Abstract
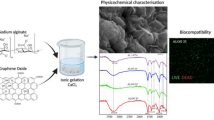
Cell encapsulation for treatment of diseases like type 1 diabetes (T1D) has great potential when used in combination with development of insulin responsive beta cells. However, for translation of this therapy into clinical practice, there is a need for suitable encapsulation devices. Here, we report development of polyurethane-zwitterionic acrylate double network-based membranes for macro device-based cell encapsulation. Polyurethane hydrogels with 60 to 90% water content (WC) were evaluated for permeability and hydrogels with 80 and 90% WC were found to have highest permeability. Structural characterization of these hydrogels’ samples prepared cryogenically by scanning electron microscopy (cryo-SEM) revealed that 90% WC hydrogels were nanoporous with large interconnected pores. Tuning of porosity and structure was achieved by blending of hydrogels with varying WC resulting in pores of ~ 200 nm size. These membranes supported viability of encapsulated cells after removal of cytotoxic leachables by ethanol treatment. Double network formation was performed by UV polymerization and incorporation of zwitterionic groups was confirmed by ATR and WC of hydrogels. Varying of zwitterion type is allowed for tuning of WC of hydrogels. Gene expression of RAW 264.7 macrophages on exposure to the hydrogels found the zwitterionic double network hydrogels to be less stimulating than the bare hydrogel. To determine translational potential of the hydrogel, sterilization of the hydrogels using supercritical carbon dioxide was evaluated. Survivor enumeration testing revealed that the kill rate for the process ~ 1 log10 per 8 min and 2-h treatment is sufficient for sterility assurance level (SAL) of 10−6. Thus, we have developed hydrogel polyurethane membranes suitable for cell encapsulation in macro devices.
Lay Summary
We want to develop a device for cell encapsulation which is needed for treating diseases like T1D. In these devices, cells will be loaded and implanted in the body. These encapsulated cell secretions would provide the function of various endocrine organs. We have developed a hydrogel-based nanoporous membrane which would hold the cells and allow for exchange of nutrients and cell secretions.
Future Studies
After the development of membrane, future studies will focus on evaluating the immune response to the hydrogel as well as long term delivery of immune modulatory drugs to prevent fibrosis. Various drug encapsulation and delivery designs will be evaluated for controlled localized delivery of the drugs. The optimum combination would then be combined with the hydrogels device and test their efficacy in regulating cell viability and immune response in animal models.









Similar content being viewed by others
References
National diabetes statistics report: estimates of diabetes and its burden in the united states. Atlanta, GA: Department of Health and Human Services, Centers for Disease Control and Prevention; 2014.
Kawahara T, Kin T, Kashkoush S, Gala-Lopez B, Bigam DL, Kneteman NM, et al. Portal vein thrombosis is a potentially preventable complication in clinical islet transplantation. Am J Transplant. 2011;11(12):2700–7. https://doi.org/10.1111/j.1600-6143.2011.03717.x.
Nanji SA, Shapiro AMJ. Islet transplantation in patients with diabetes mellitus. BioDrugs. 2004;18(5):315–28. https://doi.org/10.2165/00063030-200418050-00004.
Kieffer TJ. Closing in on mass production of mature human beta cells. Cell Stem Cell. 2016;18(6):699–702. https://doi.org/10.1016/j.stem.2016.05.014.
Schulz TC. Concise review: manufacturing of pancreatic endoderm cells for clinical trials in type 1 diabetes. Stem Cells Transl Med. 2015;4(8):927–31. https://doi.org/10.5966/sctm.2015-0058.
Schulz TC, Young HY, Agulnick AD, Babin MJ, Baetge EE, Bang AG, et al. A scalable system for production of functional pancreatic progenitors from human embryonic stem cells. PLoS One. 2012;7(5):e37004. https://doi.org/10.1371/journal.pone.0037004.
Olabisi RM. Cell microencapsulation with synthetic polymers. J Biomed Mater Res A. 2015;103(2):846–59. https://doi.org/10.1002/jbm.a.35205.
Onoe H, Okitsu T, Itou A, Kato-Negishi M, Gojo R, Kiriya D, et al. Metre-long cell-laden microfibres exhibit tissue morphologies and functions. Nat Mater. 2013;12(6):584–90. https://doi.org/10.1038/Nmat3606.
