Abstract
Introduction
Recently, large channel endoscopic systems and full endoscopic visualization technique have been used to perform unilateral laminotomy for bilateral decompression (ULBD) treatment for lumbar central spinal stenosis (LCSS). However, various endoscopic systems possess different design parameters, which may affect the technical points and treatment outcomes. The object of this retrospective study was to compare the efficiency, safety, and effectiveness of ULBD under the iLESSYS Delta system versus the Endo-Surgi Plus system.
Methods
In the period from October 2020 to April 2021, ULBD was performed using the iLESSYS Delta system or Endo-Surgi Plus system to treat LCSS. Patients were classified into two groups based on the endoscopy system employed. Patient demographics, perioperative indexes, complications, and imaging characteristics were reviewed. Clinical outcomes were quantified using back and leg visual analog scale (VAS) scores and Oswestry Disability Index (ODI) at the time points of follow-up.
Results
Thirty-two patients were assigned to the iLESSYS Delta system group and 37 to the Endo-Surgi Plus system group. In the comparison between the two groups, the Endo-Surgi Plus system possessed a shorter incision length and operation time (p < 0.005), and no statistical differences in other aspects were observed. The dural sacs of both groups were significantly expanded postoperatively compared to preoperatively (p < 0.001). Both groups experienced improvements in VAS and ODI scores at all time points (p < 0.001) and equally low frequency of complications.
Conclusions
Current research suggests that both the Endo-Surgi Plus system and iLESSYS Delta system achieved favorable high safety and clinical outcomes in ULBD for treatment of LCSS. The use of a fully visualized trephine may have increased the efficiency of the Endo-Surgi Plus system. Moreover, the Endo-Surgi Plus system may be associated with a wider decompression range and indications.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Why carry out this study? |
Lumbar spinal stenosis (LSS) is the most common degenerative disease of the spine, seriously affecting the quality of life of patients and causing a huge public health financial burden. |
The extensive compression environment of lumbar central canal stenosis (LCSS) brings great challenges to endoscopic treatment. |
Large channel spinal endoscopy and full endoscopic visualization technique improved the efficiency and visualization of endoscopic surgery. |
This study aimed to compare the efficiency, safety, and effectiveness of unilateral laminotomy for bilateral decompression (ULBD) treatment for LCSS using the iLESSYS Delta system and the Endo-Surgi Plus system, and to provide a reference for spine surgeons to make surgical decisions. |
What was learned from the study? |
Current research suggests that both the Endo-Surgi Plus system and iLESSYS Delta system achieved favorable high safety and clinical outcomes in ULBD for treatment of LCSS. The use of a fully visualized trephine may have increased the efficiency of the Endo-Surgi Plus system. |
Introduction
Lumbar spinal stenosis (LSS) is a prominent cause of neurogenic intermittent claudication and low back pain, as well as the most common reason for spine surgery in the elderly over 65 years old, with a mean prevalence between 11% and 39% [1, 2]. LSS mainly included central spinal stenosis, lateral recess stenosis, and foraminal stenosis as assessed by anatomy and imageology [3, 4]. When the nerve structure is compressed in the aforementioned narrow space, it can cause corresponding symptoms and seriously affect the quality of life. Open laminectomy, which is a classic surgical method for the treatment of LSS, can completely decompress the stenosis of the spinal canal and effectively relieve symptoms [5]. However, as a result of extensive dissection of paravertebral muscles and massive destruction of the posterior osseoligamentous complex, the incidence of postoperative paravertebral muscle denervation atrophy, infection, instability, and other complications remains high, which leads to untenable patient suffering [6,7,8,9].
Percutaneous spinal endoscopy, which offers the advantages of less trauma, less bleeding, and faster recovery, has gradually become an effective alternative to traditional spinal open surgery and is favored by physicians and patients over the last two decades [10, 11]. Despite this, the technique has its inherent defects, such as limited view and operative area, inadequate decompression, a steep learning curve, and narrow indications [10, 12,13,14]. Patients with LSS, especially those with lumbar central spinal stenosis (LCSS), were formerly thought to be ineligible for spinal endoscopy [15]. On the other hand, the unilateral laminotomy for bilateral decompression (ULBD) technique could avoid excessive damage to the interspinous ligaments and facet joints [16,17,18,19], and when combined with the microendoscopic discectomy system (MED), the trauma caused by the approach is further reduced [20,21,22,23]. However, MED-ULBD has significant limitations in terms of the light source and perspective and it often needs microscope coordination, limiting its clinical applicability.
Recently, percutaneous spinal endoscopy has seen the introduction of the large channel endoscope systems and full endoscopic visualization technique, which has greatly improved the visualization, working space, safety, and efficiency [24,25,26,27]. On this basis, the endoscopic unilateral laminotomy for bilateral decompression (Endo-ULBD) procedure incorporating the concepts of targeting, precision, and minimal invasiveness has been used in the treatment of LCSS and achieved a good curative effect [25]. However, various endoscopic devices from different manufacturers with diverse components and design parameters may affect the indications, operational points, and clinical efficacy and obscure the evaluation system.
In this study, Endo-ULBD was performed on patients with single-segment LCSS utilizing two large channel endoscopic systems, the inter Laminar Endoscopic Surgical System (iLESSYS Delta, Joimax GmbH, Germany) and the Plus Endoscopic Spine Surgical System (Endo-Surgi Plus, Unin-tech GmbH, China). We focused on comparing the efficiency, safety, and effectiveness as well as evaluating the technical points and indications of the two systems for the treatment of LCSS.
