Abstract
Purpose
This study aimed to evaluate the clinical features, prognostic factors, and survival outcomes for patients with intracranial nongerminomatous germ cell tumors (NGGCTs), with a particular focus on treatment toxicity for long-term survivors.
Methods
Intracranial NGGCTs treated with platinum-based chemotherapy and craniospinal irradiation (CSI) in our institution were retrospectively analyzed. Hematological complications following sequential chemoradiotherapy as well as height and weight in childhood survivors were evaluated. Plasma growth hormone (GH) concentrations prior to and after radiotherapy were obtained for the comparisons.
Results
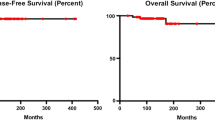
A total of 111 intracranial NGGCTs were included. The 3‑year overall survival (OS) and event-free survival (EFS) rates were 83.5% ± 3.9% and 71.0% ± 4.8%, respectively. A combined treatment modality consisting of ≥ 4 cycles of platinum-based chemotherapy and CSI was associated with an improved OS (P = 0.003) and EFS (P < 0.001). Thrombocytopenia of any grade occurred in 35.4% (34/96) of patients, and the threshold age for an increased risk of thrombocytopenia was 14 years (area under the curve AUC = 0.752, P < 0.0001) as derived from receiver operating characteristic (ROC) analysis. Growth impediment was found in 8 of 56 (14%) patients. The age for receiving radiotherapy was found to inversely correlate with height development, revealing a cut-off age of 11.5 years for risking growth impairment (AUC = 0.806, P = 0.004). Consistently, a significant decline in plasma growth hormone after radiotherapy was observed in patients ≤ 11.5 years (P < 0.01) but not patients > 11.5 years. (P > 0.05).
Conclusion
Our study suggested that a combined treatment modality with at least four cycles of chemotherapy and CSI was safe and effective for patients with intracranial NGGCTs. Radiotherapy should be used with caution for patients < 11.5 years due to growth impairment.




Similar content being viewed by others
References
Sano K (1999) Pathogenesis of intracranial germ cell tumors reconsidered. JNS 90(2):258–264
Kong Z, Wang Y, Dai C, Yao Y, Ma W, Wang Y (2018) Central nervous system germ cell tumors: a review of the literature. J Child Neurol 33(9):610–620
Cavenee WK, Louis DN, Ohgaki H, Wiestler OD (2007) WHO classification of tumours of the central nervous system vol 1. WHO Regional Office Europe,
Lee SH, Jung K‑W, Ha J, Oh C‑M, Kim H, Park HJ, Yoo H, Won Y‑J (2017) Nationwide population-based incidence and survival rates of malignant central nervous system germ cell tumors in Korea, 2005–2012. Cancer Res Treat 49(2):494
Matsutani M, Sano K, Takakura K, Fujimaki T, Nakamura O, Funata N, Seto T (1997) Primary intracranial germ cell tumors: a clinical analysis of 153 histologically verified cases. J Neurosurg 86(3):446–455. https://doi.org/10.3171/jns.1997.86.3.0446
Calaminus G, Andreussi L, Garré ML, Kortmann RD, Schober R, Göbel U (1997) Secreting germ cell tumors of the central nervous system (CNS). First results of the cooperative German/Italian pilot study (CNS sGCT). Klin Padiatr 209(4):222–227. https://doi.org/10.1055/s-2008-1043954
