Abstract
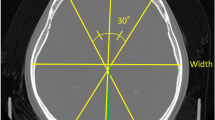
Prior to computed tomography (CT), plain skull radiographs were often the first study in the patient with suspected central nervous system disease (Shapiro and Robinson 1980). Subtle clues to the intracranial contents could be discerned by the presence of calcification, skull erosion, and signs of increased intracranial pressure, as with demineralization of the sellae or an increase in the size of mastoid emissary veins, as well as by recognition of diseases primarily affecting the osseous structure of the skull in the form of sclerotic and/or lytic lesions (Fig. 1). CT revolutionized the radiologist’s ability to see the intrinsic structure of the skull in cross-section. This has decreased the demand for skull x-rays. Magnetic resonance imaging (MRI) has further decreased the demands for skull films, by showing the intracranial contents even more exquisitely than CT. Today, the skull radiograph plays a relatively limited role in the evaluation of the pediatric patient. Except in the evaluation of trauma, craniosynostosis, and known genetic diseases affecting the cranial structures, the skull x-ray tends to be a procedure that follows the recognition of its need on the basis of another examination, such as CT, MRI, or the radionuclide study.
Similar content being viewed by others
References
Bartynski WS, Barnes PD, Wallman JK. Cranial CT of autosomal recessive osteoporosis. AJNR Am J Neuroradiol. 1989;10:543–50.
Fernbach SK, Naidich TP. Radiological evaluation of craniosynostosis. In: Cohen Jr MM, editor. Craniosynostosis: diagnosis, evaluation and management. New York: Raven; 1986. p. 191–214.
Friend SH, Bernards R, Rogelj S, Weinberg RA, Rapaport JM, Albert DM, Dryja TP. A human DNA segment with properties of the gene that predisposes to retinoblastoma and osteosarcoma. Nature. 1986;232:643–6.
Greenberg HS, Deck MD, Vikram B, Chu FC, Posner JB. Metastasis to the base of the skull: clinical findings in 43 patients. Neurology. 1981;31:530–7.
Hecht JT, Nelson FW, Butler IJ, Horton WA, Scott Jr CI, Wassman ER, Mehringer CM, Rimoin DL, Pauli RM. Computed tomography of the foramen magnum: achondroplastic values compared to normal standards. Am J Med Genet. 1985;20:355–60.
Jarvis JL, Keats TE. Cleidocranial dysostosis. AJNR Am J Neuroradiol. 1974;121:5–16.
Kornreich L, Grunebaum M, Ziv N, Cohen Y. Osteogenic sarcoma of the calvarium in children: CT manifestations. Neuroradiology. 1988;30:439–41.
Lee YY, Van Tassel P. Craniofacial chondrosarcomas: imaging findings in 15 untreated cases. AJNR Am J Neuroradiol. 1989;10:165–70.
Lee YY, Van Tassell P, Raymond AK. Intracranial dural chondrosarcoma. AJNR Am J Neuroradiol. 1988;9:1189–93.
Lipson SJ. Dysplasia of the odontoid process in Morquio’s syndrome causing quadriparesis. J Bone Joint Surg. 1977;59A:340–4.
Madeline LA, Elster AD. Suture closure in the human chondrocranium: CT assessment. Radiology. 1995;196:747–56.
Meyer J, Oot R, Lindfors K. CT appearance of clival chordomas. J Comput Assist Tomogr. 1986;10:34–8.
Moore JB, Kulkarni R, Crutcher DC, Bhimani S. MRI in multifocal eosinophilic granuloma: staging disease and monitoring response to therapy. Am J Pediatr Hematol Oncol. 1989;11:174–7.
Oot RF, Melville GE, New PF, Austin-Seymour M, Munzenrider J, Pile-Spellman J, Spagnoli M, Shoukimas GM, Momose KJ, Carroll R, et al. The role of MR and CT in evaluating clival chordomas and chondrosarcomas. AJR Am J Roentgenol. 1988;151:567–75.
Pozo JL, Crockar HA. Ransford AO. Basilar impression in osteogenesis imperfecta. J Bone Joint Surg (Br). 1984;66:233.
Rawlings CE, Wilkins RH. Solitary eosinophilic granuloma of the skull. Neurosurgery. 1984;15:155–61.
Rousseau F, Bonaventure J, Legeai-Mallet L, Pelet A, Rozet JM, Maroteaux P, Le Merrer M, Munnich A. Mutations in the gene encoding fibroblast growth factor receptor-3 in achondroplasia. Nature. 1994;371:252–4.
Shapiro R, Robinson F. The embryogenesis of the human skull: an anatomic and radiographic atlas. Cambridge, MA: Harvard University Press; 1980.
Shiang R, Thompson LM, Zhu YZ, Church DM, Fielder TJ, Bocian M, Winokur ST, Wasmuth JJ. Mutations in the transmembrane domain of FGFR3 cause the most common genetic form of dwarfism, achondroplasia. Cell. 1994;78:335–42.
Sulik KK, Johnston MC, Smiley SJ, Speight HS, Jarvis BE. Mandibulofacial dysostosis (Treacher Collins syndrome): a new proposal for its pathogenesis. Am J Med Genet. 1987;27:359–72.
Sze G, Uichanco III LS, Brant-Zawadzki MN, Davis RL, Gutin PH, Wilson CB, Norman D, Newton TH. Chordomas: MR imaging. Radiology. 1988;166:187–91.
Tefft M, Fernandez C, Donaldson M, Newton W, Moon TE. Incidence of meningeal involvement by rhabdomyosarcoma of the head and neck in children: a report of the Intergroup Rhabdomyosarcoma Study (IRS). Cancer. 1978;42:253–8.
Thomas SL, Childress MH, Quinton B. Hypoplasia of the odontoid with atlanto-axial subluxation in Hurler’s syndrome. Pediatr Radiol. 1985;15:353–4.
Watts RW, Spellacy E, Kendall BE, du Boulay G, Gibbs DA. Computed tomography studies on patients with mucopolysaccharidoses. Neuroradiology. 1981;21:9–23.
Zimmerman RA, Bilaniuk LT. Age related incidence of pineal calcification detected by CT. Radiology. 1982;142:659–62.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer-Verlag Berlin Heidelberg
About this entry
Cite this entry
Zimmerman, R.A. (2016). Skull Development and Abnormalities. In: Rossi, A. (eds) Pediatric Neuroradiology. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-662-46258-4_60-1
Download citation
DOI: https://doi.org/10.1007/978-3-662-46258-4_60-1
Received:
Accepted:
Published:
Publisher Name: Springer, Berlin, Heidelberg
Online ISBN: 978-3-662-46258-4
eBook Packages: Springer Reference MedicineReference Module Medicine