Abstract
Alzheimer’s disease (AD) is progressive and ultimately fatal, with current drugs failing to reverse and cure it. This study aimed to find plant species which may provide therapeutic bioactivities targeted to causal agents proposed to be driving AD. A novel toolkit methodology was employed, whereby clinical symptoms were translated into categories recognized in ethnomedicine. These categories were applied to find plant species with therapeutic effects, mined from ethnomedical surveys. Survey locations were mapped to assess how this data is at risk. Bioactivities were found of therapeutic relevance to 15 hypothesised causal bases for AD. 107 species with an ethnological report of memory improvement demonstrated therapeutic activity for all these 15 causal bases. The majority of the surveys were found to reside within biodiversity hotspots (centres of high biodiversity under threat), with loss of traditional knowledge the most common threat. Our findings suggest that the documented plants provide a large resource of AD therapeutic potential. In demonstrating bioactivities targeted to these causal bases, such plants may have the capacity to reduce or reverse AD, with promise as drug leads to target multiple AD hallmarks. However, there is a need to preserve ethnomedical knowledge, and the habitats on which this knowledge depends.
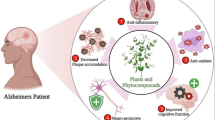
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
The global incidence of Alzheimer’s disease (AD) and other dementias is 43·8 million and rising, and a cause of 2·4 million deaths annually [1]. AD is also recalcitrant against modern pharmacological interventions, with a failure of treatments to reverse and cure disease progression [2,3,4,5,6]. Therapeutic strategies remain limited due to a lack of knowledge of the precise mechanisms underlying the observed pathology [7]. For Alzheimer’s treatment from 2002 to 2012, 413 clinical trials were performed, assessing 221 agents, with none being found to show disease-modifying potential [8]. The US Food and Drug Administration licensed only one AD drug in that duration (memantine), which provides just a minor clinical benefit [9]. Subsequently in 2021 the monoclonal antibody (mAb) Aducanumab was licensed by the U.S. Food and Drug Administration (FDA) for AD treatment, based on demonstrating amyloid reduction, but the drug has limited impact on reducing cognitive decline and disease progression (reviewed by [10, 11]). Trials with other mAbs, vaccines and other agents are still ongoing, with some providing symptomatic relief, but none showing strong evidence of halting the disease (reviewed by [5]).
There is thus a search for more effective drugs, and evidence is mounting that plants may provide such a source. Of the new therapeutic drugs approved by the FDA and similar organizations in several of the years from 1981 to 2019, 50% of all approvals were derived from natural products, including plants [12, 13]. However, it is likely that the bioactivity of most plant species remains to be investigated [14], and this represents a huge untapped resource.
Of the most useful drugs derived from plants, 80% were discovered by follow-up of ethnomedical uses (plants used in traditional medical practices) [15]. Screening indigenous community ethnomedicine data can increase the “hit rate” for discovery of novel active compounds [16]. This is because it is the application of a knowledge-based strategy to detect therapeutic potential. This is in contrast to the screening of natural compounds at random, which has a low hit rate for identification of relevant bioactivity [14]. Moreover, for drugs derived from ethnomedicine, ethnomedical uses can provide insight of efficacy and safety [17], often long-established over many generations.
This study aimed firstly to find and document plant species with reported therapeutic effects of AD relevance. A toolkit methodology was applied, which involved construction of therapeutic categories which could be recognized by ethnomedical practitioners. These categories were then applied to mine ethnological data in search of therapeutic potential of relevance to neurodegenerative diseases (NDs). The rationale for this is to attain a wide set of relevant terms to maximise the mining of therapeutic data. Although some hallmarks and symptoms, such as memory impairment, are easily recognised by both clinicians and ethnomedical practitioners, certain hallmarks such as neurotoxicity, of central importance in numerous NDs, cannot be easily translated into terms in ethnomedical use. Anti-neurotoxic effects in plants may indeed exist, which could be revealed from a wider probing of the many medicinal effects reported. The relevance of the findings to a wider range of ND diseases are reported separately. This study focuses on the relevance of the findings to AD.
A second aim was to map the geographical locations of the mined ethnomedical surveys, to assess how this ethnomedical data may be at risk, since mapping anthropogenic threats is a key tool to guide management of these threats [18]. The world’s greatest biodiversity hotspots (BDH) are centres of high biodiversity that are under threat [19, 20], defined as having lost at least 70% of their primary native vegetation (https://www.cepf.net/our-work/biodiversity-hotspots/hotspots-defined). In most hotspots, it is estimated that less than 10% of natural intact vegetation remains [21]. The survey locations were mapped to establish how many were located in these BDHs and therefore at elevated risk. The surveys were examined systematically to discover what the threats were of most concern to the authors, to inform responses appropriate to how any valuable ethnomedical data of relevant therapeutic potential can be preserved.
The leading factor in AD pathogenesis remains unknown [22]. Numerous hypotheses have been proposed in which the disease is postulated to be initiated or driven by a particular causal agent (reviewed by [23, 24]). We were interested in finding what specific causal agents AD can be attributed to, since these provide a focus to be targeted therapeutically. Our third aim was thus to search the literature for various causal hypotheses for Alzheimer’s disease, for which plant species mined in this study may provide bioactivities of AD therapeutic potential. The implication is that if plants can be found which can target the underlying causes of neurodegeneration driving AD pathogenesis, this could be of fundamental importance in the search for more effective therapies, since to date no drugs halt and remediate disease progression.
2 Results and discussion
2.1 Overview
2001 plant species were identified with reported uses for alleviating pathologies relevant to NDs, by application of the toolkit methodology (Additional files 1: Additional Table S1, 2: Table S2). Bioactivities of therapeutic relevance were discovered from the literature for 1339 of these 2001 species (67%) (Additional file 3: Table S3). Bioactivities were found for every one of the toolkit categories, and also beyond the toolkit categories (i.e., species with an ethnomedical use demonstrating other bioactivities of ND therapeutic potential). This paper focuses on the relevance of the data to AD.
We found that plant bioactivities were found of therapeutic relevance to 15 hypothesised causal bases for AD (Table 1). This plant therapeutic potential for a wide range of causal agents implicated in driving AD pathogenesis is evidence that the toolkit methodology is useful for providing a wide reach in the search of this potential.
2.2 Plant bioactivities of relevance to AD causal hypotheses
The study found reports of plant therapeutic bioactivities potentially relevant to the following hypothesised causal bases and dysregulated processes. In this section the therapeutic effects are documented in more detail.
2.2.1 The amyloid hypothesis
The dominant model of AD pathogenesis is the amyloid hypothesis, in which the accumulation of Aβ is proposed to be causal [25, 26]. In the AD brain, lesions known as neuritic plaques are found, consisting of microscopic foci of amyloid protein deposition [27]. George Glenner identified a distinctive amyloid β (Aβ) peptide found in these deposits [28], and proposed that the Aβ causes destruction of neuronal fibres, which is intrinsic to the ensuing dementia of AD [29]. This pathology has come to be associated with aberrant metabolism of the amyloid precursor protein (APP) [30]. These findings have led to the amyloid cascade hypothesis, in which an imbalance between production and clearance of Aβ peptides initiates the complex pathological cascade of AD [31, 32]. A variant of the cascade view is the amyloid-β oligomer (AβO) hypothesis, which postulates that the brain damage of AD is instigated by toxic soluble amyloid oligomers [33]. Substantial evidence supports these hypotheses: for instance, mutations in APP lead to more aggressive AD; humans with Down’s syndrome have 3 copies of APP and invariably develop AD; patients with an APP mutation that decreases Aβ are associated with reduced AD and cognitive decline; and in animal and cell models Aβ induces tau hyperphosphorylation, reduces synapse density and impairs memory; and blocking AβO production reverses synapse loss and memory impairment in APP mice (reviewed by [25, 34]). Moreover, various Aβ monoclonal antibodies (mAb) such as Aducanumab reduce brain Aβ brain deposits and result in small clinical improvements (reviewed by [35]). Such evidence provides a rationale for the targeting of Aβ in AD disease pathology, but there is a scepticism that mAb treatments reduce cognitive decline, in spite of the Food and Drug Administration in the United States licencing Aducanumab for AD treatment [11, 36]. Clinical effects of mAb also significantly increase the risk of adverse events (https://www.eisai.com/news/2018/news201866.html accessed 25 Oct 2021).
The search thus remains for alternative, more effective treatments to target AD amyloid pathology. Of therapeutic relevance to this, 46 plant species (Table 2) and 42 phytochemicals (Additional file 5: Table S5) have been found to demonstrate anti-amyloid activity in a variety of human cell line, animal in vivo and in vitro studies. Seven of these species (Allium sativum, Bacopa monnieri, Centella asiatica, Cocos nucifera, Convolvulus prostratus, Moringa oleifera and Rosmarinus officinalis all demonstrated both memory/ cognitive improvement and anti-amyloid activities, providing evidence that the anti-amyloid activity may be of therapeutic effect in alleviating AD memory/cognitive dysfunction.
The therapeutic effects result from a variety of mechanisms, which provide potential to target the various amyloid ligands and amyloidogenic processes. For instance, in a randomized, placebo-controlled, double-blind, multicentre 52-week phase 2 trial of resveratrol (Table 3) in individuals with mild to moderate AD, CSF Aβ40 levels significantly declined [37].
In various pre-clinical studies, treatment with Cornus officinalis, Cyperus rotundus, Fragaria x ananassa, Opuntia ficus-indica and Satureja hortensis inhibited Aβ aggregation [43, 45, 48, 49]. Decrease in amyloid plaque deposition resulted from treatment with Centella asiatica [72] and Coptis chinensis [40]. Rosmarinic acid (Table 3) (from sources such as Rosmarinus officinalis) decreased brain deposition of A11-positive Aβ oligomers [64]. Uncaria tomentosa disaggregated preformed Aβ fibrils [65]. Cajanus cajan stimulated amyloid β clearance [76]. Bacopa monnieri inhibited Aβ42 fibrillogenesis [56]. In mouse neurons exposed with metal–associated Aβ, EGCG (Epigallocatechin-3-gallate) (Table 3) increased cell survival [77] (Additional file 5: Table S5).
Molecular mechanisms have also been elucidated. Moringa oleifera decreased amyloid production via β -site APP cleaving enzyme (BACE1) downregulation [53]. Morus alba reduced cerebral Aβ production and Aβ plaque burden via upregulation of amyloid-degrading protease (e.g., NEP, IDE) [54]. Olea europaea blocked formation of toxic Aβ oligomers [63]. Phyllanthus emblica and silymarin (a mixture containing mainly silybin) (Table 3) from Silybum marianum reduced expression of amyloid precursor protein [41, 42]. Vaccinium myrtillus inhibited aggregation of Aβ1–42 via suppression of p44/42 MAPK [75]. Resveratrol remodelled Aβ into non-toxic structures [67]. Similarly, brasilin (Table 3) (from Caesalpinia sappan) remodelled Aβ fibrils into less toxic aggregates [66]. Apium graveolens treatment led to amyloid precursor protein (APP) processing toward a non-amyloidogenic pathway [38].
However, there is a body of evidence that confutes the amyloid cascade hypothesis as the central event in AD pathogenesis (reviewed by [78, 79]). For instance, there are numerous human subjects who were cognitively normal (without clinical expression of AD) despite harbouring brain amyloid plaque deposits [80,81,82]. Moreover, mice genetically engineered to produce brain amyloid deposits do not demonstrate neurodegeneration or cognitive decline [83], suggesting that Aβ does not provide a sufficient cause for the complex symptoms of AD [84] (for counter-arguments to these and other objections, see [25]).
2.2.2 The tau hypothesis
An alternative framework is the tau hypothesis, which states that the principle causative substance of AD is tau, not Aβ (reviewed by [79]). Tau is a protein regulating the function of microtubules, its microtubule binding affinity being determined by its phosphorylation [85]. In AD, tau becomes hyperphosphorylated, aggregating into toxic neurofibrillary tangles (NFTs) within neurons [86, 87]. Moreover, tau may have a pathogenic role in mediating Aβ toxicity in AD [88]. Tau hyperphosphorylation may be induced by various factors, such as impaired glucose metabolism [89]. Evidence for a causative role for tau is suggested by an association between the spreading of pathological tau and the patterns of neurodegeneration, and that tau lesions occur prior to Aβ accumulation (reviewed by [79]).
Of therapeutic relevance, at least 20 plant species or their associated phytochemical extracts have demonstrated anti-tau bioactivity in various pre-clinical models (Table 4), via several mechanisms.
For instance, in pre-clinical models, reduced tau hyperphosphorylation was demonstrated in treatments with either L-3-n-butylphthalide (L-NBP) (Table 3) (from Apium graveolens) [103], EGCG (Table 3) (from Camellia sinensis) [91] or genistein (Table 3) (from Glycine max) [94]. In all these examples, the anti-tau effects were associated with cognitive or memory improvements. Other species, such as Convolvulus prostratus, reduced tau gene expression [39]. Uncaria tomentosa disaggregated tau tangles/filaments [65]. Resveratrol (from species such as Vitis vinifera) reduced tau pathology [101] and myricanol (from Myrica cerifera) enhanced tau clearance [102].
Another possibility is the “dual pathway” model of causality, in which Aβ and tau may be linked to a common upstream driver [104], for which combined Aβ and tau-directed therapies have been proposed [105]. Plant species and derived phytochemicals demonstrating both anti-amyloid and anti-tau activity are attractive candidates for this combination strategy. Such species include Curcuma longa, Fibraurea recisa, Fragaria ananassa, Moringa oleifera, Morus alba, Uncaria tomentosa, and the phytochemicals berberine and resveratrol (Table 3) (Additional file 5: Table S5).
In some of the studies, anti-tau effects were associated with yet other activities of therapeutic relevance. For instance, with resveratrol treatment, reduced aberrant amyloid production and tau pathology were also associated with enhanced proteasome activity [101]. Uncaria tomentosa treatment led not only to anti-amyloid and anti-tau effects but also memory improvement and anti-inflammatory activity [65]. With Moringa oleifera, anti-amyloid and anti-tau effects were associated with rescued cognitive impairment and recovery of decreased synaptic proteins [53].
Molecular mechanisms have also been revealed. For example, mice treated with L-NBP led to reduced tau hyperphosphorylation at Ser199, Thr205, Ser396, and Ser404 sites. Also expressions of cyclin-dependent kinase and glycogen synthase kinase 3β, key kinases involved in tau phosphorylation, were reduced [90].
2.2.3 The ubiquitin–proteasome hypothesis
According to the ubiquitin–proteasome hypothesis, impairment of the ubiquitin–proteasome system, by which damaged proteins are dismantled, is at the root of neurodegenerative diseases such as AD [106]. A protein quality control (PQC) system consists chiefly of molecular chaperones such as heat shock proteins. These survey misfolded proteins, unfolding and refolding them into natively functional forms [107] (reviewed by [108]). Misfolded proteins that are unable to be refolded are degraded through two protein clearance pathways, the ubiquitin–proteasome system (UPS) and the autophagy-lysosome pathway (reviewed by [109]). In the UPS system, ubiquitin protein becomes conjugated to the misfolded protein, enabling the protein’s recognition and degradation within a multimeric enzyme cascade system known as the proteasome [110]. There is evidence for a central role of the UPS in AD pathology. For instance, in the AD brain, ubiquitinated proteins are found to accumulate, proteasome activity is decreased, and there is malfunction in the UPS pathway [111, 112], with a consequent impairment of neurotoxic protein clearance [113].
These systems are of intense interest for developing novel therapeutic interventions for AD [114, 115], and several plant species have demonstrated a role in the targeting of these pathways. Treatment with resveratrol enhanced mouse brain proteasome function, and this was associated with attenuation of aberrant amyloid production and reduced tau pathology [101]. Betulinic acid (Table 3) (from sources such as (Betula pubescens and Ziziphus mauritiana) [116] activated proteasome activity in human cell lines [117]. Sulforaphane (Table 3) (from sources such as Brassica oleracea) [118] mediated degradation of misfolded huntingtin protein in mice and human cell lines through the UPS pathway [119]. Sulforaphane was also found to ameliorate scopolamine-induced memory impairment in a rat model [120]. Mouse cell lines treated with sulforaphane protected cells from Aβ1–42-mediated cell death by upregulation of the 26S proteasome [121]. These evidences taken together suggest that these various phytochemicals have therapeutic potential for targeting proteasome impairment in AD.
2.2.4 Impaired autophagy hypothesis
Another hypothesis is that autophagy dysfunction plays an important role in AD pathophysiology [122]. If the UPS is impaired or cannot recognise the misfolded proteins, the misfolded proteins are destined for autophagy. This is a process of degradation and recycling of cell components within lysosomes [123], orchestrated by a complex network of proteins [124]. Autophagy dysfunction is implicated in AD (reviewed by [125]). Pharmacological agents acting to modulate autophagy are being explored for AD therapy [126, 127], and several plant species demonstrate this potential (Additional file 4: Table S4). For instance, in a clinical trial with resveratrol, the lysosomal/ phagosomal pathway was upregulated, indicating induction of autophagy [128]. Resveratrol also induced autophagy by directly inhibiting the mTOR-ULK1 pathway in an in vitro study [129]. Treatment of mice with the ginsenoside Rg2 (Table 3) (from Panax ginseng) induced autophagy, resulting in enhanced clearance of protein aggregates [69]. Berberine (from sources such as Coptis chinensis, Phellodendron amurense and Hydrastis canadensis) induced autophagy in numerous cell types including neurons, by mechanisms including AMPK/mTOR signaling upregulation [130, 131]. Phenolic acids from Eucommia ulmoides leaves may also activate autophagy via the autophagy regulators (Pink1, Beclin1, Ulk2, and Atg5) [132]. Urolithin A (Table 3) (from Punica granatum) induced autophagic flux in mouse and human neurons, which also contributed to inhibition of neuroinflammation [133].
2.2.5 The inflammation hypothesis
Inflammation is a normal host defence response triggered by damaging agents such as traumatic injury and invading pathogens, and is diminished once the tissue is repaired and resolved [134]. However, these normal mechanisms fail when there is an abnormal activation of inflammatory factors, leading to a chronic neuroinflammatory state, with harmful consequences [135]. The neuroinflammatory process involves the recruitment of numerous cellular and molecular immune components [136]. These include microglia and astrocytes, non-neuronal immune cells collectively known as glia, resident within the CNS. Microglia exhibit a surveillance function, with long processes in dynamic activity to constantly sense their surroundings [137]. This enables them to perform their housekeeping functions such as phagocytic engulfment of damaged tissue and elimination of pathogens [138]. During CNS damage or infection, microglia are activated and recruited to the site of insult, where they secrete small proteins called cytokines which can promote inflammation (pro-inflammatory) (e.g., IL-1, IL-6) or promote anti-inflammatory pathways (e.g., IL-4, IL-10) [134]. The secretion of proinflammatory cytokines can be beneficial, leading to the clearing of cell debris and promotion of regeneration [139]. However, disruption of microglial housekeeping (such as by persistent production of aberrant toxic proteins) leads to an exaggerated proinflammatory response [140]. This causes the microglia to shift to a reactive phenotype, secreting neurotoxins that kill neurons; hence correcting this maladaptive response may be a potential mode for disease-modifying therapy [141].
