Abstract
Background
Respiratory syncytial virus (RSV) is the leading cause of respiratory infections in children, elderly, and immunocompromised individuals. Severe infection is associated with short- and long-term morbidity including pneumonia, recurrent wheezing, and abnormal pulmonary function, and several lines of evidence indicate that impaired adaptive immune responses during infection are critical in the pathophysiology of RSV-mediated disease. Myeloid Dendritic cells (mDCs) play a pivotal role in shaping antiviral immune responses in the respiratory tract; however, few studies have examined the interactions between RSV and individual mDC subsets. In this study, we examined the effect of RSV on the functional response of primary mDC subsets (BDCA-1+ and BDCA-3+) isolated from peripheral blood.
Methods
BDCA-1+ and BDCA-3+ mDCs were isolated from the peripheral blood of healthy adults using FACS sorting. Donor-matched BDCA-1+ and BDCA-3+ mDCs were infected with RSV at a multiplicity of infection (MOI) of 5 for 40 hours. After infection, cells were analyzed for the expression of costimulatory molecules (CD86, CD80, and PD-L1), cytokine production, and the ability to stimulate allogenic CD4+ T cell proliferation.
Results
Both BDCA-1+ and BDCA-3+ mDCs were susceptible to infection with RSV and demonstrated enhanced expression of CD86, and the inhibitory costimulatory molecules CD80 and PD-L1. Compared to BDCA-3+ mDCs, RSV-infected BDCA-1+ mDC produced a profile of cytokines and chemokines predominantly associated with pro-inflammatory responses (IL-1β, IL-6, IL-12, MIP-1α, and TNF-α), and both BDCA-1+ and BDCA-3+ mDCs were found to produce IL-10. Compared to uninfected mDCs, RSV-infected BDCA-1+ and BDCA-3+ mDCs demonstrated a reduced capacity to stimulate T cell proliferation.
Conclusions
RSV infection induces a distinct pattern of costimulatory molecule expression and cytokine production by BDCA-1+ and BDCA-3+ mDCs, and impairs their ability to stimulate T cell proliferation.
The differential expression of CD86 and pro-inflammatory cytokines by highly purified mDC subsets in response to RSV provides further evidence that BDCA-1+ and BDCA-3+ mDCs have distinct roles in coordinating the host immune response during RSV infection. Findings of differential expression of PD-L1 and IL-10 by infected mDCs, suggests possible mechanisms by which RSV is able to impair adaptive immune responses.
Similar content being viewed by others
Introduction
Respiratory Syncytial Virus (RSV), a ssRNA pneumovirus of the paramyxoviridae family, is the leading cause of acute lower respiratory tract infections in children, elderly, and immunocompromised patients. More than 95% of children become infected with RSV by 2 years of age, and approximately 50% of children infected in the first year of life are reinfected during the second year [1]. Reinfection continues throughout life, re-emerging as a major cause of community-acquired pneumonia in the elderly [2]. RSV infection is associated with short- and long-term morbidity including pneumonia, recurrent wheezing, and abnormal pulmonary function. Moreover, RSV bronchiolitis has been identified as the highest independent risk factor for the development of asthma and allergic sensitization later in life [3].
Primary RSV infection is controlled by T cell responses which are crucial in viral clearance and limiting disease severity. Weak antiviral cytotoxic responses and decreased numbers of CD4+ and CD8+ T cells in the lower respiratory tract of infants with severe infection [4, 5] along with the susceptibility to repeat infections with RSV strongly suggest that the failure to develop adaptive T cell responses is critical in the pathophysiology of RSV-mediated disease. Additionally, the balance between Th1 and Th2 cytokines produced by T cells plays a crucial role in determining the outcome of infection, and severe RSV infection may be associated with skewing the Th1/Th2 balance of the virus-specific response towards Th2 [6, 7]. However, the mechanisms by which RSV is able to manipulate host immunity are not fully understood.
Dendritic cells (DCs) are an important first line of defense against invading pathogens and are regarded as the most potent antigen presenting cell (APC) type. Upon antigen recognition, DCs produce cytokines and costimulatory signals needed to guide T cell differentiation, ultimately determining the quality and quantity of the resulting immune response. Human DC populations are defined based on their lineage and expression of unique Blood Dendritic Cell Antigens (BDCA), and depending on their derivation, direct immune responses through either the initiation or modulation of immunity. Plasmacytoid DCs (pDCs), characterized by expression of BDCA-2, mediate antiviral immunity via the production of IFN-α [8]. Myeloid DCs (mDCs) are particularly efficient in the uptake, processing and presentation of antigens and can be further subdivided into distinct subsets identified by differential expression of either BDCA-1 (BDCA-1+) or BDCA-3 (BDCA-3+).
The lung contains an elaborate network of dendritic cells that regulate the local environment. During respiratory infections, both tissue-resident DCs, as well as recruited DCs, are activated as part of the host immune response [9]. Although present at much lower frequencies than BDCA-1+ mDCs in peripheral blood, the DC network in the airway mucosa is comprised predominately of BDCA-3+ mDCs [10]. Studies of mDC subsets isolated from human lungs and blood suggest that each subset exhibits distinct roles in coordinating the immune response against pathogens [11–14]. Although the relationship between mDCs found in the lung and peripheral blood is not clear, parallel phenotypic analysis and transcriptome mapping provides evidence that lung and other non-lymphoid tissue BDCA-3+ mDCs are potentially related to blood BDCA-3+ mDCs [15]. The relationship of blood to tissue BDCA-1+ mDCs was not as clearly defined, but did show clustering of their gene signatures [15]. Thus, even though it is likely that lung DCs may in some ways be functionally distinct from blood DCs, these studies demonstrate that blood mDC subsets are potentially related to mDC subsets found in tissues.
As key regulators of immunity, DCs are an ideal target for the virus to exert its immune altering mechanisms. In this regard, a possible role for mDCs in RSV infection is evidenced by observations of increased numbers of mDCs in the airways, and decreased numbers of mDCs in the blood of children with acute RSV infection, suggesting that DCs are recruited out of the blood to the site of infection [16]. Correlations between the number of mDCs and the level of pro-inflammatory cytokines in the nasal cavity of RSV-infected patients indicates that mDCs may represent an important source of inflammatory cytokines during the host immune response against infection [16]. Additionally, RSV infection inhibits the capacity of monocyte derived DCs (Mo-DCs) to stimulate T-cell proliferation in vitro[17, 18] and impairs the function of pulmonary DCs in RSV-infected mice [19]. Taken together, these results suggest that infection with RSV impairs the ability of host immune response to adequately clear viral pathogens by altering DC mediated immune responses.
However, current RSV-mDC studies often utilize murine DCs or mDCs derived in vitro from human monocytes, and even though Mo-DCs have many characteristics similar to myeloid blood DCs [20–22], studies have not shown direct functional correlations between in vitro derived Mo-DCs and individual mDC subsets isolated from lymph nodes or blood [14, 23, 24]. Thus, studies using Mo-DCs may not adequately recapitulate the function of primary mDCs during RSV infection. Few studies have examined the interactions between viral pathogens and primary human mDC subsets, especially BDCA-3+ mDCs. To identify cell-specific responses of primary mDC subsets to RSV infection, we examined the expression of costimulatory markers and production of cytokines by BDCA-1+ and BDCA-3+ mDCs after exposure to RSV. The functional response after infection was evaluated by examining their ability to stimulate T cell proliferation in a mixed lymphocyte reaction. To our knowledge, this is one of the first studies to examine the functional response of highly purified BDCA-1+ and BDCA-3+ mDCs to RSV.
