Abstract
Background
Determining the mental capacity of psychiatric patients for making healthcare related decisions is crucial in clinical practice. This meta-review of review articles comprehensively examines the current evidence on the capacity of patients with a mental illness to make medical care decisions.
Methods
Systematic review of review articles following PRISMA recommendations. PubMed, Scopus, CINAHL and PsycInfo were electronically searched up to 31 January 2020. Free text searches and medical subject headings were combined to identify literature reviews and meta-analyses published in English, and summarising studies on the capacity of patients with serious mental illnesses to make healthcare and treatment related decisions, conducted in any clinical setting and with a quantitative synthesis of results. Publications were selected as per inclusion and exclusion criteria. The AMSTAR II tool was used to assess the quality of reviews.
Results
Eleven publications were reviewed. Variability on methods across studies makes it difficult to precisely estimate the prevalence of decision-making capacity in patients with mental disorders. Nonetheless, up to three-quarters of psychiatric patients, including individuals with serious illnesses such as schizophrenia or bipolar disorder may have capacity to make medical decisions in the context of their illness. Most evidence comes from studies conducted in the hospital setting; much less information exists on the healthcare decision making capacity of mental disorder patients while in the community. Stable psychiatric and non-psychiatric patients may have a similar capacity to make healthcare related decisions. Patients with a mental illness have capacity to judge risk-reward situations and to adequately decide about the important treatment outcomes. Different symptoms may impair different domains of the decisional capacity of psychotic patients. Decisional capacity impairments in psychotic patients are temporal, identifiable, and responsive to interventions directed towards simplifying information, encouraging training and shared decision making. The publications complied satisfactorily with the AMSTAR II critical domains.
Conclusions
Whilst impairments in decision-making capacity may exist, most patients with a severe mental disorder, such as schizophrenia or bipolar disorder are able to make rational decisions about their healthcare. Best practice strategies should incorporate interventions to help mentally ill patients grow into the voluntary and safe use of medications.
Similar content being viewed by others
Background
In 1995, Appelbaum and Grisso stated that competence to consent to treatment relied on four legal standards: the ability to communicate a choice; the ability to understand relevant information; the ability to appreciate the situation and its likely consequences; and the ability to manipulate information rationally [1]. In healthcare, the capacity to make decisions regarding treatment is closely related to the autonomy, the exercise of self-governance, and the ability of an individual to take intentional actions [2]. The capacity to consent to treatment is often used in the clinical assessment of the ability to engage in authentic autonomous decision-making, a fundamental element of a person’s dignity and rights [3].
Assessment of mental capacity has become a key component of daily clinical practice [4, 5]. Mental health legislation and medical ethics increasingly require physicians to empower patients to make decisions, and to respect the patient’s wishes with regard to accepting or refusing therapy [4, 6]. However, it has been reported that coercive treatment, involuntary hospitalisations and medications are currently overused [7]; this has a direct negative impact on patients’ adherence to treatment and on their engagement and participation in shared decision-making with their healthcare professionals [8].
An increasing number of publications are assessing decision-making capacity in mental health. However, comparisons and contrasts of the findings of these articles are lacking and it becomes difficult to draw clear conclusions on what is the actual capacity of individuals with serious mental illnesses to make decisions about their healthcare and treatments [9]. This meta-review of review articles was designed as a comprehensive synthesis of the current state of knowledge in the field, with the aim of assessing the available evidence on the decision-making capacity of patients with various mental illnesses (especially schizophrenia, psychosis and bipolar disorder) with regard to the management of their disease and their treatment. The review compares the conclusions of various comprehensive publications, discusses the strength of these conclusions, and identifies existing gaps in the evidence.
Methods
The review of the literature was conducted in accordance with the Preferred Reporting Items for Systematic Review and Meta-Analysis (PRISMA) guidelines [10]. A series of steps, including the definition of the search strategy, identification and selection of publications, data extraction and synthesis, and quality assessment was followed.