Astrocytes, comprising 25–50% of the brain volume, have a myriad of roles, such as ion homeostasis, neurotransmitter clearance, energy supply to neurons, synapse formation, remodelling of neural circuits [142], learning and memory [143], and the limiting of inflammation [144]. Astrocyte dysfunction has now been implicated in AD, associated with both loss-of-function and gain of toxicity phenotypes [145]. For instance, cytokine combinations such as TNF-α and IFN-γ stimulate astrocytes to generate Aβ, and since astrocytes outnumber neurons in the brain, astrocytes may be a significant source of Aβ during neuroinflammation in AD [146]. In an in vitro neuron-astrocyte co-culture, inhibition of astrocyte activation with an anti-inflammatory agent reduced the astrocytic inflammatory response and associated neuronal loss [147]. Astrocytes can thus be a therapeutic target for drug discovery [148].
The inflammation hypothesis for AD is based on the adverse effects of a pro-inflammatory brain microenvironment [149, 150], in which neuroinflammation (inflammation within the CNS) has a vital role in driving the pathogenesis and progression of AD [151]. A modification of this is the amyloid cascade—inflammation hypothesis, which envisages AD resulting from the inflammatory response induced by Aβ, later enhanced by aggregates of tau [152].
Supporting evidence for an inflammatory involvement in causality includes a reduced prevalence of AD in patients with rheumatoid arthritis treated with non-steroidal inflammatory drugs (NSAIDs) [153,154,155]; preceding clinical AD onset, an elevation of plasma inflammatory proteins [156] and microglial activation markers [157]; inflammatory markers co-localising with amyloid and tau deposition [158] (reviewed by [159]); and cognitively normal patients with profuse amyloid and tau deposits demonstrating lower levels of inflammation compared with AD patients [160].
Of relevance to the targeting of these neuroinflammatory processes, at least 21 plant species have been found to demonstrate anti-neuroinflammatory activity (Table 5).
For instance, rats treated with Fibraurea recisa showed anti-neuroinflammatory activity and also anti-amyloidogenic and anti-tau effects [74]. In another rat model, Peristrophe bicalyculata treatment led to anti-neuroinflammatory activity and reduced cognitive decline [163].
At least 9 species demonstrated reduced microglial or astrocyte activation (Additional file 4: Table S4), and this was associated with enhanced clearance of Aβ with Vaccinium myrtillus [75] (Table 5). Cajaninstilbene acid (Table 3) (from Cajanus cajan) reduced reactivity of both microglia and astrocytes, as well as stimulating Aβ clearance [76].
Evidence in favour of an anti-inflammatory involvement of AD causality based on therapeutic NSAID effects have been called into question. NSAIDs have failed to delay the onset of AD in adults with a family history of dementia [175]. There is also the possibility that AD does indeed develop less often in rheumatoid arthritis patients, but it is difficult to exclude the possibility that this is unrelated to anti-inflammatory drugs [176].
NSAIDs also increase the frequency of adverse health effects such as cardiotoxicity, upper gastrointestinal bleeding and perforation, notably with cyclooxygenase-2 (COX-2) inhibitors [177]. Medicinal plants demonstrating both COX and Lipoxygenase (LOX) inhibition bioactivity such as Canarium patentinervium may have less adverse effects, since there is evidence that dual COX and LOX inhibition reduces gastric and cardiovascular side effects [178].
Nuclear factor-κB (NF-κB) is a network hub consisting of a family of transcription factors [179, 180]. It serves as a pivotal mediator of inflammatory responses, inducing expression of various pro-inflammatory genes, and sustained NF-κB activation is integral to the persistence of inflammation [181]. Drug discovery units are searching for inhibitors of the NF-κB pathway as a pivotal target for AD pathologies [181, 182], thus medicinal plants demonstrating such activity are of therapeutic potential. For instance, treatment of mouse microglia with Tussilago farfara inhibited NF-κB inhibition and reduced microglial activation [174]. NF-κB inhibition was also demonstrated in a mouse microglia inflammation model treated with sulforophane [183]. However, targeting NF-κB may require cell-type specificity to preclude off-target deleterious effects [184].
2.2.6 The immune hypothesis
According to the immune hypothesis proposed by Fiala and colleagues [185, 186], a dysfunctional immune system may be the main player in the pathogenesis of AD [187]. In this view, a number of dysfunctional immune elements have been implicated. The innate immune response (which subjects are born with) primarily involves immune microglia cells within the brain, as described earlier. In AD, microglia change from a homeostatic state to disease-related pro-inflammatory phenotypes which cause neuronal damage [188]. There is also an adaptive immune system response, involving a proliferation of lymphocytes (types of white blood cells) circulating peripherally in the body outside the brain. T lymphocytes (the T denoting their thymus origin) have a major sub-set, T-helper (TH) cells, which “help” other immune cells, and can also be distinguished by their surface cluster of differentiation (CD) protein expression profile, notably ones expressing CD4, which once activated by antigens become CD4+ T cells. There are numerous CD4+ T cell subsets, such as T helper 1 (TH1), T helper 2 (TH2), T helper 17 (TH17), T helper 22 (TH22) and regulatory T cells (Treg) [189]. A number of research studies have implicated immune dysfunction in AD pathogenesis and clinical progression (reviewed by [190]). For instance, elevated peripheral immune-inflammatory markers are associated with future cognitive decline and phosphorylated tau [191, 192]. Also in AD, T cells invade the CNS when the blood–brain barrier (BBB) is disrupted, and localize in regions associated with AD neuropathology, where they are associated with neurotoxicity and enhanced inflammation (reviewed by [193]).
There is a lack of success with immunotherapy trials for AD to date, perhaps due to recruited patients being affected with the established disease that can no longer be halted [190]. Hence there is a search for novel immunomodulatory treatments which may alter the AD course [187], and a number of plants demonstrate this potential (Additional file 4: Table S4). For instance, in addition to microglial enhanced clearance of Aβ, sodium rutin (Table 3) (derived from sources such as Ruta graveolens) activated microglial phagocytosis of Aβ amyloid via up-regulation of phagocytosis-related receptors [194].
TH17 immune cells produce the cytokine interleukin-17A (IL-17A), and in AD patients there is an association between brain amyloid levels and elevated TH17 cytokine production (reviewed by [195]). IL-17 also inhibits hippocampal neurogenesis [196]. Extracts of Allium sativum inhibited IL-17 gene expression in human blood mononuclear cells [197]. In an autoimmune encephalomyelitis mouse model of multiple sclerosis, carnosol (Table 3) (originally extracted from Rosmarinus officinalis) promoted a microglial switch to an immunomodulatory phenotype and suppressed reactive TH17 cells [198].
In the TH1/TH2 paradigm first proposed by Mosmann and colleagues, TH1 and TH17 cells release pro-inflammatory and TH2 cells anti-inflammatory cytokines respectively [199]. This view has become expanded, in which both TH1 and TH2 cells together orchestrate a variety of adaptive immune responses to maintain a healthy CNS [200], with the TH1/TH2/TH17/Treg cell balance resulting in either a tissue-protective or tissue-destructive immuno-inflammatory response [201]. A dysfunctional TH1/TH2 ratio has been regarded as a causative event in neurodegeneration. Several plants demonstrate a TH1 to TH2 shift. For instance, treatment with Nigella sativa favours a shift to a TH2 cytokine profile in mouse lymphocytes [202], and in human lymphocytes with Sambucus nigra [203].
Prostaglandin E2 (PGE2) is a downstream lipid product of the COX pathway, and a major modulator of inflammation [204]. In aging mice, inhibition of PGE2 in myeloid cells (non-lymphocyte peripheral immune cells e.g., monocytes, macrophages) promoted a more homeostatic anti-inflammatory state and reducing cognitive decline [205]. Since rejuvenating non-brain myeloid cells by reducing PGE2 signaling reverses age-related cognitive decline, this manipulation of the peripheral immune system can have a profound therapeutic effect within the brain [206]. Hence plants with this capacity for PGE2 /E2 reduction could also be of therapeutic potential. For instance, mangosteen (from Garcinia mangostana) inhibited E2 synthesis in rat glioma cells [207]. In mouse microglial cells curcumin (Table 3) (from Curcuma longa) reduced PGE2 and also reduced the inhibitory effect of PGE2 on Aβ42-induced microglial phagocytosis [208].
2.2.7 The oxidative stress hypothesis
According to the Oxidative Stress Hypothesis, free radical-associated oxidation appears to have a fundamental role in driving the pathogenesis of neuron degeneration and death in AD [209,210,211]. Reactive oxygen species (ROS) are oxygen-derived compounds with highly reactive free radicals, such as anion superoxide (O2·–). Reactive nitrogen species (RNS) are free radicals derived from nitrogen (e.g., peroxynitrite) [212]. Harmful effects of ROS/RNS are known as oxidative stress/ nitrosative stress respectively. Supporting evidence of a role for these stresses in AD progression includes a brain region correspondence between AD pathology and oxidative stress markers [213, 214] (reviewed by [215]). For instance, the oxidation marker 8-hydroxy-2’-deoxyguanosine (OH8dG) increases with aging and is further still increased in the AD brain [216]. Subjects with a diet high in fruits and vegetables had higher plasma anti-oxidants, lower oxidative stress biomarkers and better cognitive performance compared with subjects with a low fruit and vegetable consumption [217]. Hence a good anti-oxidant status appears to be protective against cognitive decline [22].
However, anti-oxidant treatments have failed to reduce oxidative damage (the ‘anti-oxidant paradox’) [218], suggesting that oxidative stress is a downstream effect. Another reason for this failure may be that in contrast to anti-oxidant supplements containing a single/ few anti-oxidants, plants contain phytochemicals with a wide range of anti-oxidant properties [219]. Particularly promising are plants with high anti-oxidant capacity associated with other therapeutic effects targeted to AD pathologies in various preclinical models. For instance, in an AD mouse model, treatment with apigenin (Table 3) (from sources such as Elsholtzia rugulosa) inhibited oxidative stress, lowered insoluble Aβ levels and amyloid plaque burden, and rescued learning and memory [51]. In other animal models, reduced oxidative stress was associated with heat shock protein modulation with allicin (from Allium sativum) (Table 3) [220], AChE inhibition with Elettaria cardamomum [221], memory improvement and anti-aging effects with Polygonatum sibiricum [222], anti-atherosclerotic activity with Cynara scolymus [223], reduced apoptotic cell death with Moringa oleifera [224], DNA damage protection with Pilea microphylla [225] and anti-hyperlipidemic effects with Carthamus tinctorius [226].
Oxidative stress and inflammation are interdependent, thus therapeutic agents may be required that target both inflammation and oxidative stress simultaneously [227]. Many plants demonstrate anti-inflammatory and anti-oxidant/reduced ROS activities (Additional file 3: Table S3) in studies associating the two, such as in a human study with Campomanesia speciosa treatment [228].
Nuclear factor erythroid 2-related factor 2 (Nrf2) is a master regulator of anti-oxidative responses, inducing expression of anti-oxidants, anti-inflammatory mediators and cytoprotective genes [229]. Its expression is decreased in AD patients [230]. Administration of Nrf2 activators reverses memory and synaptic impairments in AD rodent models [231], indicating that Nrf2 pathway activation is a therapeutic target for AD. Plants reported to demonstrate increased Nrf2 expression are thus also of potential therapeutic relevance. For instance, in human cell lines, quercetin (found in numerous plants such as Crataegus spp.) upregulated Nrf2 expression and subsequent expression of anti-oxidant enzymes [232]. Similarly, in other human cell line models, Nrf2 was activated with phenethyl isothiocyanate (from Nasturtium officinale) [233] and plumbagin (from Plumbago zeylanica) [234]. These examples suggest that such plants have therapeutic potential in targeting various oxidative stress effects that may be integral to numerous pathologies implicated in AD.
2.2.8 The mitochondrial cascade hypothesis
According to the “mitochondrial cascade hypothesis”, mitochondrial dysfunction triggers Aβ accumulation and AD pathogenesis [235, 236]. Evidence of impaired mitochondrial function is suggested by low brain glucose consumption, decreased oxygen utilization and impaired enzyme gene expression in AD (reviewed by [237]). Moreover, mitochondrial dysfunction precedes Aβ in a senescent AD rat model, suggesting that mitochondrial dysfunction may mediate or even initiate the development of AD pathology [238]. Treatment strategies aimed at boosting mitochondrial and bioenergetic function have shown some benefit in mainly animal models of AD, but clinical trials lag behind the more predominant target strategies such as amyloid [237]. Hence plants reported to enhance mitochondrial functions could provide novel treatment prospects (Table 6; Additional file 4: Table S4). For example, in a double blind RCT clinical study of 63 post-menopausal women, treatment with Panax ginseng resulted in increased mitochondrial DNA numbers, improved anti-oxidant status and reduced fatigue symptoms [239]. In a double blind RCT clinical trial enrolling 364 cancer patients, treatment with Panax quinquefolius led to a significant improvement in fatigue symptoms [240]. In various pre-clinical models, plant species demonstrated a number of activities, such as reduced mitochondrial dysfunction with Boerhavia diffusa [241], restored mitochondrial integrity with Hippophae rhamnoides [242] and increased mitochondrial biogenesis with Paullinia cupana [243]. A molecular mechanism for mitochondrial biogenesis was demonstrated in mouse muscle cells treated with Cinnamomum cassia, which stimulated energy expenditure via upregulation of mitochondrial biogenesis factors such as PGC1αα, NRF-1, and Tfam [244].
2.2.9 The neurogenesis hypothesis
New neurons continue to be generated in the adult human brain from endogenous neural stem cells, mainly in specialized niches within the hippocampus [251] (reviewed by [252]). Most brain areas also appear to possess progenitor cells capable of generating new neurons and glial cells [253, 254]. A neurogenesis hypothesis for AD has been raised as a possibility [255], based on experimentally-reduced neurogenesis resulting in impaired memory in animal models [256]. There is also evidence of impaired neurogenesis in AD (reviewed by [257]). For instance, Moreno-Jiménez et al. [258] demonstrated that adult hippocampal neurogenesis (AHN) persists into the ninth decade in healthy humans, but progressively declines in AD. AHN is also reduced in early stages of cognitive decline, suggesting that AHN deficits may proceed and even promote cognitive deficits in AD [259]. Thus, identifying drugs to stimulate AHN could provide novel therapeutic strategies for AD patients [260]. A number of medicinal plants demonstrating neurogenic activity could provide such sources. For instance, Calotropis procera root accelerated neuronal regeneration in a mouse nerve injury model [261]. Neurotrophic factors such as brain-derived neurotrophic factor (BDNF) and nerve growth factor (NGF) enhance the growth and survival of neurons (https://www.nature.com/subjects/neurotrophic-factors). The phytochemical morin (Table 3) (from sources such as Morus alba and Acridocarpus orientalis) demonstrated increased BDNF and NGF in a rat model [262].
Both neurogenic and memory/cognitive improvement activity were demonstrated in 9 species documented in this study (Additional file 3: Table S3). For example, mice treated with Prunella vulgaris demonstrated improved cognitive performance, associated with up‐regulation of adult hippocampal neurogenesis [263]. Sominone (Table 3) (from Withania somnifera) enhanced memory in mice via activation of RET (a receptor for the glial cell line-derived neurotrophic factor) [264]. With oil palm phenolics (from Elaeis guineensis), treated mice showed improved learning and cognitive ability, associated with up-regulation of genes in the Bdnf network and synaptogenesis genes such as Arc and Fos [265].
2.2.10 The cholinergic hypothesis
In the cholinergic hypothesis, memory dysfunction and the cause of AD are attributed to disruption of the cholinergic neurotransmitter system within the brain [266,267,268]. Cholinergic neurons produce the neurotransmitter acetylcholine (ACh), which mediates its action within the synapse and is then inactivated by the enzyme, acetylcholinesterase (AChE) [269]. In AD acetylcholine is depleted, due to structural alterations in cholinergic synapses, loss of specific ACh receptors and death of ACh-generating neurons, all of which lead to a relative accumulation and activity of AChE [270]. Cholinesterase inhibitors (AChEIs) increase available ACh within the synapses of cholinergic neurons by inhibiting its degradation, but lead to only a modest improvement on cognition [271], with limited effects on the pathology and the disease progression [272]. However, AChEIs may have potentially disease-modifying effects [273]. Clinical trials with AChEIs on AD and VD patients have demonstrated a slowing of brain atrophy, which is implicated in AD pathology [274]. AChEIs are also associated with lower risk of stroke and death [275, 276]. A limitation is that AChEIs mediate adverse gastrointestinal symptoms at doses that are too low to be effective, and there are other adverse effects such as cardiac arrhythmia [268, 277]. Hence there remains much room for improvement in this drug class [278], and a search for drugs with more CNS-selective AChE inhibition profiles [279] would be desirable. From this study the 34 plant species with a documented AChEI activity are thus of prospective interest (Table 7; Additional file 4: Table S4).
For instance, AChE inhibition was associated with improved memory and/or cognition in rodent studies with extracts from Carthamus tinctorius [281], Evolvulus alsinoides [282] and Xylia xylocarpa [285]. In an in vitro and rat brain cell study, sarsasapogenin (Table 3) (from Asparagus racemosus) demonstrated AChE inhibition, anti-amyloidogenic activity, anti-oxidant and neuroprotective effects, suggesting a multi target directed ligand potential of sarsasapogenin for AD therapy [50].
2.2.11 The vascular hypothesis
The vascular hypothesis of AD (VHAD) proposes that an impaired vascular system is a major contributor to AD disease progression [286, 287]. In this view, vascular risk factors to AD result in chronic brain hypoperfusion, leading to oxidative stress and a neuronal energy crisis, with progressive neurodegeneration and eventually AD [288]. There are various supportive evidences for VHAD (reviewed by [288]). For instance, vascular dysfunction and reduced cerebral blood flow (CBF) occur before Aβ and hyperphosphorylated tau accumulation [289]. Patients exhibiting multiple vascular risk factors to AD demonstrate a faster rate of cognitive decline [290]. A chronic, ischemic-hypoxic state provoked by vascular dysfunction is sufficient to activate APP processing and thence brain Aβ deposition [291]. Positron emission tomography image assessments accurately predict conversion to AD in hypometabolic mild cognitive impairment patients, indicating that impaired cerebral blood flow reduces glucose supply for the brain’s metabolic needs [292]. A variant of the VHAD is the two-hit vascular hypothesis, which envisages that BBB damage allows leakage of neurotoxic molecules, resulting in neuronal dysfunction and impaired amyloid-β clearance (hit one). These processes lead to accumulation of Aβ in the brain (hit two), with neurotoxic effects [293].
Plants have been found to demonstrate therapeutic activities for various vascular risk factors including endothelial inflammation, atherosclerosis, hyperlipidemia, platelet agglutination and thrombotic components, which are next examined in more detail. An attractive characteristic of some of these species is that they provide multiple activities to target the diverse vascular pathologies implicated in AD.
2.2.11.1 Anti-hypertensive bioactivity
Patients developing AD and VD have been found to have higher blood pressure than cognitively normal individuals [294]. Hypertension leads to impairment of cerebral blood vessels and their occlusion, damaging the brain regions the vessels serve [295]. Hypertension also impairs vascular clearance of brain Aβ [296] and increases amyloid and tau deposition [297, 298]. In a meta-analysis of 12 RCTs, blood pressure lowering with antihypertensive agents was associated with a reduced risk of dementia [299], although data for patients with established AD are more scarce [300]. However, there is an incidence of adverse drug effects and adverse other outcomes [301]. A major issue is adherence with treatment (global average < 50%) [302]. Prospectively such limitations may be ameliorated by the many plants demonstrating anti-hypertensive activity.