Materials and methods
Isolation of mDC subsets
Buffy coats prepared by the University of Texas Medical Branch (UTMB) blood blank from healthy adult donors who fulfilled criteria for blood donations were obtained. The donor’s identity, race, and age remained anonymous to investigators. This study was approved by UTMB’s Institutional Review Board. Peripheral blood mononuclear cells (PBMCs) were separated from buffy coats by Ficoll-hypaque density centrifugation and enriched for mDCs using an mDC cell isolation kit (Miletnyi Biotec, Auburn, CA) to deplete magnetically labeled non-mDCs. In preparation for FACS sorting, the DC enriched fraction was stained with the following fluorochrome-conjugated monoclonal antibodies (mAbs[clone]): PE-BDCA-3[1A4], APC-BDCA-1[AD5-8E7], FITC-BDCA-2[AC144], and FITC-lineage marker cocktail containing CD3[SK7], CD14[MΦP9], CD16[3G8], CD19[SJ25C1], CD20[L27], CD56[NCAM16.2] purchased from eBiosciences (San Diego, CA), Miltenyi Biotec, and BD Biosciences (San Jose, CA) respectively. Cells were stained in the presence of FcR-blocking reagent (Miltenyi Biotec) to minimize non-specific binding.
Sorting and flow cytometric data acquisition was performed on a FACSAria (BD Biosciences) capable of 9-color analysis running FACS Diva software. BDCA-3+ mDCs were sorted as FITC-, APC-, PEhi and BDCA-1+ were sorted as FITC-, APC+, PEdim with routine post-sort analysis to ensure purity ≥95%.
Virus preparation and infection
Preparation of sucrose-purified RSV (Long strain) has been previously described [18]. RSV was inactivated by exposing the virus to ultraviolet light [18]. For infection, 1×104 cells of donor-matched BDCA-1+ or BDCA-3+ mDCs were resuspended in 200 μl of cRPMI (RPMI 1640 medium + 2 mmol/liter L-glutamine + 10% FBS + 50 μM 2-ME + 100UI/ml penicillin-streptomycin) and incubated for 40 hours at 37°C with RSV or ultraviolet-inactivated RSV (UV-RSV) at a multiplicity of infection (MOI) of 5 [18, 25]. As TLR3 is known to be expressed on BDCA-1+ and BDCA-3+ mDCs [13], cells cultured in the presence of 10 μg/ml of purified poly I:C (InvivoGen, San Diego, CA) served as positive controls and uninfected cells served as negative controls.
FACS analysis of DCs
Mock and RSV-infected BDCA-1+ and BDCA-3+ mDCs were first stained with Fixable Viability Dye eFlour 780 (eBioscience). To detect intracellular expression of RSV antigens, BDCA-1+ and BDCA-3+ mDCs were fixed with Cytofix/Cytoperm™ (Pharmingen), permeabilized with Perm/Wash™ buffer (Pharmingen), and stained with FITC-conjugated anti-RSV antibody (Biosource, Camarillo, CA) as previously described [18]. For costimulatory molecule analysis, mDCs were stained with FITC-PD-L1[M1H1], v450-CD86[2331(FUN-1)], and PE-Cy7-CD80[L307.4] (BD Biosciences) or in a separate set of experiments, PerCP Cy5.5-HLA-DR[L243]. Flow cytometric data acquisition was performed on a BD LSRII Fortessa capable of 18-color analysis running FACS Diva software (BD Biosciences). FloJo V7.6.3 software was used to analyze all flow cytometry data.
Bio-plex assay
After 40 hours, cell free supernatants were collected and tested for cytokines IL-1β, IL-1rα IL-6, IL-7, IL-8, IL-10, IL-12(p70), IFN-γ, CXCL10, TNF-α, G-CSF, MCP-1, MIP-1α, MIP-1β, and RANTES using the Luminex-based Bio-Plex system (Bio-Rad Laboratories, Hercules, CA). The lower limit of detection for all cytokines measured in this assay is 3 pg/ml. When comparing cytokine production between subsets, the fold change in concentration (infected/uninfected) was used to normalize results across cell types.
Allogenic MLR
Allogenic CD4+ T cells were isolated from PBMCs by negative immunomagnetic selection using a CD4+ T cell isolation kit (Miletnyi Biotec, Auburn, CA). Routine post sort purity was >96% as determined by flow cytometry. To track proliferation, T cells were labeled with 10 μM CFSE (Invitrogen, Grand Island, NY) according to the manufacturer’s instructions. Donor matched BDCA-1+ and BDCA-3+ mDCs were incubated for 24 hours at 37°C with RSV, UV- RSV, or poly I:C. After 24 hours, cells were washed and cocultured with the CFSE-labeled allogenic T cells at a ratio of 1:5 in RPMI containing 5% FCS for 6 days at 37°C. T cells alone and T cells incubated with soluble CD3 and CD28 were included as controls. Prior to flow cytometry, cells were stained with PerCP-Cy™ 5.5-CD3[SK7] and PE-Cy™ 7-CD4[RPT-A] (BD Biosciences). Proliferation of CD3+ CD4+ T cells was measured on a BD LSRII Fortessa running FACS Diva software (BD Biosciences) and analyzed using FloJo V7.6.3 software.
Statistical analysis
Statistical Analysis was performed with InStat 5.02 biostatistics package (GraphPad Software, San Diego, CA) using student’s paired t-tests to ascertain differences between uninfected and infected cells of the same type or student’s t-tests to ascertain differences between cell types. Significance was defined as p ≤0.05. Prior to analysis, data sets were log transformed to normalize non-normally distributed data.
Results
Isolation and characterization of mDC subsets
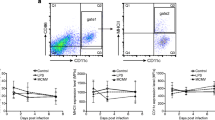
MDC subsets were isolated from PBMCs using a two step procedure [13]. PBMCS were first enriched for mDCs using a myeloid dendritic cell isolation kit to deplete non-myeloid DCs via negative immunoselection, followed by flow cytometry to eliminate residual pDCs and lineage positive cells and sort for BDCA-1+ and BDCA-3+ cells (Figure 1A). Consistent with reported frequencies in blood [13], we were routinely able to isolate approximately 1×104 BDCA-3+ mDCs per 1×108 PBMCS and 1×105 BDCA-1+ mDCs per 1×108 PBMCs with a post-sort purity ≥95% (Figure 1B). At baseline, both subsets demonstrated similar expression of HLA-DR and CD86, but did not express CD80 or PD-L1 (Figure 1C).
Isolation and phenotypic characterization of mDC subsets. ( A ) PBMCs were gated on SSC and FSC to exclude dead cells and debris. Cells were then gated to exclude lineage positive cells and pDCs. Lineage (Lin)-, BDCA-2- cells were then gated for expression of BDCA-1 and BDCA-3. BDCA-1+ mDCs were sorted as Lin-, BDCA-2-, BDCA-1+, BDCA-3dim and BDCA-3+ mDCs were sorted as Lin-, BDCA-2-, BDCA-1-, BDCA-3hi. ( B ) Post-sort purity for all sorted cells was ≥95%. Data is from one donor and is representative of 6 donors. ( C ) Expression of maturation and costimulatory molecules by freshly isolated cells. Filled curves= isotype, solid line=mDC. Data is from one donor and is representative of 3 donors.
