Abstract
Alzheimer’s disease (AD) is the most common type of dementia associated with amyloid beta (Aβ) deposition. Dysfunction of the neuronal clearance pathway promotes the accumulation of Aβ. The plasminogen-activating system (PAS) is controlled by various enzymes like tissue plasminogen activators (tPA). Neuronal tPA enhances the conversion of plasminogen to plasmin, which cleaves Aβ; this function is controlled by many inhibitors of PAS, including a plasminogen-activating inhibitor (PAI-1) and neuroserpin. Therefore, the objective of the present narrative review was to explore the potential role of tPA/neuroserpin in the pathogenesis of AD. PAI-1 activity is increased in AD, which is involved in accumulating Aβ. Progressive increase of Aβ level during AD neuropathology is correlated with the over-production of PAI-1 with subsequent reduction of plasmin and tPA activities. Reducing plasmin and tPA activities promote Aβ by reducing Aβ clearance. Neuroserpin plays a critical role in the pathogenesis of AD as it regulates the expression and accumulation of Aβ. Higher expression of neuroserpin inhibits the neuroprotective tPA and the generation of plasmin with subsequent reduction in the clearance of Aβ. These observations raise conflicting evidence on whether neuroserpin is neuroprotective or involved in AD progression. Thus, neuroserpin over-expression with subsequent reduction of tPA may propagate AD neuropathology.
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s (AD) is a heterogeneous neurodegenerative disease with intricate neuropathological disorders. AD is the most common type of dementia, accounting for about 70% [1]. AD was first recognized by German psychiatrist Alois Alzheimer in 1906 in women with memory impairment [1]. AD affects 6% of the general population aged more than 65%, mainly in women, though 10% of early-onset dementia affecting people aged 30–60 years is attributed to AD [2]. Notoriously, AD affects 50 million people globally and is regarded as the 7th leading cause of death in the USA [2].
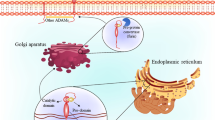
AD is associated with extracellular deposition of amyloid beta (Aβ), mainly Aβ1-42 in the neocortex and hippocampus, leading to dementia and cognitive decline [3]. AD is characterized by intracellular accumulation of phosphorylated tau proteins as neurofibrillary tangles (NFTs) and extracellular deposition of Aβ as neuritic plaques [1, 4, 5]. These neuropathological features remain the chief criteria for AD [4]. However, different mechanisms are proposed for AD pathogenesis, including inflammation, oxidative stress, cholinergic dysfunction, and impairment of the melatonin pathway [4, 5] (Fig. 1).
These changes affect the lysosomal and endosomal clearance pathways by developing synaptic dysfunction and forming senile amyloid plaques derived from transmembrane amyloid precursor protein (APP) [6]. A defective neuronal clearance pathway due to the dysfunction of degradation enzymes could be a possible mechanism for accumulating Aβ and NFTs in AD [7]. Protease enzymes such as matrix metalloproteinase 9 (MMP-9), endothelin converting enzyme, neprilysin, insulin-degrading enzyme, and plasmin are involved in the degradation and clearance of Aβ and NFTs [8, 9]. Notably, plasmin formed from plasminogen by the action of tissue plasminogen activators (tPA) cleaves monomeric and fibrillar Aβ [10]. Besides, tPA is highly expressed in the brain and implicated in disorders including cerebellar motor learning, hippocampal long-term potentiation, amygdala-mediated anxiety, and hypothalamic endocrine dysfunction [11]. Significantly, tPA is inhibited by serine proteases, including neuroserpin, α2-antiplasmin, and protease nexin-1 [11]. In addition, tPA is highly expressed in brain areas with high plaque deposition, while plasmin level is reduced in AD [10, 11].
Plasminogen activator inhibitor-1 (PAI-1) regulates the expression of vascular tPA, which has a fibrinolytic effect [12]. It has been shown that tPA has pleiotropic properties in the central nervous system (CNS), including neurogenesis, synaptic plasticity, neurodegeneration, regulation of blood–brain barrier (BBB) permeability, and neurovascular coupling [13, 14]. Besides, neuroserpin is regarded as a potent inhibitor of tPA and implicated in the pathogenesis of AD through dysregulation of Aβ and NFTs clearance [13, 14].
Moreover, cyclin-dependent kinase 5 (cdk5) and its activator p35 are one of the chief tau phosphorylation systems involved in the regulation of neuronal polarity during the development of CNS [15]. Aβ promotes cdk5 activity, increasing intra-neuronal accumulation of tau protein [16]. The formation of the cdk5-p35 complex by Aβ triggers the neurodegeneration process [16]. A previous experimental study conducted by Alvarez et al. [17] demonstrated that inhibition of cdk5 attenuates Aβ-induced neuronal death.
Depending on this scientific rationale, the objective of the present narrative review was to explore the potential role of the tPA/neuroserpin axis in the pathogenesis of AD.
Plasminogen activating system in AD
The plasminogen-activating system (PAS) is controlled by various enzymes, including tissue plasminogen activators (tPA) and urokinase plasminogen activator (uPA) for the synthesis of plasmin [18]. PAS is also regulated by plasminogen-activating inhibitor type 1 and type 2 (PA1-1) and (PAI-2), respectively [19]. Outside the CNS, PAS regulates fibrinolysis and homeostasis control [19]. PAS regulates AD pathogenesis; plasmin can cleave non-aggregated and aggregated fibrillar Aβ [20]. It has been reported that plasmin could attenuate Aβ-induced neuronal injury and death by enhancing Aβ clearance in the animal model study [21]. Jacobsen et al. [20] found that pharmacological inhibition of PAI-1 improves Aβ clearance via plasmin-mediated proteolysis in hippocampal slices from transgenic mice. Furthermore, plasmin activity is reduced in AD patients compared to healthy controls [11]. An in-vitro study observed that plasmin activity was reduced in the hippocampus of patients with AD due to a defect in the binding activity of plasmin. High neuronal membrane cholesterol impairs plasmin binding activity with the development of PAS dysfunction in AD [11]. Reduction of plasmin activity in AD patients is correlated with higher expression of ApoE, which is essential for neuronal cholesterol homeostasis and pathogenesis of AD [22]. Therefore, alteration of neuronal lipid raft through the expression of ApoE could be a possible mechanism in reducing plasmin activity and development of AD [21, 23]. A previous study by Ledesma et al. [24] confirmed that plasmin activity was reduced in the brains of AD patients. However, PAS and plasmin activity were not altered in AD patients’ temporal and frontal cortex homogenates [25]. A postmortem study involving 20 AD, 15 vascular dementia, and 20 healthy controls showed that plasminogen mRNA was normal in AD compared to controls [25]. This finding did not support the role of plasmin in the pathogenesis of AD. The cerebrospinal fluid (CSF) analysis study of AD patients and healthy controls revealed that tPA and PAI-1 levels were not altered compared to the controls [3]. The author concluded that plasmin activity in the CSF did not reflect the severity of AD pathology, so it was not valuable in diagnosing AD [3]. Notoriously, plasmin deficiency is not a secondary event but rather a primary event involved in the pathogenesis of AD [26].
