Abstract
Background
Intracellular Ca2+ overload induced by extracellular Ca2+ entry has previously been confirmed to be an important mechanism for the cardiotoxicity as well as the acute heart dysfunction induced by jellyfish venom, while the underlying mechanism remains to be elucidated.
Methods
Under extracellular Ca2+-free or Ca2+-containing conditions, the Ca2+ fluorescence in isolated adult mouse cardiomyocytes pre-incubated with tentacle extract (TE) from the jellyfish Cyanea capillata and β blockers was scanned by laser scanning confocal microscope. Then, the cyclic adenosine monophosphate (cAMP) concentration and protein kinase A (PKA) activity in primary neonatal rat ventricular cardiomyocytes were determined by ELISA assay. Furthermore, the effect of propranolol against the cardiotoxicity of TE was evaluated in Langendorff-perfused rat hearts and intact rats.
Results
The increase of intracellular Ca2+ fluorescence signal by TE was significantly attenuated and delayed when the extracellular Ca2+ was removed. The β adrenergic blockers, including propranolol, atenolol and esmolol, partially inhibited the increase of intracellular Ca2+ in the presence of 1.8 mM extracellular Ca2+ and completely abolished the Ca2+ increase under an extracellular Ca2+-free condition. Both cAMP concentration and PKA activity were stimulated by TE, and were inhibited by the β adrenergic blockers. Cardiomyocyte toxicity of TE was antagonized by β adrenergic blockers and the PKA inhibitor H89. Finally, the acute heart dysfuction by TE was antagonized by propranolol in Langendorff-perfused rat hearts and intact rats.
Conclusions
Our findings indicate that β adrenergic receptor/cAMP/PKA signaling contributes to the intracellular Ca2+ overload through intracellular Ca2+ release by TE from the jellyfish C. capillata.
Similar content being viewed by others
Background
Jellyfish is one of the main groups in the marine biological species and ecosystem diversity. In recent years, the jellyfish explosion is no longer an unfamiliar topic, but became another marine ecological disaster after the red tides. Jellyfish outbreaks cause harm to fishery resources and marine ecosystem [1, 2], and negatively affect human beings who live near coast. What’s more, jellyfish sting is the most common injury by marine organisms, with an estimated 150 million envenomation patients annually [3], and the victims may suffer from a severe pain, itch, swelling, inflammation, dyspnea, arrhythmias, cardiac failure, pulmonary edema or even death [4,5,6].
Jellyfish envenomation has been attributed to the release of toxins from nematocysts in tentacles, and the injuries provoked by jellyfish are characterized by cytotoxicity [7,8,9,10], cardiotoxicity [11, 12], neurotoxicity [13], myotoxicity [14] and other toxicities. However, the most potent pharmacological effect exhibited by jellyfish venoms is on the cardiovascular system, and an acute heart failure caused by the cardiotoxicity of jellyfish venom is the major cause of fatal jellyfish envenomation [15]. Attempts to purify toxins from jellyfish venoms have been largely unsuccessful, and only approximately several hemolytic proteins have been purified and just a few of them have been characterized [16,17,18,19,20]. There was little information about the cardiotoxic component of jellyfish venoms, due to its extreme instability and the difficulties of toxin purification. Some studies have been carried out about jellyfish cardiovascular toxicity, describing the chemical and biological properties of the toxic components and their intervention by several different reagents, and the results have exhibited that a sudden influx of Ca2+ into heart muscle cells is an important reason for cardiovascular collapse [21, 22].
We have previously confirmed that extracellular Ca2+ entry plays a pivotal role in acute heart failure by tentacle extract (TE) from the jellyfish Cyanea capillata. Inhibition of extracellular Ca2+ influx is a promising antagonistic alternative for heart injuries by jellyfish venom [23]. In this study, we are aiming to update the current information on the mechanism of cardiotoxicity of TE from the jellyfish C. capillata. Our study revealed that β adrenergic receptor (βAR)/ cyclic adenosine monophosphate (cAMP)/ protein kinase A (PKA) signaling contributes to the intracellular Ca2+ release by TE from the jellyfish C. capillata. β blockades appear to exert anti-adrenergic effects against the cardiotoxicity of TE from the respects of fluorescent Ca2+ scanning, cardiomyocyte toxicity, isolated Langendorff-perfused rat hearts and intact rats.
Methods
Preparation of TE from the jellyfish C. capillata
Specimens of C. capillata were collected in June 2015 in the Sanmen Bay, East China Sea, and identified by Professor Huixin Hong from the Fisheries College of Jimei University (Xiamen, China). The removed tentacles were preserved in plastic bags on dryice and immediately shipped to Shanghai, where the samples were frozen at −70 °C untill use. The TE was prepared following the method as described in previous reports [24]. Briefly, frozen tentacles were thawed at 4 °C and immersed in seawater (prepared in the laboratory by solving 28 g of NaCl, 5 g of MgCl2·6H2O, 0.8 g of KCl and 1.033 g of CaCl2 in 1, 000 ml water) at a mass/volume ratio of 1:1 to allow autolysis of the tissues for 4 days. The mixture was stirred for 30 min twice daily. The autolyzed mixture was filtered by a 100 mesh cell strainer thrice and the filtrate was centrifuged at 10,000×g for 15 min thrice. The resultant supernatant was the TE. All the procedures were performed at 4 °C or in an ice bath. TE was centrifuged at 10,000×g for 15 min to remove the sediments, followed by dialysis against phosphate buffer saline (PBS) (0.01 mol/L, pH 7.4) for 8 h before use. Protein concentration was determined using the method of Bradford [25], with fetal bovine serum albumin as a standard.