RSV infects BDCA-1+ and BDCA-3+mDCs
Work from our lab has previously shown that human Mo-DCs are permissive to RSV infection [18]. To determine the susceptibility of primary mDCs to infection, the intracellular expression of viral proteins by BDCA-1+ and BDCA-3+ infected with RSV at a MOI=5 for 12, 24, or 40 hours was examined using flow cytometry. The greatest percentage of infected cells was detected at 40 hours, with 20-25% of BDCA-1+ mDCs and 18-23% of BDCA-3+ mDCs demonstrating expression of viral proteins (Figure 2). Cells exposed to UV-RSV (non-replicating virus) did not express RSV antigen. Cell viability decreased between 24 and 40 hours; however, there was no difference in the number of viable cells after exposure to RSV and UV-RSV at each time point. In BDCA1+ mDCs, maximal infection occurred at a MOI=5 and increasing the MOI did not result in a further increase in the number of virus-positive cells, whereas, in BDCA-3+ mDCs using an MOI=10 did increase the number of virus-positive cells by approximately 4% (data not shown). As there was no statistically significant difference between the rates of infection in BDCA-1+ and BDCA-3+ mDCs at a MOI=5, this MOI was used for all subsequent RSV infection experiments.
BDCA-1+and BDCA-3+mDCs are susceptible to infection with RSV. BDCA-1+ and BDCA-3+ mDCs were incubated in media alone or exposed to RSV and UV-inactivated RSV at a MOI=5 for 12, 24, or 40 hours. Cells were stained for intracellular expression of RSV protein, and the percentage of RSV-infected cells was quantified using flow cytometry to detect expression of anti-RSV antibody. Filled grey curve=uninfected cells, solid line=infected cells. Data is from one donor, and is representative of 3 donors.
RSV infection modulates costimulatory molecule expression
T cell activation depends, in addition to the binding of MHC/peptide complexes by T cell receptors, on the recognition of positive or negative costimulatory molecules expressed by DCs. Depending on whether they bind to CD28 or CTLA-4 receptors on T cells, CD86 and CD80 expressed on mDCs can deliver either stimulatory (CD28) or inhibitory (CTLA-4) signals for T cell activation. Additionally, the programmed death-1 (PD-1) receptor and its ligands PD-L1 and PD-L2 deliver inhibitory signals that regulate the balance between tolerance vs. T cell activation and immune-mediated tissue damage. Engagement of PD-1 by its ligands blocks T cell proliferation and cytokine production [26] and promotes the development, expansion, and survival of Tregs [27, 28]. Previous work from our lab demonstrated increased expression of CD86, CD80, and PD-L1, but not PD-L2, on RSV-infected Mo-DCs [18, 19]. Therefore, to assess the effect of RSV infection on the regulation of costimulatory molecule expression in primary mDC subsets, the expression of CD86, CD80, and PD-L1 was examined on RSV infected BDCA-1+ and BDCA-3+ mDCs using flow cytometry. In all donors, both RSV-infected BDCA-1+ and BDCA-3+ mDCs demonstrated enhanced expression of CD86, CD80, and PD-L1 as compared to uninfected cells (Figure 3A). However, CD86 expression by RSV-infected BDCA-1+ mDCs was not found to be significantly different from expression by uninfected cells (Figure 3B). Exposure to UV-RSV also induced expression of CD86 and CD80 in BDCA-1+ and BDCA-3+ mDCs, but did not induce expression of PD-L1 in either subtype (Additional file 1: Figure S1).
RSV infection induces upregulation of costimulatory molecules on BDCA-1+and BDCA-3+mDCs. BDCA-1+ and BDCA-3+ mDCs were incubated in media alone or infected with RSV at a MOI=5 for 40 h. ( A ) Costimulatory molecule expression was analyzed using flow cytometry. Dashed line= uninfected cells, solid line = infected cells. Data is from one donor and is representative of 5 donors. ( B ) Bar graph represent the change in mean fluorescent intensity (MFI) of expression by infected cells over uninfected cells (mean + SEM of 5 donors). Linear data is reported on a logarithmic scale. The dotted line represents a 2 fold induction. *=statistically significant difference (p≤0.05) in expression by infected mDCs as compared to uninfected mDCs by student’s paired t-test.
DC subsets express discreet TLR profiles [13, 29], however both BDCA-1+ and BDCA-3+ mDCs have been shown to express TLR3 [13]. Activation with poly I:C upregulates the expression of costimulatory molecules on BDCA-1+ and BDCA-3+ mDCs (Additional file 2: Figure S2A-B). To characterize the strength and specificity of costimulatory molecule expression induced by RSV, the fold change in CD86, CD80, and PD-L1 expression by mDCs infected with RSV was compared to mDCs activated with poly I:C. In BDCA-1+ mDCs, PD-L1 expression was significantly greater on RSV-infected cells than poly I:C activated cells (Figure 4A); in BDCA-3+ mDCs, expression of CD86 and PD-L1 was significantly greater on RSV-infected cells than poly I:C activated cells (Figure 4B). Together, these results suggest although viral replication is not necessary for mDC activation; PD-L1 is differentially induced by RSV infection.
Comparison of costimulatory molecule expressed by mDC subsets in response to RSV and poly I:C. ( A ) BDCA-1+ and ( B ) BDCA-3+ mDCs were incubated in media alone, infected with RSV at a MOI=5, or activated with poly I:C for 40 h. Bar graphs represent the change in mean fluorescent intensity (MFI) of expression by infected cells over uninfected cells (mean + SEM of 5 donors). Linear data is reported on a logarithmic scale. The dotted line represents a 2 fold induction. *=statistically significant difference (p≤0.05) in expression by RSV-infected mDCs as compared to poly I:C-activated mDCs by student’s paired t-test.
RSV infection induces cytokine production by BDCA-1+ and BDCA-3+mDCs
The cytokines and chemokines produced by activated mDCs affect both innate and adaptive immune responses. To examine the profile of cytokines produced by primary mDC subsets in response to RSV, cytokine production by RSV-infected BDCA-1+ and BDCA-3+ mDCs was examined using a Luminex-based assay. Compared to uninfected cells of the same type, RSV-infected BDCA-1+ mDCs demonstrated significant increases in the production of IL-1β, IL-1rα, IL-6, IL-8, IL-10, IL-12, G-CSF, TNF-α, CXCL10, MCP-1, MIP-1α, MIP-1β, and RANTES (Figure 5A). In three of the six donors, IFN-γ was also produced by RSV-infected BDCA-1+ mDCs, with high levels produced by only one of the three (data not shown). The significance of these findings is unclear since with the exception of IFN-γ, the pattern of production for all other cytokines was consistent among most donors. In RSV-infected BDCA-3+ mDCs, IL-8, IL-10, IL-12, and RANTES levels were found to be significantly increased as compared to uninfected cells of the same type (Figure 5B), however for most donors, the amount of IL-12 produced by RSV-infected BDCA-3+ mDCs did not reach a 2 fold increase from uninfected cells. IFN-γ was not produced by RSV-infected BDCA-3+ mDCs in any of the six donors. Overall, RSV induced a more robust cytokine response from BDCA-1+ mDCs compared to BDCA-3+ mDCs. With the exception of IL-12 and IP-10, exposure to both RSV and UV-RSV induced cytokine production in BDCA-1+ and BDCA-3+ mDCs (data not shown) suggesting that as in Mo-DCs, [30, 31] viral replication is not necessary for mDC activation. IFN-α is a key mediator of anti-viral immunity. In a preliminary set of experiments with three donors, production of IFN-α by RSV-infected BDCA-1+ and BDCA-3+ mDCs was measured using ELISA. Neither BDCA-1+ or BDCA-3+ mDCs from any of the three donors produced detectable levels of IFN-α (data not shown). As these results coincided with previous findings in RSV-infected Mo-DCs [18], no further donors were tested.
