Abstract
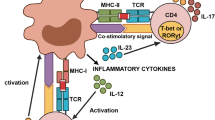
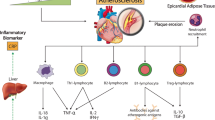
Inflammation is a critical driver of all stages of atherosclerosis, from lesion development to plaque rupture. Cytokines are mediators of the immune response and in atherosclerosis, the balance of anti- and pro-inflammatory cytokines is tipped in favor of the latter, resulting in persistent and unresolved inflammation. Although reducing plasma cholesterol levels mainly via the use of statins has positively impacted patient outcomes and reduced mortality rates, the presence of significant residual inflammation and cardiovascular risk posttherapy emphasizes the prevailing risk of primary and secondary events driven by inflammation independently of hyperlipidemia. Given the dominant role of inflammation in driving pathogenesis, alternative therapeutic avenues beyond targeting lowering of plasma lipids are required. This chapter will discuss the role of inflammation and pro-inflammatory cytokines in driving atherogenesis and disease progression, the therapeutic potential of targeting cytokines for atherosclerosis and promising avenues in this area.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Banyer JL, Hamilton NH, Ramshaw IA et al (2000) Cytokines in innate and adaptive immunity. Rev Immunogenet 2(3):359–373
Ait-Oufella H, Taleb S, Mallat Z et al (2011) Recent advances on the role of cytokines in atherosclerosis. Arterioscler Thromb Vasc Biol 31:969–979
Ramji DP, Davies TS (2015) Cytokines in atherosclerosis: key players in all stages of disease and promising therapeutic targets. Cytokine Growth Factor Rev 26:673–685
Moss JWE, Ramji DP (2016) Cytokines: roles in atherosclerosis disease progression and potential therapeutic targets. Future Med Chem 8(11):1317–1330
Tousoulis D, Oikonomou E, Economou EK et al (2016) Inflammatory cytokines in atherosclerosis: current therapeutic approaches. Eur Heart J 37(22):1723–1732
Tedgui A, Mallat Z (2006) Cytokines in atherosclerosis: pathogenic and regulatory pathways. Physiol Rev 86:515–581
Libby P (2017) Interleukin-1 beta as a target for atherosclerosis therapy: the biological basis of CANTOS and beyond. J Am Coll Cardiol 70(18):2278–2289
Lichtman AH, Binder CJ, Tsimikas S et al (2013) Adaptive immunity in atherogenesis: new insights and therapeutic approaches. J Clin Invest 123:27–36
Nus M, Mallat Z (2016) Immune-mediated mechanisms of atherosclerosis and implications for the clinic. Expert Rev Clin Immunol 12:1217–1237
Hansson GK, Libby P, Tabas I (2015) Inflammation and plaque vulnerability. J Intern Med 278:483–493
Libby P, Ridker PM, Hansson GK (2009) Inflammation in atherosclerosis: from pathophysiology to practice. J Am Coll Cardiol 54:2129–2138
Mason JC, Libby P (2015) Cardiovascular disease in patients with chronic inflammation: mechanisms underlying premature cardiovascular events in rheumatologic conditions. Eur Heart J 36:428–484
McLaren JE, Michael DR, Ashlin TG et al (2011) Cytokines, macrophage lipid metabolism and foam cells: implications for cardiovascular disease therapy. Prog Lipid Res 50:331–347
Shirai T, Hilhorst M, Harrison DG et al (2015) Macrophages in vascular inflammation - from atherosclerosis to vasculitis. Autoimmunity 48(3):139–151
Stewart CR, Stuart LM, Wilkinson K et al (2010) CD36 ligands promote sterile inflammation through assembly of a Toll-like receptor 4 and 6 heterodimer. Nat Immunol 11(2):155–161
Tall AR, Yven-Charvet L (2015) Cholesterol, inflammation and innate immunity. Nat Rev Immunol 15:104–116
Dinarello CA (2018) Overview of the IL-1 family in innate inflammation and acquired immunity. Immunol Rev 281:8–27