Adult mouse cardiomyocyte isolation
Single cardiomyocytes were obtained from adult male Kunming mice (22–25 g) using an enzymatic dissociation technique [26]. The hearts were excised from heparinized and deeply anaesthetized mice, cannulated and mounted on a Langendorff apparatus. After a digest perfusion for 8–10 min with perfusion buffer (mM: 10 HEPES, 0.6 Na2HPO4, 113 NaCl, 4.7 KCl, 12 NaHCO3, 0.6 KH2PO4, 1.2 MgSO4∙7H2O, 10 KHCO3, 30 Taurine, 10 2,3-Butanedine monoxime, 5.5 Glucose, pH 7.46) containing 773 U/ml collagenase type II (Worthington, USA), the ventricular tissue was cut into small pieces and gently stirred in stopping buffer containing perfusion buffer, 10% fetal bovine serum and 12.5 μM CaCl2 for 10–15 min, then transfered the upper cell suspension to a 25 ml beaker. After reintroduction the Ca2+ to a final concentration of 1 mM, the collected cells were kept at room temperature until experimental use.
Measurement of intracellular Ca2+ by laser scanning confocal microscope (LSCM)
The intracellular Ca2+ imaging in cardiomyocyte was performed using an Olympus FV1000 confocal microscope (Olympus, Japan). The adult mouse cardiomyocytes were loaded with Fluo-4 AM (25 μM, Invitrogen) for 20 min to indicate the intracellular Ca2+. Under extracellular Ca2+-free or Ca2+-containing conditions, the cardiomyocytes after TE treatment (60 μg/ml) were ratiometrically scanned with an excitation wavelength at 488 nm and emission wavelength longer than 505 nm for 10 min with a 10-s interval. To confirm the participation of β adrenergic signaling in TE-induced intracellular Ca2+ overload, the cardiomyocytes were pre-incubated for 5 min with three different types of β blockers propranolol, atenolol and esmolol, and the PKA inhibitor H89, respectively.
Primary neonatal rat cardiomyocyte incubation
Primary neonatal rat ventricular cardiomyocytes (NRVMs) were isolated from 1 to 2-day-old Sprague–Dawley (SD) rats by type II collagenase digestion. Briefly, the ventricles were excised, cut into small pieces, and incubated for 20 min thrice in D-Hanks’ balanced salt solution (g/L: 8 NaCl, 0.4 KCl, 1 Glucose, 0.06 KH2PO4, 0.0475 Na2HPO4) containing 0.125% collagenase type II. The detached cells were collected and gradient centrifuged for 26 min at 2800×g with a separation medium 60% percoll (at the bottom) and 40% percoll (at the top) in D-Hanks’ balanced salt solution. Then the cell suspension was collected and filled with the Dulbecco’s modified Eagle’s medium (DMEM) to centrifuge at 1500×g for 10 min. The isolated cardiomyocytes were plated at a density of 5 × 105 cells/ml in DMEM supplemented with 20% fetal bovine serum in the presence of 0.1 mM 5-bromo-2-deoxyuridine (BrdU). Cell cultures were maintained for 48 h at 37 °C with 5% CO2 prior to being used in the experiments.
cAMP assay
The intracellular cAMP concentration was determined by an ELISA kit (Ray Biotech, Inc., USA) in different treatments. The NRVMs were planted in a 24-well plate with the cell density 5 × 105 cells/ml. After the intervention of β adrenergic receptor blockers (propranolol, atenolol and esmolol, respectively) for 5 min, the TE (60 μg/ml) was added and the myocardial cells were incubated for 45 min. After treatment, the cells were washed gently with ice-cold PBS, and lysed with RIPA buffer (Beyotime, China). The supernatant was obtained by a centrifugation of 10,000×g for 10 min at 4 °C. The concentration of cAMP was determined according to the manual of cAMP ELISA kit. Values for the changes of cAMP concentration were calculated as A/A0, where A was the cAMP concentration of intervention group and A0 was that of control group without any treatment.
Determination of PKA activity
Primary neonatal rat cardiomyocytes were planted in 24-well plates at a density of 5 × 105 cells/well, the cell lysate was obtained as described above. After the β blocker treatment for 5 min at 37 °C in a humidified incubator in HEPES containing TE (60 μg/ml), the PKA activity of cardiomyocytes was measured using an ELISA kit (Enzo Life Sciences International, Inc., USA).
Cardiomyocyte toxicity of TE and its intervention
NRVMs were treated with TE from the jellyfish C. capillata for 24 h at the dose of 60 μg/ml. Cardiomyocyte toxicity of TE was evaluated with the Cell Counting Kit-8 (CCK-8, Tokyo, Japan). Three β blockers, including propranolol, atenolol and esmolol, and PKA inhibitor H89 were pre-administrated 30 min before the TE administration. After each treatment, 10 μl of CCK-8 solution was added and the cells were continuously incubated at 37 °C for 2 h. The absorbance of each well was measured with a spectrophotometric microplate reader at 450 nm by the following equation: viability% = [(AS-AB)/(AC-AB)] × 100%, where AS is the absorbance of the samples, AC is the absorbance of the PBS, and AB is the absorbance of the background.
