Abstract
Purpose
To evaluate the effectiveness of all radioprotective measures in underage patients who undergo a dental radiodiagnostic examination.
Methods
A systematic review was performed including randomised controlled trials (RCTs), or cluster trials, cohort studies, cross-sectional studies, case–control studies and comparative in vitro research. These studies examined the healthy underage human population (below 18 years) undergoing a dental radiodiagnostic examination. All radioprotective measures were included except for justification as an intervention. The primary outcomes were in vivo mortality and morbidity. Some surrogate or indirect outcomes such as in vitro effective dose and organ absorbed doses were also accepted. Secondary outcomes with regards to image quality and therapeutic value were also analysed.
Results
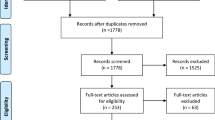
Eighteen papers were eligible for implementation. Fifteen studies underwent narrative synthesis. Regression analysis was performed on three studies.
Conclusion
The following radioprotective measures can reduce the exposure dose. For lateral cephalometry: collimation, filtration, the fastest receptor type and circumstantial thyroid shielding. For oblique lateral radiographs: the shortest exposure time, a smaller horizontal angulation, a longer focus to skin distance. For intraoral radiography: rectangular collimation, the fastest image receptor speed and thyroid shielding when the thyroid gland is in line of or very close to the primary beam. For panoramic radiographs: collimation, the fastest receptor type and the use of automatic exposure control (AEC) or manual adjustment of intensity. For cone-beam computed tomography: collimation, the largest voxels size in relation to the treatment need, change in image settings such as ultra-low dose settings, shorter exposure time, a lower amount of projections, lower beam intensity, reduction of the potential, use of a thyroid shield except in two situations and the use of AEC. All of the changes in exposure parameters should be performed while maintaining a sufficient therapeutic value on an individual and indication-based level.


Similar content being viewed by others
References
Al Najjar A, Colosi D, Dauer LT, Prins R, Patchell G, Branets I, et al. Comparison of adult and child radiation equivalent doses from 2 dental cone-beam computed tomography units. Am J Orthod Dentofacial Orthop. 2013;143(6):784–92. https://doi.org/10.1016/j.ajodo.2013.01.013.
Alcaraz M, Garcia-Vera MC, Bravo LA, Martinez-Beneyto Y, Armero D, Morant JJ, et al. Collimator with filtration compensator: clinical adaptation to meet European Union recommendation 4F on radiological protection for dental radiography. Dentomaxillofac Radiol. 2009;38(6):413–20. https://doi.org/10.1259/dmfr/15580890.
Aps JK. Cone beam computed tomography in paediatric dentistry: overview of recent literature. Eur Arch Paediatr Dent. 2013a;14(3):131–40. https://doi.org/10.1007/s40368-013-0029-4.
Aps JK. Three-dimensional imaging in paediatric dentistry: a must-have or you’re not up-to-date? Eur Arch Paediatr Dent. 2013b;14(3):129–30. https://doi.org/10.1007/s40368-013-0034-7.
Aps JK. To beam or not to beam: that is the question. Dentomaxillofac Radiol. 2013c;42(2):20120375. https://doi.org/10.1259/dmfr.20120375.
Aps JK, Scott JM. Oblique lateral radiographs and bitewings; estimation of organ doses in head and neck region with Monte Carlo calculations. Dentomaxillofac Radiol. 2014;43(6):20130419. https://doi.org/10.1259/dmfr.20130419.
Arai Y, Tammisalo E, Iwai K, Hashimoto K, Shinoda K. Development of a compact computed tomographic apparatus for dental use. Dentomaxillofac Radiol. 1999;28(4):245–8. https://doi.org/10.1038/sj/dmfr/4600448.
Berkhout WE, Sanderink GC, Van der Stelt PF. Does digital radiography increase the number of intraoral radiographs? A questionnaire study of Dutch dental practices. Dentomaxillofac Radiol. 2003;32(2):124–7. https://doi.org/10.1259/dmfr/97410196.