Garlanda C, Dinarello CA, Mantovani A et al (2013) The interleukin-1 family: back to the future. Immunity 39:1003–1018
Dinarello CA (2009) Immunological and inflammatory functions of the interleukin-1 family. Annu Rev Immunol 27:519–550
Libby P, Ordovas JM, Auger KR et al (1986) Endotoxin and tumor necrosis factor induce interleukin-1 gene expression in adult human vascular endothelial cells. Am J Pathol 124:179–186
Libby P, Ordovas JM, Birinyi LK et al (1986) Inducible interleukin-1 expression in human vascular smooth muscle cells. J Clin Invest 78:1432–1438
Wolfs IMJ, Donners MMPC, de Winther MPJ (2011) Differentiation factors and cytokines in the atherosclerotic plaque micro-environment as a trigger for macrophage polarisation. Thromb Haemost 106(5):763–771
Chinetti-Gbaguidi G, Colin S, Staels B (2015) Macrophage subsets in atherosclerosis. Nat Rev Cardiol 12(1):10–17
Leitinger N, Schulman IG (2013) Phenotypic polarization of macrophages in atherosclerosis. Arterioscler Thromb Vasc Biol 33(6):1120–1126
Libby P, Warner SJ, Friedman GB (1988) Interleukin 1: a mitogen for human vascular smooth muscle cells that induces the release of growth-inhibitory prostanoids. J Clin Invest 81:487–498
Khallou-Laschet J, Varthaman A, Fornasa G et al (2010) Macrophage plasticity in experimental atherosclerosis. PLoS One 5:e8852
Robertson AK, Hansson GK (2006) T cells in atherogenesis: for better or for worse? Arterioscler Thromb Vasc Biol 26:2421–2432
Zhang H, Park Y, Wu J et al (2009) Role of TNF-α in vascular dysfunction. Clin Sci 116:219–230
Pober JS, Sessa WC (2007) Evolving functions of endothelial cells in inflammation. Nat Rev Immunol 7(10):803–815
Frostegard J (2013) Immunity, atherosclerosis and cardiovascular disease. BMC Med 11:117. https://doi.org/10.1186/1741-7015-11-117
Dinarello CA, Ikejima T, Warner SJC et al (1987) Interleukin-1 induces interleukin-1. I. Induction of circulating interleukin-1 in rabbits in vivo and in human mononuclear cells in vitro. J Immunol 139:1902–1910
Warner SJC, Auger KR, Libby P (1987) Interleukin-1 induces interleukin-1. II. Recombinant human interleukin-1 induces interleukin-1 production by adult human vascular endothelial cells. J Immunol 139:1911–1917
Patel MN, Carroll RG, Galvan-Pena S et al (2017) Inflammasome priming in sterile inflammatory disease. Trends Mol Med 23(2):165–180
Geng Y-J, Libby P (1995) Evidence for apoptosis in advanced human atheroma. Co-localization with interleukin-1 converting enzyme. Am J Pathol 147:251–266
Latz E, Xiao TS, Stutz A (2013) Activation and regulation of the inflammasomes. Nat Rev Immunol 13:397–411
Prochnicki T, Mangan MS, Latz E (2016) Recent insights into the molecular mechanisms of the NLRP3 inflammasome activation. F1000Res 5:1469
Grebe A, Hoss F, Latz E (2018) NLRP3 inflammasome and the IL-1 pathway in atherosclerosis. Circ Res 122:1722–1740
Zimmer S, Grebe A, Latz E (2015) Danger signaling in atherosclerosis. Circ Res 116:323–340
Duewell P, Kono H, Rayner KJ et al (2010) NLRP3 inflammasomes are required for atherogenesis and activated by cholesterol crystals. Nature 464:1357–1361
Tschopp J, Schroder K (2010) NLRP3 inflammasome activation: the convergence of multiple signalling pathways on ROS production? Nat Rev Immunol 10(3):210–215
Biasucci LM, Liuzzo G, Fantuzzi G et al (1999) Increasing levels of interleukin(1L)-1Ra and IL-6 during the first 2 days of hospitalization in unstable angina patients are associated with increased risk of in-hospital coronary events. Circulation 99:2079–2084