Search strategy for identification and selection of publications
The aim of the search strategy was to provide a comprehensive list of published literature reviews assessing decision making capacity in patients with mental disorders. Four electronic databases (the Cumulative Index to Nursing and Allied Health Literature [CINAHL], PsycInfo, PubMed and Scopus) were searched up to 31 January 2020. The search strategy is described in Additional file 1. Free text searches and medical subject headings were combined to identify literature reviews published in English, summarising studies conducted in any clinical setting and with a quantitative synthesis of results. Selection of publications was carried out as per inclusion and exclusion criteria (Table 1). Lists of references in the key papers retrieved were further checked to identify other relevant articles.
Potentially relevant abstracts were assessed by two expert reviewers to identify all papers suitable for inclusion. Full text copies were requested. Reviews which were identified after mutual agreement were included and data were extracted. A third reviewer was involved in the process to resolve any disagreements on the selection of publications.
Data extraction and quality assessment
Data extraction was carried out by one researcher. A data extraction form that covered citation, country, population, interventions, comparators, outcomes, settings, review type, aims, literature review size, strengths and limitations and key findings of the review as stated by authors was used to extract data (Tables 2 and 3). The AMSTAR II (A MeaSurement Tool to Assess systematic Reviews) [22] assessment tool was used to assess the quality of reviews.
Results
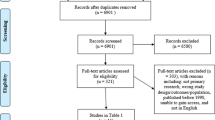
A total of 1973 hits were initially identified; 1938 were either duplicated or deemed not relevant for the review based on the assessment of titles and abstracts; 22 full text publications were initially considered valid and retrieved for closer examination; 11 were excluded because they referred to diseases excluded from the review or did not assess decision making capacity. Data was finally extracted from 11 publications (Fig. 1).
The number of studies included in each review apprised varied between 7 [18, 20] and 63 [16], and the number of patients with a mental disorder ranged from 6 [13] to 2483 [15]. Schizophrenia or schizoaffective disorders [12, 13, 19, 20] and psychosis [14, 18, 21] were the most frequently explored mental illnesses. The general healthy population or patients with a non-mental disorder were the usual study comparators. Therefore, decisional capacity variance among mental illnesses of different nature has been little explored (Tables 2 and 3).
Prevalence of decision-making capacity
Information on the prevalence of capacity for making healthcare decisions among psychiatry patients can be derived from two systematic reviews. One systematic review of 37 empirical, quantitative studies of mental capacity in a mixed population of psychiatric patients reported that up to 67% of participants had the capacity to decide whether to be admitted to a psychiatric unit while a median of 71% had capacity for making treatment decisions (a median of 29%, interquartile range (IQR) 22–44, lacked capacity) [17]. Another systematic review (40 articles) found that 26% (95% confidence interval (CI): 18 to 36) to 67% (95% CI: 35 to 88) of people with schizophrenia or other non-affective disorders were able to make medical decisions related or unrelated to the management of their condition [(median: 48% (95% CI: 29 to 66)] [19]. In both reviews, up to three quarters of severe mental disorder patients, including individuals with schizophrenia would have capacity to make medical decisions in the context of their illness, in particular specific decisions related with their treatments [17, 19]. Both reviews are also coincident in that heterogeneity between studies was high, with considerable variation in study design and measurements [17, 19].
Decisional capacity in different clinical settings and patient groups
Four reviews assessed patients in diverse settings and explored the degree of impairment in each dimension of decision-making capacity. Lepping et al. [15] reported that 55% of patients in psychiatric and 66% of patients in non-psychiatric settings had the capacity to make medical decisions. Appreciation of the problem and necessity for treatment were more frequently compromised in psychiatric patients, while non-psychiatric patients struggled primarily with reasoning. The authors found a significant variation between studies due to heterogeneity in designs and methods that reached 86% in psychiatric settings and 90% in non-psychiatric settings. Jeste et al. [13] reported a 48 to 79% overlap between people with schizophrenia and non-psychiatric patients on the MacArthur subscales, which indicated that most patients with schizophrenia had comparably adequate decision-making capacity [13]. Psychotic inpatients had several characteristics which temporarily limited their capacity and distinguished them from outpatients. Greater severity of positive and negative symptoms, experiencing a stressful life event (e.g., hospitalisation), and often receiving higher doses of medication adversely impacted cognition among psychiatric inpatients [15]. Community-dwelling or clinically stable outpatients were much closer to non-psychiatric subjects in terms of the capacity for decision-making. The authors concluded that similar proportions of non-psychiatric and psychiatric outpatients either had or lacked capacity to consent to treatment or to hospital admission, and that impairment in the capacity to make decisions was not a distinguishing feature of schizophrenia patients [13, 15].
