Abstract
Background
β2-Adrenergic receptors (β2AR) play important regulatory roles in a variety of cells and organ systems and are important therapeutic targets in the treatment of airway and cardiovascular disease. Prolonged use of β-agonists results in tolerance secondary to receptor down-regulation resulting in reduced therapeutic efficiency. The purpose of this work is to evaluate the signaling capabilities of the β2AR expressed by a recombinant adeno-associated viral (AAV) vector that also included an enhanced green fluorescent protein (EGFP) gene (AAV-β2AR/EGFP).
Results
By epifluorescence microscopy, ~40% of infected HEK 293 cells demonstrated EGFP expression. β2AR density measured with [3H]dihydroalprenolol ([3H]DHA) increased either 13- or 77-fold in infected cells compared to mock infected controls depending on the culture conditions used. The [3H]DHA binding was to a single receptor population with a dissociation constant of 0.42 nM, as would be expected for wild-type β2AR. Agonist competition assays with [3H]DHA showed the following rank order of potency: isoproterenol>epinephrine> norepinephrine, consistent with β2AR interaction. Isoproterenol-stimulated cyclic AMP levels were 5-fold higher in infected cells compared to controls (314 ± 43 vs. 63.4 ± 9.6 nmol/dish; n = 3). Receptor trafficking demonstrated surface expression of β2AR with vehicle treatment and internalization following isoproterenol treatment.
Conclusions
We conclude that HEK 293 cells infected with AAV-β2AR/EGFP effectively express β2AR and that increased expression of these receptors results in enhanced β2AR signaling. This method of gene transfer may provide an important means to enhance function in in vivo systems.
Similar content being viewed by others
Background
The β2-adrenergic receptor (β2AR) is a member of the guanine nucleotide regulatory protein (G-protein) coupled receptor superfamily that mediates the effects of the catecholamines epinephrine and norepinephrine. β2ARs are widely expressed in a variety of tissues including the airways of the lung and the cardiovascular system. β2ARs mediate airway smooth muscle relaxation, increase ciliary motility, improve ion transport across epithelium, and reduce inflammatory cell mediator release. In the cardiovascular system, β2ARs regulate vascular tone and enhance chronotropic effects on cardiac muscle [1, 2].
Investigators have previously used viral gene transfer and transgenic animal models to demonstrate that physiologic responsiveness to catecholamines can be enhanced by increasing β2AR expression. Over-expression of β2AR has been shown to have beneficial effects in the failing heart. Transgenic over-expression of β2AR and β-adrenergic receptor kinase 1 (βARK1) inhibitor in cardiac muscle results in improvement in cardiac contractile function caused by changes in β2AR activation and signaling [3, 4]. Adenoviral-mediated gene transfer of β2AR to failing rabbit cardiac myocytes [5] and ex vivo to adult rat hearts [6] results in restoration of β2AR signaling in cardiac muscle. Likewise, adenoviral-mediated β2AR gene delivery to rat carotid arteries leads to enhanced vasorelaxation in response to isoproterenol when compared to control animals [7].
Transgenic over-expression of β2AR in airway smooth muscle using a smooth muscle-specific promoter is associated with protection against methacholine-induced bronchoconstriction [8]. Similarly, targeted over-expression of β2AR in mouse airway epithelium using a Clara cell-specific promoter results in reduced airway responsiveness to both methacholine and ozone [9]. These data in airway epithelium confirmed the importance of airway relaxation mediated through airway epithelial β2AR [10]. Transgenic over-expression of β2AR in type II alveolar cells results in enhanced alveolar fluid clearance [11]. Furthermore, adenoviral-mediated over-expression of β2AR in human lung epithelial cells (A549) is associated with enhanced fluid clearance and responsiveness to endogenous catecholamines [12].
The application of β2AR gene transfer to a variety of cell types is especially appealing in light of the myriad of important physiological functions of β2AR. The strategy of our work is to develop a useful gene delivery model for increased expression of the β2AR utilizing an adeno-associated viral (AAV) vector. While other viral vectors have proven useful in β2AR gene transfer in animal models, we have chosen to use AAV due to its long term potential as a gene delivery system for use in humans. We have developed a recombinant AAV containing the β2AR and enhanced green fluorescent protein (EGFP). The purpose of this study is to evaluate the signaling capabilities of the expressed β2AR. Our findings demonstrate that expression of β2AR can be significantly increased in infected cells and that the expressed receptors serve to enhance physiologic responsiveness to adrenergic agonists.
