Abstract
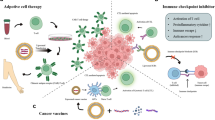
Immunotherapy has gradually emerged as the most promising anticancer therapy. In addition to conventional anti-PD-1/PD-L1 therapy, anti-CTLA-4 therapy, CAR-T therapy, etc., immunotherapy can also be induced by stimulating the maturation of immune cells or inhibiting negative immune cells, regulating the tumor immune microenvironment and cancer vaccines. Lipid nanovesicle drug delivery system includes liposomes, cell membrane vesicles, bacterial outer membrane vesicles, extracellular vesicles and hybrid vesicles. Lipid nanovesicles can be used as functional vesicles for cancer immunotherapy, and can also be used as drug carriers to deliver immunotherapy drugs to the tumor site for cancer immunotherapy. Here, we review recent advances in five kinds of lipid nanovesicles in cancer immunotherapy and assess the clinical application prospects of various lipid nanovesicles, hoping to provide valuable information for clinical translation in the future.
Similar content being viewed by others
Background
As one of the diseases with the highest mortality, a cancer diagnosis is usually considered a death sentence for most people. To date, thousands of scientists and doctors have spent great deal of energy in cancer research, and their efforts have greatly improved the survival chances of cancer patients. According to authoritative statistics, the mortality rate of cancer has decreased since 1991 and has continued to decline through 2017, which is mainly due to the declining mortality of breast cancer, colorectal cancer, lung cancer and prostate cancer [1,2,3,4].
Currently, a variety of cancer therapies have been applied in the clinic, such as surgery, radiotherapy, chemotherapy, immunotherapy, gene therapy, radionuclide therapy, endocrine therapy and photodynamic therapy (PDT) [5,6,7,8,9,10]. However, although there are a large number of cancer-related basic research studies, drug developments and clinical trials every year, the limitations of antitumor drugs are consistently an unavoidable topic, especially the side effects [11,12,13,14,15,16]. Most of the side effects of anticancer drugs are due to toxicity to nontumor tissues, especially for traditional therapies. For example, chemotherapy can cause the cardiotoxicity, peripheral neurotoxicity, myelosuppression, alopecia, nausea and vomiting [17,18,19,20,21]. To maximize clinical efficacy while minimizing side effects, cancer-targeted nanoparticles have been tried to be used in cancer therapy. Due to the unique nanoscale size of nanoparticles and the special tumor pathological environment, nanoparticles can easily enter and be retained in tumor tissue, which is also known as the enhanced permeability and retention (EPR) effect [22,23,24]. For example, Liu et al. designed a highly effective supramolecular nanomicellar drug formulation carrying doxorubicin, which exhibited potent anticancer activity for pancreatic ductal adenocarcinoma (PDAC) [25]. Moreover, to further improve the aggregation ability of nanoparticles in tumor tissues, most scientists modify the surface of nanoparticles to actively target tumors, to improve their targeting ability. For instance, He et al. designed Angiopep-2 coupled polymersomes targeting glioblastoma to increase the concentration of drugs in glioblastoma and reduce the aggregation of drugs in noncancer areas, which achieved a great curative effect [26].
According to the Web of Science, there are thousands of studies about the application of nanoparticles in cancer therapy annually. However, only a few nanoparticles have been applied in the clinic. Most studies remain at the stage of animal experiments. Here we list three main reasons that hinder the clinical translation of nanoparticles. Firstly, most nanoparticles have complex components, which make them difficult to metabolize. Secondly, the high cost of production and difficult quality control would greatly increase the medical expenses of patients, which limits the popularization and application of nanoparticles in the clinic. Lastly, unquantifiable toxicology and pharmacokinetics lead to uncertain safety effects and therapeutic effects [27]. Nevertheless, in the past few decades, a number of nanoparticles have been approved for cancer therapy by the Food and Drug Administration (FDA), most of which are liposome-based nanoparticles [28], such as Eligard [29], DaunoXome [30], Marqibo [31], Onivyde [32], Doxil [33], Abraxane [34], Ontak [35] and Nanotherm [36] (Table 1). Similar to liposomes, cell membrane vesicles, bacterial outer membrane vesicles (OMVs) and extracellular vesicles (EVs) also have phospholipid membranes, which possess good biocompatibility and efficient drug loading capacity and exhibit potential for clinical translation. Here, we classified liposomes, cell membrane vesicles, bacterial outer membrane vesicles, extracellular vesicles and hybrid vesicles as lipid nanovesicles.
In 2018, Chen and his colleagues proposed that the concept of tumor immunotherapy should change from enhancement to normalization. They concluded that traditional tumor immunotherapy mainly focuses on enhancing immunity by using effector cells/molecules to stimulate the immune system to directly attack tumor cells, which is also called “passive” immunotherapy, such as antibody-targeted therapies (e.g., Her2/neu monoclonal antibody (mAb) [37], anti-EGFR mAb [38] and anti-CD20 mAb) and adoptive immune cell therapies (e.g., macrophage-based adoptive cell therapy [39], chimeric antigen receptor (CAR)-T [40], CAR-NK [41] and adoptive CD8+ T-cell therapy [42]). Recently, immune checkpoint related therapies have attracted more attention, including programmed death-1 (PD-1), programmed death ligand 1 (PD-L1) [43, 44] and CD47 [45, 46]. Moreover, the FDA has approved several anti-PD-1/PD-L1 drugs since 2014. In addition, there are a variety of immunomodulatory drugs and cancer vaccines that can stimulate the immune system modulating the cancer immune microenvironment and improving the local immune status of cancer, and they are defined as “active” immunotherapies. In summary, they presented a theory of water flow in pipelines (Fig. 1), and an unobstructed pipeline represents normal immunity. Under pathological conditions, the pipeline is blocked, which means that the immune response is insufficient. The immune enhancement approach can slightly improve the flow by increasing the pressure with the risk of breaking the pipeline, which means that improving the immune response by enhancers would also cause adverse effects. In contrast, the immune normalization approach identifies and removes the block and restores the flow without pipeline damage [47].

Reprint with permission from [47]. Copyright 2018, Elsevier
Schematic illustration of the Immune-Normalization versus Immune-Enhancement Approaches. Using proper flow and drainage of a pipeline as a comparison for the antitumor immune response. The flow of the pipeline can be insufficient when a blockade impairs flow, as the antitumor immune response can be insufficient when there is an immune impairment. The immune enhancement approach is illustrated as an increase inflow or pressure to return to proper function/flow with the risk of breaking the pipe (adverse effects). In contrast, the immune normalization approach would be to identify and try to unblock this specific blockage and restore the flow.
Here, we focus on the recent advances in lipid nanovesicle drug delivery systems (LNDDSs) in cancer immunotherapy and from these cutting-edge studies, we analyze the current challenges and future perspectives of LNDDS for translational in cancer immunotherapy (Fig. 2).
Liposomes in cancer immunotherapy
Liposomes were first discovered in 1965 by Bangham et al. [48]. Liposomes are spherical lipid bilayer vesicles with hydrophobic and hydrophilic regions. As one of the best candidates for drug delivery systems, liposomes possess good drug loading capacity and biocompatibility. With the development of tumor immunotherapy, how to combine liposome drug delivery systems with immunotherapy has become a new research topic [49, 50].
As one of the most successful types of immunotherapy, immune checkpoints, as potential cancer immunotherapy targets, have also been applied to liposome drug delivery systems. Considering that cancer cells can escape immune surveillance by surface overexpression of CD47 and PD-L1, Shu et al. designed an epithelial cell adhesion molecule (EpCAM)-targeted cationic liposome with si-PD-L1 and si-CD47, which could actively target EpCAM overexpressing cancer cells and knockdown the PD-L1 and CD47 proteins. This liposome-based dual-blockade cancer cell immune checkpoint therapeutic strategy effectively activated anticancer T cells and nature killer (NK) cells, and promoted the release of cytokines such as interferon-γ (IFN-γ) and interleukin-6 (IL-6), which exhibit good anticancer abilities [51].
In the clinic, due to individual differences and cancer heterogeneity, traditional anti-PD-1/PD-L1 therapy cannot achieve the ideal therapeutic effect for most patients. To solve this problem, scientists have combined anti-PD-1/PD-L1 therapy with other therapeutic strategies, such as Improving cancer immunogenicity and activating anti-cancer immune cells (dendritic cells (DCs), T cells, NK cells, tumor-associated macrophages (TAMs), etc.) and decreasing the number of suppressor immune cells (e.g., T regulatory cells (Tregs) and myeloid-derived suppressor cells (MDSCs)). Chen et al. prepared a liposome that dual-modified anti-PD-L1 and mannose for targeting PD-L1 on cancer cells and mannose receptor (MR, aka CD206) on TAMs. Moreover, this liposome was encapsulated with an antiangiogenic drug (regorafenib) and an mTOR inhibitor (rapamycin) to ameliorate the tumor immune microenvironment (TIME). This kind of liposome delivery system can simultaneously inhibit angiogenesis, repolarize TAMs, inhibit glycolysis, reprogram immune cells and effectively reduce the tumor volume and is a promising liposome delivery system for cancer combination therapy [52]. Guido Kroemer and Laurence Zitvogel discovered and put forward the concept of immunogenic cell death (ICD). ICD can improve the immunogenicity of tumors and turn “cold tumors” into “hot tumors”, so that immune cells can recognize tumors easily, which provides a new idea for cancer treatment [53]. Tu et al. use liposome as the carrier, co-deliver the chidamide (CHI), an epigenetic modulator, and BMS-202 (a PD-L1 inhibitor) as a synergistic cancer treatment strategy. They verified that CHI could induce ICD in triple-negative breast cancer (TNBC) and enhance cancer immunogenicity. In addition, CHI can increase the levels of major histocompatibility complex-I (MHC-I) and MHC-II on TNBC cells, which can promote antigen presentation and T-cell recognition. Furthermore, CHI can promote DC maturation and activate NK cells. Combined with anti-PD-L1 drugs, this liposome can effectively inhibit tumor growth and metastasis [54] (Fig. 3). Xiong et al. designed a two-in-one nanoplatform (IR775@Met@Lip), and the photosensitizer IR775 and metformin were encapsulated in liposomes. PDT, as a promising strategy, can generate reactive oxygen species (ROS) to damage cancer cells and promote anticancer immunity by increasing the secretion of IFN-γ. However, the increased secretion of IFN-γ induced by PDT would extremely increase the expression of PD-L1 on the cancer cells, and it would weaken the function of T cells. Metformin (Met), as an oral hypoglycemic drug, is used as a treatment drug for type II diabetes clinically [55, 56]. Recent studies have found that metformin can reduce the expression of PD-L1 on the surface of cancer cells [57]. In this liposome drug delivery system, Met can remedy the side effects of PDT and reduce the expression of PD-L1 on the tumor surface. Combined with the advantages of PDT in tumor treatment, this IR775@Met@Lip system can be a promising cancer therapy modality [58].

