Abstract
Background
Postoperative delirium is a common complication following various operative procedures with an incidence rate of 10–77 %.
Aim
To analyze various risk factors for postoperative delirium after spine surgery in the middle- and old-aged patients.
Methods
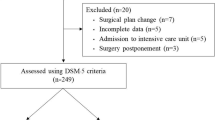
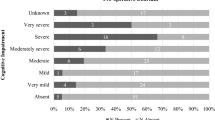
This study retrospectively reviewed 451 patients (226 males and 225 females, an average age of 65.1 ± 18.3 years) who underwent spinal surgery in our hospital between January 2010 and August 2015. Patients who had features of acute onset and fluctuating course and any two of the other features were diagnosed with delirium. Cognitive tests consisting of Clinical Dementia Rating and Global Deterioration Scale were performed to evaluate delirium. T tests were used for statistical analysis of the difference between the two groups, and logistic regression analyses were used for determining the risk factors.
Results
A total of 42 (9.3 %) patients were diagnosed with delirium. Delirious and non-delirious patients had no difference in age, gender, BMI, education level, drug treatment, comorbid disease history, surgical history, preoperative blood pressure, intraoperative blood loss, blood transfusion, use of surgical implants, surgical site, use of fentanyl and propofol, and preoperative VAS score. Intraoperative hypotension and use of dezocine were related to postoperative delirium (P = 0.03 and P = 0.07). The multiple regression equation was Y = −0.11 + 0.52 × X 0 + 0.21 × X 1, where X 0 = amount of dezocine, X 1 = instances of intraoperative hypotension.
Conclusion
Postoperative delirium commonly occurs after spine surgery. Intraoperative hypotension <80 mmHg and intraoperative use of dezocine represent valuable new predictors of the risk of delirium.
Similar content being viewed by others
References
Chrispal A, Mathews KP, Surekha V (2010) The clinical profile and association of delirium in geriatric patients with hip fractures in a tertiary care hospital in India. J Assoc Phys India 58:15–19
Brauer C, Morrison RS, Silberzweig SB et al (2000) The cause of delirium in patients with hip fracture. Arch Intern Med 160:1856–1860
Takeuchi M, Takeuchi H, Fujisawa D et al (2012) Incidence and risk factors of postoperative delirium in patients with esophageal cancer. Ann Surg Oncol 19:3963–3970
Ushida T, Yokoyama T, Kishida Y et al (2009) Incidence and risk factors of postoperative delirium in cervical spine surgery. Spine 34:2500–2504
Seo JS, Park SW, Lee YS et al (2014) Risk factors for delirium after spine surgery in elderly patients. J Korean Neurosurg Soc 56:28–33
Shi C, Yang C, Gao R et al (2015) Risk factors for delirium after spinal surgery: a meta-analysis. World Neurosurg 84:1466–1472
Kawaguchi Y, Kanamori M, Ishihara H et al (2006) Postoperative delirium in spine surgery. Spine J 6:164–169
Deiner S, Silverstein J (2009) Postoperative delirium and cognitive dysfunction. Br J Anaesth 103(suppl 1):i41–i46
Saczynski JS, Marcantonio ER, Quach L et al (2012) Cognitive trajectories after postoperative delirium. N Engl J Med 367:30–39
Steiner LA (2011) Postoperative delirium. Part 1: pathophysiology and risk factors. EJA 28:628–636
Sasajima Y, Sasajima T, Uchida H et al (2000) Postoperative delirium in patients with chronic lower limb ischaemia: What are the specific markers? Eur J Vasc Endovasc Surg 20:132–137
Kazmierski J, Kowman M, Banach M et al (2006) Preoperative predictors of delirium after cardiac surgery: a preliminary study. Gen Hosp Psychiatry 28:536–538
Tei M, Wakasugi M, Kishi K et al (2016) Incidence and risk factors of postoperative delirium in elderly patients who underwent laparoscopic surgery for colorectal cancer. Int J Colorectal Dis 31:67–73
DeCrane SK, Sands L, Ashland M et al (2011) Factors associated with recovery from early postoperative delirium. J PeriAnesth Nurs 26:231–241
Thornlow DK, Anderson R, Oddone E (2009) Cascade iatrogenesis: factors leading to the development of adverse events in hospitalized older adults. Int J Nurs Stud 46:1528–1535
Visser L, Prent A, van der Laan MJ et al (2015) Predicting postoperative delirium after vascular surgical procedures. J Vasc Surg 62:183–189
Gao R, Yang Z, Li M et al (2008) Probable risk factors for postoperative delirium in patients undergoing spinal surgery. Eur Spine J 17:1531–1537