Results
Efficiency of gene delivery in HEK 293 cells
A recombinant adeno-associated viral (rAAV) vector was designed to include tandem cassettes encoding the human β2AR and enhanced green fluorescent protein (EGFP) genes and was designated AAV-β2AR/EGFP (Figure 1). To evaluate for efficiency of viral unit transfer into AAV-β2AR/EGFP infected cells, the detection of EGFP was used as a surrogate or screening marker for β2AR expression. HEK 293 cells were visualized using epifluorescence microscopy. Approximately 40% of cells infected with AAV-β2AR/EGFP (200 transducing units/cell) demonstrated green fluorescence (Figure 2), while mock infected cells lacked EGFP expression (data not shown). These results indicate that HEK 293 cells are readily infected with a recombinant AAV and that the EGFP cassette was expressed.
Recombinant AAV structures. A. In wild-type AAV, the rep region encodes products required for AAV DNA replication. The lip and cap regions encode the virion capsid proteins. The internal terminal repeats (ITR) are required in cis for AAV packaging and integration into host DNA. B. AAV-β2AR/EGFP represents the complete recombinant vector with tandem β2AR and EGFP cassettes driven by separate CMV promoters.
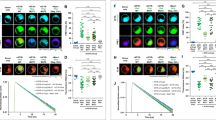
Analysis of EGFP expression in infected HEK 293 cells. Cells were cultured in 10% FBS and were infected with AAV-β2AR/EGFP and screened for EGFP expression as a surrogate marker of β2AR expression efficiency. Using epifluorescence microscopy to compare phase contrast (A) and green fluorescence (B), EGFP expression was observed in ~40% of cells present, as seen in this representative image. This experiment was performed 5 times with similar results. Scale bar, 10 μM.
Pharmacologic specificity of recombinant β2-adrenergic receptors
To determine the pharmacologic characteristics of the recombinant β2AR, we used HEK 293 cells because of their low endogenous expression of β2AR. We first sought to determine the characteristics of the expressed receptor in saturation binding experiments. [3H]dihydroalprenolol ([3H]DHA) binding to membranes prepared from AAV-β2AR/EGFP-infected HEK 293 cells was to a single, saturable site that displayed high affinity as shown in a representative Scatchard plot (Figure 3). Separate experiments with four different membrane preparations established a binding site concentration (Bmax) of 5.05 ± 1.0 pmol/mg protein (n = 4) and a dissociation constant (Kd) of 0.42 ± 0.1 nM (n = 4). These findings demonstrate [3H]DHA binding to a single population of receptors with affinity expected for wild-type β2AR [13].
Saturation binding of [3H]DHA to membranes prepared from HEK 293 cells cultured in 10% FBS and infected with AAV-β2AR/EGFP. Membranes were incubated at 30°C for 20 minutes with increasing concentrations of [3H]DHA. Non-specific binding was defined with 0.1 μM (-)-propranolol. Inset: Direct plot showing total binding (closed circles), nonspecific binding (closed triangles), and specific binding (open circles). These data were representative of four separate experiments.
The specificity of [3H]DHA binding was examined in competition binding assays using various adrenergic agonists (Figure 4). In five separate experiments, the rank order potency of agonist binding to membranes prepared from HEK 293 cells infected with AAV-β2AR/EGFP was isoproterenol (Ki = 1.9 ± 0.7 μM) > epinephrine (Ki = 5.7 ± 2.5 μM) > norepinehrine (Ki = 22.8 ± 7.7 μM) (n = 5). This rank order potency is consistent with a β2AR interaction.
Adrenergic agonist competition with [3H]DHA binding to membranes prepared from HEK293 cells cultured in 10% FBS that had been infected with AAV-β2AR/EGFP. Membranes were incubated at 30°C for 20 minutes with [3H]DHA and increasing concentrations of either (-)-isoproterenol (circles), (-)-epinephrine (squares), or (-)-norepinephrine (triangles). These data were representative of four separate experiments.
Increased β2AR expression in AAV-β2AR/EGFP infected HEK 293 cells
HEK 293 cells express low levels of β2AR [14]. To determine the capability of AAV-β2AR/EGFP to increase β2AR expression in HEK 293 cells, ligand binding assays were employed in AAV-β2AR/EGFP infected and mock-infected cells grown in DMEM supplemented with 10% FBS. Mock infected HEK 293 cells demonstrated specific binding of [3H]DHA to a single saturable site at a level of 39 ± 11 fmol/106 cells. β2AR levels were significantly (p < 0.001) increased in AAV-β2AR/EGFP infected cells to 501 ± 82 fmol/106 cells, representing a 13-fold increase in β2AR expression levels when comparing AAV-β2AR/EGFP infected cells to mock-infected cells (Figure 5). To further assess the role of serum source on β2AR expression in infected HEK 293 cells, we conducted similar studies using 5% CS. In cells cultured in DMEM with 5% CS, background β2AR expression was lower than in cells grown in 10% FBS, with mock-infected cells showing β2AR levels of 5.5 ± 3.4 fmol/106 cells. β2AR levels were significantly increased (p < 0.001) in AAV-β2AR/EGFP infected cells to 428 ± 95 fmol/106 cells, representing a 77-fold increase in β2AR levels when comparing AAV-β2AR/EGFP infected cells to mock-infected cells grown in 5% CS (Figure 5). This dramatic increase in receptor expression when comparing cells grown in 5% CS to those grown in 10% FBS was due to differences in baseline β2AR expression in mock-infected cells. Interestingly, the absolute level of β2AR expression after AAV-β2AR/EGFP infection was not different between culture conditions. Overall, these results indicate that β2AR levels can be significantly increased in HEK293 cells infected with AAV-β2AR/EGFP, but that there may be an upper limit for membrane expression of β2AR in this cell line.
