Abstract
Introduction
It has been suggested that fluoroquinolone antibiotics increase the risk of developing collagen-associated adverse events such as aortic dissection and aortic aneurysm. These are life-threatening emergencies that need to be prevented.
Objectives
We performed this systematic review to clarify the association between fluoroquinolones and three collagen-associated adverse events: aortic aneurysm or aortic dissection, retinal detachment, and tendon disorders.
Methods
We searched PubMed, Embase, and Scopus for observational studies up to January 2019. Cohort and case–control studies were included if they reported data on the risk of collagen-related adverse events associated with fluoroquinolone exposure versus no exposure. We assessed the quality of the included studies using the Newcastle–Ottawa Scale. Effect statistics were pooled using random-effects models. Sensitivity and subgroup analyses were performed to identify any source of heterogeneity.
Results
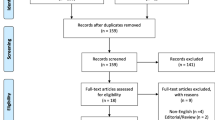
After screening 2729 citations, we included 22 observational studies (12 cohort studies and ten case–control studies) with 19,207,552 participants. Current use of fluoroquinolones was significantly associated with aortic aneurysm and aortic dissection (odds ratio [OR] 2.20; 95% confidence interval [CI] 1.92–2.52), tendon disorders (OR 1.89; 95% CI 1.53–2.33), and retinal detachment (sensitivity analysis, OR 1.25; 95% CI 1.01–1.53). Past fluoroquinolone use (> 30 and ≤ 365 days) was associated with retinal detachment (OR 1.27; 95% CI 1.09–1.47).
Conclusions
Fluoroquinolone use incurs a risk of developing three collagen-associated diseases (aortic aneurysm or aortic dissection, retinal detachment, and tendon disorders). Patients at an increased risk of collagen-associated diseases should not use fluoroquinolones unless no other options are available.






Similar content being viewed by others
References
Hicks LA, Taylor TH, Hunkler RJUS. Outpatient antibiotic prescribing, 2010. New Engl J Med. 2013;368(15):1461–2. https://doi.org/10.1056/NEJMc1212055.
Pasternak B, Inghammar M, Svanstrom H. Fluoroquinolone use and risk of aortic aneurysm and dissection: nationwide cohort study. BMJ. 2018;360:k678. https://doi.org/10.1136/bmj.k678.
Kaleagasioglu F, Olcay E. Fluoroquinolone-induced tendinopathy: etiology and preventive measures. Tohoku J Exp Med. 2012;226(4):251–8. https://doi.org/10.1620/tjem.226.251.
Redgrave LS, Sutton SB, Webber MA, Piddock LJV. Fluoroquinolone resistance: mechanisms, impact on bacteria, and role in evolutionary success. Trends Microbiol. 2014;22(8):438–45. https://doi.org/10.1016/j.tim.2014.04.007.
Akali AU, Niranjan NS. Management of bilateral Achilles tendon rupture associated with ciprofloxacin: a review and case presentation. J Plast Reconstr Aesthetic Surg. 2008;61(7):830–4. https://doi.org/10.1016/j.bjps.2006.08.005.
Stinner DJ, Orr JD, Hsu JR. Fluoroquinolone-associated bilateral patellar tendon rupture: A case report and review of the literature. Mil Med. 2010;175(6):457–9. https://doi.org/10.7205/MILMED-D-09-00142.
Shybut TB, Puckett ER. Triceps ruptures after fluoroquinolone antibiotics: a report of 2 cases. Sports Health. 2017;9(5):474–6. https://doi.org/10.1177/1941738117713686.
Tsai WC, Hsu CC, Chen CPC, Chang HN, Wong AMK, Lin MS, et al. Ciprofloxacin up-regulates tendon cells to express matrix metalloproteinase-2 with degradation of type i collagen. J Orthop Res. 2011;29(1):67–73. https://doi.org/10.1002/jor.21196.
Rampal S, Kaur R, Sethi R, Singh O, Sood N. Ofloxacin-associated retinopathy in rabbits: role of oxidative stress. Hum Exp Toxicol. 2008;27(5):409–15. https://doi.org/10.1177/0960327108092295.
Van der Linden PD, Sturkenboom MCJM, Herings RMC, Leufkens HGM, Stricker BHC. Fluoroquinolones and risk of Achilles tendon disorders: case-control study. Br Med J. 2002;324(7349):1306–7.
Van der Linden PD, Sturkenboom MCJM, Herings RMC, Leufkens HMG, Rowlands S, Stricker BHC. Increased risk of Achilles tendon rupture with quinolone antibacterial use, especially in elderly patients taking oral corticosteroids. Arch Intern Med. 2003;163(15):1801–7. https://doi.org/10.1001/archinte.163.15.1801.
Seeger JD, West WA, Fife D, Noel GJ, Johnson LN, Walker AM. Achilles tendon rupture and its association with fluoroquinolone antibiotics and other potential risk factors in a managed care population. Pharmacoepidemiol Drug Saf. 2006;15(11):784–92. https://doi.org/10.1002/pds.1214.