Another meta-analysis of ten studies showed that compared to healthy controls, patients with schizophrenia or schizoaffective disorder were significantly more likely to have impaired decision-making capacity in terms of understanding, reasoning, appreciation and expression of a choice in clinical research and treatment, as measured by the MacArthur Competence Assessment Tool (MacCAT) instruments [20]. The standardised mean differences were more significant in older than in younger age subgroups, suggesting that, compared to their healthy counterparts, the impairment of decision-making capacity could be more obvious in older patients than in younger patients. In some of the studies included in this meta-analysis, decisional capacity improved in patients with schizophrenia following intensive educational interventions.
Another systematic review explored the degree of impairment in each dimension of decision-making capacity in schizophrenia patients compared to non-psychiatric controls, as assessed by the MacCAT [12]. The odds for a decreased understanding and a decreased appreciation were some five times higher in individuals with schizophrenia than in non-mentally ill controls, those for decreased reasoning almost four times higher, and those for a decreased aptitude to express a choice was over six times higher. The use of an enhanced informed consent form contributed to significant improvements in decision-making capacity compared to the use of standard forms. The authors concluded that even if patients with schizophrenia have a significantly decreased decision-making capacity, they should be considered to be as competent as non-mentally ill controls unless very severe changes were identifiable during the clinical examination [12].
In these four systematic reviews, the decisional capacity of patients with a psychiatric disease was compared with that of patients with a non-psychiatric clinical condition or with that of healthy individuals. All reviews are concurrent in the fact that impairments in decisional capacity can be found in both psychiatric and non-psychiatric patients, and therefore the diagnosis of a psychiatric condition should not be the upfront reason of incapacity. Despite most research being conducted in the hospital setting, those fewer addressing decisional capacity in psychiatric outpatients showed that their capacity to make medical decisions can be much alike to that of the non-psychiatric individuals. Likewise, studies coincidently acknowledge that decisional impairments amongst psychiatric inpatients are temporal and responsive to information-enhancing interventions.
Determining factors of decisional capacity in psychosis patients
In a systematic review and meta-analysis of factors that help or hinder treatment decision-making capacity in psychosis (23 studies, n = 1823) a moderate to large negative association between total psychotic symptom severity and the capacity of participants to understand information relevant to treatment decisions was found [14]. Poor insight was also associated with patients’ poor capacity to make treatment related decisions. Verbal cognitive function, metacognitive ability and years spent in education were positively associated with the ability of psychiatric individuals to understand information relating to treatment decision making. Decision-making capacity responded favourably to interventions, such as the simplification of the information, shared decision-making, and metacognitive training [14].
Likewise, Ruissen et al. [18] reported the findings of seven articles that assessed the relationship between competence to decide and insight of psychiatric inpatients and outpatients and of psychotic and non-psychotic patients. A large overlap between insight and competence to decide was reported among psychotic (schizophrenia, schizoaffective disorder, and psychotic episodes) and bipolar disorder (comprising both manic and depressive episodes) patients implying that a strong correlation existed between insight and capacity for making decisions, including decisions related to medical treatments and hospital admission. Psychotic patients with adequate insight were generally competent in making medical decisions.
Both reviews report findings on the capacity of psychotic patients to make treatment and other disease-related decisions. They are coincident in the relevance of insight as a determining factor of psychiatric patients’ decisional capacity. As expected, the burden and severity of psychotic symptoms can seriously compromise patients’ ability to make decisions.