Reprint with permission from [54]. Copyright 2021, American Chemical Society
CHI/BMS-202@lipF-Mediated Synergistic TNBC Treatment. a Schematic Illustration of CHI/BMS-202@lipF-Mediated Synergistic TNBC Treatment. b Treatment schedule for CHI/BMS-202@lipF-mediated antitumor combination therapy in vivo. c Average tumor volume. d Survival rate of mice with various treatments (n = 8).
MDSCs, as inhibitory cells, exist in the tumor environment. The immune response can be obstructed by MDSCs through various mechanisms [59]. As one of the star products in liposomes, Doxil has been widely used in the clinic. Compared with free doxorubicin (DOX), Doxil exhibits lower cardiotoxicity [60, 61]. Recently, DOX has been proven to have the potential to enhance immunity and inhibit the population and function of MDSCs [62]. Jamshid et al. designed a new liposomal platform, modified P5 peptide on Doxil. This liposome can stimulate the immune system and decrease the effect of MDSCs, which can effectively inhibit tumor growth [63].
A recent study showed that indoleamine 2,3-dioxygenase 1 (IDO-1) is highly expressed in tumors and can promote the induction of Tregs and inhibit the growth of infiltrating T cells [64]. Several IDO-1 inhibitors have shown an efficient immunomodulatory ability by reversing the immunosuppressive TIME [65,66,67]. Nevertheless, limited by the water solubility and bioavailability of IDO inhibitors, liposomes are a suitable drug carrier for IDO inhibitors [68, 69]. To solve the problem of drug delivery of IDO inhibitors, Mei et al. encapsulated the indoximod (IND) prodrug in the lipid bilayer of liposomes combined with mitoxantrone (MTO) in the hydrophilic layer. Compared with liposomal MTO, the immune response was significantly enhanced by co-delivery an IDO-1 inhibitor in IDO-overexpressed cancers, such as renal cancer (RENCA) and breast cancer (4T1 and EMT6) [67].
Since the end of 2019, the world has been experiencing a severe pandemic due to the outbreak of coronavirus disease-19 (COVID-19) [70, 71]. To date, the most effective preventive measure is vaccination, and among all of the vaccines, the messenger ribonucleic acid (mRNA) vaccine is the most effective and widely used vaccine. Most FDA-approved COVID-19 vaccines are delivered by lipid nanoparticles, such as BNT162b2 (BioNTech/Pfizer) and mRNA-1273 (Moderna) [72]. Similarly, although there are officially approved products in the clinic, mRNA vaccines still exhibit great potential in cancer immunotherapy [73]. As one of the most popular mRNA delivery carriers, cationic liposomes can concentrate mRNA and can be easily absorbed by antigen-presenting cells (APCs). Mai et al. attempted to encapsulate positively charged protamine concentrated mRNA with cationic liposomes. The nasal administration of the cationic liposome/protamine complex can promote the maturation of dendritic cells and contribute to inducing an antitumor immune response in vivo, to inhibit the growth of tumors, which proves that cationic liposomes can be used as an efficient and safe carrier for mRNA cancer vaccine in future clinical translation [74] (Fig. 4).

Reprint with permission from [74]. Copyright 2020, Elsevier Inc
a Schematic illustration of synthesis process of cationic liposome/protamine complex (LPC) and immunotherapy in Lewis lung cell. b Transmission electron micrograph of LPC/mRNA. Scale bar = 200 nm. c Tumor growth of mice bearing LLC during treatment. Stimulation of CD4+T cells (d) and CD8+T cells e in the spleen. Data are presented as the mean ± SD (n = 4). *p < 0.05, ***p < 0.001. f and g Spleen cells from mice after administration of different formulations collected 1 week after the final immunization and cultured with CK19 for 72 h. The supernatants were collected and the production of cytokines IL-4 and IL-2 was measured. The results are presented as the mean ± SD of experiments performed in triplicate. Data are presented as the mean ± SD *p < 0.05, **p < 0.01, ***p < 0.001.
In summary, as one of the best nano drug carriers, liposomes are convenient to prepare and possess high drug encapsulation efficiency, which exhibit great clinical translation potential. However, liposomes don’t have therapeutic function. In addition to conventional drug loading, we also need to endow them with some functions through chemical or physical methods, such as targeting ability, immunotherapeutic ability and so on. However, the preparation process of large-scale functional liposomes is complex and cumbersome, which makes the preparation process difficult to quality control and increases the difficulty of clinical translation.
Cell membrane vesicles in cancer immunotherapy
After the great translational success of liposomes in the clinic, biomembrane-based vesicles have also been considered to be an efficient drug delivery system [75]. Recently, a variety of vesicles derived from different cell membranes have been developed, such as vesicles derived from the membrane of leukocytes, red blood cells, platelets, mesenchymal stem cells and cancer cells etc. [76, 77].
Among all kinds of cell sources, cancer cells can be successfully applied in cancer immunotherapy, especially as vaccine carriers [78,79,80,81]. Christopher et al. prepared a tumor membrane vesicles (TMVs) vaccine, isolated TMVs from 4T1 tumor tissue, and modified immunostimulatory IL-12 and B7-1 (CD80) molecules on the surface of TMVs. TMV-based vaccine-mediated immunotherapy combined with anti-cytotoxic T-lymphocyte-associated protein 4 monoclonal antibody (anti-CTLA-4 mAb) treatment effectively stimulated the immune system, enhanced the immunity of CD8+ T cells, reduced tumor metastasis and improved the survival rate [82]. Liu et al. designed a DC targeted nanovaccine by modifying functionalized DC targeted deoxyribonucleic acid (DNA) in TMVs, which combined with immune checkpoint blockade treatment can target DCs and trigger a robust anticancer immune response [83] (Fig. 5). Flavia and his colleagues developed a multistage nanovaccine (NV). They encapsulated thermally oxidized porous silicon (TOPSi) into acetalated dextran (AcDEX) or spermine-modified AcDEX (SpAcDEX) polymeric particles, named TOPSi@AcDEX, which can stimulate DCs and the secretion of proinflammatory cytokines with biodegradability and biocompatibility. Subsequently, TOPSi@AcDEX was encapsulated with TMVs, and the antigenic composition of tumor lysate combined with the adjuvant properties of TOPSi@AcDEX greatly enhanced the anticancer immune system [84]. Recently, Liu et al. designed a tumor vaccine named NP@FM that fused cytomembranes of DCs and tumor cells. Owing to the membrane of DCs, NP@FM emerged antigen-presenting ability. Since NP@FM contained tumor membrane fragments, DCs can recognize NP@FM and induce maturation of DCs, thereby activate antitumor immunity [85]. Furthermore, Jiang et al. engineered cancer cell membrane with co-stimulatory marker, and developed a biomimetic nanoparticle platform that can direct stimulate T cells without professional antigen presenting cells. This novel cancer immunotherapy strategy bypassed the traditional antigen presentation process and exhibited strong immune activation ability [86] (Fig. 6). Meng and his colleagues prepared genetically programmable fusion tumor cell membrane vesicles (Fus-CVs) for double-targeting immune checkpoint blockade therapy, which displayed SIRP-α variants and PD-1. Fus-CVs can significantly increase the phagocytosis of macrophages to cancer cells, promote antigen presentation ability, and activate T-cell immunity. Consequently, Fus-CVs can effectively inhibit the recurrence and metastasis of post-surgery tumor [87]. These results indicated that TMV-based personalized tumor vaccine immunotherapy can effectively improve the immune response and enhance the efficacy of immunotherapeutic drugs, which has great potential for clinical application.
a Schematic illustration to show the preparation of nano vaccines from tumor-cell-derived CMVs and their functions to induce antitumor immunity. b A TEM image of cancer CMVs. c The survival curves of different groups of mice with CT26 tumors after various treatments. d Growth curves of CT26 tumors on mice after various treatments. The statistical data of effective memory T cells (TEM) e and central memory T cells (TCM) (f) in the peripheral blood before rechallenging the mice with secondary tumors. Reprint with permission from [83].

Reprint with permission from [86]. Copyright 2020, WILEY‐VCH Verlag GmbH & Co. KGaA, Weinheim
a Schematic of engineered cell-membrane-coated nanoparticles for direct antigen presentation. b Expression of CD69 by OT-I CD8 + T cells in the draining lymph nodes 3 days after administration of [CD80/OVA]NPs or control nanoparticles into C57BL/6 mice adoptively transferred with OT-I splenocytes (n = 4, mean + SD). c Secretion of IFN-γ by draining lymph node cells 4 days after administration of [CD80/OVA]NPs or control nanoparticles into C57BL/6 mice adoptively transferred with OT-I splenocytes (n = 3, mean + SD). Average tumor sizes (f) and survival (h) over time for the therapeutic efficacy study (n = 6; mean ± SEM). ***p < 0.001, ****p < 0.0001 (compared to [CD80/OVA]NP); one-way ANOVA.
In addition to TMV-based nanoplatforms, genetically engineered cellular vesicles have also demonstrated competitiveness in cancer immunotherapy. Li et al. prepared CD64 presenting cellular NVs derived from overexpressed CD64 HEK 293 T cells so that PD-L1 antibody can easily conjugate with NVs. Additionally, to inhibit Tregs, they encapsulated a low dosage of cyclophosphamide (CP) into NVs. These new NVs enhanced the function of T cells with a PD-L1 antibody and activated CD8 T cells with a low dosage of CP, effectively prolonging the survival time of mice [88] (Fig. 7). Similarly, Zhang’s group genetically engineered H293T cells to express PD-1 receptors on the surface of their membranes, and then nanovesicles with PD-1 receptors (PD-1 NVs) were obtained. PD-1 NVs can disrupt the PD-1/PD-L1 immune inhibitory axis. In addition, PD-1 NVs can also carry a variety of different therapeutic drugs to achieve collaborative treatment, which makes PD-1 NVs a multifunctional immunotherapy nanoplatform [89] (Fig. 8).

