Abstract
Background
Induction of immunogenic cell death (ICD) is considered a promising strategy for cancer immunotherapy. Stattic is an inhibitor of STAT3, which is found constitutively active in many cancers and plays a major role in cancer progression.
Objectives
In the present study, we proposed to evaluate whether stattic can enhance the effects of chemotherapy in the induction of ICD in cancer cells harboring hyperactive STAT3.
Methods
The growth inhibitory effects of stattic and chemo agents including doxorubicin (DOX) and oxaliplatin (OXP) were evaluated using MTT assay in B16F10 and CT26 cell lines. Flow cytometry was applied to study cell apoptosis and calreticulin (CRT) surface exposure. The levels of high mobility group box 1 (HGMB1), heat shock protein70 (HSP70) and interleukin-12 (IL-12) were measured using ELISA.
Results
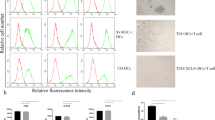
Treatment of B16F10 and CT26 cells with stattic in combination with DOX resulted in synergistic antitumor effects with combination index being 0.82 and 0.87, respectively. Interestingly, we found a higher level of ICD markers including CRT expression as well as HMGB1 and HSP70 secretion in the cells received combination therapy of stattic and DOX as compared with monotherapies. Moreover, exposure of dendritic cells (DCs) to conditioned media (CM) from cancer cells treated with stattic and/or DOX resulted in secretion of IL-12, which is an indicator of DCs maturation and induction of Th1 response. OXP and stattic monotherapy induced ICD in CT26 cells and stimulated IL-12 secretion by DCs; however, we did not observe a significant increase in the level of ICD in CT26 cells and IL-12 secretion by DCs when CT26 cells were treated with stattic and OXP combination as compared with monotherapy groups.
Conclusion
These findings indicate that STAT3 inhibitory stattic can increase ICD induced by DOX.

Graphical abstract





Similar content being viewed by others
References
Voena C, Chiarle R. Advances in cancer immunology and cancer immunotherapy. Discov Med. 2016;21(114):125–33.
Kalathil SG, Thanavala Y. High immunosuppressive burden in cancer patients: a major hurdle for cancer immunotherapy. Cancer Immunol Immunother. 2016;65(7):813–9.
Devaud C, John LB, Westwood JA, Darcy PK, Kershaw MH. Immune modulation of the tumor microenvironment for enhancing cancer immunotherapy. Oncoimmunology. 2013;2(8):e25961.
Obeid M, Tesniere A, Ghiringhelli F, Fimia GM, Apetoh L, Perfettini J-L, et al. Calreticulin exposure dictates the immunogenicity of cancer cell death. Nat Med. 2007;13(1):54–61.
Radogna F, Diederich M. Stress-induced cellular responses in immunogenic cell death: implications for cancer immunotherapy. Biochem Pharmacol. 2018.
Bezu L, Gomes-da-Silva LC, Dewitte H, Breckpot K, Fucikova J, Spisek R, et al. Combinatorial strategies for the induction of immunogenic cell death. Front Immunol. 2015;6:187.
Tesniere A, Apetoh L, Ghiringhelli F, Joza N, Panaretakis T, Kepp O, et al. Immunogenic cancer cell death: a key-lock paradigm. Curr Opin Immunol. 2008;20(5):504–11.
Panaretakis T, Joza N, Modjtahedi N, Tesniere A, Vitale I, Durchschlag M, et al. The co-translocation of ERp57 and calreticulin determines the immunogenicity of cell death. Cell Death Differ. 2008;15(9):1499–509.
Aymeric L, Apetoh L, Ghiringhelli F, Tesniere A, Martins I, Kroemer G, et al. Tumor cell death and ATP release prime dendritic cells and efficient anticancer immunity. Cancer Res. 2010;70(3):855–8.
