(3):517–529. doi:10.1016/j.neuron.2007.09.032
Krishnan V, Han MH, Graham DL, Berton O, Renthal W, Russo SJ, Laplant Q, Graham A, Lutter M, Lagace DC, Ghose S, Reister R, Tannous P, Green TA, Neve RL, Chakravarty S, Kumar A, Eisch AJ, Self DW, Lee FS, Tamminga CA, Cooper DC, Gershenfeld HK, Nestler EJ (2007) Molecular adaptations underlying susceptibility and resistance to social defeat in brain reward regions. Cell 131(2):391–404. doi:10.1016/j.cell.2007.09.018
Berton O, McClung CA, Dileone RJ, Krishnan V, Renthal W, Russo SJ, Graham D, Tsankova NM, Bolanos CA, Rios M, Monteggia LM, Self DW, Nestler EJ (2006) Essential role of BDNF in the mesolimbic dopamine pathway in social defeat stress. Science 311(5762):864–868. doi:10.1126/science.1120972
LaPlant Q, Vialou V, Covington HE III, Dumitriu D, Feng J, Warren BL, Maze I, Dietz DM, Watts EL, Iniguez SD, Koo JW, Mouzon E, Renthal W, Hollis F, Wang H, Noonan MA, Ren Y, Eisch AJ, Bolanos CA, Kabbaj M, Xiao G, Neve RL, Hurd YL, Oosting RS, Fan G, Morrison JH, Nestler EJ (2010) Dnmt3a regulates emotional behavior and spine plasticity in the nucleus accumbens. Nat Neurosci 13(9):1137–1143. doi:10.1038/nn.2619
Unternaehrer E, Luers P, Mill J, Dempster E, Meyer AH, Staehli S, Lieb R, Hellhammer DH, Meinlschmidt G (2012) Dynamic changes in DNA methylation of stress-associated genes (OXTR, BDNF) after acute psychosocial stress. Transl Psychiatry 2:e150. doi:10.1038/tp.2012.77
Soliman A, O’Driscoll GA, Pruessner J, Holahan AL, Boileau I, Gagnon D, Dagher A (2008) Stress-induced dopamine release in humans at risk of psychosis: a [11C]raclopride PET study. Neuropsychopharmacology 33(8):2033–2041. doi:10.1038/sj.npp.1301597
Mizrahi R, Addington J, Rusjan PM, Suridjan I, Ng A, Boileau I, Pruessner JC, Remington G, Houle S, Wilson AA (2012) Increased stress-induced dopamine release in psychosis. Biol Psychiatry 71(6):561–567. doi:10.1016/j.biopsych.2011.10.009
Barnett JH, Werners U, Secher SM, Hill KE, Brazil R, Masson K, Pernet DE, Kirkbride JB, Murray GK, Bullmore ET, Jones PB (2007) Substance use in a population-based clinic sample of people with first-episode psychosis. Br J Psychiatry 190:515–520. doi:10.1192/bjp.bp.106.024448
Arseneault L, Cannon M, Witton J, Murray RM (2004) Causal association between cannabis and psychosis: examination of the evidence. Br J Psychiatry 184:110–117
Sekine Y, Iyo M, Ouchi Y, Matsunaga T, Tsukada H, Okada H, Yoshikawa E, Futatsubashi M, Takei N, Mori N (2001) Methamphetamine-related psychiatric symptoms and reduced brain dopamine transporters studied with PET. Am J Psychiatry 158(8):1206–1214
Lehrmann E, Colantuoni C, Deep-Soboslay A, Becker KG, Lowe R, Huestis MA, Hyde TM, Kleinman JE, Freed WJ (2006) Transcriptional changes common to human cocaine, cannabis and phencyclidine abuse. PLoS One 1:e114. doi:10.1371/journal.pone.0000114
Numachi Y, Yoshida S, Yamashita M, Fujiyama K, Naka M, Matsuoka H, Sato M, Sora I (2004) Psychostimulant alters expression of DNA methyltransferase mRNA in the rat brain. Ann N Y Acad Sci 1025:102–109. doi:10.1196/annals.1316.013
Kumar A, Choi KH, Renthal W, Tsankova NM, Theobald DE, Truong HT, Russo SJ, Laplant Q, Sasaki TS, Whistler KN, Neve RL, Self DW, Nestler EJ (2005) Chromatin remodeling is a key mechanism underlying cocaine-induced plasticity in striatum. Neuron 48(2):303–314. doi:10.1016/j.neuron.2005.09.023
van Os J, Bak M, Hanssen M, Bijl RV, de Graaf R, Verdoux H (2002) Cannabis use and psychosis: a longitudinal population-based study. Am J Epidemiol 156(4):319–327. doi:10.1093/Aje/Kwf043