In clinical trials, 17 plant species have significantly reduced hypertension (for examples, see Table 8). For instance, in treatment of hypertensive patients with aged garlic (Allium sativum) for 12 weeks, blood pressure was reduced by 12.5%, comparable to that achieved with common antihypertensive medication [303]. Similarly, in a review of 10 randomised double-blind placebo controlled trials, Allium sativum treatment was associated with blood pressure reductions in patients with an elevated systolic blood pressure (SBP) [312]. In a systematic review of the effects of beetroot juice on blood pressure of humans in 22 eligible studies, the overall SBP was significantly lower (3.55 mm Hg) in the beetroot juice–supplemented groups than in the control groups [313].
In a double-blind, randomised parallel arm study in 90 elderly individuals with mild cognitive impairment, drinking high flavanol (≈ 990 mg) cocoa (from Theobroma cacao) was associated with significantly reduced SBP and diastolic blood pressure. The treatment was also associated with improved cognitive function [314].
2.2.11.2 Anti-atherosclerotic activity
AD patients also demonstrate atherosclerotic vascular wall thickening [315], reducing cerebral O2/nutrient supply which may lead to neuronal loss [316]. Atherosclerosis is associated with an elevation in triglyceride-rich lipoproteins and low-density lipoproteins (LDL), and low levels of protective high-density lipoprotein (HDL) [317]. The disease develops initially from injury to the vascular endothelium, such as from toxins (e.g., oxidized cholesterol). This results in an activated and leaky endothelium with increased cytokine expression, and monocytes and T‐lymphocyte recruitment. These migrate, along with various modified lipids such as oxidized low-density lipoprotein, through the leaky endothelium into the sub-endothelial space, and proliferate. An excessive inflammatory response of these various cells leads to atherosclerotic plaque formation, which can impede blood flow within the vessel, with ischaemic or fatal consequences (reviewed by [318, 319]). Medical interventions have majored on reduction of cholesterol and lipid levels with dietary modification and strategies employing intensive lipid-lowering agents including statins [320]. However, adverse side effects including muscle pain, fatigue and potentially life-threatening rhabdomyolysis, are reported in 10% to 25% of patients receiving statin therapy [321]. There can also be impaired mitochondrial function [322], which could aggravate AD-related mitochondrial dysfunction. In view of these factors, plants with lipid-lowering capability provide an alternative treatment option (Table 8; Additional file 4: Table S4). For instance, in a double blind RCT trial of 26 patients with metabolic syndrome treated with red yeast rice and olive extract supplement, LDL cholesterol was lowered by 24% [308]. Blood pressure was also significantly reduced. An RCT trial with 67 hyperlipidemic patients treated with Salvia officinalis resulted in a reduction of total cholesterol, triglyceride (TG), LDL and very low-density lipoprotein in the sage group compared with baseline [309]. In a prospective double blind study of 17 overweight menopausal women given a diet supplemented with Chenopodium quinoa (quinoa), there was a significant reduction in LDL cholesterol and TG compared with baseline [323].
2.2.11.3 Improved vascular endothelial function
However, there is now considerable evidence that atherosclerosis is a chronic inflammatory disease [324]. Clinical trials have shown that targeting inflammation can reduce cardiovascular events [317]. The healthy vascular endothelium inhibits platelet adhesion to the surface [325] but cardiovascular risk factors (e.g., hypertension) increase oxygen free radical production, causing the endothelium to switch to a pro-coagulant, pro-inflammatory and vasoconstrictor phenotype [326, 327].
The 38 species of plants with demonstrated anti-platelet aggregation/improved endothelial function have a bearing on these pathologies (Table 8; Additional file 4: Table S4). For instance, in a randomised controlled clinical trial, consumption of apple (Malus pumila) improved endothelial function in individuals with cardiovascular disease risk [311]. Phyllanthus amarus treatment improved endothelial function and prevented hypertension effects in a rat hypertension model [328]. Molecular mechanisms have been discovered: for instance, EGCG (from Camellia sinensis) demonstrated anti-inflammatory effects on endothelial cells, via inhibition of the MAPK/ERK pathway and downstream inflammatory markers such as TNF-α, IL-6, and ICAM-1 expression [329].
2.2.11.4 Thrombolytic activity
Atherosclerosis continues to develop to form atherosclerotic plaques, which are mainly unstable, and their rupture triggers thrombus formation, which can occlude the vessel [330], leading to the decreased cerebral blood flow associated with AD [316]. Seven plant species in this study were found to possess a thrombolytic activity (the capacity to dissolve thrombi), for instance in human and animal blood cell models with Mauritia flexuosa [331], and Typha angustifolia [332] (Table 8).
2.2.11.5 Anti-obesity activity
Obesity (particularly as indicated by increased waist circumference) increases the risk of AD and dementia [333, 334]. In obesity, excess circulating fatty acids cause adipose tissue cells to become dysfunctional, inducing dyslipidemia and inflammation, which contribute to atherosclerosis [335, 336]. Several plant species surveyed in this study demonstrated anti-obesity activities (Additional file 4: Table S4). For instance, obese rats treated with Cyphomandra betacea extracts raised high-density lipoprotein cholesterol and total anti-oxidant status, and lowered total cholesterol, body weight and pro-inflammatory TNF-α and IL-6 activities [337]. With Cinnamomum cassia treatment, weight gain in obese mice was reduced by increasing energy expenditure via up-regulation of mitochondrial biogenesis [244]. In mice fed a high-fat diet, Alstonia scholaris treatment attenuated lipogenesis by reducing expression of lipogenic enzymes ACC-1, PPARγ, LXRα and SCD-1, and upregulating expression of lipolytic enzymes CPT1A, PPARα and ACOX1 [338].
2.2.12 The metal ion hypothesis
Certain metals are essential nutrients for the body’s metabolism. For instance, iron has a role in a network of 151 components orchestrating respiration, energy metabolism, DNA synthesis and neurotransmission [339]. The metal ion hypothesis proposes a role of metal ions in AD pathogenesis [340], based on evidence of dysregulation in metal homeostasis (reviewed by [341]). For instance, elevated levels of zinc, copper and iron are found in the brains of AD patients [342]. Such metals interact with amyloid and tau, promoting their aggregation and neuronal toxicity [343]. These effects have been ameliorated by the application of iron, copper, zinc and nickel metal chelators in AD animal/ in vitro models [344,345,346]. Such chelators bind with the metal to form less toxic metal complexes which can be excreted [347]. It has thus been suggested that chelation therapy is a promising treatment strategy [348]. However, in clinical trials, synthetic chelators have shown limited efficacy for AD treatment and are associated with adverse side effects [349, 350] such as allergic reactions, along with liver, renal, eye and auditory toxicities [351, 352] and may even worsen AD pathology [353]. The plants in this study may provide more promising and safer alternatives, in which metal chelation or other metal-reduction activity was reported in 30 species (Additional file 4: Table S4). For instance, in several clinical studies with thalassemia patients, iron overload was reduced by treatment with Nigella sativa extract [354] and silymarin (from Silybum marianum) [355] (reviewed by [356]) and in a case report with Camellia sinensis [357]. In rodent models, iron overload was reduced by treatment with extracts from Emblica officinalis [358] and Triticum aestivum [359].
Iron chelation activity is demonstrated in in vitro models in 19 species (Additional file 4: Table S4). Moreover, these plants all demonstrate pleiotropic effects of AD therapeutic potential. For instance, Cocos nucifera demonstrated both iron chelation, anti-amyloid and anti-tau activity (Additional file 3: Table S3). Commonly, the active phytochemicals of such plants are polyphenols of dietary origin, which are considered safe, and thus represent strong candidates for metal chelation therapy in AD [360].
Exposure to non-essential metals (e.g., lead, arsenic, cadmium and aluminium) can also exacerbate AD brain pathogenesis. For instance, lead, arsenic and cadmium increase APP and BACE1 expression, leading to increased Aβ production, plaque formation and tau phosphorylation [361, 362]. Aluminium competes with iron binding sites, resulting in increased iron-mediated ROS, and accumulates in neurons [341]. Medicinal plants from the current survey have also demonstrated activities to reduce non-essential metal toxicity. For instance, in patients with chronic occupational lead poisoning, treatment with allicin (from Allium sativum) resulted in clinical improvement, which could be attributed to lead chelation, reduced oxidative stress and inhibition of lead absorption from the gut [363]. Curcumin (from Curcuma longa) reduced arsenic-induced oxidative stress and induced DNA repair expression in a chronically arsenic-exposed human population [364]. A reversal or reduction of arsenic-induced toxicity in rat models was demonstrated with silibinin (from Silybum marianum) [365] and Ananas comosus [366]. Lead induced toxicity in rats was ameliorated by treatment with Zingiber officinale [367] and Moringa oleifera [368]. In another rat model, treatment with Cynara scolymus leaf extract protected against cadmium toxicity [369]. In an aluminium exposed mouse model, Allium cepa treatment reduced brain aluminium deposition, possibly via PPAR-γ receptor agonism, to reduce aluminium transfer across the BBB [370]. In a rat model, aluminium toxicity-induced neurodegeneration was reduced by treatment with Aloe vera [371]. The effects were also associated with reduced memory deficits. Solanum lycopersicum extract protected mouse keratinocytes from nickel toxicity [372]. In a rat brain mitochondria model, the phytochemical EGCG protected against cadmium-induced damage, with in vitro evidence supporting metal chelating activity [373]. Further species demonstrating reduction of metal toxicity are reviewed by Amadi et al. [351] and Susan et al. [374].
2.2.13 The oestrogen hypothesis
Worldwide around 62% of persons with AD are women [375]. A major driver for this risk may be the precipitous decline in oestrogens with the menopause [376], which suggests that oestrogens have a neuroprotective role. Oestrogens have essential brain functions such as regulation of synaptic plasticity and learning [377] and also reduce oxidative injury, Aβ toxicity, and Aβ generation (reviewed by [378]). Thus oestrogen replacement therapy has been advocated, but from a review of nine clinical trials of oestrogen-containing hormone therapy, the findings suggested that hormone therapy (HT) fails to improve AD cognitive symptoms [379]. For instance, in an RCT treatment of 42 post-menopausal women with raloxifene, a selective oestrogen receptor modulator, no cognitive benefits were conferred in the treated group [380]. However, oestrogen provided a neuroprotective effect if administered to women under 50 years of age. This has been explained by the “critical window” or “window of opportunity” hypothesis, which suggests that the neuroprotective effects of oestrogen depend on age at the time of administration [381]. This is supported by clinical evidence that dementia risk is increased by surgical removal of ovaries prior to the menopause, which results in prematurely reducing sex steroid hormone production [382]. Opinion remains divided whether HT in postmenopausal women provides beneficial or harmful oncological and cardiovascular effects. Clinical data taken in total neither establishes nor refutes the possibility that HT causes breast cancer [383], and for cancer survivors the oncological risk of HT varies with the cancer type, with an increased risk associated with breast and brain cancers [384]. According to a revised global consensus statement, with menopausal HT there is an increased risk of venous thromboembolism and ischemic stroke, and if initiated over the age of 65 increased risk of dementia [385]. Medicinal plants rich in phytoestrogens provide a potentially safer therapeutic alternative. Phytoestrogens are a group of non-steroidal polyphenolic plant metabolites that induce the action of endogenous oestrogens, often by binding to oestrogen receptors [386]. Although almost ubiquitous in plant products, levels may be quite low or moderate in most foods, but are particularly high in soya-based foods and other legumes [387]. Of the plants documented in this study, 18 species demonstrated significant oestrogenic activity (Additional file 4: Table S4). For instance, in an RCT study of postmenopausal women treated with Glycine max (soy bean), therapeutic effects on reproductive system atrophy were attributed to oestrogenic action via an increased percentage of oestrogen receptor positive cells [388]. RCTs examining the effects of soy treatment have reported mixed results [389]. Beneficial effects in post-menopausal women included improved visual memory [390] and cognitive performance [391]. In men, enhanced working memory was reported, suggesting a role for oestrogen in mental processes in males [392]. A study reported negative effects [393] although it had limitations (e.g., short duration of 16 weeks). Moreover, the treatment given was soy milk, which is relatively low in phytoestrogen content [394] in contrast to high levels in other soy foods such as the soya bean and soya flour [387]. Overall, the data from RCTs indicate a need for further, much larger studies with more controlled methodological standards and mediating factors [389].
Oestrogenic activity or high phytoestrogen content was demonstrated on rodent and in vitro models with 19 plant species (Additional file 4: Table S4). For instance, in an ovariectomized rat model, phytoestrogens from Glycine max resulted in improved memory performance, which may be attributed to increased bdnf and synaptic protein gene expression [395]. In other ovariectomized rodent models Pueraria lobata extract promoted oestrogenic activity, by upregulating expression of oestrogen receptor α (ER-α) [396] and Medicago sativa prevented bone loss induced by oestrogen deficiency [397]. Many of these plant species also demonstrate other bioactivities of AD therapeutic potential. For instance, genistein (from Glycine max) alleviates hyperphosphorylation of tau protein through regulating CAMK4 [94].
Male sex hormones (androgens) in men, but also women, have roles in reproduction, cardiac health, bone remodelling, muscle mass, and brain function [398]. Reduced androgen levels in aged men and women may also be risk factors for cognitive impairments and AD, and thus testosterone therapy may have potential benefits [399]. Testosterone–raising activity is demonstrated in rat models with Pistacia atlantica, Punica granatum, Tamarindus indica, and Zingiber officinale. Tamarindus indica is noteworthy in its capacity to raise both oestrogen and testosterone levels [400], indicating a promising pleiotropic potential in targeting various hormone deficiencies implicated in AD.
2.2.14 The infectious agent hypothesis
Itzhaki and colleagues [401] have summarized evidence in favour of an infectious agent in AD which may have a causative role in the pathology. For instance, pathogen signatures specifically colocalize with AD pathology. Moreover, antivirals such as acyclovir block virus-induced Aβ and tau pathology in vitro [402]. Microbes implicated in AD include Herpes simplex virus type 1 (HSV1) and type 2 (HSV2), Garcinia mangostana, Escherichia coli, and several spirochaete and fungal species [401, 403]. Of therapeutic potential are the 769 species demonstrating anti-microbial activity, the most common bioactivity documented in this study (Additional file 3: Table S3; for examples, see Additional file 6: Table S6). For instance, Alstonia scholaris demonstrated effective anti-viral and anti-bacterial activity against HSV-1 [404] and E. coli [405], which are both implicated in AD brain pathology.
The studies were reported in various preclinical models, with anti-bacterial effects being predominantly in vitro. The anti-microbial inhibition ranged from highly potent to more moderate inhibition, according to the species. For instance, with Gossypium barbadense and Ficus benghalensis, HSV-1 inhibition was 99.9% and 96.6% respectively [406] and with Coptis chinensis it was 100% inactivated [407]. Another example of high potency is the anti-bacterial activity of Dacryodes edulis, which was higher than that of gentamicin, the standard reference drug [408]. Morinda lucida extracts were more active against all the tested bacteria than the standard antibiotics (chloramphenicol and ciprofloxacin) [409]. Justicia gendarussa inhibited HIV reverse transcription, by inhibition of both the early and late gene transcription at levels greater than the drug AZT [410].
Clinically approved antiviral drugs exist for only 10 of the 220 + viruses known to infect humans [411]. This highlights a crucial need for anti-viral drug discovery. The 202 plant species in this study documented with anti-viral activity could provide a source of novel anti-viral agents, with the capacity to act by a number of mechanisms. For example, Phyllanthus amarus targeted various stages of the HIV life cycle, thereby presenting multiple antiviral activities, and demonstrated significant anti-HIV activity in human-derived cells [412]. Isatis tinctoria acted on human influenza virus by targeting viral endocytosis, interfering with viral ribonuclear protein export from the nucleus [413]. Urtica dioica inhibited SARS-CoV infection in mice by targeting adsorption or penetration stages of the replication cycle, and by binding to the SARS-CoV spike glycoprotein [414]. An obstacle to the eradication of HIV is the persistence of latent virus in infected patients. Euphorbia tirucalli demonstrated a capacity to eliminate this latent viral reservoir. This is executed in a dual action, by upregulation of the pathway to reactivate the virus out of latency, and downregulation of the viral surface proteins essential for HIV replication [415]. This is of potential high relevance in targeting latent viruses in the brain, implicated in AD pathogenesis [416]. Punica granatum demonstrated multiple anti-viral activity against HSV, Sindbis virus, polio [417], influenza, [418] and HIV [419], indicating a broad spectrum anti-viral activity to target as yet unidentified viral pathogens involved in AD.
Another example of an infectious agent implicated in AD is Porphyromonas gingivalis, a key bacterium in chronic periodontitis. The pathogen was identified in the brain of AD patients, bacterial toxin levels correlating with tau and ubiquitin pathology [420]. Of therapeutic relevance are medicinal plants such as Musa paradisiaca and Pistacia lentiscus, which demonstrated anti-bacterial activity specifically against Porphyromonas gingivalis [421, 422] (Additional file 3: Table S3).
2.2.15 The gut microbiome hypothesis
Alterations in gut microbial communities in AD patients may result in pathophysiological changes in the brain [103, 423]. This hypothesis is supported by evidence of decreased microbial diversity in the gut microbiome of AD patients [424]; an increase in pro-inflammatory gut bacterial taxa is associated with brain amyloid pathology in AD patients [425]; and mice raised with germ-free gut conditions have less cerebral amyloid deposition [426]. Gut microbiome alterations may increase permeability of the gut barrier and result in immune activation, impaired BBB, neuroinflammation, and ultimately neurodegeneration [427]. In an RCT study of healthy older adults, a probiotics-rich diet was associated with reduced inflammatory-causing gut microbiota and improved mental flexibility [428]. Modulation of gut microbiota in AD mouse models led to restoration of an impaired ubiquitin proteasome system and autophagy, reduced cognitive decline and amyloid deposition [429, 430]. These findings suggest that targeting impaired gut microbiota is a promising therapeutic strategy. In the current study, reports of gut microbiota modulation activity were found for Morus alba, Punica granatum and Vaccinium myrtillus. For instance, in a randomised cross-over human trial with Punica granatum consumption, subjects were conferred with higher gut microbiome diversity and more favourable microbiota profile [431]. Resveratrol and quercetin administration in rat models also modified gut microbiota favourably (reviewed by [432]). Various species (e.g., Olea europaea, Solanum lycopersicum) documented in this study are components of the Mediterranean diet. Frail adults’ adherence to a Mediterranean diet was associated with microbiome alterations, reduced inflammation and improved cognitive function, suggesting that such a diet has a beneficial impact on the gut microbiome, which in turn may promote healthier aging [433].
2.2.16 Other effects: apoptosis and aging
Apoptosis, a programme of controlled cell death [434], may have a role in the neuronal cell death associated with AD, based on evidence of increased apoptosis in the AD brain compared with the normal brain [435, 436]. 25 plant species in this study had reports of anti-apoptotic bioactivity (Additional file 4: Table S4). For instance, fibrauretine (Palmatine chloride) (Table 3) from Fibraurea recisa suppressed pro-apoptotic caspase-3 and Bax protein expression, and increased anti-apoptotic Bcl-2 expression in an AD mouse model [74].
Age is the main risk factor for AD, with cellular senescence and other hallmarks of aging thought to contribute to AD pathology [437, 438]. 13 plant species were found to exhibit anti-aging activity (Additional file 4: Table S4), with molecular mechanisms such as upregulation of telomerase activity.