β2AR expression in infected vs. control HEK 293 cells. HEK 293 cells were cultured in DMEM with either 5% CS or 10% FBS then either mock infected (control) or infected with AAV-β2AR/EGFP. Cells were harvested and incubated at 30°C for 20 minutes with a saturating concentration of [3H]DHA to determine β2AR levels as described in Methods. Non-specific binding was defined with 0.1 μM (-)-propranolol. Values are the means ± S.E. from five different experiments.
Enhanced cAMP signaling in infected HEK 293 cells
Binding of agonist to the β2AR results in adenylyl cyclase activation and conversion of ATP to cyclic AMP [15]. To evaluate the ability of the recombinant β2AR to activate early receptor signaling pathways, isoproterenol-stimulated cyclic AMP accumulation was measured in HEK 293 cells infected with AAV-β2AR/EGFP (Figure 6). Cells were treated with the phosphodiesterase inhibitor, IBMX, at the time of isoproterenol treatment to maximize the cyclic AMP signal. In mock-infected (control) cells, cyclic AMP accumulation was 4.83 ± 0.42 nmoles/dish in the absence of isoproterenol and 63.4 ± 9.6 nmoles/dish in the presence of isoproterenol, representing a 13-fold increase in cyclic AMP accumulation in isoproterenol-treated, mock infected cells. In AAV-β2AR/EGFP infected cells, cyclic AMP accumulation increased from 4.69 ± 0.84 nmoles/dish in the absence of isoproterenol stimulation to 314 ± 43 nmoles/dish in the presence of isoproterenol, representing a 67 fold increase in cyclic AMP accumulation. The increase in cyclic AMP production in AAV-β2AR/EGFP infected cells was significantly different from control, mock infected cells (p < 0.05). These data indicate that in addition to binding agonists with the expected pharmacologic specificity, the recombinant β2AR was capable of interacting with downstream intracellular signaling proteins to stimulate cyclic AMP accumulation.
Isoproterenol-stimulated cyclic AMP production in HEK 293 cells cultured in 10% FBS and infected with AAV-β2AR/EGFP. HEK 293 cells were either mock infected (control) or infected with AAV-β2AR/EGFP. Four days later, the cells were incubated with 250 μM IBMX and either 10 μM (-)-isoproterenol or vehicle for 15 min at 37°C, and cyclic AMP was measured as described in Materials and Methods. Values are the means ± S.E. from three separate experiments.
Intracellular trafficking of recombinant β2AR in infected HEK 293 cells
Previous reports indicate that ligand-induced trafficking of the β2AR begins in the early endosome [14, 16]. Through further intracellular signaling, the internalized β2AR is then either recycled to the plasma membrane or is committed to a degradation pathway terminating in the lysosome [17]. To determine if the recombinant β2AR expressed from AAV-β2AR/EFGP retains receptor trafficking in HEK 293 cells, receptor distribution was assessed using a polyclonal antibody to the cytoplasmic tail of the β2AR labeled with a Texas Red fluorochrome. Recombinant receptors were localized to the cell surface after treatment with vehicle alone, with minimal evidence for intracellular distribution (Figures 7, Panel A). Following isoproterenol treatment for 20 minutes, recombinant β2AR were observed to move from the cell surface to small, punctate intracellular vesicles with minimal surface expression noted (Figure 7, Panel B). Following isoproterenol treatment for 24 hours, recombinant β2AR were noted to traffick to both large and small, perinuclear vesicles as would be expected for wild-type receptors following prolonged agonist exposure (Figure 7, Panel C). Additionally, images obtained after 24 hour agonist treatment suggest that some receptors were located on the plasma membrane possibly due to efficient recycling mechanisms as is seen with native β2AR [18] or due to the abundance of expressed β2AR. These results indicate that agonist induced trafficking of recombinant β2AR remains intact with ligand-induced internalization of receptor but with retention of some cell surface expression, even after prolonged agonist exposure. These results further suggest that an added benefit of recombinant β2AR expression is persistence of β2AR on the cell surface in the continuing presence of agonist.