Bramer WM, Giustini D, de Jonge GB, Holland L, Bekhuis T. De-duplication of database search results for systematic reviews in EndNote. J Med Libr Assoc. 2016;104(3):240–3. https://doi.org/10.3163/1536-5050.104.3.014.
Brasil DM, Pauwels R, Coucke W, Haiter-Neto F, Jacobs R. Image quality optimization of narrow detector dental computed tomography for paediatric patients. Dentomaxillofac Radiol. 2019. https://doi.org/10.1259/dmfr.20190032.
Brenner D, Elliston C, Hall E, Berdon W. Estimated risks of radiation-induced fatal cancer from pediatric CT. Am J Roentgenol. 2001;176(2):289–96. https://doi.org/10.2214/ajr.176.2.1760289.
Brenner DJ, Doll R, Goodhead DT, Hall EJ, Land CE, Little JB, et al. Cancer risks attributable to low doses of ionizing radiation: assessing what we really know. Proc Natl Acad Sci USA. 2003;100(24):13761–6. https://doi.org/10.1073/pnas.2235592100.
Crane GD, Abbott PV. Radiation shielding in dentistry: an update. Aust Dent J. 2016;61(3):277–81. https://doi.org/10.1111/adj.12389.
Dauer LT, Branets I, Stabulas-Savage J, Quinn B, Miodownik D, Dauer ZL, et al. Optimising radiographic bitewing examination to adult and juvenile patients through the use of anthropomorphic phantoms. Radiat Prot Dosimetry. 2014;158(1):51–8. https://doi.org/10.1093/rpd/nct196.
Davis AT, Safi H, Maddison SM. The reduction of dose in paediatric panoramic radiography: the impact of collimator height and programme selection. Dentomaxillofac Radiol. 2015;44(2):20140223. https://doi.org/10.1259/dmfr.20140223.
de Las Heras Gala H, Schofer F, Schofer H, Sanchez Casanueva RM, Zervides C, Mair K, et al. A patient-centric approach to quality control and dosimetry in CT including CBCT. Phys Med. 2018;47:92–102. https://doi.org/10.1016/j.ejmp.2018.02.005.
Espelid I, Mejare I, Weerheijm K. EAPD guidelines for use of radiographs in children. Eur J Paediatr Dent. 2003;4(1):40–8.
EzEldeen M, Stratis A, Coucke W, Codari M, Politis C, Jacobs R. As low dose as sufficient quality: optimization of cone-beam computed tomographic scanning protocol for tooth autotransplantation planning and follow-up in children. J Endod. 2017;43(2):210–7. https://doi.org/10.1016/j.joen.2016.10.022.
Fryback DG, Thornbury JR. The efficacy of diagnostic imaging. Med Decis Making. 1991;11(2):88–94. https://doi.org/10.1177/0272989X9101100203.
García Vera MdC. Reducción de dosis en la telerradiografía lateral de cráneo en pediatría: nueva técnica de colimación con filtración compensada. 2006.
Gavala S, Donta C, Tsiklakis K, Boziari A, Kamenopoulou V, Stamatakis HC. Radiation dose reduction in direct digital panoramic radiography. Eur J Radiol. 2009;71(1):42–8. https://doi.org/10.1016/j.ejrad.2008.03.018.
Gijbels F, Jacobs R, Bogaerts R, Debaveye D, Verlinden S, Sanderink G. Dosimetry of digital panoramic imaging. Part I: Patient exposure. Dentomaxillofac Radiol. 2005;34(3):145–9. https://doi.org/10.1259/dmfr/28107460.
Guerrero ME, Noriega J, Castro C, Jacobs R. Does cone-beam CT alter treatment plans? Comparison of preoperative implant planning using panoramic versus cone-beam CT images. Imaging Sci Dent. 2014;44(2):121–8. https://doi.org/10.5624/isd.2014.44.2.121.
Guyatt G, Oxman AD, Akl EA, Kunz R, Vist G, Brozek J, et al. GRADE guidelines: 1. Introduction—GRADE evidence profiles and summary of findings tables. J Clin Epidemiol. 2011;64(4):383–94.