RSV infection induces cytokine production by BDCA-1+and BDCA-3+mDCs. ( A ) BDCA-1+ and ( B ) BDCA-3+ mDCs were isolated and incubated with RSV or media for 40 hours. Cytokine and chemokine levels were measured in cell-free supernatant by multiplex assay. Data represent cytokine production in pg/ml. Box and whisker plots show the median (central bar), interquartiles (boxes), and range (whiskers) of the data from 6 donors. Linear data is reported on a logarithmic scale. *= Statistically significant (p≤0.05) difference in cytokine concentration between infected and uninfected cells as calculated by student’s paired t-test.
BDCA-1+ and BDCA-3+ mDCs produce proinflammatory cytokines in response to activation with poly I:C (Additional file 3: Figures S3A and 3B). To characterize the strength and specificity of the cytokines produced by RSV-infected BDCA-1+ and BDCA-3+ mDCs, the fold change (agonist/untreated) in cytokine production in response to RSV and poly I:C was compared for each subset. Although the cytokine profiles produced by BDCA-1+ mDCs in response to RSV and poly I:C were similar, RSV-infected BDCA-1+ mDCs did produce significantly greater amounts of IL-1rα, IL-6, IL-8, IL-10, MCP-1, MIP-1β, and TNF-α (Figure 6A). As compared to activation with poly I:C, BDCA-3+ mDCs infected with RSV produced significantly greater amounts of IL-1rα and IL-10, but decreased amounts of IL-1β, IL-8, MIP-1α, MIP-1β, and TNF-α (Figure 6B).
Comparison of cytokines produced by mDC subsets in response to RSV and poly I:C. ( A ) BDCA-1+ and ( B ) BDCA-3+ mDCs were isolated and incubated with RSV, poly I:C or media alone for 40 hours. Cytokine and chemokine levels were measured in cell-free supernatant by multiplex assay. Data represents the mean + SEM of the fold change in cytokine production by treated cells as compared to untreated cells of the same type from 5 donors. Linear data is reported on a logarithmic scale. The dotted line represents a 2 fold induction. *= Statistically significant (p≤0.05) difference in cytokine production by RSV-infected mDCs as compared to poly I:C-activated mDCs by student’s paired t-test.
IL-12 and IFN-γ promote Th1 polarization [32]. The cytokine signature associated with Th2 skewing is not as clearly defined; however along with IL-4, IL-10 and low levels of IL-12 have been identified as Th2 polarizing signals [32, 33]. Other pro-inflammatory cytokines and chemokines also regulate T cell differentiation, and IL-1β, IL-6, TNF-α, MIP-1α, and MIP-1β are reported to have important roles in promoting DC maturation and inducing Th1 responses [34–36]. To determine whether the cytokines and chemokines associated with polarization of T cell responses were differentially induced by RSV-infected BDCA-3+ and BDCA-1+ mDCs, the fold change (infected/uninfected) in production of these cytokines by each cell type was compared (Figure 7). In general the fold changes in cytokine and chemokine production were lower in BDCA-3+ mDCs compared to BDCA-1+ mDCs, which may in part be related to the slightly higher levels of cytokine production by uninfected BDCA-3+ mDCs. Compared to BDCA-3+ mDCs, RSV-infected BDCA-1+ mDC were found to produce significantly increased amounts of IL-1β, IL-6, IL-12, MIP-1α, and TNF-α; production of MIP-1β and IL-10 was not significantly different between the two subsets. Neither BDCA-1+ or BDCA-3+ mDCs were found to produce IL-4.
Comparison of cytokines produced by RSV-infected BDCA-1+and BDCA-3+mDCs. DC subsets were isolated and incubated with RSV or media for 40 hours. Cytokine and chemokine levels were measured in cell-free supernatant by multiplex assay. Data represents the mean + SEM of the fold change in cytokine production by infected cells as compared to uninfected cells of the same type from 6 donors. Linear data is reported on a logarithmic scale. The dotted line represents a 2 fold induction. *= Statistically significant (p≤0.05) difference in cytokine production between RSV-infected BDCA-1+ and BDCA-3+ mDC as calculated by students t-test.
RSV infection impairs the capacity of BDCA-1+ and BDCA-3+mDCs to stimulate T cell proliferation
BDCA-1+ and BDCA-3+ mDCs are powerful and equivalent stimulators of allogenic CD4+ T cells [13]; however, RSV-infected Mo-DCs demonstrate a decreased capacity to stimulate T-cell proliferation [17, 18]. To assess whether RSV infection affects the capacity of BDCA-1+ and BDCA-3+ mDCs to stimulate T cell proliferation, allogenic CD4+ T cells labeled with CFSE were cocultured with BDCA-1 and BDCA-3 mDCs exposed to RSV, or poly I:C for 6 days. T cell proliferation was measured using flow cytometry to examine CFSE expression by CD3+, CD4+ T cells. As compared to uninfected DCs or those activated with poly I:C, RSV-infected mDCs demonstrate a reduced capacity to stimulate the proliferation of allogenic T cells; UV inactivation of the virus restored the ability of BDCA-1+ and BDCA-3+ mDCs to stimulate T cell proliferation (Figure 8A-B).
RSV-infected BDCA-1+and BDCA-3+mDCs impair CD4+T cell proliferation. BDCA-1+ and BDCA-3+ mDC were incubated with RSV, UV-RSV, poly I:C or media for 24 hours. Cells were washed and cocultured with CFSE-labeled allogenic CD4+ T cells for 6 days, ( A ) On day 6, cells were stained with mAb against CD3 and CD4, and T cell proliferation was measured by examining CFSE expression on CD3+, CD4+ T cells. Data is from one donor and is representative of data from 3 donors. Bar graphs represent the percent of proliferating CD4+ CD3+ T cells after 6 days in coculture with untreated or treated (B) BDCA-1+ and (C) BDCA-3+ mDCs. Data represents the mean + SEM of the percent of proliferating T cells from 3 donors. *= Statistically significant (p≤0.05) difference in the percent of proliferating T cells after coculture with infected and uninfected cells as calculated by students paired t-test.
Discussion
In this study, we examined the effect of RSV infection on primary human mDC subsets isolated from peripheral blood. To ensure purity of the specific mDC populations among donors, BDCA-1+ and BDCA-3+ mDCs were isolated using multicolor FACs sorting with parameters similar to those previously published [13]. This method allowed us to consistently obtain sufficient numbers of both populations with purity ≥95% for all donors. Similar to Mo-DCs [17, 18], we demonstrate that primary mDC subsets are susceptible to infection with RSV. Consistent with previous reports [25], BDCA-1+ and BDCA-3+ mDCs show similar rates of RSV infection. While mDC activation is not dependent on viral replication, we demonstrate that RSV infection induces a distinct pattern of costimulatory molecule expression and cytokine production by BDCA-1+ and BDCA-3+ mDCs, and impairs their ability to stimulate T cell proliferation.
