Abstract
Purpose of Review
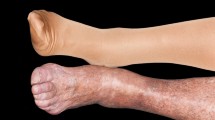
Stasis dermatitis is an inflammatory dermatosis of the lower extremities that most commonly occurs in elderly patients with underlying chronic venous insufficiency. In this article, we review the pathogenesis, clinical presentation, diagnostic approach, differential diagnosis, and management strategies of stasis dermatitis.
Recent Findings
Stasis dermatitis can be confused with a variety of cutaneous disorders, including cellulitis, allergic contact dermatitis, pigmented purpuric dermatoses, and lymphedema; therefore, dermatology consultation of patients with lower extremity rash can help improve outcomes and decrease costs. Treatment of stasis dermatitis focuses on correction of the underlying venous insufficiency with compression or minimally invasive venous procedures and management of symptoms and skin changes with emollients and topical steroids.
Summary
Stasis dermatitis is an important disease with which clinicians should be familiar. Prompt recognition and treatment of stasis dermatitis can be important in the prevention of complications, such as venous ulcerations.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Stasis dermatitis | American Academy of Dermatology [Internet]. [cited 2018 May 15]. Available from: https://www.aad.org/public/diseases/eczema/stasis-dermatitis.
Chadachan V, Dean SM, Eberhardt RT. Cutaneous changes in peripheral arterial vascular disease. In: Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, Wolff K, editors. Fitzpatrick’s dermatology in general medicine [Internet]. 8th ed. New York: The McGraw-Hill Companies; 2012. [cited 2018 May 15]. Available from: accessmedicine.mhmedical.com/content.aspx?aid=56080898.
• Sundaresan S, Migden MR, Silapunt S. Stasis dermatitis: pathophysiology, evaluation, and management. Am J Clin Dermatol. 2017;18(3):383–90. This review article provided a great overview of stasis dermatitis and touched upon the prevalence and economic impact, pathogenesis, clinical features, and management options.
McGuckin M, Waterman R, Brooks J, Cherry G, Porten L, Hurley S, et al. Validation of venous leg ulcer guidelines in the United States and United Kingdom. Am J Surg. 2002;183(2):132–7.
Bergan JJ, Schmid-Schönbein GW, Smith PDC, Nicolaides AN, Boisseau MR, Eklof B. Chronic venous disease. N Engl J Med. 2006;355(5):488–98.
Herouy Y, Mellios P, Bandemir E, Dichmann S, Nockowski P, Schöpf E, et al. Inflammation in stasis dermatitis upregulates MMP-1, MMP-2 and MMP-13 expression. J Dermatol Sci. 2001;25(3):198–205.
Wenk J, Foitzik A, Achterberg V, Sabiwalsky A, Dissemond J, Meewes C, et al. Selective pick-up of increased iron by deferoxamine-coupled cellulose abrogates the iron-driven induction of matrix-degrading metalloproteinase 1 and lipid peroxidation in human dermal fibroblasts in vitro: a new dressing concept. J Invest Dermatol. 2001;116(6):833–9.
Gosnell AL, Nedorost ST. Stasis dermatitis as a complication of amlodipine therapy. J Drugs Dermatol. 2009;8(2):135–7.
Beebe-Dimmer JL, Pfeifer JR, Engle JS, Schottenfeld D. The epidemiology of chronic venous insufficiency and varicose veins. Ann Epidemiol. 2005;15(3):175–84.
Fiebig A, Krusche P, Wolf A, Krawczak M, Timm B, Nikolaus S, et al. Heritability of chronic venous disease. Hum Genet. 2010;127(6):669–74.
Ruckley CV, Evans CJ, Allan PL, Lee AJ, Fowkes FGR. Chronic venous insufficiency: clinical and duplex correlations. The Edinburgh Vein Study of venous disorders in the general population. J Vasc Surg. 2002;36(3):520–5.
Hogan DJ. Widespread dermatitis after topical treatment of chronic leg ulcers and stasis dermatitis. CMAJ Can Med Assoc J. 1988;138(4):336–8.
Hirschmann JV, Raugi GJ. Lower limb cellulitis and its mimics: part II. Conditions that simulate lower limb cellulitis. J Am Acad Dermatol. 2012;67(2):177.e1–9. quiz 185–6
Zygmunt JA. Duplex ultrasound for chronic venous insufficiency. J Invasive Cardiol. 2014;26(11):E149–55.
Hepburn M, Dooley DP, Ellis MW. Alternative diagnoses that often mimic cellulitis. Am Fam Physician. 2003;67(12):2471.
Oh C, Pang S, Chlebicki M, Ho Z, Thirumoorthy T. Cellulitis: making the right diagnosis and its management: a Singapore experience. Hong Kong Journal of Dermatology and Venerology. 2012;20(1):13–19.
Keller EC, Tomecki KJ, Chadi AM. Distinguishing cellulitis from its mimics. Cleve Clin J Med. 2012;79(8):547–52.