Gwet K. Kappa statistic is not satisfactory for assessing the extent of agreement between raters. Stat Methods Inter-rater Reliab Assess. 2002;1(6):1–6.
Hayakawa Y, Kobayashi N, Kuroyanagi K, Nishizawa K. Paediatric absorbed doses from rotational panoramic radiography. Dentomaxillofac Radiol. 2001;30(5):285–92. https://doi.org/10.1038/sj/dmfr/4600625.
Hedesiu M, Marcu M, Salmon B, Pauwels R, Oenning AC, Almasan O, et al. Irradiation provided by dental radiological procedures in a pediatric population. Eur J Radiol. 2018;103:112–7. https://doi.org/10.1016/j.ejrad.2018.04.021.
Hidalgo A, Davies J, Horner K, Theodorakou C. Effectiveness of thyroid gland shielding in dental CBCT using a paediatric anthropomorphic phantom. Dentomaxillofac Radiol. 2015;44(3):20140285. https://doi.org/10.1259/dmfr.20140285.
Horner K, Rushton V, Tsiklakis K, Hirschmann PN, van der Stelt PF, Glenny A-M et al. European guidelines on radiation protection in dental radiology; the safe use of radiographs in dental practice. European Commission, Directorate-General for Energy and Transport. Radiation Protection: EU2004 2004. Report No.: 92-984-5958-1.
ICRP. The 1990 recommendations of the international commission on radiological protection. ICRP publication 60. Ann ICRP. 1991;21(1–3).
ICRP. The 2007 recommendations of the international commission on radiological protection. ICRP publication 103. Ann ICRP. 2007;37(2–4):1–332. https://doi.org/10.1016/j.icrp.2007.10.003.
ICRP. Managing patient dose in digital radiology. ICRP Publication 93. Ann ICRP 2004;34.
Johnson KB, Ludlow JB, Mauriello SM, Platin E. Reducing the risk of intraoral radiographic imaging with collimation and thyroid shielding. Gen Dent. 2014;62(4):34–40.
Kaeppler G, Dietz K, Reinert S. Diagnostic accuracy of in vitro panoramic radiographs depending on the exposure. Dentomaxillofac Radiol. 2007a;36(2):68–74. https://doi.org/10.1259/dmfr/53852973.
Kaeppler G, Dietz K, Reinert S. Possibilities of dose reduction in lateral cephalometric radiographs and its effects on clinical diagnostics. Dentomaxillofac Radiol. 2007b;36(1):39–44. https://doi.org/10.1259/dmfr/15761373.
Khong PL, Ringertz H, Donoghue V, Frush D, Rehani M, Appelgate K, et al. ICRP publication 121: radiological protection in paediatric diagnostic and interventional radiology. Ann ICRP. 2013;42(2):1–63. https://doi.org/10.1016/j.icrp.2012.10.001.
Kleinerman RA. Cancer risks following diagnostic and therapeutic radiation exposure in children. Pediatr Radiol. 2006;36(Suppl 2):121–5. https://doi.org/10.1007/s00247-006-0191-5.
Land CE. Estimating cancer risks from low doses of ionizing radiation. Science. 1980;209(4462):1197–203.
Little MP. Heterogeneity of variation of relative risk by age at exposure in the Japanese atomic bomb survivors. Radiat Environ Biophys. 2009;48(3):253–62.
Little MP, Wakeford R, Tawn EJ, Bouffler SD, Berrington de Gonzalez A. Risks associated with low doses and low dose rates of ionizing radiation: why linearity may be (almost) the best we can do. Radiology. 2009;251(1):6–12. https://doi.org/10.1148/radiol.2511081686.
Ludlow JB. A manufacturer’s role in reducing the dose of cone beam computed tomography examinations: effect of beam filtration. Dentomaxillofac Radiol. 2011;40(2):115–22. https://doi.org/10.1259/dmfr/31708191.
Ludlow JB, Ivanovic M. Comparative dosimetry of dental CBCT devices and 64-slice CT for oral and maxillofacial radiology. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;106(1):106–14. https://doi.org/10.1016/j.tripleo.2008.03.018.