Analysis of β2AR trafficking in AAV-β2AR/EGFP infected HEK 293 cells. Cells were cultured in 10% FBS and treated with either vehicle (A), 10 μM isoproterenol for 20 minutes (B) or 10 μM isoproterenol for 24 hr (C) and analyzed via epifluorescence microscopy using polyclonal antibody to the cytoplasmic tail of β2AR. Mock infected HEK 293 cells demonstrated no β2AR staining (data not shown). Recombinant β2AR showed predominantly surface staining in the presence of vehicle (A). Following 20 minute isoproterenol treatment, recombinant β2AR were sequestered internally (B). Following 24 hour isoproterenol treatment, recombinant β2AR demonstrated trafficking to large, perinuclear vesicles with some β2AR demonstrated on the surface (C). This experiment was performed 3 times with identical results. Scale bar, 10 μM.
Discussion
In this study, we have developed and tested a model for the delivery of the genes encoding the β2AR and enhanced green fluorescent protein to cultured cells. We have demonstrated that utilization of a recombinant AAV vector provides an effective means of gene delivery without evidence of cell toxicity four days after infection. We have also shown that expressed recombinant β2AR have pharmacologic and functional properties characteristic of wild type β2AR but with enhanced expression and signaling. These findings provide a new model for the study of β2AR expression in tissue that is efficient and serves as a framework for study in physiologically relevant tissue (e.g, airway cells or lung tissue).
The role of gene transfer in the treatment of disease is evolving and shows promise in many disorders [19]. Transfer of the β2AR gene to cardiac, vascular, and airway epithelial tissue has been accomplished using adenoviral vectors [6, 7, 12]. Similarly, adenoviral-mediated transfer of the β-adrenergic receptor kinase 1 (βARK1) inhibitor gene, important in controlling β2AR activation and signaling, has been performed in cardiac myocytes [5]. Enhanced expression of β2AR or signaling pathway components in cardiac tissue has resulted in improvements in cardiac function [20], while over-expression of β2AR in vasculature results in enhanced vasorelaxation [7]. Similarly, adenoviral-mediated transfer of the β2AR gene to airway epithelium improved fluid clearance and response to catecholamines [12]. For β2AR gene delivery, we have chosen to utilize an adeno-associated viral vector. The AAV system provides several advantages over other viral vectors including: 1) its ability to transduce both dividing and non-dividing cells; 2) its broad tropism; 3) its ability to integrate into the host genome; 4) its status as a nonpathogenic virus; and 5) its lack of induction of a cell-mediated immune response [21]. One important limitation to the use of AAV vectors for gene transfer is the size constraint in gene packaging, limited to 4.7 kb, the size of the AAV genome. Because the β2AR is a relatively small, intronless gene it is well-suited for AAV vector delivery. Our system is the first to use AAV to enhance β2AR expression thus providing a model that has applicability toward our ultimate target, human disease.
Our investigation has focused at present on both the development of an efficient recombinant AAV system to deliver the β2AR gene to cultured cells and functional testing to determine that the β2AR expressed following infection of HEK 293 cells with AAV-β2AR/EGFP has properties characteristic of wild-type β2AR but with the ability to significantly enhance signaling and impart improved responsiveness to hormone. HEK 293 cells were chosen for study because of their ease of culture, low endogenous β2AR expression, and prior utility in other studies of β2AR function [14]. Four days after infection, up to 40% of infected cells expressed EGFP, and β2AR levels were increased significantly compared to mock infected cells. Cells cultured in 10% FBS demonstrated a 13-fold increase in receptor expression, while those cultured in 5% CS demonstrated a 77-fold increase. This difference was due to higher receptor expression in mock-infected (control) cells when cultured in 10% FBS with the absolute level of receptor expression being equivalent despite growth media conditions. Ligand binding studies demonstrated that recombinant β2AR represented a single population of receptors with pharmacological properties that were identical to wild-type β2AR. These studies also suggest that an upper limit for membrane expression of recombinant receptors may have been reached in HEK 293 cells.
It has been long recognized that epinephrine and norepinephrine acting through β2AR modulate a variety of important cellular and tissue functions [1]. Although these effects may be beneficial to the host, prolonged use of agonist agents has been associated with detrimental effects through the well-known phenomenon of tachyphylaxis or tolerance [22, 23]. Tachyphylaxis results from a culmination of molecular events including receptor desensitization, sequestration and down-regulation [24]. Thus, we have asked an important, physiologically relevant question. Can over-expression of β2AR using an AAV-mediated delivery system reduce β2AR tachyphylaxis? We hypothesized that this could occur through three possible mechanisms: 1) through addition of increased numbers of β2AR to the cell, 2) through enhanced recycling, and/or 3) through reduced receptor down-regulation.