Calaminus G, Kortmann R, Worch J, Nicholson JC, Alapetite C, Garrè ML, Patte C, Ricardi U, Saran F, Frappaz D (2013) SIOP CNS GCT 96: final report of outcome of a prospective, multinational nonrandomized trial for children and adults with intracranial germinoma, comparing craniospinal irradiation alone with chemotherapy followed by focal primary site irradiation for patients with localized disease. Neuro-Oncology 15(6):788–796. https://doi.org/10.1093/neuonc/not019
Calaminus G, Frappaz D, Kortmann RD, Krefeld B, Saran F, Pietsch T, Vasiljevic A, Garre ML, Ricardi U, Mann JR, Göbel U, Alapetite C, Murray MJ, Nicholson JC (2017) Outcome of patients with intracranial non-germinomatous germ cell tumors-lessons from the SIOP-CNS-GCT-96 trial. Neuro-Oncology 19(12):1661–1672. https://doi.org/10.1093/neuonc/nox122
Goldman S, Bouffet E, Fisher PG, Allen JC, Robertson PL, Chuba PJ, Donahue B, Kretschmar CS, Zhou T, Buxton AB, Pollack IF (2015) Phase II trial assessing the ability of neoadjuvant chemotherapy with or without second-look surgery to eliminate measurable disease for nongerminomatous germ cell tumors: a children’s oncology group study. J Clin Oncol 33(22):2464–2471. https://doi.org/10.1200/jco.2014.59.5132
Fangusaro J, Wu S, MacDonald S, Murphy E, Shaw D, Bartels U, Khatua S, Souweidane M, Lu HM, Morris D, Panigrahy A, Onar-Thomas A, Fouladi M, Gajjar A, Dhall G (2019) Phase II trial of response-based radiation therapy for patients with localized CNS nongerminomatous germ cell tumors: a children’s oncology group study. J Clin Oncol 37(34):3283–3290. https://doi.org/10.1200/jco.19.00701
Odagiri K, Omura M, Hata M, Aida N, Niwa T, Ogino I, Kigasawa H, Ito S, Adachi M, Inoue T (2012) Treatment outcomes, growth height, and neuroendocrine functions in patients with intracranial germ cell tumors treated with chemoradiation therapy. Int J Radiat Oncol Biol Phys 84(3):632–638. https://doi.org/10.1016/j.ijrobp.2011.12.084
Tso WWY, Liu APY, Lee TMC, Cheuk KL, Shing MK, Luk CW, Ling SC, Ku DTL, Li K, Yung AWY, Fung CW, Chan SHS, Ho ACC, Ho FKW, Ip P, Chan GCF (2019) Neurocognitive function, performance status, and quality of life in pediatric intracranial germ cell tumor survivors. J Neurooncol 141(2):393–401. https://doi.org/10.1007/s11060-018-03045-3
Liang SY, Yang TF, Chen YW, Liang ML, Chen HH, Chang KP, Shan IK, Chen YS, Wong TT (2013) Neuropsychological functions and quality of life in survived patients with intracranial germ cell tumors after treatment. Neuro-Oncology 15(11):1543–1551. https://doi.org/10.1093/neuonc/not127
Sun X, Yang Q (2018) Consensus of multidisciplinary diagnosis and treatment on primary central nervous system germ cell tumors in children. J Chin Pediatr Blood Cancer 23(6):281–286
Fangusaro J, Wu S, MacDonald S, Murphy E, Shaw D, Bartels U, Khatua S, Souweidane M, Lu H‑M, Morris D, Panigrahy A, Onar-Thomas A, Fouladi M, Gajjar A, Dhall G (2019) Phase II trial of response-based radiation therapy for patients with localized CNS nongerminomatous germ cell tumors: a children’s oncology group study. J Clin Oncol 37(34):3283–3290. https://doi.org/10.1200/jco.19.00701
Li H, Ji CY, Zong XN, Zhang YQ (2009) Height and weight standardized growth charts for Chinese children and adolescents aged 0 to 18 years. Zhonghua Er Ke Za Zhi 47(7):487–492
Kim JW, Kim WC, Cho JH, Kim D‑S, Shim K‑W, Lyu CJ, Won SC, Suh C‑O (2012) A multimodal approach including craniospinal irradiation improves the treatment outcome of high-risk intracranial nongerminomatous germ cell tumors. Int J Radiat Oncol Biol Phys 84(3):625–631
