Abstract
Background
Molecular tests are the mainstay of detecting severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). However, their accessibility can be limited by the long examination time and inability to evaluate multiple samples at once.
Objective
This study evaluated the analytical performance of the newly developed rapid molecular assays GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B.
Method
This prospective study was conducted between 14 December 2020 and 9 January 2021 at a polymerase chain reaction (PCR) center. Samples were collected from the nasopharynx with flocked swabs. Molecular tests were performed with the GENECUBE® system and reference reverse transcription (RT)-PCR, and the results of the two assays were compared.
Result
Among 1065 samples, 81 (7.6%) were positive for SARS-CoV-2 on the reference RT-PCR. Three showed discordance between GENECUBE® HQ SARS-CoV-2 and the reference RT-PCR; the total, positive, and negative samples of concordance for the two assays were 99.7%, 100%, and 99.7%, respectively. All discordant cases were positive with GENECUBE® HQ SARS-CoV-2 and negative with the reference RT-PCR. SARS-CoV-2 was detected in all three samples using another molecular assay for SARS-CoV-2. For GENECUBE® FLU A/B, the total, positive, and negative samples of concordance for the two assays were 99.5%, 100%, and 99.1%.
Conclusion
The GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B demonstrated sufficient analytical performance to detect SARS-CoV-2 and influenza virus A/B.
Similar content being viewed by others
We prospectively evaluated the analytical performance of the newly developed rapid molecular assays GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B. |
The two assays showed a >99% concordance rate compared with a reference polymerase chain reaction, which indicated sufficient analytical performance to detect severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and influenza virus A/B. |
1 Introduction
The severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), which causes coronavirus disease 2019 (COVID-19), has rapidly spread worldwide [1]. The healthcare system was globally inundated with patients with COVID-19 and suffered a detrimental burden [1]. During the pandemic, the timely and accurate identification of patients with SARS-CoV-2 is essential for early isolation and treatment [2].
Several guidelines have recommended nucleic acid amplification tests (NAATs) be used for SARS-CoV-2 testing because of their high sensitivity and specificity [3, 4]. However, conventional NAATs usually take several hours to days to provide results [5] and cannot concurrently detect other respiratory viruses with similar manifestations to SARS-CoV-2. To overcome these drawbacks, automated multiplex polymerase chain reaction (PCR) systems capable of detecting multiple respiratory pathogens in a short period of time have been developed [6].
GENECUBE® (TOYOBO Co., Ltd., Osaka, Japan) is a rapid, fully automated genetic analyzer that uses the Qprobe-PCR method [7]. The system automatically prepares reaction mixtures and amplifies and detects target genes in a short time and can analyze up to eight samples and four items at the same time in a single run. GENECUBE® has been applied for several pathogens, including Mycobacterium tuberculosis [8], M. avium, M. intracellulare, Neisseria gonorrhoeae [9], Chlamydia trachomatis [9], Mycoplasma pneumoniae [7, 10], Staphylococcus aureus (nuc and mecA) [11], and the toxin gene of Clostridioides difficile [12].
To evaluate the SARS-CoV-2 and influenza A/B virus, the authors of the present study (HS and AS) created two new molecular assays named GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B, which were approved in Japan in October and December 2020, respectively. The GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B can be performed simultaneously or independently within approximately 25 minutes using purified or heat-inactivated respiratory samples.
In this study, we evaluated the analytical performance of GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B.
2 Methods
A prospective comparison between the GENECUBE® examination and reference real-time PCR method was performed with nasopharyngeal samples obtained between 14 December 2020 and 9 January 2021 at a PCR center in Tsukuba, Ibaraki Prefecture, Japan. During the COVID-19 endemic period, sample collection for PCR in the Tsukuba district was intensively performed at a drive-through facility at the PCR center in Tsukuba Medical Center Hospital (TMCH) following a referral from a local public health center and 63 primary care facilities and among healthcare workers at TMCH. Because of the low prevalence rate of influenza and the lack of fresh samples, we used preserved universal transport medium™ (UTM™) samples, provided a sufficient amount was remaining. The samples had initially been used for our previous studies [13, 14] and stored at -80 °C; most of them were collected during the endemic season of 2017–2018. After thawing, these samples simultaneously underwent both the GENECUBE® FLU A/B assays and a reference real-time reverse transcription (RT)-PCR examination.