2.3 Plants with ethnological use of memory improvement demonstrate bioactivities of therapeutic relevance to 15 causal bases for AD
The next part of our study focused more particularly on the subset of 107 species in which the ethnological report of memory improvement was validated by an AD-relevant bioactivity. We found that the various species within this subset together demonstrated therapeutic activity for all AD causal bases hypothesised in the previous Section (Additional file 7: Table S7). 69 of these species demonstrated multiple bioactivities of AD therapeutic relevance (for examples see Table 9). Some of the species or their phytochemical extracts demonstrated pleiotropic activity targeted to many of the causal bases. For three of these species (Centella asiatica, Rosmarinus officinalis and Zingiber officinale) the ethnomedical use of memory improvement is also validated by clinical studies confirming memory/cognitive improvement, along with multiple other bioactivities of relevance.
The implication is that the effectiveness of this set of plants is based on their action in targeting multiple key pathologies implicated in AD. If this is so, the plant species with ethnological reports of memory improvement could provide an attractive source of drug leads of AD therapeutic potential.
2.4 Distribution of surveys
2.4.1 Overall distribution pattern of surveys with ND relevance
The distribution of the surveys from which data of ND relevance was mined are indicated in Fig. 1. Of the 67 countries represented by the surveys, these were located most commonly in Africa, Asia, Central and South America. This suggests a particular abundance of studies of ND relevance from those continents. More than one survey within a country was mined if there were sufficiently distinct habitat types or regional identity between them (e.g., Amazonian versus Atlantic Forest of Brazil) or where ND-relevant data richness was revealed in the literature searches. The latter is exemplified by India, in which 10 separate surveys were found that cited species with uses reported for memory improvement. The overall distribution pattern of the surveys across the world revealed by online search engines reflects the abundance of ethnomedical surveys for certain countries (e.g., India, Nigeria), but a paucity of surveys for other countries (e.g., Chad, Libya).
Distribution of ethnomedical surveys with potential therapeutic relevance for neurodegenerative diseases. The survey distribution on the map indicates that the surveys were located most commonly in Africa, Asia, Central and South America, suggesting an abundance of studies of ND relevance from those continents. There is also an abundance of surveys for certain countries (e.g., India, Nigeria), with the biggest cluster of surveys [40 in all] in India, Bangladesh and Pakistan combined. 90 out of 157 (57%) of the studies were found to reside within biodiversity hotspots and therefore are under threat. Inset: surveys located in Pacific islands
Figure 1 demonstrates that the biggest cluster of surveys [40 in total] occurs in India, Bangladesh and Pakistan. This cluster is concentrated particularly in the Himalayan ranges and environs, and although this may be associated with the very high species diversity there, there are other countries with even higher species diversity in which ethnomedical surveys are less common, such as parts of South America. For instance, the Pacific region of Columbia has one of the highest pockets of biodiversity in the world with 50,000 species of plants, and yet both scientific knowledge on Colombian flora and ethnomedical investigations are lacking [439]. The cluster of surveys yielding such high levels of data in the India-Bangladesh-Pakistan country block could be attributed to the philosophy of the Ayurvedic medicine system, in which every plant on earth is considered to have a medicinal property [440], which provides great motivation to search for novel medicinal plant uses, although this could return false positives.
2.4.2 Data at risk—an assessment of causes of concern
The surveys were then mapped in relation to the locations of biodiversity hotspots (BDH) (Fig. 1). 90 out of 157 (57%) of the studies were found to reside within BDHs and therefore are under threat. Since BDH regions have by definition lost at least 70% of their native vegetation, species with valuable therapeutic potential may already have been lost, and there is a threat to the survival of the remaining species. For instance, 40 of the included surveys reside in the Himalayan BDH. In a recent study of 12 Himalayan regions within this BDH, of 112 documented medicinal plant species, 19 species were found to be at risk of extinction, with seven species being critically endangered [441]. The threats are not limited to the BDH regions either. The BDH regions represent only 36 of the world’s most threatened areas, with numerous areas outside BDH status still being vulnerable, such as much of the Brazilian Amazon forest [442]. Another example outside a BDH is a study in Mizoram, India, in which 13 of the 81 species of therapeutic ND relevance listed were reported to be rare, vulnerable or endangered there [443].
Next, the 115 main surveys were examined systematically to determine what the specific threats of concern were to the authors. The threat of most common concern was loss of traditional knowledge (reported by 58% of authors). This was a problem reported in communities worldwide, ranging from South America to Europe, Asia and the Pacific. For instance, in Albania the knowledge erosion is due to urbanization and economic migration away from the villages [444]. In Ethiopia, India and Nepal the knowledge erosion is attributed to the younger generation’s disinterest in ethnomedical knowledge or a lack of knowledge flow [445,445,447]. In Fiji, Martinique and the Philippines its decline is the result of preferences for Western-type medicine [448,448,450]. Once such knowledge is lost, a major consequence reported in Italy is that the remedies that remain treat only unimportant pathologies [451].
The second-most common threat was habitat loss (reported by 34% of authors). For instance, the Atlantic Forest region of Brazil agriculture is now based on brazilwood, sugarcane, coffee and cattle. Relocating 50% of the Brazilian population to cities once covered by forest resulted in only 5% of the original forest remaining [452]. In Ethiopia, habitat loss resulted from various anthropogenic threats such as deforestation to expand agricultural land and for firewood collection [447]. Medicinal plants can also be under threat from invasive weeds [453] and grazing [454]. Over-harvesting is an issue in countries such as Peru [455]. This can lead to species with ND therapeutic potential becoming rare, as for Sideritis athoa in Turkey [454] and in Vietnam for Aquilaria crassna, which is now critically endangered [456].
Loss of medicinal knowledge and habitat loss are often intertwined. As Ji and colleagues comment regarding the Lisu people, in NW Yunnan, China, over-exploitation and deforestation have led to disappearance of some medicinal plants and the associated knowledge of their use [457]. Similar such associations were reported in Côte d'Ivoire [458] and Ethiopia [453].
Analysis of the knowledge erosion problem can be found in the study by Voeks and Leony [459], who attribute the key reason for this loss to formal education access, in which the healing properties of their forests and fields no longer find their way into the curriculum. In contrast to this, traditional knowledge (TK) is sustained in the Kenyan Masai tribe by children spending time with their parents, and this TK persists even with children’s enrolment into formal education [460].
Several remedial strategies are illustrated from the authors surveyed in this study. For instance, harvesting of medicinal plants which are introduced species have less impact on the local habitat, in order to preserve sites of native species under threat [461]. This low-impact harvesting of medicinal plants can bring economic benefits, such as the agro-industrial credit initiative in Panama for producers of medicinal plants that can be marketed [462]. In the Hakka communities of China there is already an awareness of which plants are endangered, and over-harvesting is prevented by using more common species [463]. Environmental education can be fostered by key individuals of a community being included into management programs [461]. The Nicobarese community harvest mainly the leaves of the plants, since these are the most renewable parts [464]. In Northern Peru, healers are open to new knowledge, watching international health trends to incorporate new species such as Noni (Morinda citrifolia) fruits into their own repertoire, the fruit products being harnessed in local plant pharmacies to benefit the local economy and population [455]. One of the most striking examples of an improvement in ethnomedical knowledge in recent years has occurred in Kyrgyzstan. Under the 70 years of Soviet rule, traditional medicinal practices in such Central Asian societies were neglected and suppressed, leading to a loss of TK [465]. However, in the post-Soviet era there has been a remarkable revival of ancestral TK [466].
2.5 Future perspectives
The bioactivities documented in this study of therapeutic relevance to the various pathological causal bases for AD are mainly pre-clinical or in vitro studies. These provide a basis for further studies to ascertain clinical relevance, standardize dosage, ensure safety, and characterize deleterious off-target effects. State of the art technologies exist, such as sequencing, metabolomic and proteomic tools, to excavate undiscovered plant metabolites, improve yield and eliminate toxic compounds from valuable plant extracts [467, 468]. Plant tissue culture techniques can eliminate the reliance on wild plants under threat [469].
The ability of the plant products to cross the BBB can be tested with various in vitro and in vivo BBB models [470]. However, major challenges remain with current BBB models, which have limited ability to recapitulate barrier dysfunction and plaque deposition [471]. Promising next generation models apply tissue engineering technologies, which aim to more effectively replicate BBB architecture [472]. For instance, an in vitro 3D neurovascular model under development combines cells from the nervous system with a BBB endothelial cell interface, which could provide a platform to assess drug effects on neural function [473, 474].
There are yet other less known causal bases implicated in AD pathology [24], for which a plant therapeutic role is largely unexplored. For instance, according to the calcium homeostasis hypothesis, Aβ destabilizes neuronal calcium homeostasis, which renders neurons more vulnerable to environmental insults [475]. There is evidence, for example, of cognitive decline in AD associated with changes in calcineurin/nuclear factor of activated T-cells (NFAT) signaling [476]. Thus NFAT inhibition and application of other agents aiming to correct neuronal Ca2+ dysregulation are therapeutic strategies for AD treatments [477, 478]. However, here too there is potential from medicinal plants, with phytochemicals (e.g., gossypol, kaempferol and arctigenin) demonstrating NFAT and calcineurin inhibition [479], which could be promising candidates for further investigation.
Another underlying factor driving AD pathology may be meningeal lymphatic vessel dysfunction, which thus might be therapeutically targeted [480]. In peripheral tissues, the lymphatic system drains wastes from the spaces between cells, but no such system has been found within the CNS. However, waste fluids have been found to drain into spaces surrounding the blood vessels, a paravascular pathway or “glymphatic” system, so-called because of dependence on glial cells and function similar to the peripheral lymphatic system [481]. Since Aβ is transported along this route, its impairment may contribute to accumulation of amyloid [482], tau and lead to neurodegeneration [483]. Plants with therapeutic bioactivity in stimulating lymphatic drainage, such as Aesculus hippocastanum [484], could thus be explored for a possible similar role in improving glymphatic function.
The study excluded algae, in view of taxonomic placements outside the plant kingdom (Plantae), but there is a new consensus that red and green algae should be placed within Plantae [485]. Promising algal neuroprotective activities of relevance to AD have been reported. For instance in pre-clinical models, fucoxanthin (from the alga Sargussum horneri) inhibited Aβ assembly, reversed memory impairment and enhanced bdnf expression [486]. Future studies could investigate the potential of other algal species, which are underexplored [487].
The focus of the paper was the therapeutic potential of plants for the causal pathologies of AD, but there is also scope to explore a role for plants in relief of AD-related symptoms in addition to memory and cognitive improvement. For instance, subjects with AD show a higher prevalence of sarcopenia (degenerative loss of skeletal muscle mass and strength) [488]. The plants Withania somnifera and Silybum marianum rescued myotubes of sarcopenic subjects, indicating the potential of such plants to reverse the muscle functional decline in sarcopenia [489].
Some of the causal hypotheses are founded on evidence of the causal agent appearing early or earlier than other proposed causalities. An early chronology in the appearance of a pathology in pre-symptomatic individuals in itself does not prove its causality in the disease. There is a need to probe this further, to establish if AD clinical symptoms can convincingly be attributed to a specific causal agent. There is a need also for further clarity of the relationships between the various proposed causal factors: is it a linear and hierarchical one, with upstream and downstream effects, or is it a syndromic disease driven by multiple initial causes? The answers to these question are still needed, to inform more effective targeting of drugs to the key causal agents.
Initiatives to maintain and promote the vanishing ethnomedical knowledge are needed, which may provide valuable information of yet further novel plant species of therapeutic relevance. Gaps need to be filled in TK (such as effective dosage) that is fragmentary in the ethnological literature for species with important therapeutic potential. There is a need to document species that are vulnerable or at risk of extinction, and if possible, to reduce the risks. For instance, the survey of plants within the Himalayan BDH recommended prohibition of unmanaged harvesting of medicinally important threatened plants from the wild, encouraging instead their cultivation [441]. There are alternative modes of cultivation, such as micropropagation, which enable rapid regeneration of plantlets [490]. Another alternative is hydroponic technology, in which nutrients are supplied to the plant in irrigation water [491]. Several medicinal plant species grown with hydroponics have produced higher biomass in a much shorter time period, with a higher concentration of bioactive secondary metabolites, compared with field-grown plants [492]. There are challenges to such cultivation, such as unavailability of seeds, equipment costs, and difficulties of domesticating plants from the wild [493]. There can be a need too for crop management skills to monitor and modify nutrient solutions [494]. However, some of these obstacles are being overcome. For instance, simplified hydroponics, focused on low production costs, have produced promising results in rural communities throughout South America [495, 496].
Finally, this study was not exhaustive. Whilst around 46% of the angiosperm families are represented in this data, the number of species (1339) documented with therapeutic bioactivities is still quite small in relation to the estimated ≥ 300,000 species just within the angiosperms alone. Since many of these species still remain to be surveyed for their ND therapeutic potential, it is likely that the plant kingdom has an even greater repository of potential yet to be tapped. There is thus all the more need for TK and habitats to be preserved so that this resource is not lost.
3 Conclusions
Our first aim was to search for plant species with reported therapeutic effects of AD relevance. Our findings suggest that the documented plants provide a large resource of AD therapeutic potential. The toolkit methodology was found useful for providing a wide reach in the search of this potential. The bioactivity reports of AD relevance were mainly pre-clinical. However, clinical studies were also found, conferring anti-amyloid effects, autophagy induction, increased mitochondrial biogenesis and improved energy metabolism, anti-hypertensive and anti-hyperlipidemic effects, improved endothelial function, reduced iron overload, reduced metal toxicities, oestrogenic activity, anti-microbial effects for pathogens implicated in AD, and gut microbiome modulation to a more favourable microbiota profile. These findings demonstrate that the capacity of plants to target AD pathologies can be translated across to humans. There is much scope for further exploration of the pre-clinical studies that mostly remain to be tested for clinical efficacy. Particularly promising are plant multiple molecular mechanisms targeted to a pathology. For instance, the plants can reduce Aβ via various mechanisms including BACE1 downregulation, upregulation of amyloid-degrading protease, blocking formation of toxic Aβ oligomers, reducing expression of amyloid precursor protein, and remodelling Aβ into non-toxic structures. There are prospects that at least some of the 46 plant species demonstrating these effects may possess phytochemicals that are BBB permeable, and reach their target pathology.
For our second aim, to assess how this ethnomedical data may be at risk, we found that 58% of the mined ethnomedical surveys reside within biodiversity hotspots and are thus under threat, with loss of traditional knowledge the threat most commonly reported. There is therefore an urgent need to preserve the knowledge of ethnomedical use, as well as the habitats on which this knowledge depends. Encouraging signs such as the reversal of such knowledge loss in Central Asian countries such as Kyrgystan indicate that this can indeed be possible.
Our third aim was to find AD causal hypotheses for which the mined plants may have therapeutic relevance. The outcome was that the documented plants in total demonstrated bioactivities targeted to 15 proposed causal pathologies. In particular, the species with an ethnological report of memory improvement as a subset, together demonstrated therapeutic activity for all these AD causal bases, from which it is concluded that this ethnological data is a very valuable resource of AD therapeutic relevance. The fact that there are a large number of AD causal hypotheses is an indication that multiple pathologies may be involved in a complex interplay, and that a primary causal agent (if it exists) remains to be unequivocally discerned. A number of the individual plant species also demonstrated pleiotropic therapeutic bioactivities for a range of pathologies implicated in the various causal hypotheses. These findings suggest that such plants have promise as drug leads to target these multiple hallmarks of pathology. By further probing of their molecular effects, the plants may also provide insight into delineating more clearly the causal basis or bases of AD, which is still crucially needed to inform therapeutic strategies.
4 Materials and methods
4.1 Toolkit methodology and data extraction
Three literature searches were performed using the databases PubMed and Google Scholar, conducted from October 2017 to March 2022, with no time limits on the years of publication. Additional sources of data included reference lists of included articles. The first search enabled an assessment of ND pathologies and symptoms, in order to construct therapeutic categories recognized by ethnomedical practitioners (Additional file 1: Table S1). The search terms of numerous neurodegenerative diseases were applied in relation to terms such as pathology and symptoms (e.g., Alzheimer’s disease AND pathology). A second search consisted of finding ethnomedical surveys containing species with reported ethnological uses which could also be of ND therapeutic potential. The search terms were: ethnomedical survey, ethnobotanical survey, medicinal plants, medical herb, ethnobotany OR indigenous tribe. These search term alternatives were then also combined with country-specific searches to find further surveys not revealed in the initial searches. The therapeutic categories were then applied as a toolkit to find plant species with reported therapeutic effects of ND relevance, mined from 115 ethnomedical surveys. A further 42 ethnomedical surveys were mined for therapeutic benefit of a single symptom only (e.g., memory improvement). Thus, 157 surveys were studied in total (Additional file 2: Table S2). In addition, two ethnomedical databases were accessed: the Prelude database of medicinal plants in Sub-Saharan Africa [497] (http://www.metafro.be/prelude) and the Native American Ethnobotany database (http://naeb.brit.org). The surveys were also analysed to determine how the data may be at risk, and the specific threats of concern to the authors were documented. A third search was to find various hypothesized causal bases for Alzheimer’s disease, and for bioactivities of the above documented plants which could be of therapeutic relevance to these causal bases. For method details with reference to inclusion/exclusion criteria and taxonomy, see S File 1.
4.2 Mapping of survey locations
The RStudio package was used to map the locations of the studies, using the rgdal, rgeos, dplyr and ggplot2 packages. Biodiversity hotspots spatial data was obtained from Hoffman and colleagues [498]. Locations of the studies were determined from maps included in the surveys, and where necessary precise coordinates were obtained using LatLong (www.latlong.net).
Abbreviations
- ACh:
-
Acetylcholine
- AChE:
-
Acetylcholinesterase
- AChEIs:
-
Acetylcholinesterase inhibitors
- AD:
-
Alzheimer’s disease
- AHN:
-
Adult hippocampal neurogenesis
- APP:
-
Amyloid precursor proteins
- Aβ:
-
Amyloid β
- AβO:
-
Amyloid- β oligomer
- BACE1:
-
β-Site APP cleaving enzyme
- BBB:
-
Blood brain barrier
- BDH:
-
Biodiversity hotspots
- BDNF:
-
Brain-derived neurotrophic factor
- C:
-
Cholesterol
- [C]:
-
Number of untreated controls
- CBF:
-
Cerebral blood flow
- CD:
-
Cluster of differentiation
- COX-2:
-
Cyclooxygenase-2
- CSF:
-
Cerebro-spinal fluid
- CVD:
-
Cardio-vascular disease
- E2:
-
Prostaglandin E2
- EGCG:
-
Epigallocatechin-3-gallate
- ER-α:
-
Oestrogen receptor α
- FDA:
-
Food and Drug Administration
- HDL:
-
High-density lipoproteins
- HSV1:
-
Herpes simplex Virus type 1
- HSV2:
-
Herpes simplex Virus type 2
- HT:
-
Hormone therapy
- ICAM-1:
-
Intercellular cell adhesion molecule-1
- IL-6:
-
IL-17, interleukin-6, interleukin-17 etc.