Van der Linden PD, Van de Lei J, Nab HW, Knol A, Stricker BHC. Achilles tendinitis associated with fluoroquinolones. Br J Clin Pharmacol. 1999;48(3):433–7. https://doi.org/10.1046/j.1365-2125.1999.00016.x.
Yee CL, Duffy C, Gerbino PG, Stryker S, Noel GJ. Tendon or joint disorders in children after treatment with fluoroquinolones or azithromycin. Pediatr Infect Dis J. 2002;21(6):525–9. https://doi.org/10.1097/00006454-200206000-00009.
Sode J, Obel N, Hallas J, Lassen A. Use of fluroquinolone and risk of Achilles tendon rupture: a population-based cohort study. Eur J Clin Pharmacol. 2007;63(5):499–503. https://doi.org/10.1007/s00228-007-0265-9.
Hori K, Yamakawa K, Yoshida N, Ohnishi K, Kawakami J. Detection of fluoroquinolone-induced tendon disorders using a hospital database in Japan. Pharmacoepidemiol Drug Saf. 2012;21(8):886–9. https://doi.org/10.1002/pds.3285.
Morales DR, Slattery J, Pacurariu A, Pinheiro L, McGettigan P, Kurz X. Relative and absolute risk of tendon rupture with fluoroquinolone and concomitant fluoroquinolone/corticosteroid therapy: population-based nested case-control study. Clin Drug Investig. 2019;39(2):205–13. https://doi.org/10.1007/s40261-018-0729-y.
Tanne JH. FDA adds “black box” warning label to fluoroquinolone antibiotics. BMJ. 2008;337:a816. https://doi.org/10.1136/bmj.a816.
Etminan M, Forooghian F, Brophy JM, Bird ST, Maberley D. Oral fluoroquinolones and the risk of retinal detachment. J Am Med Assoc. 2012;307(13):1414–9. https://doi.org/10.1001/jama.2012.383.
Pasternak B, Svanström H, Melbye M, Hviid A. Association between oral fluoroquinolone use and retinal detachment. J Am Med Assoc. 2013;310(20):2184–90. https://doi.org/10.1001/jama.2013.280500.
Choi SY, Lim HA, Yim HW, Park YH. Administration of oral fluoroquinolone and the risk of rhegmatogenous retinal detachment: a nationwide population-based study in Korea. PLoS One. 2018;13(4):e0195563. https://doi.org/10.1371/journal.pone.0195563.
Eftekhari K, Ghodasra DH, Haynes K, Chen J, Kempen JH, Vanderbeek BL. Risk of retinal tear or detachment with oral fluoroquinolone use: a cohort study. Pharmacoepidemiol Drug Saf. 2014;23(7):745–52. https://doi.org/10.1002/pds.3623.
Daneman N, Lu H, Redelmeier DA. Fluoroquinolones and collagen associated severe adverse events: a longitudinal cohort study. BMJ Open. 2015;5(11):e010077. https://doi.org/10.1136/bmjopen-2015-010077.
Lee CC, Gabriel Lee MT, Chen YS, Lee SH, Chen YS, Chen SC, et al. Risk of aortic dissection and aortic aneurysm in patients taking oral fluoroquinolone. JAMA Intern Med. 2015;175(11):1839–47. https://doi.org/10.1001/jamainternmed.2015.5389.
Pouzaud F, Bernard-Beaubois K, Thevenin M, Warnet JM, Hayem G, Rat P. In vitro discrimination of fluoroquinolones toxicity on tendon cells: involvement of oxidative stress. J Pharmacol Exp Ther. 2004;308(1):394–402. https://doi.org/10.1124/jpet.103.057984.
Baugé C, Leclercq S, Conrozier T, Boumediene K. TOL19-001 reduces inflammation and MMP expression in monolayer cultures of tendon cells. BMC Complement Altern Med. 2015;15(1):217. https://doi.org/10.1186/s12906-015-0748-7.
Kumbhar GB, Khan AM, Rampal S. Evaluation of gatifloxacin for its potential to induce antioxidant imbalance and retinopathy in rabbits. Hum Exp Toxicol. 2015;34(4):372–9. https://doi.org/10.1177/0960327114530743.
Belavic JM. Fluoroquinolone-induced tendinopathy. Nurse Pract. 2009;34(1):17–8. https://doi.org/10.1097/01.NPR.0000343751.83969.1b.
Fife D, Zhu V, Voss E, Levy-Clarke G, Ryan P. Exposure to oral fluoroquinolones and the risk of retinal detachment: retrospective analyses of two large healthcare databases. Drug Saf. 2014;37(3):171–82. https://doi.org/10.1007/s40264-014-0138-y.
Kuo SC, Chen YT, Lee YT, Fan NW, Chen SJ, Li SY, et al. Association between recent use of fluoroquinolones and rhegmatogenous retinal detachment: a population-based cohort study. Clin Infect Dis. 2014;58(2):197–203. https://doi.org/10.1093/cid/cit708.