The ethics committee of TMCH approved the present study (approval number: 2020-046), and informed consent was obtained from patients for their participation in the part of the current research that used fresh samples.
2.1 Sample Collection and Procedures for Comparisons
For sample collections, we obtained a nasopharyngeal sample for PCR with FLOQSwab™ (Copan Italia S.p.A., Brescia, Italy) as previously described [15]. The swab sample was diluted in 3 mL of UTM™ (Copan Italia S.p.A.), and the UTM™ was then transferred to a microbiology laboratory located next to the drive-through sample-collecting facility of the PCR center.
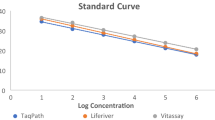
After obtaining the UTM™ samples, purification and RNA extraction were performed with a magLEAD 6gC (Precision System Science Co., Ltd., Chiba, Japan) from 200 µL aliquots of UTM™. The RNA was eluted in 100 µL for GENECUBE®, then a reference real-time RT-PCR examination was performed with the LightCycler® 96 Real-Time PCR System (Roche, Basel, Switzerland) using a method developed by the National Institute of Infectious Diseases (NIID), Japan, for SARS-CoV-2 [16] and influenza virus [17]. In brief, 5 μL of the extracted RNA was used for one-step quantitative RT-PCR with the THUNDERBIRD® Probe One-step qRT-PCR kit (TOYOBO Co., Ltd., Osaka, Japan). The EDX SARS-CoV-2 standard (Exact Diagnostics, Fort Worth, TX, USA) was used to make a standard curve for quantification. Regarding the reference real-time RT-PCR examination for influenza virus type A/B, AMPLIRUN® INFLUENZA RNA CONTROL (Vircell, Granada, Spain) was used as a standard. The quality of extraction compared with the QIAamp® Viral RNA Mini Kit (QIAGEN N.V., Hilden, Germany) is summarized in Table 1a, b in the electronic supplementary material (ESM). A duplicate analysis for N2 genes was performed for the evaluation of SARS-CoV-2.
If discordance was recognized between GENECUBE® and the reference real-time RT-PCR, a re-evaluation was performed with an Xpert® Xpress SARS-CoV-2 and GeneXpert® (Cepheid Inc., Sunnyvale, CA, USA) for SARS-CoV-2 [18] and with the Biofire® FilmArray® Respiratory Panel version 2.1 (BioFire Diagnostics, Salt Lake City, UT, USA) for the influenza virus [19]. As additional comparisons, heat extraction was performed for GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B and compared with the reference real-time RT-PCR.
2.2 GENECUBE® Assay Evaluation with GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B
GENECUBE® can analyze SARS-CoV-2 and the influenza virus simultaneously or independently according to the examiner’s request using the GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B. The RT-PCR conditions were as follows: reverse transcription reaction 42 °C for 2 min, denaturation at 97 °C for 15 s, and 50 cycles of 97 °C for 1 s, 58 °C for 3 s, and 63 °C for 5 s. Each ramp rate was approximately 2.4 °C/s for 42 °C, 14.6 °C/s for 97 °C, 7.0 °C/s for 58 °C, and 2.4 °C/s for 63 °C. The RT-PCR products were subjected to a melting point analysis, the conditions of which were as follows: 94 °C for 30 s and 39 °C for 30 s, followed by heating from 40 to 75 °C in increments of 0.40 °C/s. Data were analyzed automatically and displayed on the GENECUBE® monitor after completion of the assay evaluation (Fig. 1A).
Workflow of the two extraction methods for the GENECUBE® assay in this study. A For the automated purification method, viral RNA extraction was performed with a magLEAD 6gC from 200-µL aliquots of universal transport medium™ (UTM™). The RNA was eluted in 100 µL for the GENECUBE® assay. B For the heat-extraction method, 100-µL aliquots of UTM™ were mixed with 10 μL of proteinase K solution and heated at 65 °C for 5 minutes and 95 °C for 5 minutes. The inactivated samples were then diluted with an equal volume of lysis buffer and used for the GENECUBE® assay
For the GENECUBE® examination with the heat-extraction method, 100 µL aliquots of UTM™ were mixed with 10 μL of proteinase K solution (Kanto Chemical Co., Inc., Tokyo, Japan) and heated at 65 °C for 5 min and 95 °C for 5 min. The inactivated samples were diluted with an equal volume of lysis buffer and used for the assay evaluation (Fig. 1B).