The use of fluorescent microscopy to monitor trafficking of receptors in cells can provide further insight related to the fate of the β2AR following agonist activation. In stable transfection models, β2AR have been shown to sequester to the intracellular environment within minutes after agonist activation and co-localize with transferrin-containing compartments, characteristic of recycling endosomes [14, 17]. Using a β2AR-GFP fusion gene, Kallal and Benovic demonstrated that with prolonged agonist treatment, β2AR co-localize with dextran-labeled compartments, characteristic of lysosomes [17]. Our initial studies confirm that recombinant β2ARs localize to the plasma membrane prior to agonist treatment and efficiently sequester to intracellular vesicles following agonist treatment. Our findings also indicate persistence of receptor expression on the cell surface following ligand-induced activation and intracellular trafficking. Persistence of surface expression may provide a physiologic advantage for the cell or tissue by supplying addition receptors for ligand binding.
Adeno-associated viral vector mediated gene transfer has been successful in human trials [19, 21] and is the subject of ongoing research. Genes delivered by AAV vectors include factor IX and factor VIII for hemophilia, the cystic fibrosis transmembrane reductance regulator (CFTR) for cystic fibrosis, and glial cell line-derived neurotrophic factor (GDNF) and glutamic acid decarboxylase for Parkinson's disease. The ability to efficiently deliver β2AR to airway tissue has the potential to enhance bronchodilation, improve fluid and ion transport and reduce airway inflammation. These functions may have particular relevance in diseases of airway hyperresponsiveness such as asthma or chronic obstructive pulmonary disease. Transfer of the β2AR gene to cardiac muscle and the vasculature can improve chronotropic function, reduce dilation and enhance vasorelaxation [5–7, 20]. For relevance in therapeutic delivery for humans, studies related to long-term gene expression, episomal expression or DNA integration, and potential adverse effects must be addressed.
Conclusions
In summary, this study has demonstrated that β2AR expressed in HEK 293 cells infected with AAV-β2AR/EGFP demonstrate enhanced expression and signaling. This system provides a useful, well-characterized model for future study of β2AR regulation and function. Future studies utilizing AAV-β2AR/GFP should include in vitro studies assessing the destiny of endogenous receptors in cells infected with recombinant AAV-β2AR/EGFP. These studies should be conducted in physiologically relevant cell types such as airway smooth muscle or epithelium. Using AAV to enhance β2AR delivery and signaling should also be studied in animal models of airway hyperresponsiveness to assess the physiologic impact of AAV vector mediated β2AR over-expression.
Methods
Recombinant AAV preparation
A recombinant adeno-associated viral (rAAV) vector was designed to include tandem cassettes encoding the human β2AR and enhanced green fluorescent protein (EGFP) genes and was designated AAV-β2AR/EGFP (Figure 1). Cassettes containing the β2AR and EFGP genes, both driven by CMV promoters, were cloned into pAV53-LR, a plasmid vector containing the internal terminal repeats (ITRs) from AAV (provided by Dr. Juinyan Dong, Medical University of South Carolina, Charleston, SC). Briefly, the β2AR gene was PCR-amplified from human genomic DNA using a forward primer (5'CATATAAAGCTT- CAGCCAGTGCGCTTACCTGC3') engineered with a Hind III site (underlined) upstream of the ATG, and a reverse primer (5'CATATAGGATCC GTTTAGTGTTCTGTTGGGCGG3') engineered with a BamH I site (underlined) downstream of the stop codon. The PCR fragment was subcloned into pCEP4 vector (Invitrogen, Carlsbad, CA) using Hind III and BamH I sites. The pCEP4 vector provided the CMV promoter and SV40 polyA tail adenlyation signal. The β2AR moiety was released with Sal I and subcloned into the Xho I site of pAV53-LR. To track infection levels using a surrogate marker gene, the EGFP gene cassette was inserted into the AAV-β2AR vector. The EGFP gene was obtained from PCR amplification of pEGFP-C1 plasmid (Clontech) using a forward primer (5'CATATAGCATGC CCGTATTACCGCCATG-CATTAG3') and a reverse primer (5'CATATAGCATGC GCCGATTTCGGCCTATTGG-TTA3') both engineered with Sph I sites (underlined). The EGFP insert was subcloned into the multiple cloning site of the AAV-β2AR vector using the Sph I site. The final recombinant vector, designated AAV-β2AR/EGFP, has a total length of 4,691 base pairs encoding the β2AR and EGFP genes both driven by separate CMV promoters and containing separate polyadenylation signal sequences. Cassette orientation and sequence were determined using automated DNA sequencing. The AAV-β2AR /EGFP vector was sent to the University of North Carolina Virus Vector Core Facility (Chapel Hill, NC) for viral production. Stock preparations used in experiments ranged from 1.0–3.5 × 1010 transducing units/ml.
