Opinion statement
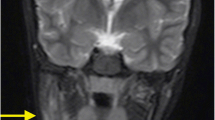
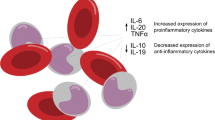
Chronic non-bacterial osteomyelitis (CNO), also known as chronic recurrent multifocal osteomyelitis (CRMO), is an autoinflammatory bone disorder that primarily affects children. CNO mainly affects long bones in the lower extremities, vertebral bodies, clavicle, mandible, and pelvic bones. No laboratory biomarker has been shown reliable for clinical monitoring yet. Imaging especially whole-body MRI with STIR images has become the gold standard of monitoring disease because of its sensitivity to detect active lesions. In children with suspected CNO, regional MRI at minimum is recommended to determine the presence of bone edema and adjacent soft tissue inflammation and/or periosteal reaction. Basic laboratory workups are usually performed by referring physicians to screen for malignancy and infectious osteomyelitis. When a child has CNO-associated conditions such as psoriasis, inflammatory bowel disease, or multiple CNO lesions in characteristic sites, a bone biopsy may be postponed. However, in children with a unifocal lesion other than clavicle or ill appearance, an MRI-guided bone biopsy with bacterial, fungal, and mycobacterial cultures as well as pathology review is strongly recommended to exclude alternative diagnoses. Nonsteroidal anti-inflammatory drugs (NSAIDs) remain the first-line treatment. However, non-responders and children with frequent relapses require other treatments such as short-term glucocorticoids, disease-modifying anti-rheumatic drugs (DMARDs), TNF-α inhibiters, and/or bisphosphonates. In children with associated arthritis without sacroiliitis, DMARDs may be considered for both conditions. In children with sacroiliitis and CNO, TNF-α inhibiters are preferred. When active spinal lesions are present, bisphosphonate may be chosen as first-line treatment or used in combination with other agents. Repeated MRI is recommended to determine the response to treatment because pain relief can occur despite persistent bone inflammation. Long-term follow-up is recommended as some patients continue to have ongoing disease activity into adulthood.
Similar content being viewed by others
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance
• Wipff J, Costantino F, Lemelle I, Pajot C, Duquesne A, Lorrot M, et al. A large national cohort of French patients with chronic recurrent multifocal osteitis. Arthritis Rheumatol. 2015;67:1128–37. The largest CNO cohort reported three homogeneous phenotypes using cluster analysis. Majority of patients with unifocal presentation developed multifocal lesions during long-term follow-up.
Jansson A, Renner ED, Ramser J, Mayer A, Haban M, Meindl A, et al. Classification of non-bacterial osteitis: retrospective study of clinical, immunological and genetic aspects in 89 patients. Rheumatology (Oxford). 2007;46:154–60.
• Voit AM, Arnoldi AP, Douis H, Bleisteiner F, Jansson MK, Reiser MF, et al. Whole-body magnetic resonance imaging in chronic recurrent multifocal osteomyelitis: clinical longterm assessment may underestimate activity. J Rheumatol. 2015;42:1455–62. The first study using whole-body MRI in adult patients who had childhood disease onset provided evidence of persistent inflammation of CRMO into adulthood regardless of clinical disease status. It highlights the importance of continuing monitoring of disease with imaging and appropriate treatment for CRMO patients during their adulthood. It also demonstrated that many patients have ongoing pain in the absence of inflammation on MRI.
Hofmann SR, Morbach H, Schwarz T, Rösen-Wolff A, Girschick HJ, Hedrich CM. Attenuated TLR4/MAPK signaling in monocytes from patients with CRMO results in impaired IL-10 expression. Clin Immunol Elsevier Inc.; 2012;145:69–76.
• Hofmann SR, Kubasch AS, Range U, Laass MW, Morbach H, Girschick HJ, et al. Serum biomarkers for the diagnosis and monitoring of chronic recurrent multifocal osteomyelitis (CRMO). Rheumatol Int Springer Berlin Heidelberg; 2016;36:769–79. This study explored the potential of serum biomarkers to distinguish between patients with CRMO or Crohn’s disease and healthy individuals.