- L-NBP:
-
L-3-n-butylphthalide
- LOX:
-
Lipoxygenase
- mAb:
-
Monoclonal antibody
- MetS:
-
Metabolic syndrome
- N:
-
Number of patients treated
- NDs:
-
Neurodegenerative diseases
- NFAT:
-
Nuclear factor of activated T-cells
- NFTs:
-
Neurofibrillary tangles
- NF-κB:
-
Nuclear factor-κB
- NGF:
-
Nerve growth factor
- RNS:
-
Reactive nitrogen species
- Nrf2:
-
Nuclear factor erythroid 2-related factor 2
- NSAIDs:
-
Non-steroidal inflammatory drugs
- OH8dG:
-
8-Hydroxy-2′-deoxyguanosine
- Ox:
-
Oxidised
- PGE2:
-
Prostaglandin E2
- PQC:
-
Protein quality control
- RCT:
-
Randomised control trial
- ROS:
-
Reactive oxygen species
- SBP:
-
Systolic blood pressure
- TG:
-
Triglyceride
- TH :
-
T-helper
- TH1:
-
T helper 1
- TH2:
-
T helper 2
- TH17:
-
T helper 17
- TH22:
-
T helper 22
- TK:
-
Traditional knowledge
- TNF-α:
-
Tumour necrosis factor alpha
- Treg:
-
Regulatory T cells
- UPS:
-
Ubiquitin–proteasome system
- VHAD:
-
Vascular hypothesis of AD
- VLDL:
-
Very low-density lipoprotein
References
Nichols E, Szoeke CE, Vollset SE, Abbasi N, Abd-Allah F, Abdela J, et al. Global, regional, and national burden of Alzheimer’s disease and other dementias, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. The Lancet Neurology. 2019;18(1):88–106.
Yiannopoulou KG, Anastasiou AI, Zachariou V, Pelidou SH. Reasons for failed trials of disease-modifying treatments for Alzheimer disease and their contribution in recent research. Biomedicines. 2019;7(4):97.
Breijyeh Z, Karaman R. Comprehensive review on Alzheimer’s disease: causes and treatment. Molecules. 2020;25(24):5789.
Dekker FA, Rüdiger SGD. The mitochondrial Hsp90 TRAP1 and Alzheimer’s disease. Front Mol Biosci. 2021;8: 697913.
Lin P, Sun J, Cheng Q, Yang Y, Cordato D, Gao J. The development of pharmacological therapies for Alzheimer’s disease. Neurol Ther. 2021;10(2):609–26.
Collins AE, Saleh TM, Kalisch BE. Naturally occurring antioxidant therapy in Alzheimer’s disease. Antioxidants (Basel). 2022;11(2):213.
Fouka M, Mavroeidi P, Tsaka G, Xilouri M. In search of effective treatments targeting α-synuclein toxicity in synucleinopathies: pros and cons. Front Cell Dev Biol. 2020;8:894.
Cummings JL, Morstorf T, Zhong K. Alzheimer’s disease drug-development pipeline: few candidates, frequent failures. Alzheimers Res Ther. 2014;6(4):37.
McShane R, Westby MJ, Roberts E, Minakaran N, Schneider L, Farrimond LE, et al. Memantine for dementia. Cochrane Database Syst Rev. 2019;3:CD003154.
Vander Zanden CM, Chi EY. Passive immunotherapies targeting amyloid beta and tau oligomers in Alzheimer’s disease. J Pharm Sci. 2020;109(1):68–73.
Mullard A. Landmark Alzheimer’s drug approval confounds research community. Nature. 2021;594(7863):309–10.
Newman DJ, Cragg GM. Natural products as sources of new drugs over the 30 years from 1981 to 2010. J Nat Prod. 2012;75(3):311–35.
Newman DJ, Cragg GM. Natural products as sources of new drugs over the nearly four decades from 01/1981 to 09/2019. J Nat Prod. 2020;83(3):770–803.
Atanasov AG, Waltenberger B, Pferschy-Wenzig EM, Linder T, Wawrosch C, Uhrin P, et al. Discovery and resupply of pharmacologically active plant-derived natural products: a review. Biotechnol Adv. 2015;33(8):1582–614.
Fabricant DS, Farnsworth NR. The value of plants used in traditional medicine for drug discovery. Environ Health Perspect. 2001;109(Suppl 1):69–75.
Houghton PJ. Synergy and polyvalence: paradigms to explain the activity of herbal products. Eval Herbal Med Products. 2009;85:94.
Atanasov AG, Zotchev SB, Dirsch VM, Supuran CT, Taskforce INPS. Natural products in drug discovery: advances and opportunities. Nat Rev Drug Discov. 2021;20(3):200–16.
Ostwald A, Tulloch VJ, Kyne PM, Bax NJ, Dunstan PK, Ferreira LC, et al. Mapping threats to species: method matters. Mar Policy. 2021;131: 104614.
Myers N, Mittermeier RA, Mittermeier CG, da Fonseca GA, Kent J. Biodiversity hotspots for conservation priorities. Nature. 2000;403(6772):853–8.
Mittermeier RA, Turner WR, Larsen FW, Brooks TM, Gascon C. Global biodiversity conservation: the critical role of hotspots. Biodiversity hotspots: Springer; 2011. p. 3–22.
Habel JC, Rasche L, Schneider UA, Engler JO, Schmid E, Rödder D, et al. Final countdown for biodiversity hotspots. Conserv Lett. 2019;12(6): e12668.
Mecocci P, Boccardi V, Cecchetti R, Bastiani P, Scamosci M, Ruggiero C, et al. A long journey into aging, brain aging, and Alzheimer’s disease following the oxidative stress tracks. J Alzheimers Dis. 2018;62(3):1319–35.
Du X, Wang X, Geng M. Alzheimer’s disease hypothesis and related therapies. Transl Neurodegener. 2018;7:2.
Liu PP, Xie Y, Meng XY, Kang JS. History and progress of hypotheses and clinical trials for Alzheimer’s disease. Signal Transduct Target Ther. 2019;4:29.
Selkoe DJ, Hardy J. The amyloid hypothesis of Alzheimer’s disease at 25 years. EMBO Mol Med. 2016;8(6):595–608.
Hampel H, Hardy J, Blennow K, Chen C, Perry G, Kim SH, et al. The amyloid-β pathway in Alzheimer’s disease. Mol Psychiatry. 2021;26(10):5481–503.
Selkoe DJ. Alzheimer’s disease: genes, proteins, and therapy. Physiol Rev. 2001;81:741.
Glenner GG, Wong CW. Alzheimer’s disease: initial report of the purification and characterization of a novel cerebrovascular amyloid protein. Biochem Biophys Res Commun. 1984;120(3):885–90.
Glenner GG. Amyloid beta protein and the basis for Alzheimer’s disease. Prog Clin Biol Res. 1989;317:857–68.
Beyreuther K, Masters CL. Amyloid precursor protein (APP) and beta A4 amyloid in the etiology of Alzheimer’s disease: precursor-product relationships in the derangement of neuronal function. Brain Pathol. 1991;1(4):241–51.
Hardy JA, Higgins GA. Alzheimer’s disease: the amyloid cascade hypothesis. Science. 1992;256(5054):184–5.
Golde TE. Alzheimer’s disease–the journey of a healthy brain into organ failure. Mol Neurodegener. 2022;17(1):1–19.
Cline EN, Bicca MA, Viola KL, Klein WL. The amyloid-β oligomer hypothesis: beginning of the third decade. J Alzheimers Dis. 2018;64(s1):S567–610.
Ferreira ST, Lourenco MV, Oliveira MM, De Felice FG. Soluble amyloid-b oligomers as synaptotoxins leading to cognitive impairment in Alzheimer’s disease. Front Cell Neurosci. 2015;9:191.
Avgerinos KI, Ferrucci L, Kapogiannis D. Effects of monoclonal antibodies against amyloid-β on clinical and biomarker outcomes and adverse event risks: a systematic review and meta-analysis of phase III RCTs in Alzheimer’s disease. Ageing Res Rev. 2021;68: 101339.
Spires-Jones TL. Alzheimer’s research-breakthrough or breakdown? Brain Commun. 2021;3(4):fcab217.
Turner RS, Thomas RG, Craft S, van Dyck CH, Mintzer J, Reynolds BA, et al. A randomized, double-blind, placebo-controlled trial of resveratrol for Alzheimer disease. Neurology. 2015;85(16):1383–91.
Peng Y, Sun J, Hon S, Nylander AN, Xia W, Feng Y, et al. L-3-n-butylphthalide improves cognitive impairment and reduces amyloid-β in a transgenic model of Alzheimer’s disease. J Neurosci. 2010;30(24):8180–9.
Bihaqi SW, Singh AP, Tiwari M. Supplementation of Convolvulus pluricaulis attenuates scopolamine-induced increased tau and Amyloid precursor protein (AβPP) expression in rat brain. Indian J Pharmacol. 2012;44(5):593.
Durairajan SSK, Liu L-F, Lu J-H, Chen L-L, Yuan Q, Chung SK, et al. Berberine ameliorates β-amyloid pathology, gliosis, and cognitive impairment in an Alzheimer’s disease transgenic mouse model. Neurobiol Aging. 2012;33(12):2903–19.
Yaghmaei P, Azarfar K, Dezfulian M, Ebrahim-Habibi A. Silymarin effect on amyloid-β plaque accumulation and gene expression of APP in an Alzheimer’s disease rat model. DARU J Pharm Sci. 2014;22(1):1–7.
Justin Thenmozhi A, Dhivyabharathi M, William Raja TR, Manivasagam T, Essa MM. Tannoid principles of Emblica officinalis renovate cognitive deficits and attenuate amyloid pathologies against aluminum chloride induced rat model of Alzheimer’s disease. Nutr Neurosci. 2016;19(6):269–78.
Ma H, Johnson SL, Liu W, DaSilva NA, Meschwitz S, Dain JA, et al. Evaluation of polyphenol anthocyanin-enriched extracts of blackberry, black raspberry, blueberry, cranberry, red raspberry, and strawberry for free radical scavenging, reactive carbonyl species trapping, anti-glycation, anti-β-amyloid aggregation, and microglial neuroprotective effects. Int J Mol Sci. 2018;19(2):461.
Ogunruku OO, Oboh G, Passamonti S, Tramer F, Boligon AA. Capsicum annuum var. grossum (Bell Pepper) Inhibits β-Secretase Activity and β-Amyloid1–40 Aggregation. J Med Food. 2017;20(2):124–30.
Briffa M, Ghio S, Neuner J, Gauci AJ, Cacciottolo R, Marchal C, et al. Extracts from two ubiquitous Mediterranean plants ameliorate cellular and animal models of neurodegenerative proteinopathies. Neurosci Lett. 2017;638:12–20.
Kleinrichert K, Alappat B. Comparative analysis of antioxidant and anti-amyloidogenic properties of various polyphenol rich phytoceutical extracts. Antioxidants. 2019;8(1):13.
Shin SJ, Jeong Y, Jeon SG, Kim S, Lee S-K, Choi HS, et al. Uncaria rhynchophylla ameliorates amyloid beta deposition and amyloid beta-mediated pathology in 5XFAD mice. Neurochem Int. 2018;121:114–24.
Lee J-E, Kim M-S, Park S-Y. Effect of natural antioxidants on the aggregation and disaggregation of beta-amyloid. Trop J Pharm Res. 2017;16(11):2629–35.
Ishigaki Y, Tanaka H, Akama H, Ogara T, Uwai K, Tokuraku K. A microliter-scale high-throughput screening system with quantum-dot nanoprobes for amyloid-β aggregation inhibitors. PLoS ONE. 2013;8(8): e72992.
Kashyap P, Muthusamy K, Niranjan M, Trikha S, Kumar S. Sarsasapogenin: a steroidal saponin from Asparagus racemosus as multi target directed ligand in Alzheimer’s disease. Steroids. 2020;153: 108529.
Zhao L, Wang J-L, Liu R, Li X-X, Li J-F, Zhang L. Neuroprotective, anti-amyloidogenic and neurotrophic effects of apigenin in an Alzheimer’s disease mouse model. Molecules. 2013;18(8):9949–65.
Pakdeepak K, Chokchaisiri R, Tocharus J, Jearjaroen P, Tocharus C, Suksamrarn A. 5, 6, 7, 4’-Tetramethoxyflavanone protects against neuronal degeneration induced by dexamethasone by attenuating amyloidogenesis in mice. EXCLI J. 2020;19:16.
Mahaman YAR, Huang F, Wu M, Wang Y, Wei Z, Bao J, et al. Moringa oleifera alleviates homocysteine-induced Alzheimer’s disease-like pathology and cognitive impairments. J Alzheimers Dis. 2018;63(3):1141–59.
Du Y, Qu J, Zhang W, Bai M, Zhou Q, Zhang Z, et al. Morin reverses neuropathological and cognitive impairments in APPswe/PS1dE9 mice by targeting multiple pathogenic mechanisms. Neuropharmacology. 2016;108:1–13.
Boubakri A, Leri M, Bucciantini M, Najjaa H, Ben Arfa A, Stefani M, et al. Allium roseum L. extract inhibits amyloid beta aggregation and toxicity involved in Alzheimer’s disease. PLoS ONE. 2020;15(9):e0223815.
Malishev R, Shaham-Niv S, Nandi S, Kolusheva S, Gazit E, Jelinek R. Bacoside-A, an Indian traditional-medicine substance, inhibits β-amyloid cytotoxicity, fibrillation, and membrane interactions. ACS Chem Neurosci. 2017;8(4):884–91.
Morshedi D, Kesejini TS, Aliakbari F, Karami-Osboo R, Shakibaei M, Marvian AT, et al. Identification and characterization of a compound from Cuminum cyminum essential oil with antifibrilation and cytotoxic effect. Res Pharm Sci. 2014;9(6):431.
Dhouafli Z, Rigacci S, Leri M, Bucciantini M, Mahjoub B, Tounsi MS, et al. Screening for amyloid-β aggregation inhibitor and neuronal toxicity of eight Tunisian medicinal plants. Ind Crops Prod. 2018;111:823–33.
Wang Q, Yu X, Patal K, Hu R, Chuang S, Zhang G, et al. Tanshinones inhibit amyloid aggregation by amyloid-β peptide, disaggregate amyloid fibrils, and protect cultured cells. ACS Chem Neurosci. 2013;4(6):1004–15.
McLaurin J, Kierstead ME, Brown ME, Hawkes CA, Lambermon MH, Phinney AL, et al. Cyclohexanehexol inhibitors of Aβ aggregation prevent and reverse Alzheimer phenotype in a mouse model. Nat Med. 2006;12(7):801–8.
Weinberg RP, Koledova VV, Shin H, Park JH, Tan YA, Sinskey AJ, et al. Oil palm phenolics inhibit the in vitro aggregation of β-amyloid peptide into oligomeric complexes. Int J Alzheimer’s Dis. 2018;2018:1.
Wang Y, Xia Z, Xu J-R, Wang Y-X, Hou L-N, Qiu Y, et al. α-Mangostin, a polyphenolic xanthone derivative from mangosteen, attenuates β-amyloid oligomers-induced neurotoxicity by inhibiting amyloid aggregation. Neuropharmacology. 2012;62(2):871–81.
Diomede L, Rigacci S, Romeo M, Stefani M, Salmona M. Oleuropein aglycone protects transgenic C. elegans strains expressing Aβ42 by reducing plaque load and motor deficit. PLoS ONE. 2013;8(3):e58893.
Hamaguchi T, Ono K, Murase A, Yamada M. Phenolic compounds prevent Alzheimer’s pathology through different effects on the amyloid-β aggregation pathway. Am J Pathol. 2009;175(6):2557–65.
Snow AD, Castillo GM, Nguyen BP, Choi PY, Cummings JA, Cam J, et al. The Amazon rain forest plant Uncaria tomentosa (cat’s claw) and its specific proanthocyanidin constituents are potent inhibitors and reducers of both brain plaques and tangles. Sci Rep. 2019;9(1):1–28.
Du W-J, Guo J-J, Gao M-T, Hu S-Q, Dong X-Y, Han Y-F, et al. Brazilin inhibits amyloid β-protein fibrillogenesis, remodels amyloid fibrils and reduces amyloid cytotoxicity. Sci Rep. 2015;5(1):1–10.
Ladiwala ARA, Lin JC, Bale SS, Marcelino-Cruz AM, Bhattacharya M, Dordick JS, et al. Resveratrol selectively remodels soluble oligomers and fibrils of amyloid Aβ into off-pathway conformers. J Biol Chem. 2010;285(31):24228–37.
Sehgal N, Gupta A, Valli RK, Joshi SD, Mills JT, Hamel E, et al. Withania somnifera reverses Alzheimer’s disease pathology by enhancing low-density lipoprotein receptor-related protein in liver. Proc Natl Acad Sci U S A. 2012;109(9):3510–5.
Fan Y, Wang N, Rocchi A, Zhang W, Vassar R, Zhou Y, et al. Identification of natural products with neuronal and metabolic benefits through autophagy induction. Autophagy. 2017;13(1):41–56.
Chen F, Eckman EA, Eckman CB. Reductions in levels of the Alzheimer’s amyloid beta peptide after oral administration of ginsenosides. FASEB J. 2006;20(8):1269–71.
Rezai-Zadeh K, Shytle D, Sun N, Mori T, Hou H, Jeanniton D, et al. Green tea epigallocatechin-3-gallate (EGCG) modulates amyloid precursor protein cleavage and reduces cerebral amyloidosis in Alzheimer transgenic mice. J Neurosci. 2005;25(38):8807–14.
Dhanasekaran M, Holcomb LA, Hitt AR, Tharakan B, Porter JW, Young KA, et al. Centella asiatica extract selectively decreases amyloid beta levels in hippocampus of Alzheimer’s disease animal model. Phytother Res. 2009;23(1):14–9.
Shytle RD, Tan J, Bickford PC, Rezai-Zadeh K, Hou L, Zeng J, et al. Optimized turmeric extract reduces β-Amyloid and phosphorylated Tau protein burden in Alzheimer’s transgenic mice. Curr Alzheimer Res. 2012;9(4):500–6.
Xing Z, He Z, Wang S, Yan Y, Zhu H, Gao Y, et al. Ameliorative effects and possible molecular mechanisms of action of fibrauretine from Fibraurea recisa Pierre on d-galactose/AlCl 3-mediated Alzheimer’s disease. RSC Adv. 2018;8(55):31646–57.
Zhu Y, Bickford PC, Sanberg P, Giunta B, Tan J. Blueberry opposes beta-amyloid peptide-induced microglial activation via inhibition of p44/42 mitogen-activation protein kinase. Rejuvenation Res. 2008;11(5):891–901.
Wang LS, Tao X, Liu XM, Zhou YF, Zhang MD, Liao YH, et al. Cajaninstilbene Acid Ameliorates Cognitive Impairment Induced by Intrahippocampal Injection of Amyloid-β. Front Pharmacol. 2019;10:1084.
Hyung SJ, DeToma AS, Brender JR, Lee S, Vivekanandan S, Kochi A, et al. Insights into antiamyloidogenic properties of the green tea extract (-)-epigallocatechin-3-gallate toward metal-associated amyloid-β species. Proc Natl Acad Sci U S A. 2013;110(10):3743–8.
Gulisano W, Maugeri D, Baltrons MA, Fà M, Amato A, Palmeri A, et al. Role of amyloid-β and tau proteins in Alzheimer’s disease: confuting the amyloid cascade. J Alzheimers Dis. 2018;64(s1):S611–31.
Kametani F, Hasegawa M. Reconsideration of amyloid hypothesis and tau hypothesis in Alzheimer’s disease. Front Neurosci. 2018;12:25.
Davis DG, Schmitt FA, Wekstein DR, Markesbery WR. Alzheimer neuropathologic alterations in aged cognitively normal subjects. J Neuropathol Exp Neurol. 1999;58(4):376–88.