Cell culture and infection
The human embryonic kidney cell line, HEK 293, was used for all experiments. HEK 293 cells were grown in DMEM supplemented with 10% fetal bovine (FBS). Supplemental studies assessing the role of growth media on receptor expression were conducted using 5% calf serum (CS) in place of FBS. HEK 293 cells at a cell density of 0.25 × 106 cells/well in 6 well plates were transduced by addition of AAV-β2AR/EGFP (200 transducing units/cell in 1 ml of media per well). Approximately 16 hrs after initial viral application, 1 ml of growth media was added to each well. Assays to determine β2AR expression levels and function were performed on day 4 following infection.
Ligand binding assays to determine receptor specificity
Partially purified membrane preparations were obtained from AAV-β2AR/EGFP infected HEK 293 cells, cultured in DMEM with 10% FBS, by differential centrifugation as previously described [13]. Briefly, cells were washed with ice-cold phosphate-buffered saline (PBS) and scraped into ice-cold PBS with a rubber policeman. The cells were centrifuged at 250 × g for 5 minutes, resuspended in assay buffer (50 mM pH 7.4 Tris-HCl, 2 mM MgCl2) and homogenized with a glass-glass homogenizer followed by sonication (5–10 second bursts at setting 6) with a Tekmar Model AS1 Sonic Disrupter. The nuclei were removed by centifugation at 600 × g for 10 minutes. Membranes were obtained from the resulting supernatant by centrifugation at 30,000 × g for 15 minutes, then resuspended in assay buffer and centrifuged again. The final pellets were resuspended in assay buffer, aliquoted, and stored at -80°C. Protein concentrations of membrane preparations were determined by the method of Bradford [25] using bovine serum albumin as the standard. [3H]Dihydroalprenolol (DHA) (Dupont-NEN, Boston, MA; specific activity = 120 Ci/mmole) was used to identify β2AR as previously described [13]. In saturation experiments, aliquots of HEK 293 cell membranes (final concentration in assay tube = 70 μg/ml) were incubated with 7 different concentrations of [3H]DHA ranging from approximately 0.05 to 5 nM. In competition experiments, membrane aliquots were incubated with approximately 1 nM [3H]DHA and increasing concentrations of the competitors isoproterenol, epinephrine, and norepinehrine (range 10-9 to 10-4 moles/liter). Nonspecific binding was defined with 0.1 μM (-)-propranolol. Data from saturation experiments were analyzed using LIGAND [26]. Inhibition constants were calculated using the method of Cheng and Prusoff [27].
Ligand binding assays to establish the effects of β-agonists on β2AR expression
The effects of β-agonist treatment on β2AR expression were determined by growing AAV-β2AR/EGFP infected HEK 293 cells in DMEM containing 10% FBS. To determine the impact of a less enriched media on β2AR expression, infected HEK 293 cells were also cultured in DMEM with 5% CS. [3H]DHA was used in ligand binding assays to determine β2AR levels as previously described [13]. Approximately 1.2 × 106 cells/ml were incubated in triplicate with a single saturating concentration of [3H]DHA (~5 nM). Nonspecific binding was defined with 0.1 μM (-)-propranalol.
Cyclic AMP determination
Both AAV-β2AR/EGFP infected and mock-infected HEK 293 cells were cultured in DMEM with 10% FBS then in serum-free media overnight. For cyclic AMP determination, cells were then treated either with vehicle or 10 μM isoproterenol and the phosphodiesterase inhibitor, isobutylmethylxanthine (IBMX, 250 μM), for 10 minutes. Cellular cyclic AMP levels were determined by radioimmunoassay using the Biotrak CAMP Assay System (Amersham Life Sciences, Arlington Heights, IL).
Fluorescence microscopy and receptor trafficking
For fluorescence microscopy, HEK 293 cells were cultured in DMEM with 10% FBS at a density of 2.5 × 105 cells/well on glass coverslips, infected with AAV-β2AR/EGFP and treated on day 4 with vehicle or 10 μM isoproterenol for 24 hrs at 37°C. Cells were fixed with 1% paraformaldehyde at the designated time intervals. Efficiency of cell infection was evaluated through imaging of green fluorescence as an indicator of EGFP expression. β2ARs were detected with a rabbit polyclonal antibody specific to the cytoplasmic tail of the human β2AR (1:500 dilution; Bethyl Laboratories, Montgomery, TX) and Texas Red-labeled (red fluorescence) goat anti-rabbit IgG antibody (1:200 dilution; T2767; Molecular Probes, Eugene, OR) as previously described [28]. Fluorescence imaging was then performed with a Zeiss Axiovert digital deconvolution microscope (Carl Zeiss, Inc., Thornwood, NY). For EGFP expression, cells were visualized using epifluorescence microscopy with a 100× oil objective. For β2AR detection, images were collected using a 100× oil objective in Z-stacks then digital deconvolution was performed using AxioVision 3.1 (Carl Zeiss, Inc.). Images were then converted to tagged-image files (tiff) for comparison.