Capacity of people with mental illness to make risk-reward decisions and to choose treatments
The capacity of mental illness patients for making value-based decisions was explored in literature reviews of studies based on gambling tasks and on preferences for medication-associated outcomes methods. A systematic review and meta-analysis explored the factors which may help or hinder the ability to make risk-reward decision making in a pooled sample of 4264 individuals with psychosis, based on their performance on the Iowa Gambling Tasks (IGT) and the Cambridge Gambling Tasks (CGT) [21, 23, 24]. Compared with healthy individuals, people with psychosis had moderately impaired risk-reward decision-making ability (g = − 0.57, 95% CI − 0.66 to − 0.48; I2 45%; moderate quality) [21]. They were also more likely to value rewards over losses (k = 6, N = 516, g = 0.38, 95% CI: 0.05 to 0.70, I2 64%), and to base decisions on recent rather than past outcomes (k = 6, N = 516, g = 0.30, 95% CI: − 0.04 to 0.65, I2 68%). Analysis of the positive or negative influence of the type and dose of antipsychotics on decision-making capacity was inconclusive. The authors suggested that, although people with non-affective psychosis may make less effective decisions than healthy individuals in the IGT and CGT, their difficulties were moderate and comparable with those observed in other clinical groups.
Mukherjee and Kable [16] calculated that around 27% of patients with various mental disorders were similar to healthy individuals when deciding about losses and rewards on the IGT. Furthermore, individuals with mental illnesses had fewer deficits than individuals with frontal lobe lesions, for instance. The assessment of the severity of impairment across types of mental illnesses did not demonstrate any significant differences according to specific psychiatric diagnosis.
Eiring et al. [11] investigated the relative value adults with a mental illness place on treatment outcomes, including the attributes of particular medications or medication classes and the consequences and health states associated with their use. It reported that patients were able to provide valid preference measures with the different methods applied, generally understood the tasks, and gave sufficiently consistent answers. Among patients with schizophrenia, positive, acute or psychotic symptoms appeared consistently among the least desirable outcomes. Negative symptoms, such as reduced capacity for emotion, were found more desirable or less important than positive symptoms. Independence received high ratings and inpatient status low ratings. Overall, patients with schizophrenia tended to value disease states higher and side effects lower than other groups and perceived side effects more negatively than their therapists. Patients with bipolar disorder gave low values to mania and severe depression and reported weight gain to be important.
These reviews provide consistent evidence on the fact that patients with a serious mental disease, such as schizophrenia or bipolar disorder can make risk-reward decisions in the context of their illness and treatments. Furthermore, the studies summarised in the reviews show that these patients may achieve a level of ability for making value-based decisions equal to non-psychiatric patients. They can reliably decide about the important treatment outcomes and their most desirable treatment attributes.
Quality assessment
Reviews presented well-framed research questions based on the evidence based PICOS model [25] (Table 2) and were high quality according to the AMSTAR II assessment tool (Table 3) [22]. AMSTAR II was developed to evaluate systematic reviews of randomised trials or non-randomised studies of healthcare interventions, or both. Publications included in this review complied satisfactorily the AMSTAR II critical domains. No critical weaknesses were identified in the assessment. Therefore, the reviews provided an accurate and comprehensive summary of the results of studies of decision-making capacity in mental disorder patients.
Discussion
This meta-review review brings together a set of high-quality reviews on the capacity of individuals with a severe mental illness to make decisions about their healthcare. It presents a thorough synthesis of current systematic review literature concerning the decision-making capacity of patients with mental disorders, including psychotic, schizophrenia and bipolar disorder individuals. It provides a picture of the state of the field in the complex task of assessing patients’ decisional capacity in psychiatry. It comprehensively summarizes a body of evidence supporting the idea that the decision-making capacity of psychiatric patients with serious mental illness is preserved in most circumstances and challenges the understanding that people with severe mental illnesses are unable to make their own choices [8].