Reprint with permission from [88]. Copyright 2021, Ivyspring International Publisher
a Schematic of preparation of CD64-NVs-aPD-L1-CP and immune boosting mechanism of NVs. b Average tumor sizes for the treated mice (n = 5). The experimental data were shown as mean ± SEM. c Survival curves for the mice treated with PBS (#1), CD64-NVs (#2), CD64-NVs-aPD-L1 (#3), CD64-NVs-CP (#4), CP + aPD-L1 (#5) and CD64-NVs-CP-aPD-L1 (#6) groups. (n = 5). d Representative plots of T cells in tumors of different treatment detected by flow cytometry (Gated on CD3+). e Representative plots of Foxp3 in Tregs infiltrating in tumors detected by the flow cytometry (gated on CD4+).
a Schematic illustration and characterization of PD-1 blockade cellular NVs for cancer immunotherapy. b The TEM image showed the shape and size of PD-1 NVs. Scale bar: 100 nm. c Cryoscanning electron microscopy (CSEM) image showed the natural shape of the PD-1 NVs (Scale bar: 100 nm). d Average tumor volumes of the treated mice in different groups (n = 7). Error bar, mean ± s.e.m. e Survival curves for the mice received the treatment of PD-1 NVs, PD-L1 antibody, and free NVs (n = 10). (f) IFN-γ levels in serum from mice isolated at day 20 after mice received the first indicated treatment (n = 3). Error bar, mean ± s.d. g Quantitative analysis of T cells (gated on CD3+ cells) in treated tumor analyzed by flow cytometry (n = 3). Error bar, mean ± s.d. Reprint with permission from [89].
As we mentioned before, CD47 is highly expressed on the surface of tumor cells. There are several CD47 antagonists being tested in clinic trails. However, M2-type macrophages restrict the efficacy of CD47 antagonists and CD47 antagonists would cause serious anemia and thrombocytopenia. In order to improve the effect of anti-CD47 immunotherapy, Rao et al. designed a hybrid cell membrane nanovesicles (known as hNVs), which consists of platelet-derived NVs (P-NVs), M1 macrophage-derived NVs (M1-NVs) and cancer cell-derived NV overexpressing high-affinity SIRP-α variants (SαV-C-NVs). The hNVs can accumulate in surgical wound sites and target circulating tumor cells (CTCs) in the blood by P-NVs. M1-NVs can repolarize M2 macrophages into M1 macrophages. In this study, hNVs effectively amplified macrophage responses against cancer recurrence and metastasis after surgery [90] (Fig. 9).

Reprint with permission from [90]. Copyright © 2020, Springer Nature
a Schematic showing the hNVs consist of engineered SαV-C-NVs, M1-NVs, and P-NVs. b Schematic showing the hNVs efficiently interact with CTCs in the blood, accumulate in the post-surgical tumor bed, repolarize TAMs towards M1 phenotype, and block the CD47-SIRPα ‘don’t eat me’ pathway, thus promoting macrophage phagocytosis of cancer cells, as well as boosting antitumor T cell immunity. c Average tumor growth kinetics and d survival rate in different groups. All data are presented as mean ± S.D. (n = 6 for the hNVs-treated group, n = 5 for the other groups). Statistical significance was calculated via 2way ANOVA with a Tukey’s test d or log-rank (Mantel–Cox) test e. e Flow cytometric analysis of M2-like macrophages (CD206+) and M1-like macrophages (CD80+) in tumor gating on F4/80+CD11b+CD45+ cells. (f) Flow cytometric analysis of CD8+ and CD4+ T cells in tumor gating on CD45+ cells. g Cytokine levels in tumors from mice isolated 5 days after different treatments. All data are presented as mean ± S.D. (n = 4). Statistical significance was calculated via ordinary one-way ANOVA with a Tukey’s test. *p < 0.05; **p < 0.01; ***p < 0.001.
NK cells, as a type of innate immune cell, are the first line of resistance to cancer and infection. What’s more, NK cells can mediate M1-macrophage polarization and specifically target cancer cells by proteins expressed on the surface of NK cell membranes. Based on the characteristics mentioned above, Deng’s group developed a novel immunotherapy strategy based on the NK cell membrane with PDT, which named as NK-NPs. This study demonstrated that NK-NPs can target to cancer cells and enhance M1-macrophage polarization by NK cell membrane to produce anticancer immunity. In addition, PDT can induce ICD to enhance the anticancer immunity efficacy stimulated by NK cell membrane [91].
All in all, cell membrane vesicles are more like a kind of functional liposomes. There are a large number of tumor specific antigens (TSAs) and tumor associated antigens (TAAs) on the surface of tumor derived cell membrane vesicles, which can induce the maturation of APCs, while cell membrane vesicles derived from immune cells can affect the tumor immune microenvironment and play an important role in immune activation effect through their own biological functions. For most cell membrane vesicles, the expected biological functions can be obtained by transfection, so as to activate antitumor immunity. Compared with liposomes, which need to be endowed with biological functions by physical or chemical methods, cell membrane vesicles have inherent advantages in this regard. However, cell membrane vesicles are often obtained from cell lines, which will cause a certain degree of immune rejection. At the same time, high acquisition cost and low yield also limit the clinical translation of cell membrane vesicles.
Bacterial outer membrane vesicles in cancer immunotherapy
Outer membrane vesicles (OMVs) are spherical nanovesicles that are naturally released by gram-negative bacteria with a lipid bilayer and the size is approximately 20–250 nm [92, 93]. In 1997, Bermudes and his colleagues found that Salmonella can be a novel drug delivery platform for targeting cancer [94]. However, the toxicity of bacteria limits their clinical translation as anticancer carriers in cancer immunotherapy. OMVs are released from bacteria, so that OMVs possess a composition similar to that of bacteria. Additionally, genetically engineered attenuated bacteria can produce OMVs with reduced endotoxicity. Therefore, attenuated OMVs have application value in cancer immunotherapy.
Keman et al. attempted to establish an OMVs-based flexible tumor vaccine platform to display target antigens by genetic engineering and “Plug-and-Display” technology [95,96,97]. They found that antigen can easily fuse with ClyA protein on the surface of OMVs. Therefore, this OMV-based tumor vaccine platform can stably integrate with antigens and efficiently accumulate in lymph nodes, which means that OMV-based tumor vaccines can efficiently deliver antigens to lymph nodes and present antigens to DCs, leading to antigen-specific T-lymphocyte-mediated anticancer immune responses [98] (Fig. 10). OMVs can break the tolerance of B cells and the surface of OMVs is rich in lipopolysaccharides (LPSs) and outer membrane proteins, which are the major components of pathogen-associated molecular patterns (PAMPs). This makes OMV a perfect natural adjuvant. Huang et al. modified basic fibroblast growth factor (BFGF), an angiogenic molecule, on the surface of OMVs. As an anticancer vaccine, BFGF-OMVs can break the tolerance of B cells, so that persistent and high levels of anti-BFGF autoantibodies can be produced by the immune system, which exhibits persistent, efficient, and multifunctional tumor suppression effects [99]. These studies showed that OMV, as a natural adjuvant, is one of the most suitable platforms for cancer vaccines.

Reprint with permission from [98]. Copyright © 2021, Springer Nature
a Schematic illustration of ClyA-Catcher (CC) OMVs system for antigen display. b TEM and DLS analysis of CC OMVs. Scale bar, 100 nm. c The maturation status of DCs in inguinal lymph nodes on days 17 post immunization. The percentage of CD80+ and CD86+ cells in CD11c+ cells was assessed by flow cytometry. d Flow cytometry analysis of the percentage of IFN-γ+ cytotoxic T lymphocytes in splenocytes re-stimulated with OVA257–264 antigen. Tumor volumes (e) were recorded, and survival rate (f) was monitored after immunized with the indicated formulations on days 3, 7, and 11. g Tumors were harvested on day 29 for flow cytometry analysis (n = 4) of the following immune cells: CD3+, CD3+CD8+, CD3+CD4+, CD3+CD4+Foxp3+ T lymphocytes, activated neutrophils (CD11b+Ly6G+ cells), macrophages (F4/80+ cells), dendritic cells (CD11c+ cells), and MDSCs (CD11b+Gr1+ cells). The data are shown as mean ± SD. Statistical analysis was performed by two-tailed unpaired t test (e, g) and two-sided log-rank test (f). N.S. no significance.
Due to the existence of multiple biological barriers, the efficiency of nanodrug delivery will be greatly reduced. To overcome this issue, Li et al. reported an OMV-based nanoplatform that encapsulated NPs@Pt into OMVs. OMVs can be recognized and phagocytized by neutrophils, so that neutrophils can be a temporary carrier. According to the tendency of neutrophils to undergo inflammation, the author suggested that through photothermal therapy (PTT), an inflammatory region can be created in the tumor area, so that neutrophils can carry NPs@Pt into the tumor area. On the one hand, it can improve the delivery efficiency of drugs; on the other hand, it can make up for the incomplete curative effect of PTT [100].
Qing et al. found that OMVs would rapidly lead to serious systemic inflammatory responses via intravenous (i.v.) injection. To address this issue, the authors used calcium phosphate with high biocompatibility to encapsulate OMVs with pH sensitive nanoshells. In the slightly acidic microenvironment of the tumor, the calcium phosphate shell is dissolved, which can neutralize the acidic TME but can also expose OMVs to the tumor tissue and stimulate the local immune response [101].
To summarize, the biological characteristic of OMV makes it an ideal natural adjuvant, which will be beneficial for cancer immunotherapy. In addition, same as the other kinds of nanoparticles, OMV has the potential to load both hydrophilic and hydrophobic drugs, so that OMV as an adjuvant can combine other therapeutic methods (e.g., PDT, PTT, targeted therapy, etc.) to activate anticancer immunity. However, the drug encapsulation efficiency depends on the ability of drugs to cross the OMVs’ membrane barrier. What’s more, detoxification of OMV is an urgent problem to be solved for OMV-based nanoparticles and how to maintain a balance between detoxification and retaining enough efficacy of adjuvanticity is a topic that needs to be in-depth discussed [92].