Role of tPA in AD
The action of tPA is modulated by PAI-1, α2 macroglobulin, and streptokinase (Fig. 2). tPA is categorized as a serine protease essential for clot lysis; thus, activation of tPA by thrombolytic agents such as reteplase, alteplase, and tenecteplase is integral in the management of acute ischemic stroke within 3–4 h, myocardial infarction, arterial thrombosis, pulmonary embolism, and deep vein thrombosis [27, 28].
Principally, tPA plays a different function in the CNS as neurons and astrocytes express it. It regulates synaptic growth, neuronal migration, synaptic plasticity, modulation of neurotransmission, and cognitive enhancing effects [29]. Remarkably, tPA is synthesized, stored in the neurons, and released upon neuronal depolarization [30]. Neuronal tPA enhances the conversion of plasminogen to plasmin; this function is controlled by inhibitors of PAS, including PA1-1 and neuroserpin [31]. Experimental evidence confirmed that tPA and uPA exert neuroprotective effects independent of plasmin generation after ischemic stroke [31]. Rapid release of tPA from presynaptic neurons following brain ischemic events protects the synapses from the harmful effects of ischemia. In addition, released uPA during recovery promotes neuronal and synapse repairs [31]. These findings suggest neuroprotective and neuro-restorative effects of tPA and uPA. Thus, PAS could be a potential target in the modulation of pathologic processes in various neurodegenerative diseases.
Moreover, the plasminogen level in the AD brain was documented to be not altered compared to the matched controls due to impairment of plasminogen activation by tPA [32]. The underlying cause for the reduction of tPA is due to the co-localization of tPA with Aβ, which impairs tPA activity [32]. However, the tPA level did not change, but its activity was dramatically reduced in the AD brain compared to the controls [32]. TPA activity is notably reduced with aging, which may provoke AD development. TPA activity is significantly reduced in the AD brain compared to the control [33].
Role of PAI-1 in AD
It has been observed that PAI-1 activity and level are increased in AD according to the findings from animal and human studies [33, 34]. A case–control study illustrated that higher expression of PAI-1 and low tPA/PAI-1 ratio was observed in diabetic patients with cognitive impairment and memory dysfunction [34]. A higher PAI-1 plasma level is regarded as a potential biomarker in the detection of AD [35]. PAI-1 plasma level is negatively correlated with cognitive function [35]. A case–control study confirmed that AD patients' PAI-1 plasma level was reduced compared to controls [35]. In addition, the PAI-1 level was not changed in the frontal cortex in mice and human AD brains [36]. Higher PAI-1 and low tPA levels correlate with Aβ deposition in AD. Hence, reduced tPA may be the causal mechanism in AD development. Supporting this notion, tPA-deficient mice had defects in the removal of injected human Aβ1-42 as compared with wild-type mice [36].
Similarly, a more significant accumulation of Aβ1-42 was demonstrated in mice with genetically reduced endogenous tPA production [37]. It has been shown that tPA activity and expression are higher around Aβ plaques in the brains of human APP over-expressing Tg2576 mice, which have undergone a genetic ablation of tPA [37]. Reduction of tPA in the brain triggers the accumulation of Aβ1-42 with significant expression of a synaptic function-associated protein involved in developing synaptic dysfunction and cognitive deficits [37]. Different evidence from preclinical studies proposed that failure of synaptic function may occur earlier before the progression of neuronal loss and development of AD [38]. A cohort study illustrated that miR-210-3p, which reflects synaptic dysfunction, increased in AD patients [38]. Tian et al. [39] observed that blood extracellular vesicles carrying synaptic function-associated protein are potential biomarkers for diagnosing AD. A cross-sectional study showed that extracellular vesicle plasma levels were reduced in AD patients [40]. These findings suggest that synaptic dysfunctions precede symptomatic AD, and biomarkers of synaptic dysfunctions could be helpful in the detection of high-risk subjects.
The interaction between Aβ and PAS
It has been suggested that plaques play a critical role in sequestering the soluble form of Aβ to reduce its neurotoxic effect in AD [41]. Later on, plaque sequestration capacity is reduced with the time of AD progression, and soluble Aβ can diffuse extracellularly, causing extensive synaptic dysfunction and neuronal injury [42]. Sciaccaluga et al. [43] suggested that Aβ oligomers trigger intracellular and extracellular neurotoxicities through interaction with cell membrane ion channels and receptors. These pathological changes promote a profound imbalance between inhibitory and excitatory neurotransmitters with hyper-excitability development in AD [43]. In this state, hyper-excitability contributes to the deposition of Aβ and the development of neurodegeneration. Thus, an imbalance of neurotransmissions is attributed to oligomer Aβ deposition, and the reverse is invalid [40]. An imaging study and computational neuronal modeling involving AD patients demonstrated significant subpopulation alteration in the excitatory/inhibitory axis concerning the severity of Aβ deposition compared to the controls [40]. Therefore, synaptic dysfunction with the development of excitatory/inhibitory imbalance promotes Aβ-induced neuronal injury in AD.
Moreover, apolipoprotein E (ApoE) predisposes to the development and progression of AD in about 40% and is involved in the impairment of Aβ clearance [44, 45]. Soluble Aβ density isolated from AD patients is correlated with synaptic dysfunction and cognitive deficits. Soluble Aβ effect on tau protein phosphorylation and neurotoxicity had been confirmed in crossing human APP with tau transgenic mice [44]. Therefore, monoclonal antibodies against soluble Aβ could be effective against the progression of AD pathogenesis [46]. Human clinical trials that tested monoclonal antibodies, including solanezumab and bapineuzumab, against soluble Aβ were evaluated in managing mild-moderate AD [46]. Solanezumab in the Phase III trial was effective in treating AD patients. In addition, monoclonal antibodies, including gantenerumab, which binds fibrillary, and crenezumab, which binds soluble Aβ, revealed promising effects in preventing AD in pre-symptomatic susceptible subjects [46]. Aducanumab was the monoclonal antibody approved by the FDA in 2003 to manage mild AD [47].