Authors across studies are coincident in emphasising that most patients with a severe mental disorder are able to make rational decisions about their medical care and to participate in decision-making regarding treatments despite temporal impairments. Thus, most often the degree of impairment that may be inherent to the mental disorder does not constitute incapacity to make decisions. The findings also reveal that patients with psychotic disorders or other severe mental illnesses can make complex risk-reward decisions in usual clinical practice. Small deviations from optimal performance may arise due to deficits in the ability to fully represent the value of different choices and response options, a finding that aligns with results from experimental research in patients with schizophrenia [26].
Most of the reviews addressed the capacity to make decisions in people with severe mental disorders either already hospitalised or requiring hospital admission. This means that most studies included patients with more severe symptoms less responsive to usual therapies [27]. Even in these more ill psychiatric populations, between 60 and 70% had capacity to make some treatment decisions [1, 17, 19]. Hospitalised patients usually have greater care needs, even when their psychiatric symptoms are controlled, exhibit significantly more severe negative, positive, and manic symptoms, and have lower global functioning than outpatients [28]. Therefore, despite the scarcity of studies measuring decisional capacity in routine ambulatory practice in psychiatry, it can be expected a high level of health-related decision-making capacity in patients in everyday life in the community. Rigorous studies investigating this question as a primary outcome would be much welcome.
This meta- review also shows that people with schizophrenia have the capacity to make other difficult decisions related, for instance, to giving consent for hospital admission or to the type of treatment they prefer to receive. Likewise, other studies have reported that patients with schizophrenia or bipolar disorder are able to describe prodromal symptoms of relapse and to suggest a treatment and the need for hospitalisation in advance; that they can request or refuse medications and state their preferences for pre-emergency interventions, non-hospital alternatives and non-medical personal care [29,30,31]. In such circumstances, shared decision making and advancing crisis management plans may help reduce insecurity and improve healthcare outcomes for the patient with a mental illness. Studies have found that being involved in decision-making, whenever decisional capacity exists, renders more positive treatment results, better medication adherence, higher self-efficacy and autonomy, and lower decisional uncertainty among patients with mental disorders [32, 33].
Patients’ awareness of decisional capacity and having the opportunity for sharing decisions on future care (crisis planning) for psychosis reduces the use of compulsory inpatient treatment by approximately 40% over 15 to 18 months [33]. In this context, advance directives are fundamental to ensure the timely provision of medical treatments, thus minimising decisional impairments in the acute stages of psychosis [34]. Psychosocial interventions are also important to address the complex health needs of people with serious mental illnesses. Combined with anti-psychotics, psychosocial interventions highly contribute to reduce the severity of symptoms, to benefit functioning, to encourage decision making and to decrease hospital readmissions [35].
Nevertheless, clinicians play the crucial role of judging the capacity of patients with severe mental disorder to decide about their treatments and healthcare, and tools exist to guide their assessment [36]. The final decision depends entirely on clinical judgement, based on the practitioner’s knowledge of the patient and of the course of the disease.
Beyond acute episodes, the findings also support the notion that continued training and learning, simplification and enhancement of the information improve the capacity of patients with severe mental disorders for decision-making both in hospital and in everyday life [37]. The results of various studies demonstrate that brief interventions aimed at recovering capacity for understanding can help schizophrenia patients to perform very much like healthy people in the four dimensions of decisional capacity (understanding, appreciation, reasoning and expression of a choice) [38]. Regular information reinforcement, strengthening neurocognitive functioning and training are important to maintain long-term levels of competence and to maximise decision making capacities of patients [39, 40].
In sum, people with severe mental illness can benefit greatly from anticipation, prevention, gradual learning, enhanced information and enriched shared decision-making in order to strengthen their autonomous decision-making capacity, to increase their autonomy and to ultimately contribute to reducing the stigma of mental illness. Being able to make decisions in anticipation of, for instance, agitation or other acute symptoms should help patients to gain a sense of control over their own lives, and to enhance their health-related quality of life [41]. This review contributes to the growing body of evidence suggesting that the best medical practice should help severe mentally ill patients to grow into voluntary healthcare, safe users of medications.
