Abstract
Background
Sexually transmitted infections (STIs) are major infectious diseases worldwide. Around one million people get STIs every day and among them a high burden of the diseases seen in Sub-Saharan African countries. In most developing countries, including Ethiopia, STIs are diagnosed only using syndromic methods, although there seems to be no consensus between syndromic and laboratory-based research.
Objective
To compare the effectiveness of a syndromic versus laboratory-based approach in the diagnosis of sexually transmitted infections, especially Neisseria gonorrhoeae (NG) and Treponema pallidum (TP), infections among those attending a public health center in Addis Ababa, Ethiopia.
Methods
a cross-sectional study was conducted from April 2019 to March 2020, at selected health centers STIs clinics in Addis Ababa, Ethiopia. A total of 325 study participants were involved. From each participant after having socio-demographic data, additional blood, urethral and vaginal discharge was collected. Then serological, Gram stain, culture, and biochemical tests were performed. SPSS version 23 was used to enter and analyze data. All relevant bodies provided ethical approval, and each study participant gave written informed consent.
Results
Among the total participants 167 (51.4%) were males; 177 (54.5%) between ages of 26 and 35; and 178(54.8%) single. Of the total 325 NG, and 125 TP syndromic managed suspected cases, only 163 (50%) and 38 (30.4%) were laboratory- confirmed positive cases respectively. However, there was no statistically significant difference between NG and TP syndromic versus laboratory diagnostic confirmed cases (P-value > 0.005).
Conclusion
The present study indicated that even if, there were no statistical differences between syndromic versus Laboratory diagnosis confirmed NG and TP cases, more than half of syndromic cases could not be confirmed by laboratory diagnosed tests. Thus, to strengthen the present findings, further large-scale studies are recommended.
Plain language summary
Sexually transmitted infections (STIs) are the leading infectious diseases worldwide, and the majority of cases are recorded in developing countries, including Ethiopia. However, diagnosis of STIs in most developing countries done syndromic based, since the laboratory-based tests are relatively expensive, need skilled manpower, and time taking. Therefore regular assessments on how closely related STIs syndromic versus laboratory-based diagnosis should be done, for the proper management of the diseases. In this regard, the present study demonstrated that there was no statistically significant difference between syndromic versus laboratory-based diagnosis of some certain STIs infections; Neisseria gonorrhoeae (NG) and Treponema pallidum (TP), in selected public health centers in Addis Ababa, Ethiopia. However, more than half of syndromic cases could not be confirmed by laboratory diagnosed tests. Thus, to narrow the gap between the two diagnostic approaches, regular training, updates, and similar studies need to cascade in the country. In the meantime, in other developing countries too, regular assessment on STIs syndromic versus laboratory-based diagnosis should be done, to control and prevent STIs infections worldwide.
Similar content being viewed by others
Introduction
The term "sexually transmitted diseases" (STDs) refers to the various clinical symptoms and diseases caused by pathogens spread through sexual activity. More than thirty viral, bacterial, and parasitic infections can be transmitted from person to person through sexual transmission, including vaginal, oral, and anal sex, and some of these, such as syphilis and HIV, can be transmitted from mother to fetus [1,2,3,4].
Gonorrheal is a bacterial disease, caused by Neisseria gonorrhoeae (NG). It is a gram-negative intracellular diplococcic, non-capsulated, and Oxidase-positive organism. It is transmitted during sexual intercourse; by attaching itself to the host via the Pilli, and infecting mucous membranes of the urethra, endo-cervix, pharynx, or rectum [2, 5].
NG left untreated, may lead to prostatitis and epididymitis in men, and into the pelvic areas in women. Thus the bacteria may result, in infertility, ectopic pregnancy, and chronic pelvic pain, as well as prostates, pharyngitis, and on rare occasions, fever, rash, and arthritis. During pregnancy, the organism can spread to their babies' eyes and cause gonococcal ophthalmia and serious conjunctivitis in newborns [6].
Neisseria gonorrhoeae diagnosis may be suggestive, presumptive, or definitive. As a result, we used a presumptive diagnosis approach in this research, and most of the time, NG becomes resistant to many antibiotics that were previously very effective to treat. The most common treatment for Neisseria gonorrhoeae is a single intramuscular injection of 250 mg Ceftriaxone, according to Center for Disease Control (CDC) guidelines [1].