It has been shown that soluble Aβ in AD affects the protective role of tPA through activation of PAI-1, which is involved in the accumulation of Aβ and inhibition activation of neuroprotective brain-derived neurotrophic factor (BDNF) [48]. Pro-BDNF is cleaved and activated to BDNF by plasmin that regulates the memory process and neuronal activity. Thus, through activation of the BDNF pathway, tPA improves synaptic plasticity in AD [49]. Therefore, modulation of tPA/PAI-1 could be a therapeutic strategy in managing AD (Fig. 3). These pathological changes through activation of p75NTR disrupt long-term potentiation and synaptic plasticity with the development of neurodegeneration and cognitive deficits. As well, activation of transient receptor kinase B (TrKB) by BDNF and N-methyl-D-aspartate (NMDR) by tPA promote neurogenesis and synaptic plasticity with amelioration of cognitive deficit in AD [50, 51].
Role of tissue plasminogen activators (tPA) in Alzheimer’s disease: neuronal tPA enhances the conversion of plasminogen to plasmin that prevents Aβ deposition and enhances the activation of neuroprotective brain-derived neurotrophic factor (BDNF). Activation of transient receptor kinase B (TrKB) by BDNF and N-methyl-D-aspartate (NMDR) by tPA promotes neurogenesis and synaptic plasticity with amelioration of cognitive deficit in AD-soluble Aβ activates plasminogen activator inhibitor (PAI-1) that responsible for the accumulation of Aβ and inhibition activation of BDNF leading to activation of p75 that disrupt synaptic plasticity with the development of neurodegeneration and cognitive deficits
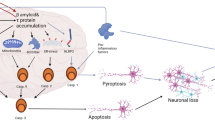
Indeed, soluble Aβ is more toxic than non-soluble ones in the neurons, leading to cognitive dysfunction through induction of synaptic dysfunction, disruption of signaling pathways, and AD neuropathology [41, 52]. It has been shown that soluble Aβ affects synaptic dysfunction through inhibition of tPA and activation of PAI-1 with subsequent effect on the expression of BDNF (Gregnani et al. 2020). An experimental study confirmed that soluble Aβ impairs the expression of BDNF through modulation of the tPA/PAI-1 axis in the AD mouse model [53]. Thus, the exaggeration of PAI-1 activity in AD attenuates the expression of tPA and plasmin generation from plasminogen [53]. Further reduction of BDNF due to the reduction of plasmin leads to neuronal atrophy and neuronal deaths [54] (Fig. 4).
It has been reported that a progressive increase of Aβ level during AD neuropathology is correlated with the over-production of PAI-1 with subsequent reduction of plasmin and tPA levels and activities [55]. In turn, the reduction of plasmin and tPA activities promotes Aβ accumulation by reducing Aβ clearance [56]. As well, Aβ-induced tPA dysfunction leads to neurovascular disorders [57]. Thus, exogenous tPA or pharmacological inhibition of PAI-1 can attenuate Aβ-induced neurovascular dysfunction [56]. Likewise, Aβ activates astrocyte expression of PAI-1 in the cerebral cortex [58]. Injection of exogenous Aβ in mice brains promotes the expression of PAI-1 [58]. Besides, different studies revealed that pro-inflammatory cytokines reduce tPA and increase the formation of PAI-1 [59, 60]. For example, tranexamic acid has an anti-inflammatory effect by inhibiting tPA by reducing plasmin-mediated complement activation. Since tranexamic acid does not affect uPA, it increases uPA-mediated plasmin generation and complements activation by releasing pro-inflammatory cytokines [61]. Besides, IL-6 activates the release of PAI-1 and promotes the development of endothelial dysfunction during cytokine-releasing syndrome [60]. Notably, higher expression of pro-inflammatory cytokines and inflammatory processes around Aβ plaques promote the expression of PAI-1 in the brain of AD patients [61]. Thus, anti-inflammatory agents might be a therapeutic strategy to prevent Aβ accumulation.
Taken together, inherited or acquired defect in the brain plasmin/tPA pathway promotes the accumulation of Aβ, which stimulates the expression and generation of PAI-1. In this state, activated PAI-1 reduces the neuroprotective effect of plasmin with further Aβ accumulation. Therefore, there is a positive feedback loop between PAI-1 expression and the pathogenesis of AD.
Neuroserpin in AD
Neuroserpin is a protease inhibitor involved in various physiological functions, including synapse formation and axonal growth [62]. Neuroserpin is mainly expressed in the CNS, responsible for synaptogenesis and axonogenesis during embryonic life and regulation of synaptic plasticity in adults [62]. Neuroserpin is also expressed outside the CNS in the pancreas, testis, liver, kidney, and immune cells [63]. Outside the CNS, neuroserpin regulates the expression of chemokines by T cells, migration of immune cells, T cell activation, and regulation of immunoinflammatory response [62]. It has been reported that neuroserpin is intricate in the pathogenesis of atherosclerosis and vascular inflammation [64, 65]. Remarkably, neuroserpin has potent anti-inflammatory effects through modulation of T cell activation and invasion during vascular inflammation and formation of atherosclerotic plaques [64, 65]. A cross-sectional study revealed that neuroserpin level was higher in patients with rheumatoid arthritis and correlated with disease severity [65]. Therefore, increasing neuroserpin levels during systemic inflammatory disorders could be a compensatory mechanism to mitigate inflammatory reactions through modulation of T cell response [64]. Loef et al. [66] observed that neuroserpin had an anti-inflammatory effect by inhibiting T cell proliferation and clustering. This effect is mediated by inhibiting the expression of tPA and plasmin-mediated release of annexin-A and F-actin, which are involved in T cell proliferation [66].
These observations illustrated that peripheral neuroserpin has systemic anti-inflammatory effects and regulates immunoinflammatory response.
In the CNS, neuroserpin expression is increased progressively at the perinatal period. It is sustained in adulthood in all brain regions, mainly the hippocampus, neocortex, olfactory bulb, and amygdala, which engage with memory and learning [67]. Neuroserpin plays a crucial role in the development and maturation of CNS, though its function in the mature brain is linked with synaptogenesis and synaptic plasticity [67]. An experimental study demonstrated that neuroserpin-knockout mice experience cognitive dysfunction due to impairment of synaptic function and hippocampal dysfunction [68].