Maity A, H‑KG S, Janss A, Belasco JB, Rorke L, Phillips PC, Sutton LN, Goldwein JW (2004) Craniospinal radiation in the treatment of biopsy-proven intracranial germinomas: twenty-five years’ experience in a single center. Int J Radiat Oncol Biol Phys 58(4):1165–1170
Robertson PL, DaRosso RC, Allen JC (1997) Improved prognosis of intracranial non-germinoma germ cell tumors with multimodality therapy. J Neurooncol 32(1):71–80
Baranzelli MC, Patte C, Bouffet E, Couanet D, Habrand JL, Portas M, Lejars O, Lutz P, Gall EL, Kalifa C (1997) Nonmetastatic intracranial germinoma: the experience of the French society of pediatric oncology. Cancer 80(9):1792–1797
Jennings MT, Gelman R, Hochberg F (1985) Intracranial germ-cell tumors: natural history and pathogenesis. J Neurosurg 63(2):155–167
Dearnaley D, A’hern R, Whittaker S, Bloom H (1990) Pineal and CNS germ cell tumors: Royal Marsden Hospital experience 1962–1987. Int J Radiat Oncol Biol Phys 18(4):773–781
Einhorn LH, Donohue J (1977) Cis-diamminedichloroplatinum, vinblastine, and bleomycin combination chemotherapy in disseminated testicular cancer. Ann Intern Med 87(3):293–298
Bosl GJ, Yagoda A, Whitmore JW, Sogani P, Herr H, Vugrin D, Dukeman M, Golbey R (1984) VP-16-213 and cisplatin in the treatment of patients with refractory germ cell tumors. Am J Clin Oncol 7(4):327–330
Matsukado Y, Abe H, Tanaka R, Kobayashi T, Yamashita J, Nishimoto A, Ushio Y, Sato K, Matsutani M, Takakura K (1986) Cisplatin, vinblastine and bleomycin (PVB) combination chemotherapy in the treatment of intracranial malignant germ cell tumors-—a preliminary report of a phase II study—the Japanese Intracranial germ cell tumor study group. Gan No Rinsho 32(11):1387–1393
Kellie SJ, Boyce H, Dunkel IJ, Diez B, Rosenblum M, Bruaidi L, Finlay JL (2004) Primary chemotherapy for intracranial nongerminomatous germ cell tumors: results of the second international CNS germ cell study group protocol. J Clin Oncol 22(5):846–853
Zhang J, Huang Y, Sun Y, He A, Zhou Y, Hu H, Yao Y, Shen Z (2019) Impact of chemotherapy cycles and intervals on outcomes of nonspinal Ewing sarcoma in adults: a real-world experience. BMC Cancer 19(1):1168
Yen M‑S, Twu N‑F, Lai C‑R, Horng H‑C, Chao K‑C, Juang C‑M (2009) Importance of delivered cycles and nomogram for intraperitoneal chemotherapy in ovarian cancer. Gynecol Oncol 114(3):415–419
Zhang W‑Y, Zhang W‑J, Bai Y, Yuan H‑H, Liu F, Gao J, Gong Y‑F, Jiang B (2013) Impact of adjuvant chemotherapy cycles on prognosis of resectable stomach cancer: a retrospective analysis. Asian Pac J Cancer Prev 14(1):381–386
Stevens SK, Moore SG, Kaplan ID (1990) Early and late bone-marrow changes after irradiation: MR evaluation. AJR Am J Roentgenol 154(4):745–750. https://doi.org/10.2214/ajr.154.4.2107669
Georgiou KR, Hui SK, Xian CJ (2012) Regulatory pathways associated with bone loss and bone marrow adiposity caused by aging, chemotherapy, glucocorticoid therapy and radiotherapy. Am J Stem Cells 1(3):205–224
Alapetite C, Brisse H, Patte C, Raquin MA, Gaboriaud G, Carrie C, Habrand JL, Thiesse P, Cuilliere JC, Bernier V, Ben-Hassel M, Frappaz D, Baranzelli MC, Bouffet E (2010) Pattern of relapse and outcome of non-metastatic germinoma patients treated with chemotherapy and limited field radiation: the SFOP experience. Neuro-Oncology 12(12):1318–1325. https://doi.org/10.1093/neuonc/noq093