Methods
Study Design and Consent
This is a retrospective cohort study. This study was performed in accordance with the Declaration of Helsinki (as revised in 2013), approved by the Medical Ethics Committee of The Affiliated Hospital of Qingdao University (No. QYFY WZLL 27073) and informed consent was obtained from enrolled patients.
Patients
Sixty-nine patients with single-segment LCSS who underwent Endo-ULBD at the Affiliated Hospital of Qingdao University from October 2020 to April 2021 were enrolled. They were divided into the iLESSYS Delta system group or the Endo-Surgi Plus system group according to the endoscopy system used.
Inclusion Criteria
Inclusion criteria are as follows: (I) patients had the typical symptoms of neurological claudication with unilateral or bilateral leg pain and low back pain that failed to respond to conservative treatment for at least 3 months; (II) single-segment LCSS confirmed by MRI/CT images, consistent with the segmental location of symptoms and signs; (III) patients underwent Endo-ULBD using the iLESSYS Delta system or Endo-Surgi Plus system; (IV) complete follow-up lasted for 12 months.
Exclusion Criteria
Exclusion criteria are as follows: (I) MRI/CT images showed stenosis involving two or more segments or with significant foraminal stenosis; (II) flexion–extension lateral films suggest lumbar segmental instability; (III) patients with obvious cauda equina syndrome or combined with fractures, tumors, and associated infection of the canal stenosis segment or with mental disorders; (IV) previous lumbar surgery history.
Endoscopic Instruments
Both endoscopy systems extended the diameter of the working cannula and the endoscopic internal working channel as compared to the conventional spinal endoscopy system represented by TESSYS. The Endo-Surgi Plus system features a uniquely designed lockable U/T combination working cannula, and collocates a fully visualized trephine which could replace the T cannula position for bone decompression under endoscopic direct view. In contrast, the iLESSYS Delta system includes a wider diameter and shorter length of working cannula and endoscopic internal working channel to facilitate operation and positioning, and the primary bone decompression was conducted using an Endo-high speed drill. In addition, both endoscopy systems are equipped with radiofrequency electrode, grasping forceps, and Endo-Kerrison punches for soft tissue removal and aid bone decompression. Table 1 and Fig. 1 demonstrate the appearance and parameters of the two large channel endoscopy systems.
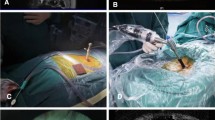
iLESSYS Delta system and Endo-Surgi Plus system. The iLESSYS Delta system has an endoscope channel and working cannula of shorter length and larger diameter (a) and uses the Endo-high speed drill and Endo-Kerrison punch as main tools for bone decompression (b). The Endo-Surgi Plus system has an endoscope channel and combined working cannulas (U and T) of longer length and smaller diameter (c), and uses the fully visualized trephine (whole tooth and half teeth) and Endo-Kerrison punch as main tools for bone decompression (d)
Anesthesia and Approach
All patients underwent general anesthesia with endotracheal intubation and the main surgical procedures were performed by the same skilled surgeon. The patient was prone on the Wilson frame with the hips and knees slightly bent. The skin incision was usually selected on the side with severe symptoms, with a length of 1–2 cm, and its exact location with surface projection of the inner upper margin of the inferior pedicle was confirmed by fluoroscopy. Then, the serial dilators were advanced to the target through the incision. After introducing the working cannula, the dilators were removed and the endoscope was introduced.
Surgical Techniques for Endo-Surgi Plus System
First, the nucleus pulposus forceps and radiofrequency electrode were used to clean the soft tissue and hemostasis under the endoscope so that the interlaminar window was exposed. The lower edge of the superior lamina, the upper edge of the inferior lamina, and the middle and lower portions of the inferior articular process were removed using the fully visualized trephine until the cephalic, caudal, and lateral boundaries of the ligamentum flavum appeared. The contralateral ligamentum flavum was also exposed by undercutting the base of the spinous process and the ventral portion of the contralateral lamina. Then, the ligamentum flavum was removed completely to enlarge the central canal and expose the ipsilateral traversing nerve root, dural sac, and dorsal of the contralateral traversing nerve root. The fully visualized trephine (half toothed) or Endo-Kerrison punch could be used for further excision of the medial side of the articular process to decompress the lateral recess and completely reveal the shoulder of the traversing nerve root when the bilateral articular process is cohesive and hyperplastic. Subsequently, ipsilateral and/or contralateral discectomy was performed depending on whether there is a disc herniation on the ventral side. Throughout the process, the angle and position of the working cannula can be flexibly changed to provide sufficient operating space (Figs. 2 and 3). A typical case is shown in Fig. 4.