Isolated Langendorff-perfused rat hearts
Male SD rats (280–320 g) were anaesthetized with a mixture of urethane (1.2 g/kg i.p.) and heparin (400 IU/kg i.p.). The heart was rapidly excised and placed into an ice-cold Krebs solution. Then the heart was mounted onto a Langendorff apparatus and retrogradely perfused using a peristaltic pump (MPA-2000, Alcott Biotech, Shanghai, China) with warm Krebs solution (37 °C, pH 7.40). The Krebs solution, equilibrated with a mixture of 95% O2 and 5% CO2, was adjusted to keep a constant flow rate of 12–16 ml/min, thus maintaining an initial perfusion pressure of 60–80 mmHg. A fluid-filled balloon was introduced into the left ventricle through a polyethylene cannula. The initial balloon volume was set to generate the Lvedp of 2–8 mmHg. After a 20-min stabilization period, the isolated perfused heart was pre-treated with 1 μmol/L propranolol followed by the TE administered in bolus (180 μg). Heart indexes, including heart rate (HR), left ventricular developed pressure (LVDP), left ventricular end-diastolic pressure (LVEDP) and maximal ascending and descending derivative of left ventricle (± dP/dtmax), were recorded/calculated by the MPA-2000 bio-signal analysis system.
In vivo preparation
Effects of the venom and propranolol on blood pressure and heart rate were evaluated in male SD rats (220–250 g, provided by the Laboratory Animal Center of the Second Military Medical University, Shanghai) anaesthetized with urethane (1.2 g/kg i.p.). Heparinized polyethylene catheters were implanted into the left femoral artery and external jugular vein for mean arterial pressure (MAP) recording and venom injection, respectively. During all experiments, animals breathed spontaneously. 0.75 mg/kg propranolol was pre-administrated, followed by 0.5 mg/kg TE through the external jugular vein in intact rats. The mean blood pressure (BP) was recorded through a blood pressure transducer (Alcott Biotech, Shanghai, China) and signals were processed using the MPA-2000.
Statistics
All the quantitative data were expressed as mean ± SD. The graphs were built using GraphPad Prism 5 for each experiment. Analysis of variance (ANOVA) was used to analyze the effects of TE administration and the invention either by β blockers or H89. A statistical significance was indicated by P < 0.05.
Results
Intracellular Ca2+-overload induced by TE
We have previously displayed that extracellular Ca2+ entry plays a pivotal role in acute heart failure by TE from jellyfish C. capillata. In this study, fluorescent Ca2+ indicator Fluo-4 AM and frame scanning of confocal microscopy were used to firstly record the intracellular Ca2+ concentration affected by TE in adult mouse cardiomyocytes. Congruously, the signal of Ca2+ fluorescence started to rise at less than 1 min, and got to the maximum with a very bright vision at around 5 min after 60 μg/ml TE administration. The F/F0 got to and stayed at an approximate maximum value of 12 until cell death that normally occurred 15 min later. To exclude the influence of extracellular Ca2+ entry through either Ca2+ pore or Na+-Ca2+ exchanger, we repeated the experiments in a bath solution without Ca2+. Intracellular Ca2+ still increased after 60 μg/ml TE administration, just in a much slower and weaker manner. The time-to-maximum was at about 10 min after TE administration, with a peak F/F0 value very close to that induced by TE under 1.8 mM extracellular Ca2+ condition. In addition, the cardiomyocytes under Ca2+ free condition went to die at least 30 min later, or even without morphological changes and cell death (Fig. 1). These results showed the importance of extracellular Ca2+ entry in the process of intracellular Ca2+ overload induced by TE, on the other hand, the phenomenon of TE-induced intracellular Ca2+ release under Ca2+ free condition drew our attention.
Effect of tentacle extract (TE) from jellyfish Cyanea capillata on intracellular Ca2+ concentration in adult mouse cardiomyocytes. Intracellular Ca2+ concentration was recorded using the Ca2+ indicator Fluo-4 AM and frame scanning mode by laser scanning confocal microscope. a. The representative fluorescent Ca2+ scanning images of cardiomyocytes affected by 60 μg/ml TE within 10 min under 1.8 mM Ca2+ extracellular solution and Ca2+-free condition. b. The traces of F/F0 values after TE administration under 1.8 mM extracellular Ca2+ or Ca2+ free condition. Data are shown by mean ± SD (n = 6)
TE-induced intracellular Ca2+-overload hindered by β-blockade
During the process of cardiac excitation-contraction (E-C) coupling, sympathetic excitation through β adrenergic signaling stimulates both Ca2+ release of cardiac ryanodine receptors (RyR2s) and Ca2+ uptake through sarcoplasmic reticulum Ca2+ pump, therefore enhancing both contraction and relaxation with fear, stress, exercise or excitation. Here β blockers, including propranolol, atenolol and esmolol, were used to check if TE has a pseudo adrenergic effect that stimulates the intracellular Ca2+ release in isolated adult mouse cardiomyocytes. Under the 1.8 mM extracellular Ca2+ condition, all the β blockers showed a partial inhibitory effect on TE-induced intracellular Ca2+ overload. In the β blocker groups, the elevation of intracellular Ca2+ was much slower with an obviously delayed time-to-peak value, and the maximal F/F0 of fluorescent Ca2+ signals was around 5, much smaller than that of the control. To our great surprise, all the three blockers almost abolished the elevation of intracellular Ca2+: we did not see any increase of intracellular Ca2+ within 10 min after TE administration (Fig. 2). Therefore, the results that β-blockade hindered the elevation of intracellular Ca2+ caused by TE indicated that β adrenergic singling might mediate the TE-induced intracellular Ca2+ release, contributing to the acute heart injuries after jellyfish envenomation.