Fang H, Ang B, Xu X, Huang X, Wu Y, Sun Y, et al. TLR4 is essential for dendritic cell activation and anti-tumor T-cell response enhancement by DAMPs released from chemically stressed cancer cells. Cell Mol Immunol. 2014;11(2):150–9.
Kepp O, Galluzzi L, Martins I, Schlemmer F, Adjemian S, Michaud M, et al. Molecular determinants of immunogenic cell death elicited by anticancer chemotherapy. Cancer Metastasis Rev. 2011;30(1):61–9.
Montico B, Nigro A, Casolaro V, Dal CJ. Immunogenic apoptosis as a novel tool for anticancer vaccine development. Int J Mol Sci. 2018;19(2):594.
Pol J, Vacchelli E, Aranda F, Castoldi F, Eggermont A, Cremer I, et al. Trial watch: immunogenic cell death inducers for anticancer chemotherapy. Oncoimmunology. 2015;4(4):e1008866.
Paolini A, Pasi F, Facoetti A, Mazzini G, Corbella F, Di Liberto R, et al. Cell death forms and HSP70 expression in U87 cells after ionizing radiation and/or chemotherapy. Anticancer Res. 2011;31(11):3727–31.
Schust J, Sperl B, Hollis A, Mayer TU, Berg T. Stattic: a small-molecule inhibitor of STAT3 activation and dimerization. Chem Biol. 2006;13(11):1235–42.
Yang CH, Fan M, Slominski AT, Yue J, Pfeffer LM. The role of constitutively activated STAT3 in B16 melanoma cells. Int J Interferon Cytokine Mediat Res. 2010;2010(2):1–7.
Corvinus FM, Orth C, Moriggl R, Tsareva SA, Wagner S, Pfitzner EB, et al. Persistent STAT3 activation in colon cancer is associated with enhanced cell proliferation and tumor growth. Neoplasia. 2005;7(6):545–55.
Wang X, Crowe PJ, Goldstein D, Yang J-L. STAT3 inhibition, a novel approach to enhancing targeted therapy in human cancers. Int J Oncol. 2012;41(4):1181–91.
Ilkovitch D, Lopez DM. Immune modulation by melanoma-derived factors. Exp Dermatol. 2008;17(12):977–85.
Wang Y, Shen Y, Wang S, Shen Q, Zhou X. The role of STAT3 in leading the crosstalk between human cancers and the immune system. Cancer Lett. 2018;415:117–28.
Yu H, Kortylewski M, Pardoll D. Tumour immunology: crosstalk between cancer and immune cells: role of STAT3 in the tumour microenvironment. Nat Rev Immunol. 2007;7(1):41.
Jing N, Tweardy DJ. Targeting Stat3 in cancer therapy. Anti-Cancer Drugs. 2005;16(6):601–7.
Yang H, Yamazaki T, Pietrocola F, Zhou H, Zitvogel L, Ma Y et al. STAT3 inhibition enhances the therapeutic efficacy of immunogenic chemotherapy by stimulating type 1 interferon production by cancer cells. Cancer Res. 2015:canres. 1122.2015.
Yue P, Turkson J. Targeting STAT3 in cancer: how successful are we? Expert Opin Investig Drugs. 2009;18(1):45–56.
Lee DS, Grandis JR, Johnson DE. STAT3 as a Major Contributor to Chemoresistance. Targeting Cell Survival Pathways to Enhance Response to Chemotherapy. Elsevier; 2019. p. 145–67.
Chou T-C. Theoretical basis, experimental design, and computerized simulation of synergism and antagonism in drug combination studies. Pharmacol Rev. 2006;58(3):621–81.
Garg SM, Vakili MR, Molavi O, Lavasanifar A. Self-associating poly (ethylene oxide)-block-poly (α-carboxyl-ε-caprolactone) drug conjugates for the delivery of STAT3 inhibitor JSI-124: potential application in Cancer immunotherapy. Mol Pharm. 2017;14(8):2570–84.
K-j S, Ryung Choi K, Ryu C-K, Lee SJ, Kim HJ, Lee H. Induction of immunogenic cell death of tumors by newly synthesized heterocyclic quinone derivative. PLoS One. 2017;12(3):e0173121.