Erten-Lyons D, Woltjer R, Dodge H, Nixon R, Vorobik R, Calvert J, et al. Factors associated with resistance to dementia despite high Alzheimer disease pathology. Neurology. 2009;72(4):354–60.
Chételat G, La Joie R, Villain N, Perrotin A, de La Sayette V, Eustache F, et al. Amyloid imaging in cognitively normal individuals, at-risk populations and preclinical Alzheimer’s disease. Neuroimage Clin. 2013;2:356–65.
Kim J, Chakrabarty P, Hanna A, March A, Dickson DW, Borchelt DR, et al. Normal cognition in transgenic BRI2-Aβ mice. Mol Neurodegener. 2013;8(1):1–12.
Herrup K. The case for rejecting the amyloid cascade hypothesis. Nat Neurosci. 2015;18(6):794–9.
Medina M, Avila J. The role of extracellular Tau in the spreading of neurofibrillary pathology. Front Cell Neurosci. 2014;8:113.
Wang Y, Mandelkow E. Tau in physiology and pathology. Nat Rev Neurosci. 2016;17(1):22–35.
Marcucci V, Kleiman J. Biomarkers and their implications in Alzheimer’s disease: a literature review. Explor Res Hypothesis Med. 2021.
Ittner LM, Ke YD, Delerue F, Bi M, Gladbach A, van Eersel J, et al. Dendritic function of tau mediates amyloid-β toxicity in Alzheimer’s disease mouse models. Cell. 2010;142(3):387–97.
Gong C-X, Liu F, Grundke-Iqbal I, Iqbal K. Impaired brain glucose metabolism leads to Alzheimer neurofibrillary degeneration through a decrease in tau O-GlcNAcylation. J Alzheimers Dis. 2006;9(1):1–12.
Peng Y, Hu Y, Xu S, Li P, Li J, Lu L, et al. L-3-n-butylphthalide reduces tau phosphorylation and improves cognitive deficits in AβPP/PS1-Alzheimer’s transgenic mice. J Alzheimers Dis. 2012;29(2):379–91.
Rezai-Zadeh K, Arendash GW, Hou H, Fernandez F, Jensen M, Runfeldt M, et al. Green tea epigallocatechin-3-gallate (EGCG) reduces β-amyloid mediated cognitive impairment and modulates tau pathology in Alzheimer transgenic mice. Brain Res. 2008;1214:177–87.
George RC, Lew J, Graves DJ. Interaction of cinnamaldehyde and epicatechin with tau: implications of beneficial effects in modulating Alzheimer’s disease pathogenesis. J Alzheimers Dis. 2013;36(1):21–40.
Chen J, Deng X, Liu N, Li M, Liu B, Fu Q, et al. Quercetin attenuates tau hyperphosphorylation and improves cognitive disorder via suppression of ER stress in a manner dependent on AMPK pathway. J Funct Foods. 2016;22:463–76.
Ye S, Wang T-T, Cai B, Wang Y, Li J, Zhan J-X, et al. Genistein protects hippocampal neurons against injury by regulating calcium/calmodulin dependent protein kinase IV protein levels in Alzheimer’s disease model rats. Neural Regen Res. 2017;12(9):1479.
Monti MC, Margarucci L, Riccio R, Casapullo A. Modulation of tau protein fibrillization by oleocanthal. J Nat Prod. 2012;75(9):1584–8.
Nguyen DK, Dai TTX. Study on tau-aggregation inhibitors in Alzheimer’s disease of methanol extracts of several medicinal plants collected in the Mekong Delta, Vietnam. Sci Technol Dev J-Nat Sci. 2017;1(T2):21–8.
Cornejo A, Aguilar Sandoval F, Caballero L, Machuca L, Muñoz P, Caballero J, et al. Rosmarinic acid prevents fibrillization and diminishes vibrational modes associated to β sheet in tau protein linked to Alzheimer’s disease. J Enzyme Inhib Med Chem. 2017;32(1):945–53.
Radenahmad N, Saleh F, Sawangjaroen K, Vongvatcharanon U, Subhadhirasakul P, Rundorn W, et al. Young coconut juice, a potential therapeutic agent that could significantly reduce some pathologies associated with Alzheimer’s disease: novel findings. Br J Nutr. 2011;105(5):738–46.
Kim G-H, Lim K, Yang HS, Lee J-K, Kim Y, Park S-K, et al. Improvement in neurogenesis and memory function by administration of Passiflora incarnata L. extract applied to sleep disorder in rodent models. J Chem Neuroanatomy. 2019;98:27–40.
Ahmadi M, Taherianfard M, Shomali T. Zataria multiflora could improve hippocampal tau protein and TNFα levels and cognitive behavior defects in a rat model of Alzheimer’s disease. Avicenna J Phytomed. 2019;9(5):465.
Corpas R, Griñán-Ferré C, Rodríguez-Farré E, Pallàs M, Sanfeliu C. Resveratrol induces brain resilience against Alzheimer neurodegeneration through proteostasis enhancement. Mol Neurobiol. 2019;56(2):1502–16.
Jones JR, Lebar MD, Jinwal UK, Abisambra JF, Koren J III, Blair L, et al. The diarylheptanoid (+)-a R, 11 S-myricanol and two flavones from bayberry (Myrica cerifera) destabilize the microtubule-associated protein Tau. J Nat Prod. 2011;74(1):38–44.
Peng Y, Tao H, Wang S, Xiao J, Wang Y, Su H. Dietary intervention with edible medicinal plants and derived products for prevention of Alzheimer’s disease: a compendium of time-tested strategy. J Funct Foods. 2021;81: 104463.
Small SA, Duff K. Linking Aβ and tau in late-onset Alzheimer’s disease: a dual pathway hypothesis. Neuron. 2008;60(4):534–42.
Roda AR, Serra-Mir G, Montoliu-Gaya L, Tiessler L, Villegas S. Amyloid-beta peptide and tau protein crosstalk in Alzheimer’s disease. Neural Regen Res. 2022;17(8):1666–74.
Hernández F, Diaz-Hernández M, Avila J, Lucas JJ. Testing the ubiquitin–proteasome hypothesis of neurodegeneration in vivo. Trends Neurosci. 2004;27(2):66–9.
Hartl FU. Molecular chaperones in cellular protein folding. Nature. 1996;381(6583):571–80.
Ciechanover A, Kwon YT. Protein quality control by molecular chaperones in neurodegeneration. Front Neurosci. 2017;11:185.
Hommen F, Bilican S, Vilchez D. Protein clearance strategies for disease intervention. J Neural Transm (Vienna). 2021;129:141.
Ciechanover A. The ubiquitin-proteasome proteolytic pathway. Cell. 1994;79(1):13–21.
de Vrij FM, Fischer DF, van Leeuwen FW, Hol E. Protein quality control in Alzheimer’s disease by the ubiquitin proteasome system. Prog Neurobiol. 2004;74(5):249–70.
Hegde AN, Smith SG, Duke LM, Pourquoi A, Vaz S. Perturbations of Ubiquitin-Proteasome-Mediated Proteolysis in Aging and Alzheimer’s Disease. Front Aging Neurosci. 2019;11:324.
Boland B, Yu WH, Corti O, Mollereau B, Henriques A, Bezard E, et al. Promoting the clearance of neurotoxic proteins in neurodegenerative disorders of ageing. Nat Rev Drug Discov. 2018;17(9):660–88.
Schmidt MF, Gan ZY, Komander D, Dewson G. Ubiquitin signalling in neurodegeneration: mechanisms and therapeutic opportunities. Cell Death Differ. 2021;28(2):570–90.
Le Guerroué F, Youle RJ. Ubiquitin signaling in neurodegenerative diseases: an autophagy and proteasome perspective. Cell Death Differ. 2021;28(2):439–54.
Moghaddam MG, Ahmad FBH, Samzadeh-Kermani A. Biological activity of betulinic acid: a review. 2012.
Huang L, Ho P, Chen C-H. Activation and inhibition of the proteasome by betulinic acid and its derivatives. FEBS Lett. 2007;581(25):4955–9.
Yagishita Y, Fahey JW, Dinkova-Kostova AT, Kensler TW. Broccoli or sulforaphane: is it the source or dose that matters? Molecules. 2019;24(19):3593.
Liu Y, Hettinger CL, Zhang D, Rezvani K, Wang X, Wang H. Sulforaphane enhances proteasomal and autophagic activities in mice and is a potential therapeutic reagent for Huntington’s disease. J Neurochem. 2014;129(3):539–47.
Park HS, Hwang ES, Choi GY, Kim HB, Park KS, Sul JY, et al. Sulforaphane enhances long-term potentiation and ameliorate scopolamine-induced memory impairment. Physiol Behav. 2021;238: 113467.
Park H-M, Kim J-A, Kwak M-K. Protection against amyloid beta cytotoxicity by sulforaphane: role of the proteasome. Arch Pharmacal Res. 2009;32(1):109–15.
Di Meco A, Curtis ME, Lauretti E, Praticò D. Autophagy dysfunction in Alzheimer’s disease: mechanistic insights and new therapeutic opportunities. Biol Psychiat. 2020;87(9):797–807.
Yim WW, Mizushima N. Lysosome biology in autophagy. Cell Discov. 2020;6:6.
Ramesh N, Pandey UB. Autophagy dysregulation in ALS: when protein aggregates get out of hand. Front Mol Neurosci. 2017;10:263.
Limanaqi F, Biagioni F, Gambardella S, Familiari P, Frati A, Fornai F. Promiscuous roles of autophagy and proteasome in neurodegenerative proteinopathies. Int J Mol Sci. 2020;21(8):3028.
Uddin M, Stachowiak A, Mamun AA, Tzvetkov NT, Takeda S, Atanasov AG, et al. Autophagy and Alzheimer’s disease: from molecular mechanisms to therapeutic implications. Front Aging Neurosci. 2018;10:4.
Watanabe Y, Taguchi K, Tanaka M. Ubiquitin, autophagy and neurodegenerative diseases. Cells. 2020;9(9):2022.
Konings E, Timmers S, Boekschoten MV, Goossens GH, Jocken JW, Afman LA, et al. The effects of 30 days resveratrol supplementation on adipose tissue morphology and gene expression patterns in obese men. Int J Obes (Lond). 2014;38(3):470–3.
Park D, Jeong H, Lee MN, Koh A, Kwon O, Yang YR, et al. Resveratrol induces autophagy by directly inhibiting mTOR through ATP competition. Sci Rep. 2016;6(1):1–11.
Fan X, Wang J, Hou J, Lin C, Bensoussan A, Chang D, et al. Berberine alleviates ox-LDL induced inflammatory factors by up-regulation of autophagy via AMPK/mTOR signaling pathway. J Transl Med. 2015;13:92.
Fan D, Liu L, Wu Z, Cao M. Combating Neurodegenerative diseases with the plant alkaloid berberine: molecular mechanisms and therapeutic potential. Curr Neuropharmacol. 2019;17(6):563–79.
Zhang S, Yu Z, Xia J, Zhang X, Liu K, Sik A, et al. Anti-Parkinson’s disease activity of phenolic acids from Eucommia ulmoides Oliver leaf extracts and their autophagy activation mechanism. Food Funct. 2020;11(2):1425–40.
Velagapudi R, Lepiarz I, El-Bakoush A, Katola FO, Bhatia H, Fiebich BL, et al. Induction of autophagy and activation of SIRT-1 deacetylation mechanisms mediate neuroprotection by the pomegranate metabolite urolithin A in BV2 microglia and differentiated 3D human neural progenitor cells. Mol Nutr Food Res. 2019;63(10):1801237.
Lucas SM, Rothwell NJ, Gibson RM. The role of inflammation in CNS injury and disease. Br J Pharmacol. 2006;147(S1):S232–40.
Sochocka M, Diniz BS, Leszek J. Inflammatory response in the CNS: friend or foe? Mol Neurobiol. 2017;54(10):8071–89.
Shastri A, Bonifati DM, Kishore U. Innate immunity and neuroinflammation. Mediators Inflamm. 2013;2013: 342931.
Nimmerjahn A, Kirchhoff F, Helmchen F. Resting microglial cells are highly dynamic surveillants of brain parenchyma in vivo. Science. 2005;308(5726):1314–8.
Mariani MM, Kielian T. Microglia in infectious diseases of the central nervous system. J Neuroimmune Pharmacol. 2009;4(4):448–61.
Biber K, Owens T, Boddeke E. What is microglia neurotoxicity (Not)? Glia. 2014;62(6):841–54.
Perry VH, Holmes C. Microglial priming in neurodegenerative disease. Nat Rev Neurol. 2014;10(4):217–24.
Hickman S, Izzy S, Sen P, Morsett L, El Khoury J. Microglia in neurodegeneration. Nat Neurosci. 2018;21(10):1359–69.
Kim SK, Nabekura J, Koizumi S. Astrocyte-mediated synapse remodeling in the pathological brain. Glia. 2017;65(11):1719–27.
Alberini CM, Cruz E, Descalzi G, Bessières B, Gao V. Astrocyte glycogen and lactate: new insights into learning and memory mechanisms. Glia. 2018;66(6):1244–62.
Sofroniew MV. Astrocyte barriers to neurotoxic inflammation. Nat Rev Neurosci. 2015;16(5):249–63.
Sofroniew MV, Vinters HV. Astrocytes: biology and pathology. Acta Neuropathol. 2010;119(1):7–35.
Zhao J, O’Connor T, Vassar R. The contribution of activated astrocytes to Aβ production: implications for Alzheimer’s disease pathogenesis. J Neuroinflammation. 2011;8(1):1–17.
Garwood C, Pooler A, Atherton J, Hanger D, Noble W. Astrocytes are important mediators of Aβ-induced neurotoxicity and tau phosphorylation in primary culture. Cell Death Dis. 2011;2(6):e167.
Gorshkov K, Aguisanda F, Thorne N, Zheng W. Astrocytes as targets for drug discovery. Drug Discovery Today. 2018;23(3):673–80.
Griffin WST, Barger SW. Neuroinflammatory cytokines—the common thread in Alzheimer’s pathogenesis. US neurology. 2010;6(2):19.
Albaret G, Sifré E, Floch P, Laye S, Aubert A, Dubus P, et al. Alzheimer’s disease and helicobacter pylori infection: inflammation from stomach to brain? J Alzheimers Dis. 2020;73(2):801–9.
Leng F, Edison P. Neuroinflammation and microglial activation in Alzheimer disease: where do we go from here? Nat Rev Neurol. 2021;17(3):157–72.
McGeer PL, McGeer EG. The amyloid cascade-inflammatory hypothesis of Alzheimer disease: implications for therapy. Acta Neuropathol. 2013;126(4):479–97.
in’t Veld BA, Ruitenberg A, Hofman A, Launer LJ, van Duijn CM, Stijnen T, et al. Nonsteroidal antiinflammatory drugs and the risk of Alzheimer’s disease. N Engl J Med. 2001;345(21):1515–21.
Vlad SC, Miller DR, Kowall NW, Felson DT. Protective effects of NSAIDs on the development of Alzheimer disease. Neurology. 2008;70(19):1672–7.
Nichols MR, St-Pierre MK, Wendeln AC, Makoni NJ, Gouwens LK, Garrad EC, et al. Inflammatory mechanisms in neurodegeneration. J Neurochem. 2019;149(5):562–81.
Engelhart MJ, Geerlings MI, Meijer J, Kiliaan A, Ruitenberg A, van Swieten JC, et al. Inflammatory proteins in plasma and the risk of dementia: the Rotterdam study. Arch Neurol. 2004;61(5):668–72.
Alcolea D, Martínez-Lage P, Sánchez-Juan P, Olazarán J, Antúnez C, Izagirre A, et al. Amyloid precursor protein metabolism and inflammation markers in preclinical Alzheimer disease. Neurology. 2015;85(7):626–33.
Streit WJ, Braak H, Xue QS, Bechmann I. Dystrophic (senescent) rather than activated microglial cells are associated with tau pathology and likely precede neurodegeneration in Alzheimer’s disease. Acta Neuropathol. 2009;118(4):475–85.
Heneka MT, Carson MJ, El Khoury J, Landreth GE, Brosseron F, Feinstein DL, et al. Neuroinflammation in Alzheimer’s disease. Lancet Neurol. 2015;14(4):388–405.
Lue L-F, Brachova L, Civin WH, Rogers J. Inflammation, Aβ deposition, and neurofibrillary tangle formation as correlates of Alzheimer’s disease neurodegeneration. J Neuropathol Exp Neurol. 1996;55(10):1083–8.
Kim N, Martinez CC, Jang DS, Lee JK, Oh MS. Anti-neuroinflammatory effect of Iresine celosia on lipopolysaccharide-stimulated microglial cells and mouse. Biomed Pharmacother. 2019;111:1359–66.
Deng L-L, Yuan D, Zhou Z-Y, Wan J-Z, Zhang C-C, Liu C-Q, et al. Saponins from Panax japonicus attenuate age-related neuroinflammation via regulation of the mitogen-activated protein kinase and nuclear factor kappa B signaling pathways. Neural Regen Res. 2017;12(11):1877.
Njan AA, Adenuga FO, Ajayi AM, Sotunde O, Ologe MO, Olaoye SO, et al. Neuroprotective and memory-enhancing effects of methanolic leaf extract of Peristrophe bicalyculata in rat model of type 2 diabetes mellitus. Heliyon. 2020;6(5): e04011.
Dutta K, Patel P, Rahimian R, Phaneuf D, Julien JP. Withania somnifera reverses transactive response DNA binding protein 43 proteinopathy in a mouse model of amyotrophic lateral sclerosis/frontotemporal lobar degeneration. Neurotherapeutics. 2017;14(2):447–62.
Moon M, Kim HG, Choi JG, Oh H, Lee PK, Ha SK, et al. 6-Shogaol, an active constituent of ginger, attenuates neuroinflammation and cognitive deficits in animal models of dementia. Biochem Biophys Res Commun. 2014;449(1):8–13.
Li C, Zhang C, Zhou H, Feng Y, Tang F, Hoi MP, et al. Inhibitory effects of betulinic acid on LPS-induced neuroinflammation involve M2 microglial polarization via CaMKKβ-dependent AMPK activation. Front Mol Neurosci. 2018;11:98.
Ma J, Ren Q, Dong B, Shi Z, Zhang J, Jin D-Q, et al. NO inhibitory constituents as potential anti-neuroinflammatory agents for AD from Blumea balsamifera. Bioorg Chem. 2018;76:449–57.
Choi WJ, Kim SK, Park HK, Sohn UD, Kim W. Anti-inflammatory and anti-superbacterial properties of sulforaphane from shepherd’s purse. Korean J Physiol Pharmacol. 2014;18(1):33–9.
Li R, Huang YG, Fang D, Le WD. (−)-Epigallocatechin gallate inhibits lipopolysaccharide-induced microglial activation and protects against inflammation-mediated dopaminergic neuronal injury. J Neurosci Res. 2004;78(5):723–31.
Lim H-S, Kim YJ, Kim B-Y, Park G, Jeong S-J. The anti-neuroinflammatory activity of tectorigenin pretreatment via downregulated NF-κB and ERK/JNK pathways in BV-2 microglial and microglia inactivation in mice with lipopolysaccharide. Front Pharmacol. 2018;9:462.
Grossi C, Rigacci S, Ambrosini S, Ed Dami T, Luccarini I, Traini C, et al. The polyphenol oleuropein aglycone protects TgCRND8 mice against Aß plaque pathology. PLoS ONE. 2013;8(8):e71702.