Effect of β blockers on TE-induced Ca2+ increase in isolated adult mouse cardiomyocytes. β-blockers propranolol, atenolol and esmolol were preincubated for 5 min with the cardiomyocytes followed by 60 μg/ml TE administration with or without 1.8 mM extracellular Ca2+. a. The representative fluorescent Ca2+ scanning images of cardiomyocytes affected by the β blockers on TE-induced intracellular Ca2+ overload under 1.8 mM Ca2+ extracellular solution and Ca2+-free condition. b The traces of F/F0 values affected by the β blockers on TE-induced intracellular Ca2+ overload under 1.8 mM extracellular Ca2+ condition (n = 6). c The traces of F/F0 values affected by the β blockers on TE-induced intracellular Ca2+ overload under extracellular Ca2+ free condition. Data are shown by mean ± SD (n = 6)
cAMP
The concentration of the second messenger cAMP that is associated with the β adrenergic stimulation was tested by ELISA in primary neonatal rat cardiomyocytes. TE significantly increased the concentration of cAMP which reached 1.5 times of that in the control. All the β blockers, including propranolol, atenolol and esmolol, prevented the cAMP increase, and no difference was seen among the three groups (Fig. 3), further supporting that TE was able to activate the β adrenergic signaling.
Effect of TE on cAMP concentration and its intervention by β blockers. The cAMP concentration was tested by ELISA in primary neonatal rat cardiomyocytes. The cells were pretreated for 5 min with β-blockers (propranolol, atenolol and esmolol, respectively) before TE administration (60 μg/ml, 45 min). The data are expressed as mean ± SD (n = 6). * P < 0.05 vs. the control. # P < 0.05 vs. TE
PKA activity
The principal function of cAMP on Ca2+ homeostasis during sympathetic excitation is to activate PKA activity. Similar with cAMP concentration, PKA activity in primary neonatal rat cardiomyocytes increased after TE administration, which was also antagonized by the β blockers propranolol, atenolol and esmolol (Fig. 4). Meanwhile, the PKA inhibitor H89 that cutoff the relationship between β adrenergic receptor and Ca2+ release brought about an expected lower and delayed elevation of intracellular Ca2+ in isolated mouse cardiomyocytes (Fig. 5). Combing the above results, a frame of βAR/cAMP/PKA pathway that mediates the intracellular Ca2+ release by TE emerges.
Effect of TE on PKA activity and its intervention by β blockers. The PKA activity was tested by ELISA in primary neonatal rat cardiomyocytes. The cells were pretreated for 5 min with β-blockers (propranolol, atenolol and esmolol, respectively) before TE administration (60 μg/ml, 45 min). Data are expressed as mean ± SD. * P < 0.05 vs. the control. # P < 0.05 vs. TE
Effect of H89 on TE-induced intracellular Ca2+ increase in isolated mouse cardiomyocytes. The PKA inhibitor H89 was preincubated for 5 min with the cardiomyocytes followed by 60 μg/ml TE administration with or without 1.8 mM extracellular Ca2+. a. The representative fluorescent Ca2+ scanning images of cardiomyocytes affected by H89 on TE-induced intracellular Ca2+ increase. b. The traces of F/F0 values affected by H89 on TE-induced intracellular Ca2+ increase (n = 6). Data are shown by mean ± SD (n = 6)
Antagonistic effects of βAR blockers on TE-induced cardiomyocyte toxicity
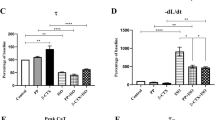
By CCK8 assay, we further analyzed the antagonistic effects of the β blockers and PKA inhibitor H89 on cardiomyocyte toxicity of TE in primary neonatal rat cardiomyocytes that was observed by us previously. All the reagents displayed a significant inhibition on the cardiomyocyte toxicity of TE (Fig. 6), further supporting that the intracellular Ca2+ release was mediated through βAR/cAMP/PKA signaling.
Cardiomyocyte toxicity induced by TE and its intervention by β blockers and H89. Primary neonatal rat cardiomyocytes were preincubated for 30 min with β-blockers propranolol (a), atenolol (b) and esmolol (c), and PKA inhibitor H89 (d), respectively, followed by 60 μg/ml TE administration, then the cell viability was evaluated by CCK8 assay. Data are expressed as mean ± SD (n = 8). * P < 0.05 vs. the control, ** P < 0.01 vs. the control
In vitro effect of βAR blocker on TE-induced acute heart dysfunction
Propranolol was selected as a representative to examine the in vitro antagonistic effect of β blockers on the TE-induced acute heart dysfunction in isolated Langendorff-perfused rat hearts. Propranolol at 1 μmol/L was pre-administrated followed by TE at a dose of 180 μg through the external jugular vein. After TE administration, HR decreased from 293 ± 29 beats per minute (bpm) to 256 ± 26 bpm (Fig. 7a). LVDP declined significantly (Fig. 7b), LVEDP elevated obviously (Fig.7c), both +dP/dtmax and –dP/dtmin decreased accordingly (Fig.7d and e). All these indexes except HR were partially recovered in the propranolol-treated group (Fig. 7), indicating that propranolol could partially attenuate the TE-induced acute heart dysfunction in Langendorff-perfused rat hearts.