Schematic of unilateral laminotomy for bilateral decompression (a–d). Bone decompression of the central spinal canal was performed using the Endo-high speed drill or fully visualized trephine (a, c), and decompression of lateral recess was performed after complete resection of the ligamentum flavum (b, d). The working cannula of the iLESSYS Delta system can only be suspended on the dorsal of the spinal canal (a, b), while the combined working cannulas can penetrate the spinal canal and help push off the dural sac in the Endo-Surgi Plus system (c, d). Before the operation, the “initial point” is pre-marked (e, red circle) and the working cannulas are placed accordingly (f). A large number of blood clots were observed under endoscopy (g) in a patient with postoperative hematoma and evacuation of hematoma was performed (h). This figure has been adapted using an image created with BioRender.com
Intraoperative endoscopic views of unilateral laminotomy for bilateral decompression by Endo-Surgi Plus system. a The interlaminar window was identified. b Fully visualized trephine was used to resect the upper edge of inferior lamina exposing the boundary of the ligamentum flavum (c). d Fully visualized trephine was used to resect the base of the spinous process. e The ligamentum flavum was being resected and the epidural space was exposed. f, g The medial of the ipsilateral facet was resected to decompress the lateral recess. h The medial of the contralateral facet was resected to decompress the lateral recess. SL superior lamina, IL inferior lamina, LF ligamentum flavum, BLF boundary of the ligamentum flavum, BSP base of spinous process, DS dural sac
A 73-year-old male patient presented with neurological claudication of both legs and underwent unilateral laminotomy for bilateral decompression using Endo-Surgi Plus system. a Preoperative 3D CT, b–e preoperative axial and sagittal MRI showed grade D (Schizas classification) central stenosis at the L4/5 segment. f Postoperative 3D CT showed significant enlargement of the left interlaminar window at L4/5 and good preservation of the facet joint. g–j Postoperative axial and sagittal MRI showed that the central canal is widely decompressed and enlarged to grade A
Surgical Techniques for iLESSYS Delta System
The surgical procedure of the iLESSYS Delta system is similar to that of the Endo-Surgi Plus system. The anatomy of the interlaminar window was also identified first under the endoscope. The bony edges of the interlaminar window, the base of the spinous process, and the ventral portion of the contralateral lamina are thinned respectively by the Endo-high speed drill (8000 rpm) and the remaining thin layer of bone was removed by the Endo-Kerrison punch. Then, the ligamentum flavum could be completely removed from the boundary to enlarge the central canal. To decompress the lateral recess completely, the hyperplasia of the articular processes may require removal by Endo-Kerrison punch and Endo-high speed drill. At the same time, the iLESSYS Delta system allowed removal of the ipsilateral herniated disc following exploration (Figs. 2 and 5). A typical case is shown in Fig. 6.
Intraoperative endoscopic views of unilateral laminotomy for bilateral decompression by iLESSYS Delta system. a The interlaminar window was identified. b Endo-high speed drill was used to thin the lower edge of the superior lamina. c Endo-Kerrison punch was used to remove the thinning lamina and expose the boundary of the ligamentum flavum. d Grinding the base of the spinous process. e The ligamentum flavum was separated from the boundary for complete resection. f, g The medial of the ipsilateral facet was resected to decompress the lateral recess. h The medial of the contralateral facet was resected to decompress the lateral recess
A 66-year-old female patient presented with neurological claudication of both legs and underwent unilateral laminotomy for bilateral decompression using iLESSYS Delta system. a Preoperative 3D CT, b–e preoperative axial and sagittal MRI showed grade C (Schizas classification) central stenosis at the L4/5 segment. f Postoperative 3D CT showed significant enlargement of the right interlaminar window at L4/5 and good preservation of the facet joint. g–j Postoperative axial and sagittal MRI showed that the central canal is widely decompressed and enlarged to grade A
Procedural Endpoint
The procedural endpoint was when the decompression range reached the cephalic and caudal boundaries of the ligamentum flavum and the inner wall of the bilateral pedicle, and the dural sac and nerve root recovery rhythmic pulsation indicated that decompression is complete. After careful exploration and adequate hemostasis, the endoscope and working cannula were removed and the incision was closed with tissue glue.
Postoperative Care
Antiphlogistic, analgesic, and dehydration drugs were administered intravenously after surgery. Out-of-bed activity was initiated and functional exercises started with waist circumference.
Outcome Assessment and Follow-Up
Perioperative parameters such as operation time, incision length, postoperative hospital stay, and surgical complications between the two groups were recorded and compared. Schizas classification of preoperative and postoperative lumbar MRI reflects the dural sac expansion [28]. Visual analogue scale (VAS) for back and leg pain and Oswestry Disability Index (ODI) were calculated preoperatively and at 1 day, 3 months, 6 months, and 12 months after surgery to evaluate the clinical efficacy. The patient satisfaction was evaluated according to the modified MacNab criteria at the final follow-up.
Sample Size
The primary outcome measure, operative time, was recorded for the first 10 patients in the iLESSYS Delta system group (78 ± 13.37 min) and Endo-Surgi Plus system group (66 ± 14.49 min). On the basis of the data of the pilot study, considering a two-sided 0.05 significance level, with a power of 0.9, we estimated that at least 64 patients (32 per group) were required.
Statistical Processing
The data of categorical variables were expressed as frequency and percentage. The chi-square test was used for count data such as sex, surgical segment, and complications, and the Wilcoxon test was used for ranked data (paired samples or independent samples) such as MacNab criteria and Schizas classification. The data of numerical variables were represented by mean and standard deviation, normality was determined using the Shapiro–Wilk test, and comparisons were made using the t test (age, BMI, operation time, incision length, and hospital stay). Moreover, intra- and inter-group differences in VAS and ODI scores at each time point were evaluated using two-way repeated-measures analysis of variance (ANOVA). P < 0.05 indicates that the difference is statistically significant. SPSS version 25.0 software (SPSS Inc., Chicago, IL, USA) was used for the statistical analysis of all data.
Results
A total of 69 patients were recruited and divided into two groups. Among them, 37 of the patients were enrolled in the Endo-Surgi Plus system group and 32 in the iLESSYS Delta system group. There was a good balance between the two groups in sex, age, BMI, surgical segment, and Schizas classification (Table 2).