Strazzula L, Cotliar J, Fox LP, Hughey L, Shinkai K, Gee SN, et al. Inpatient dermatology consultation aids diagnosis of cellulitis among hospitalized patients: a multi-institutional analysis. J Am Acad Dermatol. 2015;73(1):70–5.
• Milani-Nejad N, Zhang M, Kaffenberger BH. Association of dermatology consultations with patient care outcomes in hospitalized patients with inflammatory skin diseases. JAMA Dermatol. 2017;153(6):523–8. This article discussed the importance of early identification and management of lower extremity inflammatory skin diseases which can improve outcomes among hospitalized patients.
Ko LN, Garza-Mayers AC, St John J, Strazzula L, Vedak P, Shah R, et al. Effect of dermatology consultation on outcomes for patients with presumed cellulitis: a randomized clinical trial. JAMA Dermatol. 2018;154(5):529–36.
Contact dermatitis - Symptoms and causes - Mayo Clinic [Internet]. [cited 2018 May 18]. Available from: https://www.mayoclinic.org/diseases-conditions/contact-dermatitis/symptoms-causes/syc-20352742.
Landeck L, Uter W, John SM. Patch test characteristics of patients referred for suspected contact allergy of the feet--retrospective 10-year cross-sectional study of the IVDK data. Contact Dermatitis. 2012;66(5):271–8.
Opie J, Lee A, Frowen K, Fewings J, Nixon R. Foot dermatitis caused by the textile dye Basic Red 46 in acrylic blend socks. Contact Dermatitis. 2003;49(6):297–303.
Bolognia J, Jorizzo J, Schaffer J. Dermatology. 3rd ed; 2012.
Id reaction (autoeczematization): background, pathophysiology, epidemiology. 2018 Mar 23 [cited 2018 May 16]; Available from: https://emedicine.medscape.com/article/1049760-overview#a6.
Plachouri K-M, Florou V, Georgiou S. Therapeutic strategies for pigmented purpuric dermatoses: a systematic literature review. J Dermatol Treat. 2018;0(0):1–5.
• Ratchford EV, Evans NS. Approach to Lower Extremity Edema. Curr Treat Options Cardiovasc Med. 2017;19(3):16. This article provided a great overview of lower extremity edema, which is in the differential diagnosis for stasis dermatitis, helping to differentiate between the two.
Alavi A, Sibbald RG, Phillips TJ, Miller OF, Margolis DJ, Marston W, et al. What’s new: management of venous leg ulcers: approach to venous leg ulcers. J Am Acad Dermatol. 2016;74(4):627–40. quiz 641–2
Neumann HA. Compression therapy with medical elastic stockings for venous diseases. Dermatol Surg. 1998;24(7):765–70.
Carroll C, Hummel S, Leaviss J, Ren S, Stevens JW, Cantrell A, et al. Systematic review, network meta-analysis and exploratory cost-effectiveness model of randomized trials of minimally invasive techniques versus surgery for varicose veins. Br J Surg. 2014;101(9):1040–52.
Aziz Z, Tang WL, Chong NJ, Tho LY. A systematic review of the efficacy and tolerability of hydroxyethylrutosides for improvement of the signs and symptoms of chronic venous insufficiency. J Clin Pharm Ther. 2015;40(2):177–85.
Barrett JM, Allen B, Ockelford A, Goldman MP. Microfoam ultrasound-guided sclerotherapy treatment for varicose veins in a subgroup with diameters at the junction of 10 mm or greater compared with a subgroup of less than 10 mm. Dermatol Surg. 2004;30(11):1386–90.
Almeida JI, Raines JK. Ambulatory phlebectomy in the office. Perspect Vasc Surg Endovasc Ther. 2008;20(4):348–55.
Klassen W. Office management of stasis ulcer and stasis dermatitis. Can Fam Physician. 1983;29:279–83.
Luz BSR, Araujo CS, Atzingen DANCV, Mendonça AR d A, Mesquita Filho M, de Medeiros ML. Evaluating the effectiveness of the customized Unna boot when treating patients with venous ulcers. An Bras Dermatol. 2013;88(1):41–9.
Pittler MH, Ernst E. Horse chestnut seed extract for chronic venous insufficiency. Cochrane Database Syst Rev. 2006;1:CD003230.
Maroo N, Choudhury S, Sen S, Chatterjee S. Oral doxycycline with topical tacrolimus for treatment of stasis dermatitis due to chronic venous insufficiency: a pilot study. Indian J Pharmacol. 2012;44(1):111–3.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Alexandra Rzepecki and Rachel Blasiak declare no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Dermatology and Wound Care
Rights and permissions
About this article
Cite this article
Rzepecki, A.K., Blasiak, R. Stasis Dermatitis: Differentiation from Other Common Causes of Lower Leg Inflammation and Management Strategies. Curr Geri Rep 7, 222–227 (2018). https://doi.org/10.1007/s13670-018-0257-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13670-018-0257-x