In vitro effects of propranolol on the TE-induced acute heart dysfunction. Propranolol at 1 μmol/L was pre-administrated followed by a dose of 180 μg TE in Langendorff-perfused rat hearts. Parameters including HR (a), LVDP (b), LVEDP (c), dp/dtmax (d) and -dp/dtmin (e) were recorded. Data are expressed as mean ± SD (n = 8), * P < 0.05 vs. the control, # P < 0.05 vs. TE
In vivo effect of βAR blocker on the TE-induced decrease of blood pressure
Blood pressure was determined in order to evaluate the antagonistic effect of propranolol on the TE-induced acute heart dysfunction in intact rats. Pre-administration of 0.5 mg/kg propranolol greatly recovered the TE-induced decrease of blood pressure (Fig. 8), indicating that propranolol prevents against the acute heart dysfunction in vivo.
In vivo effects of propranolol on the TE-induced declination of blood pressure (BP). Propranolol at 0.75 mg/kg was pre-administrated, followed by 0.5 mg/kg TE through the external jugular vein in intact rats. The representative images (a) and parameters (b) of BP were displayed. Data are expressed as mean ± SD (n = 8)
Discussion
Cardiotoxicity by jellyfish venom
The cardiotoxicity of jellyfish venom showed great variations. Patients with the famous Irukandij syndrome presented with a significant and ongoing pain but with no or minimal skin markings, tachycardia, hypertension followed by hypotension and pulmonary oedema, indicating a significant cardiac dysfunction and life-threatening induced by the jellyfish Carukia barnesi [27, 28]. Venom from Okinawan box-jellyfish (Habu-kurage), Chiropsalmus quadrigatus, produced an increase in contraction of isolated rat right atrial preparation in a concentration-dependent manner that was significantly inhibited by diltiazem [29]. Intravenous administration of the nematocyst venom from Chiropsalmus quadrigatus produced a dose-dependent hypertension and bradycardia immediately, followed by a significant depressive response of blood pressure and irreversible cardiac arrest in anaesthetized rats and rabbits, which were not affected by prazosin, atropine or BQ123 but attenuated by nicardipine [30, 31]. Intravenous injection of 10 μg/kg nematocyst venom produced a transient pressor response followed by cardiovascular collapse in anaesthetized rats whereas 100 μg/kg TE produced a more prolonged hypertensive effect without cardiovascular collapse that was attenuated by 50 μg/kg prazosin, indicating that a distinct difference of cardiovascular pharmacological effects between nematocyst venom and TE [32].
The manifestation of acute heart dysfunction reported by us from the TE of jellyfish C. capillata mainly displayed in three aspects, including HR decrease, systolic and diastolic dysfunction and imbalance between cardiac oxygen supply and demand. Both in vitro and in vivo investigation displayed that HR decreased dose-dependently that occurred immediately and partially recovered in 10 min after TE administration, indicating a blemish of the sinus node/conduction system [15, 33]. The significant decrease of BPs and LVPs implied a serious injury of left ventricle. Moreover, the serious decrease of EVR and elevation of ST-T segment in ECG indicated an imbalance between the cardiac oxygen supply and demand that might be attributed to the serious coronary spasm [34]. Thus, the acute heart dysfunction caused by TE from jellyfish C. capillata is related to the direct injuries of sinus node/conduction system, ventricular working cells, as well as myocardial ischemia and hypoxia by coronary spasm [23].
Extracellular Ca2+ entry
The exact mechanism of the acute heart dysfunction is not clear, however, intracellular Ca2+ overload induced by extracellular Ca2+ entry has been congruously recognized as an important mechanism underlying the cardiotoxicity of jellyfish venom. As early as 1973, Calton and Burnett found the effect of two jellyfish toxins on calcium ion transport [35]. Since from 1983, the Ca2+ antagonists verapamil, diltiazem and nifedipine were sequentially reported to antagonize cardiotoxicity of the venom from Chironex fleckeri [36], Portuguese man-o’war (Physalia physalis) [37], Carybdea rastonii [38, 39] or C. capillata [33]. However, another study reported that the verapamil had no effect on Ca2+ influx whilst La3+, a non-specific channel and pore blocker, inhibited the Ca2+ influx, consistent with the presence of a pore-forming toxin existing in the venoms which was demonstrated by transmission electron microscopy in the case of C. fleckeri [21]. It was also reported that the venom from the jellyfish C. fleckeri caused extracellular Na+ entry and intracellular Ca2+ overload in cardiomyocytes that was not inhibited by blockers of Ca2+ or Na+ channels or by inhibitors of Na+/K+ ATPase or Na+/H+ exchange in the sarcoplasmic reticulum, but blocked by prior exposure to a solution which contained no Na+ and by Ni2+, indicating a possible mechanism of intracellular Ca2+ overload induced by jellyfish venom via the Na+/Ca2+ exchange [22].
TE from C. capillata led to an intracellular Ca2+ overload that was greatly weakened after removal of the Ca2+ in extracellular solution in this study, further supporting the importance of extracellular Ca2+ entry. Although the extracellular Ca2+ entry can be prevented by the L-type Ca2+ blockers, the mechanism of extracellular Ca2+ entry is now dominated by the existence of pore-forming complex in jellyfish venom that allows a non-specific translocation of Ca2+ across the cell membrane [10, 23]. So far, more than 10 hemolytic proteins have been identified as a novel protein family taxonomically restricted cnidarian toxins (42–46 kDa), from the jellyfish species C. rastoni, C. fleckeri, Cyanea nozakii Kishinouye and Chironex yamaguchii (as C. quadrigatus), respectively [7, 16, 18, 40, 41]. Bioinformatic analysis indicates that these novel proteins function as the non-selective cation pore-forming proteins from jellyfish venoms and thereby contributing to the extracellular Ca2+ entry. However, this is not the only situation, comparative functional analysis of the two pairs of structurally similar hemolytic proteins from Chironex feckeri, CfTX-1/2 and CfTX-A/B, showed that CfTX-1/2 caused profound effects on the cardiovascular system of anaesthetized rats, whereas CfTX-A/B elicited only minor cardiovascular effects but displayed a hemolytic activity at least 30 times greater than that of CfTX-1/2, indicating that the hemolytic proteins of jellyfish venoms have structural diversification and functional selection during evolution [41].
