Abstract
Purpose
To evaluate the association between metabolic abnormalities and cardiovascular risk factors in patients with chronic hypoparathyroidism (HPP).
Patients and methods
Patients 18 years and older, glomerular filtration > 30 mL/min/1.73 m2 and no documented coronary artery disease were selected. Serum calcium, phosphorus, glucose, lipids, PTH, 25(OH)D and FGF23 were measured. Cardiovascular risk was estimated by the European Society of Cardiology (ESC) calculator. Transthoracic echocardiogram and carotid ultrasound were performed to detect carotid plaques (CP), carotid intima–media thickness (IMT), cardiac valve calcification (CVC), and left ventricular hypertrophy (LVH).
Results
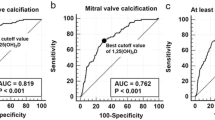
Thirty-seven patients (94.6% female), aged 56.0 ± 13.5 years and HPP duration 7.0 (4.0; 11.3) years, were included. Fifteen were classified as low cardiovascular risk, 9 as intermediate risk, 9 as high risk and none as very high risk. The prevalence of CP, CVC and LVH was 24.3%, 24.3% and 13.5%, respectively. IMT values were within normal ranges in all cohort. FGF23 were not associated with CP, IMT, CVC or LVH. After logistic regression, phosphorus was the only significant metabolic variable impacting CVC in univariate analysis (OR 2.795; 95% CI 1.132–6.905; p = 0.026), as well as in the multivariate analysis (OR 3.572; 95% CI 1.094–11.665; p = 0.035). Analysis by ROC curve showed serum phosphorus > 5.05 mg/dL (AUC 0.748; CI 0.584–0.877; p = 0.05) as the best cutoff point associated with valve heart calcification (sensitivity 78%; negative predictive value 91.3%).
Conclusion
Hyperphosphatemia was associated with CVC in HPP patients. Further studies are needed to investigate whether the control of hyperphosphatemia may reduce cardiovascular risk in this population.


Similar content being viewed by others
References
Clarke BL, Brown EM, Collins MT et al (2016) Epidemiology and diagnosis of hypoparathyroidism. J Clin Endocrinol Metab 101(6):2284–2299. https://doi.org/10.1210/jc.2015-3908
Imel EA, Biggin A, Schindeler A, Munns CF (2019) FGF23, Hypophosphatemia, and Emerging Treatments. JBMR Plus 3(8):1–9. https://doi.org/10.1002/jbm4.10190
Gafni RI, Collins MT (2019) Hypoparathyroidism. N Engl J Med. https://doi.org/10.1056/NEJMcp1800213
Pamuk N, Akkan T, Dağdeviren M et al (2020) Central and peripheral blood pressures and arterial stiffness increase in hypoparathyroidism. Arch Endocrinol Metab 64(4):374–382. https://doi.org/10.20945/2359-3997000000234
Rattazzi M, Bertacco E, Del Vecchio A, Puato M, Faggin E, Pauletto P (2013) Aortic valve calcification in chronic kidney disease. Nephrol Dial Transpl 28(12):2968–2976. https://doi.org/10.1093/ndt/gft310
Linefsky JP, O’Brien KD, Sachs M et al (2014) Serum phosphate is associated with aortic valve calcification in the Multi-ethnic Study of Atherosclerosis (MESA). Atherosclerosis 233(2):331–337. https://doi.org/10.1016/j.atherosclerosis.2013.12.051
Abramowitz Y, Jilaihawi H, Chakravarty T, Mack MJ, Makkar RR (2015) Mitral annulus calcification. J Am Coll Cardiol 66(17):1934–1941. https://doi.org/10.1016/j.jacc.2015.08.872
Meena D, Prakash M, Gupta Y, Bhadada S, Khandelwal N (2015) Carotid, aorta and renal arteries intima-media thickness in patients with sporadic idiopathic hypoparathyroidism. Indian J Endocrinol Metab 19(2):262–266. https://doi.org/10.4103/2230-8210.149320
Ackerman KE, Sokoloff NC, De Nardo MG, Clarke HM, Lee H, Misra M (2015) Fractures in relation to menstrual status and bone parameters in young athletes. Med Sci Sports Exerc 47(8):1577–1586. https://doi.org/10.1249/MSS.0000000000000574
Singal AK, Bataller R, Ahn J, Kamath PS, Shah VH (2018) ACG clinical guideline: alcoholic liver disease. Am J Gastroenterol 113(2):175–194. https://doi.org/10.1038/ajg.2017.469
Haring R, Enserro D, Xanthakis V et al (2016) Plasma fibroblast growth factor 23: clinical correlates and association with cardiovascular disease and mortality in the Framingham Heart Study. J Am Heart Assoc. https://doi.org/10.1161/JAHA.116.003486
Levey AS, Stevens LA, Schmid CH et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150:604–612. https://doi.org/10.7326/0003-4819-150-9-200905050-00006
Mach F, Baigent C, Catapano AL et al (2019) ESC/EAS Guidelines for the management of dyslipidaemias: lipid modification to reduce cardiovascular risk. Eur Heart J 41(1):111–188. https://doi.org/10.1093/eurheartj/ehz455
Lang RM, Badano LP, Mor-Avi V et al (2015) Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging Recommendations for Cardiac. J Am Soc Echocardiogr 28:1–39. https://doi.org/10.1016/j.echo.2014.10.003
Eleid MF, Foley TA, Said SM, Pislaru SV, Rihal CS (2016) Severe mitral annular calcification: multimodality imaging for therapeutic strategies and interventions. JACC Cardiovasc Imaging 9(11):1318–1337. https://doi.org/10.1016/j.jcmg.2016.09.001
