Abstract
Introduction
Some studies have shown an increase in alcohol use disorders (AUD) after Roux-en-Y gastric bypass surgery (RYGB), but its relationship with binge eating disorder (BED) has not been fully explored. The purpose of this study was to determine the prevalence of AUD and BED after RYGB and also to evaluate if BED is predictive of late postoperative occurrence of AUD or BED.
Methods
Patients (n = 46) submitted to RYGB, in a tertiary outpatient weight management service at a Federal University of Sao Paulo, Brazil, were tested for BED and AUD using the Questionnaire on Eating and Weight Patterns-Revised (QEWP-R) and AUDIT, respectively. BED was tested before surgery, while both disorders were evaluated with a follow-up period of 12 ± 1.6 years after RYGB.
Results
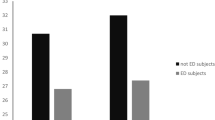
No patients reported AUD before RYBP. After a mean period of 12 years from surgery, ten patients (21.7%) were diagnosed with AUD. Before surgery, BED was present in 24 patients (52.2%) and it was detected in seven out of these 24 patients (29.2%) after RYGB. Thirteen new cases of BED (28.2%) were detected after surgery; total of 20 patients (43.5%) with BED. No association was found between pre- and postsurgery BED (p = 0.148). After RYGB, four out of 24 patients (16.6%) with presurgery BED developed AUD, and no association was found between presurgery BED and postsurgery AUD (p = 0.384). Seven out of ten patients (70%) with AUD after RYGB also developed BED, but no statistical significance was found between these two disorders (p = 0.061).
Conclusion
The presence of BED before RYGB did not predict AUD and BED after RYGB. Nevertheless, factors involved in a possible association between BED and AUD after surgery remain to be determined.
Level of evidence
Level III, cohort study.

Similar content being viewed by others
References
Bruschi Kelles SM, Diniz MFHS, Machado CJ, Barreto SM (2014) Mortality rate after open Roux-in-Y gastric bypass: a 10-year follow-up. Braz J Med Biol Res 47(7):617–625. https://doi.org/10.1590/1414-431X20143578
Sjöström L, Narbro K, Sjöström CD, Karason K, Larsson B, Wedel H, Bengtsson C (2007) Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med 357(8):741–752 https://doi.org/10.1056/NEJMoa066254
Gorrell S et al (2018) Gender differences in relations between alcohol-related compensatory behavior and eating pathology. Eat Weight Disord. https://doi.org/10.1007/s40519-018-0545-7
Thompson-Memmer C, Glassman T, Diehr A (2018) Drunkorexia: a new term and diagnostic criteria. J Am Coll Health 4:1–7. https://doi.org/10.1080/07448481.2018.1500470
Conason A, Teixeira J, Hsu CH, Puma L, Knafo D, Geliebter A (2013) Substance use following bariatric weight loss surgery. JAMA Surg 148(2):145–150. https://doi.org/10.1001/2013.jamasurg.265
Östlund MP, Backman O, Marsk R, Stockeld D, Lagergren J, Rasmussen F, Näslund E (2013) Increased admission for alcohol dependence after gastric bypass surgery compared with restrictive bariatric surgery. JAMA Surg 148(4):374–377. https://doi.org/10.1001/jamasurg.2013.700
Suzuki J, Haimovici F, Chang G (2012) Alcohol use disorders after bariatric surgery. Obes Surg 22(2):201–207. https://doi.org/10.1007/s11695-010-0346-1
White GE et al (2018) Alcohol use thresholds for identifying alcohol-related problems before and following Roux-en-Y gastric bypass. Ann Surg. https://doi.org/10.1097/SLA.0000000000003078
Mechanick JI, Kushner RF, Sugerman HJ, Gonzalez-Campoy JM, Collazo-Clavell ML, Guven S et al (2008) American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic and bariatric surgery medical guidelines for clinical practice for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient. Surg Obes Relat Dis 4(5):S109–S184. https://doi.org/10.1038/oby.2009.28
Segal A, Fandiñob J (2002) Indications and contraindications for performing bariatric operations Bariatric surgery indications and contraindications. Rev Bras Psiquiatr 24(Supl III): 68–72. https://doi.org/10.1590/S1516-44462002000700015
Ivezaj V, Stoeckel LE, Avena NM, Benoit SC, Conason A, Davis JF et al (2017) Obesity and addiction: can a complication of surgery help us understand the connection? Obes Rev 18(7):765–775. https://doi.org/10.1111/obr.12542
Blum K, Bailey J, Gonzalez AM, Oscar-Berman M, Liu Y, Giordano J et al (2012) Neuro-genetics of reward deficiency syndrome (RDS) as the root cause of “addiction transfer”: a new phenomenon common after bariatric surgery. J Genet Syndr Gene Ther. https://doi.org/10.4172/2157-7412.S2-001
Schulte EM, Yokum S, Potenza MN, Gearhardt AN (2016) Neural systems implicated in obesity as an addictive disorder: from biological to behavioral mechanisms. Prog Brain Res 223: 329–346. https://doi.org/10.1016/bs.pbr.2015.07.011