Syphilis is caused by a microorganism called Treponema pallidum (TP), which is a motile spirochete and helically coiled microorganism. Sexual contact is one way for Treponema pallidum to spread. Syphilis is a chronic disorder that is divided into three phases based on clinical results, making recovery and follow-up easier. There are three types of syphilis infection: primary, secondary, and tertiary [1, 7, 8].
TP may also infect the central nervous system, causing neuro-syphilis at any point of the disease. Syphilis diagnosis may be conclusive using Darkfield microscopic examinations or presumptive while using Venereal Disease Research Laboratory (VDRL) and Treponema pallidum Rapid test [1, 8,9,10,11].
In general, syndromic, and laboratory-based diagnoses are two forms of STI diagnosis approaches. Except in rare cases, laboratory diagnosis is the most accurate process. Laboratory diagnosis of STIs, due to requiring specialized testing equipment and skilled technicians, is costly, time-consuming, and findings may not be available at the time of the visit; in most health institutions mainly in developing ones, may result delay in the start of treatment [1, 8,9,10,11].
Thus, in certain developing countries, such as Ethiopia, the syndromic STI diagnosis is the only possible option. Since it is cost-effective, simple, and fast investigations, syndromic diagnosis of STIs is critical for immediate treatment. However, asymptomatic infections are impossible to detect because they are based on subjective judgment. Furthermore, this approach has the potential to lead to over diagnosis and care. Since syndromic diagnosing technique has a major impact on socioeconomic, individually as well as in the region, client morale, healthcare provider integrity, and can be exposed to drug resistance [2, 3, 12,13,14,15,16,17,18,19,20,21,22,23,24,25]. Therefore regular assessments and updates on how closely related Syndromic versus laboratory-based diagnosis of STI diagnosis so essential to provide quality medical services for the patients.
Materials and methods
Study area
This research was carried out in three health centers; Janmeda health center woreda 06, Arada health center woreda 10, and Gerji health center woreda 13, Addis Ababa, Ethiopia. The selected health centers are administered under the Addis Ababa Health Bureau in Addis Ababa, Ethiopia. The study sample was tested at the Ethiopian Public Health Institute's Clinical Bacteriology and Mycology National Reference Laboratory, which is ISO certified laboratory, in Addis Ababa, Ethiopia.
Study design and period
A cross-sectional study was conducted to compare the Syndromic approach versus Laboratory-based approach on STI at a selected Health center in Addis Ababa, Ethiopia, from April 2019–March 2020.
Source population
All clients who visited in selected health center outpatient department out patient department, (OPD) for medical service with a compliant of sign and symptoms of STI.
Study population
All eligible clients who visited in selected health center OPD for STI according to WHO standard Syndromic approach STI management guideline.
Inclusion and exclusion criteria
Inclusion criteria
Clients who visited the study site OPD and have a history or signs and symptoms of Neisseria gonorrhoeae and Treponema pallidum and willing to participate in the study.
Exclusion criteria
Clients who have no signs and symptoms of Neisseria gonorrhoeae and Treponema pallidum and patients having a history of taking antibiotics for the past 10 days are to be excluded.
Study variables
During the study, the socio-demographic status of each study participant, such as age, sex, occupational status, marital status, and educational status was included. In addition, during study participant selection, Symptoms of STIs included abdominal pain, abnormal genital discharge, foul smell in the genital area, excessive genital secretions, swelling of lymph nodes in the genital area, itching in the genital area, burning pain on micturition, pain during intercourse, and genital ulcers were considered.
Measurement and data collection
Sample size calculation and sampling method
In this study sample size was calculated by using single population proportion formula with a confidence interval of 95% and 5% marginal error by taking prevalence of the case (74.1%) from a study conducted at Gondar town hospital and health centers, Ethiopia [26]. And by adding 10%of calculated sample sizes for contingency, finally, the sample size was determined to be three hundred twenty-five. And convenience sampling method is used [1, 27].
Data collection procedure
After taking written informed consent from each study participant, Standard questionnaires were used for collecting socio-demographic data by trained Health care workers. For those clients not attending formal education and poor in reading and writing (here considered as illiterate), the data collectors read the consent form, and when the study participants agreed, signed on the consent form. After completion, it was cleared for completeness, unrecorded value, and unlikely response, and manually cleaned all Laboratory results were registered on the data collection sheet. Complete physical and clinical assessment was performed on all study participants as per the WHO guideline.