Barkai U, Rotem A, de Vos P. Survival of encapsulated islets: more than a membrane story. World J Transplant. 2016;6(1):69–90. https://doi.org/10.5500/wjt.v6.i1.69.
Teramura Y, Iwata H. Bioartificial pancreas microencapsulation and conformal coating of islet of Langerhans. Adv Drug Deliv Rev. 2010;62(7–8):827–40. https://doi.org/10.1016/j.addr.2010.01.005.
Blasi P, Luca G, Mancuso F, Schoubben A, Calvitti M, Giovagnoli S, et al. Conformal polymer coatings for pancreatic islets transplantation. Int J Pharm. 2013;440(2):141–7. https://doi.org/10.1016/j.ijpharm.2012.10.010.
Carlsson PO, Espes D, Sedigh A, Rotem A, Zimerman B, Grinberg H, et al. Transplantation of macroencapsulated human islets within the bioartificial pancreas betaAir to patients with type 1 diabetes mellitus. Am J Transplant. 2018;18(7):1735–44. https://doi.org/10.1111/ajt.14642.
Henry RR, Pettus J, Wilensky J, Shapiro AMJ, Senior PA, Roep B, et al. Initial clinical evaluation of VC-01TM combination product-a stem cell-derived islet replacement for type 1 diabetes (T1D). Diabetes. 2018;67:138–OR. https://doi.org/10.2337/db18-138-OR.
de Vos P, Lazarjani HA, Poncelet D, Faas MM. Polymers in cell encapsulation from an enveloped cell perspective. Adv Drug Deliv Rev. 2014;67–68:15–34. https://doi.org/10.1016/j.addr.2013.11.005.
Selimović Š, Oh J, Bae H, Dokmeci M, Khademhosseini A. Microscale strategies for generating cell encapsulating hydrogels. Polymers. 2012;4(3):26. https://doi.org/10.3390/polym4031554.
Handel N, Gutierrez J. Long-term safety and efficacy of polyurethane foam-covered breast implants. Aesthet Surg J. 2006;26(3):265–74. https://doi.org/10.1016/j.asj.2006.04.001.
Castel N, Soon-Sutton T, Deptula P, Flaherty A, Parsa FD. Polyurethane-coated breast implants revisited: a 30-year follow-up. Arch Plast Surg. 2015;42(2):186–93. https://doi.org/10.5999/aps.2015.42.2.186.
Stokes K, Cobain K. Polyether polyurethanes for implantable pacemaker leads.pdf. Biomaterials. 1982;3(4):7.
Ward RS, White KA, Wolcott CA, Wang AY, Kuhn RW, Taylor JE, et al. Development of a hybrid artificial pancreas with a dense polyurethane membrane. ASAIO J. 1993;39(3):M261–M7.
Xie X, Doloff JC, Yesilyurt V, Sadraei A, McGarrigle JJ, Omami M, et al. Reduction of measurement noise in a continuous glucose monitor by coating the sensor with a zwitterionic polymer. Nat Biomed Eng. 2018;2:894–906. https://doi.org/10.1038/s41551-018-0273-3.
Liu X, Jin Q, Ji Y, Ji J. Minimizing nonspecific phagocytic uptake of biocompatible gold nanoparticles with mixed charged zwitterionic surface modification. J Mater Chem. 2012;22(5):1916–27. https://doi.org/10.1039/C1JM14178C.
Carr L, Cheng G, Xue H, Jiang S. Engineering the polymer backbone to strengthen nonfouling sulfobetaine hydrogels. Langmuir. 2010;26(18):14793–8. https://doi.org/10.1021/la1028004.
Zhang L, Cao Z, Bai T, Carr L, Ella-Menye JR, Irvin C, et al. Zwitterionic hydrogels implanted in mice resist the foreign-body reaction. Nat Biotechnol. 2013;31(6):553–6. https://doi.org/10.1038/nbt.2580.
Wang K, Hou WD, Wang X, Han CS, Vuletic I, Su N, et al. Overcoming foreign-body reaction through nanotopography: biocompatibility and immunoisolation properties of a nanofibrous membrane. Biomaterials. 2016;102:249–58. https://doi.org/10.1016/j.biomaterials.2016.06.028.
Smith RS, Zhang Z, Bouchard M, Li J, Lapp HS, Brotske GR, et al. Vascular catheters with a nonleaching poly-sulfobetaine surface modification reduce thrombus formation and microbial attachment. Sci Transl Med. 2012;4(153):153ra32-ra32. https://doi.org/10.1126/scitranslmed.3004120.