Enhanced expression of CD86, CD80, and PD-L1 on RSV-infected mDCs coincides with the costimulatory molecule expression on RSV-infected Mo-DCs and murine lung mDCs which have an impaired capacity to stimulate T cell proliferation [18, 19]. These findings suggest that the expression of inhibitory molecules by infected mDCs may contribute to their decreased capacity to stimulate T cell activation. As CD80 is a highly effective ligand for CTLA-4 on activated T cells [37], upregulation of CD80 on BDCA-1+ and BDCA-3+ mDCs provides a possible mechanism by which RSV could inhibit T cell proliferation. CD86 seems to be more important in CD28 interactions, and in Tregs, CD28 activation provides critical signals needed for proliferation and survival [38, 39], thus providing an additional mechanism for the suppression of reactive T cell responses. Our findings of significant levels of CD86 induction by RSV-infected BDCA-3+ mDCs may then indicate a differential role for BDCA-1+ and BDCA-3+ mDCs in Treg homeostasis during RSV infection. However, it is likely the relative expression levels of CD80 and CD86 on mDCs dictates the balance between stimulatory and inhibitory outcomes and work in conjunction to regulate T cell proliferation. The differential expression of PD-L1 by RSV-infected BDCA-1+ and BDCA-3+ mDCs suggests another mechanism by which RSV infection could impair the ability of mDCs to stimulate T cell proliferation as seen in mice [19].
The cytokine milieu present at the time of TCR activation is crucial in determining the outcome of T cell responses, and DC-derived cytokines and chemokines are at the center of a complex network of cells that regulate these signals. We found that RSV-infected BDCA-1+ mDC produced a profile of cytokines and chemokines associated with pro-inflammatory responses, whereas BDCA-3+ mDCs did not. Whether the differences in the cytokine profiles produced by RSV-infected BDCA-1+ and BDCA-3+ mDCs are due to inherent functional differences purported to exist between the subsets, or represents differences in the way RSV interacts with each mDC subtype is unclear. Activation with poly I:C has been shown to induce the production of pro-inflammatory cytokines from both BDCA-1+ and BDCA-3+ mDCs, as well as the increased production of IL-12(p70) by BDCA-3+ mDCs when activated with a cocktail of poly I:C and additional activation signals [13]. However, in contrast to purified toll like receptor agonists, viral pathogens likely activate multiple signaling pathways that lead to alternative patterns of cytokine expression by each cell type. Our findings of IL-12(p70) production by infected BDCA-1+ and not BDCA-3+ mDCs, may then represent responses specific to infection with RSV. Findings that as compared to activation with poly I;C, RSV infected BDCA-1+ mDCs produced greater amounts of proinflammatory and immunoregulatory cytokines, whereas RSV-infected BDCA-3+ mDCs produced decreased amounts of proinflammatory cytokines and increased amounts of immunoregulatory cytokines, provides additional evidence for RSV-specific responses. However, the TLRs governing RSV recognition, and their subsequent responses, in primary mDC subsets have yet to be defined. Thus, we cannot exclude the possibility that the differences in cytokine expression between RSV and poly I:C treated DCs are related to differences in the strength or quality of TLR activation by RSV, rather than from a virus-specific effect on cell activation. Further work is needed to determine the cytokine profiles produced by BDCA-1+ and BDCA-3+ mDCs in response to infection with other viral pathogens.
The balance of pro-inflammatory cytokines, in particular IL-12, produced by RSV-infected BDCA-1+ mDCs suggests that BDCA-1+ mDCs may promote Th1 responses, whereas RSV-infected BDCA-3+ mDCs, which produce IL-10 in the setting of low IL-12, may skew naïve T cells away from Th1 with possible polarization towards Th2 responses. Although mDCs were not found to produce IL-4, RSV-infected BDCA-1+ mDCs produced a number of chemokines implicated in the recruitment of cells known to produce IL-4 [40]. The potentially divergent roles of RSV-infected BDCA-1+ and BDCA-3+ mDCs in the polarization of T cell responses may explain why despite findings of Th2 responses in vivo[7, 41], in vitro studies have not demonstrated the ability of RSV-infected Mo-DCs to bias naïve T cells towards Th2 responses [6, 17, 42]. Of note, our findings of IL-12 production by BDCA-1+ mDCs and the lack of significant production of G-CSF, MCP-1 or MIP-1α by BDCA-3+ mDCs are in contrast to a recently published report by Johnson et al. examining the impact of RSV infection on the maturation and cytokine response of primary human mDCs isolated using sequential immunomagnetic selection alone [25]. These differences may be related to their use of a recombinant RSV strain, as well as differences in the methodologies used to isolate and culture mDC subsets. In prior reports, IL-12 and IFN-γ production by Mo-DCs [18] and cord-blood derived DCs [30, 31] infected with non-recombinant RSV strains has been demonstrated.
Interestingly, both BDCA-1+ and BDCA-3+ mDCs produced IL-10 in response to RSV. DC-derived IL-10 is shown to act in an autocrine fashion to inhibit pro-inflammatory cytokine production and impair the capacity of DCs to foster Th1 responses [43]. IL-10 produced by RSV-infected BDCA-1+ and BDCA-3+ mDCs may then also contribute to the impaired T cell responses seen in vivo. In prior reports using RSV-infected Mo-DCs, adding IL-10 blocking antibody did not restore T cell proliferation or function [17]. However, in vitro models of E. coli infection demonstrating that infected BDCA-1+ mDCs, but not Mo-DCs, impair T cell proliferation in an IL-10 dependent manner [44], provide further evidence that findings in Mo-DCs may not reflect the function of primary mDCs. IL-10 has also been used in vitro to generate tolerogenic DCs that are functionally anergic, and capable of generating and expanding Tregs [45, 46]. In vivo activation of pathways by pathogens that promote IL-10 production by DCs could therefore induce functionally tolerogenic DCs [47]. Tolerogenic DCs are characterized by decreased production of pro-inflammatory cytokines and increased production of IL-10 [46]. Similar findings in RSV-infected BDCA-3+ mDCs suggest that they may be functionally tolerogenic. Although RSV-infected BDCA-1+ mDCs also produced IL-10, the concomitant induction of IL-12 and other pro-inflammatory cytokines suggests a non-tolerogenic phenotype, which may explain why RSV-infected Mo-DCs were not found to generate T cells with suppressive properties [17]. Studies in murine models of acute RSV infection [48, 49] indicate that Tregs play an important role in determining the balance between effective antiviral immunity and controlling harmful immunopathology in the host response against RSV. Our findings suggest a possible mechanism for homeostatic regulation of the Treg compartment by BDCA-3+ mDCs during RSV infection.
Similar to studies using Mo-DCs and murine DCs [17–19], RSV infection of BDCA-1+ and BDCA-3+ mDCs impairs their ability to stimulate CD4+ T cell proliferation in a mixed lymphocyte reaction. The lack of inhibition mDCs exposed to UV-inactivated RSV suggests that viral replication is required to trigger these events. The mechanism underlying this inhibitory effect is unknown; however, our findings of differential expression PD-L1 and IL-10 by RSV-infected mDCs suggest that RSV modulates the function of BDCA-1+ and BDCA-3+ mDCs. Although we did consider that the loss of stimulatory function may be due to reduced viability of infected cells, there was no difference in cell viability between uninfected or RSV-infected mDCs.
