Abstract
Introduction
Comparing medications in observational settings requires differences in patient characteristics to be accounted for. Propensity score (PS) methods can address these differences, but PS weighting approaches may introduce bias.
Methods
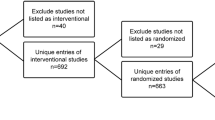
Within a cohort study of anticoagulant initiators from October 2010 through to December 2012, PS values for dabigatran relative to warfarin were estimated, and study outcomes (stroke or major bleeding) among the cohort were identified. The PS was used to match initiators and results compared with those obtained using inverse probability of treatment weighting (IPTW) and standardized morbidity ratio (SMR) weighting. Hazard ratios (HRs) for study outcomes were estimated using a proportional hazards regression model.
Results
There were 23,543 dabigatran and 50,288 warfarin initiators, and matching formed 19,189 pairs (81.5% of dabigatran initiators) which resulted in a pooled stroke HR of 0.77 (95% confidence interval [CI] 0.54–1.09), and a pooled major hemorrhage HR of 0.75 (95% CI 0.65–0.87). The IPTW results for stroke (HR = 0.00; 95% CI 0.00–0.56) and major hemorrhage (HR = 0.08; 95% CI 0.08–0.10) substantially differed, while the SMR-weighted results for stroke (HR = 0.65; 95% CI 0.42–1.03) and major hemorrhage (HR = 0.73; 95% CI 0.61–0.85) differed only slightly from matching.
Conclusions
In this example, different applications of the same PS led to substantially different results, a finding that was particularly apparent with IPTW, and this was remedied by truncating extreme weights. If IPTW is used, information regarding the weights applied along with sensitivity analyses could avoid misrepresentation of study results, and would enhance their interpretation.


Similar content being viewed by others
References
Ageno W, Gallus AS, Wittkowsky A, et al. Oral anticoagulant therapy: antithrombotic therapy and prevention of thrombosis, 9th ed: American college of chest physicians evidence-based clinical practice guidelines. Chest. 2012;141(2 Suppl):e44S–88S.
You JJ, Singer DE, Howard PA, et al. Antithrombotic therapy for atrial fibrillation: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of chest physicians evidence-based clinical practice guidelines. Chest. 2012;141(2 Suppl):e531S–75S.
Connolly SJ, Ezekowitz MD, Yusuf S, et al. Dabigatran versus warfarin in patients with atrial fibrillation. N Engl J Med. 2009;361(12):1139–51.
Connolly SJ, Wallentin L, Yusuf S. Additional events in the RE-LY trial. N Engl J Med. 2014;371(15):1464–5.
Graham DJ, Reichman ME, Wernecke M, et al. Cardiovascular, bleeding, and mortality risks in elderly Medicare patients treated with dabigatran or warfarin for non-valvular atrial fibrillation. Circulation. 2014;131(2):157–64.
Schneeweiss S, Huybrechts KF, Gagne JJ. Interpreting the quality of health care database studies on the comparative effectiveness of oral anticoagulants in routine care. Comp Eff Res. 2013;3:33–41.
Hernandez I, Baik SH, Piñera A, et al. Risk of bleeding with dabigatran in atrial fibrillation. JAMA Intern Med. 2015;175(1):18–24.
Li L, Greene T. A weighting analogue to pair matching in propensity score analysis. Int J Biostat. 2013;9(2):215–34.
Sturmer T, Rothman KJ, Avorn J, et al. Treatment effects in the presence of unmeasured confounding: dealing with observations in the tails of the propensity score distribution–a simulation study. Am J Epidemiol. 2010;172(7):843–54.
Seeger JD, Daniels G. Commercial insurance databases. In: Strom BL, Kimmel SE, Hennessy S, editors. Pharmacoepidemiology. Philadelphia: Wiley; 2012.
Lip GY, Nieuwlaat R, Pisters R, et al. Refining clinical risk stratification for predicting stroke and thromboembolism in atrial fibrillation using a novel risk factor-based approach: the euro heart survey on atrial fibrillation. Chest. 2010;137(2):263–72.
Johnson ES, Bartman BA, Briesacher BA, et al. The incident user design in comparative effectiveness research. Pharmacoepidemiol Drug Saf. 2013;22(1):1–6.