2.3 Evaluation of the Limit of Detection and the Feasibility of Pooled Testing for GENECUBE® HQ SARS-CoV-2
To evaluate the limit of detection (LOD), 12 fresh SARS-CoV-2-positive UTM™ samples obtained within 3 days before the evaluation were measured for their viral loads and diluted with UTM™ to approximate concentrations of <100 copies/test and < 10 copies/test (Table 2 in the ESM). In total, 24 positive samples were prepared for the evaluation of LODs and measured in quadruplicate for three examination methods: the reference RT-PCR method, GENECUBE® with the automated purification method, and GENECUBE® with the heat-extraction method. To validate the LODs obtained from the 24 samples, we also made six different concentrations of samples (5 copies/μL, 2.5 copies/μL, 1.25 copies/μL, 0.625 copies/μL, 0.3125 copies/μL, 0.15625 copies/μL) from SARS-CoV-2 reference material (AccuPlex™ SARS-CoV-2 Reference Material Kit, SeraCare; SeraCare Life Sciences, Inc., Milford, MA, USA) and UTM™ and evaluated each sample ten times.
The feasibility of pooled testing for GENECUBE® HQ SARS-CoV-2 was also evaluated. A pool size of five was chosen according to the protocol for pooled sample testing for COVID-19 established by the Ministry of Health, Labour and Welfare of Japan. For the pooled analysis, 60 pooled samples were prepared: 20 of five pooled negative samples, 20 of four pooled negative samples, and one low viral load sample (30 < cycle threshold [Ct] value < 35), 20 of four pooled negative samples, and one moderate to high viral load sample (Ct value < 30). The RNA was extracted with a magLEAD 6gC from 200 µL aliquots of UTM™ and eluted in 50 µL; purified samples were then evaluated using GENECUBE® HQ SARS-CoV-2 and reference real-time RT-PCR.
Fresh positive influenza virus UTM™ samples were not obtained during the study, and the LOD study was not performed for GENECUBE® FLU A/B.
2.4 Statistical Analyses
The positive concordance rate, negative concordance rate, and total concordance rate of the GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B compared with reference real-time RT-PCR were calculated using the Clopper and Pearson methods with 95% confidence intervals. All calculations were conducted using the R 3.3.1 software program (The R Foundation, Vienna, Austria).
3 Results
3.1 Analytical Sensitivity of GENECUBE® HQ SARS-CoV-2
The results of the LOD evaluation are summarized in Tables 1 and 2. For the examination with fresh SARS-CoV-2-positive UTM™ samples (Table 1), reference RT-PCR correctly detected as few as 5 copies/test, whereas GENECUBE® with the automated extraction method detected as few as 6 copies/test as determined by the reference RT-PCR examination, and GENECUBE® with the heat-extraction method detected as few as 17 copies/test as determined by the reference RT-PCR examination. For the reproducibility test with reference material (Table 2), GENECUBE® with the automated extraction method detected 100% (10/10) of 1.25 copies/μL sample (12.2 copies/test determined by the reference RT-PCR), and GENECUBE® with the heat-extraction method also detected 100% (10/10) of 5 copies/μL sample (56.8 copies/test determined by the reference RT-PCR).
3.2 Comparison of GENECUBE® HQ SARS-CoV-2 and Reference RT-PCR
During the study period, we evaluated 1065 nasopharyngeal samples. Of these, 486 (45.6%) were obtained from symptomatic patients and 579 (54.4%) were obtained from asymptomatic patients. Reference RT-PCR provided positive results for 81 samples, with a median Ct value of 18.5 (Ct < 20, n = 49; 20 ≤ Ct < 30, n = 25; 30 ≤ Ct, n = 7).
The comparison of the GENECUBE® HQ SARS-CoV-2 assay with the reference RT-PCR for purified samples is summarized in Table 3. The total, positive, and negative concordance of the two assays was 99.7% (1062/1065), 100% (81/81), and 99.7% (981/984), respectively. Of the three samples with discordance between the two assays, all samples were negative using the reference RT-PCR assay and positive using the GENECUBE® assay. SARS-CoV-2 was detected in all three samples by the GeneXpert® for SARS-CoV-2 (Table 4).