Statistical analysis
Data are presented as the mean ± S.E.M. Comparisons between groups were made by using one-way analysis of variance (ANOVA) with Newman-Keuls post hoc testing. The 0.05 level of probability was accepted as significant. Computations were performed using the SigmaStat software package (Jandel Scientific, San Rafael, CA).
References
Hein L, Kobilka BK: Adrenergic receptor signal transduction and regulation. Neuropharmacology. 1995, 34: 357-366. 10.1016/0028-3908(95)00018-2.
Nijkamp FP, Engels F, Henricks PA, Van Oosterhout AJ: Mechanisms of beta-adrenergic receptor regulation in lungs and its implications for physiological responses. Physiol Rev. 1992, 72: 323-367.
Rockman HA, Choi DJ, Akhter SA, Jaber M, Giros B, Lefkowitz RJ, Caron MG, Koch WJ: Control of myocardial contractile function by the level of b-adrenergic receptor kinase 1 in gene-targeted mice. J Biol Chem. 1998, 273: 18180-18184. 10.1074/jbc.273.29.18180.
Koch WJ, Rockman HA, Samama P, Hamilton RA, Bond RA, Milano CA, Lefkowitz RJ: Cardiac function in mice overexpressing the b-adrenergic receptor kinase or a bARK inhibitor. Science. 1995, 268: 1350-1353.
Akhter SA, Skaer CA, Kypson AP, McDonald PH, Peppel KC, Glower DD, Lefkowitz RJ, Koch WJ: Restoration of b-adrenergic signaling in failing cardiac ventricular myocytes via adenoviral-mediated gene transfer. Proc Natl Acad Sci U S A. 1997, 94: 12100-12105. 10.1073/pnas.94.22.12100.
Kypson AP, Peppel K, Akhter SA, Lilly RE, Glower DD, Lefkowitz RJ, Koch WJ: Ex vivo adenovirus-mediated gene transfer to the adult rat heart. J Thorac Cardiovasc Surg. 1998, 115: 623-630.
Gaballa MA, Peppel K, Lefkowitz RJ, Aguirre M, Dolber PC, Pennock GD, Koch WJ, Goldman S: Enhanced vasorelaxation by overexpression of b2-adrenergic receptors in large arteries. J Mol Cell Cardiol. 1998, 30: 1037-1045. 10.1006/jmcc.1998.0668.
McGraw DW, Forbes SL, Kramer LA, Witte DP, Fortner CN, Paul RJ, Liggett SB: Transgenic overexpression of beta(2)-adrenergic receptors in airway smooth muscle alters myocyte function and ablates bronchial hyperreactivity. J Biol Chem. 1999, 274: 32241-32247. 10.1074/jbc.274.45.32241.
McGraw DW, Forbes SL, Mak JC, Witte DP, Carrigan PE, Leikauf GD, Liggett SB: Transgenic overexpression of b2-adrenergic receptors in airway epithelial cells decreases bronchoconstriction. Am J Physiol Lung Cell Mol Physiol. 2000, 279: L379-L389.
Flavahan NA, Aarhus LL, Rimele TJ, Vanhoutte PM: Respiratory epithelium inhibits bronchial smooth muscle tone. J Appl Physiol. 1985, 58: 834-838.
McGraw DW, Fukuda N, James PF, Forbes SL, Woo AL, Lingrel JB, Witte DP, Matthay MA, Liggett SB: Targeted transgenic expression of beta(2)-adrenergic receptors to type II cells increases alveolar fluid clearance. Am J Physiol Lung Cell Mol Physiol. 2001, 281: L895-L903.
Dumasius V, Sznajder JI, Azzam ZS, Boja J, Mutlu GM, Maron MB, Factor P: beta(2)-adrenergic receptor overexpression increases alveolar fluid clearance and responsiveness to endogenous catecholamines in rats. Circ Res. 2001, 89: 907-914.
Cao W, McGraw DW, Lee TT, Dicker-Brown A, Hiller FC, Cornett LE, Jones SM: Expression of functional beta 2-adrenergic receptors in a rat airway epithelial cell line (SPOC1) and cell density-dependent induction by glucocorticoids. Exp Lung Res. 2000, 26: 421-435. 10.1080/01902140050130347.
von Zastrow M, Kobilka BK: Ligand-regulated internalization and recycling of human b2-adrenergic receptors between the plasma membrane and endosomes containing transferrin receptors. J Biol Chem. 1992, 267: 3530-3538.