Simonyi A, Chen Z, Jiang J, Zong Y, Chuang DY, Gu Z, et al. Inhibition of microglial activation by elderberry extracts and its phenolic components. Life Sci. 2015;128:30–8.
Alkuwari A, Al Naemi M, Vito P, Stilo R, Ahmed T, Al NH. Biological activities of Lycium shawii leaves extract. Int J Pharm Biol Arch. 2012;3:697–700.
Lim HJ, Dong G-Z, Lee HJ, Ryu J-H. In vitro neuroprotective activity of sesquiterpenoids from the flower buds of Tussilago farfara. J Enzyme Inhibition Med Chem. 2015;30(5):852–6.
Meyer P-F, Tremblay-Mercier J, Leoutsakos J, Madjar C, Lafaille-Maignan M-É, Savard M, et al. INTREPAD: a randomized trial of naproxen to slow progress of presymptomatic Alzheimer disease. Neurology. 2019;92(18):e2070–80.
Peters R, Breitner J, James S, Jicha GA, Meyer PF, Richards M, et al. Dementia risk reduction: why haven’t the pharmacological risk reduction trials worked? An in-depth exploration of seven established risk factors. Alzheimers Dement (N Y). 2021;7(1): e12202.
Drazen JM. COX-2 inhibitors–a lesson in unexpected problems. N Engl J Med. 2005;352(11):1131–2.
Mogana R, Teng-Jin K, Wiart C. The medicinal timber Canarium patentinervium Miq. (Burseraceae Kunth.) is an anti-inflammatory bioresource of dual inhibitors of cyclooxygenase (COX) and 5-lipoxygenase (5-LOX). Int Scholarly Res Notices. 2013;2013.
Oeckinghaus A, Ghosh S. The NF-kappaB family of transcription factors and its regulation. Cold Spring Harb Perspect Biol. 2009;1(4): a000034.
Albensi BC. What is nuclear factor kappa B (NF-κB) doing in and to the mitochondrion? Front Cell Dev Biol. 2019;7:154.
Srinivasan M, Lahiri DK. Significance of NF-κB as a pivotal therapeutic target in the neurodegenerative pathologies of Alzheimer’s disease and multiple sclerosis. Expert Opin Ther Targets. 2015;19(4):471–87.
Liu T, Zhang L, Joo D, Sun S-C. NF-κB signaling in inflammation. Signal Transduct Target Ther. 2017;2(1):1–9.
Heiss E, Herhaus C, Klimo K, Bartsch H, Gerhäuser C. Nuclear factor κB is a molecular target for sulforaphane-mediated anti-inflammatory mechanisms. J Biol Chem. 2001;276(34):32008–15.
Frakes AE, Ferraiuolo L, Haidet-Phillips AM, Schmelzer L, Braun L, Miranda CJ, et al. Microglia induce motor neuron death via the classical NF-κB pathway in amyotrophic lateral sclerosis. Neuron. 2014;81(5):1009–23.
Fiala M, Cribbs DH, Rosenthal M, Bernard G. Phagocytosis of amyloid-beta and inflammation: two faces of innate immunity in Alzheimer’s disease. J Alzheimers Dis. 2007;11(4):457–63.
Avagyan H, Goldenson B, Tse E, Masoumi A, Porter V, Wiedau-Pazos M, et al. Immune blood biomarkers of Alzheimer disease patients. J Neuroimmunol. 2009;210(1–2):67–72.
Chee SEJ, Solito E. The impact of ageing on the CNS immune response in Alzheimer’s disease. Front Immunol. 2021;12: 738511.
Fan Z, Brooks DJ, Okello A, Edison P. An early and late peak in microglial activation in Alzheimer’s disease trajectory. Brain. 2017;140(3):792–803.
Chatzileontiadou DS, Sloane H, Nguyen AT, Gras S, Grant EJ. The many faces of CD4+ T cells: Immunological and structural characteristics. Int J Mol Sci. 2020;22(1):73.
Bettcher BM, Tansey MG, Dorothée G, Heneka MT. Peripheral and central immune system crosstalk in Alzheimer disease—a research prospectus. Nat Rev Neurol. 2021;17(11):689–701.
Walker KA, Gottesman RF, Wu A, Knopman DS, Gross AL, Mosley TH, et al. Systemic inflammation during midlife and cognitive change over 20 years: the ARIC Study. Neurology. 2019;92(11):e1256–67.
Bettcher BM, Johnson SC, Fitch R, Casaletto KB, Heffernan KS, Asthana S, et al. Cerebrospinal fluid and plasma levels of inflammation differentially relate to CNS markers of Alzheimer’s disease pathology and neuronal damage. J Alzheimers Dis. 2018;62(1):385–97.
Wu K-M, Zhang Y-R, Huang Y-Y, Dong Q, Tan L, Yu J-T. The role of the immune system in Alzheimer’s disease. Ageing Res Rev. 2021;70: 101409.
Pan R-Y, Ma J, Kong X-X, Wang X-F, Li S-S, Qi X-L, et al. Sodium rutin ameliorates Alzheimer’s disease–like pathology by enhancing microglial amyloid-β clearance. Sci Adv. 2019;5(2):eaau6328.
Cipollini V, Anrather J, Orzi F, Iadecola C. Th17 and cognitive impairment: possible mechanisms of action. Front Neuroanat. 2019;13:95.
Liu Q, Xin W, He P, Turner D, Yin J, Gan Y, et al. Interleukin-17 inhibits adult hippocampal neurogenesis. Sci Rep. 2014;4(1):1–8.
Moutia M, Seghrouchni F, Abouelazz O, Elouaddari A, Al Jahid A, Elhou A, et al. Allium sativum L. regulates in vitro IL-17 gene expression in human peripheral blood mononuclear cells. BMC Complement Altern Med. 2016;16(1):1–10.
Li X, Zhao L, Han J-J, Zhang F, Liu S, Zhu L, et al. Carnosol modulates Th17 cell differentiation and microglial switch in experimental autoimmune encephalomyelitis. Front Immunol. 2018;9:1807.
Mosmann TR, Cherwinski H, Bond MW, Giedlin MA, Coffman RL. Two types of murine helper T cell clone. I. Definition according to profiles of lymphokine activities and secreted proteins. J Immunol. 1986;136(7):2348–57.
Burgaletto C, Munafò A, Di Benedetto G, De Francisci C, Caraci F, Di Mauro R, et al. The immune system on the TRAIL of Alzheimer’s disease. J Neuroinflammation. 2020;17(1):1–11.
Balaji S, Cholan PK, Victor DJ. An emphasis of T-cell subsets as regulators of periodontal health and disease. J Clin Transl Res. 2021;7(5):648–56.
Majdalawieh AF, Hmaidan R, Carr RI. Nigella sativa modulates splenocyte proliferation, Th1/Th2 cytokine profile, macrophage function and NK anti-tumor activity. J Ethnopharmacol. 2010;131(2):268–75.
Schön C, Mödinger Y, Krüger F, Doebis C, Pischel I, Bonnländer B. A new high-quality elderberry plant extract exerts antiviral and immunomodulatory effects in vitro and ex vivo. Food Hydrocolloids. 2021;32(1):650–62.
Ricciotti E, FitzGerald GA. Prostaglandins and inflammation. Arterioscler Thromb Vasc Biol. 2011;31(5):986–1000.
Minhas PS, Latif-Hernandez A, McReynolds MR, Durairaj AS, Wang Q, Rubin A, et al. Restoring metabolism of myeloid cells reverses cognitive decline in ageing. Nature. 2021;590(7844):122–8.
Talan J. Key immune system molecules are a potential target for Alzheimer’s disease. Neurol Today. 2021;21(5):1–32.
Nakatani K, Atsumi M, Arakawa T, Oosawa K, Shimura S, Nakahata N, et al. Inhibitions of histamine release and prostaglandin E2 synthesis by mangosteen, a Thai medicinal plant. Biol Pharm Bull. 2002;25(9):1137–41.
He GL, Luo Z, Yang J, Shen TT, Chen Y, Yang XS. Curcumin ameliorates the reduction effect of PGE2 on Fibrillar β-amyloid peptide (1–42)-induced microglial phagocytosis through the inhibition of EP2-PKA signaling in N9 microglial cells. PLoS ONE. 2016;11(1): e0147721.
Butterfield DA, Stadtman ER. Protein oxidation processes in aging brain. Adv Cell Aging Gerontol. 1997;2:161–91.
Markesbery WR. Oxidative stress hypothesis in Alzheimer’s disease. Free Radic Biol Med. 1997;23(1):134–47.
Buccellato FR, D’Anca M, Fenoglio C, Scarpini E, Galimberti D. Role of oxidative damage in alzheimer’s disease and neurodegeneration: From pathogenic mechanisms to biomarker discovery. Antioxidants. 2021;10(9):1353.
Cristiana F. Introductory chapter: The biology of reactive species: IntechOpen; 2018.
Hensley K, Hall N, Subramaniam R, Cole P, Harris M, Aksenov M, et al. Brain regional correspondence between Alzheimer’s disease histopathology and biomarkers of protein oxidation. J Neurochem. 1995;65(5):2146–56.
Padurariu M, Ciobica A, Lefter R, Lacramioara Serban I, Stefanescu C, Chirita R. The oxidative stress hypothesis in Alzheimer’s disease. Psychiatria Danubina. 2013;25(4):0–409.
Cheignon C, Tomas M, Bonnefont-Rousselot D, Faller P, Hureau C, Collin F. Oxidative stress and the amyloid beta peptide in Alzheimer’s disease. Redox Biol. 2018;14:450–64.
Mecocci P, MacGarvey U, Beal MF. Oxidative damage to mitochondrial DNA is increased in Alzheimer’s disease. Ann Neurol. 1994;36(5):747–51.
Polidori MC, Praticó D, Mangialasche F, Mariani E, Aust O, Anlasik T, et al. High fruit and vegetable intake is positively correlated with antioxidant status and cognitive performance in healthy subjects. J Alzheimers Dis. 2009;17(4):921–7.
Halliwell B. The antioxidant paradox: less paradoxical now? Br J Clin Pharmacol. 2013;75(3):637–44.
Bøhn SK, Myhrstad MC, Thoresen M, Holden M, Karlsen A, Tunheim SH, et al. Blood cell gene expression associated with cellular stress defense is modulated by antioxidant-rich food in a randomised controlled clinical trial of male smokers. BMC Med. 2010;8:54.
Liu SG, Ren PY, Wang GY, Yao SX, He XJ. Allicin protects spinal cord neurons from glutamate-induced oxidative stress through regulating the heat shock protein 70/inducible nitric oxide synthase pathway. Food Funct. 2015;6(1):321–30.
Chowdhury S, Kumar S. Alpha-terpinyl acetate: a natural monoterpenoid from Elettaria cardamomum as multi-target directed ligand in Alzheimer’s disease. J Funct Foods. 2020;68: 103892.
Zheng S. Protective effect of Polygonatum sibiricum Polysaccharide on D-galactose-induced aging rats model. Sci Rep. 2020;10(1):2246.
Bogavac-Stanojevic N, Kotur Stevuljevic J, Cerne D, Zupan J, Marc J, Vujic Z, et al. The role of artichoke leaf tincture (Cynara scolymus) in the suppression of DNA damage and atherosclerosis in rats fed an atherogenic diet. Pharm Biol. 2018;56(1):138–44.
Galuppo M, Giacoppo S, De Nicola GR, Iori R, Navarra M, Lombardo GE, et al. Antiinflammatory activity of glucomoringin isothiocyanate in a mouse model of experimental autoimmune encephalomyelitis. Fitoterapia. 2014;95:160–74.
Prabhakar K, Veerapur V, Bansal P, Parihar VK, Kandadi MR, Kumar PB, et al. Antioxidant and radioprotective effect of the active fraction of Pilea microphylla (L.) ethanolic extract. Chemico-Biol Interactions. 2007;165(1):22–32.
Koyama N, Kuribayashi K, Seki T, Kobayashi K, Furuhata Y, Suzuki K, et al. Serotonin derivatives, major safflower (Carthamus tinctorius L.) seed antioxidants, inhibit low-density lipoprotein (LDL) oxidation and atherosclerosis in apolipoprotein E-deficient mice. J Agric Food Chem. 2006;54(14):4970–6.
Biswas SK. Does the interdependence between oxidative stress and inflammation explain the antioxidant paradox? Oxidative Med Cell Longevity. 2016;2016.
Viecili PRN, Borges DO, Kirsten K, Malheiros J, Viecili E, Melo RD, et al. Effects of Campomanesia xanthocarpa on inflammatory processes, oxidative stress, endothelial dysfunction and lipid biomarkers in hypercholesterolemic individuals. Atherosclerosis. 2014;234(1):85–92.
Vomund S, Schäfer A, Parnham MJ, Brüne B, Von Knethen A. Nrf2, the master regulator of anti-oxidative responses. Int J Mol Sci. 2017;18(12):2772.
Ramsey CP, Glass CA, Montgomery MB, Lindl KA, Ritson GP, Chia LA, et al. Expression of Nrf2 in neurodegenerative diseases. J Neuropathol Exp Neurol. 2007;66(1):75–85.
Davies DA, Adlimoghaddam A, Albensi BC. Role of Nrf2 in synaptic plasticity and memory in Alzheimer’s disease. Cells. 2021;10(8):1844.
Li C, Zhang W-J, Frei B. Quercetin inhibits LPS-induced adhesion molecule expression and oxidant production in human aortic endothelial cells by p38-mediated Nrf2 activation and antioxidant enzyme induction. Redox Biol. 2016;9:104–13.
Dayalan Naidu S, Sutherland C, Zhang Y, Risco A, de la Vega L, Caunt CJ, et al. Heat shock factor 1 is a substrate for p38 mitogen-activated protein kinases. Mol Cell Biol. 2016;36(18):2403–17.
Son TG, Camandola S, Arumugam TV, Cutler RG, Telljohann RS, Mughal MR, et al. Plumbagin, a novel Nrf2/ARE activator, protects against cerebral ischemia. J Neurochem. 2010;112(5):1316–26.
Swerdlow RH, Khan SM. A “mitochondrial cascade hypothesis” for sporadic Alzheimer’s disease. Med Hypotheses. 2004;63(1):8–20.
Swerdlow RH, Burns JM, Khan SM. The Alzheimer’s disease mitochondrial cascade hypothesis: progress and perspectives. Biochim Biophys Acta. 2014;1842(8):1219–31.
Perez Ortiz JM, Swerdlow RH. Mitochondrial dysfunction in Alzheimer’s disease: role in pathogenesis and novel therapeutic opportunities. Br J Pharmacol. 2019;176(18):3489–507.
Tyumentsev MA, Stefanova NA, Muraleva NA, Rumyantseva YV, Kiseleva E, Vavilin VA, et al. Mitochondrial dysfunction as a predictor and driver of Alzheimer’s disease-like pathology in OXYS rats. J Alzheimers Dis. 2018;63(3):1075–88.
Chung TH, Kim JH, Seol SY, Kim YJ, Lee YJ. The effects of Korean red ginseng on biological aging and antioxidant capacity in postmenopausal women: a double-blind randomized controlled study. Nutrients. 2021;13(9):3090.
Barton DL, Liu H, Dakhil SR, Linquist B, Sloan JA, Nichols CR, et al. Wisconsin Ginseng (Panax quinquefolius) to improve cancer-related fatigue: a randomized, double-blind trial, N07C2. J Natl Cancer Inst. 2013;105(16):1230–8.
Prathapan A, Vineetha VP, Raghu KG. Protective effect of Boerhaavia diffusa L. against mitochondrial dysfunction in angiotensin II induced hypertrophy in H9c2 cardiomyoblast cells. PLoS ONE. 2014;9(4):e96220.
Narayanan S, Ruma D, Gitika B, Sharma S, Pauline T, Ram MS, et al. Antioxidant activities of seabuckthorn (Hippophae rhamnoides) during hypoxia induced oxidative stress in glial cells. Mol Cell Biochem. 2005;278(1):9–14.
Lima NDS, Teixeira L, Gambero A, Ribeiro ML. Guarana (Paullinia cupana) stimulates mitochondrial biogenesis in mice fed high-fat diet. Nutrients. 2018;10(2):165.
Song MY, Kang SY, Kang A, Hwang JH, Park YK, Jung HW. Cinnamomum cassia prevents high-fat diet-induced obesity in mice through the increase of muscle energy. Am J Chin Med. 2017;45(5):1017–31.
Kumar A, Prakash A, Dogra S. Naringin alleviates cognitive impairment, mitochondrial dysfunction and oxidative stress induced by D-galactose in mice. Food Chem Toxicol. 2010;48(2):626–32.
Nagoor Meeran MF, Laham F, Azimullah S, Tariq S, Ojha S. α-Bisabolol abrogates isoproterenol-induced myocardial infarction by inhibiting mitochondrial dysfunction and intrinsic pathway of apoptosis in rats. Mol Cell Biochem. 2019;453(1):89–102.
Yousuf S, Atif F, Ahmad M, Hoda N, Ishrat T, Khan B, et al. Resveratrol exerts its neuroprotective effect by modulating mitochondrial dysfunctions and associated cell death during cerebral ischemia. Brain Res. 2009;1250:242–53.
Elekofehinti OO, Kamdem JP, Meinerz DF, Kade IJ, Adanlawo IG, Rocha JBT. Saponin from the fruit of Solanum anguivi protects against oxidative damage mediated by Fe2+ and sodium nitroprusside in rat brain synaptosome P2 fraction. Arch Pharmacal Res. 2015:1–7.
Nogueira L, Ramirez-Sanchez I, Perkins GA, Murphy A, Taub PR, Ceballos G, et al. (-)-Epicatechin enhances fatigue resistance and oxidative capacity in mouse muscle. J Physiol. 2011;589(Pt 18):4615–31.
Tian J, Li G, Liu Z, Fu F. Hydroxysafflor yellow A inhibits rat brain mitochondrial permeability transition pores by a free radical scavenging action. Pharmacology. 2008;82(2):121–6.
Altman J, Das GD. Autoradiographic and histological evidence of postnatal hippocampal neurogenesis in rats. J Comp Neurol. 1965;124(3):319–35.
Niklison-Chirou MV, Agostini M, Amelio I, Melino G. Regulation of adult neurogenesis in mammalian brain. Int J Mol Sci. 2020;21(14):4869.
Palmer TD, Markakis EA, Willhoite AR, Safar F, Gage FH. Fibroblast growth factor-2 activates a latent neurogenic program in neural stem cells from diverse regions of the adult CNS. J Neurosci. 1999;19(19):8487–97.
Kuhn HG, Toda T, Gage FH. Adult hippocampal neurogenesis: a coming-of-age story. J Neurosci. 2018;38(49):10401–10.
Bailey JA, Lahiri DK. A novel effect of rivastigmine on pre-synaptic proteins and neuronal viability in a neurodegeneration model of fetal rat primary cortical cultures and its implication in Alzheimer’s disease. J Neurochem. 2010;112(4):843–53.
Rola R, Raber J, Rizk A, Otsuka S, VandenBerg SR, Morhardt DR, et al. Radiation-induced impairment of hippocampal neurogenesis is associated with cognitive deficits in young mice. Exp Neurol. 2004;188(2):316–30.
Essa H, Peyton L, Hasan W, León BE, Choi DS. Implication of adult hippocampal neurogenesis in Alzheimer’s disease and potential therapeutic approaches. Cells. 2022;11(2):286.
