Abstract
Background
Biliary adenofibroma is an exceptionally rare benign liver tumor with the potential for malignant transformation. In literature, only 21 cases have been described.
Clinical presentation
In a healthy 63-year-old woman, a partly solid, partly cystic mass in the left lobe of the liver during a routine ultrasound examination was found. The computed tomography (CT) scan of the abdomen showed a 6.3 × 5.0-cm multilobulated cystic, partly hypervascularized mass in the liver segment IVa, with extension into segments II and IVb. There was no evidence of lymph node or distant metastases. Extirpation of the tumor was indicated by the multidisciplinary tumorboard. Microscopic examination showed a biphasic composed tumor with tubules embedded in fibrous stroma. In addition, there were also areas with pseudopapillary projections, as well as parts with focal cribriform-like growth pattern, which have been indicated as a possible sign of malignant transformation. Additionally, we found two different polymorphisms in the encoded TP53 und KIT in both distinct morphology tumor areas by molecular analysis, which ensured a tumor in malignant transformation. The patient has been alive for 24 months after R0 resection without tumor recurrence. Further investigation of more cases of this rare entity is necessary to proof molecular genesis.
Conclusions
We report a rare case of a biliary adenofibroma with transition to an intrahepatic cholangiocellular carcinoma and present a brief literature review.
Similar content being viewed by others
Background
Biliary adenofibroma is a very rare liver tumor. According to the WHO 2010, biliary adenofibroma is classified as a benign tumor. On the other hand, several authors attributing malignant potential to this entity. Depending on tumor diameter, proliferation activity, and p53 accumulation, the lesions are considered to be premalignant neoplasias [1]. Histogenesis and biological behavior are still poorly understood. Herein, we report a morphomolecular case of a biliary adenofibroma with transition to an intrahepatic cholangiocellular carcinoma and present a brief literature review.
Clinical presentation
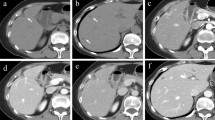
In a 63-year-old female patient, an ultrasound examination due to unspecific abdominal complaints showed a partly solid, partly cystic mass in the left lobe of the liver. The consecutive CT scan showed a 6.3 × 5-cm multilobulated, cystic, partly hypervascularized tumor in liver segment IVa, with extension into segments II and IVb (Fig. 1). The lesion displaced the left and middle hepatic veins and extended cranially just below the liver capsule. It has a malignant appearance with arterial and portal venous phase venous enhancement, but not typically for one of the common liver tumors like CCC, HCC, or metastasis. There was no evidence for the presence of hepatic metastasis or a primary tumor located elsewhere in diagnostic imaging. MRI which would be the gold standard was not performed.
The patient had no other concomitant disease. Notably, inquiring family history, the grandmother and father had died of “liver cancer”. Alcohol and nicotine consumption was denied. Exposure to liver-toxic substances could not be determined. The physical examination and the laboratory revealed no pathological findings. The tumor markers including AFP, CEA, and CA 19-9 were not elevated.
In sonographically guided transcutaneous biopsy of the liver, the lesion was histomorphologically rich in connective tissue with irregularly shaped and in part significantly dilated glandular structures with mild atypia and increased hyperchromasia of the cells. Immunohistochemistry showed expression of CK7 in the absence of immune reaction with antibodies to cadherin 17, TTF-1, and S100P. The finding was considered consistent with a primary adenocarcinoma of the bile duct in accordance with the radiological imaging. Based on these findings, in our interdisciplinary tumor board, decision was made for surgical resection. A left hemihepatectomy was performed and the postoperative course was uneventful. Postoperative follow-up and computed tomography 24 months postoperatively showed no evidence of recurrence or metastasis.
Pathological findings
The left hemihepatectomy specimen (14.5 × 14.5 × 5.9 cm) showed macroscopically a well-defined, micro- to small-cystic lesion with focal solid areas, a maximum of 65 mm in diameter, and a gray cut surface (Fig. 2). The cysts discharged a clear, non-mucinous fluid. The remaining liver parenchyma was homogeneously grayish brown on the cut surface.