Sample collection
Appropriate ureteral and vaginal discharge and blood (serum) samples were collected by a trained clinical nurse. The ureteral and vaginal discharges were transported by Amies transport media to the analysis site following SOPs (adopted from ISO-15189 for sample management). Meanwhile, the blood (Serum) VDRL tests were done at the data collection site medical laboratory units, following the standard SOPS.
Laboratory analysis
For isolation and identification of Neisseria gonorrhoeae
The transported specimen was inoculated on to modified Thayer Martin media, containing vancomycin, colistin, nystatin, and trimethoprim. Then it was incubated under 5–10% CO2 for 24–72 h, meanwhile, a parallel Gram stain was performed to look for polymorph nuclear leucocytes with Gram-negative intracellular diplococci microscopically. Then the isolates were identified as Neisseria gonorrhoeae by presumptive diagnosis method based on colony morphology, Gram staining, catalase test, Oxidase test, and superoxide test.
For rapid immune chromatographic syphilis tests
Serum was used to detect Treponema pallidum by presumptive method Venereal Disease Research Laboratory and Treponema pallidum Rapid test. The test procedure and result reading were performed according to the manufacturer’s instructions ad SOPs.
For both tests, IQC tests were performed with known negative and positive control samples [26].
Data quality assurance
-
• Pre-tested standardized questionnaire was used for comprehensiveness, effectiveness, reliability, and validity.
-
• Training was given for data collectors on data collection procedures with the support of investigators and trained responsible bodies.
-
• Culture media sterility was ensured by incubating in 5% CO2 enriched wet atmosphere candle jar each batch of the prepared media at 37 °C for 24 h and the Performance of prepared media was checked by inoculating with control ATCC strains of Neisseria gonorrhoeae.
-
• Implementing standards based on quality Assurance measurements SOP available on investigation site throughout the whole process of data collection and Laboratory work
-
• SOPs were followed for pre-analytical, analytical, and post-analytical processes in the study site.
Data analysis and interpretation
For data entry and analysis, SPSS (the Statistical Package for Social Sciences for Windows) version 23 statistical software was used. Bivariate analysis was used to determine socio-demographic characteristics versus Neisseria gonorrhoeae, Treponema pallidum and percentage was calculated.
Ethical considerations
The study was approved by the Research and Ethics Committee of the Addis Ababa University College of Health Sciences Department of Medical Laboratory Technology, Ethical clearance was obtained from Addis Ababa Public Health Research and Emergency Management Directorate. The study aim and details were explained to each study participant before obtaining their written consent for data and specimen collection, Confidentiality was maintained at all levels by using codes rather than names of the study participants and the involvement of participants in the study was a voluntary basis.
Participants were informed of their rights to resign from the study at any level of the study without any restriction if they were feeling uncomfortable in the study. Their results of all positive individuals were reported to the respective health facilities for better management of the patients.
Result
Socio-demographic characteristics
A total of 325 STI symptomatically diagnosed and treated patients were enrolled in the study, and of them 167 (51.4%) were males and the remaining 158 (48.6%) were females. The majority of the study participants were between the ages of 26 and 35. (54.5 %). According to the marital status analysis, the majority of people were single 178 (54.8%); whereas only 19 (5.8%) were illiterate. In addition, 221 (68.1%) were non-healthcare practitioners, and 8 (2.5%) were commercial sex workers, as shown in Table 1.
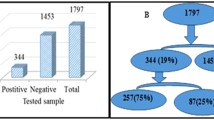
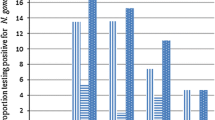
In the present study, among the 325 syndromic Neisseria gonorrhoeae suspected study participants, only 163 (50 %) were laboratory-confirmed positive cases; whereas among 125 syndromic Treponema pallidum suspected study participants, only 38 (30.4 %) were laboratory-confirmed positive cases, as shown in Table 2. Among the 163 laboratory-confirmed NG positive cases, 126 were male, and 37 females; meanwhile among 38 laboratory-confirmed TP positive cases, 26 were male and 12 females.
Although there was no statistical difference between NG and TP syndromic versus laboratory diagnostic confirmed cases (P-value > 0.005), the present study showed big differences seen between the two STIs diagnostic approaches in the selected health centers in Addis Ababa, Ethiopia (Table 2).