Corrao G, Zambon A, Bertù L, Mauri A, Paleari V, Rossi C, et al. Evidence of tendinitis provoked by fluoroquinolone treatment a case-control study. Drug Saf. 2006;29(10):889–96. https://doi.org/10.2165/00002018-200629100-00006.
Moher D, Liberati AF, Tetzlaff J, Tetzlaff JF, Altman DG, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. (1539-3704 (Electronic)).
Hartling L, Milne A, Hamm MP, Vandermeer B, Ansari M, Tsertsvadze A, et al. Testing the Newcastle Ottawa Scale showed low reliability between individual reviewers. J Clin Epidemiol. 2013;66(9):982–93. https://doi.org/10.1016/j.jclinepi.2013.03.003.
Singh S, Nautiyal A. Aortic dissection and aortic aneurysms associated with fluoroquinolones: a systematic review and meta-analysis. Am J Med. 2017;130(12):1449. https://doi.org/10.1016/j.amjmed.2017.06.029.
Chui CSL, Wong ICK, Wong LYL, Chan EW. Association between oral fluoroquinolone use and the development of retinal detachment: a systematic review and meta-analysis of observational studies. J Antimicrob Chemother. 2015;70(4):971–8. https://doi.org/10.1093/jac/dku507.
Alves C, Penedones A, Mendes D, Batel Marques F. A systematic review and meta-analysis of the association between systemic fluoroquinolones and retinal detachment. Acta Ophthalmol. 2016;94(5):e251–9. https://doi.org/10.1111/aos.12931.
Jupiter DC, Fang X, Ashmore Z, Shibuya N, Mehta HB. The relative risk of achilles tendon injury in patients taking quinolones. Pharmacotherapy. 2018;38(9):878–87. https://doi.org/10.1002/phar.2162.
Etminan M, Maberley DAL. Improving reporting quality in ophthalmologic observational studies that use big data: the case of retinal detachment associated with fluoroquinolone use. (2168-6173 (Electronic)).
FDA warns about increased risk of ruptures or tears in the aorta blood vessel with fluoroquinolone antibiotics in certain patients. https://www.fda.gov/Drugs/DrugSafety/ucm628753.htm.
Disabling and potentially permanent side effects lead to suspension or restrictions of quinolone and fluoroquinolone antibiotics. https://www.ema.europa.eu/en/documents/press-release/disabling-potentially-permanent-side-effects-lead-suspension-restrictions-quinolone-fluoroquinolone_en.pdf. Accessed 1 Mar 2019.
Corps AN, Harrall RL, Curry VA, Fenwick SA, Hazleman BL, Riley GP. Ciprofloxacin enhances the stimulation of matrix metalloproteinase 3 expression by interleukin-1beta in human tendon-derived cells. A potential mechanism of fluoroquinolone-induced tendinopathy. Arthritis Rheum. 2002;46(11):3034–40. https://doi.org/10.1002/art.10617.
LeMaire SA, Zhang L, Luo W, Ren P, Azares AR, Wang Y, et al. Effect of ciprofloxacin on susceptibility to aortic dissection and rupture in mice. JAMA Surg. 2018;153(9):e181804. https://doi.org/10.1001/jamasurg.2018.1804.
Amin M, Pushpakumar S, Muradashvili N, Kundu S, Tyagi SC, Sen U. Regulation and involvement of matrix metalloproteinases in vascular diseases. Front Biosci (Landmark edition). 2016;21:89–118.
Feltgen N, Walter P. Rhegmatogenous retinal detachment–an ophthalmologic emergency. Dtsch Arztebl Inter. 2014;111(1–2):12–22. https://doi.org/10.3238/arztebl.2014.0012.
Baek YH, Park SJ, Jeong S, Oh IS, Jeong HE, Park KH, et al. Signal detection between fluoroquinolone use and the risk of rhegmatogenous retinal detachment: sequence symmetry analysis using nationwide South Korean healthcare database between 2004 and 2015. Clin Drug Investig. 2018. https://doi.org/10.1007/s40261-018-0708-3.
Acknowledgements
The authors thank all the authors of the original articles. We also appreciate Dr. Mouniir SA Durgahee for editing work.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicts of interest
Xin-yu Yu, Ding-sheng Jiang, Jing Wang, Rui Wang, Tai-qiang Chen, Kan Wang, Xiang Wei, and Shi-yi Cao have no conflicts of interest that are directly relevant to the content of this study.
Funding
This review was supported by the National Natural Science Foundation of China (NSFC, 71603091).
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yu, X., Jiang, Ds., Wang, J. et al. Fluoroquinolone Use and the Risk of Collagen-Associated Adverse Events: A Systematic Review and Meta-Analysis. Drug Saf 42, 1025–1033 (2019). https://doi.org/10.1007/s40264-019-00828-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40264-019-00828-z