Markedly, neuroserpin polymorphism and dysfunction trigger its intracellular accumulation with the development of wide-spectrum diseases like familial encephalopathy with neuroserpin inclusion body (FENIB) [69]. Alterations in the expression and activity of neuroserpins are associated with the development of different neuropathological disorders. For example, neuroserpin deficiency increases neuronal injury and infarct size in mice with experimental ischemic stroke [70]. It has been shown that administration of neuroserpin in the experimental animal with an ischemic stroke leads to a neuroprotective effect, as evidenced by the reduction of cerebral infarct size [71]. Indeed, higher neuroserpin expression correlates with better clinical outcomes in patients with ischemic stroke [72]. Besides, neuroserpin has a neuroprotective effect against NMDA-induced neurotoxicity [73]. Likewise, neuroinflammatory response and reaction are reversed by neuroserpin, which maintains BBB integrity [74]. The neuroprotective role of neuroserpin is related to the inhibition of tPA-induced neuroinflammation, microglial activation, and BBB injury [72]. Moreover, neuroserpin is implicated in the pathogenesis of bipolar disorders. A case–control study illustrated that neuroserpin plasma levels were lower in patients with bipolar disorders compared to healthy controls [75].
Genetic variations of neuroserpin expression are linked with the development of various neurological disorders, including FENIB, myoclonic epilepsy, AD, cancer, and glaucoma (Fig. 5) [69].
Neuroserpin plays a critical role in the pathogenesis of AD; it regulates the expression and accumulation of Aβ [76]. Neuroserpin forms a binary complex with Aβ1-42, which inactivates neuroserpin as an inhibitor of tPA and blocks the polymerization process [77]. However, neuroserpin has a role in accelerating the accumulation of Aβ, which is dissimilar from that of mature amyloid fibril. In vitro studies demonstrated that neuroserpin attenuates Aβ-induced neurotoxicity [77]. Therefore, the interaction between neuroserpin and Aβ1-42 induces the formation of the non-toxic oligomer to protect the neurons in AD. An experimental study conducted by Fabbro et al. [78] illustrated that neuroserpin-deficient mice have a higher reduction in the accumulation of Aβ1-42, suggesting a possible role of neuroserpin in the aggregation of Aβ and the development of AD. Higher expression of neuroserpin inhibits the neuroprotective tPA and generation of plasmin with the reduction in the clearance of Aβ (Fig. 6) [78]. Ablation of neuroserpin in mice improves clearance of Aβ and reduces Aβ accumulation through activation of tPA [78]. Mutation and conformational changes in neuroserpin are associated with the onset and severity of dementia in patients with neurodegenerative diseases [79].
Role of neuroserpin in the pathogenesis of Alzheimer’s disease: Neuroserpin forms a binary complex with amyloid beta (Aβ)1–42, which inactivates neuroserpin as an inhibitor of tissue plasminogen activators (tPA) that protect the neurons in AD. Increasing neuroserpin levels is linked with the reduction of brain-derived neurotrophic factor (BDNF) in the late stage of AD due to the inhibition of plasmin
Moreover, it has been suggested that Aβ acts as an enhancer for the polymerization of neuroserpin [80]. Increasing neuroserpin level is also associated with neuronal toxicity and uncontrolled excitation [81]. These observations raise conflicting evidence of whether neuroserpin is neuroprotective or involved in AD progression. Previous studies implicate neuroserpin’s role in AD pathogenesis [82]. A case–control study demonstrated that neuroserpin level in CSF was higher in AD patients compared to controls [82]. Thus, CSF neuroserpin level could be a diagnostic biomarker for AD. CSF neuroserpin level is also correlated with tau protein phosphorylation biomarkers in the CSF [82].
Similarly, CSF neuroserpin and plasminogen levels are increased in patients with AD and mild cognitive impairment but without significant differences [83]. Notably, the expression of neuroserpin is reduced in the advanced stage of AD after extensive neuronal loss. Distribution of inhibitors and activators of tPA were assessed in brain tissues from 20 AD patients, and 20 healthy controls showed that neuroserpin expression was reduced, while PAI-1 was increased in temporal and frontal cortices [84]. Higher expression of neuroserpin is associated with a significant reduction of tPA activity with subsequent Aβ accumulation [78, 84]. It has been observed that tPA/plasmin activity was decreased in AD patients compared to controls [78, 84].
Moreover, dysregulation of autophagy and the development of endoplasmic reticulum stress are associated with the accumulation of misfolded proteins, which affect neuroserpin activity in AD [85, 86]. Remarkably, thyroid hormone induces the expression of neuroserpin in AD [85]. Analysis of brain tissues of AD patients in a postmortem study revealed that the expression of thyroid hormone receptors was higher than controls [87]. Bavarsad et al. [87] suggested that thyroid disorders, either hyperthyroidism or hypothyroidism, may be involved in the pathogenesis of AD as thyroid hormones affect memory and cognitive functions [88, 89]. A prospective cross-sectional study of 69 patients showed that thyroid-stimulating hormone levels and thyroid hormones correlated with cerebral tau burden and cognitive dysfunction [88]. These findings implicate thyroid hormones in the pathogenesis of AD. The underlying cause for the association between thyroid disorders and AD is the upregulation of neuroserpin expression and AD neuropathology. Moreover, increasing neuroserpin levels is linked with the reduction of BDNF in AD due to the inhibition of plasmin, which is involved in the activation conversion of pro-BDNF to BDNF [90].
These observations proposed that increased neuroserpin expression in the initial stage of AD might be protective against aggregation and accumulation of Aβ. However, increased neuroserpin expression in the late stage of AD may increase disease severity by inhibiting tPA/plasmin activity [77].
The link between neuroserpin and tPA/plasmin in AD
The potential link between neuroserpin and tPA/plasmin in AD has been reported in different studies [91]. Neuroserpin, via inhibition of tPA and, to a lesser extent, uPA induces accumulation of Aβ [91]. tPA participates in various physiological processes regardless of plasminogen activation, including synaptic plasticity, neuronal growth, and brain development [92]. However, tPA is also intricate in many neuropathological disorders; it participates in the development of excitotoxicity and associated neuronal injury following ischemic stroke [93,94,95]. The physiological role of neuronal tPA is protective, whereas pathological induction release of tPA is associated with detrimental neurological disorders [91]. Therefore, modulation of neuronal tPA by neuroserpin is essential to find the effect of tPA on synaptic plasticity. Neuroserpin attenuates tPA-induced cell proliferation and migration in vitro and visual cortical plasticity [91]. However, in animal model studies, tPA activity was documented to be unaffected by neuroserpin in mice [96].