Hofmann SR, Schwarz T, Möller JC, Morbach H, Schnabel A, Rösen-Wolff A, et al. Chronic non-bacterial osteomyelitis is associated with impaired Sp1 signaling, reduced IL10 promoter phosphorylation, and reduced myeloid IL-10 expression. Clin Immunol Elsevier Inc.; 2011;141:317–27.
Hofmann SR, Roesen-Wolff A, Hahn G, Hedrich CM. Update: cytokine dysregulation in chronic nonbacterial osteomyelitis (CNO). Int J Rheumatol 2012;2012:doi: 10.1155/2012/310206.
Scianaro R, Insalaco A, Bracci Laudiero L, De Vito R, Pezzullo M, Teti A, et al. Deregulation of the IL-1β axis in chronic recurrent multifocal osteomyelitis. Pediatr Rheumatol Online J. 2014;12:30.
Carr AJ, Cole WG, Roberton DM, Chow CW. Chronic multifocal osteomyelitis. J Bone Joint Surg (Br). 1993;75:582–91.
Jansson AF, Muller TH, Gliera L, Ankerst DP, Wintergerst U, Belohradsky BH, et al. Clinical score for nonbacterial osteitis in children and adults. Arthritis Rheum. 2009;60:1152–9.
• Roderick MR, Shah R, Rogers V, Finn A, Ramanan AV. Chronic recurrent multifocal osteomyelitis (CRMO)—advancing the diagnosis. Pediatr Rheumatol Pediatr Rheumatol. 2016;14(1):47. doi:10.1186/s12969-016-0109-1. This article proposed new diagnostic criteria of CNO. The use of the Bristol diagnostic criteria by an experienced clinician may reduce the need of bone biopsy in some CNO patients.
Bollen A-M, Eyre DR. Bone resorption rates in children monitored by the urinary assay of collagen type I cross-linked peptides. Bone. 1994;15:31–4.
Jansson AF, Grote V. Nonbacterial osteitis in children: data of a German Incidence Surveillance Study. Acta Paediatr. 2011;100:1150–7.
• Schnabel A, Range U, Hahn G, Siepmann T, Berner R, Hedrich CM. Unexpectedly high incidences of chronic non-bacterial as compared to bacterial osteomyelitis in children. Rheumatol Int Springer Berlin Heidelberg; 2016;36:1737–1745. A cohort study from a tertiary center in Germany showed a similar incidence rate of non-bacterial osteomyelitis and infectious osteomyelitis. The result confirmed the underestimate of disease prevalence and incidence of CNO.
Hospach T, Langendoerfer M, von Kalle T, Maier J, Dannecker GE. Spinal involvement in chronic recurrent multifocal osteomyelitis (CRMO) in childhood and effect of pamidronate. Eur J Pediatr. 2010;169:1105–11.
• Zhao Y, Chauvin NA, Jaramillo D, Burnham JM. Aggressive therapy reduces disease activity without skeletal damage progression in chronic nonbacterial osteomyelitis. J Rheumatol. 2015;42:1245–51. doi:10.3899/jrheum.141138. Further characterization of MRI findings from patients with CNO provided more comprehensive evaluation of disease status and response to treatment in patients with CNO.
Gleeson H, Wiltshire E, Briody J, Hall J, Chaitow J, Sillence D, et al. Childhood chronic recurrent multifocal osteomyelitis: pamidronate therapy decreases pain and improves vertebral shape. J Rheumatol. 2008;35:707–12.
Guérin-Pfyffer S, Guillaume-Czitrom S, Tammam S, Koné-Paut I. Evaluation of chronic recurrent multifocal osteitis in children by whole-body magnetic resonance imaging. Jt Bone Spine. 2012;79:616–20.
Neubauer H, Evangelista L, Morbach H, Girschick H, Prelog M, Köstler H, et al. Diffusion-weighted MRI of bone marrow oedema, soft tissue oedema and synovitis in paediatric patients: feasibility and initial experience. Pediatr Rheumatol Online J. 2012;10:20.
