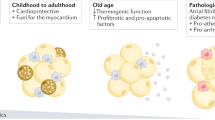
Abstract
Background
The aim of this study was to assess the role of lipolysis of epicardial adipose tissue (EAT) in cardiac function after myocardial infarction (MI).
Methods
We used a rat model of MI with or without EAT removal to study the effects of EAT lipolysis on cardiovascular function. Echocardiography and cardiac catheterization were used to determine cardiac function, and infarct size and histopathology specimens were analyzed in postmortem sections. Inflammatory responses were evaluated via flow cytometry and Elisa analyses.
Results
We found that the lipolysis of EAT increased significantly after MI. Removal of the EAT after MI (MI-EAT) improved cardiac function by nearly 10% and decreased the infarct area by 6% when compared with rats retaining EAT after MI (MI+EAT). Furthermore, the removal of EAT reduced the number of CD45-positive leukocytes (50 vs. 34.8%) and increased the ratio of macrophage/leukocytes (56 vs. 75%) in the infarcted heart. Compared with the MI+EAT group, the concentration of tumor necrosis factor-alpha and interleukin 1‑beta were reduced in the MI-EAT group.
Conclusion
Lipolysis of EAT increased significantly after MI. Removal of EAT improved cardiac function, in part, by weakening the inflammatory response.
Zusammenfassung
Hintergrund
Ziel der vorliegenden Studie war es, die Bedeutung der Lipolyse von epikardialem Fettgewebe (EAT, „epicardial adipose tissue“) für die Herzfunktion nach Myokardinfarkt (MI) zu untersuchen.
Methoden
Die Autoren verwendeten ein Rattenmodell des MI mit oder ohne Fettentfernung, um die Auswirkungen der Lipolyse des EAT auf die kardiovaskuläre Funktion zu untersuchen. Mit der Echokardiographie und der Herzkatheteruntersuchung wurde die Herzfunktion erfasst. Infarktgröße und Histopathologie wurden anhand der Obduktionsbefunde ermittelt. Entzündliche Reaktionen wurden mittels Durchflusszytometrie und ELISA-Tests untersucht.
Ergebnisse
Die Autoren stellten fest, dass die Lipolyse des EAT nach MI signifikant anstieg. Die Entfernung des EAT nach MI (MI-EAT) führte zur Verbesserung der Herzfunktion um fast 10% und zur Abnahme des Infarktareals um 6% im Vergleich zu Ratten mit erhaltenem EAT nach MI (MI+EAT). Außerdem kam es durch die Entfernung des EAT zur Verminderung der Anzahl CD45-positiver Leukozyten (50 vs. 34,8%) und zum Anstieg des Quotienten aus Makrophagen und Leukozyten (56 vs. 75%) im infarzierten Herzgewebe. Gegenüber der MI+EAT-Gruppe waren die Werte für Tumornekrosefaktor-alpha und Interleukin 1‑beta in der MI-EAT-Gruppe vermindert.
Schlussfolgerung
Die Lipolyse des EAT nahm signifikant nach MI zu. Mit der Entfernung des EAT kam es zur verbesserten Herzfunktion, teilweise durch Abschwächung der Entzündungsreaktion.




Similar content being viewed by others
References
Klionsky DJ, Abdelmohsen K, Abe A et al (2016) Guidelines for the use and interpretation of assays for monitoring autophagy (3rd edition). Autophagy 12(1):1–222
Sacks HS, Fain JN (2007) Human epicardial adipose tissue: a review. Am Heart J 153(6):907–917
Cherian S, Lopaschuk GD, Carvalho E (2012) Cellular cross-talk between epicardial adipose tissue and myocardium in relation to the pathogenesis of cardiovascular disease. Am J Physiol Endocrinol Metab 303(8):E937–E949
Nakazato R, Shmilovich H, Tamarappoo BK et al (2011) Interscan reproducibility of computer-aided epicardial and thoracic fat measurement from noncontrast cardiac CT. J Cardiovasc Comput Tomogr 5(3):172–179
Iacobellis G, Willens HJ, Barbaro G, Sharma AM (2008) Threshold values of high-risk echocardiographic epicardial fat thickness. Obesity 16(4):887–892
Nelson AJ, Worthley MI, Psaltis PJ et al (2009) Validation of cardiovascular magnetic resonance assessment of pericardial adipose tissue volume. J Cardiovasc Magn Reson 11:15
Iacobellis G, Corradi D, Sharma AM (2005) Epicardial adipose tissue: anatomic, biomolecular and clinical relationships with the heart. Nat Clin Pract Cardiovasc Med 2(10):536–543
Nichols JH, Samy B, Nasir K et al (2008) Volumetric measurement of pericardial adipose tissue from contrast-enhanced coronary computed tomography angiography: a reproducibility study. J Cardiovasc Comput Tomogr 2(5):288–295
Mahabadi AA, Massaro JM, Rosito GA et al (2009) Association of pericardial fat, intrathoracic fat, and visceral abdominal fat with cardiovascular disease burden: the Framingham Heart Study. Eur Heart J 30(7):850–856
Rosito GA, Massaro JM, Hoffmann U et al (2008) Pericardial fat, visceral abdominal fat, cardiovascular disease risk factors, and vascular calcification in a community-based sample: the Framingham Heart Study. Circulation 117(5):605–613
Ding J, Hsu FC, Harris TB et al (2009) The association of pericardial fat with incident coronary heart disease: the Multi-Ethnic Study of Atherosclerosis (MESA). Am J Clin Nutr 90(3):499–504
Chaldakov GN, Fiore M, Stankulov IS et al (2004) Neurotrophin presence in human coronary atherosclerosis and metabolic syndrome: a role for NGF and BDNF in cardiovascular disease? Prog Brain Res 146:279–289