Khare M, Taylor AH, Konje JC, Bell SC (2006) Delta9-tetrahydrocannabinol inhibits cytotrophoblast cell proliferation and modulates gene transcription. Mol Hum Reprod 12(5):321–333. doi:10.1093/molehr/gal036
van Winkel R, van Beveren NJ, Simons C (2011) AKT1 moderation of cannabis-induced cognitive alterations in psychotic disorder. Neuropsychopharmacology 36(12):2529–2537. doi:10.1038/npp.2011.141
van Winkel R (2011) Family-based analysis of genetic variation underlying psychosis-inducing effects of cannabis: sibling analysis and proband follow-up. Arch Gen Psychiatry 68(2):148–157. doi:10.1001/archgenpsychiatry.2010.152
Franklin TB, Russig H, Weiss IC, Graff J, Linder N, Michalon A, Vizi S, Mansuy IM (2010) Epigenetic transmission of the impact of early stress across generations. Biol Psychiatry 68(5):408–415. doi:10.1016/j.biopsych.2010.05.036
Dias BG, Ressler KJ (2014) Parental olfactory experience influences behavior and neural structure in subsequent generations. Nat Neurosci 17(1):89–96. doi:10.1038/nn.3594
van Os J, Rutten BP, Poulton R (2008) Gene–environment interactions in schizophrenia: review of epidemiological findings and future directions. Schizophr Bull 34(6):1066–1082. doi:10.1093/schbul/sbn117
Niwa M, Jaaro-Peled H, Tankou S, Seshadri S, Hikida T, Matsumoto Y, Cascella NG, Kano S, Ozaki N, Nabeshima T, Sawa A (2013) Adolescent stress-induced epigenetic control of dopaminergic neurons via glucocorticoids. Science 339(6117):335–339. doi:10.1126/science.1226931
Davies MN, Volta M, Pidsley R, Lunnon K, Dixit A, Lovestone S, Coarfa C, Harris RA, Milosavljevic A, Troakes C, Al-Sarraj S, Dobson R, Schalkwyk LC, Mill J (2012) Functional annotation of the human brain methylome identifies tissue-specific epigenetic variation across brain and blood. Genome Biol 13(6):R43. doi:10.1186/gb-2012-13-6-r43
Horvath S, Zhang Y, Langfelder P, Kahn RS, Boks MP, van Eijk K, van den Berg LH, Ophoff RA (2012) Aging effects on DNA methylation modules in human brain and blood tissue. Genome Biol 13(10):R97. doi:10.1186/gb-2012-13-10-r97
Slieker RC, Bos SD, Goeman JJ, Bovee JV, Talens RP, van der Breggen R, Suchiman HE, Lameijer EW, Putter H, van den Akker EB, Zhang Y, Jukema JW, Slagboom PE, Meulenbelt I, Heijmans BT (2013) Identification and systematic annotation of tissue-specific differentially methylated regions using the Illumina 450 k array. Epigenetics Chromatin 6(1):26. doi:10.1186/1756-8935-6-26
Mill J, Heijmans BT (2013) From promises to practical strategies in epigenetic epidemiology. Nat Rev Genet 14(8):585–594. doi:10.1038/nrg3405
Dempster E, Viana J, Pidsley R, Mill J (2013) Epigenetic studies of schizophrenia: progress, predicaments, and promises for the future. Schizophr Bull 39(1):11–16. doi:10.1093/schbul/sbs139
Acknowledgments
JvO and BPFR have received funding from the European Community’s Seventh Framework Programme under Grant Agreement No. HEALTH-F2-2009-241909 (Project EU-GEI), and BPFR has received funding from the Netherlands Organisation for Scientific Research (NWO; VENI Award No. 916.11.086).
Conflict of interest
There is no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pishva, E., Kenis, G., van den Hove, D. et al. The epigenome and postnatal environmental influences in psychotic disorders. Soc Psychiatry Psychiatr Epidemiol 49, 337–348 (2014). https://doi.org/10.1007/s00127-014-0831-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-014-0831-2