Abstract
Purpose
Systematic knowledge about the prevalence and the treatment effects of cancer pain in patients attending a general oncology outpatient department is limited. The purpose of this study was to investigate the prevalence of pain in a large representative cohort of patients attending a general oncology outpatient department in order to guide further screening, classification, and treatment of pain.
Material and methods
A cross-sectional study among patients visiting the outpatient clinic with histologically verified cancer, age ≥18 years, adequate cognitive function, and no surgical procedures last 24 h were included. Pain was assessed by the Brief Pain Inventory and the Alberta Breakthrough Pain Assessment Tool.
Results
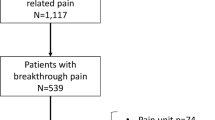
Three hundred five patients were included. The mean age was 60 years, 94 % had a WHO performance status of 0–1 and 59 % received oncological treatment with a curative intent. The mean score for average pain last 24 h (numerical rating scale, 0–10) and current pain was 1.84 and 1.08, respectively. Twenty-two percent reported pain score of ≥4 as their average pain in the previous 24 h. Twenty-one percent reported breakthrough pain (BTP). In multivariate analyses, sleep, BTP, age, treatment intent, and comorbidity was significantly associated with mean average pain in the previous 24 h and explained 29 % of the variability of average pain in the previous 24 h.
Conclusion
Of the patients at an oncology outpatient clinic, 22 % reported clinically significant pain. These findings indicate that all patients are candidates to be screened for pain and, if present, a more detailed pain diagnosis should be established before any interventions can be recommended.
Similar content being viewed by others
References
Barbera L, Seow H, Howell D, Sutradhar R, Earle C, Liu Y, Stitt A, Husain A, Sussman J, Dudgeon D (2010) Symptom burden and performance status in a population-based cohort of ambulatory cancer patients. Cancer 116:5767–5776
Cleeland CS (1989) Measurement of pain by subjective report. In: Chapman CR, Loeser JD (eds) Advances in pain research and therapy. Raven, New York, pp 391–403
O’Connor M, Weir J, Butcher I, Kleiboer A, Murray G, Sharma N, Thekkumpurath P, Walker J, Fallon M, Storey DJ, Sharpe M (2011) Pain in patients attending a specialist cancer service: prevalence and association with emotional distress. J Pain Symptom Manage 43(1):29–38
Mercadante S, Radbruch L, Caraceni A, Cherny N, Kaasa S, Nauck F, Ripamonti C, De Conno F (2002) Episodic (breakthrough) pain: Consensus Conference of an Expert Working Group of the European Association for Palliative Care. Cancer 94:832–839
Zeppetella G, O’Doherty CA, Collins S (2000) Prevalence and characteristics of breakthrough pain in cancer patients admitted to a hospice. J Pain Symptom Manage 20:87–92
Portenoy RK, Hagen NA (1990) Breakthrough pain: definition, prevalence and characteristics. Pain 41:273–281
Payne R (2007) Recognition and diagnosis of breakthrough pain. Pain Med 8(Suppl 1):S3–S7
Portenoy RK, Bruns D, Shoemaker B, Shoemaker SA (2010) Breakthrough pain in community-dwelling patients with cancer pain and noncancer pain, part 1: prevalence and characteristics. J Opioid Manag 6:97–108
Valeberg BT, Miaskowski C, Hanestad BR, Bjordal K, Moum T, Rustoen T (2008) Prevalence rates for and predictors of self-reported adherence of oncology outpatients with analgesic medications. Clin J Pain 24:627–636
Fainsinger RL, Nekolaichuk C, Lawlor P, Hagen N, Bercovitch M, Fisch M, Galloway L, Kaye G, Landman W, Spruyt O, Zhukovsky D, Bruera E, Hanson J (2010) An international multicentre validation study of a pain classification system for cancer patients. Eur J Cancer 46:2896–2904