Extracellular vesicles in cancer immunotherapy
In 1980, Trams et al. first proposed the term “exosome” [102]. EVs include microvesicles, exosomes and apoptotic bodies. Studies have shown that almost all living cells can secrete EVs, which are isolated from various kinds of biological fluids [103, 104]. EVs express the same membrane proteins as the source cells, so tumor-derived extracellular vesicles (TEVs) have the potential to become tumor vaccines [105]. Muzaffer et al. used 4T1/Her2 cell-derived exosomes as a novel exosome-based therapeutic vaccine nanoplatform. To improve the immune response to TSAs on the surface of tumor derived exosomes (TEXs), the authors chose nucleic acid-based adjuvants to induce innate immunity. Consequently, CpG oligonucleotides (CpG ODNs) and polyinosinic-polycytidylic acid (p(I:C)) were co-encapsulated into 4T1/Her2 cell-derived exosomes, which could generate humoral and cell-mediated immune responses simultaneously [106]. A previous study showed that DCs and T cells can be significantly activated by single miRNAs (Let-7i, miR-155 and miR-142) [107], Adeleh et al. designed tumor-derived EVs encapsulated with multiple miRNAs (including Let-7i, miR-155 and miR-142), which could improve the survival rate and inhibit tumor growth [108].
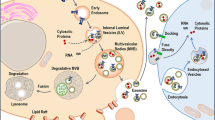
Immune cells-derived EVs, such as DCs, are also promising nanoplatforms for immunotherapy [109]. DC-derived small EVs, also named DC-sEVs, contain several immunologically relevant components, making DC-sEVs a novel candidate for cancer immunotherapy. However, DC-sEVs cannot induce sufficient anticancer immunity. To compensate make up for this defect, Akihiro et al. added ovalbumin (OVA) create DC-sEVs with high immunity, and added LPS and IFN-γ to prepare DC-sEVs with high immune activity. Then, sEVs were collected from activated DCs (also named activated-DCOVA-sEVs), and the activated-DCOVA-sEVs exhibited great therapeutic effects in tumor-bearing mice [110]. It is noteworthy that there are several basic researches and clinic trails reported that mature DC derived sEVs exhibited immunogenic potential and had capability to activate the T cells and NK cells. On the contrary, immature DC derived sEVs can induce Treg cells and even play an important role in maintaining peripheral tolerance [111,112,113]. Therefore, mature DC derived sEVs are more suitable as nanocarrier in cancer immunotherapy. Moreover, M1 macrophage-derived EVs (M1-EVs) also hold great potential in cancer immunotherapy. Ding et al. developed an M1-EV-based vehicle encapsulated with chlorin e6 (Ce6), prodrug aldoxorubicin (Dox-EMCH) and bis [2,4,5-trichloro-6-(pentyloxycarbonyl) phenyl] oxalate (CPPO), named M1CCD. After tail vein administration, M1-EVs can specifically target the tumor area and polarize macrophages from M2-like tumor-associated macrophages (M2-TAMs) to M1-like tumor-associated macrophages (M1-TAMs). In addition to the immune activation effect, H2O2 can also be produced. Chemical energy was generated by the reaction between H2O2 and CPPO, which can activate Ce6 without light and produce ROS. ROS can induce membrane rupture to release the prodrug Dox-EMCH, which can be activated by the acidic tumor microenvironment. The treatment strategy integrates immunotherapy, photodynamic therapy and chemotherapy, which enhances the therapeutic effect of cancer [114] (Fig. 11).

Reprint with permission from [114]
a Schematic illustration of the trimodal anticancer therapy by using M1CCD. b TEM image of M1CCD. Scale bar: 200 nm. c Production levels of IL-6 and TNF-α in M2 macrophages assayed by ELISA after different treatments for 24 h. d Tumor growth curves for all treated groups and (e) survival rates of tumor-bearing mice receiving different treatments in vivo. f Time-dependent ratios of the M1 phenotype to the M2 phenotype in tumor tissues after treatment with M1CCD.
Additionally, adoptive T-cell therapy, such as chimeric antigen receptor T-cell (CAR-T) Immunotherapy, has emerged as a promising immunotherapy for various kinds of cancers [115]. Despite the unique therapeutic effect of CAR-T immunotherapy, it also has serious side effects that cannot be ignored, such as cytokine release syndrome (CRS) [116]. Fu et al. found that CAR-containing exosomes released from CAR-T cells express ample cytotoxic molecules and will not be weakened by anti-PD-L1 treatment. Moreover, CAR exosomes are much safer than CAR-T therapy in CRS models [117].
In recent years, it has been reported that bone marrow mesenchymal stem cells (BMSCs) or BMSC-derived exosomes have tumor-homing functions in several mouse models [118, 119], which makes BMSC and BMSC-derived exosomes promising nanovesicle drug delivery platforms. Zhou et al. developed a BMSCs-derived exosome-based nanovesicle, electroporation-loaded galectin-9 siRNA, for reversing tumor immunosuppression by M2-TAMs and modified it with ICD-triggered OXA-prodrug on the surface of exosomes (iEXO-OXA). This nanovesicle drug delivery system can elicit anticancer immunity by reversing M2-TAMs polarization, cytotoxic T lymphocyte recruitment and Treg downregulation and exhibits excellent therapeutic effects [120] (Fig. 12).

Reprint with permission from [120]. Copyright 2020, Elsevier Ltd
a Pancreatic cancer-targeting exosomes for enhancing immunotherapy and reprogramming tumor microenvironment. b The statistic of tumoral bioluminescence and c survival rate in vivo (n = 8, i.v., 5 mg OXA/kg, ~ 108 exosomes per mouse). d Statistical results of M1/M2 ratio (n = 3). Statistical results of (e) mature DCs, (f) CD8+T cells, and (e) Treg cells in orthotopic PANC-02 tumor-bearing mice after various treatments analyzed by flow cytometry. Data presented as means ± SD, one-way ANOVA, *p < 0.05, ***p < 0.001, ****p < 0.0001. (Groups: 1. PBS; 2. GEM; 3.OXA; 4. Scrbl-iEXO; 5. iEXO; 6. EXO-OXA; 7. iEXO-OXA).
In conclusion, EVs inherit the biological characteristics of the originated cells. Among all kinds of EVs, immune cells-derived EVs play a significant role in tumor immune microenvironment and can be used as promising candidate nanocarriers for cancer immunotherapy. Notably, that the immature DCs and M2 macrophages derived EVs would promote the tumor suppressive immune microenvironment, so they are not recommended as nanocarriers in tumor immunotherapy. Besides, although tumor-derived EVs can stimulate the anticancer immunity, tumor-derived EVs are still considered to be involved in tumorigenesis and immune escape. Similar to tumor-derived EVs, BMSC-derived EVs show good biosafety, but BMSC-derived EVs would reduce DCs maturation, promote the polarization of M2 macrophages and increase the infiltration of Tregs. So, if we attempt to use tumor-derived EVs or BMSC-derived EVs as the nanocarriers in cancer immunotherapy, we need to weigh the pros and cons [121]. Moreover, the drug encapsulation efficiency of EVs is limited, and also has the disadvantages of low yield and high cost, which hinders the progress of clinical translation.
Hybrid nanovesicles in cancer immunotherapy
The nanovesicles mentioned above have their own characteristics. Fusion of different types of nanovesicles can compensate for the defects of single nanovesicle [122]. Among them, bacterial OMVs have strong immunogenicity and natural adjuvant properties, which can play an important role in tumor immunotherapy. To improve the efficacy of other types of nanovesicles in cancer immunotherapy, bacterial OMVs are often mixed with other types of nanovesicles to form hybrid vesicles to participate in cancer immunotherapy. Zhai et al. designed a novel biomimetic nanoplatform, named PLOVs, by fusing OMVs and photosensitive liposomes carrying CD38 siRNA (PTSLs). PTSLs can induce ICD by PTT and enhance the function of T cells by CD38 siRNA. Moreover, OMVs can enhance the immune response through their own adjuvant effect [123]. Wang’s group and Chen’s group both developed OMV-cancer cell member vesicle (OMV-CMV) nanoplatforms with PTT. CMVs have homing characteristics and can specifically target tumors, and the TSA on the surface of CMVs can stimulate the anticancer immunity through mature APCs. However, due to the inability to effectively stimulate the maturation of APCs in the TME, it is necessary to use immune stimulants to stimulate the maturation of APCs. Fortunately, as a natural adjuvant, OMVs can accomplish this function. Both OMV-CMVs exhibited excellent targeting ability and immune activation ability and achieved good cancer immunotherapy effects [124, 125]. Similar to the strategies mentioned above, Zou et al. designed a personalized immunotherapy strategy and formed a new functional vesicle (mTOMV) by hybridizing an OMV with the cell membrane from a tumor (mT). mTOMV effectively inhibits the growth and metastasis of tumors with a simple preparation procedure and good biocompatibility [126] (Fig. 13).

Reprint with permission from [126]. Copyright 2021, Wiley‐VCH GmbH
a Schematic Illustration of the Hybrid Vesicles from Bacteria Outer Membrane and Tumor Cell Membrane to Enhance Innate Immune Response for Personalized Immunotherapy. b TEM image of mTOMV. Scale bar = 50 nm. c Hydrodynamic size distribution and PDI of mT, OMV, and mTOMV. d The percentage of CD11b+NKG2D+ cells in 4T1 tumors (n = 3). e The percentage of CD80+CD86+ cells in 4T1 tumors (n = 3). f The percentage of CD3+CD8+ cells in 4T1 tumors (n = 3). g The percentage of CD80+CD86+ cells in lymph nodes (n = 3). h The percentage of CD3+CD8+ cells in lymph nodes (n = 3). i The relative tumor volume of CT26 tumors treated with control, mT, OMV, mT + OMV, and mTOMV, respectively (n = 7). Data are represented as mean ± SD. Statistical significances were calculated via one-way ANOVA, *p < 0.05, ***p < 0.001, ****p < 0.0001.
As the most successful nanovesicles in clinical translation, liposomes possess good biosafety and drug loading efficiency. Natural nanovesicles, such as exosomes can specifically express some proteins by genetic engineering of source cells, but with insufficient encapsulation of drugs [127, 128]. Cheng et al. designed hybrid therapeutic nanovesicles, which fused gene-engineered CD47 overexpressing exosomes with drug-loaded thermosensitive liposomes, named hGLV. By fusing liposomes with exosomes, the difficulty of liposome-modified proteins and the problem of the low drug loading rate of exosomes were solved. The novel hybrid nanovesicle exhibited the long blood circulation and enhanced the phagocytosis of cancer cells by macrophages, achieved a great photothermal treatment effect and effectively inhibited the growth of tumors [129] (Fig. 14).