To our knowledge, this is one of the first studies to examine the functional responses of highly purified mDC subsets to infection with RSV. We recognize that using a reductionist in vitro model does not represent the interactions between the complex network of mDC subsets in the lungs and blood during natural infection and a suitable human model to further study these questions is needed. Furthermore, although RSV primarily affects young children, mDC subsets were isolated from the peripheral blood of healthy adults due to the feasibility of obtaining sufficient volumes of blood from pediatric populations. It is not well known whether age dependent differences in mDC subset function exist [50]. However, despite these limitations, this study provides novel evidence for a virus-specific and subset specific-effect of RSV infection on the functional response of BDCA-1+ and BDCA-3+ mDCs.
Conclusions
It is not known what type of mDCs are present in the lungs during natural RSV infection, or how host genetic and environmental factors affect the downstream function of BDCA-1+ and BDCA-3+ mDCs interacting with virus. However, findings of increased frequencies of BDCA-3+ mDCs in the peripheral blood of atopic asthmatics [51] suggest that the balance and function of individual mDC subsets during RSV infection plays a crucial role in determining the short- and long-term sequela of disease. Defining the mechanisms by which RSV is able to modulate virus-specific immune responses will provide important new insights into the immunopathogenesis of RSV infection and the role mDC subsets play in the host immune response against pathogens as a whole.
Abbreviations
- APC:
-
Allophycocyanin
- BDCA:
-
Blood Dendritic Cell Antigen
- CD:
-
Cluster of differentiation
- DCs:
-
Dendritic cells
- EDTA:
-
Ethylenediaminetetraacetic acid
- FACS:
-
Fluorescence Activated Cell Sorting
- FBS:
-
Fetal bovine serum
- FITC:
-
Fluorescein isothiocyanate
- FSC:
-
Forward scatter
- GM-CSF:
-
Granulocyte macrophage colony-stimulating factor
- HLA:
-
Human leukocyte antigen
- IFN:
-
Interferon
- IL:
-
Interleukin
- mAb:
-
Monoclonal antibody
- MACS:
-
Magnetic Activated Cell Sorting
- mDCs:
-
Myeloid dendritic cells
- MLR:
-
Mixed lymphocyte reaction
- Mo-DCs:
-
Monocyte derived dendritic cells
- MOI:
-
Multiplicity of infection
- PBMC:
-
Peripheral blood mononuclear cells
- pDCs:
-
Plasmacytoid dendritic cells
- PE:
-
Phycoerythrin
- Per Cp-Cy5.5:
-
Peridinin Chlorophyll Protein Complex conjugated with cyanine dye
- RSV:
-
Respiratory syncytial virus
- SSC:
-
Side scatter
- SEM:
-
Standard error of the mean
- Th:
-
T helper cell
- TLR:
-
Toll-like Receptor
- Treg:
-
T regulatory cells.
References
Glezen WP, Taber LH, Frank AL, Kasel JA: Risk of primary infection and reinfection with respiratory syncytial virus. Am J Dis Child. 1986, 140: 543-546.
Dowell SF, Anderson LJ, Gary HE, Erdman DD, Plouffe JF, File TM, Marston BJ, Breiman RF: Respiratory syncytial virus is an important cause of community-acquired lower respiratory infection among hospitalized adults. J Infect Dis. 1996, 174: 456-462. 10.1093/infdis/174.3.456.
Sigurs N, Bjarnason R, Sigurbergsson F, Kjellman B: Respiratory syncytial virus bronchiolitis in infancy is an important risk factor for asthma and allergy at age 7. Am J Respir Crit Care Med. 2000, 161: 1501-1507. 10.1164/ajrccm.161.5.9906076.
Tripp R, Moore D, Barskey A, Jones L, Moscatiello C, Keyserling H, Anderson LJ: Peripheral blood mononuclear cells from infants hospitalized because of respiratory syncytial virus infection express T helper-1 and T helper-2 cytokines and CC chemokine messenger RNA. J Infect Dis. 2002, 185: 1388-1394. 10.1086/340505.
Welliver TP, Garofalo RP, Hosakote Y, Hintz KH, Avendano L, Sanchez K, Velozo L, Jafri H, Chavez-Bueno S, Ogra PL, et al: Severe human lower respiratory tract illness caused by respiratory syncytial virus and influenza virus is characterized by the absence of pulmonary cytotoxic lymphocyte responses. J Infect Dis. 2007, 195: 1126-1136. 10.1086/512615.
Munir S, Hillyer P, Le Nouen C, Buchholz UJ, Rabin RL, Collins PL, Bukreyev A: Respiratory syncytial virus interferon antagonist NS1 protein suppresses and skews the human T lymphocyte response. PLoS Pathog. 2011, 7: e1001336-e1001336. 10.1371/journal.ppat.1001336.
Sung RY, Hui SH, Wong CK, Lam CW, Yin J: A comparison of cytokine responses in respiratory syncytial virus and influenza A infections in infants. Eur J Pediatr. 2001, 160: 117-122. 10.1007/s004310000676.
McKenna K, Beignon A-S, Bhardwaj N: Plasmacytoid dendritic cells: linking innate and adaptive immunity. J Virol. 2005, 79: 17-27. 10.1128/JVI.79.1.17-27.2005.
Vermaelen K, Pauwels R: Pulmonary dendritic cells. Am J Respir Crit Care Med. 2005, 172: 530-551. 10.1164/rccm.200410-1384SO.
Demedts IK, Brusselle GG, Vermaelen KY, Pauwels R: Identification and characterization of human pulmonary dendritic cells. Am J Respir Cell Mol Biol. 2005, 32: 177-184. 10.1165/rcmb.2004-0279OC.
Demedts IK, Bracke KR, Maes T, Joos GF, Brusselle GG: Different roles for human lung dendritic cell subsets in pulmonary immune defense mechanisms. Am J Respir Cell Mol Biol. 2006, 35: 387-393. 10.1165/rcmb.2005-0382OC.
Bachem A, Guttler S, Hartung E, Ebstein F, Schaefer M, Tannert A, Salama A, Movassaghi K, Opitz C, Mages HW, et al: Superior antigen cross-presentation and XCR1 expression define human CD11c+CD141+ cells as homologues of mouse CD8+ dendritic cells. J Exp Med. 2010, 207: 1273-1281. 10.1084/jem.20100348.
Jongbloed SL, Kassianos AJ, McDonald KJ, Clark GJ, Ju X, Angel CE, Chen C-JJ, Dunbar PR, Wadley RB, Jeet V, et al: Human CD141+ (BDCA-3)+ dendritic cells (DCs) represent a unique myeloid DC subset that cross-presents necrotic cell antigens. J Exp Med. 2010, 207: 1247-1260. 10.1084/jem.20092140.
Robbins SH, Walzer T, Dembele D, Thibault C, Defays A, Bessou G, Xu H, Vivier E, Sellars M, Pierre P, et al: Novel insights into the relationships between dendritic cell subsets in human and mouse revealed by genome-wide expression profiling. Genome Biol. 2008, 9: R17-R17. 10.1186/gb-2008-9-1-r17.