The operation time (66.35 ± 13.05 versus 76.88 ± 13.66 min) and incision length (12.65 ± 1.34 versus 18.03 ± 1.7 mm) in the Endo-Surgi Plus system group was shorter than in the iLESSYS Delta system group and the difference was statistically significant (p < 0.005). The postoperative hospital stay in both groups was comparable (2.06 ± 1.11 days in iLESSYS Delta system group and 2.24 ± 0.83 days in Endo-Surgi Plus system group, p = 0.442). In the iLESSYS Delta system group, nerve root injury occurred in two cases with a complication rate of 6.25% and there was one case of root injury and one case of hematoma in the Endo-Surgi Plus system group, with a complication rate of 5.41%; however, the results did not show a statistical difference between the groups (p = 0.784) (Table 3).
The postoperative VAS and ODI scores at each follow-up point in both groups were significantly improved time-dependently compared with the preoperative counterparts (p < 0.05), while comparisons between the two groups revealed no differences in scores at the same times. According to Schizas classification, the dural sac area was significantly expanded in both groups compared to preoperative values (p < 0.001), while they were roughly equal in the same period between the two groups. As for the MacNab criteria, the combined excellent and good rate of the two groups was 81.25% in the iLESSYS Delta system group and 81.08% in the Endo-Surgi Plus system group at the final follow-up; however, the results did not demonstrate a statistical difference (p = 0.773) (Table 4 and Fig. 7).
Visualization of data comparison of functional outcomes of LCSS treated using the iLESSYS Delta system and Endo-Surgi Plus system. Visual analog scale (VAS) scores for back pain (a), VAS scores for leg pain (b), and Oswestry disability index (ODI) scores (c) showed a significantly improved trend postoperatively compared with preoperative values in both groups
Discussion
The complexity of LCSS is that its compression source comes from all directions, including the ligamentum flavum, facet joint, intervertebral disc, posterior longitudinal ligament, and sometimes concurrently with lumbar spondylolisthesis and scoliosis [4, 29]. Therefore, tissue resection in one direction may be difficult and ineffective. Extensive total laminectomy, which was first proposed, is canonical until today, and there are still many imperfections, for example, that could lead to iatrogenic instability. Even with instrument fixation and interbody fusion, additional serious complications seem to occur, such as adjacent segmental disease, internal fixation failure, and poor intervertebral fusion [30, 31].
The rapid aging of the population and criticism relating to postoperative complications continue to drive the updating and integration of spinal surgical concepts, techniques, and equipment, and experienced surgeons have never stopped exploring less invasive and effective treatment choices. Since 1981, there has been a growing understanding of “limited decompression” which means that symptom elimination may not necessitate extensive decompression, but can reduce pressure to a level below the threshold for triggering symptoms [32,33,34]. Poletti [35] began the exploration of unilateral laminotomy for bilateral ligamentectomy for patients with central canal stenosis caused by ligamentum flavum hypertrophy in 1995, and Spetzger [18, 19] formally proposed and named the technique “unilateral laminotomy for bilateral decompression” in 1997. Later, the combination with MED resulted in ULBD being less invasive. On the other hand, Yeung [36] designed the Yeung endoscopy spine system (YESS) in 1997, and after several improvements, the percutaneous endoscopic technique was highly recommended in the treatment of some degenerative disc diseases. As a result of the small operation channel, poor visualization, and low decompression efficiency, the wide compression environment posed a great challenge for the treatment of LCSS under percutaneous endoscopy. It was not until 2011, when Ruetten [37] introduced a drill into the endoscopic system, that Endo-ULBD was used to treat spinal stenosis. Although Ruetten mentioned that the trend of spinal surgery had shifted from “aggressive” to “selective” at that time, the objective of adequate and accurate decompression has not changed in the treatment of LCSS. However, the standard endoscopy system with 6.0 mm for working cannula and 3.7 mm for endoscopic internal working channel reduced the degree of visualization and decompression efficiency of surgery, so the application of Endo-ULBD was still limited.
The emergence of the large channel endoscopic systems and full endoscopic visualization technique for the transforaminal or interlaminar approach of percutaneous endoscopic surgery is a qualitative improvement, no matter the indications, surgical efficiency, and surgical safety aspects [38, 39]. The expansion of the working cannula and endoscopic internal working channel can increase the anatomical structure and visual field, improve the degree of freedom for operation, and is also the basis of the full endoscopic visualization technique. In addition, the larger channel can accommodate larger size and higher strength instruments, improving surgical efficiency. These innovations shine a light on the application of Endo-ULBD for LCSS treatment [25]. In our study, both types of large channel endoscopic systems had ideal clinical outcomes when applied in Endo-ULBD for the treatment of LCSS. In addition, we summarized the indications and technical points of the two sets of equipment in continuous practice.
The iLESSYS Delta system, which was introduced in 2016, significantly improved the difficulty of decompressing bony stenosis that existed with traditional spinal endoscopic surgery. A large working cannula combined with the Endo-high speed drill and Endo-Kerrison punch allows for comprehensive removal of bony structures. When bony decompression is performed under the iLESSYS Delta system, the necessary procedures include thinning the bone with the Endo-high speed drill, and complete removal of the residual bony compressor with the Endo-Kerrison punch. These cumbersome processes and the small effective working diameter of the instruments, to some extent, reduced the efficiency of bony decompression and prolong the operation time compared with the Endo-Surgi Plus system. The working cannula has a large outer diameter and short length, and the field of vision can be changed freely by adjusting the angle, but it can only be suspended on the dorsal side of the spinal canal instead of penetrating the spinal canal. The soft tissue bleeding deep in the spinal canal is difficult to control, and it is impossible to expose and deal with the contralateral intervertebral disc herniation. The maximum spinal canal decompression can only be performed at a range of 270° (Fig. 2).