Ludlow JB, Koivisto J. Dosimetry of orthodontic diagnostic FOVs using low dos CBCT protocol. 2015 IADR/AADR/CADR General Session & Exhibition; Boston, USA2015.
Ludlow JB, Walker C. Assessment of phantom dosimetry and image quality of i-CAT FLX cone-beam computed tomography. Am J Orthod Dentofacial Orthop. 2013;144(6):802–17. https://doi.org/10.1016/j.ajodo.2013.07.013.
Ludlow JB, Davies-Ludlow LE, White SC. Patient risk related to common dental radiographic examinations: the impact of 2007 International Commission on Radiological Protection recommendations regarding dose calculation. J Am Dent Assoc. 2008;139(9):1237–43. https://doi.org/10.14219/jada.archive.2008.0339.
Ludlow JB, Timothy R, Walker C, Hunter R, Benavides E, Samuelson DB. Correction to Effective dose of dental CBCT–a meta analysis of published data and additional data for nine CBCT units. Dentomaxillofac Radiol. 2015a;44(7):20159003. https://doi.org/10.1259/dmfr.20159003.
Ludlow JB, Timothy R, Walker C, Hunter R, Benavides E, Samuelson DB, et al. Effective dose of dental CBCT-a meta analysis of published data and additional data for nine CBCT units. Dentomaxillofac Radiol. 2015b;44(1):20140197. https://doi.org/10.1259/dmfr.20140197.
Marcu M, Hedesiu M, Salmon B, Pauwels R, Stratis A, Oenning ACC, et al. Estimation of the radiation dose for pediatric CBCT indications: a prospective study on ProMax3D. Int J Paediatr Dent. 2018;28(3):300–9. https://doi.org/10.1111/ipd.12355.
Mazonakis M, Damilakis J, Raissaki M, Gourtsoyiannis N. Radiation dose and cancer risk to children undergoing skull radiography. Pediatr Radiol. 2004;34(8):624–9.
Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009a;151(4):264–9.
Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009b;6(7):e1000097. https://doi.org/10.1371/journal.pmed1000097.
Mota de Almeida FJ, Knutsson K, Flygare L. The effect of cone beam CT (CBCT) on therapeutic decision-making in endodontics. Dentomaxillofac Radiol. 2014;43(4):20130137. https://doi.org/10.1259/dmfr.20130137.
Mozzo P, Procacci C, Tacconi A, Martini PT, Andreis IA. A new volumetric CT machine for dental imaging based on the cone-beam technique: preliminary results. Eur Radiol. 1998;8(9):1558–64.
Nemtoi A, Czink C, Haba D, Gahleitner A. Cone beam CT: a current overview of devices. Dentomaxillofac Radiol. 2013;42(8):20120443. https://doi.org/10.1259/dmfr.20120443.
Oenning AC, Jacobs R, Pauwels R, Stratis A, Hedesiu M, Salmon B, et al. Cone-beam CT in paediatric dentistry: dIMITRA project position statement. Pediatr Radiol. 2017. https://doi.org/10.1007/s00247-017-4012-9.
Oenning AC, Pauwels R, Stratis A, De Faria Vasconcelos K, Tijskens E, De Grauwe A, et al. Halve the dose while maintaining image quality in paediatric Cone Beam CT. Sci Rep. 2019;9(1):5521. https://doi.org/10.1038/s41598-019-41949-w.
Pakbaznejad Esmaeili E, Ekholm M, Haukka J, Evalahti M, Waltimo-Siren J. Are children’s dental panoramic tomographs and lateral cephalometric radiographs sufficiently optimized? Eur J Orthod. 2016;38(1):103–10. https://doi.org/10.1093/ejo/cjv076.
Panmekiate S, Rungwittayathon P, Suptaweeponboon W, Tangtraitham N, Pauwels R. Optimization of exposure parameters in dental cone beam computed tomography using a 3-step approach. Oral Surg Oral Med Oral Pathol Oral Radiol. 2018;126(6):545–52. https://doi.org/10.1016/j.oooo.2018.08.004.