Zoghbi WA, Adams D, Bonow RO et al (2017) Recommendations for noninvasive evaluation of native valvular regurgitation: a report from the American Society of Echocardiography developed in collaboration with the society for cardiovascular magnetic resonance. J Am Soc Echocardiogr 30(4):303–371. https://doi.org/10.1016/j.echo.2017.01.007
Freire CMV, de Alcantara ML, dos Santos SN et al (2015) Recomendação para a Quantificação pelo Ultrassom da Doença Aterosclerótica das Artérias Carótidas e Vertebrais: Grupo de Trabalho do Departamento de Imagem Cardiovascular da Sociedade Brasileira de Cardiologia DIC-SBC. Arq Bras Cardiol Imagem Cardiovasc 28:1–64. https://doi.org/10.5935/2318-8219.20150018
Gupta A, Winer K, Econs MJ, Marx SJ, Collins MT (2004) FGF-23 is elevated by chronic hyperphosphatemia. J Clin Endocrinol Metab 89(9):4489–4492. https://doi.org/10.1210/jc.2004-0724
Gutiérrez OM, Mannstadt M, Isakova T et al (2008) Fibroblast growth factor 23 and mortality among patients undergoing hemodialysis. N Engl J Med 359(6):584–592. https://doi.org/10.1056/nejmoa0706130
Faul C, Amaral AP, Oskouei B et al (2011) FGF23 induces left ventricular hypertrophy. J Clin Invest 121(11):4393–4408. https://doi.org/10.1172/JCI46122
Pelliccia A, Maron BJ, De Luca R, Di Paolo FM, Spataro A, Culasso F (2002) Remodeling of left ventricular hypertrophy in elite athletes after long-term deconditioning. Circulation 105(8):944–949. https://doi.org/10.1161/hc0802.104534
Burchfield JS, Xie M, Hill JA (2013) Pathological ventricular remodeling: Mechanisms: part 1 of 2. Circulation 128(4):388–400. https://doi.org/10.1161/CIRCULATIONAHA.113.001878
Rundek T, Arif H, Boden-Albala B, Elkind MS, Paik MC, Sacco RL (2008) Carotid plaque, a subclinical precursor of vascular events: the Northern Manhattan Study. Neurology 70(14):1200–1207. https://doi.org/10.1212/01.wnl.0000303969.63165.34
Bilezikia JP (2020) Hypoparathyroidism. J Clin Endocrinol Metab 105(6):1–15. https://doi.org/10.1210/clinem/dgaa113
Razzaque MS (2011) The dualistic role of vitamin D in vascular calcifications. Kidney Int 79(7):708–714. https://doi.org/10.1038/ki.2010.432
van Gils MJ, Bodde MC, Cremers LGM, Dippel DWJ, Van der Lugt A (2013) Determinants of calcification growth in atherosclerotic carotid arteries; a serial multi-detector CT angiography study. Atherosclerosis 227(1):95–99. https://doi.org/10.1016/j.atherosclerosis.2012.12.017
Cozzolino M, Gallieni M, Brancaccio D (2008) The mechanisms of hyperphosphatemia-induced vascular calcification. Int J Artif Organs 31(12):1002–1003. https://doi.org/10.1177/039139880803101203
Underbjerg L, Sikjaer T, Rejnmark L (2018) Long-term complications in patients with hypoparathyroidism evaluated by biochemical findings: a case-control study. J Bone Miner Res 33(5):822–831. https://doi.org/10.1002/jbmr.3368
Agarwal P, Prakash M, Singhal M, Bhadada SK, Gupta Y, Khandelwal N (2015) To assess vascular calcification in the patients of hypoparathyroidism using multidetector computed tomography scan. Indian J Endocrinol Metab 19(6):785–790. https://doi.org/10.4103/2230-8210.167545
Bortnick AE, Xu S, Kim RS et al (2019) Biomarkers of mineral metabolism and progression of aortic valve and mitral annular calcification: the Multi-Ethnic Study of Atherosclerosis. Atherosclerosis 285:79–86. https://doi.org/10.1016/j.atherosclerosis.2019.04.215
Bellasi A, Di Lullo L, Raggi P (2018) Cardiovascular calcification: the emerging role of micronutrients. Atherosclerosis 273:119–121. https://doi.org/10.1016/j.atherosclerosis.2018.04.019
Dweck MR, Boon NA, Newby DE (2012) Calcific aortic stenosis: a disease of the valve and the myocardium. J Am Coll Cardiol 60(19):1854–1863. https://doi.org/10.1016/j.jacc.2012.02.093
Raggi P, Boulay A, Chasan-Taber S et al (2002) Cardiac calcification in adult hemodialysis patients: a link between end-stage renal disease and cardiovascular disease? J Am Coll Cardiol 39(4):695–701. https://doi.org/10.1016/S0735-1097(01)01781-8
Hisamatsu T, Miura K, Fujiyoshi A et al (2018) Serum magnesium, phosphorus, and calcium levels and subclinical calcific aortic valve disease: a population-based study. Atherosclerosis 273:145–152. https://doi.org/10.1016/j.atherosclerosis.2018.03.035
Acknowledgements
We are grateful to the Federal University of Rio de Janeiro and Federal Hospital of Bonsucesso for helping us with this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all the authors, the corresponding author states that there is no conflict of interest.
Ethical approval
The study was approved by the Research Ethics Committee and registered at Plataforma Brazil (CAAE 00360918.0.0000.5253) and conducted from August 2017 to February 2020.
Informed consent
Informed consent was obtained from all the individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Polonine, S., de Santa Rosa, R.G., Farias, M.L.F. et al. Hyperphosphatemia is associated with cardiac valve calcification in chronic hypoparathyroidism. J Endocrinol Invest 45, 1359–1366 (2022). https://doi.org/10.1007/s40618-022-01770-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-022-01770-1