The Endo-Surgi Plus system, launched in 2018, has a wider range of indications. The length and diameter of the U/T combined cannula are moderate, which makes the endoscopic vision field larger and the anatomical structure easier to identify. Meanwhile, the cannula itself can penetrate the spinal canal, which is more conducive to decompression and hemostasis. The coordinate rotation of the combined cannulas can push out the nerves and dural sac to better expose the bilateral lateral recess and intervertebral disc and could achieve 360° spinal canal decompression when necessary. The application of the fully visualized trephine with a larger diameter makes the efficiency of bony decompression significantly higher than that of the Endo-high speed drill and Endo-Kerrison punch. It should be noted that it is difficult to identify the depth and direction of decompression and there is a risk of trephine slip during bony decompression, which may damage nerves and dural sac. At the beginning of decompression, one must rotate the trephine in the direction of the sawtooth to firmly lock the position and then reverse rotate to improve efficiency. When the piece of bone is seen rotating with the trephine, it has been dissociated. Certainly, the Endo-Kerrison punch can also be used to remove the remaining small pieces of bone (Fig. 2).
The location of the cannula is crucial for accurate decompression. We marked the surface projection of the inner upper margin of the pedicle which was identified on the anteroposterior fluoroscopy parallel to the intervertebral space as the operation “initial point”. The placement of the cannula and endoscope at the “initial point” is convenient to dissect the interlaminar window, lamina, and articular process under the endoscope, and conducive to the subsequent adjustment of cannula position, providing the best vision and operation space. The lower portion of the inferior articular process corresponding to the “initial point” is the bony structure where excision is required first. Then, the safe deep area is exposed, medial to the ligamentum flavum and lateral to the superior articular process. This allows the identification of anatomical structures and locations in the spinal canal and subsequent decompression with excellent visualization. It is necessary to choose appropriate instruments such as fully visualized trephine (whole tooth or half tooth), Endo-Kerrison punch, and Endo-high speed drill according to the situation during decompression of bony stenosis, while important markers such as the midline of the ligamentum flavum can assist in judging the anatomy and localization.
The key to treating the narrow central canal is to remove hypertrophic ligamentum flavum, proliferative and cohesive facet joints, and some attached osteophytes. The limited decompression strategy followed by Endo-ULBD only requires removal of the ligamentum flavum after partial excision of the medial facet joint and ventral lamina. Although the decompression range of this minimally invasive surgery is far less than that of traditional open surgery, it has been reported in the literature that it has comparable efficacy. Ruetten’s [37] study results show that Endo-ULBD is a sufficient and safe supplement and alternative to conventional procedures and offers the advantages of being minimally invasive. In Zhao’s study [25], compared with the traditional posterior lumbar interbody fusion (PLIF) procedure, Endo-ULBD applied to LSS achieved a better lumbar function score in the early postoperative period, with the advantages of less trauma, fast recovery, and short operation time. Consistently, our study showed that the excellent and good rates in both groups were over 80%, and the postoperative VAS and ODI scores steadily improved over time compared with those before surgery. There is no difference in functional scores between the two groups. In terms of imaging evaluation of Schizas classification, the dural sac was generally well expanded after surgery. These data indicate that the clinical efficacy of Endo-ULBD is not inferior to open surgery while minimizing trauma.
Compared with other spinal canal decompression operations reported in the literature, including total laminectomy (124.4 ± 34.2 min) [40], minimally invasive ULBD (77 ± 28 min) [16], Med-ULBD (56.4 ± 4.7 min) [41], and Endo-ULBD (68.9 ± 10.0 min) [42], the operative time of both groups in this study was at a similar level (66.35 ± 13.05 min in the Endo-Surgi Plus system group versus 76.88 ± 13.66 min in the iLESSYS Delta system group). Interestingly, the operation time of the Endo-Surgi Plus group is less than that of the iLESSYS Delta group (p < 0.005). We believe that the use of the fully visualized trephine does simplify the process and improve its efficiency. ULBD minimizes unnecessary excision of bone and joint structures, and studies have shown that the procedure did reduce the high incidence of instability and reoperation that occurred after traditional laminectomy [43,44,45,46,47]. However, Kuo reported that the reoperation rate in the ULBD group at the 5-year follow-up was up to 10.4% and was more frequent at the index surgical level. Biomechanical studies have demonstrated that the facet joint is subjected to a great deal of rotation and flexion stress and it is important for segmental stability; the range to which the facet joint resection will not affect the stability of the spine continues to be controversial [48, 49]. Here, we also recommend that no more than half of the facet joint be removed, but further research is needed to provide high-quality evidence.
Bleeding seriously affects the identification of the field vision under the endoscope, impedes decompression operations, and increases the probability of complications such as nerve injury, and frequent hemostasis reduces work efficiency and increases surgical time. Moreover, postoperative hematoma is a disaster for patients. In the Endo-Surgi Plus group, one patient suffered a hematoma that presented as acute pain in the lower extremities 12 h after surgery and gradually evolved to numbness and weakness. Spinal canal exploration was performed under the endoscope, and a large number of blood clots were found in the spinal canal, and the pulsing of the dural sac disappeared. The symptoms improved significantly after the evacuation of hematoma. In our study, to reduce bleeding, epinephrine diluents were applied to infiltrating layers along the predetermined incision and cannula path to the lamina surface before cannula placement. After that, the soft tissue on the lamina surface was bluntly exfoliated during the advance of the first stage dilators. We prefer to use general anesthesia and keep systolic pressure at about 110 mmHg to reduce bleeding while avoiding discomfort caused by unsatisfactory local anesthesia and increased cerebrospinal fluid pressure due to saline perfusion [50].