Reprint with permission from [129]. Copyright 2021, Elsevier Ltd
a The design principle of hGLV and the antitumor mechanism of hGLV through PTT combined with immunotherapy. b A typical morphology of hGLV obtained by TEM. c Size distribution of lip, exos and hGLV. d Quantitative of the expression of CD47 on the surface of I/R@hELV and I/R@hGLV by Flow Nano Analyzer. ICD evaluation. e Flow cytometric analysis of CRT exposure on the surface of CT26 cells, f The levels of HMGB1 and g ATP levels in the supernatant of CT26 cells. Antitumor Efficacy of I/R@hGLV plus laser in vivo. h Tumor volume growth curves and (i) Kaplan–Meier survival analysis of the mice bearing CT26 tumors after treatment. Quantitative analysis of DCs maturation in the spleens induced by different treatments on mice bearing CT26 tumors. ***p < 0.001, **p < 0.01, *p < 0.05.
In brief, hybrid vesicles can combine the advantages of different types of vesicles to achieve a better therapeutic effect than single type of vesicles do. However, it still faces the disadvantages of high production cost and low yield. Moreover, it is more difficult to prepare hybrid vesicles than single type of vesicles, which makes the clinical translation of hybrid vesicles much harder than the other type of vesicles we mentioned before.
Concluding and future perspectives
As one type of lipid-nanovesicle (LNV), the clinical application of liposome chemotherapy drugs has greatly improved the survival time of cancer patients. Because they have the same lipid bilayer structure as cells, LNVs possess great biocompatibility, which means that LNVs have great potential for translation. In addition, immunotherapy has been a great success in cancer therapy, but the immunotherapeutic drugs approved by the FDA are not effective for all kinds of cancer, and only a minority of patients benefit from it. Moreover, some immune checkpoint blockade (ICB) treatments can cause serious systemic side effects [130, 131]. This makes us wonder whether LNDDSs can be used for cancer immunotherapy to solve the current problems of immunotherapy. For this reason, we summarize the latest advances in LNDDSs in cancer immunotherapy.
Liposomes, as the star product of LNVs, possess good biocompatibility. In addition, compared with other kinds of LNVs, liposomes have better drug loading capacity regardless of whether the drug is hydrophobic or hydrophilic [132]. Moreover, in order to obtain the biological function of liposomes and achieve the purpose of cancer immunotherapy or targeting tumors, we need to modify the surface of liposome membrane with proteins or peptides through postinsertion or chemical bonds. Although liposomes have a complete and mature preparation process, the complex modification process and difficult purification still bring challenges to the clinical translation of engineered liposomes, which will limit the application of liposomes in cancer treatment.
Bacterial outer membrane vesicles are derived from gram-negative bacteria, so that OMVs can stimulate a nonspecific immune response, which makes OMVs a natural adjuvant. According to existing studies, OMVs are most suitable as a perfect auxiliary component of tumor vaccines. Due to their adjuvant property, OMVs need to combine with other anti-cancer treatments to activate specific anti-cancer immunity. Also, it’s more suitable for OMVs to combine with other nanovesicles to form hybrid vesicles for cancer immunotherapy. OMVs also have an obvious disadvantage: the endotoxins of OMVs will lead to a systemic immune response, so they need to be attenuated, while retaining sufficient adjuvant effect. To address this issue, it is necessary to quantify the toxicity reduction of OMVs in the future to ensure their toxicity is in a controllable range while maintaining its adjuvant effect.
Cell membrane vesicles and EVs also have great clinical translation potential. Among the different kinds of cell-derived vesicles, tumor-derived cell membrane vesicles and tumor-derived EVs both express TSAs on the surface of membranes and can be used as tumor vaccines for cancer immunotherapy. However, although TSAs are located on the surface of vesicle membranes, it is still necessary to stimulate the tumor microenvironment and activation of immune cells (e.g., APCs, T cells, macrophages) to achieve the ideal therapeutic effect. In addition, PD-L1 expressed on the surface of tumor cell membrane is a recognized mechanism of tumor immune escape which may lead to tumor progression and even the emergence of local metastasis. In particular, Chen et al. found that tumor exosomal PD-L1 would suppress the function of CD8 T cells extremely hinder the development and application of this kind of LNV [133]. Moreover, except for some immunosuppressive cell-derived cell membranes and immunosuppressive cell-derived EVs, such as immature DCs-derived vesicles, M2 macrophages-derived vesicles and so on, most immune cell-derived cell membrane vesicles and immune cell-derived EVs can induce anticancer immunity, but the anticancer effect is very limited. Therefore, this therapeutic strategy needs to be combined with other therapeutic methods to produce a stronger immune response in cancer. Conventional cell-derived vesicles include BMSC-derived vesicles, platelet-derived vesicles, H293T cell-derived vesicles, etc. Compared with other cell-derived vesicles mentioned above, conventional cell-derived vesicles can’t directly stimulate cancer immunity. In particular, BMSC-derived vesicles will induce tumor suppressive immune microenvironment. However, conventional cell-derived vesicles also possess the advantages other cell-derived vesicles don’t have. For example, BMSC-derived vesicles have homing ability and can target tumor sites specifically, platelet-derived vesicles can accumulate in surgical wound sites and target CTCs in the blood, which is suitable for the patients after tumor surgery, H293T cell-derived vesicles can be engineered by transfecting the H293T cell, which is easy to transfect and also known as the “tool cell”. What’s more, it is worth noting that most cell membrane vesicles are originated from cell lines, which may induce immune rejection in model mice or patients. Additionally, high cost and low yield also restrict the clinical translation of cell membrane vesicles and EVs.
In summary, we introduced LNVs and the application progress in cancer immunotherapy. LNVs, as nanoparticles with clinical translation potential will benefit patients by large-scale application in the future. The biggest issue facing liposomes is that compare with the other LNVs it is complex to modify the proteins on their surface, and it is difficult to purify after modification. OMVs and tumor-derived vesicles are candidates for tumor vaccines. However, OMVs need to find a balance between reducing toxicity and maintaining adjuvant function. Tumor derived vesicles can promote the occurrence and development of tumors and may lead to tumor metastasis. Researchers need to weigh the benefits of tumor derived vesicles-based cancer immunotherapy for patients. For most EVs and OMVs, there are many methods to encapsulate drugs, such as electroporation, co-incubation, sonication and so on, however, the low drug encapsulation efficiency is an urgent problem needs to be solved. For the LNVs mentioned in this review, it is limited in clinical translation owing to its high cost, low yield and huge workload. Once we overcome this problem, EVs will have broad application prospects. In the future, novel and multifunctional nanoplatforms based on LNVs will be developed, and we are confident in LNVs’ clinical translation for cancer immunotherapy.
Abbreviations
- LNDDS:
-
Lipid nanovesicle drug delivery system
- PDT:
-
Photodynamic therapy
- EPR:
-
Enhanced permeability and retention
- FDA:
-
Food and drug administration
- OMV:
-
Outer membrane vesicle
- PDAC:
-
Pancreatic ductal adenocarcinoma
- EV:
-
Extracellular vesicle
- mAb:
-
Monoclonal antibody
- CAR:
-
Chimeric antigen receptor
- PD-1:
-
Programmed death-1
- PD-L1:
-
Programmed death ligand 1 ()
- EpCAM:
-
Epithelial cell adhesion molecule
- IFN-γ:
-
Interferon-γ
- IL-6:
-
Interleukin-6
- NK:
-
Nature killer
- DC:
-
Dendritic cell
- TAM:
-
Tumor-associated macrophage
- Treg:
-
T regulatory cell
- MDSC:
-
Myeloid-derived suppressor cell
- MR:
-
Mannose receptor
- TIME:
-
Tumor immune microenvironment
- ICD:
-
Immunogenic cell death
- CHI:
-
Chidamide
- MHC-I:
-
Major histocompatibility complex-I
- TNBC:
-
Triple-negative breast cancer
- ROS:
-
Reactive oxygen species
- Met:
-
Metformin
- DOX:
-
Doxorubicin
- IDO-1:
-
2,3-Dioxygenase 1
- IND:
-
Indoximod
- MTO:
-
Mitoxantrone
- COVID-19:
-
Coronavirus disease-19
- mRNA:
-
Messenger ribonucleic acid ()
- TMV:
-
Tumor membrane vesicle
- CTLA-4:
-
Cytotoxic T-lymphocyte-associated protein 4
- DNA:
-
Deoxyribonucleic acid
- NV:
-
Nanovaccine
- TOPSi:
-
Thermally oxidized porous silicon
- AcDEX:
-
Acetalated dextran
- SpAcDEX:
-
Spermine-modified AcDEX
- CP:
-
Cyclophosphamide
- LPS:
-
Lipopolysaccharide
- PAMPs:
-
Pathogen-associated molecular patterns
- BFGF:
-
Basic fibroblast growth factor
- PTT:
-
Photothermal therapy
- TEV:
-
Tumor-derived extracellular vesicle
- TEX:
-
Tumor derived exosome
- CpG ODN:
-
CpG oligonucleotide
- p(I:C):
-
Polyinosinic-polycytidylic acid
- CPPO:
-
Bis [2,4,5-trichloro-6-(pentyloxycarbonyl) phenyl] oxalate
- CAR-T:
-
Chimeric antigen receptor T-cell
- CRS:
-
Cytokine release syndrome
- BMSC:
-
Bone marrow mesenchymal stem cell
- CMV:
-
Cancer cell member vesicle
- APC:
-
Antigen-presenting cell
- LNV:
-
Lipid-nanovesicle
- ICB:
-
Immune checkpoint blockade
- TSA:
-
Tumor special antigen
- TAAs:
-
Tumor associated antigens
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2020. CA Cancer J Clin. 2020;70:7–30.
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A. Global cancer statistics, 2012. CA Cancer J Clin. 2015;65:87–108.
Torre LA, Siegel RL, Ward EM, Jemal A. Global cancer incidence and mortality rates and trends–an update. Cancer Epidemiol Biomarkers Prev. 2016;25:16–27.
Ferlay J, Colombet M, Soerjomataram I, Parkin DM, Pineros M, Znaor A, Bray F. Cancer statistics for the year 2020: an overview. Int J Cancer. 2021;149:778–89.
