Abstract
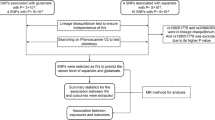
Exposures to copper have become a health concern. We aim to explore the broad clinical effects of blood copper concentrations. A total of 376,346 Caucasian subjects were enrolled. We performed a Mendelian randomization and phenome-wide association study (MR-PheWAS) to evaluate the causal association between copper and a wide range of outcomes in UK Biobank, and we constructed a protein–protein interaction network. We found association between blood copper concentrations and five diseases in the overall population and nine diseases in male. MR analysis implicated a causal role of blood copper in five diseases (overall population), including prostate cancer (OR = 0.87, 95% CI 0.77–0.98), malignant and unknown neoplasms of the brain and nervous system (OR = 0.58, 95% CI 0.38–0.89), and hypertension (OR = 0.94, 95% CI 0.90–0.98), essential hypertension (OR = 0.94, 95% CI 0.90–0.98) and cancer of brain and nervous system (OR = 0.63, 95% CI 0.41–0.98). For male, except for dysphagia being newly associated with blood copper (OR = 1.39, 95% CI 1.18–1.63), other MR results were consistent with the overall population. In addition, the PPI network showed possible relationship between blood copper and four outcomes, namely brain cancer, prostate cancer, hypertension, and dysphagia. Blood copper may have causal association with prostate cancer, malignant and unknown neoplasms of the brain and nervous system, hypertension, and dysphagia. Considering that copper is modifiable, exploring whether regulation of copper levels can be used to optimize health outcomes might have public health importance.


Similar content being viewed by others
Availability of data and material
The genetic and phenotypic UK Biobank data are available upon application from the UK Biobank (www.ukbiobank.ac.uk/).
Code availability
The code that support the findings of this study are available from the corresponding author upon reasonable request.
References
Akanle OA, Akintanmide A, Durosinmi MA, Oluwole AF, Spyrou NM (1999) Elemental analysis of blood of Nigerian hypertensive subjects. Biol Trace Elem Res 71–72:611–616. https://doi.org/10.1007/bf02784250
Bergomi M, Rovesti S, Vinceti M, Vivoli R, Caselgrandi E, Vivoli G (1997) Zinc and copper status and blood pressure. J Trace Elements Med Biol Organ Soc Miner Trace Elements (GMS) 11:166–169. https://doi.org/10.1016/s0946-672x(97)80047-8
Burgess S, Scott RA, Timpson NJ, Davey Smith G, Thompson SG (2015) Using published data in Mendelian randomization: a blueprint for efficient identification of causal risk factors. Eur J Epidemiol 30:543–552. https://doi.org/10.1007/s10654-015-0011-z
Burgess S, Bowden J, Fall T, Ingelsson E, Thompson SG (2017) Sensitivity analyses for robust causal inference from mendelian randomization analyses with multiple genetic variants. Epidemiology 28:30–42. https://doi.org/10.1097/ede.0000000000000559
Bycroft C, Freeman C, Petkova D, Band G, Elliott LT, Sharp K, Motyer A, Vukcevic D, Delaneau O et al (2018) The UK Biobank resource with deep phenotyping and genomic data. Nature 562:203–209. https://doi.org/10.1038/s41586-018-0579-z
Canatan H, Bakan I, Akbulut M, Halifeoglu I, Cikim G, Baydas G, Kilic N (2004) Relationship among levels of leptin and zinc, copper, and zinc/copper ratio in plasma of patients with essential hypertension and healthy normotensive subjects. Biol Trace Elem Res 100:117–123. https://doi.org/10.1385/bter:100:2:117