The comparison of the GENECUBE® HQ SARS-CoV-2 assay with the heat-extraction method with the reference RT-PCR is summarized in Table 3. The total, positive, and negative concordance of the two assays was 99.7% (1062/1065), 97.5% (79/81), and 99.9% (983/984), respectively. Of the three samples with discordance between the two assays, one sample was negative using the reference RT-PCR assay and positive using the GENECUBE® assay with the heat-extraction method. SARS-CoV-2 was detected from the sample by the GeneXpert®for SARS-CoV-2. The other two samples were positive using the reference RT-PCR assay and negative using the GENECUBE® assay with the heat-extraction method (Table 4).
3.3 Evaluation of GENECUBE®HQ SARS-CoV-2 for Pooled Samples
The results of the pooling testing with GENECUBE® HQ SARS-CoV-2 are summarized in Table 3 in the ESM. The GENECUBE® HQ SARS-CoV-2 showed a positive result for every pooled sample with a low viral load (20/20; 100%) and with a moderate-high viral load (20/20; 100%). The reference RT-PCR assay was negative in four pooled samples with low viral load.
3.4 Comparison of GENECUBE® FLU A/B with Reference RT-PCR
The comparison of GENECUBE® FLU A/B assay with the reference RT-PCR is summarized in Table 5. A total of 81 preserved positive UTM™ samples (A: 48 samples, B: 33 samples) were used for the evaluation. Among these 81 positive samples, the sensitivity of antigen testing was 65.4% (53/81).
For purified samples, the total, positive, and negative concordance of the two assays was 99.5% (192/193), 100% (80/80), and 99.1% (112/113), respectively. One sample with discordance between the two assays was negative using the reference RT-PCR assay and positive using the GENECUBE® FLU A/B assay. The influenza virus was not detected from the sample by FilmArray® (Table 6).
The comparison of the GENECUBE® FLU A/B assay with the heat-extraction method with the reference RT-PCR is summarized in Table 5. The total, positive, and negative concordance of the two assays was 97.4% (188/193), 93.8% (75/80), and 100% (113/113), respectively. Of the five samples with discordance between the two assays, all samples were positive using the reference RT-PCR assay and negative using the GENECUBE® FLU A/B assay with heat-extraction method (Table 6).
4 Discussion
In this study, GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B showed high analytical performance. The total concordance rate in clinical samples was over 99% between the two tests. For GENECUBE® FLU A/B, the total concordance rate with the reference RT-PCR was 99.5%. GENECUBE® HQ SARS-CoV-2 provided comparable LODs with the reference RT-PCR and successfully detected SARS-CoV-2 in all positive pooled samples.
The N2 assay of NIID was reported to have a high sensitivity and accuracy for detecting SARS-CoV-2 [20]. For the evaluations using purified samples, three discordant cases existed between GENECUBE® HQ SARS-CoV-2 and the reference real-time RT-PCR. Most molecular examinations accurately detect SARS-CoV-2 [21], but some discordance among different systems has been reported [20, 22, 23]. All our discordant cases tested positive with both GENECUBE® HQ SARS-CoV-2 and GeneXpert®, so it appears that these samples indeed contained SARS-CoV-2. When evaluating the pooled samples with a low viral load, we also recognized a similar discordance, with GENECUBE® HQ SARS-CoV-2 positive/the reference PCR negative. The sensitivity of molecular examinations may differ between experimental and clinical samples [24]. In this study, we observed the insufficient amplification of the target with the reference real-time RT-PCR (Fig. 1 in the ESM) and recognized the inhibition that was not indicated in the LOD experiment with diluted UTM™ samples. Multiple factors can influence the results of NAATs, including the quality of the extracted RNA, the presence of RT-PCR inhibitors, genomic mutations [23], and stochasticity observed in very low viral concentrations [19]. These factors may have contributed to the discrepancy in our samples.