Kremen J, Dolinkova M, Krajickova J et al (2006) Increased subcutaneous and epicardial adipose tissue production of proinflammatory cytokines in cardiac surgery patients: possible role in postoperative insulin resistance. J Clin Endocrinol Metab 91(11):4620–4627
Marchington JM, Pond CM (1990) Site-specific properties of pericardial and epicardial adipose tissue: the effects of insulin and high-fat feeding on lipogenesis and the incorporation of fatty acids in vitro. Int J Obes 14(12):1013–1022
Anzai A, Anzai T, Nagai S et al (2012) Regulatory role of dendritic cells in postinfarction healing and left ventricular remodeling. Circulation 125(10):1234–1245
Haunso S, Paaske WP, Sejrsen P, Amtorp O (1980) Capillary permeability in canine myocardium as determined by bolus injection, residue detection. Acta Physiol Scand 108(4):389–397
Shichita T, Sugiyama Y, Ooboshi H et al (2009) Pivotal role of cerebral interleukin-17-producing gammadeltaT cells in the delayed phase of ischemic brain injury. Nat Med 15(8):946–950
Yan X, Anzai A, Katsumata Y et al (2013) Temporal dynamics of cardiac immune cell accumulation following acute myocardial infarction. J Mol Cell Cardiol 62:24–35
Deng J, Liu S, Zou L, Xu C, Geng B, Xu G (2012) Lipolysis response to endoplasmic reticulum stress in adipose cells. J Biol Chem 287(9):6240–6249
Robert-Sargeant S, Doyle W (1993) Fats of life (continuing education credit). Nurs Stand 7(26 Suppl NU):9–16
Resorlu H, Akbal A, Resorlu M et al (2015) Epicardial adipose tissue thickness in patients with ankylosing spondylitis. Clin Rheumatol 34(2):295–299
Vahdat K, Azizi F, Zandi K, Assadi M, Nabipour I (2012) Chronic inflammation is correlated with percentage of body fat independent of the burden of infection. Inflammation 35(4):1322–1329
Alp H, Eklioglu BS, Atabek ME et al (2014) Evaluation of epicardial adipose tissue, carotid intima-media thickness and ventricular functions in obese children and adolescents. J Pediatr Endocrinol Metab 27(9–10):827–835
Burgeiro A, Fuhrmann A, Cherian S et al (2016) Glucose uptake and lipid metabolism are impaired in epicardial adipose tissue from heart failure patients with or without diabetes. Am J Physiol Endocrinol Metab 310(7):E550–E564
Marchington JM, Mattacks CA, Pond CM (1989) Adipose tissue in the mammalian heart and pericardium: structure, foetal development and biochemical properties. Comp Biochem Physiol B 94(2):225–232
Volkova LP, Bondarenko MI, Severin NF (1981) Lipid peroxide and free fatty acid dynamics in acute myocardial infarct. Vrach Delo 12:35–38
Fazekas T, Szekeres L (1989) Effects of the lipolysis inhibiting agent beta-pyridylcarbinol (Ronicol) in acute myocardial ischaemia. Acta Physiol Hung 74(2):169–174
Mattacks CA, Pond CM (1988) Site-specific and sex differences in the rates of fatty acid/triacylglycerol substrate cycling in adipose, tissue and muscle of sedentary and exercised dwarf hamsters (Phodopus sungorus). Int J Obes 12(6):585–597
Fitzgibbons TP, Czech MP (2014) Epicardial and perivascular adipose tissues and their influence on cardiovascular disease: basic mechanisms and clinical associations. J Am Heart Assoc 3(2):e000582
Mazurek T, Zhang L, Zalewski A et al (2003) Human epicardial adipose tissue is a source of inflammatory mediators. Circulation 108(20):2460–2466
Ouwens DM, Sell H, Greulich S, Eckel J (2010) The role of epicardial and perivascular adipose tissue in the pathophysiology of cardiovascular disease. J Cell Mol Med 14(9):2223–2234
Bell D, Jackson M, Nicoll JJ, Millar A, Dawes J, Muir AL (1990) Inflammatory response, neutrophil activation, and free radical production after acute myocardial infarction: effect of thrombolytic treatment. Br Heart J 63(2):82–87
Nah DY, Rhee MY (2009) The inflammatory response and cardiac repair after myocardial infarction. Korean Circ J 39(10):393–398
Frangogiannis NG, Smith CW, Entman ML (2002) The inflammatory response in myocardial infarction. Cardiovasc Res 53(1):31–47
van Amerongen MJ, Harmsen MC, van Rooijen N, Petersen AH, van Luyn MJ (2007) Macrophage depletion impairs wound healing and increases left ventricular remodeling after myocardial injury in mice. Am J Pathol 170(3):818–829
Acknowledgements
This work was supported by the National Natural Science Foundation of China (No: 81170177, 81030002, and 8147054).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
H.-X. Chang, X.-J. Zhao, Q.-L. Zhu, Q. Hou, and Y. Li declare that they have no competing interests.
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Additional information
Hai-Xia Chang and Xiao-Jing Zhao contributed equally to this work.
Rights and permissions
About this article
Cite this article
Chang, H., Zhao, X., Zhu, Q. et al. Removal of epicardial adipose tissue after myocardial infarction improves cardiac function. Herz 43, 258–264 (2018). https://doi.org/10.1007/s00059-017-4555-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-017-4555-4