Knudsen AK, Brunelli C, Kaasa S, Apolone G, Corli O, Montanari M, Fainsinger R, Aass N, Fayers P, Caraceni A, Klepstad P, European Palliative Care Research Collaborative, European Pharmacogenetic Study (2011) Which variables are associated with pain intensity and treatment response in advanced cancer patients? Implications for a future classification system for cancer pain. Eur J Pain 15:320–327
Cleeland CS (1991) Pain assessment in cancer. CRC Press, Boca Raton
Daut RL, Cleeland CS, Flanery RC (1983) Development of the Wisconsin Brief Pain Questionnaire to assess pain in cancer and other diseases. Pain 17:197–210
Hagen N, Stiles C, Nekolaichuk C, Biondo P, Carlson L, Fisher K, Fainsinger R (2008) The Alberta Breakthrough Pain Assessment Tool for Cancer Patients: a validation study using a Delphi process and patient think-aloud interviews. J Pain Symptom Manage 17:136–152
Klepstad P, Loge JH, Borchgrevink PC, Mendoza TR, Cleeland CS, Kaasa S (2002) The Norwegian Brief Pain Inventory Questionnaire: translation and validation in cancer pain patients. J Pain Symptom Manage 24:517–525
Cleeland CS, Gonin R, Hatfield AK, Edmonson JH, Blum RH, Stewart JA, Pandya KJ (1994) Pain and its treatment in outpatients with metastatic cancer. N Engl J Med 330:592–596
Shvartzman P, Friger M, Shani A, Barak F, Yoram C, Singer Y (2003) Pain control in ambulatory cancer patients—can we do better? J Pain Symptom Manage 26:716–722
Davies A, Zeppetella G, Andersen S, Damkier A, Vejlgaard T, Nauck F, Radbruch L, Sjolund KF, Stenberg M, Buchanan A (2011) Multi-centre European study of breakthrough cancer pain: pain characteristics and patient perceptions of current and potential management strategies. Eur J Pain 15:756–763
Portenoy RK, Payne D, Jacobsen P (1999) Breakthrough pain: characteristics and impact in patients with cancer pain. Pain 81:129–134
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Groll DL, To T, Bombardier C, Wright JG (2005) The development of a comorbidity index with physical function as the outcome. J Clin Epidemiol 58:595–602
Klepstad P, Fladvad T, Skorpen F, Bjordal K, Caraceni A, Dale O, Davies A, Kloke M, Lundstrom S, Maltoni M, Radbruch L, Sabatowski R, Sigurdardottir V, Strasser F, Fayers PM, Kaasa S (2011) Influence from genetic variability on opioid use for cancer pain: a European genetic association study of 2294 cancer pain patients. Pain 152:1139–1145
Hjermstad MJ, Lie HC, Caraceni A, Currow DC, Fainsinger RL, Gundersen OE, Haugen DF, Heitzer E, Radbruch L, Stone PC, Strasser F, Kaasa S, Loge JH (2012) Computer-based symptom assessment is feasible in patients with advanced cancer: results from an international multicenter study, the EPCRC-CSA. J Pain Symptom Manage 44:639–654
Fainsinger RL, Nekolaichuk CL (2008) A “TNM” classification system for cancer pain: the Edmonton Classification System for Cancer Pain (ECS-CP). Support Care Cancer 16:547–555
Knudsen AK, Brunelli C, Klepstad P, Aass N, Apolone G, Corli O, Montanari M, Caraceni A, Kaasa S (2012) Which domains should be included in a cancer pain classification system? Analyses of longitudinal data. Pain 153:696–703
Acknowledgments
Rita Fossbakk and May Remmem, nurse practitioners at the Department of Oncology, University Hospital in Trondheim, Norway, participated in outlining the preliminary framework of the study and data collection.
Conflict of interests
Pål Klepstad declares an advisory role in Orion Pharma; however, this company has not been involved in or sponsored the present study. The other authors of this article declare no conflict of interest. The first author has full control of all primary data and agrees to allow the journal to review the data if requested.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Raj, S.X., Thronaes, M., Brunelli, C. et al. A cross-sectional study on prevalence of pain and breakthrough pain among an unselected group of outpatients in a tertiary cancer clinic. Support Care Cancer 22, 1965–1971 (2014). https://doi.org/10.1007/s00520-014-2178-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-014-2178-3