Ray WA. Evaluating medication effects outside of clinical trials: new-user designs. Am J Epidemiol. 2003;158(9):915–20.
Schneeweiss S, Gagne JJ, Glynn RJ, et al. Assessing the comparative effectiveness of newly marketed medications: methodological challenges and implications for drug development. Clin Pharmacol Ther. 2011;90(6):777–90.
Hernan MA, Hernandez-Diaz S, Robins JM. Randomized trials analyzed as observational studies. Ann Intern Med. 2013;159(8):560–2.
Schneeweiss S. A basic study design for expedited safety signal evaluation based on electronic healthcare data. Pharmacoepidemiol Drug Saf. 2010;19(8):858–68.
Andrade SE, Harrold LR, Tjia J, et al. A systematic review of validated methods for identifying cerebrovascular accident or transient ischemic attack using administrative data. Pharmacoepidemiol Drug Saf. 2012;21(Suppl 1):100–28.
Wahl PM, Rodgers K, Schneeweiss S, et al. Validation of claims-based diagnostic and procedure codes for cardiovascular and gastrointestinal serious adverse events in a commercially-insured population. Pharmacoepidemiol Drug Saf. 2010;19(6):596–603.
Cunningham A, Stein CM, Chung CP, et al. An automated database case definition for serious bleeding related to oral anticoagulant use. Pharmacoepidemiol Drug Saf. 2011;20(6):560–6.
Cox DR. Regression models and life tables. J R Stat Soc Series B Methodol. 1972;34(2):187–220.
Jones DR. Meta-analysis: weighing the evidence. Stat Med. 1995;14(2):137–49.
Vrijens B, Urquhart J. Methods for measuring, enhancing, and accounting for medication adherence in clinical trials. Clin Pharmacol Ther. 2014;95(6):617–26.
Gagne JJ, Glynn RJ, Rassen JA, et al. Active safety monitoring of newly marketed medications in a distributed data network: application of a semi-automated monitoring system. Clin Pharmacol Ther. 2012;92(1):80–6.
Rosenbaum PR, Rubin DB. The central role of the propensity score in observational studies for causal effects. Biometrika. 1983;70(1):41–55.
Westreich D, Cole SR, Schisterman EF, et al. A simulation study of finite-sample properties of marginal structural Cox proportional hazards models. Stat Med. 2012;31(19):2098–109.
Cole SR, Hernan MA. Constructing inverse probability weights for marginal structural models. Am J Epidemiol. 2008;168(6):656–64.
Wang Y, Petersen M, Bangsberg D, et al. Diagnosing bias in the inverse probability of treatment weighted estimator resulting from violation of experimental treatment assignment. UC Berkeley Division of Biostatistics Working Paper Series. 2006. Working Paper 211. http://biostats.bepress.com/ucbbiostat/paper211. Accessed 22 Nov 2016.
Schartum-Hansen H, Løland KH, Svingen GFT, et al. Use of loop diuretics is associated with increased mortality in patients with suspected coronary artery disease, but without systolic heart failure or renal impairment: an observational study using propensity score matching. PLoS One. 2015;10(6):e0124611.
Lauffenburger JC, Farley JF, Gehi AK, et al. Effectiveness and safety of dabigatran and warfarin in real-world US patients with non-valvular atrial fibrillation: a retrospective cohort study. J Am Heart Assoc. 2015;4:1–12.
Acknowledgements
The useful comments provided by Kristina Zint, PharmD of Boehringer Ingelheim are acknowledged.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This research was supported by a research contract with Boehringer-Ingelheim. The research contract granted Brigham & Women’s Hospital the right to publication of the results.
Conflict of interest
John Seeger, Kate Bykov, Krista Huybrechts, and Sebastian Schneeweiss received funding support through the research contract with Boehringer-Ingelheim. Dorothee Bartels is an employee of Boehringer-Ingelheim, the manufacturer of dabigatran.
Ethical Approval
Patient data were de-identified and the study was approved by the Brigham and Women’s Hospital institutional review board.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Seeger, J.D., Bykov, K., Bartels, D.B. et al. Propensity Score Weighting Compared to Matching in a Study of Dabigatran and Warfarin. Drug Saf 40, 169–181 (2017). https://doi.org/10.1007/s40264-016-0480-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40264-016-0480-3