Small sample size, heterogeneity, language and selection bias of participants were among the limitations frequently reported by the authors of the studies reviewed. However, since the publications included in the meta- review were systematic reviews and meta-analyses, the risk of bias was minimised. Nonetheless, it was limited to publications appeared in English. Although the search was comprehensive, papers in many other languages including French, Germany. Italian or Spanish may not have been identified. Several frequent mental illnesses were excluded for reasons of study feasibility. Important mental health conditions, such as dementia, depression and other disorders have not been addressed which may have limited the scope of the meta-review.
Conclusions
This meta-review of review articles provides a comprehensive synthesis of the current state of knowledge on the capacity of patients with mental illnesses to make decisions about their healthcare and medical treatments. It provides clinicians and other healthcare practitioners a summary of the evidence on the topic, contrasting key findings. It shows that whilst impairments in decision-making capacity may exist, most patients with a severe mental disorder are able to make adequate decisions about the care of their health. It denotes that best practice strategies should help mentally ill patients to exercise their decisional capacity to develop into autonomous and reliable users of medications. Keeping a sense of control over their illness and life may help them to improve the outcomes of their treatments and their health-related quality of life.
Availability of data and materials
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- Abreviation:
-
Description
- AMSTAR:
-
A MeaSurement Tool to Assess systematic Reviews
- CGT:
-
Cambridge Gambling Tasks
- CI:
-
Confidence Interval
- CINAHL:
-
Cumulative Index to Nursing and Allied Health Literature
- IGT:
-
Iowa Gambling Tasks
- IQR:
-
InterQuartile Range
- MacCAT:
-
MacArthur Competence Assessment Tool
- MacCAT-CR:
-
MacArthur Competence Assessment Tool for Clinical Research
- MacCAT-T:
-
MacArthur Competence Assessment Tool for Treatment
- NNT:
-
Number Needed to Treat
- OR:
-
Odds Ratios
- PRISMA:
-
Preferred Reporting Items for Systematic Review and Meta-Analysis
- SD:
-
Standard Deviation
- SE:
-
Standard Error
- SMD:
-
Standardized Mean Difference
References
Appelbaum P, Grisso T. The MacArthur treatment competence study. I: mental illness and competence to consent to treatment. Law Hum Behav. 1995;19(2):105–26.
Owen GS, Freyenhagen F, Richardson G, Hotopf M. Mental capacity and decisional autonomy: an interdisciplinary challenge. Inquiry. 2009;52(1):79–107.
Jeste D, Eglit G, PPalmer B, Martinis J, Blanck P, Saks E. Supported decision making in serious mental illness. Psychiatry. 2018;81(1):28–40.
United Nations. Convention on the rights of persons with disabilities. Report of the Convention. 2006; Available from: https://www.un.org/disabilities/documents/convention/convention_accessible_pdf.pdf.
Harding R, Taşcıoğlu E. Supported decision-making from theory to practice: implementing the right to enjoy legal capacity. Societies. 2018;8(2):25.
Morrissey F. The united nations convention on the rights of persons with disabilities: a new approach to decision-making in mental health law. Eur J Health Law. 2012;19(5):423–40.
Mahomed F, Stein MA, Patel V. Involuntary mental health treatment in the era of the United Nations convention on the rights of persons with disabilities. PLoS Med. 2018;15(10):e1002679.
Danzer G, Rieger SM. Improving medication adherence for severely mentally ill adults by decreasing coercion and increasing cooperation. Bull Menn Clin. 2016;80(1):30–48.
Smith V, Devane D, Begley C, Clarke M. Methodology in conducting a systematic review of systematic reviews of healthcare interventions. BMC Med Res Methodol. 2011;11(1):15 Available from: http://www.biomedcentral.com/1471-2288/11/15.