Histologically, the tumor was composed of two distinct areas. The majority of the lesion showed multiple ducts variable in size, irregular in shape, and angulated with dilation to cysts, lined by a cuboidal single layer to columnar epithelium of the biliary phenotype. Mucin or bile production was not apparent. The tumor was in parts sharply demarcated with a pseudocapsular fibrosis facing the adjacent liver parenchyma (Fig. 3a). The tumor cells showed relatively monomorphic round to oval nuclei with a predominantly fine chromatin and in part with small, inconspicuous nucleoli and an eosinophilic cytoplasm (Fig. 3b). Mitoses were rarely found here (< 1 per 10 high-power fields (HPF)). The cell borders were well defined. In the lumen of tubulocystic proliferations were varying degrees of erythrocytes most likely due to secondary bleeding. The multicystic lesion was embedded in a dense and partially hyalinized, variable broad fibrous spindled stroma. The stroma showed no ovarian-like stromal changes. In the stroma, there was a variably densely mixed inflammatory infiltrate. The other part of the tumor showed crowded, back-to-back, anastomosing tubules with closely packed nuclei. In these areas, a more columnar type arrangement with predominantly basal oriented and partly pseudostratified nuclei was seen. The nuclei were characterized by low to moderate atypia. The nuclear membrane showed distinct contour and predominantly prominent nucleoli. The mitotic rate was here very rare (< 1 per 10 HPF). Atypical mitotic figures could not be detected. In this part, the tumor was accompanied by a tender, sometimes hardly distinguishable stroma (Fig. 3c). In addition, there were also areas with pseudopapillary projections, as well as parts with a focal cribriform-like growth pattern (Fig. 3d). In these areas, invasive growth in the adjacent liver parenchyma could be detected (Fig. 3e). There was no lymphangiosis or hemangiosis carcinomatosa.
a Microscopic findings of the tumor. Low magnification shows crowded, back-to-back tubulare structures (left side; adenocarcinoma) and parts of tubulocystic formations embedded in dense fibrous stroma (center; biliary adenofibroma) with adjacent normal liver parenchym (right side) (H&E × 20). The black circle indicates the bengin part of tumor (bililary adenofibroma) and the blue circle the malignant part of tumor (adenocarcinoma). These two different parts of tumor were marked on the histological slide for subsequent dissection. b At higher magnification, the cysts lined by a bland cuboidal single layer to columnar epithelium of the biliary phenotype with uniform nuclei without feature of malignancy; biliary adenofibroma (H&E × 400). c The areas of macroscopically solid appearance shows irregular pattern with crowded, anastomosing tubules. The nuclei closely packed, pseudostratified with heterogeneously distributed chromatin and prominent nucleoli; adenocarcinoma (H&E × 400). d Focal, the neoplasm shows a complex architecture, composed of pseudopapillary and cribriform-like tubules in a dense stroma; adenocarcinoma (H&E × 100). e In the peripheral area reveals irregularly glandular structures infiltrate the adjacent liver parenchyma; adenocarcinoma (H&E × 200). f Ki67 proliferation index in benign part of the tumor (biliary adenofibroma) less than 10 % (Ki67 staining × 200). g Ki67 proliferation index in the malignant part of the tumor (adenocarcinoma) significantly increased to 20–30 % (Ki67 staining × 200)
Immunohistochemically, the epithelial cells stained diffusely positive for cytokeratin 7 and focally positive in single cells/cell groups for Cadherin 17 and CD56. Individual cell nuclei showed weak nuclear staining for p53. Muc1 was expressed on the apical surfaces of most epithelial cells. The stroma cells were diffusely smooth muscle-actin positive. The markers inhibin, calretinin, S100P, ERG, Muc2, Muc4, Muc5, and Muc6 were completely negative. Immunohistochemistry of the mismatch repair proteins revealed nuclear expression obtained from the markers MLH1, MSH2, MSH6, and PMS2. The Ki67 labeling index differs in the benign and malignant tumor components, from 5–10 % in biliary adenofibroma to 20–30% in the adenocarcinoma (Fig. 3f, g).
In addition, parts of the biliary adenofibroma as well as the cholangiocellular carcinoma component were examined for mutational status. The material was macrodissected and purified DNA was sequenced with Next-Generation Sequencing on the MiSeq platform (Illumina). The following genes were examined by the target enrichment using the TruSight Tumor Panel 15: AKT 1, BRAF, EGFR, ERBB2, FOXL2, GNA11, GNAQ, KIT, KRAS, MET, NRAS, PDGFRA, PIK3CA, RET, and TP53. No pathogenic variants could be found in the mentioned gene sections. Only two different polymorphisms (NM_000546.5: c.215C> G, TP53; NM_000222.2: c.1621A> C, KIT) were found in the biliary adenofibroma well as in the cholangiocellular carcinoma.
Discussion
This case report describes one of the very rare cases of a biliary adenofibroma of the liver with proven transition to a well-differentiated adenocarcinoma of the biliary type.
Tsui et al. [2] were the first to describe this cystic liver lesion as a benign, complex, tubulocystic tumor with a bland spindle-cell stromal component. To date, there are only 21 case reports in the literature, 7 of which showed malignant transformation in a pre-existing biliary adenofibroma (Table 1). In majority, the reported biliary adenofibromas showed transition into papillary or tubulopapillary growth patterns. This histomorphological picture suggests a neoplastic progression of the tumor. Kaminsky et al. also described a microcystic growth pattern, as well as a neuroendocrine differentiation [3]. Another case showed pulmonary metastases after 3 years [4].