Wen L, Zhong G, Zhang Y, Zhong M. Risk and prognosis of secondary bladder cancer after postoperative radiotherapy for gynecological cancer. Bosn J Basic Med Sci. 2021. https://doi.org/10.17305/bjbms.2021.6338.
Malik D, Mahendiratta S, Kaur H, Medhi B. Futuristic approach to cancer treatment. Gene. 2021;805: 145906.
Elston MS, Love A, Kevat D, Carroll R, Siow ZR, Pattison S, Boyle V, Segelov E, Strickland AH, Wyld D, et al. Pituitary function following peptide receptor radionuclide therapy for neuroendocrine tumours. Cancer Med. 2021;10:8405–11.
Chen YC, Yu J, Metcalfe C, De Bruyn T, Gelzleichter T, Malhi V, Perez-Moreno PD, Wang X: Latest generation estrogen receptor degraders for the treatment of hormone receptor-positive breast cancer. Expert Opin Investig Drugs 2021:1–15.
Luyten K, Van Loy T, Cawthorne C, Deroose CM, Schols D, Bormans G, Cleeren F. D-Peptide-based probe for CXCR4-targeted molecular imaging and radionuclide therapy. Pharmaceutics. 2021;13:1619.
Ding Y, Yang R, Yu W, Hu C, Zhang Z, Liu D, An Y, Wang X, He C, Liu P, et al. Chitosan oligosaccharide decorated liposomes combined with TH302 for photodynamic therapy in triple negative breast cancer. J Nanobiotechnology. 2021;19:147.
Devlin EJ, Denson LA, Whitford HS. Cancer treatment side effects: a meta-analysis of the relationship between response expectancies and experience. J Pain Symptom Manage. 2017;54(245–258): e242.
Floyd JD, Nguyen DT, Lobins RL, Bashir Q, Doll DC, Perry MC. Cardiotoxicity of cancer therapy. J Clin Oncol. 2005;23:7685–96.
Le Saux O, Falandry C. Toxicity of cancer therapies in older patients. Curr Oncol Rep. 2018;20:64.
Xu Y, Fu Y, Zhu B, Wang J, Zhang B. Predictive biomarkers of immune checkpoint inhibitors-related toxicities. Front Immunol. 2023;2020:11.
Herrmann J. Vascular toxic effects of cancer therapies. Nat Rev Cardiol. 2020;17:503–22.
Dibs K, Palmer JD, Olausson A, Bourekas E, Boulter D, Ayan AS, Cochran ER, Yildiz V, Grecula JC, Arnett ALH, et al. Circumferential stereotactic body radiotherapy for spine metastasis: the feasibility, toxicity and local control. Int J Radiat Oncol Biol Phys. 2021;111: e607.
Maxwell MB, Maher KE. Chemotherapy-induced myelosuppression. Semin Oncol Nurs. 1992;8:113–23.
Chon SY, Champion RW, Geddes ER, Rashid RM. Chemotherapy-induced alopecia. J Am Acad Dermatol. 2012;67:e37-47.
Razvi Y, Chan S, McFarlane T, McKenzie E, Zaki P, DeAngelis C, Pidduck W, Bushehri A, Chow E, Jerzak KJ. ASCO, NCCN, MASCC/ESMO: a comparison of antiemetic guidelines for the treatment of chemotherapy-induced nausea and vomiting in adult patients. Support Care Cancer. 2019;27:87–95.
Arinno A, Maneechote C, Khuanjing T, Ongnok B, Prathumsap N, Chunchai T, Arunsak B, Kerdphoo S, Shinlapawittayatorn K, Chattipakorn SC, Chattipakorn N. Cardioprotective effects of melatonin and metformin against doxorubicin-induced cardiotoxicity in rats are through preserving mitochondrial function and dynamics. Biochem Pharmacol. 2021;192: 114743.
Kawashiri T, Inoue M, Mori K, Kobayashi D, Mine K, Ushio S, Kudamatsu H, Uchida M, Egashira N, Shimazoe T. Preclinical and clinical evidence of therapeutic agents for paclitaxel-induced peripheral neuropathy. Int J Mol Sci. 2021;22:8733.
Xu WJ, Cai JX, Li YJ, Wu JY, Xiang D. Recent progress of macrophage vesicle-based drug delivery systems. Drug Deliv Transl Res. 2022. https://doi.org/10.1007/s13346-021-01110-5.
Chen X, Huang Y, Chen H, Chen Z, Chen J, Wang H, Li D, Su Z. Augmented EPR effect post IRFA to enhance the therapeutic efficacy of arsenic loaded ZIF-8 nanoparticles on residual HCC progression. J Nanobiotechnology. 2022;20:34.
Zhang XP, Chen XJ, Li BZ, Xu S, Wu ZL, Hu MG, Zhao ZM, Zhao GD, Wang CR, Hong W, et al. Active targeted Janus nanoparticles enable anti-angiogenic drug combining chemotherapy agent to prevent postoperative hepatocellular carcinoma recurrence. Biomaterials. 2022;281: 121362.
Liu J, Chen C, Wei T, Gayet O, Loncle C, Borge L, Dusetti N, Ma X, Marson D, Laurini E, et al. Dendrimeric nanosystem consistently circumvents heterogeneous drug response and resistance in pancreatic cancer. InExploration. 2021;1:21–34.
He C, Zhang Z, Ding Y, Xue K, Wang X, Yang R, An Y, Liu D, Hu C, Tang Q. LRP1-mediated pH-sensitive polymersomes facilitate combination therapy of glioblastoma in vitro and in vivo. J Nanobiotechnology. 2021;19:29.
Chen H, Shou K, Chen S, Qu C, Wang Z, Jiang L, Zhu M, Ding B, Qian K, Ji A, et al. Smart self-assembly amphiphilic cyclopeptide-dye for near-infrared window-II imaging. Adv Mater. 2021;33:e2006902.
Bobo D, Robinson KJ, Islam J, Thurecht KJ, Corrie SR. Nanoparticle-based medicines: a review of FDA-approved materials and clinical trials to date. Pharm Res. 2016;33:2373–87.
Sartor O. Eligard: leuprolide acetate in a novel sustained-release delivery system. Urology. 2003;61:25–31.
DaunoXome approved. AIDS Patient Care STDS 1996, 10:263.
FDA approves liposomal vincristine (Marqibo) for rare leukemia. Oncology (Williston Park) 2012, 26:841.
Frampton JE. Liposomal irinotecan: a review in metastatic pancreatic adenocarcinoma. Drugs. 2020;80:1007–18.
Safra T, Muggia F, Jeffers S, Tsao-Wei DD, Groshen S, Lyass O, Henderson R, Berry G, Gabizon A. Pegylated liposomal doxorubicin (doxil): reduced clinical cardiotoxicity in patients reaching or exceeding cumulative doses of 500 mg/m2. Ann Oncol. 2000;11:1029–33.
Yardley DA. Nab-Paclitaxel mechanisms of action and delivery. J Control Release. 2013;170:365–72.
Duvic M, Talpur R. Optimizing denileukin diftitox (Ontak) therapy. Future Oncol. 2008;4:457–69.
Rivera Gil P, Huhn D, del Mercato LL, Sasse D, Parak WJ. Nanopharmacy: Inorganic nanoscale devices as vectors and active compounds. Pharmacol Res. 2010;62:115–25.
Chen JS, Lan K, Hung MC. Strategies to target HER2/neu overexpression for cancer therapy. Drug Resist Updat. 2003;6:129–36.
Trivedi S, Concha-Benavente F, Srivastava RM, Jie HB, Gibson SP, Schmitt NC, Ferris RL. Immune biomarkers of anti-EGFR monoclonal antibody therapy. Ann Oncol. 2015;26:40–7.
Anderson NR, Minutolo NG, Gill S, Klichinsky M. Macrophage-based approaches for cancer immunotherapy. Cancer Res. 2021;81:1201–8.
Sterner RC, Sterner RM. CAR-T cell therapy: current limitations and potential strategies. Blood Cancer J. 2021;11:69.
Basar R, Daher M, Rezvani K. Next-generation cell therapies: the emerging role of CAR-NK cells. Blood Adv. 2020;4:5868–76.
Jiang X, Xu J, Liu M, Xing H, Wang Z, Huang L, Mellor AL, Wang W, Wu S. Adoptive CD8(+) T cell therapy against cancer: challenges and opportunities. Cancer Lett. 2019;462:23–32.
Han Y, Liu D, Li L. PD-1/PD-L1 pathway: current researches in cancer. Am J Cancer Res. 2020;10:727–42.
Yi M, Zheng X, Niu M, Zhu S, Ge H, Wu K. Combination strategies with PD-1/PD-L1 blockade: current advances and future directions. Mol Cancer. 2022;21:28.
Logtenberg MEW, Scheeren FA, Schumacher TN. The CD47-SIRPalpha immune checkpoint. Immunity. 2020;52:742–52.
Veillette A, Chen J. SIRPalpha-CD47 immune checkpoint blockade in anticancer therapy. Trends Immunol. 2018;39:173–84.
Sanmamed MF, Chen L. A paradigm shift in cancer immunotherapy: from enhancement to normalization. Cell. 2018;175:313–26.
Bangham AD, Standish MM, Watkins JC. Diffusion of univalent ions across the lamellae of swollen phospholipids. J Mol Biol. 1965;13:238–52.
Yuba E. Liposome-based immunity-inducing systems for cancer immunotherapy. Mol Immunol. 2018;98:8–12.
Zahednezhad F, Saadat M, Valizadeh H, Zakeri-Milani P, Baradaran B. Liposome and immune system interplay: challenges and potentials. J Control Release. 2019;305:194–209.
Lian S, Xie R, Ye Y, Xie X, Li S, Lu Y, Li B, Cheng Y, Katanaev VL, Jia L. Simultaneous blocking of CD47 and PD-L1 increases innate and adaptive cancer immune responses and cytokine release. EBioMedicine. 2019;42:281–95.
Chen B, Gao A, Tu B, Wang Y, Yu X, Wang Y, Xiu Y, Wang B, Wan Y, Huang Y. Metabolic modulation via mTOR pathway and anti-angiogenesis remodels tumor microenvironment using PD-L1-targeting codelivery. Biomaterials. 2020;255: 120187.