Haniffa M, Shin A, Bigley V, McGovern N, Teo P, See P, Wasan PS, Wang X-N, Malinarich F, Malleret B, et al: Human tissues contain CD141hi cross-presenting dendritic cells with functional homology to mouse CD103+ nonlymphoid dendritic cells. Immunity. 2012, 37: 60-73. 10.1016/j.immuni.2012.04.012.
Gill M, Palucka AK, Barton T, Ghaffar F, Jafri H, Banchereau J, Ramilo O: Mobilization of plasmacytoid and myeloid dendritic cells to mucosal sites in children with respiratory syncytial virus and other viral respiratory infections. J Infect Dis. 2005, 191: 1105-1115. 10.1086/428589.
De Graaff PM, De Jong EC, Van Capel TM, Van Dijk ME, Roholl PJM, Boes J, Luytjes W, Kimpen JLL, Van Bleek GM: Respiratory syncytial virus infection of monocyte-derived dendritic cells decreases their capacity to activate CD4 T cells. J Immunol. 2005, 175: 5904-5911.
Guerrero-Plata A, Casola A, Suarez G, Yu X, Spetch L, Peeples ME, Garofalo RP: Differential response of dendritic cells to human metapneumovirus and respiratory syncytial virus. Am J Respir Cell Mol Biol. 2006, 34: 320-329. 10.1165/rcmb.2005-0287OC.
Guerrero-Plata A, Kolli D, Hong C, Casola A, Garofalo RP: Subversion of pulmonary dendritic cell function by paramyxovirus infections. J Immunol. 2009, 182: 3072-3083. 10.4049/jimmunol.0802262.
Sallusto F, Lanzavecchia A: Efficient presentation of soluble antigen by cultured human dendritic cells is maintained by granulocyte/macrophage colony-stimulating factor plus interleukin 4 and downregulated by tumor necrosis factor alpha. J Exp Med. 1994, 179: 1109-1118. 10.1084/jem.179.4.1109.
Vuckovic S, Fearnley DB, Mannering SI, Dekker J, Whyte LF, Hart DN: Generation of CMRF-44+ monocyte-derived dendritic cells: insights into phenotype and function. Exp Hematol. 1998, 26: 1255-1264.
Thurner B, Roder C, Dieckmann D, Heuer M, Kruse M, Glaser A, Keikavoussi P, Kampgen E, Bender A, Schuler G: Generation of large numbers of fully mature and stable dendritic cells from leukapheresis products for clinical application. J Immunol Methods. 1999, 223: 1-15. 10.1016/S0022-1759(98)00208-7.
Osugi Y, Vuckovic S, Hart DN: Myeloid blood CD11c(+) dendritic cells and monocyte-derived dendritic cells differ in their ability to stimulate T lymphocytes. Blood. 2002, 100: 2858-2866. 10.1182/blood.V100.8.2858.
MacDonald KPA, Munster DJ, Clark GJ, Dzionek A, Schmitz J, Hart DNJ: Characterization of human blood dendritic cell subsets. Blood. 2002, 100: 4512-4520. 10.1182/blood-2001-11-0097.
Johnson TR, Johnson CN, Corbett KS, Edwards GC, Graham BS: Primary human mDC1, mDC2, and pDC dendritic cells are differentially infected and activated by respiratory syncytial virus. PLoS One. 2011, 6: e16458-e16458. 10.1371/journal.pone.0016458.
Probst HC, McCoy K, Okazaki T, Honjo T, van den Broek M: Resting dendritic cells induce peripheral CD8+ T cell tolerance through PD-1 and CTLA-4. Nat Immunol. 2005, 6: 280-286.
Beswick EJ, Pinchuk IV, Das S, Powell DW, Reyes VE: Expression of the programmed death ligand 1, B7-H1, on gastric epithelial cells after Helicobacter pylori exposure promotes development of CD4+ CD25+ FoxP3+ regulatory T cells. Infect Immun. 2007, 75: 4334-4341. 10.1128/IAI.00553-07.
Krupnick AS, Gelman AE, Barchet W, Richardson S, Kreisel FH, Turka LA, Colonna M, Patterson GA, Kreisel D: Murine vascular endothelium activates and induces the generation of allogeneic CD4+25+Foxp3+ regulatory T cells. J Immunol. 2005, 175: 6265-6270.
Pulendran B: Variegation of the immune response with dendritic cells and pathogen recognition receptors. J Immunol. 2005, 174: 2457-2465.
Bartz H, Buning-Pfaue F, Turkel O, Schauer U: Respiratory syncytial virus induces prostaglandin E2, IL-10 and IL-11 generation in antigen presenting cells. Clin Exp Immunol. 2002, 129: 438-445. 10.1046/j.1365-2249.2002.01927.x.
Chi B, Dickensheets HL, Spann KM, Alston MA, Luongo C, Dumoutier L, Huang J, Renauld JC, Kotenko SV, Roederer M, et al: Alpha and lambda interferon together mediate suppression of CD4 T cells induced by respiratory syncytial virus. J Virol. 2006, 80: 5032-5040. 10.1128/JVI.80.10.5032-5040.2006.
De Jong EC, Smits HH, Kapsenberg ML: Dendritic cell-mediated T cell polarization. Springer Semin Immunopathol. 2005, 26: 289-307. 10.1007/s00281-004-0167-1.
Benwell RK, Hruska JE, Fritsche KL, Lee DR: Double stranded RNA- relative to other TLR ligand-activated dendritic cells induce extremely polarized human Th1 responses. Cell Immunol. 2010, 264: 119-126. 10.1016/j.cellimm.2010.05.008.
Sa L, Cyster JG: Chemokines as regulators of T cell differentiation. Nat Immunol. 2001, 2: 102-107. 10.1038/84205.
Sporri R, Reis e Sousa C: Inflammatory mediators are insufficient for full dendritic cell activation and promote expansion of CD4+ T cell populations lacking helper function. Nat Immunol. 2005, 6: 163-170.
Rajkovic I, Dragicevic A, Vasilijic S, Bozic B, Dzopalic T, Tomic S, Majstorovic I, Vucevic D, Djokic J, Balint B, Colic M: Differences in T-helper polarizing capability between human monocyte-derived dendritic cells and monocyte-derived Langerhans'-like cells. Immunology. 2011, 132: 217-225. 10.1111/j.1365-2567.2010.03356.x.
Collins AV, Brodie DW, Gilbert RJ, Iaboni A, Manso-Sancho R, Walse B, Stuart DI, van der Merwe PA, Davis SJ: The interaction properties of costimulatory molecules revisited. Immunity. 2002, 17: 201-210. 10.1016/S1074-7613(02)00362-X.
Zheng Y, Manzotti CN, Liu M, Burke F, Mead KI, Sansom DM: CD86 and CD80 differentially modulate the suppressive function of human regulatory T cells. J Immunol. 2004, 172: 2778-2784.
Tang Q, Henriksen KJ, Boden EK, Tooley AJ, Ye J, Subudhi SK, Zheng XX, Strom TB, Bluestone JA: Cutting edge: CD28 controls peripheral homeostasis of CD4+CD25+ regulatory T cells. J Immunol. 2003, 171: 3348-3352.
Commins SP, Borish L, Steinke JW: Immunologic messenger molecules: cytokines, interferons, and chemokines. J Allergy Clin Immunol. 2010, 125: S53-S72. 10.1016/j.jaci.2009.07.008.