Liggett SB: Update on current concepts of the molecular basis of beta2-adrenergic receptor signaling. J Allergy Clin Immunol. 2002, 110: S223-S227. 10.1067/mai.2002.129945.
von Zastrow M, Kobilka BK: Antagonist-dependent and -independent steps in the mechanism of adrenergic receptor internalization. J Biol Chem. 1994, 269: 18448-18452.
Kallal L, Gagnon AW, Penn RB, Benovic JL: Visualization of agonist-induced sequestration and down-regulation of a green fluorescent protein-tagged b2-adrenergic receptor. J Biol Chem. 1998, 273: 322-328. 10.1074/jbc.273.1.322.
Cao TT, Deacon HW, Reczek D, Bretscher A, von Zastrow M: A kinase-regulated PDZ-domain interaction controls endocytic sorting of the b2-adrenergic receptor. Nature. 1999, 401: 286-290. 10.1038/45816.
Factor P: Gene therapy for acute diseases. Mol Ther. 2001, 4: 515-524. 10.1006/mthe.2001.0504.
Rockman HA, Koch WJ, Lefkowitz RJ: Cardiac function in genetically engineered mice with altered adrenergic receptor signaling. Am J Physiol. 1997, 272: H1553-H1559.
Stilwell JL and Samulski,RJ: Adeno-associated virus vectors for therapeutic gene transfer. Biotechniques. 2003, 34: 148-159.
Sears MR, Taylor DR, Print CG, Lake DC, Li QQ, Flannery EM, Yates DM, Lucas MK, Herbison GP: Regular inhaled beta-agonist treatment in bronchial asthma. Lancet. 1990, 336: 1391-1396. 10.1016/0140-6736(90)93098-A.
Sears MR: Adverse effects of beta-agonists. J Allergy Clin Immunol. 2002, 110: S322-S328. 10.1067/mai.2002.129966.
Benovic JL: Novel beta2-adrenergic receptor signaling pathways. J Allergy Clin Immunol. 2002, 110: S229-S235. 10.1067/mai.2002.129370.
Bradford MM: A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem. 1976, 72: 248-254. 10.1006/abio.1976.9999.
Munson PJ, Rodbard D: Ligand: a versatile computerized approach for characterization of ligand-binding systems. Anal Biochem. 1980, 107: 220-239. 10.1016/0003-2697(80)90515-1.
Cheng Y, Prusoff WH: Relationship between the inhibition constant (K1) and the concentration of inhibitor which causes 50 per cent inhibition (I50) of an enzymatic reaction. Biochem Pharmacol. 1973, 22: 3099-3108. 10.1016/0006-2952(73)90196-2.
Jones SM, Foreman SK, Shank BB, Kurten RC: EGF receptor downregulation depends on a trafficking motif in the distal tyrosine kinase domain. Am J Physiol Cell Physiol. 2002, 282: C420-C433.
Acknowledgements
We are grateful to Dr. Richard Kurten, Director of the Digitial and Confocal Microscopy Facility, Department of Physiology and Biophysics, University of Arkansas for Medical Sciences, for advice during the use of the facilities in the University of Arkansas for Medical Sciences Digital and Confocal Microscopy Laboratory that is supported by NIH Grants 1 P20 RR 16460 and PAR-98-092, 1-R24 CA82899.
This work was supported by National Institute of Allergy and Infectious Disease Grant 1K23-AI-01818 (SM Jones), American Heart Association Grant 9960280Z (SM Jones), a grant from the Arkansas Biosciences Institute (LE Cornett) and the Davidson C. Roy Trust to the UAMS Foundation (FC Hiller).
Author information
Authors and Affiliations
Corresponding author
Additional information
Authors' Contributions
SMJ carried out the immunofluorescence assays, participated in study design and project oversight and drafted the manuscript. FCH participated in study design. SEJ conducted vector cloning, sequencing and cyclic AMP assays. SKF conducted western blot and ligand binding assays. LMP participated in immunofluorescence and western blot assays. LEC conceived the study and participated in its design and coordination. All authors read and approved the final manuscript.
Authors’ original submitted files for images
Below are the links to the authors’ original submitted files for images.
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Jones, S.M., Hiller, F.C., Jacobi, S.E. et al. Enhanced β2-adrenergic receptor (β2AR) signaling by adeno-associated viral (AAV)-mediated gene transfer. BMC Pharmacol 3, 15 (2003). https://doi.org/10.1186/1471-2210-3-15
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1471-2210-3-15