Darge K, Jaramillo D, Siegel MJ. Whole-body MRI in children: current status and future applications. Eur J Radiol. 2008;68:289–98.
Hofmann C, Wurm M, Schwarz T, Neubauer H, Beer M, Girschick H, et al. A standardized clinical and radiological follow-up of patients with chronic non-bacterial osteomyelitis treated with pamidronate. Clin Exp Rheumatol. 2014;32:604–9.
• Roderick M, Shah R, Finn A, Ramanan AV. Efficacy of pamidronate therapy in children with chronic non-bacterial osteitis: disease activity assessment by whole body magnetic resonance imaging. Rheumatology (Oxford). 2014;53:1973–6. Whole-body MRI was used to determine response to pamidronate in children with CNO and poor response to NSAIDs.
Morbach H, Schneider P, Schwarz T, Hofmann C, Raab P, Neubauer H, et al. Comparison of magnetic resonance imaging and Technetium-labelled methylene diphosphonate bone scintigraphy in the initial assessment of chronic non-bacterial osteomyelitis of childhood and adolescents. Clin Exp Rheumatol. 2012;30:578–82.
Miettunen PM, Wei X, Kaura D, Reslan WA, Aguirre AN, Kellner JD. Dramatic pain relief and resolution of bone inflammation following pamidronate in 9 pediatric patients with persistent chronic recurrent multifocal osteomyelitis (CRMO). Pediatr Rheumatol Online J. 2009;7:2.
Beck C, Morbach H, Beer M, Stenzel M, Tappe D, Gattenlöhner S, et al. Chronic nonbacterial osteomyelitis in childhood: prospective follow-up during the first year of anti-inflammatory treatment. Arthritis Res Ther. 2010;12:R74.
Girschick HJ, Raab P, Surbaum S, Trusen A, Kirschner S, Schneider P, et al. Chronic non-bacterial osteomyelitis in children. Ann Rheum Dis. 2005;64:279–85.
Hedrich CM, Hofmann SR, Pablik J, Morbach H, Girschick HJ. Autoinflammatory bone disorders with special focus on chronic recurrent multifocal osteomyelitis (CRMO). Pediatr Rheumatol Online J. 2013;11:47.
Walsh P, Manners PJ, Vercoe J, Burgner D, Murray KJ. Chronic recurrent multifocal osteomyelitis in children: nine years’ experience at a statewide tertiary paediatric rheumatology referral centre. Rheumatology (Oxford). 2015;54:1688–91.
Johnsson A, Flatø B, Knudsen P, Lilleby V. Clinical outcome in a Norwegian cohort of patients with chronic recurrent multifocal osteomyelitis. Scand J Rheumatol Informa Healthcare. 2015;44:513–4.
Wintrich S, Horneff G. Characteristics and outcomes of chronic non-bacterial osteitis in children. Eur J Rheumatol. 2015;2:139–42.
Kaiser D, Bolt I, Hofer M, Relly C, Berthet G, Bolz D, et al. Chronic nonbacterial osteomyelitis in children: a retrospective multicenter study. Pediatr Rheumatol Online J Pediatr Rheumatol. 2015;13:25.
Kahn MF, Hayem F, Hayem G, Grossin M. Is diffuse sclerosing osteomyelitis of the mandible part of the synovitis, acne, pustulosis, hyperostosis, osteitis (SAPHO) syndrome?. Analysis of seven cases. Oral Surgery, Oral Med Oral Pathol 1994;78:594–8.
Girschick HJ, Krauspe R, Tschammler A, Huppertz HI. Chronic recurrent osteomyelitis with clavicular involvement in children: diagnostic value of different imaging techniques and therapy with non-steroidal anti-inflammatory drugs. Eur J Pediatr. 1998;157:28–33.
Handrick W, Hörmann D, Voppmann A, Schille R, Reichardt P, Tröbs RB, et al. Chronic recurrent multifocal osteomyelitis—report of eight patients. Pediatr Surg Int. 1998;14:195–8.
Hayem G, Bouchaud-Chabot A, Benali K, Roux S, Palazzo E, Silbermann-Hoffman O, et al. SAPHO syndrome: a long-term follow-up study of 120 cases. Semin Arthritis Rheum. 1999;29:159–71.
