Abstract
Context
Hypogonadism in Prader–Willi syndrome (PWS) is generally attributed to hypothalamic dysfunction or to primary gonadal defect. MKRN3, a maternal imprinted gene located on 15q11.2-q13 region, encodes makorin ring finger protein 3, whose deficiency causes precocious puberty, an extremely rare symptom in PWS.
Objective
This study aimed to evaluate MKRN3 levels in patients with PWS and to analyze its correlation with sexual hormone levels, insulin resistance and Body Mass Index (BMI).
Methods
We performed an observational cross-sectional study and enrolled 80 patients with genetically confirmed diagnosis of PWS with median age of 9.6 years.
Results
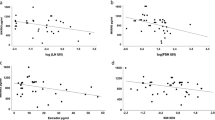
MKRN3 levels were measurable in 49 PWS patients with a geometric mean of 34.9 ± 22 pg/ml (median: 28.4). Unmeasurable levels of MKRN3 were found in 31 patients. No statistically significant differences were found between patients with and without measurable MKRN3 levels for any clinical, biochemical, or genetic characteristics. However, MKRN3 levels were inversely correlated with HOMA-IR index (p: 0.005) and HbA1c (p: 0.046) values. No statistically significant correlations were found between MKRN3 and LH, estradiol and testosterone concentrations, pubertal development and genetic defect, whereas a direct correlation with FSH was found (p: 0.007).
Conclusions
The typical genetic defect of PWS should lead to unmeasurable levels of the MKRN3 protein due to the inactivation of the paternal allele. Measurable circulating MKRN3 could suggest the possible involvement of tissue-specific imprinting mechanisms and other regulatory factors in gene expression. Correlations with HOMA-IR index, HbA1c, and FSH suggest peripheral actions of MKRN3, but future studies are warranted to investigate this topic.

Similar content being viewed by others
References
Cassidy SB, Schwartz S, Miller JL, Driscoll DJ (2012) Prader–Willi syndrome. Genet Med 14:10–26
Butler MG (2011) Prader–Willi syndrome: obesity due to genomic imprinting. Curr Genomics 12:204–215
Angulo MA, Butler MG, Cataletto ME (2015) Prader–Willi syndrome: a review of clinical, genetic, and endocrine findings. J Endocrinol Invest 38:1249–1263
Heksch R, Kamboj M, Anglin K, Obrynba K (2017) Review of Prader–Willi syndrome: the endocrine approach. Transl Pediatr 6(4):274–285
Costa RA, Ferreira IR, Cintra HA et al (2019) Genotype-phenotype relationships and endocrine findings in Prader–Willi syndrome. Front Endocrinol (Lausanne) 13(10):864
Siemensma EP, de Lind van Wijngaarden RF, Otten BJ et al (2012) Testicular failure in boys with Prader–Willi syndrome: longitudinal studies of reproductive hormones. J Clin Endocrinol Metab 97:E452
Eldar-Geva T, Hirsch HJ, Rabinowitz R et al (2009) Primary ovarian dysfunction contributes to the hypogonadism in women with Prader–Willi syndrome. Horm Res 72(3):153–9.120
Eldar-Geva T, Hirsch HJ, Benarroch F, Rubinstein O, GrossTsur V (2010) Hypogonadism in females with Prader–Willi syndrome from infancy to adulthood: variable combinations of a primary gonadal defect and hypothalamic dysfunction. Eur J Endocrinol 162(2):377–384
Radicioni A, Di Giorgio G, Grugni G et al (2012) Multiple forms of hypogonadism of central, peripheral or combined origin in males with Prader–Willi syndrome. Clin Endocrinol (Oxf) 76:72–77
Gross-Tsur V, Hirsch HJ, Benarroch F, Eldar-Geva T (2012) The FSH-inhibin axis in Prader–Willi syndrome: heterogeneity of gonadal dysfunction. Reprod Biol Endocrinol 10:10–39
Yellapragada V, Liu X, Lund C et al (2019) MKRN3 interacts with several proteins implicated in puberty timing but does not influence GNRH1 expression. Front Endocrinol (Lausanne) 8(10):48
Valadares LP, Meireles CG, De Toledo IP et al (2019) MKRN3 mutations in central precocious puberty: a systematic review and meta-analysis. J Endocr Soc 3(5):979–995