Moher D, Liberati A, Tetzlaff J, Altman D, Group. P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097 Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2707599/pdf/pmed.1000097.pdf.
Eiring Ø, Landmark BF, Aas E, Salkeld G, Nylenna M, Nytrøen K. What matters to patients? A systematic review of preferences for medication-associated outcomes in mental disorders. BMJ Open. 2015;5(4):1–13.
Hostiuc S, Rusu MC, Negoi I, Drima E. Testing decision-making competency of schizophrenia participants in clinical trials. A meta-analysis and meta-regression. BMC Psychiatry. 2018;18(1):2.
Jeste DV, Depp CA, Palmer BW. Magnitude of impairment in decisional capacity in people with schizophrenia compared to normal subjects: an overview. Schizophr Bull. 2006;32(1):121–8.
Larkin A, Hutton P. Systematic review and meta-analysis of factors that help or hinder treatment decision-making capacity in psychosis. Br J Psychiatry. 2017;211(4):205–15.
Lepping P, Stanly T, Turner J. Systematic review on the prevalence of lack of capacity in medical and psychiatric settings. Clin Med J R Coll Physicians London. 2015;15(4):337–43.
Mukherjee D, Kable JW. Value-based decision making in mental illness: a meta-analysis. Clin Psychol Sci. 2014;2(6):767–82.
Okai D, Owen G, McGuire H, Singh S, Churchil R, Hotopf M. Mental capacity in psychiatric patients systematic review. Br J Psychiatry. 2007;191:291–7.
Ruissen AM, Widdershoven GAM, Meynen G, Abma TA, van Balkom AJLM. A systematic review of the literature about competence and poor insight. Acta Psychiatr Scand. 2012;125(2):103–13.
Spencer BWJ, Shields G, Gergel T, Hotopf M, Owen GS. Diversity or disarray? A systematic review of decision-making capacity for treatment and research in schizophrenia and other non-affective psychoses. Psychol Med. 2017;47(11):1906–22.
Bin WS, Wang YY, Ungvari GS, Ng CH, Wu RR, Wang J, et al. The MacArthur competence assessment tools for assessing decision-making capacity in schizophrenia: a meta-analysis. Schizophr Res. 2017;183:56–63. Available from. https://doi.org/10.1016/j.schres.2016.11.020.
Woodrow A, Sparks S, Bobrovskaia V, Paterson C, Murphy P, Hutton P. Decision-making ability in psychosis: a systematic review and meta-analysis of the magnitude, specificity and correlates of impaired performance on the Iowa and Cambridge Gambling Tasks. Psychol Med. 2019;49(1):32–38.
Shea BJ, Reeves BC, Wells G, Thuku M, Hamel C, Moran J, et al. AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ. 2017;358:1–9.
Heerey E, Bell-Warren K, Gold J. Decision-making impairments in the context of intact reward sensitivity in schizophrenia. Biol Psychiatry. 2008;64(1):62–9.
Nestor P, Choate V, Niznikiewicz M, Levitt J, Shenton M, McCarley R. Neuropsychology of reward learning and negative symptoms in schizophrenia. Schizophr Res. 2014;159(0):506–8.
Cooke A, Smith D, Booth A. Beyond PICO. Qual Health Res. 2012;22(10):1435–43 Available from: http://journals.sagepub.com/doi/10.1177/1049732312452938.
Gold JM, Waltz JA, Prentice KJ, Morris SE, Heerey EA. Reward processing in schizophrenia: a deficit in the representation of value. Schizophr Bull. 2008;34(5):835–47.
Maguire S, Rea SM. Convery. Electroconvulsive therapy - what do patients think of their treatment? Ulster Med J. 2016;85(3):182–6.
Nakanishi M, Setoya Y, Kodaka M, Makino H, Nishimura A, Yamauchi K, et al. Symptom dimensions and needs of care among patients with schizophrenia in hospital and the community. Psychiatry Clin Neurosci. 2007;61(5):495–501.