Nevertheless, neuroserpin is neuroprotective against tPA-mediated neuronal injury during cerebral ischemic events [22]. Neuroserpin is critical in regulating synaptic connection, neuronal differentiation, synaptogenesis, and brain development, mainly in the hippocampus [22, 97]. However, over-expression of neuroserpin is associated with neuronal maturation dysfunction [98]. Indeed, higher expression of neuroserpin in AD pathogenesis had been documented in a previous study [78], though the underlying cause for the elevation of neuroserpin in AD was not fully elucidated. Up-regulation of neuroserpin during Aβ accumulation could be a compensatory mechanism to reduce Aβ-induced neurotoxicity [80, 97]. Alterations of neuronal cholesterol by the long-term effect of statins may induce neuroserpin aggregation and dysfunction [99]. As well, thyroid disorders, ischemic disorders, and neurodegenerative processes affect the expression of neuroserpin [22, 85, 87]. Thus, neuroserpin over-expression with subsequent reduction of tPA may propagate AD neuropathology.
In this bargain, neuroserpin over-expression and tPA dysfunction are not merely the sole mechanism in AD pathogenesis. Searching for the underlying causes of neuroserpin and tPA dysregulation could open a new window regarding the pathogenesis and management of AD.
Conclusions
AD is the most common type of dementia characterized by intracellular accumulation of phosphorylated tau proteins and deposition of Aβ. A defective neuronal clearance pathway due to the dysfunction of degradation enzymes could be a possible mechanism for the accumulation of Aβ. Plasmin formed from plasminogen by the action of tissue plasminogen activators (tPA) cleaves Aβ. tPA is highly expressed in brain areas with high plaque deposition that is reduced in AD. tPA is inhibited by serine proteases, including neuroserpin. Neuronal tPA enhances the conversion of plasminogen to plasmin; this function is controlled by inhibitors neuroserpin. Plasmin activity is reduced in AD patients and is correlated with higher expression of ApoE, which is essential for the pathogenesis of AD. The underlying cause for the reduction of tPA is due to the co-localization of tPA with Aβ, which impairs tPA activity. PAI-1 activity is increased in AD due to an increase in Aβ level, which is correlated with the over-production of PAI-1. Reducing plasmin and tPA activities promote Aβ by reducing Aβ clearance. Thus, there is a positive feedback loop between PAI-1 expression and the pathogenesis of AD.
Neuroserpin plays a critical role in the pathogenesis of AD; it acts as an inhibitor of tPA. Higher expression of neuroserpin inhibits the neuroprotective tPA and generation of plasmin with a reduction in the clearance of Aβ. The underlying cause for the elevation of neuroserpin in AD was not fully elucidated and may be a compensatory mechanism to reduce Aβ-induced neurotoxicity. Thus, neuroserpin over-expression with subsequent reduction of tPA may propagate AD neuropathology. In this bargain, neuroserpin over-expression and tPA dysfunction are not merely the sole mechanism in AD pathogenesis. Findings from this review cannot give a conclusion; thus, experimental, preclinical, and prospective studies are recommended in this regard.
Data availability
Not applicable.
References
Alsubaie N, Al-kuraishy HM, Al-Gareeb AI, Alharbi B, De Waard M, Sabatier J-M et al (2022) Statins use in Alzheimer disease: bane or boon from frantic search and narrative review. Brain Sci 12(10):1290
Knopman DS, Amieva H, Petersen RC, Chételat G, Holtzman DM, Hyman BT et al (2021) Alzheimer disease. Nat Rev Dis Primers 7(1):1–21
Martorana A, Sancesario GM, Esposito Z, Nuccetelli M, Sorge R, Formosa A et al (2012) Plasmin system of Alzheimer’s disease patients: CSF analysis. J Neural Transm 119(7):763–769
Yiannopoulou KG, Papageorgiou SG (2020) Current and future treatments in Alzheimer disease: an update. J Central Nerv Syst Dis 12:1179573520907397
Wong W (2020) Economic burden of Alzheimer disease and managed care considerations. Am J Manag Care 26(8 Suppl):S177–S183
Van Acker ZP, Bretou M, Annaert W (2019) Endo-lysosomal dysregulations and late-onset Alzheimer’s disease: impact of genetic risk factors. Mol Neurodegener 14(1):1–20
Almeida MF, Bahr BA, Kinsey ST (2020) Endosomal-lysosomal dysfunction in metabolic diseases and Alzheimer’s disease. Int Rev Neurobiol 154:303–324
Nalivaeva NN, Turner AJ (2019) Targeting amyloid clearance in Alzheimer’s disease as a therapeutic strategy. Br J Pharmacol 176(18):3447–3463
Yuksel M, Tacal O (2019) Trafficking and proteolytic processing of amyloid precursor protein and secretases in Alzheimer’s disease development: An up-to-date review. Eur J Pharmacol 856:172415
Stevenson TK, Moore SJ, Murphy GG, Lawrence DA (2021) Tissue plasminogen activator in central nervous system physiology and pathology: from synaptic plasticity to Alzheimer’s disease. Thieme Medical Publishers, Inc., New York
Angelucci F, Čechová K, Průša R, Hort J (2019) Amyloid beta soluble forms and plasminogen activation system in Alzheimer’s disease: consequences on extracellular maturation of brain-derived neurotrophic factor and therapeutic implications. CNS Neurosci Ther 25(3):303–313
Janson CG (2015) Convergence of stroke and Alzheimer’s neurovascular research. Sci Transl Med 7(289):289
ElAli A, Bordeleau M, Thériault P, Filali M, Lampron A, Rivest S (2016) Tissue-plasminogen activator attenuates Alzheimer’s disease-related pathology development in APPswe/PS1 mice. Neuropsychopharmacology 41(5):1297–1307
Abubakar MB, Sanusi KO, Ugusman A, Mohamed W, Kamal H, Ibrahim NH et al (2022) Alzheimer’s disease: An update and insights into pathophysiology. Front Aging Neurosci 14:742408
Advani D, Kumar P. Computational Analysis of Natural Compounds as Cyclin-Dependent Kinase-5 Inhibitors for Alzheimer's and Parkinson's Disease. 2022 IEEE Global Conference on Computing, Power and Communication Technologies (GlobConPT); 2022: IEEE; 2022. p. 1–6.
Alvarez A, Munoz JP, Maccioni RB (2001) A cdk5–p35 stable complex is involved in the β-amyloid-induced deregulation of cdk5 activity in hippocampal neurons. Exp Cell Res 264(2):266–274
Alvarez A, Toro R, Cáceres A, Maccioni RB (1999) Inhibition of tau phosphorylating protein kinase cdk5 prevents β-amyloid-induced neuronal death. FEBS Lett 459(3):421–426
Morrow GB, Mutch NJ. Past, present, and future perspectives of plasminogen activator inhibitor 1 (PAI-1). Semin Thromb Hemost; 2022: Thieme Medical Publishers, Inc. 333 Seventh Avenue, 18th Floor, New York; 2022. p. 305–13.