Haslinger-Löffler B (2008) Multiple effects of HMG-CoA reductase inhibitors (statins) besides their lipid-lowering function. Kidney Int 74(5):553–555. https://doi.org/10.1038/ki.2008.323
Bergheanu SC, Bodde MC, Jukema JW (2017) Pathophysiology and treatment of atherosclerosis: current view and future perspective on lipoprotein modification treatment. Neth Hear J 25(4):231–242. https://doi.org/10.1007/s12471-017-0959-2
Antonopoulos A, Margaritis M, Lee R et al (2012) Statins as anti-inflammatory agents in atherogenesis: molecular mechanisms and lessons from the recent clinical trials. Curr Pharm Des 18(11):1519–1530
Calderon RM, Cubeddu LX, Goldberg RB et al (2010) Statins in the treatment of dyslipidemia in the presence of elevated liver aminotransferase levels: a therapeutic dilemma. Mayo Clin Proc 85(4):349–356
Campbell CY, Rivera JJ, Blumenthal RS (2007) Residual risk in statin-treated patients: future therapeutic options. Curr Cardiol Rep 9(6):499–505. https://doi.org/10.1007/BF02938395
Libby P, Ridker PM, Hansson GK (2011) Progress and challenges in translating the biology of atherosclerosis. Nature 473(7347):317–325. https://doi.org/10.1038/nature10146
Sampson UK, Fazio S, Linton MF (2012) Residual cardiovascular risk despite optimal LDL cholesterol reduction with statins: the evidence, etiology, and therapeutic challenges. Curr Atheroscler Rep 14(1):1–10. https://doi.org/10.1007/s11883-011-0219-7
Ray KK, Wright S, Kallend D et al (2020) Two phase 3 trials of inclisiran in patients with elevated LDL cholesterol. N Engl J Med 382(16):1507–1519
Jia L, Betters JL, Yu L (2011) Niemann-pick C1-like 1 (NPC1L1) protein in intestinal and hepatic cholesterol transport. Annu Rev Physiol 73:239–259. https://doi.org/10.1146/annurev-physiol-012110-142233
Cannon CP, Blazing MA, Giugliano RP et al (2015) Ezetimibe added to statin therapy after acute coronary syndromes. N Engl J Med 25:2387–2397
Tsujita K, Sugiyama S, Sumida H et al (2015) Impact of dual lipid-lowering strategy with ezetimibe and atorvastatin on coronary plaque regression in patients with percutaneous coronary intervention. J Am Coll Cardiol 66(5):495–507
Bohula EA, Giugliano RP, Leiter LA et al (2018) Inflammatory and cholesterol risk in the FOURIER trial. Circulation 138(2):131–140
Ballantyne CM, Laufs U, Ray KK et al (2020) Bempedoic acid plus ezetimibe fixed-dose combination in patients with hypercholesterolemia and high CVD risk treated with maximally tolerated statin therapy. Eur J Prev Cardiol 27(6):593–603
Pinkosky SL, Filippov S, Srivastava RA et al (2013) AMP-activated protein kinase and ATP-citrate lyase are two distinct molecular targets for ETC-1002, a novel small molecule regulator of lipid and carbohydrate metabolism. J Lipid Res 54:134–151
Pinkosky SL, Newton RS, Day EA et al (2016) Liver-specific ATP-citrate lyase inhibition by bempedoic acid decreases LDL-C and attenuates atherosclerosis. Nat Commun 7:13457
Ballantyne CM, Banach M, Mancini GBJ et al (2018) Efficacy and safety of bempedoic acid added to ezetimibe in statin-intolerant patients with hypercholesterolemia: a randomized, placebo-controlled study. Atherosclerosis 277:195–203
Laufs U, Banach M, Mancini GBJ et al (2019) Efficacy and safety of bempedoic acid in patients with hypercholesterolemia and statin intolerance. J Am Heart Assoc 8:e011662
Ridker PM, Libby P, MacFayden JG et al (2018) Modulation of the interleukin-6 signaling pathway and incidence rates of atherosclerotic events and all-cause mortality: analyses from the Canakinumab Anti-Inflammatory Thrombosis Outcomes Study (CANTOS). Eur Heart J 39(38):3499–3507
Ridker PM, Cannon CP, Morrow D et al (2005) C-reactive protein levels and outcomes after statin therapy. N Engl J Med 352(1):20–28