James GA, Gold MS, Liu Y (2004) Interaction of satiety and reward response to food stimulation. J Addict Dis 23(3):23–37. https://doi.org/10.1300/J069v23n03_03
Steffen KJ, Engel SG, Wonderlich JA, Pollert GA, Sondag C (2015) Alcohol and other addictive disorders following bariatric surgery: prevalence, risk factors and possible etiologies. Eur Eat Disord Rev 23(6):442–450. https://doi.org/10.1002/erv.2399
Yoder R, MacNeela P, Conway R, Heary C (2018) How do individuals develop alcohol use disorder after bariatric surgery? A grounded theory exploration. Obes Surg 28(3):717–724
King WC, Chen JY, Mitchell JE, Kalarchian MA, Steffen KJ, Engel SG et al. (2012) Prevalence of alcohol use disorders before and after bariatric surgery. JAMA 307(23): 2516–2525. https://doi.org/10.1001/jama.2012.6147
Mitchell JE, Steffen K, Engel S, King WC, Chen JY, Winters K et al (2015) Addictive disorders after Roux-en-Y gastric bypass. Surg Obes Relat Dis 11(4):897–905. https://doi.org/10.1016/j.soard.2014.10.026
Borges MBF, Morgan CM, Claudino AM, Silveira DXD (2005) Validation of the Portuguese version of the Questionnaire on Eating and Weight Patterns: revised (QEWP-R) for the screening of binge eating disorder. Revista Brasileira de Psiquiatria 27(4):319–322. https://doi.org/10.1590/S1516-44462005000400012
White MA, Kalarchian MA, Masheb RM, Marcus MD, Grilo CM (2010) Loss of control over eating predicts outcomes in bariatric surgery: a prospective 24-month follow-up study. J Clin Psychiatry 71(2):175. https://doi.org/10.4088/JCP.08m04328blu
Méndez EB (1999) Uma versão brasileira do AUDIT (Alcohol Use Disorders Identification Test) [tese], Universidade Federal de Pelotas, Pelotas. https://doi.org/10.1590/S0101-60832012000300005
Macinko J, Mullachery P, Silver D, Jimenez G, Neto OLM (2015) Patterns of alcohol consumption and related behaviors in Brazil: evidence from the 2013 National Health Survey (PNS 2013). PLoS One 10(7):e0134153. https://doi.org/10.1371/journal.pone.0134153
Svensson PA, Anveden Å, Romeo S, Peltonen M, Ahlin S, Burza MA et al (2013) Alcohol consumption and alcohol problems after bariatric surgery in the Swedish obese subjects study. Obesity 21(12):2444–2451. https://doi.org/10.1002/oby.20397
Coluzzi I et al (2018) Alcohol consumption after laparoscopic sleeve gastrectomy: 1-year results. Eat Weight Disord. https://doi.org/10.1007/s40519-018-0486-1
King WC, Chen JY, Courcoulas AP, Dakin GF, Engel SG, Flum DR et al (2017) Alcohol and other substance use after bariatric surgery: prospective evidence from a US multicenter cohort study. Surg Obes Relat Dis 13(8):1392–1402. https://doi.org/10.1016/j.soard.2017.03.021
Mitchell JE, Lancaster KL, Burgard MA, Howell LM, Krahn DD, Crosby RD et al (2001) Long-term follow-up of patients’ status after gastric bypass. Obes Surg 11(4):464–468. https://doi.org/10.1016/j.soard.2017.03.021
Ertelt TW, Mitchell JE, Lancaster K, Crosby RD, Steffen KJ, Marino JM (2008) Alcohol abuse and dependence before and after bariatric surgery: a review of the literature and report of a new data set. Surg Obes Relat Dis 4(5):647–650. https://doi.org/10.1016/j.soard.2008.01.004
Cederbaum AI (2012) Alcohol metabolism. Clin Liver Dis 16(4):667–685. https://doi.org/10.1016/j.cld.2012.08.002
Pepino MY, Okunade AL, Eagon JC, Bartholow BD, Bucholz K, Klein S (2015) Effect of Roux-en-Y gastric bypass surgery: converting 2 alcoholic drinks to 4. JAMA surgery 150(11):1096–1098. https://doi.org/10.1001/jamasurg.2015.1884
Walther L, Brodén CM, Isaksson A, Hedenbro JL (2018) Alcohol consumption in obese patients before and after gastric bypass as assessed with the alcohol marker phosphatidylethanol (PEth). Obes Surg. https://doi.org/10.1007/s11695-018-3165-4
Spadola CE et al (2018) A qualitative examination of increased alcohol use after bariatric surgery among racially/ethnically diverse young adults. Obes Surg 28(6):1492–1497. https://doi.org/10.1007/s11695-017-3022-x
Polston JE, Pritchett CE, Tomasko JM, Rogers AM, Leggio L, Thanos PK, Hajnal A (2013) Roux-en-Y gastric bypass increases intravenous ethanol self-administration in obese rats. PLoS One 8(12):e83741. https://doi.org/10.1371/journal.pone.0083741
Blumenthal DM, Gold MS (2010) Neurobiology of food addiction. Curr Opin Clin Nutr Metab Care 13(4):359–365. https://doi.org/10.1097/MCO.0b013e32833ad4d4
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the ethics committee of Universidad Federal de São Paulo and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Freire, C.C., Zanella, M.T., Arasaki, C.H. et al. Binge eating disorder is not predictive of alcohol abuse disorders in long-term follow-up period after Roux-en-Y gastric bypass surgery. Eat Weight Disord 25, 637–642 (2020). https://doi.org/10.1007/s40519-019-00663-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-019-00663-2