Discussion
The main aim of our study was to evaluate syndromic versus laboratory-based diagnosis of STIs, mainly of NG and TP. Many developing countries, including Ethiopia, have adopted a syndromic approach to STI diagnosis and care. Studies indicated that the syndromic method may not be the most successful way to diagnose STI patients. Besides, obtaining the exact magnitude of STIs in most countries takes a lot of effort, due to factors, including stigma, lack of diagnostic facilities, and budget [20,21,22,23].
Our study indicated that among syndromic diagnosed 325 cases163 (50.2%) NG laboratory-confirmed, and from 125 TP cases 38 (30.4%) were laboratory-confirmed. A similar community-based syndromic versus laboratory diagnosis of sexually transmitted infections study conducted in Northern Tanzania, indicated that of the total participated 1520 women, 50% were positive for at least one STI, and of them, syphilis cases account 2.5% and gonorrhea 0.2% [28]. Another study conducted in India indicated that out of 1120 Syndromic STI cases, only 409 (36.5%) cases were confirmed in the laboratory for pathogens [23].
In our study, the laboratory-confirmed NG and TP cases were relatively higher than the compared two studies. These may be due to the laboratory diagnostic methods, distributions of STIs in different areas, study participants category (in our case both male and female, whereas only females in Tanzania). and our study focused only on NG ad TP specific STIs.
In the present study, the laboratory-confirmed NG cases were 163/325 (50.2%), with distributions of 126 (38.8%) cases male, and 37 (11.4%) cases female. Another study done in Addis Ababa, Ethiopia, showed that 7out of 58 (12.07%) urethral discharges were caused by NG [5]. In addition, a study conducted in Gondar town hospitals and health centers (Ethiopia) showed that out of 120 patients who tested positive for STIs, 89 (74.1%) were confirmed cases, and of them, 25 (20.8%) NG laboratory-confirmed ones [26].
On the other hand, our study indicated that from syndromic managed 125 TP cases, 38 (30.4%) were laboratory confirmed. Among the confirmed cases, 26 were male and 12 were females. A similar study done in India showed that out of 1120 Syndromic STI cases 2 cases (0.18%) were serologically confirmed syphilis [23]. A study done in Addis Ababa, Ethiopia, showed that four out of eight (50 %) genital ulcers were caused by syphilis [5]. A similar study conducted in Gondar town hospitals and health centers (Ethiopia) showed that out of 120 patients who tested positive for STIs, 89 (74.1%) were confirmed with TP [26].
In our study, there were no statistically significant differences seen between syndromic diagnosed NG and TP cases versus laboratory-confirmed ones (P > 0.005). A similar study conducted in northern Tanzania also indicated no statistical significance differences between patient-reported STIs symptoms and laboratory-confirmed STI tests [28]. However, large numbers of syndromic cases, in our case 49.8% of NG and 62% of TP did not confirm by the laboratory tests; and more than the number of our percentages in Tanzania similar research [28].
In most sub-Saharan African countries, STIs, including HIV is still high. Thus, as one of the control mechanisms of HIV epidemics in the region and elsewhere, as much as possible accurate laboratory-based diagnoses of STIs are so important. As disadvantages of syndromic STI diagnosis include missing of asymptomatic cases, such as NG cases [29] variations of the algorithm from country to country [30]. Thus, whenever possible, if STIs diagnosis is supported by laboratory tests, it will improve the quality of medical service and great support in STIs prevention and control strategies.
Limitations
-
There was a test specificity limitation for Treponema pallidum
-
Did not include other STI-causing pathogenic organisms.
Conclusion and recommendation
Conclusion
The present study indicated that there were no statistically significant differences between syndromic versus laboratory diagnosis confirmed NG and TP cases. However, there were more than half of syndromic cases could not be confirmed by laboratory diagnosed tests.
Recommendation
The syndromic approach for STI cases in developing countries is important, to give a quick diagnosis ad treatment of patients. However, as the laboratory method is a golden diagnostic standard, the closeness of Syndromic diagnostic methods with the laboratory-confirmed cases should be done regularly. Furthermore, to strengthen the present findings, similar large-scale studies are strongly recommended, both inland, and internationally.
Availability of data and materials
All necessary data related to the research presented within the article. However, upon request, corresponding author can provide any additional data if needed.