Eom Y-W, Kim MA, Park SS, Goo MJ, Kwon HJ, Sohn S, et al. Two distinct modes of cell death induced by doxorubicin: apoptosis and cell death through mitotic catastrophe accompanied by senescence-like phenotype. Oncogene. 2005;24(30):4765–77.
Kroemer G, Galluzzi L, Kepp O, Zitvogel L. Immunogenic cell death in cancer therapy. Annu Rev Immunol. 2013;31:51–72.
Henry CJ, Ornelles DA, Mitchell LM, Brzoza-Lewis KL, Hiltbold EM. IL-12 produced by dendritic cells augments CD8+ T cell activation through the production of the chemokines CCL1 and CCL17. J Immunol. 2008;181(12):8576–84.
Karimi MH, Ebrahimnezhad S, Namayandeh M, Amirghofran Z. The effects of cichorium intybus extract on the maturation and activity of dendritic cells. DARU J Pharm Sci. 2014;22(1):28.
Kulesza DW, Carré T, Chouaib S, Kaminska B. Silencing of the transcription factor STAT3 sensitizes lung cancer cells to DNA damaging drugs, but not to TNFα-and NK cytotoxicity. Exp Cell Res. 2013;319(4):506–16.
Ghorbani M, Sabzichi M, Ramezani F, Mohammadian J. Adjuvant therapy with stattic enriches the anti-proliferative effect of doxorubicin in human ZR-75-1 breast cancer cells via arresting cell cycle and inducing apoptosis. Biomed Pharmacother. 2019;109:1240–8.
Lin C-Y, Lee C-H, Huang C-C, Lee S-T, Guo H-R, Su S-B. Impact of high glucose on metastasis of colon cancer cells. World J Gastroenterol. 2015;21(7):2047–57.
Muller AG, Sarker SD, Saleem IY, Hutcheon GA. Delivery of natural phenolic compounds for the potential treatment of lung cancer. DARU J Pharm Sci. 2019;1:433–49.
Garg AD, Nowis D, Golab J, Vandenabeele P, Krysko DV, Agostinis P. Immunogenic cell death, DAMPs and anticancer therapeutics: an emerging amalgamation. BBA-Rev Cancer. 2010;1805(1):53–71.
Mattarollo SR, Loi S, Duret H, Ma Y, Zitvogel L, Smyth MJ. Pivotal role of innate and adaptive immunity in anthracycline chemotherapy of established tumors. Cancer Res. 2011:canres. 0753.2011.
Tongu M, Harashima N, Yamada T, Harada T, Harada M. Immunogenic chemotherapy with cyclophosphamide and doxorubicin against established murine carcinoma. Cancer Immunol Immunother. 2010;59(5):769–77.
Tesniere A, Schlemmer F, Boige V, Kepp O, Martins I, Ghiringhelli F, et al. Immunogenic death of colon cancer cells treated with oxaliplatin. Oncogene. 2010;29(4):482–91.
Diederich M. Natural compound inducers of immunogenic cell death. Arch Pharm Res. 2019:1–17.
Zhou J, Wang G, Chen Y, Wang H, Hua Y, Cai Z. Immunogenic cell death in cancer therapy: present and emerging inducers. J Cell Mol Med. 2019.
Lee S, Margolin K. Cytokines in cancer immunotherapy. Cancers. 2011;3(4):3856–93.
Acknowledgements
This study is part of a dissertation (No.128) by S.Jafari, submitted for Ph.D degree and supported financially by Biotechnology Research Center, Tabriz University of Medical Sciences.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jafari, S., Lavasanifar, A., Hejazi, M.S. et al. STAT3 inhibitory stattic enhances immunogenic cell death induced by chemotherapy in cancer cells. DARU J Pharm Sci 28, 159–169 (2020). https://doi.org/10.1007/s40199-020-00326-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40199-020-00326-z