βAR/cAMP/PKA signaling
The involvement of adrenergic system in the cardiovascular toxicity of jellyfish venom was firstly drew by the partial inhibition of the α-adrenergic antagonist phentolamine, the central antiadrenergic reagent trifluoperazine as well as the phosphodiesterase inhibitor papaverine on the aorta contraction induced by the venom of the jellyfish C. rastonii [39]. Further studies showed that the α1-adrenergic antagonist prazosin and β-adrenergic blocker propranolol attenuated the nematocyst venom-induced pressor response and tachycardia in anaesthetized rats [42, 43]. Similar results displayed that the pressor response induced by the venom of the jellyfish Alatina nr mordens was significantly inhibited by prazosin. However, these effects were not uniformed among different jellyfish species. The concentration dependent inotropic response in left atria induced by the crude venom of a newly described jellyfish Malo maxima causing Irukandji syndrome was significantly attenuated by propranolol but not by prazosin [44]. However, a prior administration of prazosin did not significantly attenuate the hypertensive response nor prevent the cardiovascular collapse induced by nematocyst venom of the jellyfish Chiropsalmus sp. [45]. Prazosin did not evidently affect the cardiovascular effects produced by nematocyst venom but significantly attenuated the pressor response produced by TE from C. fleckeri [32]. Another study on the venom from C. fleckeri displayed that both propranolol and prazosin have no effect on the cardiovascular toxicity of the nematocyst venom [46]. Therefore, previous studies from other laboratories have confirmed that the adrenergic system mainly affected the pressor but not the depressor period induced either in vivo or in vitro with different jellyfish venoms.
In this study, we are interested in the intracellular Ca2+ overload through intracellular Ca2+ release that was induced by TE from the jellyfish C. capillata. This phenomenon was hindered by β adrenergic blockers propranolol, atenolol and esmolol. cAMP concentration and PKA activity were both increased correspondingly, implying the involvement of β adrenergic signaling in cardiotoxicity of jellyfish venom. We also forwarded our studies in Langendorff-perfused rat hearts, which have got the partial antagonistic effects of propranolol on the heart dysfunction. The reason for the negative results of adrenergic blockers from previous studies can be explained by the mask of significant extracellular Ca2+ entry through pore-performing components. In intact rats, we used a gentle dose of TE from C. capillata that only led to a BP decrease of approximate 20 mmHg, and thereby allowing to display the role of β adrenergic signaling as well as the antagonistic effect of propranolol. This result is consistent with the change of intracellular Ca2+, where propranolol only partially inhibited the intracellular Ca2+ overload with normal extracellular 1.8 mM Ca2+ while completely abolished the intracellular Ca2+ increase when the extracellular Ca2+ was removed from the bath solution.
Collectively, we have firstly confirmed the involvement of the β adrenergic signaling in the intracellular Ca2+ overload through intracellular Ca2+ release as well as the cardiotoxicity of jellyfish venom from the respects of fluorescence Ca2+ scanning, cardiomyocyte toxicity and acute heart dysfunction in Langendorff-perfused rat hearts and intact rats.
Abbreviations
- ± dP/dtmax :
-
maximal ascending and descending derivative of left ventricle
- BP:
-
blood pressure
- cAMP:
-
cyclic adenosine monophosphate
- DMEM:
-
Dulbecco’s modified Eagle’s medium
- HR:
-
heart rate
- LSCM:
-
laser scanning confocal microscope;
- LVDP:
-
left ventricular developed pressure
- LVEDP:
-
left ventricular end-diastolic pressure
- MAP:
-
mean arterial pressure
- NRVMs:
-
neonatal rat ventricular cardiomyocytes
- PBS:
-
phosphate buffer saline
- PKA:
-
protein kinase A
- RyR2s:
-
ryanodine receptors
- TE:
-
tentacle extract
- βAR:
-
β adrenergic receptor
References
Kim DH, Seo JN, Yoon WD, Suh YS. Estimating the economic damage caused by jellyfish to fisheries in Korea. Fisheries Sci. 2012;78:1147–52.
Schrope M. Marine ecology: attack of the blobs. Nature. 2012;482:20–1.
Boulware DR. A randomized, controlled field trial for the prevention of jellyfish stings with a topical sting inhibitor. J Travel Med. 2006;13:166–71.
Burnett JW, Calton GJ, Burnett HW. Jellyfish envenomation syndromes. J Am Acad Dermatol. 1986;14:100–6.
Cegolon L, Heymann WC, Lange JH, Mastrangelo G. Jellyfish stings and their management: a review. Mar Drugs. 2013;11:523–50.
Mebs D. Jellyfish sting injuries. Hautarzt. 2014;65:873–8.
Chung JJ, Ratnapala LA, Cooke IM, Yanagihara AA. Partial purification and characterization of a hemolysin (CAH1) from Hawaiian box jellyfish (Carybdea alata) venom. Toxicon. 2001;39:981–90.