Change history
05 May 2022
A Correction to this paper has been published: https://doi.org/10.1186/s12978-022-01416-8
Abbreviations
- CDC:
-
Center for Disease Control
- NG:
-
Neisseria gonorrhoeae
- OPD:
-
Out patient department
- STDs:
-
Sexually transmitted diseases
- STI:
-
Sexually transmitted infection
- STIs:
-
Sexually transmitted infections
- TP:
-
Treponema pallidum
- VDRL:
-
Venereal Disease Research Laboratory
References
Workowski KA, Bolan GA. Sexually transmitted diseases treatment guidelines, 2015. MMWR Morbid Mortal Wkly Rep. 2015;6:1.
Newman L, Rowley J, Vander Hoorn S, Wijesooriya NS, Unemo M, Low N, et al. Global estimates of the prevalence and incidence off our curable sexually transmitted infections in 2012 based on systematic review and global reporting. PLoS ONE. 2015. https://doi.org/10.1371/journal.pone.0143304.
Caini S, Gandini S, Dudas M, Bremer V, Severi E, Gherasim A. Sexually transmitted infections and prostate cancer risk: a systematic review and meta-analysis. Cancer Epidemiol. 2014;38(4):329–38.
Koumans EH, Johnson RE, Knapp JS, St. Louis ME. Laboratory testing for Neisseria gonorrhoeae by recently introduced nonculture tests: a performance review with clinical and public health considerations. Clin Infect Dis. 1998;27(5):1171–80.
Harvard Health Topics A-Z, Gonorrhea. Medically reviewed on Jun 15, 2018.
Rebecca Hersher, Gonorrhea is becoming untreatable, U.N. Health Officials Warn. NPR 20165:12.
Stübs G, Schumann RR. Recognition of Treponema pallidum and other spirochetes by the innate immune system. Syphilis-Recogn Descript Diagn. 2011;1:3–18.
Kamali A, Quigley M, Nakiyingi J, Kinsman J, Kengeya-Kayondo J, Gopal R, et al. Syndromic management of sexually-transmitted infections and behaviour change interventions on transmission of HIV-1 in rural Uganda: a community randomised trial. Lancet. 2003;361(9358):645–52.
Reda AA, Fisseha S, Mengistie B, Vandeweerd JM. Standard precautions: occupational exposure and behavior of health care workers in Ethiopia. PLoS ONE. 2010;5(12): e14420.
World Health Organization. Global prevalence and incidence of selected curable sexually transmitted infections: overview and estimates. Geneva: World Health Organization; 2001.
Centres for Disease Control and Prevention. Sexually transmitted disease surveillance 2010. Atlanta, GA: US Department of Health and Human Services. 2009.
Ghebremichael M. The Syndromic versus laboratory diagnosis of sexually transmitted infections in resource-limited settings. International Scholarly Research Notices. 2014; 2014.
Moges B, Yismaw G, Kassu A, Megabiaw B, Alemu S, Amare B. Sexually transmitted infections based on the syndromic approach in Gondar town, North West Ethiopia: a retrospective study. BMC Public Health. 2013;13(1):143.
Sonkar SC, Wasnik K, Kumar A, Sharma V, Mittal P, Mishra PK, et al. Evaluating the utility of syndromic case management for three sexually transmitted infections in women visiting hospitals in Delhi, India. Sci Rep. 2017;7(1):1465.
Shethwala ND, Mulla SA, Kosambiya JK, Desai VK. Sexually transmitted infections and reproductive tract infections in female sex workers. Indian J Pathol Microbiol. 2009;52(2):198.
Expert Working Group on Canadian Guidelines for Sexually Transmitted Infections. Canadian guidelines on sexually transmitted infections. Public Health Agency of Canada, ISBN, 2013; 978-1100.
Masha SC, Cools P, Sanders EJ, Vaneechoutte M, Crucitti T. Trichomonas vaginalis and HIV infection acquisition: a systematic review and meta-analysis. Sex Transm Infect. 2018. https://doi.org/10.1136/sextrans-2018-053713.
De Waaij DJ, Dubbink JH, Ouburg S, Peters RP, Morré SA. Prevalence of Trichomonas vaginalis infection and protozoan load in South African women: a cross-sectional study. BMJ Open. 2017. https://doi.org/10.1136/bmjopen-2017-016959.
RaffeS, Soni S. Diagnostic tests for sexually transmitted infections. Medicine. 2018.