Pauwels R, Beinsberger J, Collaert B, Theodorakou C, Rogers J, Walker A, et al. Effective dose range for dental cone beam computed tomography scanners. Eur J Radiol. 2012;81(2):267–71. https://doi.org/10.1016/j.ejrad.2010.11.028.
Pauwels R, Cockmartin L, Ivanauskaite D, Urboniene A, Gavala S, Donta C, et al. Estimating cancer risk from dental cone-beam CT exposures based on skin dosimetry. Phys Med Biol. 2014a;59(14):3877–91. https://doi.org/10.1088/0031-9155/59/14/3877.
Pauwels R, Silkosessak O, Jacobs R, Bogaerts R, Bosmans H, Panmekiate S. A pragmatic approach to determine the optimal kVp in cone beam CT: balancing contrast-to-noise ratio and radiation dose. Dentomaxillofac Radiol. 2014b;43(5):20140059. https://doi.org/10.1259/dmfr.20140059.
Pauwels R, Araki K, Siewerdsen JH, Thongvigitmanee SS. Technical aspects of dental CBCT: state of the art. Dentomaxillofac Radiol. 2015;44(1):20140224. https://doi.org/10.1259/dmfr.20140224.
Pauwels R, Horner K, Vassileva J, Rehani MM. Thyroid shielding in cone beam computed tomography: recommendations towards appropriate use. Dentomaxillofac Radiol. 2019;48(7):20190014. https://doi.org/10.1259/dmfr.20190014.
Popay J, Roberts H, Sowden A, Petticrew M, Arai L, Rodgers M, et al. Guidance on the conduct of narrative synthesis in systematic reviews. Product ESRC Methods Progr Vers. 2006;1:b92.
Preston DL, Cullings H, Suyama A, Funamoto S, Nishi N, Soda M, et al. Solid cancer incidence in atomic bomb survivors exposed in utero or as young children. J Natl Cancer Inst. 2008;100(6):428–36. https://doi.org/10.1093/jnci/djn045.
Prins R, Dauer LT, Colosi DC, Quinn B, Kleiman NJ, Bohle GC, et al. Significant reduction in dental cone beam computed tomography (CBCT) eye dose through the use of leaded glasses. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112(4):502–7. https://doi.org/10.1016/j.tripleo.2011.04.041.
R Core Team. R: A language and environment for statistical computing. 2013.
Robb J. Estimates of radiation detriment in a UK population: National Radiological Protection Board. 1994.
Rush E, Thompson N. Dental radiography technique and equipment: how they influence the radiation dose received at the level of the thyroid gland. Radiography. 2007;13(3):214–20.
Sansare KP, Khanna V, Karjodkar F. Utility of thyroid collars in cephalometric radiography. Dentomaxillofac Radiol. 2011;40(8):471–5. https://doi.org/10.1259/dmfr/25040799.
Scarfe WC, Farman AG. What is cone-beam CT and how does it work? Dent Clin N Am. 2008;52(4):707–30. https://doi.org/10.1016/j.cden.2008.05.005.
Schmidt K, Velders XL, van Ginkel FC, van der Stelt PF. The use of a thyroid collar for intraoral radiography. Ned Tijdschr Tandheelkd. 1998;105(6):209–12.
Sedentexct. Radiation protection no 172: cone beam CT for dental and maxillofacial radiology. Evidence based guidelines. European commision. 2012. http://www.sedentexct.eu/files/radiation_protection_172.pdf. Accessed 03 June 2014.
Shetty A, Almeida FT, Ganatra S, Senior A, Pacheco-Pereira C. Evidence on radiation dose reduction using rectangular collimation: a systematic review. Int Dent J. 2018. https://doi.org/10.1111/idj.12411.
Shin HS, Nam KC, Park H, Choi HU, Kim HY, Park CS. Effective doses from panoramic radiography and CBCT (cone beam CT) using dose area product (DAP) in dentistry. Dentomaxillofac Radiol. 2014;43(5):20130439. https://doi.org/10.1259/dmfr.20130439.
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J. Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg. 2003;73(9):712–6.