Borzutzky A, Stern S, Reiff A, Zurakowski D, Steinberg EA, Dedeoglu F, et al. Pediatric chronic nonbacterial osteomyelitis. Pediatrics. 2012;130:e1190–7.
Catalano-Pons C, Comte A, Wipff J, Quartier P, Faye A, Gendrel D, et al. Clinical outcome in children with chronic recurrent multifocal osteomyelitis. Rheumatology (Oxford). 2008;47:1397–9.
Abril JC, Ramirez A. Successful treatment of chronic recurrent multifocal osteomyelitis with indomethacin: a preliminary report of five cases. J Pediatr Orthop. 2007;27:587–91.
Job-Deslandre C, Krebs S, Kahan A. Chronic recurrent multifocal osteomyelitis: five-year outcomes in 14 pediatric cases. Jt Bone Spine. 2001;68:245–51.
Eleftheriou D, Gerschman T, Sebire N, Woo P, Pilkington CA, Brogan PA. Biologic therapy in refractory chronic non-bacterial osteomyelitis of childhood. Rheumatology. 2010;49:1505–12.
Eisenstein ELIM, Syverson GD, Vora SS, Calvin B. Combination therapy with methotrexate and etanercept for refractory chronic recurrent multifocal osteomyelitis. J Rheumatol. 2011;38:4–6.
Zhao Y, Foster SK, Murdock TJ, Schlesinger M, Wallace CA. A rare case of chronic recurrent multifocal osteomyelitis with undifferentiated juvenile idiopathic arthritis, uveitis, and psoriasis. Case Reports Clin Med. 2016;5: doi: 10.4236/crcm.2016.57041.
Wendling D, Prati C, Aubin F. Anakinra treatment of SAPHO syndrome: short-term results of an open study. Ann Rheum Dis. 2012;71:1098-100. doi:10.1136/annrheumdis-2011-200743.
Nigrovic PA. Review: is there a window of opportunity for treatment of systemic juvenile idiopathic arthritis? Arthritis Rheumatol. 2014;66:1405-13. doi:10.1002/art.38615.
Banerjee I, Shortland GJ, Evans WD. Osteogenesis imperfecta and intravenous pamidronate. Arch Dis Child. 2002;87:562–3.
Kerrison C, Davidson JE, Cleary AG, Beresford MW. Pamidronate in the treatment of childhood SAPHO syndrome. Rheumatology (Oxford). 2004;43:1246–51.
Plotkin LI, Weinstein RS, Parfitt AM, Roberson PK, Manolagas SC, Bellido T. Prevention of osteocyte and osteoblast apoptosis by bisphosphonates and calcitonin. J Clin Invest. 1999;104:1363–74.
Maksymowych WP. Bisphosphonates for arthritis—a confusing rationale. J Rheumatol. 2003;30:430–4.
Huk OL, Zukor DJ, Antoniou J, Petit A. Effect of pamidronate on the stimulation of macrophage TNF-a release by ultra-high-molecular-weight polyethylene particles: a role for apoptosis. J Orthop Res. 2003;21:81–7.
Simm P, Allen R, Zacharin M. Bisphosphonate treatment in chronic recurrent multifocal osteomyelitis. J Pediatr. 2008;152:571–5.
Compeyrot-Lacassagne S, Rosenberg AM, Babyn P, Laxer RM. Pamidronate treatment of chronic noninfectious inflammatory lesions of the mandible in children. J Rheumatol. 2007;34:1585–9.
Green SB, Pappas AL. Effects of maternal bisphosphonate use on fetal and neonatal outcomes. Am J Heal Syst Pharm. 2014;71:2029–36.
King SM, Laxer RM, Manson D, Gold R. Chronic recurrent multifocal osteomyelitis: a noninfectious inflammatory process. Pediatr Infect Dis J. 1987;6:907–11.
Matzaroglou C, Velissaris D, Karageorgos A, Marangos M, Panagiotopoulos E, Karanikolas M. SAPHO syndrome diagnosis and treatment: report of five cases and review of the literature. Open Orthop J. 2009;3:100–6.