Kroemer G, Galluzzi L, Kepp O, Zitvogel L. Immunogenic cell death in cancer therapy. Annu Rev Immunol. 2013;31:51–72.
Tu K, Yu Y, Wang Y, Yang T, Hu Q, Qin X, Tu J, Yang C, Kong L, Zhang Z. Combination of Chidamide-Mediated epigenetic modulation with immunotherapy: boosting tumor immunogenicity and response to PD-1/PD-L1 blockade. ACS Appl Mater Interfaces. 2021;13:39003–17.
Hundal RS, Krssak M, Dufour S, Laurent D, Lebon V, Chandramouli V, Inzucchi SE, Schumann WC, Petersen KF, Landau BR, Shulman GI. Mechanism by which metformin reduces glucose production in type 2 diabetes. Diabetes. 2000;49:2063–9.
Inzucchi SE, Lipska KJ, Mayo H, Bailey CJ, McGuire DK. Metformin in patients with type 2 diabetes and kidney disease: a systematic review. JAMA. 2014;312:2668–75.
Cha JH, Yang WH, Xia W, Wei Y, Chan LC, Lim SO, Li CW, Kim T, Chang SS, Lee HH, et al. Metformin promotes antitumor immunity via endoplasmic-reticulum-associated degradation of PD-L1. Mol Cell. 2018;71(606–620): e607.
Xiong W, Qi L, Jiang N, Zhao Q, Chen L, Jiang X, Li Y, Zhou Z, Shen J. Metformin liposome-mediated PD-L1 downregulation for amplifying the photodynamic immunotherapy efficacy. ACS Appl Mater Interfaces. 2021;13:8026–41.
Safari E, Ghorghanlu S, Ahmadi-Khiavi H, Mehranfar S, Rezaei R, Motallebnezhad M. Myeloid-derived suppressor cells and tumor: Current knowledge and future perspectives. J Cell Physiol. 2019;234:9966–81.
Barenholz Y. Doxil(R)–the first FDA-approved nano-drug: lessons learned. J Control Release. 2012;160:117–34.
Wibroe PP, Ahmadvand D, Oghabian MA, Yaghmur A, Moghimi SM. An integrated assessment of morphology, size, and complement activation of the PEGylated liposomal doxorubicin products Doxil(R), Caelyx(R), DOXOrubicin, and SinaDoxosome. J Control Release. 2016;221:1–8.
Alizadeh D, Trad M, Hanke NT, Larmonier CB, Janikashvili N, Bonnotte B, Katsanis E, Larmonier N. Doxorubicin eliminates myeloid-derived suppressor cells and enhances the efficacy of adoptive T-cell transfer in breast cancer. Cancer Res. 2014;74:104–18.
Navashenaq JG, Zamani P, Nikpoor AR, Tavakkol-Afshari J, Jaafari MR. Doxil chemotherapy plus liposomal P5 immunotherapy decreased myeloid-derived suppressor cells in murine model of breast cancer. Nanomedicine. 2020;24: 102150.
Stout DL, Becker FF. Heme enzyme patterns in genetically and chemically induced mouse liver tumors. Cancer Res. 1986;46:2756–9.
Mellor AL, Lemos H, Huang L. Indoleamine 2,3-dioxygenase and tolerance: Where are we now? Front Immunol. 2017;8:1360.
Asghar K, Farooq A, Zulfiqar B, Loya A. Review of 10 years of research on breast cancer patients: focus on indoleamine 2,3-dioxygenase. World J Clin Oncol. 2021;12:429–36.
Tang K, Wu YH, Song Y, Yu B. Indoleamine 2,3-dioxygenase 1 (IDO1) inhibitors in clinical trials for cancer immunotherapy. J Hematol Oncol. 2021;14:68.
Awuah SG, Zheng YR, Bruno PM, Hemann MT, Lippard SJ. A Pt(IV) Pro-drug Preferentially Targets Indoleamine-2,3-dioxygenase, providing enhanced ovarian cancer immuno-chemotherapy. J Am Chem Soc. 2015;137:14854–7.
Li J, Cui D, Huang J, He S, Yang Z, Zhang Y, Luo Y, Pu K. Organic semiconducting pro-nanostimulants for near-infrared photoactivatable cancer immunotherapy. Angew Chem Int Ed Engl. 2019;58:12680–7.
Kannan S, Shaik Syed Ali P, Sheeza A, Hemalatha K. COVID-19 (Novel Coronavirus 2019)-recent trends. Eur Rev Med Pharmacol Sci. 2020;24:2006–11.
Munster VJ, Koopmans M, van Doremalen N, van Riel D, de Wit E. A novel coronavirus emerging in China-key questions for impact assessment. N Engl J Med. 2020;382:692–4.
Verbeke R, Lentacker I, De Smedt SC, Dewitte H. The dawn of mRNA vaccines: the COVID-19 case. J Control Release. 2021;333:511–20.
Miao L, Zhang Y, Huang L. mRNA vaccine for cancer immunotherapy. Mol Cancer. 2021;20:41.
Mai Y, Guo J, Zhao Y, Ma S, Hou Y, Yang J. Intranasal delivery of cationic liposome-protamine complex mRNA vaccine elicits effective anti-tumor immunity. Cell Immunol. 2020;354: 104143.
Wang J, Zhu M, Nie G. Biomembrane-based nanostructures for cancer targeting and therapy: from synthetic liposomes to natural biomembranes and membrane-vesicles. Adv Drug Deliv Rev. 2021;178: 113974.
Evangelopoulos M, Parodi A, Martinez JO, Yazdi IK, Cevenini A, van de Ven AL, Quattrocchi N, Boada C, Taghipour N, Corbo C, et al. Cell source determines the immunological impact of biomimetic nanoparticles. Biomaterials. 2016;82:168–77.
Rao L, Bu LL, Ma L, Wang W, Liu H, Wan D, Liu JF, Li A, Guo SS, Zhang L, et al. Platelet-facilitated photothermal therapy of head and neck squamous cell carcinoma. Angew Chem Int Ed Engl. 2018;57:986–91.
Cheung AS, Koshy ST, Stafford AG, Bastings MM, Mooney DJ. Adjuvant-loaded subcellular vesicles derived from disrupted cancer cells for cancer vaccination. Small. 2016;12:2321–33.
Fang RH, Hu CM, Luk BT, Gao W, Copp JA, Tai Y, O’Connor DE, Zhang L. Cancer cell membrane-coated nanoparticles for anticancer vaccination and drug delivery. Nano Lett. 2014;14:2181–8.
Fang RH, Kroll AV, Zhang L. Nanoparticle-based manipulation of antigen-presenting cells for cancer immunotherapy. Small. 2015;11:5483–96.
Guo Y, Wang Z, Shi X, Shen M. Engineered cancer cell membranes: an emerging agent for efficient cancer theranostics. 2022; 2: 20210171.
Pack CD, Bommireddy R, Munoz LE, Patel JM, Bozeman EN, Dey P, Radhakrishnan V, Vartabedian VF, Venkat K, Ramachandiran S, et al. Tumor membrane-based vaccine immunotherapy in combination with anti-CTLA-4 antibody confers protection against immune checkpoint resistant murine triple-negative breast cancer. Hum Vaccin Immunother. 2020;16:3184–93.
Liu B, Yang Y, Chao Y, Xiao Z, Xu J, Wang C, Dong Z, Hou L, Li Q, Liu Z. Equipping Cancer cell membrane vesicles with functional DNA as a targeted vaccine for cancer immunotherapy. Nano Lett. 2021;21:9410–8.
Fontana F, Shahbazi MA, Liu D, Zhang H, Makila E, Salonen J, Hirvonen JT, Santos HA. Multistaged Nanovaccines Based on Porous Silicon@Acetalated Dextran@Cancer Cell Membrane for Cancer Immunotherapy. Adv Mater. 2017;29:1603239.
Liu WL, Zou MZ, Liu T, Zeng JY, Li X, Yu WY, Li CX, Ye JJ, Song W, Feng J, Zhang XZ. Cytomembrane nanovaccines show therapeutic effects by mimicking tumor cells and antigen presenting cells. Nat Commun. 2019;10:3199.
Jiang Y, Krishnan N, Zhou J, Chekuri S, Wei X, Kroll AV, Yu CL, Duan Y, Gao W, Fang RH, Zhang L. Engineered Cell-Membrane-Coated Nanoparticles Directly Present Tumor Antigens to Promote Anticancer Immunity. Adv Mater. 2020;32: e2001808.
Meng QF, Zhao Y, Dong C, Liu L, Pan Y, Lai J, Liu Z, Yu GT, Chen X, Rao L. Genetically programmable fusion cellular vesicles for cancer immunotherapy. Angew Chem Int Ed Engl. 2021;60:26320–6.
Li L, Miao Q, Meng F, Li B, Xue T, Fang T, Zhang Z, Zhang J, Ye X, Kang Y, et al. Genetic engineering cellular vesicles expressing CD64 as checkpoint antibody carrier for cancer immunotherapy. Theranostics. 2021;11:6033–43.
Zhang X, Wang C, Wang J, Hu Q, Langworthy B, Ye Y, Sun W, Lin J, Wang T, Fine J, et al. PD-1 Blockade cellular vesicles for cancer immunotherapy. Adv Mater. 2018;30: e1707112.
Rao L, Wu L, Liu Z, Tian R, Yu G, Zhou Z, Yang K, Xiong HG, Zhang A, Yu GT, et al. Hybrid cellular membrane nanovesicles amplify macrophage immune responses against cancer recurrence and metastasis. Nat Commun. 2020;11:4909.
Deng G, Sun Z, Li S, Peng X, Li W, Zhou L, Ma Y, Gong P, Cai L. Cell-membrane immunotherapy based on natural killer cell membrane coated nanoparticles for the effective inhibition of primary and abscopal tumor growth. ACS Nano. 2018;12:12096–108.
Li M, Zhou H, Yang C, Wu Y, Zhou X, Liu H, Wang Y. Bacterial outer membrane vesicles as a platform for biomedical applications: an update. J Control Release. 2020;323:253–68.
Huang Y, Nieh MP, Chen W, Lei Y. Outer membrane vesicles (OMVs) enabled bio-applications: a critical review. Biotechnol Bioeng. 2022;119:34–47.
Pawelek JM, Low KB, Bermudes D. Tumor-targeted Salmonella as a novel anticancer vector. Cancer Res. 1997;57:4537–44.