Cater MA, Pearson HB, Wolyniec K, Klaver P, Bilandzic M, Paterson BM, Bush AI, Humbert PO, La Fontaine S et al (2013) Increasing intracellular bioavailable copper selectively targets prostate cancer cells. ACS Chem Biol 8:1621–1631. https://doi.org/10.1021/cb400198p
Chen F, Vallyathan V, Castranova V, Shi X (2001) Cell apoptosis induced by carcinogenic metals. Mol Cell Biochem 222:183–188. https://doi.org/10.1023/A:1017970330982
Cheng WW, Zhu Q, Zhang HY (2019) Mineral nutrition and the risk of chronic diseases: a mendelian randomization study. Nutrients. https://doi.org/10.3390/nu11020378
Chowdhury R, Ramond A, O’Keeffe LM, Shahzad S, Kunutsor SK, Muka T, Gregson J, Willeit P, Warnakula S et al (2018) Environmental toxic metal contaminants and risk of cardiovascular disease: systematic review and meta-analysis. BMJ (clin Res Ed) 362:k3310. https://doi.org/10.1136/bmj.k3310
Członkowska A, Litwin T, Chabik G (2017) Wilson disease: neurologic features. Handb Clin Neurol 142:101–119. https://doi.org/10.1016/b978-0-444-63625-6.00010-0
Czlonkowska A, Litwin T, Dusek P, Ferenci P, Lutsenko S, Medici V, Rybakowski JK, Weiss KH, Schilsky ML (2018) Wilson disease. Nat Rev Dis Primers 4:21. https://doi.org/10.1038/s41572-018-0018-3
da Silva-Júnior FP, Carrasco AE, da Silva Mendes AM, Lopes AJ, Nobre ESMA, de Bruin VM (2008) Swallowing dysfunction in Wilson’s disease: a scintigraphic study. Neurogastroenterol Motil 20:285–290. https://doi.org/10.1111/j.1365-2982.2007.01036.x
Denny JC, Bastarache L, Ritchie MD, Carroll RJ, Zink R, Mosley JD, Field JR, Pulley JM, Ramirez AH et al (2013) Systematic comparison of phenome-wide association study of electronic medical record data and genome-wide association study data. Nat Biotechnol 31:1102–1110. https://doi.org/10.1038/nbt.2749
Dusek P, Litwin T, Członkowska A (2019) Neurologic impairment in Wilson disease. Ann Transl Med 7:S64. https://doi.org/10.21037/atm.2019.02.43
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ (clin Res Ed) 315:629–634. https://doi.org/10.1136/bmj.315.7109.629
Evans DM, Zhu G, Dy V, Heath AC, Madden PA, Kemp JP, McMahon G, St Pourcain B, Timpson NJ et al (2013) Genome-wide association study identifies loci affecting blood copper, selenium and zinc. Hum Mol Genet 22:3998–4006. https://doi.org/10.1093/hmg/ddt239
Finney L, Vogt S, Fukai T, Glesne D (2009) Copper and angiogenesis: unravelling a relationship key to cancer progression. Clin Exp Pharmacol Physiol 36:88–94. https://doi.org/10.1111/j.1440-1681.2008.04969.x
Gill D, Benyamin B, Moore LSP, Monori G, Zhou A, Koskeridis F, Evangelou E, Laffan M, Walker AP et al (2019) Associations of genetically determined iron status across the phenome: A mendelian randomization study. PLoS Med 16:e1002833. https://doi.org/10.1371/journal.pmed.1002833
Guo Y, Lu Y, Jin H (2020) Appraising the role of circulating concentrations of micro-nutrients in epithelial ovarian cancer risk: a Mendelian randomization analysis. Sci Rep 10:7356. https://doi.org/10.1038/s41598-020-63909-5
Guzel S, Guzel EC, Kucukyalcin V, Kiziler AR, Cavusoglu C, Gulyasar T, Cinemre H, Aydemir B (2018) Midkine levels and its relationship with atherosclerotic risk factors in essential hypertensive patients. Niger J Clin Pract 21:894–900. https://doi.org/10.4103/njcp.njcp_309_17