Although the extraction methods may influence the RNA recovery [25, 26], both rapidity and accuracy are essential for SARS-CoV-2 testing. The heat-extraction method can be performed within about 10 minutes, enabling the GENECUBE® system to provide results less than 40 minutes after the samples arrive at the microbiology laboratory. In this study, GENECUBE® HQ SARS-CoV-2 showed an increase in its LOD when the heat-extraction method was used. However, GENECUBE® HQ SARS-CoV-2 with heat extraction showed acceptable analytical performance in clinical specimens, providing a 99.7% concordance rate with the reference real-time RT-PCR.
In the coming winter season, the co-detection of influenza virus will become important for patient management and infection control [27]. The GENECUBE® FLU A/B assay demonstrated only one discordant case with the reference RT-PCR, indicating high analytical performance. The inconsistent case was positive using GENECUBE® FLU A/B but negative using reference RT-PCR and the subsequent FilmArray® assay. This case may be a false positive; however, in our previous study using fresh samples [13], the cobas Liat Influenza A/B assay (Roche Molecular Systems, Pleasanton, CA, USA) provided a positive result for influenza B virus for the discordant sample. Further data are required to evaluate the possibility of false-positive results associated with GENECUBE® FLU A/B. Similar to GENECUBE® HQ SARS-CoV-2, the sensitivity of GENECUBE® FLU A/B was slightly reduced when using the heat-extraction method. Still, the sensitivity of GENECUBE® FLU A/B with heat extraction was comparable to that of other NAATs and far better than that of antigen tests [28].
Several limitations associated with the present study should be mentioned. First, we did not evaluate anterior nasal or saliva samples. Sample collection from the anterior nasal cavity or saliva is less invasive than that from the nasopharynx [29, 30], and several molecular examinations can adequately detect SARS-CoV-2 in these samples [30, 31]. Further research is warranted to evaluate the performance of GENECUBE® HQ SARS-CoV-2 using samples collected from body sites other than the nasopharynx. Second, the analytical performance may be affected by the future emergence of mutations of SARS-CoV-2 and the influenza virus that are involved in the target areas of GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B. Finally, we did not evaluate the fresh samples for other respiratory viruses that might co-circulate with SARS-CoV-2. The data for GENECUBE® FLU A/B were also limited because of the low prevalence of the influenza virus, especially for fresh samples.
In conclusion, GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B provided high analytical performance and the ability to evaluate multiple samples in a short period of time.
References
Coronavirus Disease (COVID-19) Situation Reports [Internet]. 2020. https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situation-reports. Accessed 21 Dec 2020.
Laboratory testing for coronavirus disease (COVID-19) in suspected human cases: interim guidance, 19 March 2020 [Internet]. 2020. https://apps.who.int/iris/handle/10665/331501. Accessed 22 Dec 2020.
Diagnostic testing for SARS-CoV-2 [Internet]. 2020. https://www.who.int/publications/i/item/diagnostic-testing-for-sars-cov-2. Accessed 22 Dec 2021.
Coronavirus Disease 2019 (COVID-19) Treatment Guidelines [Internet]. COVID-19 Treat. Guidel. https://www.covid19treatmentguidelines.nih.gov/. Accessed 18 Feb 2021.
Younes N, Al-Sadeq DW, AL-Jighefee H, Younes S, Al-Jamal O, Daas HI, et al. Challenges in laboratory diagnosis of the novel coronavirus SARS-CoV-2. Viruses Multidiscip Digit Publ Inst. 2020;12:582.
Information for Clinicians on Influenza Virus Testing. Table 4. Multiplex Assays Authorized for Simultaneous Detection of Influenza Viruses and SARS-CoV-2 by FDA | CDC [Internet]. 2020 [cited 2021 Feb 18]. Available from: https://www.cdc.gov/flu/professionals/diagnosis/table-flu-covid19-detection.html. Accessed 18 Feb 2021.
Hayashi D, Akashi Y, Suzuki H, Shiigai M, Kanemoto K, Notake S, et al. Implementation of point-of-care molecular diagnostics for Mycoplasma pneumoniae ensures the correct antimicrobial prescription for pediatric pneumonia patients. Tohoku J Exp Med. 2018;246:225–31.
Hida Y, Hisada K, Shimada A, Yamashita M, Kimura H, Yoshida H, et al. Rapid detection of the Mycobacterium tuberculosis complex by use of quenching probe PCR (geneCube). J Clin Microbiol. 2012;50:3604–8.