Bruun TUJ, Andersson AC, Draper SJ, Howarth M. Engineering a Rugged Nanoscaffold to enhance plug-and-display vaccination. ACS Nano. 2018;12:8855–66.
Zakeri B, Fierer JO, Celik E, Chittock EC, Schwfarz-Linek U, Moy VT, Howarth M. Peptide tag forming a rapid covalent bond to a protein, through engineering a bacterial adhesin. Proc Natl Acad Sci U S A. 2012;109:E690-697.
Veggiani G, Nakamura T, Brenner MD, Gayet RV, Yan J, Robinson CV, Howarth M. Programmable polyproteams built using twin peptide superglues. Proc Natl Acad Sci USA. 2016;113:1202–7.
Cheng K, Zhao R, Li Y, Qi Y, Wang Y, Zhang Y, Qin H, Qin Y, Chen L, Li C, et al. Bioengineered bacteria-derived outer membrane vesicles as a versatile antigen display platform for tumor vaccination via Plug-and-Display technology. Nat Commun. 2021;12:2041.
Huang W, Shu C, Hua L, Zhao Y, Xie H, Qi J, Gao F, Gao R, Chen Y, Zhang Q, et al. Modified bacterial outer membrane vesicles induce autoantibodies for tumor therapy. Acta Biomater. 2020;108:300–12.
Li M, Li S, Zhou H, Tang X, Wu Y, Jiang W, Tian Z, Zhou X, Yang X, Wang Y. Chemotaxis-driven delivery of nano-pathogenoids for complete eradication of tumors post-phototherapy. Nat Commun. 2020;11:1126.
Qing S, Lyu C, Zhu L, Pan C, Wang S, Li F, Wang J, Yue H, Gao X, Jia R, et al. Biomineralized bacterial outer membrane vesicles potentiate safe and efficient tumor microenvironment reprogramming for anticancer Therapy. Adv Mater. 2020;32: e2002085.
Trams EG, Lauter CJ, Salem N Jr, Heine U. Exfoliation of membrane ecto-enzymes in the form of micro-vesicles. Biochim Biophys Acta. 1981;645:63–70.
Caby MP, Lankar D, Vincendeau-Scherrer C, Raposo G, Bonnerot C. Exosomal-like vesicles are present in human blood plasma. Int Immunol. 2005;17:879–87.
Pisitkun T, Shen RF, Knepper MA. Identification and proteomic profiling of exosomes in human urine. Proc Natl Acad Sci USA. 2004;101:13368–73.
Mehanny M, Lehr CM, Fuhrmann G. Extracellular vesicles as antigen carriers for novel vaccination avenues. Adv Drug Deliv Rev. 2021;173:164–80.
Yildirim M, Yildirim TC, Turay N, Bildik T, Ibibik B, Evcili I, Ersan PG, Tokat UM, Sahin O, Gursel I. TLR ligand loaded exosome mediated immunotherapy of established mammary Tumor in mice. Immunol Lett. 2021;239:32–41.
Taghikhani A, Hassan ZM, Ebrahimi M, Moazzeni SM. microRNA modified tumor-derived exosomes as novel tools for maturation of dendritic cells. J Cell Physiol. 2019;234:9417–27.
Khani AT, Sharifzad F, Mardpour S, Hassan ZM, Ebrahimi M. Tumor extracellular vesicles loaded with exogenous Let-7i and miR-142 can modulate both immune response and tumor microenvironment to initiate a powerful anti-tumor response. Cancer Lett. 2021;501:200–9.
Fernandez-Delgado I, Calzada-Fraile D, Sanchez-Madrid F. Immune regulation by dendritic cell extracellular vesicles in cancer immunotherapy and vaccines. Cancers. 2020;12:3558.
Matsumoto A, Asuka M, Takahashi Y, Takakura Y. Antitumor immunity by small extracellular vesicles collected from activated dendritic cells through effective induction of cellular and humoral immune responses. Biomaterials. 2020;252:120112.
Seo N, Akiyoshi K, Shiku H. Exosome-mediated regulation of tumor immunology. Cancer Sci. 2018;109:2998–3004.
Quah BJ, O’Neill HC. Maturation of function in dendritic cells for tolerance and immunity. J Cell Mol Med. 2005;9:643–54.
Pitt JM, Andre F, Amigorena S, Soria JC, Eggermont A, Kroemer G, Zitvogel L. Dendritic cell-derived exosomes for cancer therapy. J Clin Invest. 2016;126:1224–32.
Ding J, Lu G, Nie W, Huang LL, Zhang Y, Fan W, Wu G, Liu H, Xie HY. Self-activatable photo-extracellular vesicle for synergistic trimodal anticancer therapy. Adv Mater. 2021;33: e2005562.
Rosenberg SA, Restifo NP. Adoptive cell transfer as personalized immunotherapy for human cancer. Science. 2015;348:62–8.
Lee DW, Gardner R, Porter DL, Louis CU, Ahmed N, Jensen M, Grupp SA, Mackall CL. Current concepts in the diagnosis and management of cytokine release syndrome. Blood. 2014;124:188–95.
Fu W, Lei C, Liu S, Cui Y, Wang C, Qian K, Li T, Shen Y, Fan X, Lin F, et al. CAR exosomes derived from effector CAR-T cells have potent antitumour effects and low toxicity. Nat Commun. 2019;10:4355.
Zhou C, Qian W, Li J, Ma J, Chen X, Jiang Z, Cheng L, Duan W, Wang Z, Wu Z, et al. High glucose microenvironment accelerates tumor growth via SREBP1-autophagy axis in pancreatic cancer. J Exp Clin Cancer Res. 2019;38:302.
He Y, Chen D, Yang L, Hou Q, Ma H, Xu X. The therapeutic potential of bone marrow mesenchymal stem cells in premature ovarian failure. Stem Cell Res Ther. 2018;9:263.
Zhou W, Zhou Y, Chen X, Ning T, Chen H, Guo Q, Zhang Y, Liu P, Zhang Y, Li C, et al. Pancreatic cancer-targeting exosomes for enhancing immunotherapy and reprogramming tumor microenvironment. Biomaterials. 2021;268: 120546.
Yong T, Li X, Wei Z, Gan L, Yang X. Extracellular vesicles-based drug delivery systems for cancer immunotherapy. J Control Release. 2020;328:562–74.
Liu G, Zhao X, Zhang Y, Xu J, Xu J, Li Y, Min H, Shi J, Zhao Y, Wei J, et al. Engineering biomimetic platesomes for pH-responsive drug delivery and enhanced antitumor activity. Adv Mater. 2019;31: e1900795.
Zhai Y, Ma Y, Pang B, Zhang J, Li Y, Rui Y, Xu T, Zhao Y, Qian Z, Gu Y, Li S. A cascade targeting strategy based on modified bacterial vesicles for enhancing cancer immunotherapy. J Nanobiotechnology. 2021;19:434.
Wang D, Liu C, You S, Zhang K, Li M, Cao Y, Wang C, Dong H, Zhang X. Bacterial vesicle-cancer cell hybrid membrane-coated nanoparticles for tumor specific immune activation and photothermal therapy. ACS Appl Mater Interfaces. 2020;12:41138–47.
Chen Q, Huang G, Wu W, Wang J, Hu J, Mao J, Chu PK, Bai H, Tang G. A hybrid eukaryotic-prokaryotic nanoplatform with photothermal modality for enhanced antitumor vaccination. Adv Mater. 2020;32: e1908185.
Zou MZ, Li ZH, Bai XF, Liu CJ, Zhang XZ. Hybrid vesicles based on autologous tumor cell membrane and bacterial outer membrane to enhance innate immune response and personalized tumor immunotherapy. Nano Lett. 2021;21:8609–18.
Kooijmans SAA, Vader P, Schiffelers RM. Tumour-bound RNA-laden exosomes. Nat Biomed Eng. 2017;1:634–6.
De La Pena H, Madrigal JA, Rusakiewicz S, Bencsik M, Cave GW, Selman A, Rees RC, Travers PJ, Dodi IA. Artificial exosomes as tools for basic and clinical immunology. J Immunol Methods. 2009;344:121–32.
Cheng L, Zhang X, Tang J, Lv Q, Liu J. Gene-engineered exosomes-thermosensitive liposomes hybrid nanovesicles by the blockade of CD47 signal for combined photothermal therapy and cancer immunotherapy. Biomaterials. 2021;275: 120964.
Robert C, Long GV, Brady B, Dutriaux C, Maio M, Mortier L, Hassel JC, Rutkowski P, McNeil C, Kalinka-Warzocha E, et al. Nivolumab in previously untreated melanoma without BRAF mutation. N Engl J Med. 2015;372:320–30.
Robert C, Schachter J, Long GV, Arance A, Grob JJ, Mortier L, Daud A, Carlino MS, McNeil C, Lotem M, et al. Pembrolizumab versus Ipilimumab in advanced melanoma. N Engl J Med. 2015;372:2521–32.
Xing H, Hwang K, Lu Y. Recent developments of liposomes as nanocarriers for theranostic applications. Theranostics. 2016;6:1336–52.
Chen G, Huang AC, Zhang W, Zhang G, Wu M, Xu W, Yu Z, Yang J, Wang B, Sun H, et al. Exosomal PD-L1 contributes to immunosuppression and is associated with anti-PD-1 response. Nature. 2018;560:382–6.
Acknowledgements
Not applicable.
Funding
We are grateful for the support by the high-level talents (333 Project) of Jiangsu Province (BRA2019024); the Key Project Foundation of Jiangsu Health and Health Committee (H2018114); the Social Development Project of the Key Research and Development Plan of Jiangsu Province (BE2018606); the China Postdoctoral Science Foundation Funded Project (2018M630605).
Author information
Authors and Affiliations
Contributions
YND, WPY, QST proposed the project; All the authors carried out reference searching; YND, LHW, HL wrote the manuscript; WPY, GLS, QST made review and final editing. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
We have included 39 figures and 1 table from previously published literature with required copyright permission. We have mentioned this in the manuscript with proper citation.
Competing interests
The authors have declared that no competing interest exists.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Ding, Y., Wang, L., Li, H. et al. Application of lipid nanovesicle drug delivery system in cancer immunotherapy. J Nanobiotechnol 20, 214 (2022). https://doi.org/10.1186/s12951-022-01429-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12951-022-01429-2