Yu H, Xing R, Liu S, Li C, Guo Z, Li P. Studies on the hemolytic activity of tentacle extracts of jellyfish Rhopilema esculentum Kishinouye: application of orthogonal test. Int J Biol Macromol. 2007;40:276–80.
Feng J, Yu H, Xing R, Liu S, Wang L, Cai S, Li P. Partial characterization of the hemolytic activity of the nematocyst venom from the jellyfish Cyanea nozakii Kishinouye. Toxicol in Vitro. 2010;24:1750–6.
Wang T, He Q, Xiao L, Wang Q, Zhang B, Wang B, et al. Mitochondrial dysfunction contributes to the cytotoxicity induced by tentacle extract from the jellyfish Cyanea capillata in rat renal tubular epithelial NRK-52E cells. Toxicon. 2013;74:1–7.
Kim E, Lee S, Kim JS, Yoon WD, Lim D, Hart AJ, Hodgson WC. Cardiovascular effects of Nemopilema nomurai (Scyphozoa: Rhizostomeae) jellyfish venom in rats. Toxicol Lett. 2006;167:205–11.
Yanagihara AA, Shohet RV. Cubozoan venom-induced cardiovascular collapse is caused by hyperkalemia and prevented by zinc gluconate in mice. PLoS One. 2012;7(12):e51368.
Sanchez-Rodriguez J, Torrens E, Segura-Puertas L. Partial purification and characterization of a novel neurotoxin and three cytolysins from box jellyfish (Carybdea marsupialis) nematocyst venom. Arch Toxicol. 2006;80:163–8.
Endean R. Separation of two myotoxins from nematocysts of the box jellyfish (Chironex fleckeri). Toxicon. 1987;25:483–92.
Xiao L, Liu G, Wang Q, He Q, Liu S, Li Y, et al. The lethality of tentacle-only extract from jellyfish Cyanea capillata is primarily attributed to cardiotoxicity in anaesthetized SD rats. Toxicon. 2010;55:838–45.
Nagai H, Takuwa K, Nakao M, Ito E, Miyake M, Noda M, Nakajima T. Novel proteinaceous toxins from the box jellyfish (sea wasp) Carybdea rastoni. Biochem Biophys Res Commun. 2000;275:582–8.
Nagai H, Takuwa K, Nakao M, Sakamoto B, Crow GL, Nakajima T. Isolation and characterization of a novel protein toxin from the Hawaiian box jellyfish (sea wasp) Carybdea alata. Biochem Biophys Res Commun. 2000;275:589–94.
Nagai H, Takuwa-Kuroda K, Nakao M, Oshiro N, Iwanaga S, Nakajima T. A novel protein toxin from the deadly box jellyfish (sea wasp, Habu-kurage) Chiropsalmus quadrigatus. Biosci Biotechnol Biochem. 2002;66:97–102.
Brinkman D, Burnell J. Identification, cloning and sequencing of two major venom proteins from the box jellyfish, Chironex fleckeri. Toxicon. 2007;50:850–60.
Lassen S, Helmholz H, Ruhnau C, Prange A. A novel proteinaceous cytotoxin from the northern Scyphozoa Cyanea capillata (L.) with structural homology to cubozoan haemolysins. Toxicon. 2011;57:721–9.
Bailey PM, Bakker AJ, Seymour JE, Wilce JA. A functional comparison of the venom of three Australian jellyfish--Chironex fleckeri, Chiropsalmus sp., and Carybdea xaymacana--on cytosolic Ca2+, haemolysis and Artemia sp. lethality. Toxicon. 2005;45:233–42.
Mustafa MR, White E, Hongo K, Othman I, Orchard CH. The mechanism underlying the cardiotoxic effect of the toxin from the jellyfish Chironex fleckeri. Toxicol Appl Pharm acol. 1995;133:196–206.
Zhang L, He Q, Wang Q, Zhang B, Wang B, Xu F, et al. Intracellular Ca2+ overload induced by extracellular Ca2+ entry plays an important role in acute heart dysfunction by tentacle extract from the jellyfish Cyanea capillata. Cardiovasc Toxicol. 2014;14:260–74.
Wang B, Liu D, Liu G, Zhang X, Wang Q, Zheng J, et al. Protective effects of batimastat against hemorrhagic injuries in delayed jellyfish envenomation syndrome models. Toxicon. 2015;108:232–9.
Bradford M. A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem. 1976;72:248–54.
Fares N, Bois P, Lenfant J, Potreau D. Characterization of a hyperpolarization-activated current in dedifferentiated adult rat ventricular cells in primary culture. J Physiol. 1998;506(Pt 1):73–82.
Little M, Pereira P, Mulcahy R, Cullen P, Carrette T, Seymour J. Severe cardiac failure associated with presumed jellyfish sting. Irukandji syndrome? Anaesth Intensive Care. 2003;31:642–7.
Tibballs J, Li R, Tibballs HA, Gershwin LA, Winkel KD. Australian carybdeid jellyfish causing “Irukandji syndrome”. Toxicon. 2012;59:617–25.
Sakanashi M, Matsuzaki T, Nakasone J, Koyama T, Sakanashi M, Kukita I, Sakanashi M. Effects of diltiazem on in vitro cardiovascular actions of crude venom obtained from Okinawan box-jellyfish (Habu-kurage), Chiropsalmus quadrigatus. Anaesth Intensive Care. 2002;30:570–7.
Noguchi K, Sakanashi M, Matsuzaki T, Nakasone J, Sakanashi M, Koyama T, et al. Cardiovascular effects and lethality of venom from nematocysts of the box-jellyfish Chiropsalmus quadrigatus (Habu-kurage) in anaesthetized rats. Toxicon. 2005;45:519–26.