Puri R, Nissen SE, Libby P et al (2013) C-reactive protein, but not low-density lipoprotein cholesterol levels, associate with coronary atheroma regression and cardiovascular events after maximally intensive statin therapy. Circulation 128(22):2395–2403
Bevilacqua MP, Pober JS, Majeau GR et al (1984) Interleukin 1 (IL-1) induces biosynthesis and cell surface expression of procoagulant activity in human vascular endothelial cells. J Exp Med 160:618–623
Bevilacqua MP, Pober JS, Wheeler ME et al (1985) Interleukin 1 acts on cultured human vascular endothelium to increase the adhesion of polymorphonuclear leukocytes, monocytes, and related leukocyte cell lines. J Clin Invest 76:2003–2011
Galea J, Armstrong J, Gadsdon P et al (1996) Interleukin-1 beta in coronary arteries of patients with ischemic heart disease. Arterioscler Thromb Vasc Biol 16:1000–1006
Shimokawa H, Ito A, Fukumoto Y et al (1996) Chronic treatment with interleukin-1 beta induces coronary intimal lesions and vasospastic responses in pigs in vivo. J Clin Invest 97:769–776
Kirii H, Niwa T, Yamada Y et al (2003) Lack of interleukin-1β decreases the severity of atherosclerosis in ApoE-deficient mice. Arterioscler Thromb Vasc Biol 23(4):656–660
Morton AC, Arnold ND, Gunn J et al (2005) Interleukin-1 receptor antagonist alters the response to vessel wall injury in a porcine coronary artery model. Cardiovasc Res 68:493–501
Elhage R, Maret A, Pieraggi MT et al (1998) Differential effects of interleukin-1 receptor antagonist and tumor necrosis factor binding protein on fatty-streak formation in apolipoprotein E-deficient mice. Circulation 97:242–244
Devlin CM, Kuriakose G, Hirsch E et al (2002) Genetic alterations of IL-1 receptor antagonist in mice affect plasma cholesterol level and foam cell lesion size. Proc Natl Acad Sci U S A 99:6280–6285
Isoda K, Sawada S, Ishigami N et al (2004) Lack of interleukin-1 receptor antagonist modulates plaque composition in apolipoprotein E-deficient mice. Arterioscler Thromb Vasc Biol 24:1068–1073
Nicklin MJ, Hughes DE, Barton JL et al (2000) Arterial inflammation in mice lacking the interleukin 1 receptor antagonist gene. J Exp Med 191:303–312
Bhaskar V, Yin J, Mirza AM et al (2011) Monoclonal antibodies targeting IL-1 beta reduce biomarkers of atherosclerosis in vitro and inhibit atherosclerotic plaque formation in Apolipoprotein E-deficient mice. Atherosclerosis 216(2):313–320
Alexander MR, Moehle CW, Johnson JL et al (2012) Genetic inactivation of IL-1 signaling enhances atherosclerotic plaque instability and reduces outward vessel remodeling in advanced atherosclerosis in mice. J Clin Invest 122:70–79
Menu P, Pellegrin M, Aubert J-F et al (2011) Atherosclerosis in ApoE-deficient mice progresses independently of the NLRP3 inflammasome. Cell Death Dis 2(3):e137–e145
Shemesh S, Kamari Y, Shaish A et al (2012) Interleukin-1 receptor type-1 in non-hematopoietic cells is the target for the pro-atherogenic effects of interleukin-1 in apoE-deficient mice. Atherosclerosis 222(2):329–336
Kamari Y, Werman-Venkert R, Shaish A et al (2007) Differential role and tissue specificity of interleukin-1alpha gene expression in atherogenesis and lipid metabolism. Atherosclerosis 195:31–38
Kamari Y, Shaish A, Shemesh S et al (2011) Reduced atherosclerosis and inflammatory cytokines in apolipoprotein-E-deficient mice lacking bone marrow-derived interleukin-1α. Biochem Biophys Res Commun 405(2):197–203
Ridker PM, Everett BM, Thuren T et al (2017) Antiinflammatory therapy with canakinumab for atherosclerotic disease. N Engl J Med 377(12):1119–1131