De B, Cahlon O, Dunkel IJ, De Braganca KC, Khakoo Y, Gilheeney SW, Souweidane MM, Wolden SL (2017) Reduced-volume radiotherapy for patients with localized intracranial nongerminoma germ cell tumors. J Neurooncol 134(2):349–356
Darzy KH, Shalet SM (2005) Hypopituitarism as a consequence of brain tumours and radiotherapy. Pituitary 8(3–4):203–211. https://doi.org/10.1007/s11102-006-6042-4
Aoyama H, Shirato H, Yoshida H, Hareyama M, Nishio M, Yanagisawa T, Kakuto Y, Watarai J, Inakoshi H, Miyasaka K (1998) Retrospective multi-institutional study of radiotherapy for intracranial non-germinomatous germ cell tumors. Radiother Oncol 49(1):55–59
Lam KS, Wang C, Yeung RT, Ma JT, Ho JH, Tse VK, Ling N (1986) Hypothalamic hypopituitarism following cranial irradiation for nasopharyngeal carcinoma. Clin Endocrinol (Oxf) 24(6):643–651. https://doi.org/10.1111/j.1365-2265.1986.tb01660.x
Brauner R, Fontoura M, Zucker JM, Devergie A, Souberbielle JC, Prevot-Saucet C, Michon J, Gluckman E, Griscelli C, Fischer A et al (1993) Growth and growth hormone secretion after bone marrow transplantation. Arch Dis Child 68(4):458–463. https://doi.org/10.1136/adc.68.4.458
Funding
This work was supported by the Natural Science Foundation of Guangdong Province (No. 2019A1515011943), China Postdoctoral Science Foundation (2020T130052ZX and 2019M662974), Science and Technology Program of Guangzhou (No. 202002030445, 202002030086), and Medical Scientific Research Foundation of Guangdong Province (No. A2020505, No.2020499, No. B2021203, No.B2021139). The funders had no role in study design, data collection and analysis, decision to publish or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
Dr. Lei Wen and Dr. Juan Li conceptualized and designed the study, drafted the initial manuscript, and reviewed and revised the manuscript. Dr. Mingyao Lai, Dr. Qingjun Hu, Dr. Changguo Shan and Dr. Hainan Li collected data, carried out the initial analyses and revised the manuscript. Dr. Ming Lu, Dr. Liang Zhang, Dr. Taihua Wu, Dr. Dan Zhu, Dr. Yuanyuan Chen and Dr. Longhua Chen helped in reviewing, acquisition, analysis and interpretation of clinical data for the work. Dr. Cheng Zhou and Dr. Linbo Cai conceptualized and designed the study, coordinated and supervised data collection, and critically revised the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding authors
Ethics declarations
Conflict of interest
L. Wen, J. Li, M. Lai, Z. Zhou, Q. Hu, G. Deng, C. Shan, R. Ai, H. Li, M. Lu, L. Zhang, T. Wu, D. Zhu, Y. Chen, L. Chen, L. Cai and C. Zhou declare that they have no competing interests.
Ethical standards
This retrospective study was approved by the Institutional Review Board with a waiver for informed consent.
Additional information
The authors Lei Wen and Juan Li contributed equally to the manuscript.
Category of study: clinical research article
Supplementary Information
66_2021_1857_MOESM3_ESM.docx
Table S1. Univariate and multivariate analysis of risk factors for event-free survival in 111 intracranial NGGCTs patients.
Rights and permissions
About this article
Cite this article
Wen, L., Li, J., Lai, M. et al. Survival outcomes, hematologic complications and growth impairment after sequential chemoradiotherapy in intracranial NGGCTs: a retrospective study. Strahlenther Onkol 198, 458–467 (2022). https://doi.org/10.1007/s00066-021-01857-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-021-01857-3