Nerve injury during spinal endoscopic surgery needs special attention. As a result of space and visual limitations, the ULBD technique has been reported to possibly increase the incidence of nerve injury and dural tears [22, 51]. In the present study, there were two cases in the iLESSYS Delta system group and one case in the Endo-Surgi Plus system group for nerve injury, both of which were identified as the nerve root outer membrane tears occurring in the process of removing the surrounding tissue adhered to the nerve root by the Endo-Kerrison punch. The was no dural sac defect in both groups. The incidence of nerve injury in the two groups was 6.25% and 2.70%, respectively, which was similar to the 3.1% in previous studies [52]. Except for the surgeon’s rich experience in endoscopic technique, the optimistic data also benefit from the excellent visualization provided by the large channel endoscopic systems and the protection of the integrity of the ligamentum flavum during bone decompression. Although Endo-Surgi Plus can push and debond the nerve and dural sac through the coordinated rotation of the U/T cannula and then remove the bilateral intervertebral discs, this may strongly stimulate the nerve and lead to postoperative paralysis. Therefore, we recommend that learners carefully carry out the program under nerve monitoring. There were no other complications in the two groups, and the overall complication rate was 6.25% in the iLESSYS Delta system group and 5.41% in the Endo-Surgi Plus system group, respectively, which was consistent with or even lower than the previous literature [23, 25, 45, 53]. It can be considered that both endoscopic systems have satisfactory safety when used to perform ULBD.
In brief, scientific and technological progress and theoretical innovation have brought about continuous qualitative change at the medical level. We believe that the large channel endoscopic systems and full endoscopic visualization technique provided excellent visualization and efficiency, which is a leap. The Endo-ULBD established on the basis of the aforementioned systems can only be deemed to be a better choice for certain types of patients at this stage, but it is certainly not the ultimate perfect choice, because medical research continues to evolve.
Limitations
There are several limitations to our study. First, this is a retrospective study with small sample size, short follow-up time, and no randomization; some biases cannot be excluded. Long-term follow-up of large samples is required to evaluate the efficacy of ULBD under large channel endoscopic systems combined with full endoscopic visualization technique for patients with LCSS. Second, since the early clinical results of this study did not occur in iatrogenic spinal instability and reoperation after Endo-ULBD, we did not conduct a specific study in this area. That does not mean it is unimportant; on the contrary, it is a subject that needs to be agreed upon.
Conclusions
Current research suggests that the two studied endoscopic systems achieved excellent early outcomes for the treatment of LCSS, with high-level safety, less bleeding, faster postoperative recovery, and fewer complications. Compared with iLESSYS Delta, Endo-Surgi Plus may have benefited from the use of the fully visualized trephine and is more effective in treating bone stenosis, with shorter surgical time. Moreover, Endo-Surgi Plus may have a wider decompression reach range and applies to the management of central canal stenosis associated with bilateral disc herniation.
References
Jensen RK, Jensen TS, Koes B, Hartvigsen J. Prevalence of lumbar spinal stenosis in general and clinical populations: a systematic review and meta-analysis. Eur Spine J. 2020;29(9):2143–63.
Deyo RA, Mirza SK, Martin BI, Kreuter W, Goodman DC, Jarvik JG. Trends, major medical complications, and charges associated with surgery for lumbar spinal stenosis in older adults. JAMA. 2010;303(13):1259–65.
Hallinan J, Zhu L, Yang K, et al. Deep learning model for automated detection and classification of central canal, lateral recess, and neural foraminal stenosis at lumbar spine MRI. Radiology. 2021;300(1):130–8.
Siebert E, Prüss H, Klingebiel R, Failli V, Einhäupl KM, Schwab JM. Lumbar spinal stenosis: syndrome, diagnostics and treatment. Nat Rev Neurol. 2009;5(7):392–403.
Nerland US, Jakola AS, Solheim O, et al. Minimally invasive decompression versus open laminectomy for central stenosis of the lumbar spine: pragmatic comparative effectiveness study. BMJ. 2015;350: h1603.
Sihvonen T, Herno A, Paljärvi L, Airaksinen O, Partanen J, Tapaninaho A. Local denervation atrophy of paraspinal muscles in postoperative failed back syndrome. Spine. 1993;18(5):575–81.
Iida Y, Kataoka O, Sho T, et al. Postoperative lumbar spinal instability occurring or progressing secondary to laminectomy. Spine. 1990;15(11):1186–9.
Crocker A, Kornilo A, Conly J, Henderson E, Rennert-May E, Leal J. Using administrative data to determine rates of surgical site infections following spinal fusion and laminectomy procedures. Am J Infect Control. 2021;49(6):759–63.
Zaina F, Tomkins-Lane C, Carragee E, Negrini S. Surgical versus non-surgical treatment for lumbar spinal stenosis. Cochrane Database Syst Rev. 2016;2016(1):10264.
Kanno H, Aizawa T, Hahimoto K, Itoi E. Minimally invasive discectomy for lumbar disc herniation: current concepts, surgical techniques, and outcomes. Int Orthop. 2019;43(4):917–22.