Stenstrom B, Henrikson CO, Holm B, Richter S. Absorbed doses from intraoral radiography with special emphasis on collimator dimensions. Swed Dent J. 1986;10(1–2):59–71.
Stratis A, Zhang G, Jacobs R, Bogaerts R, Bosmans H. Rotating and translating anthropomorphic head voxel models to establish an horizontal Frankfort plane for dental CBCT Monte Carlo simulations: a dose comparison study. Phys Med Biol. 2016a;61(24):N681–96. https://doi.org/10.1088/1361-6560/61/24/n681.
Stratis A, Zhang G, Lopez-Rendon X, Jacobs R, Bogaerts R, Bosmans H. Customisation of a Monte Carlo dosimetry tool for dental cone-beam Ct systems. Radiat Prot Dosimetry. 2016b;169(1–4):378–85. https://doi.org/10.1093/rpd/ncw024.
Theodorakou C, Walker A, Horner K, Pauwels R, Bogaerts R, Dds RJ. Estimation of paediatric organ and effective doses from dental cone beam CT using anthropomorphic phantoms. Br J Radiol. 2012;85(1010):153–60. https://doi.org/10.1259/bjr/19389412.
Tubiana M, Feinendegen LE, Yang C, Kaminski JM. The linear no-threshold relationship is inconsistent with radiation biologic and experimental data. Radiology. 2009;251(1):13–22. https://doi.org/10.1148/radiol.2511080671.
UNSCEAR. Report to the general assmebly. Volume II: scientific Annex B: effects of radiation exposure of children. 2013.
UNSCEAR. Effects of ionizing radiation (exposure from natural sources of radiation), New York, 1993. 2017.
Whaites E. Essentials of dental radiography and radiology. 4th ed. London: Churchill Livingstone; 2007.
White SC, Mallya SM. Update on the biological effects of ionizing radiation, relative dose factors and radiation hygiene. Aust Dent J. 2012;57(Suppl 1):2–8. https://doi.org/10.1111/j.1834-7819.2011.01665.x.
Yepes JF, Booe MR, Sanders BJ, Jones JE, Ehrlich Y, Ludlow JB, et al. Pediatric phantom dosimetry of Kodak 9000 cone-beam computed tomography. Pediatr Dent. 2017;39(3):229–32.
Acknowledgements
We thank Prof Johan Aps, (Univ Western Australia, Division Oral Diagnostic & Surgical Sciences, Perth, WA, Australia) for feedback on construction of the search strategy and feedback on the preliminary manuscript. Dr Ellen de Schepper, (Biostatistics Unit, Department of Public Health, Ghent University, Ghent) for the work on the statistical analysis.
Funding
This study did receive partial funding from the EAPD, providing the licence to the reviewing software used for study selection. A small part of the financing was utilised for the purchase of necessary literature.
Author information
Authors and Affiliations
Contributions
JWGVA is the guarantor, JWGVA, SR and NP drafted the protocol. JWGVA and NP developed the search strategy with feedback from all authors. JWGVA and SR performed the selection of the articles. JWGVA and SR performed data extraction. JWGVA and SR performed the quality assessment. All authors read, provided feedback and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no conflict of interest. Ghent University (UGent) is the Sponsor of this study. The EAPD and UGent are not involved in any other aspect of the project, such as the design of the project’s protocol and analysis plan, the collection, analyses and interpretation of the study results. This manuscript is one of the four systematic reviews that form the base for the renewal of the ‘EAPD guidelines for use of radiographs in children’ (Espelid et al. 2003). The policy document distracted from this review is a policy document on clinical practice and future research on the topic and is published open access on the EAPD website (http://www.eapd.eu/index.php/policies-and-guidelines). The protocol and preliminary results of this study were communicated on the 11th EAPD interim seminar (3–4 May 2019) to representatives of organisations in paediatric dentistry.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Van Acker, J.W.G., Pauwels, N.S., Cauwels, R.G.E.C. et al. Outcomes of different radioprotective precautions in children undergoing dental radiography: a systematic review. Eur Arch Paediatr Dent 21, 463–508 (2020). https://doi.org/10.1007/s40368-020-00544-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40368-020-00544-8