Huang L, Li L, Luo X, Huang S, Hou Q, Ge X, Lv Y, Mo Z, Yang X (2019) The association between serum iron status and risk of asthma: a 2-sample Mendelian randomization study in descendants of Europeans. Am J Clin Nutr 110:959–968. https://doi.org/10.1093/ajcn/nqz162
Järup L (2003) Hazards of heavy metal contamination. Br Med Bull 68:167–182. https://doi.org/10.1093/bmb/ldg032
Kedzierska K, Bober J, Ciechanowski K, Gołembiewska E, Kwiatkowska E, Noceń I, Dołegowska B, Dutkiewicz G, Chlubek D (2005) Copper modifies the activity of sodium-transporting systems in erythrocyte membrane in patients with essential hypertension. Biol Trace Elem Res 107:21–32. https://doi.org/10.1385/bter:107:1:021
Khan SN, Rahman MA, Samad A (1984) Trace elements in serum from Pakistani patients with acute and chronic ischemic heart disease and hypertension. Clin Chem 30:644–648. https://doi.org/10.1093/clinchem/30.5.644
Klotz LO, Kröncke KD, Buchczyk DP, Sies H (2003) Role of copper, zinc, selenium and tellurium in the cellular defense against oxidative and nitrosative stress. J Nutr 133:1448s-s1451. https://doi.org/10.1093/jn/133.5.1448S
Kodali HP, Pavilonis BT, Schooling CM (2018) Effects of copper and zinc on ischemic heart disease and myocardial infarction: a Mendelian randomization study. Am J Clin Nutr 108:237–242. https://doi.org/10.1093/ajcn/nqy129
Li J, Wang J, Chen X, Tong S, Fang J, Yu H (1999) Cross-sectional survey of intralymphocytic and serum elements in hypertensive patients. Chin Med J 112:641–645
Li X, Meng X, Spiliopoulou A, Timofeeva M, Wei WQ, Gifford A, Shen X, He Y, Varley T et al (2018) MR-PheWAS: exploring the causal effect of SUA level on multiple disease outcomes by using genetic instruments in UK Biobank. Ann Rheum Dis 77:1039–1047. https://doi.org/10.1136/annrheumdis-2017-212534
Li L, Yang W, Huang L, Feng X, Cheng H, Ge X, Zan G, Tan Y, Xiao L et al (2021) MR-PheWAS for the causal effects of serum magnesium on multiple disease outcomes in Caucasian descent. iScience 24:103191. https://doi.org/10.1016/j.isci.2021.103191
Liu WM, ZG Zhu, HX Leng (2004) [Analysis of the contents of K, Na, Ca, Mg, Zn, Cu, Fe and Mn in serum of middle and old-aged hypertension patients]. Guang pu xue yu guang pu fen xi = Guang pu 24:360–2
Lorincz MT (2010) Neurologic Wilson’s disease. Ann N Y Acad Sci 1184:173–187. https://doi.org/10.1111/j.1749-6632.2009.05109.x
Ma J, Betts NM (2000) Zinc and copper intakes and their major food sources for older adults in the 1994–96 continuing survey of food intakes by individuals (CSFII). J Nutr 130:2838–2843. https://doi.org/10.1093/jn/130.11.2838
McDermott JH (2000) Antioxidant nutrients: current dietary recommendations and research update. J Am Pharm Assoc (washington, DC) 40:785–99. https://doi.org/10.1016/s1086-5802(16)31126-3
Nie X, Wang Y, Zhao H, Guo M, Liu Y, Xing M (2020) As(3+) or/and Cu(2+) exposure triggers oxidative stress imbalance, induces inflammatory response and apoptosis in chicken brain. Ecotoxicol Environ Saf 203:110993. https://doi.org/10.1016/j.ecoenv.2020.110993
Okoduwa SI, Umar IA, Ibrahim S, Bello F, Habila N (2015) Age-dependent alteration of antioxidant defense system in hypertensive and type-2 diabetes patients. J Diabetes Metab Disord 14:32. https://doi.org/10.1186/s40200-015-0164-z
Olatunbosun DA, Bolodeoku JO, Cole TO, Adadevoh BK (1976) Relationship of serum copper and zinc to human hypertension in Nigerians. Bull World Health Organ 53:134–135