Currently, the WHO (2010) lists two cystic intrahepatic lesions: non-invasive mucinous cystic neoplasia with mild to severe dysplasia and mucinous cystic neoplasia with associated invasive carcinoma [1]. Mucinous cystic neoplasms in older nomenclatures were referred to as cystadenoma or cystadenocarcinoma. By definition, the tumors show a mucinous epithelium with papillary projections and an ovarian-like spindle cell stroma. The tumor presented here did not show any characteristic features of a mucinous cystic neoplasia, in particular, immunohistology was negative with antibodies to inhibin in the stroma, which is usually positive in mucinous neoplasias.
In differential diagnosis, a rarely reported primary hepatic cystic mesothelioma was excluded by the lack of immune response to calretinin antibody [18, 19].
In addition, a biliary adenofibroma is morphologically reminiscent of a von Meyenburg complex. These benign hepatic lesions are typically less than 0.5 cm in size and are assigned to the shape of the ductal plate malformation. Isolated cases with a transition to dysplasia or associated carcinoma have also been observed in these small subcapsular tubulocystic lesions [20].
Similar to the cases described in the literature (Table 1), the presented neoplasia morphologically showed a characteristic structure of a biliary adenofibroma with tubulocystic biliary epithelium and a broad fibrous, non-ovarian-like stroma. In addition, a partly abrupt, partly gradual transformation into more cell-dense tumor areas could be seen, which histologically showed characteristics of an invasive carcinoma in the form of microcystic, fine-papillary and partly cribriform epithelial formations with distinct nuclear atypia and an increased mitotic rate, comparable to the two cases described by Thompson et al. with a very similar architecture [15].
Moreover, the biliary adenofibroma and the cholangiocellular carcinoma were examined with molecular pathology analysis. The two polymorphisms found in the encoded TP53 and KIT (NM_000546.5: c.215C> G, TP53; NM_000222.2: c.1621A> C, KIT) imply that the carcinoma developed from the biliary adenofibroma since it is not a “true” mutation in the sequence-specific DNA-binding domain of the TP53 tumor suppressor gene between amino acids 102–292 [21]. Within this sequence, the most common mutations that would result in a missense or nonsense mutation are located.
Arnason et al. reported six cases with biliary adenofibroma without histological features in transition into a malignant tumor. Three tumors of them tested by array comparative genomic hybridization showed chromosomal copy number alterations, including one with amplification of CCND1 and ERBB2 [16]. These amplifications, which alter cell cycle progression, are observed frequently in a variety of tumors and may contribute to tumorigenesis.
Some authors have investigated p53 immunohistochemistry staining to predict biological behavior. However, in immohistochemistry, the p53 positivity varies widely in the literature between only single positive cell nuclei up to 50% of the total tumor [14]. Molecular pathology studies of the biliary adenofibroma have not been extensively described. Only Thompson et al. found a nonsense mutation in the tumor suppressor protein p16 INK4a, which encodes the cyclin-dependent kinase inhibitor (CDKN2A) in the gene [15].
Conclusions
We present the rare case of a biliary adenofibroma showing transition into a well-differentiated intrahepatic cholangiocarcinoma. The malignancy was subsequently proven on the basis of histomorphological criteria, like an invasive growth in the adjacent liver parenchyma, crowed growth with depletion of the stoma, prominent nucleoli, nucleus-plasma ratio, and desmoplastic stroma reaction. This tumor entity is poorly understood. More cases are required for the accurate characterization of this rare entity and its premalignant properties.
Availability of data and materials
None.
Abbreviations
- AFP:
-
Alpha-fetoprotein
- Ca 19-9:
-
Carbohydrate-Antigen 19-9
- CEA:
-
Carcinoembryonic antigen
- CT:
-
Computed tomography
- DNA:
-
Deoxyribonucleic acid
- HPF:
-
High-power field
- MLH1:
-
MutL homolog
- MRI:
-
Magnetic resonance imaging
- MSH2:
-
MutS protein homolog 2
- MSH6:
-
MutS protein homolog 6
- Muc1:
-
Mucin 1
- Muc2:
-
Mucin 2
- Muc4:
-
Mucin 4
- Muc6:
-
Mucin 6
- PMS2:
-
PMS1 Homolog 2-Mismatch Repair System Component
- S100P:
-
S100 calcium-binding protein P
- WHO:
-
World Health Organization
References
Bosman FT, Carneiro F, Hruban RH, Theise ND, eds. WHO Classification of Tumors of the Digestive System. Lyon: International Agency for Research on Cancer; 2010.