Low N, Broutet N, Adu-Sarkodie Y, Barton P, Hossain M, Hawkes S. Global control of sexually transmitted infections. Lancet. 2006;368(9551):2001–16.
Rostami MN, Rashidi BH, Habibi A, Nazari R, Dolati M. Genital infections and reproductive complications associated with Trichomonas vaginalis, Neisseria gonorrhoeae, and Streptococcus agalactiae in women of Qom, central Iran. Int J Reprod BioMed. 2017;15(6):357.
Otieno FO, Ndivo R, Oswago S, Ondiek J, Pals S, McLellan-Lemal E, et al. Evaluation of syndromic management of sexually transmitted infections within the Kisumu incidence cohort study. Int J STD AIDS. 2014;25(12):851–9.
Tankhiwale SS, Chavan SP. Comparative study of Syndromic and etiological diagnosis of sexually transmitted infection except human immunodeficiency virus in sexually transmitted infection and reproductive tract infection clinic attendees in central India. Int J Med Public Health. 2013; 3(4).
Ray K, Muralidhar S, Bala M, Kumari M, Salhan S, Gupta SM, et al. Comparative study of syndromic and etiological diagnosis of reproductive tract infections /sexually transmitted infections in women in Delhi. Int J Infect Dis. 2009; 13(6).
NIMH Collaborative HIV/STD Prevention Trial Group. Syndromic and laboratory diagnosis of sexually transmitted infection: a comparative study in China. Int J STD AIDS. 2008;19(6):381–4.
Geremew RA, Agizie BM, Bashaw AA, Seid ME, Yeshanew AG. Prevalence of selected sexually transmitted infection and associated factors among symptomatic patients attending Gondar Town hospitals and health Centers. Ethiop J Health Sci. 2017;27(6):589–600.
Etikan I, Musa SA, Alkassim RS. Comparison of convenience sampling and purposive sampling. Am J Theor Appl Stat. 2016;5(1):1–4.
Cheng Y, Paintsil E, Ghebremichael M. Syndromic versus laboratory diagnosis of sexually transmitted infections in men in Moshi District of Tanzania. AIDS Res Treat. 2020. https://doi.org/10.1155/2020/7607834.
Syndromic management of sexually transmitted infections-Canadian guidelines on sexually transmitted infections-updated Jan2010.section-4
Bosu WK. Syndromic management of sexually transmitted diseases: is it rational or scientific? Trop Med Int Health. 1999;4(2):114–9.
Acknowledgements
The authors would like to thank all the study participants and staff at the data collection site health centers. Besides, authors duly acknowledge EPHI microbiology laboratory staff, Gondar University microbiology laboratory staff, and Addis Ababa University, College of Health Sciences, School of Medical Laboratory Sciences, health science college. The authors would like to also acknowledge Miss Thuria Adem for her support in editing the manuscript. Finally, the authors thank Addis Ababa University, as well Ethiopian Public Health Institute Anti-Microbial Resistance Surveillance Program for partial financial support of the study.
Funding
Addis Ababa University College of Health Sciences Department of Medical Laboratory Technology and Ethiopian Public Health Institute Anti-Microbial Resistance Surveillance Program provided minimal financial support.
Author information
Authors and Affiliations
Contributions
EA is the first researcher who prepared the proposal, analyzed and interprets the finding, and prepared the manuscript. SF and ZW reviewed the proposal, assisted in data collection and review of the manuscript. SE and ES assisted the identification and interpretation processes, and review the manuscript. MW reviewers of the proposal, main research work, prepared final version of the manuscript. and correspondence author. All authors have read, reviewed and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The study was approved by the Research and Ethics Committee of the Addis Ababa University College of Health Sciences Department of Medical Laboratory Science and Addis Ababa Public Health Research and Emergency Management Directorate. The privacy and confidentiality of the study participants’ data were protected. This research article did not have individual person’s data in any form, or the case of children. Thus separate consent form did not attach. But, if needed we can provide. However, from where we got ethical clearance for the mentioned in the declarations.
Competing interests
The authors declare that there is no competing interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Ayalew, E., Fentaw, S., Ebrahim, S. et al. Comparison of syndromic versus laboratory-confirmed diagnosis of Neisseria gonorrhoeae and Treponema pallidum, infections at the selected health centers in Addis Ababa, Ethiopia. Reprod Health 19, 88 (2022). https://doi.org/10.1186/s12978-022-01395-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12978-022-01395-w