Padmanabhan S, Carty L, Cameron E, Ghosh RE, Williams R, Strongman H (2019) Approach to record linkage of primary care data from Clinical Practice Research Datalink to other health-related patient data: overview and implications. Eur J Epidemiol 34:91–99. https://doi.org/10.1007/s10654-018-0442-4
Palmer TM, Lawlor DA, Harbord RM, Sheehan NA, Tobias JH, Timpson NJ, Davey Smith G, Sterne JA (2012) Using multiple genetic variants as instrumental variables for modifiable risk factors. Stat Methods Med Res 21:223–242. https://doi.org/10.1177/0962280210394459
Pavão ML, Figueiredo T, Santos V, Lopes PA, Ferin R, Santos MC, Nève J, Viegas-Crespo AM (2006) Whole blood glutathione peroxidase and erythrocyte superoxide dismutase activities, serum trace elements (Se, Cu, Zn) and cardiovascular risk factors in subjects from the city of Ponta Delgada, Island of San Miguel, The Azores Archipelago, Portugal. Biomark Biochem Indic Exposure Response Suscept Chem 11:460–471. https://doi.org/10.1080/13547500600625828
Shannon P, Markiel A, Ozier O, Baliga NS, Wang JT, Ramage D, Amin N, Schwikowski B, Ideker T (2003) Cytoscape: a software environment for integrated models of biomolecular interaction networks. Genome Res 13:2498–2504. https://doi.org/10.1101/gr.1239303
Shimizu Y, Nakazato M, Sekita T, Kadota K, Arima K, Yamasaki H, Takamura N, Aoyagi K, Maeda T (2014) Association between the hemoglobin levels and hypertension in relation to the BMI status in a rural Japanese population: the Nagasaki Islands Study. Internal Med (tokyo, Jpn) 53:435–440. https://doi.org/10.2169/internalmedicine.53.1353
Shimizu Y, Sato S, Koyamatsu J, Yamanashi H, Nagayoshi M, Kadota K, Kawashiri SY, Maeda T (2017) Possible mechanism underlying the association between higher hemoglobin level and hypertension in older Japanese men. Geriatr Gerontol Int 17:2586–2592. https://doi.org/10.1111/ggi.13068
Stelzer G, Rosen N, Plaschkes I, Zimmerman S, Twik M, Fishilevich S, Stein TI, Nudel R, Lieder I et al (2016) The genecards suite: from gene data mining to disease genome sequence analyses. Curr Protoc Bioinform 54:1301–13033. https://doi.org/10.1002/cpbi.5
Sudlow C, Gallacher J, Allen N, Beral V, Burton P, Danesh J, Downey P, Elliott P, Green J et al (2015) UK biobank: an open access resource for identifying the causes of a wide range of complex diseases of middle and old age. PLoS Med 12:e1001779. https://doi.org/10.1371/journal.pmed.1001779
Szklarczyk D, Gable AL, Lyon D, Junge A, Wyder S, Huerta-Cepas J, Simonovic M, Doncheva NT, Morris JH et al (2019) STRING v11: protein-protein association networks with increased coverage, supporting functional discovery in genome-wide experimental datasets. Nucleic Acids Res 47:D607–D613. https://doi.org/10.1093/nar/gky1131
Takeuchi H, Taki Y, Nouchi R, Yokoyama R, Kotozaki Y, Nakagawa S, Sekiguchi A, Iizuka K, Yamamoto Y et al (2019) Association of copper levels in the hair with gray matter volume, mean diffusivity, and cognitive functions. Brain Struct Funct 224:1203–1217. https://doi.org/10.1007/s00429-019-01830-y
Taneja SK, Mandal R (2007) Mineral factors controlling essential hypertension–a study in the Chandigarh, India population. Biol Trace Elem Res 120:61–73. https://doi.org/10.1007/s12011-007-8013-7
Tisato F, Marzano C, Porchia M, Pellei M, Santini C (2010) Copper in diseases and treatments, and copper-based anticancer strategies. Med Res Rev 30:708–749. https://doi.org/10.1002/med.20174