Maitre E, Debien C, Nicaise P, Wyngaerden F, LeGadulec M, et al. Advanced directives in psychiatry: a review of the qualitative literature, a state-of-the-art and viewpoints. Encephale. 2013;39(4):244–51.
Wilder C, Elbogen E, Moser L, Swanson J, Swartz M. Medication preferences and adherence among individuals with severe mental illness who completed psychiatric advance directives. Psychiatr Serv. 2010;61(4):380–5.
Gergel T, Owen GS. Fluctuating capacity and advance decision-making in bipolar affective disorder - self-binding directives and self-determination. Int J Law Psychiatry [Internet]. 2015;40:92–101. Available from:. https://doi.org/10.1016/j.ijlp.2015.04.004.
Fisher A, Manicavasagar V, Kiln F, Juraskova I. Communication and decision-making in mental health: a systematic review focusing on bipolar disorder. Patient Educ Couns. 2016;99(7):1106–20. Available from:. https://doi.org/10.1016/j.pec.2016.02.011.
Stovell D, Morrison AP, Panayiotou M, Hutton P. Shared treatment decision-making and empowerment-related outcomes in psychosis: systematic review and meta-analysis. Br J Psychiatry. 2016;209(1):23–8.
Dornan J, Kennedy M, Garland J, Rutledge E, Kennedy HG. Functional mental capacity, treatment as usual and time: magnitude of change in secure hospital patients with major mental illness psychiatry. BMC Res Notes. 2015;8(1):1–9.
Asher L, Patel V, De Silva M. Community-based psychosocial interventions for people with schizophrenia in low and middle-income countries: systematic review and meta-analysis. BMC Psychiatry. 2017;17:355. https://doi.org/10.1186/s12888-017-1516-7.
Schaefer LA. MacArthur competence assessment tools. In: Kreutzer J.S., DeLuca J., Caplan B. (eds) Encyclopedia of Clinical Neuropsychology. New York: Springer; 2011.
Owen G, David A, Hayward P, et al. Retrospective views of psychiatric in-patients regaining mental capacity. Br J Psychiatry. 2009;195(5):403–7.
Moser DJ, Reese RL, Hey CT, Schultz SK, Arndt S, Beglinger LJ, et al. Using a brief intervention to improve decisional capacity in schizophrenia research. Schizophr Bull. 2006;32(1):116–20.
Wang X, Yu X, Appelbaum S, Tang H, Yao G, Si T, et al. Longitudinal informed consent competency in stable community patients with schizophrenia: a one-week training and one-year follow-up study. Schizophr Res. 2016;170(1):162–7.
Sugawara N, Yasui-Furukori N, Sumiyoshi T. Competence to consent and its relationship with cognitive function in patients with schizophrenia. Front Psychiatry. 2019;10:195. Published 2019 Apr 12. https://doi.org/10.3389/fpsyt.2019.00195.
Jacob K. Recovery model of mental illness: a complementary approach to psychiatric care. Indian J Psychol Med. 2015;37(2):117–9.
Acknowledgements
Not applicable.
Funding
Ferrer funded the development of the study and the writing of the manuscript.
Author information
Authors and Affiliations
Contributions
SP, ACB, EV designed the study. SP developed the review and produced drafts of the manuscript. SP, ACB, EV, JMR, AF, MSC interpreted the data and were major contributors in writing the manuscript. SP, ACB, EV, JMR, AF, MSC substantially revised, and approved the final manuscript. SP, ACB, EV, JMR, AF, MSC agreed to be personally accountable for the author’s own contributions and to ensure that questions related to the accuracy or integrity of any part of the work are appropriately investigated, resolved, and the resolution documented in the literature.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Additional file 1.
Meta- review search strategy.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Calcedo-Barba, A., Fructuoso, A., Martinez-Raga, J. et al. A meta-review of literature reviews assessing the capacity of patients with severe mental disorders to make decisions about their healthcare. BMC Psychiatry 20, 339 (2020). https://doi.org/10.1186/s12888-020-02756-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12888-020-02756-0