Yepes M (2021) The plasminogen activating system in the pathogenesis of Alzheimer’s disease. Neural Regen Res 16(10):1973
Jacobsen JS, Comery TA, Martone RL, Elokdah H, Crandall DL, Oganesian A et al (2008) Enhanced clearance of Aβ in brain by sustaining the plasmin proteolysis cascade. Proc Natl Acad Sci 105(25):8754–8759
Ledesma MD, Abad-Rodriguez J, Galvan C, Biondi E, Navarro P, Delacourte A et al (2003) Raft disorganization leads to reduced plasmin activity in Alzheimer’s disease brains. EMBO Rep 4(12):1190–1196
Angelucci F, Spalletta G, Iulio Fd, Ciaramella A, Salani F, Varsi A et al (2010) Alzheimer’s disease (AD) and Mild Cognitive Impairment (MCI) patients are characterized by increased BDNF serum levels. Curr Alzheimer Res 7(1):15–20
Herz J, Beffert U (2000) Apolipoprotein E receptors: linking brain development and Alzheimer’s disease. Nat Rev Neurosci 1(1):51–58
Ledesma MD, Da Silva JS, Crassaerts K, Delacourte A, De Strooper B, Dotti CG (2000) Brain plasmin enhances APP α-cleavage and Aβ degradation and is reduced in Alzheimer’s disease brains. EMBO Rep 1(6):530–535
Barker R, Love S, Kehoe PG (2010) Plasminogen and plasmin in Alzheimer’s disease. Brain Res 1355:7–15
Dotti CG, Galvan C, Ledesma MD (2004) Plasmin deficiency in Alzheimer’s disease brains: causal or casual? Neurodegener Dis 1(4–5):205–212
Mohammad Nijres B, Huntington JH, Baliulis G, Vettukattil JJ (2019) Intracoronary recombinant tissue plasminogen activator in an infant with hypoplastic left heart syndrome and complete left main coronary artery thrombosis. Catheter Cardiovasc Interv 93(7):E381–E384
Al-Thomali AW, Al-kuraishy HM, Al-Gareeb AI et al (2022) Role of Neuropilin 1 in COVID-19 Patients with Acute Ischemic Stroke. Biomedicines 10(8):2032
Rabieian R, Boshtam M, Zareei M, Kouhpayeh S, Masoudifar A, Mirzaei H (2018) Plasminogen activator inhibitor type-1 as a regulator of fibrosis. J Cell Biochem 119(1):17–27
Cai Y, Yang E, Yao X, Zhang X, Wang Q, Wang Y et al (2021) FUNDC1-dependent mitophagy induced by tPA protects neurons against cerebral ischemia-reperfusion injury. Redox Biol 38:101792
Yepes M (2019) The plasminogen activation system promotes neurorepair in the ischemic brain. Curr Drug Targets 20(9):953–959
Medina MG, Ledesma MD, Domínguez JE, Medina M, Zafra D, Alameda F et al (2005) Tissue plasminogen activator mediates amyloid-induced neurotoxicity via Erk1/2 activation. EMBO J 24(9):1706–1716
Oh SB, Suh N, Kim I, Lee J-Y (2015) Impacts of aging and amyloid-β deposition on plasminogen activators and plasminogen activator inhibitor-1 in the Tg2576 mouse model of Alzheimer׳ s disease. Brain Res 1597:159–167
Wang J, Yuan Y, Cai R, Huang R, Tian S, Lin H et al (2018) Association between plasma levels of PAI-1, tPA/PAI-1 molar ratio, and mild cognitive impairment in Chinese patients with type 2 diabetes mellitus. J Alzheimers Dis 63(2):835–845
Oh J, Lee H-J, Song J-H, Park SI, Kim H (2014) Plasminogen activator inhibitor-1 as an early potential diagnostic marker for Alzheimer’s disease. Exp Gerontol 60:87–91
Melchor JP, Pawlak R, Strickland S (2003) The tissue plasminogen activator-plasminogen proteolytic cascade accelerates amyloid-β (Aβ) degradation and inhibits Aβ-induced neurodegeneration. J Neurosci 23(26):8867–8871
Oh SB, Byun CJ, Yun J-H, Jo D-G, Carmeliet P, Koh J-Y et al (2014) Tissue plasminogen activator arrests Alzheimer’s disease pathogenesis. Neurobiol Aging 35(3):511–519
Siedlecki-Wullich D, Català-Solsona J, Fábregas C, Hernández I, Clarimon J, Lleó A et al (2019) Altered microRNAs related to synaptic function as potential plasma biomarkers for Alzheimer’s disease. Alzheimers Res Ther 11:1–11
Tian C, Stewart T, Hong Z, Guo Z, Aro P, Soltys D, et al. (2022) Blood extracellular vesicles carrying synaptic function‐and brain‐related proteins as potential biomarkers for Alzheimer's disease. Alzheimer's & Dementia.
Ranasinghe KG, Verma P, Cai C, Xie X, Kudo K, Gao X et al (2022) Altered excitatory and inhibitory neuronal subpopulation parameters are distinctly associated with tau and amyloid in Alzheimer’s disease. Life 11:e77850
Gregnani MF, Hungaro TG, Martins-Silva L, Bader M, Araujo RC (2020) Bradykinin B2 receptor signaling increases glucose uptake and oxidation: evidence and open questions. Front Pharmacol 11:1162
Padmanabhan P, Kneynsberg A, Götz J (2021) Super-resolution microscopy: a closer look at synaptic dysfunction in Alzheimer disease. Nat Rev Neurosci 22(12):723–740
Sciaccaluga M, Megaro A, Bellomo G, Ruffolo G, Romoli M, Palma E et al (2021) An unbalanced synaptic transmission: cause or consequence of the amyloid oligomers neurotoxicity? Int J Mol Sci 22(11):5991
Selkoe DJ, Hardy J (2016) The amyloid hypothesis of Alzheimer’s disease at 25 years. EMBO Mol Med 8(6):595–608
Lozupone M, Panza F (2024) Impact of apolipoprotein E isoforms on sporadic Alzheimer’s disease: Beyond the role of amyloid beta. Neural Regen Res 19(1):80–83
Panza F, Solfrizzi V, Imbimbo BP, Logroscino G (2014) Amyloid-directed monoclonal antibodies for the treatment of Alzheimer’s disease: the point of no return? Expert Opin Biol Ther 14(10):1465–1476
Mukhopadhyay S, Banerjee D (2021) A primer on the evolution of aducanumab: the first antibody approved for treatment of Alzheimer’s disease. J Alzheimers Dis 83(4):1537–1552
Camuso S, Canterini S (2023) Brain-derived neurotrophic factor in main neurodegenerative diseases. Neural Regen Res 18(3):554
Sánchez-García S, Moreno-Tamayo K, Ramírez-Aldana R, García-Peña C, Medina-Campos RH et al (2023) Insomnia Impairs Both the Pro-BDNF and the BDNF levels similarly to older adults with cognitive decline: an exploratory study. Int J Mol Sci 24(8):7387
Gao J, Li L (2023) Enhancement of neural regeneration as a therapeutic strategy for Alzheimer’s disease. Exp Ther Med 26(3):1–14
Pavon MV, Navakkode S, Wong L-W, Sajikumar S (2023) Inhibition of Nogo-A rescues synaptic plasticity and associativity in APP/PS1 animal model of Alzheimer’s disease. Semin Cell Dev Biol 2023:111–120
Sahlgren Bendtsen KM, Hall VJ (2023) The breakthroughs and caveats of using human pluripotent stem cells in modeling Alzheimer’s disease. Cells 12(3):420
Gerenu G, Martisova E, Ferrero H, Carracedo M, Rantamäki T, Ramirez MJ et al (1863) (2017) Modulation of BDNF cleavage by plasminogen-activator inhibitor-1 contributes to Alzheimer’s neuropathology and cognitive deficits. Biochem Biophys Acta 4:991–1001
Gao L, Zhang Y, Sterling K, Song W (2022) Brain-derived neurotrophic factor in Alzheimer’s disease and its pharmaceutical potential. Transl Neurodegen 11(1):1–34
Coleman M, Durrant CS, Ruscher K, Sheppard O, Özen I (2020) Beta secretase 1-dependent amyloid precursor protein processing promotes excessive vascular sprouting through NOTCH3 signaling.