Verma A, Bradford Y, Dudek S, Lucas AM, Verma SS, Pendergrass SA, Ritchie MD (2018) A simulation study investigating power estimates in phenome-wide association studies. BMC Bioinform 19:120. https://doi.org/10.1186/s12859-018-2135-0
Vivoli G, Bergomi M, Rovesti S, Pinotti M, Caselgrandi E (1995) Zinc, copper, and zinc- or copper-dependent enzymes in human hypertension. Biol Trace Elem Res 49:97–106. https://doi.org/10.1007/bf02788959
Vlad M, Caseanu E, Uza G, Petrescu M (1994) Concentration of copper, zinc, chromium, iron and nickel in the abdominal aorta of patients deceased with coronary heart disease. J Trace Elem Electrolytes Health Dis 8:111–114
Wang Y, Zeng S, Lin TM, Krugner-Higby L, Lyman D, Steffen D, Xiong MP (2014) Evaluating the anticancer properties of liposomal copper in a nude xenograft mouse model of human prostate cancer: formulation, in vitro, in vivo, histology and tissue distribution studies. Pharm Res 31:3106–3119. https://doi.org/10.1007/s11095-014-1403-6
Wu W, Jiang S, Zhao Q, Zhang K, Wei X, Zhou T, Liu D, Zhou H, Zhong R et al (2018) Associations of environmental exposure to metals with the risk of hypertension in China. Sci Total Env 622–623:184–191. https://doi.org/10.1016/j.scitotenv.2017.11.343
Yao J, Hu P, Zhang D (2018) Associations between copper and zinc and risk of hypertension in US adults. Biol Trace Elem Res 186:346–353. https://doi.org/10.1007/s12011-018-1320-3
Zhou J, Liu C, Francis M, Sun Y, Ryu MS, Grider A, Ye K (2020) The causal effects of blood iron and copper on lipid metabolism diseases: evidence from phenome-wide mendelian randomization study. Nutrients. https://doi.org/10.3390/nu12103174
Zhou J, Liu C, Sun Y, Francis M, Ryu MS, Grider A, Ye K (2021) Genetically predicted circulating levels of copper and zinc are associated with osteoarthritis but not with rheumatoid arthritis. Osteoarthr Cartil 29:1029–1035. https://doi.org/10.1016/j.joca.2021.02.564
Funding
The authors acknowledge the UK Biobank and their participants for contributing the data used in this work (approval number: 56902). This work was supported by the National Key R&D Program of China (grant number 2020YFE0201600); the National Natural Science Foundation of China (grant number 82073504); the Guangxi Natural Science Fund for Innovation Research Team (grant number 2017GXNSFGA198003).
Author information
Authors and Affiliations
Contributions
Conceptualization, data curation and funding acquisition: XY and ZM. Original draft and formal analysis: XF, WY and LH. Methodology: LL and LH. Software: HC and XG. Visualization: GZ and YT. Review and editing: LX and CL. Validation: XC.
Corresponding authors
Ethics declarations
Conflicts of interest
On behalf of all authors, the corresponding authors state that there is no conflict of interest.
Ethics approval
UK Biobank received ethical approval from the research ethics committee (reference 13/NW/0382). All participants provided informed consent to participate. The present analyses were conducted under UK Biobank application number 56902.
Consent to participate and to publish
Not applicable.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Feng, X., Yang, W., Huang, L. et al. Causal Effect of Genetically Determined Blood Copper Concentrations on Multiple Diseases: A Mendelian Randomization and Phenome-Wide Association Study. Phenomics 2, 242–253 (2022). https://doi.org/10.1007/s43657-022-00052-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43657-022-00052-3