Kyomoto M, Moro T, Takatori Y, Kawaguchi H, Ishihara K. Cartilage-mimicking, high-density brush structure improves wear resistance of crosslinked polyethylene: a pilot study. Clin Orthop Relat Res. 2011;469(8):2327–36. https://doi.org/10.1007/s11999-010-1718-5.
Garle AL, White F, Budhlall BM. Improving the antifouling properties of polypropylene surfaces by melt blending with polyethylene glycol diblock copolymers. J Appl Polym Sci. 2018;135(15):46122. https://doi.org/10.1002/app.46122.
Khandwekar AP, Patil D, Shouche Y, Doble M. The biocompatibility of sulfobetaine engineered polymethylmethacrylate by surface entrapment technique. 2009.
Trel'ova D, Salgarella AR, Ricotti L, Giudetti G, Cutrone A, Sramkova P, et al. Soft hydrogel zwitterionic coatings minimize fibroblast and macrophage adhesion on polyimide substrates. Langmuir. 2019;35(5):1085–99. https://doi.org/10.1021/acs.langmuir.8b00765.
Kumagai-Braesch M, Jacobson S, Mori H, Jia X, Takahashi T, Wernerson A, et al. The TheraCyte™ device protects against islet allograft rejection in immunized hosts. Cell Transplant. 2013;22(7):1137–46. https://doi.org/10.3727/096368912x657486.
Rafael E, Wernerson A, Arner P, Wu GS, Tibell A. In vivo evaluation of glucose permeability of an immunoisolation device intended for islet transplantation: a novel application of the microdialysis technique. Cell Transplant. 1999;8(3):317–26. https://doi.org/10.1177/096368979900800302.
Rafael E, Wu GS, Hultenby K, Tibell A, Wernerson A. Improved survival of macroencapsulated islets of Langerhans by preimplantation of the immunoisolating device: a morphometric study. Cell Transplant. 2003;12(4):407–12. https://doi.org/10.3727/000000003108746957.
Armstrong JK, Wenby RB, Meiselman HJ, Fisher TC. The hydrodynamic radii of macromolecules and their effect on red blood cell aggregation. Biophys J. 2004;87(6):4259–70. https://doi.org/10.1529/biophysj.104.047746.
Nakashima K, Kanda Y, Hirokawa Y, Kawasaki F, Matsuki M, Kaku K. MIN6 is not a pure beta cell line but a mixed cell line with other pancreatic endocrine hormones. Endocr J. 2009;56(1):45–53. https://doi.org/10.1507/endocrj.K08E-172.
Sella SR, Vandenberghe LP, Soccol CR. Bacillus atrophaeus: main characteristics and biotechnological applications - a review. Crit Rev Biotechnol. 2015;35(4):533–45. https://doi.org/10.3109/07388551.2014.922915.
Yim ES, Zhao B, Myung D, Kourtis LC, Frank CW, Carter D, et al. Biocompatibility of poly(ethylene glycol)/poly(acrylic acid) interpenetrating polymer network hydrogel particles in RAW 264.7 macrophage and MG-63 osteoblast cell lines. J Biomed Mater Res A. 2009;91(3):894–902. https://doi.org/10.1002/jbm.a.32311.
Arango Duque G, Descoteaux A. Macrophage cytokines: involvement in immunity and infectious diseases. Front Immunol. 2014;5:491. https://doi.org/10.3389/fimmu.2014.00491.
Liu JMH, Zhang J, Zhang X, Hlavaty KA, Ricci CF, Leonard JN, et al. Transforming growth factor-beta 1 delivery from microporous scaffolds decreases inflammation post-implant and enhances function of transplanted islets. Biomaterials. 2016;80:11–9. https://doi.org/10.1016/j.biomaterials.2015.11.065.
Funding
This project was made possible by the Mayo Clinic CTSA grant number UL1TR002377 from the National Center for Advancing Translational Science (NCATS), a component of the National Institutes of Health (NIH) and a grant from Khalifa Bin Zayed Al Nahyan Foundation.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
ESM 1
(PDF 234 kb)
Rights and permissions
About this article
Cite this article
Garle, A., Miller, A., Sarrafian, T. et al. Development of Nanoporous Polyurethane Hydrogel Membranes for Cell Encapsulation. Regen. Eng. Transl. Med. 6, 217–227 (2020). https://doi.org/10.1007/s40883-019-00125-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40883-019-00125-2