Park L, Zhou J, Koizumi K, Wang G, Anfray A, Ahn SJ et al (2020) tPA deficiency underlies neurovascular coupling dysfunction by amyloid-β. J Neurosci 40(42):8160–8173
Yang X, Zhang Y, Luo J-x, Zhu T, Ran Z, Mu B-R et al (2023) Targeting mitophagy for neurological disorders treatment: advances in drugs and non-drug approaches. Naunyn-Schmiedeberg’s Arch Pharmacol. 90:1–26
Liu R-M, Van Groen T, Katre A, Cao D, Kadisha I, Ballinger C et al (2011) Knockout of plasminogen activator inhibitor 1 gene reduces amyloid beta peptide burden in a mouse model of Alzheimer’s disease. Neurobiol Aging 32(6):1079–1089
Barrett CD, Moore HB, Kong Y-W, Chapman MP, Sriram G, Lim D et al (2019) Tranexamic acid mediates pro-inflammatory and anti-inflammatory signaling via complement C5a regulation in a plasminogen activator–dependent manner. J Trauma Acute Care Surg 86(1):101–107
Kang S, Tanaka T, Inoue H, Ono C, Hashimoto S, Kioi Y et al (2020) IL-6 trans-signaling induces plasminogen activator inhibitor-1 from vascular endothelial cells in cytokine release syndrome. Proc Natl Acad Sci 117(36):22351–22356
Holmes C (2013) Systemic inflammation and Alzheimer’s disease. Neuropathol Appl Neurobiol 39(1):51–68
D’Acunto E, Fra A, Visentin C, Manno M, Ricagno S, Galliciotti G et al (2021) Neuroserpin: structure, function, physiology and pathology. Cell Mol Life Sci 78(19–20):6409–6430
Lorenz N, Loef EJ, Verdon DJ, Chen C-JJ, Mansell CJ, Angel CE et al (2015) Human T cell activation induces synaptic translocation and alters expression of the serine protease inhibitor neuroserpin and its target protease. J Leucocyte Biol 97(4):699–710
Munuswamy-Ramanujam G, Dai E, Liu L, Shnabel M, Sun YM, Bartee M et al (2010) Neuroserpin, a thrombolytic serine protease inhibitor (serpin), blocks transplant vasculopathy with associated modification of T-helper cell subsets. Thromb Haemost 103(03):545–555
Tamer SA, Gürol G, Tekeoğlu İ, Harman H, Çiftçi İH (2016) A new explanation of inflammation in rheumatoid arthritis patients with respect to claudin-5, matrix metalloproteinase-9, and neuroserpin. Arch Rheumatol 31(4):299
Loef EJ, Brooks AE, Lorenz N, Birch NP, Dunbar PR (2020) Neuroserpin regulates human T cell-T cell interactions and proliferation through inhibition of tissue plasminogen activator. J Leukoc Biol 107(1):145–158
Adorjan I, Tyler T, Bhaduri A, Demharter S, Finszter CK, Bako M et al (2019) Neuroserpin expression during human brain development and in adult brain revealed by immunohistochemistry and single cell RNA sequencing. J Anat 235(3):543–554
Reumann R, Vierk R, Zhou L, Gries F, Kraus V, Mienert J et al (2017) The serine protease inhibitor neuroserpin is required for normal synaptic plasticity and regulates learning and social behavior. Learn Memory 24(12):650–659
Godinez A, Rajput R, Chitranshi N, Gupta V, Basavarajappa D, Sharma S et al (2022) Neuroserpin, a crucial regulator for axogenesis, synaptic modelling and cell–cell interactions in the pathophysiology of neurological disease. Cell Mol Life Sci 79(3):172
Gelderblom M, Neumann M, Ludewig P, Bernreuther C, Krasemann S, Arunachalam P et al (2013) Deficiency in serine protease inhibitor neuroserpin exacerbates ischemic brain injury by increased postischemic inflammation. PLoS ONE 8(5):e63118
Zhang Z, Zhang L, Yepes M, Jiang Q, Li Q, Arniego P et al (2002) Adjuvant treatment with neuroserpin increases the therapeutic window for tissue-type plasminogen activator administration in a rat model of embolic stroke. Circulation 106(6):740–745
Rodríguez-González R, Millán M, Sobrino T, Miranda E, Brea D, De La Ossa NP et al (2011) The natural tissue plasminogen activator inhibitor neuroserpin and acute ischaemic stroke outcome. Thromb Haemost 105(03):421–429
Lebeurrier N, Liot G, Lopez-Atalaya JP, Orset C, Fernandez-Monreal M, Sonderegger P et al (2005) The brain-specific tissue-type plasminogen activator inhibitor, neuroserpin, protects neurons against excitotoxicity both in vitro and in vivo. Mol Cell Neurosci 30(4):552–558
Ding S, Chen Q, Chen H, Luo B, Li C, Wang L et al (2021) The neuroprotective role of neuroserpin in ischemic and hemorrhagic stroke. Curr Neuropharmacol 19(8):1367
Çinar RK (2020) Neuroserpin in bipolar disorder. Curr Top Med Chem 20(7):518–523
Sharma A, Muresanu DF, Tian ZR, Nozari A, Lafuente JV, Buzoianu AD et al (2023) Check for updates. Progr Nanomed Neurol Dis 32:195
Kinghorn KJ, Crowther DC, Sharp LK, Nerelius C, Davis RL, Chang HT et al (2006) Neuroserpin binds Aβ and is a neuroprotective component of amyloid plaques in Alzheimer disease. J Biol Chem 281(39):29268–29277
Fabbro S, Schaller K, Seeds NW (2011) Amyloid-beta levels are significantly reduced and spatial memory defects are rescued in a novel neuroserpin-deficient Alzheimer’s disease transgenic mouse model. J Neurochem 118(5):928–938
Davis RL, Shrimpton AE, Carrell RW, Lomas DA, Gerhard L, Baumann B et al (2002) Association between conformational mutations in neuroserpin and onset and severity of dementia. The Lancet 359(9325):2242–2247
Chiou A, Hägglöf P, Orte A, Chen AY, Dunne PD, Belorgey D et al (2009) Probing neuroserpin polymerization and interaction with amyloid-β peptides using single molecule fluorescence. Biophys J 97(8):2306–2315
Lee TW, Tsang VW, Loef EJ, Birch NP. Physiological and pathological functions of neuroserpin: regulation of cellular responses through multiple mechanisms. Semin Cell Dev Biol; 2017: Elsevier; 2017. p. 152–9.