Garofalo RP, Patti J, Hintz K, Hill V, Ogra PL, Welliver RC: Macrophage inflammatory protein-1alpha (not T helper type 2 cytokines) is associated with severe forms of respiratory syncytial virus bronchiolitis. J Infect Dis. 2001, 184: 393-399. 10.1086/322788.
Le Nouen C, Hillyer P, Munir S, Winter CC, McCarty T, Bukreyev A, Collins PL, Rabin RL, Buchholz UJ: Effects of human respiratory syncytial virus, metapneumovirus, parainfluenza virus 3 and influenza virus on CD4+ T cell activation by dendritic cells. PLoS One. 2010, 5: e15017-e15017. 10.1371/journal.pone.0015017.
Corinti S, Albanesi C, La Sala A, Pastore S, Girolomoni G: Regulatory activity of autocrine IL-10 on dendritic cell functions. J Immunol. 2001, 166: 4312-4318.
Kassianos AJ, Hardy MY, Ju X, Vijayan D, Ding Y, Vulink AJ, McDonald KJ, Jongbloed SL, Wadley RB, Wells C, et al: Human CD1c (BDCA-1)+ myeloid dendritic cells secrete IL-10 and display an immuno-regulatory phenotype and function in response to Escherichia coli. Eur J Immunol. 2012, 42: 1512-1522. 10.1002/eji.201142098.
Gregori S, Tomasoni D, Pacciani V, Scirpoli M, Battaglia M, Magnani CF, Hauben E, Roncarolo MG: Differentiation of type 1 T regulatory cells (Tr1) by tolerogenic DC-10 requires the IL-10-dependent ILT4/HLA-G pathway. Blood. 2010, 116: 935-944. 10.1182/blood-2009-07-234872.
Boks MA, Kager-Groenland JR, Haasjes MS, Zwaginga JJ, Van Ham SM, Ten Brinke A: IL-10-generated tolerogenic dendritic cells are optimal for functional regulatory T cell induction–a comparative study of human clinical-applicable DC. Clin Immunol. 2012, 142: 332-342. 10.1016/j.clim.2011.11.011.
McGuirk P, McCann C, Mills KH: Pathogen-specific T regulatory 1 cells induced in the respiratory tract by a bacterial molecule that stimulates interleukin 10 production by dendritic cells: a novel strategy for evasion of protective T helper type 1 responses by Bordetella pertussis. J Exp Med. 2002, 195: 221-231. 10.1084/jem.20011288.
Fulton RB, Meyerholz DK, Varga SM: Foxp3+ CD4 regulatory T cells limit pulmonary immunopathology by modulating the CD8 T cell response during respiratory syncytial virus infection. J Immunol. 2010, 185: 2382-2392. 10.4049/jimmunol.1000423.
Loebbermann J, Thornton H, Durant L, Sparwasser T, Webster KE, Sprent J, Culley FJ, Johansson C, Openshaw PJ: Regulatory T cells expressing granzyme B play a critical role in controlling lung inflammation during acute viral infection. Mucosal Immunol. 2012, 5: 161-172. 10.1038/mi.2011.62.
Jyonouchi H, Cui C, Geng L, Yin Z, Fitzgerald-Bocarsly P: Age-dependent changes in peripheral blood dendritic cell subsets in normal children and children with specific polysaccharide antibody deficiency (SPAD). Eur J Pediatr. 2010, 169: 1233-1239. 10.1007/s00431-010-1210-y.
Yerkovich ST, Roponen M, Smith ME, McKenna K, Bosco A, Subrata LS, Mamessier E, Wikstrom ME, Le Souef P, Sly PD, et al: Allergen-enhanced thrombomodulin (blood dendritic cell antigen 3, CD141) expression on dendritic cells is associated with a TH2-skewed immune response. J Allergy Clin Immunol. 2009, 123: 209-216. 10.1016/j.jaci.2008.09.009. e204
Acknowledgment
The authors would like to thank Mark Griffin from the Flow Cytometry Core for his assistance with cell sorting analysis, Dr. Daniel Freeman from the Biostatics and Design Resource of UTMB’s Institute for Translational Sciences for his assistance with the statistical analysis, as well as Dr. Victor Reyes from the Department of Pediatrics, Division of Clinical and Experimental Immunology and Infectious Diseases and Dr. William Calhoun from the Department of Internal Medicine, Divisions of Allergy and Immunology and Pulmonary and Critical Care for their critical review of the manuscript. This project was conducted with partial support of the Institute for Translational Sciences at the University of Texas Medical Branch, including a pilot grant (to RPG) and a KL2 Career Development Award (to MRG) as part of a Clinical and Translational Science Award (UL1TR000071, KL2TR000072, PI: Brasier AB) from the National Center for Advancing Translational Sciences, and by grant HV28184 from the National Heart, Lung and Blood Institute (PI: Kurosky A).
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
The authors declare that they have no competing interests.
Authors’ contributions
MRG, DK and RPG designed the research, MRG and DK performed the research, MRG and DK analyzed the data, and MRG, DK, and RPG wrote the manuscript. All authors read and approved the final manuscript.
Electronic supplementary material
12931_2013_1384_MOESM1_ESM.tiff
Additional file 1: Figure S1: Costimulatory expression by mDC subsets exposed to UV-inactivated RSV. BDCA-1+ and BDCA-3+ mDCs were incubated in media alone, or exposed to RSV and UV-inactivated RSV (non-replicating virus) at a MOI=5 for 40 h. Costimulatory molecule expression was analyzed using flow cytometry. Dashed line= uninfected cells, solid line = RSV-infected cells, dotted line= UV-RSV exposed cells. (TIFF 470 KB)
12931_2013_1384_MOESM2_ESM.pdf
Additional file 2: Figure S2: Costimulatory molecule expression by mDCs activated with poly I:C. (A) BDCA-1+ and (B) BDCA-3+ mDCs were isolated and incubated with poly I:C or media for 40 hours. Data represent the mean fluorescent intensity (MFI) of costimulatory molecule expression (mean + SEM of 5 donors) on a linear scale. *=statistically significant difference (p≤0.05) in expression by poly I:C-activated mDCs as compared to untreated mDCs by student’s paired t-test. (PDF 32 KB)
12931_2013_1384_MOESM3_ESM.pdf
Additional file 3: Figure S3: Cytokine production by mDCs activated with poly I:C. (A) BDCA-1+ and (B) BDCA-3+ mDCs were isolated and incubated with poly I:C or media for 40 hours. Cytokine and chemokine levels were measured in cell-free supernatant by multiplex assay. Data represent cytokine production in pg/ml. Box and whisker plots show the median (central bar), interquartiles (boxes), and range (whiskers) of the data from 5 donors. Linear data is reported on a logarithmic scale. *= Statistically significant (p≤0.05) difference in cytokine concentration between treated and untreated cells as calculated by student’s paired t-test. (PDF 52 KB)
Authors’ original submitted files for images
Below are the links to the authors’ original submitted files for images.
Rights and permissions
This article is published under license to BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Gupta, M.R., Kolli, D. & Garofalo, R.P. Differential response of BDCA-1+ and BDCA-3+myeloid dendritic cells to respiratory syncytial virus infection. Respir Res 14, 71 (2013). https://doi.org/10.1186/1465-9921-14-71
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1465-9921-14-71