Abreu AP, Macedo DB, Brito VN, Kaiser UB, Latronico AC (2015) A new pathway in the control of the initiation of puberty: the MKRN3 gene. J Mol Endocrinol 54(3):131–139
Macedo DB, Abreu AP, Reis ACS et al (2014) Central precocious puberty that appears to be sporadic caused by paternally inherited mutations in the imprinted gene Makorin ring finger 3. J Clin Endocrinol Metab 99(6):E1097–E1103
Hagen CP, Sørensen K, Mieritz MG et al (2015) Circulating MKRN3 levels decline prior to pubertal onset and through puberty: a longitudinal study of healthy girls. J Clin Endocrinol Metab 100:1920–1926
Busch AS, Hagen CP, Almstrup K, Juul A (2016) Circulating MKRN3 levels decline during puberty in healthy boys. J Clin Endocrinol Metab 101:2588–2593
Grandone A, Cirillo G, Sasso M et al (2018) MKRN3 levels in girls with central precocious puberty and correlation with sexual hormone levels: a pilot study. Endocrine 59:203–208
Lee HS, Hwang JS (2013) Central precocious puberty in a girl with Prader–Willi syndrome. J Pediatr Endocrinol Metab 26:1201–1204
Crinò A, Di Giorgio G, Schiaffini R, Fierabracci A, Spera S, Maggioni A, Gattinara GC (2008) Central precocious puberty and growth hormone deficiency in a boy with Prader–Willi syndrome. Eur J Pediatr 167:1455–1458
Varimo T, Hero M, Känsäkoski J et al (2016) Circulating makorin ring-finger protein-3 (MKRN3) levels in healthy men and in men with hypogonadotropic hypogonadism. Clin Endocrinol (Oxf) 84(1):151–152
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH (2000) Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 320:1240–1243
Tanner JM, Whitehouse RH (1976) Clinical longitudinal standards for height, weight, height velocity, weight velocity, and stages of puberty. Arch Dis Child 51(3):170–179
Matthews DR, Hosker JP, Rudenski AS (1985) Homeostasis model assessment: insulin resistance and β-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28:412–419
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (2001) Executive summary of the third report of The National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (adult treatment panel III). JAMA 285:2486–2497
Habib WA, Brioude F, Azzi S et al (2019) Transcriptional profiling at the DLK1/MEG3 domain explains clinical overlap between imprinting disorders. Sci Adv 5(2):eaau9425
Chamberlain SJ, Johnstone KA, DuBose AJ et al (2004) Evidence for genetic modifiers of postnatal lethality in PWS-IC deletion mice. Hum Mol Genet 13(23):2971–2977
Rieusset A, Schaller F, Unmehopa U et al (2013) Stochastic loss of silencing of the imprinted Ndn/NDN allele, in a mouse model and humans with Prader–Willi syndrome, has functional consequences. PLoS Genet 9(9):e1003752
Rogan PK, Seip JR, White LM et al (1998) Relaxation of imprinting in Prader–Willi syndrome. Hum Genet 103(6):694–701
Seraphim CE, Canton APM, Montenegro L et al (2021) Genotype-phenotype correlations in central precocious puberty caused by MKRN3 mutations. J Clin Endocrinol Metab 106(4):1041–1050
Grandone A, Cantelmi G, Cirillo G et al (2015) A case of familial central precocious puberty caused by a novel mutation in the makorin RING finger protein 3 gene. BMC Endocr Disord 15:60
Acknowledgements
We thank all the families of patients included in the study for the support and participation.
Funding
This work was supported by a grant (390) funded by “VALERE: VAnviteLli pEr la RicErca” program of University of Campania “L. Vanvitelli”.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the Bioethics Committee of the “Bambino Gesù” Children’s Hospital (No 2092/2020).
Informed consent
The written informed consent of the parents of all enrolled patients was collected and is in our possession.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mariani, M., Fintini, D., Cirillo, G. et al. MKRN3 circulating levels in Prader–Willi syndrome: a pilot study. J Endocrinol Invest 45, 2165–2170 (2022). https://doi.org/10.1007/s40618-022-01860-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-022-01860-0