Ridker PM, Everett BM, Pradhan A et al (2018) Low-dose methotrexate for the prevention of atherosclerotic events. N Engl J Med 380(8):752–762
Westlake SL, Colebatch AN, Baird J et al (2010) The effect of methotrexate on cardiovascular disease in patients with rheumatoid arthritis: a systematic literature review. Rheumatology 49(2):295–307
Choi HK, Hernan MA, Seeger JD et al (2002) Methotrexate and mortality in patients with rheumatoid arthritis: a prospective study. Lancet 359(9313):1173–1177
Micha R, Imamura F, Wyler Von Ballmoos M et al (2011) Systematic review and meta-analysis of methotrexate use and risk of cardiovascular disease. Am J Cardiol 108(9):1362–1370
Morton AC, Rothman AM, Greenwood JP et al (2015) The effect of interleukin-1 receptor antagonist therapy on markers of inflammation in non-ST elevation acute coronary syndromes: the MRC-ILA Heart study. Eur Heart J 36(6):377–384
Abbate A, Kontos MC, Abouzaki NA et al (2015) Comparative safety of interleukin-1 blockade with anakinra in patients with ST-segment elevation acute myocardial infarction (from the VCU-ART and VCU-ART2 pilot studies). Am J Cardiol 115(3):288–292
Abbate A, Kontos MC, Grizzard JD et al (2010) Interleukin-1 blockade with anakinra to prevent adverse cardiac remodeling after acute myocardial infarction (Virginia Commonwealth University Anakinra Remodeling Trial [VCU-ART] Pilot study). Am J Cardiol 105(10):1371–1377
Abbate A, Trankle CR, Buckley LF et al (2020) Interleukin-1 blockade inhibits the acute inflammatory response in patients with ST-segment-elevation myocardial infarction. J Am Heart Assoc 9:e014941
Nidorf SM, Eikelboom JW, Budgeon CA et al (2013) Low-dose colchicine for secondary prevention of cardiovascular disease. J Am Coll Cardiol 61(4):404–410
O’Donoghue ML, Braunwald E, White HD et al (2014) Effect of darapladib on major coronary events after an acute coronary syndrome: the SOLID-TIMI 52 randomized clinical trial. JAMA 312(10):1006–1015
O’Donoghue ML, Glaser R, Cavender MA et al (2016) Effect of iosmapimod on cardiovascular outcomes in patients hospitalized with acute myocardial infarction: a randomized clinical trial. JAMA 315(15):1591–1599
Tardif J-C, Kouz S, Waters DD et al (2019) Efficacy and safety of low-dose colchicine after myocardial infarction. N Engl J Med 381(26):2497–2505
Nidorf SM, Fiolet ATL, Mosterd A et al (2020) Colchicine in patients with chronic coronary disease. N Engl J Med 383(19):1838–1847
Nidorf SM, Eikelboom JW, Thompson PL (2014) Targeting cholesterol crystal-induced inflammation for the secondary prevention of cardiovascular disease. J Cardiovasc Pharmacol Therapeut 19(1):45–52
Martinez GJ, Celermajer DS, Patel S (2018) The NLRP3 inflammasome and the emerging role of colchicine to inhibit atherosclerosis-associated inflammation. Atherosclerosis 269:262–271
Huber SA, Sakkinen P, Conze D et al (1999) Interleukin-6 exacerbates early atherosclerosis in mice. Arterioscler Thromb Vasc Biol 19:2364–2367
Schieffer B, Selle T, Hilfiker A et al (2004) Impact of interleukin-6 on plaque development and morphology in experimental atherosclerosis. Circulation 110:3493–3500
Zhang K, Huang XZ, Li XN et al (2012) Interleukin 6 destabilizes atherosclerotic plaques by downregulating prolyl-4-hydroxylase α1 via a mitogen-activated protein kinase and c-Jun pathway. Arch Biochem Biophys 528:127–133
Schuett H, Oestreich R, Waetzig GH et al (2012) Transsignaling of interleukin-6 crucially contributes to atherosclerosis in mice. Arterioscler Thromb Vasc Biol 32:281–290