Choi KC, Kim JS, Park CK. Percutaneous endoscopic lumbar discectomy as an alternative to open lumbar microdiscectomy for large lumbar disc herniation. Pain Physician. 2016;19(2):E291-300.
Sharif S, Afsar A. Learning curve and minimally invasive spine surgery. World Neurosurg. 2018;119:472–8.
Lee SH, Kang BU, Ahn Y, et al. Operative failure of percutaneous endoscopic lumbar discectomy: a radiologic analysis of 55 cases. Spine. 2006;31(10):E285–90.
Basil GW, Kumar V, Wang MY. Optimizing visualization in endoscopic spine surgery. Oper Neurosurg (Hagerstown). 2021;21(Suppl 1):S59-s66.
Ahn Y. Endoscopic spine discectomy: indications and outcomes. Int Orthop. 2019;43(4):909–16.
Thomé C, Zevgaridis D, Leheta O, et al. Outcome after less-invasive decompression of lumbar spinal stenosis: a randomized comparison of unilateral laminotomy, bilateral laminotomy, and laminectomy. J Neurosurg Spine. 2005;3(2):129–41.
Usman M, Ali M, Khanzada K, et al. Unilateral approach for bilateral decompression of lumbar spinal stenosis: a minimal invasive surgery. J Coll Physicians Surg Pak. 2013;23(12):852–6.
Spetzger U, Bertalanffy H, Naujokat C, von Keyserlingk DG, Gilsbach JM. Unilateral laminotomy for bilateral decompression of lumbar spinal stenosis. Part I: anatomical and surgical considerations. Acta Neurochir (Wien). 1997;139(5):392–6.
Spetzger U, Bertalanffy H, Reinges MH, Gilsbach JM. Unilateral laminotomy for bilateral decompression of lumbar spinal stenosis. Part II: clinical experiences. Acta Neurochir (Wien). 1997;139(5):397–403.
Guiot BH, Khoo LT, Fessler RG. A minimally invasive technique for decompression of the lumbar spine. Spine. 2002;27(4):432–8.
Khoo LT, Fessler RG. Microendoscopic decompressive laminotomy for the treatment of lumbar stenosis. Neurosurgery. 2002;51(5 Suppl):S146–54.
Mobbs RJ, Li J, Sivabalan P, Raley D, Rao PJ. Outcomes after decompressive laminectomy for lumbar spinal stenosis: comparison between minimally invasive unilateral laminectomy for bilateral decompression and open laminectomy: clinical article. J Neurosurg Spine. 2014;21(2):179–86.
Minamide A, Yoshida M, Yamada H, et al. Endoscope-assisted spinal decompression surgery for lumbar spinal stenosis. J Neurosurg Spine. 2013;19(6):664–71.
Wei FL, Du MR, Li T, et al. Therapeutic effect of large channel endoscopic decompression in lumbar spinal stenosis. Front Surg. 2021;8: 603589.
Zhao XB, Ma HJ, Geng B, Zhou HG, Xia YY. Percutaneous endoscopic unilateral laminotomy and bilateral decompression for lumbar spinal stenosis. Orthop Surg. 2021;13(2):641–50.
Li C, Tang X, Chen S, Meng Y, Zhang W. Clinical application of large channel endoscopic decompression in posterior cervical spine disorders. BMC Musculoskelet Disord. 2019;20(1):548.
Song QP, Hai B, Zhao WK, et al. Full-endoscopic foraminotomy with a novel large endoscopic trephine for severe degenerative lumbar foraminal stenosis at L(5) S(1) level: an advanced surgical technique. Orthop Surg. 2021;13(2):659–68.
Schizas C, Theumann N, Burn A, et al. Qualitative grading of severity of lumbar spinal stenosis based on the morphology of the dural sac on magnetic resonance images. Spine. 2010;35(21):1919–24.
Genevay S, Atlas SJ. Lumbar spinal stenosis. Best Pract Res Clin Rheumatol. 2010;24(2):253–65.
Okuda S, Iwasaki M, Miyauchi A, Aono H, Morita M, Yamamoto T. Risk factors for adjacent segment degeneration after PLIF. Spine. 2004;29(14):1535–40.
Fogel GR, Toohey JS, Neidre A, Brantigan JW. Outcomes of L1–L2 posterior lumbar interbody fusion with the Lumbar I/F cage and the variable screw placement system: reporting unexpected poor fusion results at L1–L2. Spine J. 2006;6(4):421–7.
Crock HV. Normal and pathological anatomy of the lumbar spinal nerve root canals. J Bone Joint Surg Br. 1981;63(4):487–90.
Young S, Veerapen R, O’Laoire SA. Relief of lumbar canal stenosis using multilevel subarticular fenestrations as an alternative to wide laminectomy: preliminary report. Neurosurgery. 1988;23(5):628–33.
Aryanpur J, Ducker T. Multilevel lumbar laminotomies: an alternative to laminectomy in the treatment of lumbar stenosis. Neurosurgery. 1990;26(3):429–32.
Poletti CE. Central lumbar stenosis caused by ligamentum flavum: unilateral laminotomy for bilateral ligamentectomy: preliminary report of two cases. Neurosurgery. 1995;37(2):343–7.
Yeung AT. Minimally invasive disc surgery with the yeung endoscopic spine system (YESS). Surg Technol Int. 1999;8:267–77.
Komp M, Hahn P, Merk H, Godolias G, Ruetten S. Bilateral operation of lumbar degenerative central spinal stenosis in full-endoscopic interlaminar technique with unilateral approach: prospective 2-year results of 74 patients. J Spinal Disord Tech. 2011;24(5):281–7.