Miyazaki N, Yamagishi Y, Izumi K, Kawashima Y, Suematsu H, Mikamo H. Evaluation of rapid measurement of Chlamydia trachomatis and Neisseria gonorrhoeae by using automatic gene analyzer “GENECUBE.” Jpn J Antibiot. 2016;69:291–8.
Morinaga Y, Suzuki H, Notake S, Mizusaka T, Uemura K, Otomo S, et al. Evaluation of GENECUBE Mycoplasma for the detection of macrolide-resistant Mycoplasma pneumoniae. J Med Microbiol. 2020;69:1346–50.
Hida Y, Uemura K, Sugimoto H, Kawashima Y, Koyanagi N, Notake S, et al. Evaluation of performance of the GENECUBE assay for rapid molecular identification of Staphylococcus aureus and methicillin resistance in positive blood culture medium. PLoS One Public Libr Sci. 2019;14:e0219819.
Hara T, Suzuki H, Oyanagi T, Koyanagi N, Ushiki A, Kawabata N, et al. Clinical evaluation of a non-purified direct molecular assay for the detection of Clostridioides difficile toxin genes in stool specimens. PLoS One Public Libr Sci. 2020;15:e0234119.
Akashi Y, Suzuki H, Ueda A, Hirose Y, Hayashi D, Imai H, et al. Analytical and clinical evaluation of a point-of-care molecular diagnostic system and its influenza A/B assay for rapid molecular detection of the influenza virus. J Infect Chemother Off J Jpn Soc Chemother. 2019;25:578–83.
Akashi Y, Suzuki H, Takeuchi Y, Ueda A, Hirose Y, Imai H, et al. Influence of illness duration on the sensitivity and specificity of influenza antigen testing: a prospective observational study using real-time PCR. Kansenshogaku Zasshi. 2021;95:9–16.
Marty FM, Chen K, Verrill KA. How to obtain a nasopharyngeal swab specimen. N Engl J Med Mass Med Soc. 2020;382:e76.
Shirato K, Nao N, Katano H, Takayama I, Saito S, Kato F, et al. Development of genetic diagnostic methods for detection for novel coronavirus 2019(nCoV-2019) in Japan. Jpn J Infect Dis. 2020;73:304–7.
National Institute of Infectious Diseases. Manual for virus detection-influenza 4th ed. [Internet]. 2018. https://www.niid.go.jp/niid/images/lab-manual/influenza20190116.pdf.
Loeffelholz MJ, Alland D, Butler-Wu SM, Pandey U, Perno CF, Nava A, et al. Multicenter evaluation of the Cepheid Xpert Xpress SARS-CoV-2 Test. J Clin Microbiol Am Soc Microbiol J. 2020. https://jcm.asm.org/content/58/8/e00926-20. Accessed 18 Feb 2021.
Creager HM, Cabrera B, Schnaubelt A, Cox JL, Cushman-Vokoun AM, Shakir SM, et al. Clinical evaluation of the BioFire® Respiratory Panel 2.1 and detection of SARS-CoV-2. J Clin Virol. 2020;129:104538.
Matsumura Y, Shimizu T, Noguchi T, Nakano S, Yamamoto M, Nagao M. Comparison of 12 molecular detection assays for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). J Mol Diagn JMD. 2021;23:164–70.
Hellou MM, Górska A, Mazzaferri F, Cremonini E, Gentilotti E, Nardo PD, et al. Nucleic acid amplification tests on respiratory samples for the diagnosis of coronavirus infections: a systematic review and meta-analysis. Clin Microbiol Infect. 2020. https://www.clinicalmicrobiologyandinfection.com/article/S1198-743X(20)30695-9/abstract. Accessed 18 Feb 2021.
Moran A, Beavis KG, Matushek SM, Ciaglia C, Francois N, Tesic V, et al. Detection of SARS-CoV-2 by use of the Cepheid Xpert Xpress SARS-CoV-2 and Roche cobas SARS-CoV-2 Assays. J Clin Microbiol Am Soc Microbiol J. 2020. https://jcm.asm.org/content/58/8/e00772-20. Accessed 18 Feb 2021.
Afzal A. Molecular diagnostic technologies for COVID-19: Limitations and challenges. J Adv Res. 2020;26:149–59.