Madan M, Bishayi B, Hoge M et al (2008) Atheroprotective role of interleukin-6 in diet- and/or pathogen-associated atherosclerosis using an ApoE heterozygote murine model. Atherosclerosis 197:504–514
Whitman SC, Ravisankar P, Daugherty A (2002) Interleukin-18 enhances atherosclerosis in apolipoprotein E(-/-) mice through release of interferon-gamma. Circ Res 90:E34–E38
Bhat OM, Kumar PU, Giridharan NV et al (2015) Interleukin-18-induced atherosclerosis involves CD36 and NF-κB crosstalk in Apo E-/- mice. J Cardiol 66(1):28–35
Pejnovic N, Vratimos A, Lee SH et al (2009) Increased atherosclerotic lesions and Th17 in interleukin-18 deficient apolipoprotein E-knockout mice fed high-fat diet. Mol Immunol 47(1):37–45
Canault M, Peiretti F, Mueller C et al (2004) Exclusive expression of transmembrane TNF-alpha in mice reduces the inflammatory response in early lipid lesions of aortic sinus. Atherosclerosis 172:211–218
Ohta H, Wada H, Niwa T et al (2005) Disruption of tumor necrosis factor-alpha gene diminishes the development of atherosclerosis in apoE-deficient mice. Atherosclerosis 180:11–17
Xiao N, Yin M, Zhang L et al (2009) Tumor necrosis factor-alpha deficiency retards early fatty-streak lesion by influencing the expression of inflammatory factors in apoE-null mice. Mol Genet Metab 96(4):239–244
Xanthoulea S, Thelen M, Pottgens C et al (2011) Absence of p55 TNF receptor reduces atherosclerosis, but has no major effect on angiotensin II induced aneurysms in LDL receptor deficient mice. PLoS 4(7):e6113
Mackesy DZ, Goalstone ML (2014) ERK5: novel mediator of insulin and TNF-stimulated VCAM-1 expression in vascular cells. J Diab 6:595–602
Rajasingh J, Bord E, Luedemann C et al (2006) IL-10-induced TNF-alpha mRNA destabilization is mediated via IL-10 suppression of p38 MAP kinase activation and inhibition of HuR expression. FASEB J 20:2112–2114
Lisinski TJ, Furie MB (2002) Interleukin-10 inhibits proinflammatory activation of endothelium in response to Borrelia burgdorferi or lipopolysaccharide but not interleukin-1 beta or tumor necrosis factor alpha. J Leukoc Biol 72:503–511
Gallagher H, Williams JO, Ferekidis N et al (2019) Dihomo-γ-linolenic acid inhibits several key cellular processes associated with atherosclerosis. Biochem Biophys Acta Mol Basis Dis 1865(9):2538–2550
Takai S, Jin D, Kawashima H et al (2009) Anti-atherosclerotic effects of dihomo-gamma-linolenic acid in ApoE-deficient mice. J Atheroscler Thromb 16(4):480–489
Bhatt DL, Steg PG, Miller M et al (2019) Cardiovascular risk reduction with icosapent ethyl for hypertriglyceridemia. N Engl J Med 380(1):11–22
Budoff MJ, Bhatt DL, Kinninger A et al (2020) Effect of icosapent ethyl on progression of coronary atherosclerosis in patients with elevated triglycerides on statin therapy: final results of the EVAPORATE trial. Eur Heart J 41:3925–3932
Acknowledgments
We thank the British Heart Foundation for financial support (grants PG/16/25/32097 and FS/17/75/33257).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Science+Business Media, LLC, part of Springer Nature
About this protocol
Cite this protocol
Chan, YH., Ramji, D.P. (2022). Key Roles of Inflammation in Atherosclerosis: Mediators Involved in Orchestrating the Inflammatory Response and Its Resolution in the Disease Along with Therapeutic Avenues Targeting Inflammation. In: Ramji, D. (eds) Atherosclerosis. Methods in Molecular Biology, vol 2419. Humana, New York, NY. https://doi.org/10.1007/978-1-0716-1924-7_2
Download citation
DOI: https://doi.org/10.1007/978-1-0716-1924-7_2
Published:
Publisher Name: Humana, New York, NY
Print ISBN: 978-1-0716-1923-0
Online ISBN: 978-1-0716-1924-7
eBook Packages: Springer Protocols