Hua W, Zhang Y, Wu X, et al. Full-endoscopic visualized foraminoplasty and discectomy under general anesthesia in the treatment of L4–L5 and L5–S1 disc herniation. Spine. 2019;44(16):E984–91.
Hua W, Zhang Y, Wu X, et al. Outcomes of discectomy by using full-endoscopic visualization technique via the interlaminar and transforaminal approaches in the treatment of L5–S1 disc herniation: an observational study. Medicine (Baltimore). 2018;97(48): e13456.
Ghogawala Z, Dziura J, Butler WE, et al. Laminectomy plus fusion versus laminectomy alone for lumbar spondylolisthesis. N Engl J Med. 2016;374(15):1424–34.
Heo DH, Lee DC, Park CK. Comparative analysis of three types of minimally invasive decompressive surgery for lumbar central stenosis: biportal endoscopy, uniportal endoscopy, and microsurgery. Neurosurg Focus. 2019;46(5):E9.
Wu MH, Wu PC, Lee CY, et al. Outcome analysis of lumbar endoscopic unilateral laminotomy for bilateral decompression in patients with degenerative lumbar central canal stenosis. Spine J. 2021;21(1):122–33.
Alimi M, Hofstetter CP, Pyo SY, Paulo D, Härtl R. Minimally invasive laminectomy for lumbar spinal stenosis in patients with and without preoperative spondylolisthesis: clinical outcome and reoperation rates. J Neurosurg Spine. 2015;22(4):339–52.
McGrath LB, White-Dzuro GA, Hofstetter CP. Comparison of clinical outcomes following minimally invasive or lumbar endoscopic unilateral laminotomy for bilateral decompression. J Neurosurg Spine. 2019;2:1–9.
Oertel MF, Ryang YM, Korinth MC, Gilsbach JM, Rohde V. Long-term results of microsurgical treatment of lumbar spinal stenosis by unilateral laminotomy for bilateral decompression. Neurosurgery. 2006;59(6):1264–9.
Kuo CC, Merchant M, Kardile MP, Yacob A, Majid K, Bains RS. In degenerative spondylolisthesis, unilateral laminotomy for bilateral decompression leads to less reoperations at 5 years when compared to posterior decompression with instrumented fusion: a propensity-matched retrospective analysis. Spine. 2019;44(21):1530–7.
Hong SW, Choi KY, Ahn Y, et al. A comparison of unilateral and bilateral laminotomies for decompression of L4–L5 spinal stenosis. Spine. 2011;36(3):E172–8.
Panjabi MM. Clinical spinal instability and low back pain. J Electromyogr Kinesiol. 2003;13(4):371–9.
Hasegawa K, Kitahara K, Shimoda H, Hara T. Facet joint opening in lumbar degenerative diseases indicating segmental instability. J Neurosurg Spine. 2010;12(6):687–93.
Zhou C, Zhang G, Panchal RR, et al. Unique complications of percutaneous endoscopic lumbar discectomy and percutaneous endoscopic interlaminar discectomy. Pain Physician. 2018;21(2):E105–12.
Tsutsumimoto T, Yui M, Uehara M, Ohta H, Kosaku H, Misawa H. A prospective study of the incidence and outcomes of incidental dural tears in microendoscopic lumbar decompressive surgery. Bone Joint J. 2014;96(5):641–5.
Hua W, Wang B, Ke W, et al. Comparison of lumbar endoscopic unilateral laminotomy bilateral decompression and minimally invasive surgery transforaminal lumbar interbody fusion for one-level lumbar spinal stenosis. BMC Musculoskelet Disord. 2020;21(1):785.
Soliman HM. Irrigation endoscopic decompressive laminotomy. A new endoscopic approach for spinal stenosis decompression. Spine J. 2015;15(10):2282–9.
Acknowledgements
Funding
This study and the journal’s Rapid Service Fee were funded by the National Natural Science Foundation of China (No. 81871804), the National Key Research and Development Program of China (No. 2019YFC0121400), and the Natural Science Foundation of Shan Dong Province (No. ZR2021MH020).
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole and have given their approval for this version to be published.
Author Contributions
Conceptualization: CZ and XM; Methodology: SH and XZ; Formal analysis and investigation: JH, AL, GL, KZ, XW, YS, DX, HZ, SM, and XL. Writing-original draft preparation: SH and XZ; Writing-review and editing: CZ, XM, HT, SH, and XZ; Funding acquisition: KZ and XW; Resources: CZ and XM; Supervision: CZ and XM.
Compliance with Ethics Guidelines
The study was performed according to the Declaration of Helsinki (as revised in 2013). The study was approved by the Medical Ethics Committee of The Affiliated Hospital of Qingdao University (No. QYFY WZLL 27,073). This study has obtained the informed consent of enrolled patients.
Disclosures
Shuo Han, Xiangxu Zeng, Kai Zhu, Xiaoqi Wu, Yanqing Shen, Jialuo Han, Antao Lin, Shengwei Meng, Hao Zhang, Guanghui Li, Xiaojie Liu, Xuexiao Ma, Hao Tao, Chuanli Zhou have nothing to disclose.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Han, S., Zeng, X., Zhu, K. et al. Clinical Application of Large Channel Endoscopic Systems with Full Endoscopic Visualization Technique in Lumbar Central Spinal Stenosis: A Retrospective Cohort Study. Pain Ther 11, 1309–1326 (2022). https://doi.org/10.1007/s40122-022-00428-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40122-022-00428-3