Ishige T, Murata S, Taniguchi T, Miyabe A, Kitamura K, Kawasaki K, et al. Highly sensitive detection of SARS-CoV-2 RNA by multiplex rRT-PCR for molecular diagnosis of COVID-19 by clinical laboratories. Clin Chim Acta Int J Clin Chem. 2020;507:139–42.
Kok T, Wati S, Bayly B, Devonshire-Gill D, Higgins G. Comparison of six nucleic acid extraction methods for detection of viral DNA or RNA sequences in four different non-serum specimen types. J Clin Virol Off Publ Pan Am Soc Clin Virol. 2000;16:59–63.
Petrillo S, Carrà G, Bottino P, Zanotto E, De Santis MC, Margaria JP, et al. A novel multiplex qRT-PCR assay to detect SARS-CoV-2 infection: high sensitivity and increased testing capacity. Microorganisms [Internet]. 2020. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7409169/. Accessed 18 Feb 2021.
CDC. CDC Diagnostic Tests for COVID-19 [Internet]. Cent. Dis. Control Prev. 2020. https://www.cdc.gov/coronavirus/2019-ncov/lab/testing.html. Accessed 18 Feb 2021.
Merckx J, Wali R, Schiller I, Caya C, Gore GC, Chartrand C, et al. Diagnostic accuracy of novel and traditional rapid tests for influenza infection compared with reverse transcriptase polymerase chain reaction. Ann Intern Med Am Coll Phys. 2017;167:394–409.
CDC. SARS-CoV-2 (COVID-19) Fact Sheet. Anterior Nasal (Nares) Specimen Collection for SARS-CoV-2 Diagnostic Testing [Internet]. Cent Dis Control Prev. 2020. https://www.cdc.gov/coronavirus/2019-ncov/downloads/lab/OASH-nasal-specimen-collection-fact-sheet_updates_2020_11_11_508.pdf. Accessed 18 Feb 2021.
Pasomsub E, Watcharananan SP, Boonyawat K, Janchompoo P, Wongtabtim G, Suksuwan W, et al. Saliva sample as a non-invasive specimen for the diagnosis of coronavirus disease 2019: a cross-sectional study. Clin Microbiol Infect. 2021;27:285.e1-285.e4.
Péré H, Podglajen I, Wack M, Flamarion E, Mirault T, Goudot G, et al. Nasal Swab Sampling for SARS-CoV-2: a Convenient Alternative in Times of Nasopharyngeal Swab Shortage. J Clin Microbiol Am Soc Microbiol J. 2020. https://jcm.asm.org/content/58/6/e00721-20. Accessed 18 Feb 2021.
Acknowledgements
The authors thank Mrs. Yoko Ueda, Mrs. Mio Matsumoto, and the staff in Tsukuba Medical Center Hospital for their intensive support of this study. Mrs. Yoko Ueda and Mrs. Mio Matsumoto significantly contributed to creating the database of this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was financially supported by TOYOBO Co., Ltd.
Conflict of Interest
TOYOBO Co., Ltd., provided support in the form of salaries to author A. Sugiyama, lecture fees to author H. Suzuki, and advisory fees to author H. Suzuki. The funder did not have any additional role in the study design, data collection and analysis, decision to publish or preparation of the manuscript.
Availability of Data and Material
Not applicable.
Ethics Approval
This study was performed in line with the principles of the Declaration of Helsinki and with the STROBE guidelines. The ethics committee of TMCH approved this study (approval number: 2020-046).
Consent to participate
All study participants provided informed consent.
Consent for publication
Not applicable.
Code availability
Not applicable.
Informed Consent
Informed consent was obtained from all participants.
Author Contributions
YK drafted the manuscript and performed the statistical analyses. YA was the chief investigator and responsible for the manuscript. HS supervised the project. AS and AN contributed to the development and execution of molecular assays. YT, SN, KN, and HI supported the preparation of this manuscript. All authors contributed to the writing of the final manuscript.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kiyasu, Y., Akashi, Y., Sugiyama, A. et al. A Prospective Evaluation of the Analytical Performance of GENECUBE® HQ SARS-CoV-2 and GENECUBE® FLU A/B. Mol Diagn Ther 25, 495–504 (2021). https://doi.org/10.1007/s40291-021-00535-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40291-021-00535-5