Koyama T, Noguchi K, Matsuzaki T, Sakanashi M, Nakasone J, Miyagi K, et al. Haemodynamic effects of the crude venom from nematocysts of the box-jellyfish Chiropsalmus quadrigatus (Habu-kurage) in anaesthetized rabbits. Toxicon. 2003;41:621–31.
Ramasamy S, Isbister GK, Seymour JE, Hodgson WC. Pharmacologically distinct cardiovascular effects of box jellyfish (Chironex fleckeri) venom and a tentacle-only extract in rats. Toxicol Lett. 2005;155:219–26.
Wang B, Zhang L, He Q, Wang Q, Wang T, Lu J, et al. Direct cardiac toxicity of the tentacle-only extract from the jellyfish Cyanea capillata demonstrated in isolated rat heart. J Cardiovas Pharm acol. 2012;59:331–8.
Wang B, Zhang B, Huo H, Wang T, Wang Q, Wu YL, et al. Detection of microvasculature alterations by synchrotron radiation in murine with delayed jellyfish envenomation syndrome. Toxicon. 2014;81:48–53.
Calton GJ, Burnett JW. The effect of two jellyfish toxins on calcium ion transport. Toxicon. 1973;11:357–60.
Burnett JW, Calton GJ. Response of the box-jellyfish (Chironex fleckeri) cardiotoxin to intravenous administration of verapamil. Med J Aust. 1983;2:192–4.
Burnett JW, Gean CJ, Calton GJ, Warnick JE. The effect of verapamil on the cardiotoxic activity of Portuguese man-o'war (Physalia physalis) and sea nettle (Chrysaora quinquecirrha) venoms. Toxicon. 1985;23:681–9.
Azuma H, Ishikawa M, Nakajima T, Satoh A, Sekizaki S. Calcium-dependent contractile response of arterial smooth muscle to a jellyfish toxin (pCrTX: Carybdea rastonii). Br J pharm acol. 1986;88:549–59.
Ozaki H, Karaki H, Nagase H, Urakawa N, Azuma H, Nakajima T. Contractile effects of jellyfish toxin extracted from Carybdea rastonii on isolated rabbit aorta. Jpn J Pharm acol. 1986;42:425–30.
Mariottini GL. Hemolytic venoms from marine cnidarian jellyfish - an overview. J Venom Res. 2014;5:22–32.
Brinkman DL, Konstantakopoulos N, McInerney BV, Mulvenna J, Seymour JE, Isbister GK, Hodgson WC. Chironex fleckeri (box jellyfish) venom proteins: expansion of a cnidarian toxin family that elicits variable cytolytic and cardiovascular effects. J Bio Chem. 2014;289:4798–812.
Ramasamy S, Isbister GK, Seymour JE, Hodgson WC. The in vivo cardiovascular effects of the Irukandji jellyfish (Carukia barnesi) nematocyst venom and a tentacle extract in rats. Toxicol Lett. 2005;155:135–41.
Winkel KD, Tibballs J, Molenaar P, Lambert G, Coles P, Ross-Smith M, et al. Cardiovascular actions of the venom from the Irukandji (Carukia barnesi) jellyfish: effects in human, rat and guinea-pig tissues in vitro and in pigs in vitro. Clin Exp Pharmacol Physiol. 2005;32:777–88.
Li R, Wright CE, Winkel KD, Gershwin LA, Angus JA. The pharmacology of Malo maxima jellyfish venom extract in isolated cardiovascular tissues: a probable cause of the Irukandji syndrome in Western Australia. Toxicol Lett. 2011;201:221–9.
Ramasamy S, Isbister GK, Seymour JE, Hodgson WC. The in vivo cardiovascular effects of an Australasian box jellyfish (Chiropsalmus sp.) venom in rats. Toxicon. 2005;45:321–7.
Hughes RJ, Angus JA, Winkel KD, Wright CE. A pharmacological investigation of the venom extract of the Australian box jellyfish, Chironex fleckeri, in cardiac and vascular tissues. Toxicol Lett. 2012;209:11–20.
Funding
This work was supported by the Young Scientists Fund of National Natural Science Foundation of China (81401578) and the National Natural Science Foundation of China (81,370,833, 81,470,518).
Availability of data and materials
All data supporting the conclusions of this study are included within the article.
Author information
Authors and Affiliations
Contributions
QW and LX conceived the study; QW, HZ and BW performed the experiments, BW and CW participated in the statistical analysis; QW drafted the manuscript; LZ and LX contributed to the critical revision of manuscript. All authors read and approved the final manuscript. QW, HZ and BW are co-first authors, LX and LZ are co-corresponding authors.
Corresponding authors
Ethics declarations
Ethics approval
The investigation was carried out in conformity with the requirements of the Ethics Committee of the Second Military Medical University and National Institutes of Health (NIH) guide for care and use of Laboratory animals (NIH Publications No. 8023). Jellyfish catching was permitted by the East China Sea Branch, State Oceanic Administration, People’s Republic of China.
Consent for publication
Not applicable.
Competing interest
The authors declare that they have no competing interest.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Wang, Q., Zhang, H., Wang, B. et al. β adrenergic receptor/cAMP/PKA signaling contributes to the intracellular Ca2+ release by tentacle extract from the jellyfish Cyanea capillata . BMC Pharmacol Toxicol 18, 60 (2017). https://doi.org/10.1186/s40360-017-0167-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s40360-017-0167-0