Tsui WM, Loo KT, Chow LT, Tse CC. Biliary adenofibroma. A heretofore unrecognized benign biliary tumor of the liver. Am J Surg Pathol. 1993;2:186–92.
Kaminsky P, Preiss J, Sasatomi E, Gerber DA. Biliary adenofibroma: a rare hepatic lesion with malignant features. Hepatology. 2017;65:380–3.
Akin O, Coskun M. Biliary adenofibroma with malignant transformation and pulmonary metastases: CT findings. Am J Roentgenol. 2002;179:280–1.
Parada LA, Bardi G, Hallén M, Hägerstrand I, Tranberg KG, Mitelman F, Johansson B. Monosomy 22 in a case of biliary adenofibroma. Cancer Genet Cytogenet. 1997;93:183–4.
Garduno-Lopez AL, Mondragon-Sanchez R, Bernal-Maldonado R, Hinojosa-Becerril CA, Meneses-Garcíab A. A case of biliary adenofibroma of the liver causing elevated serum CcvA 19-9 levels. Revista de Oncologia. 2002;4:271–3.
Varnholt H, Vauthey JN, Cin PD, et al. Biliary adenofibroma: a rare neoplasm of bile duct origin with an indolent behavior. Am J Surg Pathol. 2003;27:693–8.
Gurrera A, Alaggio R, Leone G, Aprile G, Magro G. Biliary Adenofibroma of the liver: report of a case and review of the literature. Patholog Res Int. 2010;2010:504584.
Kai K, Yakabe T, Kohya N, et al. A case of unclassified multicystic biliary tumor with biliary adenofibroma features. Pathol Int. 2012;62:506–10.
Nguyen NT, Harring TR, Holley L, Goss JA, O'Mahony CA. Biliary adenofibroma with carcinoma in situ: a rare case report. Case Rep Hepatol. 2012;2012:793963.
Nakanuma Y, Tsutsui A, Ren XS, Harada K, Sato Y, Sasaki M. What are the precursor and early lesions of peripheral intrahepatic cholangiocarcinoma? Int J Hepatol. 2014;2014:805973.
Jacobs MA, Lanciault C, Weinstein S. Incidental biliary adenofibroma with dysplastic features. BJR Case Rep. 2015;1:20150100.
Thai E, Dalla Valle R, Evaristi F, Silini EM. A case of biliary adenofibroma with malignant transformation. Pathol Res Pract. 2016;212:468–70.
Godambe A, Brunt EM, Fulling KH, Reza Kermanshahi T. Biliary adenofibroma with invasive carcinoma: case report and review of the literature. Case Rep Pathol. 2016;2016:8068513.
Thompson SM, Zendejas-Mummert B, Hartgers ML, et al. Malignant transformation of biliary adenofibroma: a rare biliary cystic tumor. J Gastrointest Oncol. 2016;7:E107–12.
Arnason T, Borger DR, Corless C, et al. Biliary adenofibroma of liver: morphology, tumor genetics, and outcomes in 6 cases. Am J Surg Pathol. 2017;41:499–505.
Esteban M, Amin J, Hertl M, Jakate S, Singh A. Double trouble: a rare case of concurrent biliary adenofibroma and hepatobiliary mucinous cystic neoplasm. ACG Case Rep J. 2018;5:e72.
Perysinakis I, Nixon AM, Spyridakis I, Kakiopoulos G, Zorzos C, Margaris I. Primary intrahepatic malignant epithelioid mesothelioma. Int J Surg Case Rep. 2014;5:1098–101.
Flemming P, Becker T, Klempnauer J, Högemann D, Kreft A, Kreipe HH. Benign cystic mesothelioma of the liver. Am J Surg Pathol. 2002;26:1523–7.
Jain D, Sarode VR, Abdul-Karim FW, Homer R, Robert ME. Evidence for the neoplastic transformation of Von-Meyenburg complexes. Am J Surg Pathol. 2000;24:1131–9.
Pavletich NP, Chambers KA, Pabo CO. The DNA-binding domain of p53 contains the four conserved regions and the major mutation hot spots. Genes Dev. 1993;7:2556–64.
Acknowledgments
The authors thank Robert Grützmann for the critical reading of the manuscript.
Funding
We have no source of funding for this article.
Author information
Authors and Affiliations
Contributions
AS diagnosed the pathological findings and wrote the manuscript. TW performed the resection and the perioperative management of the patient. DA performed the molecular analysis. CM described the radiological findings and provided the radiological imaging. GB participated in revising the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Informed consent was obtained from the patient for this publication.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Sturm, AK., Welsch, T., Meissner, C. et al. A case of biliary adenofibroma of the liver with malignant transformation: a morphomolecular case report and review of the literature. surg case rep 5, 104 (2019). https://doi.org/10.1186/s40792-019-0661-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s40792-019-0661-2