Nielsen HM, Minthon L, Londos E, Blennow K, Miranda E, Perez J et al (2007) Plasma and CSF serpins in Alzheimer disease and dementia with Lewy bodies. Neurology 69(16):1569–1579
Hanzel CE, Iulita MF, Eyjolfsdottir H, Hjorth E, Schultzberg M, Eriksdotter M et al (2014) Analysis of matrix metallo-proteases and the plasminogen system in mild cognitive impairment and Alzheimer’s disease cerebrospinal fluid. J Alzheimers Dis 40(3):667–678
Barker R, Kehoe PG, Love S (2012) Activators and inhibitors of the plasminogen system in Alzheimer’s disease. J Cell Mol Med 16(4):865–876
Subhadra B, Schaller K, Seeds NW (2013) Neuroserpin up-regulation in the Alzheimer’s disease brain is associated with elevated thyroid hormone receptor-β1 and HuD expression. Neurochem Int 63(5):476–481
Di Meco A, Curtis ME, Lauretti E, Praticò D (2020) Autophagy dysfunction in Alzheimer’s disease: mechanistic insights and new therapeutic opportunities. Biol Psychiatry 87(9):797–807
Bavarsad K, Hosseini M, Hadjzadeh MAR, Sahebkar A (2019) The effects of thyroid hormones on memory impairment and Alzheimer’s disease. J Cell Physiol 234(9):14633–14640
Choi BW, Kim S, Kang S, Won KS, Yi H-A, Kim HW (2020) Relationship between thyroid hormone levels and the pathology of Alzheimer’s disease in euthyroid subjects. Thyroid 30(11):1547–1555
AlAnazi FH, Al-kuraishy HM, Alexiou A, Papadakis M, Ashour MHM, Alnaaim SA, et al. (2023) Primary Hypothyroidism and Alzheimer's Disease: A Tale of Two. Cell Mol Neurobiol 2023/08/04.
Iulita MF, Millón MBB, Pentz R, Aguilar LF, Do Carmo S, Allard S et al (2017) Differential deregulation of NGF and BDNF neurotrophins in a transgenic rat model of Alzheimer’s disease. Neurobiol Dis 108:307–323
Nagahara AH, Merrill DA, Coppola G, Tsukada S, Schroeder BE, Shaked GM et al (2009) Neuroprotective effects of brain-derived neurotrophic factor in rodent and primate models of Alzheimer’s disease. Nat Med 15(3):331–337
Pang PT, Teng HK, Zaitsev E, Woo NT, Sakata K, Zhen S et al (2004) Cleavage of proBDNF by tPA/plasmin is essential for long-term hippocampal plasticity. Science 306(5695):487–491
Faysel MA, Singer J, Cummings C, Stefanov DG, Levine SR (2019) Disparities in the use of intravenous t-PA among ischemic stroke patients: population-based recent temporal trends. J Stroke Cerebrovasc Dis 28(5):1243–1251
AlRuwaili R, Al-kuraishy HM, Alruwaili M, Khalifa AK, Alexiou A, Papadakis M, et al. (2023) The potential therapeutic effect of phosphodiesterase 5 inhibitors in the acute ischemic stroke (AIS). Mol Cell Biochem 2023/07/03.
Al-Kuraishy HM, Hussien NR, Al-Naimi MS, Al-Gareeb AI, Lugnier C (2021) Statins therapy improves acute ischemic stroke in patients with cardio-metabolic disorders measured by lipoprotein-associated phospholipase A2 (Lp-PLA2): New focal point. Neurol India 69(6):1637
Zuccato C, Cattaneo E (2009) Brain-derived neurotrophic factor in neurodegenerative diseases. Nat Rev Neurol 5(6):311–322
Li W, Asakawa T, Han S, Xiao B, Namba H, Lu C et al (2017) Neuroprotective effect of neuroserpin in non-tPA-induced intracerebral hemorrhage mouse models. BMC Neurol 17:1–9
Huang Y, Mucke L (2012) Alzheimer mechanisms and therapeutic strategies. Cell 148(6):1204–1222
Giampietro C, Lionetti MC, Costantini G, Mutti F, Zapperi S, La Porta CA (2017) Cholesterol impairment contributes to neuroserpin aggregation. Sci Rep 7(1):43669
Acknowledgements
Not applicable.
Funding
Open Access funding enabled and organized by Projekt DEAL. Open Access funding enabled and organized by Projekt DEAL. This work was supported by the University of Witten-Herdecke Germany.
Author information
Authors and Affiliations
Contributions
NHA, HMA-K and AIA conceptualized the manuscript, wrote, edited and reviewed the main text and approved the final edition of the manuscript. SAA, AA, MP, HMS and GE-SB prepared the figures, wrote, corrected, amended and approved the final edition of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interests
The authors declare no conflict of interest.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ali, N.H., Al-kuraishy, H.M., Al-Gareeb, A.I. et al. The probable role of tissue plasminogen activator/neuroserpin axis in Alzheimer’s disease: a new perspective. Acta Neurol Belg 124, 377–388 (2024). https://doi.org/10.1007/s13760-023-02403-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13760-023-02403-x