Inouye SK (2006) Delirium in older persons. N Engl J Med 354:1157–1165
Morris JC (1993) The Clinical Dementia Rating (CDR): current version and scoring rules. Neurology 43:2412–2414
Reisberg B, Ferris SH, de Leon MJ et al (1982) The Global Deterioration Scale for assessment of primary degenerative dementia. Am J Psychiatr 139:1136–1139
Association AP (1987) Diagnostic and statistical manual of mental disorders (rev.), vol 124. Author, Washington, pp 111–126
Lipowski ZJ (1990) Delirium: acute confusional states, vol 16. Oxford University Press, New York
Agneta Edlund RN, Maria Lundström RN, Gösta Bucht MD et al (2004) Delirium before and after operation for femoral neck fracture. J Am Geriatr Soc 49:1335–1340
Wang N-Y, Hirao A, Sieber F (2015) Association between intraoperative blood pressure and postoperative delirium in elderly hip fracture patients. PLoS One 10:e0123892
Taipale PG, Ratner PA, Galdas PM et al (2012) The association between nurse-administered midazolam following cardiac surgery and incident delirium: an observational study. Int J Nurs Stud 49:1064–1073
Wesselink EM, Kappen TH, Klei WAV et al (2016) Intraoperative hypotension and delirium after on-pump cardiac surgery. Crit Care Med 60:427–433
Hirsch J (2015) Impact of intraoperative hypotension and blood pressure fluctuations on early postoperative delirium after non-cardiac surgery. Br J Anaesth 115:418–426
Liu R, Huang X-P, Yeliseev A et al (2014) Novel molecular targets of dezocine and their clinical implications. J Am Soc Anesthesiol 120:714–723
Sun Z-T, Yang C-Y, Cui Z et al (2011) Effect of intravenous dezocine on fentanyl-induced cough during general anesthesia induction: a double-blinded, prospective, randomized, controlled trial. J Anesth 25:860–863
Wan Q, Xu L, Bo Y (2014) Effects of Dexmedetomidine combined with Dezocine on cognition function and hippocampal microglia activation of rats. Int J Clin Exp Med 7:2787–2792
Walker EA, Picker MJ, Granger A et al (2004) Effects of opioids in morphine-treated pigeons trained to discriminate among morphine, the low-efficacy agonist nalbuphine, and saline. J Pharmacol Exp Ther 310:150–158
Zhu Y, Jing G, Yuan W (2011) Preoperative administration of intramuscular dezocine reduces postoperative pain for laparoscopic cholecystectomy. J Biomed Res 25:356–361
Nishikawa K, Nakayama M, Omote K et al (2004) Recovery characteristics and post-operative delirium after long-duration laparoscope-assisted surgery in elderly patients: propofol-based vs. sevoflurane-based anesthesia. Acta Anaesthesiol Scand 48:162–168
Bourne RS (2008) Delirium and use of sedation agents in intensive care. Nurs Crit Care 13:195–202
Bilotta F, Doronzio A, Stazi E et al (2011) Early postoperative cognitive dysfunction and postoperative delirium after anaesthesia with various hypnotics: study protocol for a randomised controlled trial-The PINOCCHIO trial. Trials 12:170
Carr GV, Bangasser DA, Bethea T et al (2010) Antidepressant-like effects of |[kappa]|-opioid receptor antagonists in Wistar Kyoto rats. Neuropsychopharmacol Off Publ Am Coll Neuropsychopharmacol 35:752–763
Chartoff E, Sawyer A, Rachlin A et al (2012) Blockade of kappa opioid receptors attenuates the development of depressive-like behaviors induced by cocaine withdrawal in rats. Neuropharmacology 62:167–176
Gillman KW, Parker MF, Silva M et al (2013) Design, optimization, and in vivo evaluation of a series of pyridine derivatives with dual NK 1 antagonism and SERT inhibition for the treatment of depression. Bioorg Med Chem Lett 23:407–411
Joensuu M, Tolmunen T, Saarinen PI et al (2007) Reduced midbrain serotonin transporter availability in drug-naïve patients with depression measured by SERT-specific [(123)I] nor-beta-CIT SPECT imaging. Psychiatry Res 154:125–131
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Statement of human and animal rights
This study was approved by the Ethical Review Committee of our hospital.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Jiang, X., Chen, D., Lou, Y. et al. Risk factors for postoperative delirium after spine surgery in middle- and old-aged patients. Aging Clin Exp Res 29, 1039–1044 (2017). https://doi.org/10.1007/s40520-016-0640-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-016-0640-4