Jurik AG, Moller BN, Jensen MK, Jensen JT, Graudal H. Sclerosis and hyperostosis of the manubruim sterni. Rheumatol Int. 1986;6:171–8.
Gikas PD, Islam L, Aston W, Tirabosco R, Saifuddin A, Briggs TWR, et al. Nonbacterial osteitis: A clinical, histopathological, and imaging study with a proposal for protocol-based management of patients with this diagnosis. J Orthop Sci. 2009;14:505–16.
Schilling F, Wagner AD. Azithromycin: an anti-inflammatory effect in chronic recurrent multifocal osteomyelitis? A preliminary report. Z Rheumatol. 2000;59:352–3.
Panders AK, Hadders HN. Chronic sclerosing inflammations of the jaw. Oral Surg, Oral Med Oral Pathol. 1970;30:396–412.
Johannsen A. Chronic sclerosing osteomyelitis of the mandible. Acta Radiol Diagn. 1977;18:360–8.
Collert S, Isacson J. Chronic sclerosing osteomyelitis (Garre). Clin Orthop Relat Res. 1982;164:136–40.
Jurik AG, Helmig O, Ternowitz T, Moller BN. Chronic recurrent multifocal osteomyelitis: a follow-up study. J Pediatr Orthop. 1988;8:49–58.
Merkesteyn JPR Van, Bakker DJ, Waal I Van Der, Kusen GJ, Egyedi P, Akker HP Van Den, et al. Hyperbaric oxygen treatment of chronic osteomyelitis of the jaws. Int J Oral Surg Munksgaard International Publishers Ltd.; 1984;13:386–95.
Majeed HA, Kalaawi M, Mohanty D, Teebi AS, Tunjekar MF, al-Gharbawy F, et al. Congenital dyserythropoietic anemia and chronic recurrent multifocal osteomyelitis in three related children and the association with Sweet syndrome in two siblings. J Pediatr. 1989;115:730–4.
Herlin T, Fiirgaard B, Bjerre M, Kerndrup G, Hasle H, Bing X, et al. Efficacy of anti-IL-1 treatment in Majeed syndrome. Ann Rheum Dis. 2012. doi:10.1136/annrheumdis-2012-201818.
Aksentijevich I, Masters SL, Ferguson PJ, Dancey P, Frenkel J, van Royen-Kerkhoff A, et al. An autoinflammatory disease with deficiency of the interleukin-1-receptor antagonist. N Engl J Med. 2009;360:2426–37.
Cassel SL, Janczy JR, Bing X, Wilson SP, Olivier AK, Otero JE, et al. Inflammasome-independent IL-1β mediates autoinflammatory disease in Pstpip2-deficient mice. Proc Natl Acad Sci U S A. 2014;111:1072–7.
Lukens JR, Gross JM, Calabrese C, Iwakura Y, Lamkanfi M, Vogel P, et al. Critical role for inflammasome-independent IL-1β production in osteomyelitis. Proc Natl Acad Sci U S A. 2014;111:1066–71.
Lukens JR, Gurung P, Vogel P, Johnson GR, Carter RA, Mcgoldrick DJ, et al. Dietary modulation of the microbiome affects autoinflammatory disease. Nature. 2014;516:246–9.
Acknowledgements
PJF is supported by NIH/NIAMS R01AR059703.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Yongdong Zhao declares that he has no conflict of interest.
Ronald M. Laxer declares that he has no conflict of interest.
Polly J. Ferguson reports grants from NIH/NIAMS R01 Genetic and Immunologic Basis of CRMO, during the conduct of the study.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Pediatric Rheumatology
Rights and permissions
About this article
Cite this article
Zhao, Y., Laxer, R.M. & Ferguson, P.J. Treatment Advances in Chronic Non-Bacterial Osteomyelitis and Other Autoinflammatory Bone Conditions. Curr Treat Options in Rheum 3, 17–32 (2017). https://doi.org/10.1007/s40674-017-0058-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40674-017-0058-y