Moreno-Jiménez EP, Flor-García M, Terreros-Roncal J, Rábano A, Cafini F, Pallas-Bazarra N, et al. Adult hippocampal neurogenesis is abundant in neurologically healthy subjects and drops sharply in patients with Alzheimer’s disease. Nat Med. 2019;25(4):554–60.
Tobin MK, Musaraca K, Disouky A, Shetti A, Bheri A, Honer WG, et al. Human hippocampal neurogenesis persists in aged adults and Alzheimer’s disease patients. Cell Stem Cell. 2019;24(6):974–82.
Choi SH, Tanzi RE. Is Alzheimer’s disease a neurogenesis disorder? Cell Stem Cell. 2019;25(1):7–8.
Zafar S, Anwar H, Qasim M, Irfan S, Maqbool J, Sajid F, et al. Calotropis procera (root) escalates functions rehabilitation and attenuates oxidative stress in a mouse model of peripheral nerve injury. Pak J Pharm Sci. 2020;33.
Ola MS, Aleisa AM, Al-Rejaie SS, Abuohashish HM, Parmar MY, Alhomida AS, et al. Flavonoid, morin inhibits oxidative stress, inflammation and enhances neurotrophic support in the brain of streptozotocin-induced diabetic rats. Neurol Sci. 2014;35(7):1003–8.
Park SJ, Ahn YJ, Lee HE, Hong E, Ryu JH. Standardized Prunella vulgaris var. lilacina extract enhances cognitive performance in normal naive mice. Phytother Res. 2015;29(11):1814–21.
Tohda C, Joyashiki E. Sominone enhances neurite outgrowth and spatial memory mediated by the neurotrophic factor receptor, RET. Br J Pharmacol. 2009;157(8):1427–40.
Leow S-S, Sekaran SD, Tan Y, Sundram K, Sambanthamurthi R. Oil palm phenolics confer neuroprotective effects involving cognitive and motor functions in mice. Nutr Neurosci. 2013;16(5):207–17.
Bartus RT, Dean RR, Beer B, Lippa AS. The cholinergic hypothesis of geriatric memory dysfunction. Science. 1982;217(4558):408–14.
Francis PT, Palmer AM, Snape M, Wilcock GK. The cholinergic hypothesis of Alzheimer’s disease: a review of progress. J Neurol Neurosurg Psychiatry. 1999;66(2):137–47.
Vecchio I, Sorrentino L, Paoletti A, Marra R, Arbitrio M. The state of the art on acetylcholinesterase inhibitors in the treatment of Alzheimer’s disease. J Central Nervous Syst Dis. 2021;13:11795735211029112.
Meriney SD, Fanselow E. Synaptic transmission. Academic Press; 2019.
Stanciu GD, Luca A, Rusu RN, Bild V, Beschea Chiriac SI, Solcan C, et al. Alzheimer’s disease pharmacotherapy in relation to cholinergic system involvement. Biomolecules. 2019;10(1):40.
Martinez A, Castro A. Novel cholinesterase inhibitors as future effective drugs for the treatment of Alzheimer’s disease. Expert Opin Investig Drugs. 2006;15(1):1–12.
Moreta MP, Burgos-Alonso N, Torrecilla M, Marco-Contelles J, Bruzos-Cidón C. Efficacy of acetylcholinesterase inhibitors on cognitive function in Alzheimer’s disease. Review of Reviews. Biomedicines. 2021;9(11):1689.
Haake A, Nguyen K, Friedman L, Chakkamparambil B, Grossberg GT. An update on the utility and safety of cholinesterase inhibitors for the treatment of Alzheimer’s disease. Expert Opin Drug Saf. 2020;19(2):147–57.
Cavedo E, Grothe MJ, Colliot O, Lista S, Chupin M, Dormont D, et al. Reduced basal forebrain atrophy progression in a randomized Donepezil trial in prodromal Alzheimer’s disease. Sci Rep. 2017;7(1):1–10.
Tan ECK, Johnell K, Garcia-Ptacek S, Haaksma ML, Fastbom J, Bell JS, et al. Acetylcholinesterase inhibitors and risk of stroke and death in people with dementia. Alzheimers Dement. 2018;14(7):944–51.
Secnik J, Schwertner E, Alvarsson M, Hammar N, Fastbom J, Winblad B, et al. Cholinesterase inhibitors in patients with diabetes mellitus and dementia: an open-cohort study of ~23 000 patients from the Swedish Dementia Registry. BMJ Open Diabetes Res Care. 2020;8(1).
Kho J, Ioannou A, Mandal AK, Missouris CG. Donepezil induces ventricular arrhythmias by delayed repolarisation. Naunyn Schmiedebergs Arch Pharmacol. 2021;394(3):559–60.
Greig NH, Reale M, Tata AM. New pharmacological approaches to the cholinergic system: an overview on muscarinic receptor ligands and cholinesterase inhibitors. Recent Patents on CNS Drug Discovery (Discontinued). 2013;8(2):123–41.
Moss DE. Improving anti-neurodegenerative benefits of acetylcholinesterase inhibitors in Alzheimer’s disease: are irreversible inhibitors the future? Int J Mol Sci. 2020;21(10):3438.
Saleem U, Raza Z, Anwar F, Ahmad B, Hira S, Ali T. Experimental and computational studies to characterize and evaluate the therapeutic effect of Albizia lebbeck (L.) seeds in Alzheimer’s disease. Medicina. 2019;55(5):184.
Kim JH, He MT, Kim MJ, Yang CY, Shin YS, Yokozawa T, et al. Safflower (Carthamus tinctorius L.) seed attenuates memory impairment induced by scopolamine in mice via regulation of cholinergic dysfunction and oxidative stress. Food Funct. 2019;10(6):3650–9.
Sethiya NK, Nahata A, Singh PK, Mishra S. Neuropharmacological evaluation on four traditional herbs used as nervine tonic and commonly available as Shankhpushpi in India. J Ayurveda Integr Med. 2019;10(1):25–31.
Chen Q, Chen X, Fu Z, Bais S, XunYao H. Anti-amnesic effect of Leea indica extract in scopolamine-induced amnesia of Alzheimer’s type in rats. Int J Pharmacol. 2019;15(1):116–23.
Perry NS, Bollen C, Perry EK, Ballard C. Salvia for dementia therapy: review of pharmacological activity and pilot tolerability clinical trial. Pharmacol Biochem Behav. 2003;75(3):651–9.
Lam LMT, Nguyen MTT, Nguyen HX, Dang PH, Nguyen NT, Tran HM, et al. Anti-cholinesterases and memory improving effects of Vietnamese Xylia xylocarpa. Chem Cent J. 2016;10(1):1–10.
Jack C. The vascular hypothesis of Alzheimer’s disease: bench to bedside and beyond. Neurodegener Dis. 2010;7(1–3):116–21.
Scheffer S, Hermkens DMA, van der Weerd L, de Vries HE, Daemen MJAP. Vascular hypothesis of Alzheimer disease: topical review of mouse models. Arterioscler Thromb Vasc Biol. 2021;41(4):1265–83.
de la Torre J. The vascular hypothesis of Alzheimer’s disease: a key to preclinical prediction of dementia using neuroimaging. J Alzheimers Dis. 2018;63(1):35–52.
Solis E Jr, Hascup KN, Hascup ER. Alzheimer’s disease: the link between amyloid-β and neurovascular dysfunction. J Alzheimers Dis. 2020;76(4):1179–98.
Kume K, Hanyu H, Sato T, Hirao K, Shimizu S, Kanetaka H, et al. Vascular risk factors are associated with faster decline of Alzheimer disease: a longitudinal SPECT study. J Neurol. 2011;258(7):1295–303.
Salminen A, Kauppinen A, Kaarniranta K. Hypoxia/ischemia activate processing of Amyloid Precursor Protein: impact of vascular dysfunction in the pathogenesis of Alzheimer’s disease. J Neurochem. 2017;140(4):536–49.
Inui Y, Ito K, Kato T, Group S-JS. Longer-term investigation of the value of 18F-FDG-PET and magnetic resonance imaging for predicting the conversion of mild cognitive impairment to Alzheimer’s disease: a multicenter study. J Alzheimers Dis. 2017;60(3):877–87.
Zlokovic BV. Neurovascular pathways to neurodegeneration in Alzheimer’s disease and other disorders. Nat Rev Neurosci. 2011;12(12):723–38.
Skoog I, Lernfelt B, Landahl S, Palmertz B, Andreasson LA, Nilsson L, et al. 15-year longitudinal study of blood pressure and dementia. Lancet. 1996;347(9009):1141–5.
Iadecola C, Duering M, Hachinski V, Joutel A, Pendlebury ST, Schneider JA, et al. Vascular cognitive impairment and dementia: JACC scientific expert panel. J Am Coll Cardiol. 2019;73(25):3326–44.
Shah NS, Vidal JS, Masaki K, Petrovitch H, Ross GW, Tilley C, et al. Midlife blood pressure, plasma β-amyloid, and the risk for Alzheimer disease: the Honolulu Asia Aging Study. Hypertension. 2012;59(4):780–6.
Langbaum JB, Chen K, Launer LJ, Fleisher AS, Lee W, Liu X, et al. Blood pressure is associated with higher brain amyloid burden and lower glucose metabolism in healthy late middle-age persons. Neurobiol Aging. 2012;33(4):827.e11-9.
Raz L, Bhaskar K, Weaver J, Marini S, Zhang Q, Thompson JF, et al. Hypoxia promotes tau hyperphosphorylation with associated neuropathology in vascular dysfunction. Neurobiol Dis. 2019;126:124–36.
Hughes D, Judge C, Murphy R, Loughlin E, Costello M, Whiteley W, et al. Association of blood pressure lowering with incident dementia or cognitive impairment: a systematic review and meta-analysis. JAMA. 2020;323(19):1934–44.
Lebouvier T, Chen Y, Duriez P, Pasquier F, Bordet R. Antihypertensive agents in Alzheimer’s disease: beyond vascular protection. Expert Rev Neurother. 2020;20(2):175–87.
Pires de Souza GA, Osman IO, Le Bideau M, Baudoin J-P, Jaafar R, Devaux C, et al. Angiotensin II receptor blockers (ARBs antihypertensive Agents) increase replication of SARS-CoV-2 in vero E6 cells. Front Cell Infect Microbiol. 2021;11:507.
Burnier M, Prejbisz A, Weber T, Azizi M, Cunha V, Versmissen J, et al. Hypertension healthcare professional beliefs and behaviour regarding patient medication adherence: a survey conducted among European Society of Hypertension Centres of Excellence. Blood Press. 2021;30(5):282–90.
Ried K, Frank OR, Stocks NP. Aged garlic extract lowers blood pressure in patients with treated but uncontrolled hypertension: a randomised controlled trial. Maturitas. 2010;67(2):144–50.
Siervo M, Shannon O, Kandhari N, Prabhakar M, Fostier W, Köchl C, et al. Nitrate-rich beetroot juice reduces blood pressure in tanzanian adults with elevated blood pressure: a double-blind randomized controlled feasibility trial. J Nutr. 2020;150(9):2460–8.
Shikov AN, Pozharitskaya ON, Makarov VG, Demchenko DV, Shikh EV. Effect of Leonurus cardiaca oil extract in patients with arterial hypertension accompanied by anxiety and sleep disorders. Phytother Res. 2011;25(4):540–3.
Barati Boldaji R, Akhlaghi M, Sagheb MM, Esmaeilinezhad Z. Pomegranate juice improves cardiometabolic risk factors, biomarkers of oxidative stress and inflammation in hemodialysis patients: a randomized crossover trial. J Sci Food Agric. 2020;100(2):846–54.
Wolak T, Sharoni Y, Levy J, Linnewiel-Hermoni K, Stepensky D, Paran E. Effect of tomato nutrient complex on blood pressure: a double blind, randomized dose-response study. Nutrients. 2019;11(5):950.
Verhoeven V, Van der Auwera A, Van Gaal L, Remmen R, Apers S, Stalpaert M, et al. Can red yeast rice and olive extract improve lipid profile and cardiovascular risk in metabolic syndrome: a double blind, placebo controlled randomized trial. BMC Complement Altern Med. 2015;15(1):1–8.
Kianbakht S, Abasi B, Perham M, Hashem Dabaghian F. Antihyperlipidemic effects of Salvia officinalis L. leaf extract in patients with hyperlipidemia: a randomized double-blind placebo-controlled clinical trial. Phytother Res. 2011;25(12):1849–53.
Zhao H, Yun W, Zhang Q, Cai X, Li X, Hui G, et al. Mobilization of circulating endothelial progenitor cells by dl-3-n-butylphthalide in acute ischemic stroke patients. J Stroke Cerebrovasc Dis. 2016;25(4):752–60.
Bondonno NP, Bondonno CP, Blekkenhorst LC, Considine MJ, Maghzal G, Stocker R, et al. Flavonoid-rich apple improves endothelial function in individuals at risk for cardiovascular disease: a randomized controlled clinical trial. Mol Nutr Food Res. 2018;62(3):1700674.
Reinhart KM, Coleman CI, Teevan C, Vachhani P, White CM. Effects of garlic on blood pressure in patients with and without systolic hypertension: a meta-analysis. Ann Pharmacother. 2008;42(12):1766–71.
Bahadoran Z, Mirmiran P, Kabir A, Azizi F, Ghasemi A. The nitrate-independent blood pressure-lowering effect of beetroot juice: a systematic review and meta-analysis. Adv Nutr. 2017;8(6):830–8.
Desideri G, Kwik-Uribe C, Grassi D, Necozione S, Ghiadoni L, Mastroiacovo D, et al. Benefits in cognitive function, blood pressure, and insulin resistance through cocoa flavanol consumption in elderly subjects with mild cognitive impairment: the Cocoa, Cognition, and Aging (CoCoA) study. Hypertension. 2012;60(3):794–801.
Roher AE. Cardiovascular system participation in Alzheimer’s disease pathogenesis. J Intern Med. 2015;277(4):426–8.
Lathe R, Sapronova A, Kotelevtsev Y. Atherosclerosis and Alzheimer-diseases with a common cause? Inflammation, oxysterols, vasculature. BMC Geriatr. 2014;14(1):1–30.
Libby P. The changing landscape of atherosclerosis. Nature. 2021;592(7855):524–33.
Lou-Bonafonte JM, Arnal C, Navarro MA, Osada J. Efficacy of bioactive compounds from extra virgin olive oil to modulate atherosclerosis development. Mol Nutr Food Res. 2012;56(7):1043–57.
Gibson MS, Domingues N, Vieira OV. Lipid and non-lipid factors affecting macrophage dysfunction and inflammation in atherosclerosis. Front Physiol. 2018;9:654.
Packard C, Chapman MJ, Sibartie M, Laufs U, Masana L. Intensive low-density lipoprotein cholesterol lowering in cardiovascular disease prevention: opportunities and challenges. Heart. 2021;107(17):1369–75.
Vinci P, Panizon E, Tosoni LM, Cerrato C, Pellicori F, Mearelli F, et al. Statin-associated myopathy: emphasis on mechanisms and targeted therapy. Int J Mol Sci. 2021;22(21):11687.
Mollazadeh H, Tavana E, Fanni G, Bo S, Banach M, Pirro M, et al. Effects of statins on mitochondrial pathways. J Cachexia Sarcopenia Muscle. 2021;12(2):237–51.
De Carvalho FG, Ovídio PP, Padovan GJ, Jordao Junior AA, Marchini JS, Navarro AM. Metabolic parameters of postmenopausal women after quinoa or corn flakes intake–a prospective and double-blind study. Int J Food Sci Nutr. 2014;65(3):380–5.
Wolf D, Ley K. Immunity and Inflammation in Atherosclerosis. Circ Res. 2019;124(2):315–27.
Libby P, Ridker PM, Maseri A. Inflammation and atherosclerosis. Circulation. 2002;105(9):1135–43.
Gori T. Endothelial function: a short guide for the interventional cardiologist. Int J Mol Sci. 2018;19(12):3838.
Ting KK, Coleman P, Zhao Y, Vadas MA, Gamble JR. The aging endothelium. Vasc Biol. 2021;3(1):R35–47.
Yao NA, Niazi ZR, Najmanová I, Kamagaté M, Said A, Chabert P, et al. Preventive beneficial effect of an aqueous extract of Phyllanthus amarus Schum. and Thonn. (Euphorbiaceae) on DOCA-salt-induced hypertension, cardiac hypertrophy and dysfunction, and endothelial dysfunction in rats. J Cardiovasc Pharmacol. 2020;75(6):573–83.
Zhang L, Zhang ZK, Liang S. Epigallocatechin-3-gallate protects retinal vascular endothelial cells from high glucose stress in vitro via the MAPK/ERK-VEGF pathway. Genet Mol Res. 2016;15(2).
Falk E. Pathogenesis of atherosclerosis. J Am Coll Cardiol. 2006;47(8 Suppl):C7-12.
Fuentes E, Rodríguez-Pérez W, Guzmán L, Alarcón M, Navarrete S, Forero-Doria O, et al. Mauritia flexuosa presents in vitro and in vivo antiplatelet and antithrombotic activities. Evid Based Complement Alternat Med. 2013;2013: 653257.
Umesh M, Sanjeevkumar C, Hanumantappa B, Ramesh L. Evaluation of in vitro anti-thrombolytic activity and cytotoxicity potential of Typha angustifolia L leaves extracts. Int J Pharm Pharm Sci. 2014;6(5):81–5.
Whitmer RA, Gunderson EP, Barrett-Connor E, Quesenberry CP, Yaffe K. Obesity in middle age and future risk of dementia: a 27 year longitudinal population based study. BMJ. 2005;330(7504):1360.
Blüher M. Obesity: global epidemiology and pathogenesis. Nat Rev Endocrinol. 2019;15(5):288–98.
Ohman MK, Shen Y, Obimba CI, Wright AP, Warnock M, Lawrence DA, et al. Visceral adipose tissue inflammation accelerates atherosclerosis in apolipoprotein E-deficient mice. Circulation. 2008;117(6):798–805.
Zhang T, Chen J, Tang X, Luo Q, Xu D, Yu B. Interaction between adipocytes and high-density lipoprotein:new insights into the mechanism of obesity-induced dyslipidemia and atherosclerosis. Lipids Health Dis. 2019;18(1):223.
Abdul Kadir NA, Rahmat A, Jaafar HZ. Protective effects of Tamarillo (Cyphomandra betacea) extract against high fat diet induced obesity in sprague-dawley rats. J Obes. 2015;2015: 846041.
Sun SF, Zhong HJ, Zhao YL, Ma XY, Luo JB, Zhu L, et al. Indole alkaloids of Alstonia scholaris (L.) R. Br. alleviated nonalcoholic fatty liver disease in mice fed with high-fat diet. Nat Prod Bioprospect. 2022;12(1):14.
Hower V, Mendes P, Torti FM, Laubenbacher R, Akman S, Shulaev V, et al. A general map of iron metabolism and tissue-specific subnetworks. Mol Biosyst. 2009;5(5):422–43.
Liu J-L, Fan Y-G, Yang Z-S, Wang Z-Y, Guo C. Iron and Alzheimer’s disease: from pathogenesis to therapeutic implications. Front Neurosci. 2018;12:632.
Huat TJ, Camats-Perna J, Newcombe EA, Valmas N, Kitazawa M, Medeiros R. Metal toxicity links to Alzheimer’s disease and neuroinflammation. J Mol Biol. 2019;431(9):1843–68.
Bush AI. The metal theory of Alzheimer’s disease. J Alzheimers Dis. 2013;33(Suppl 1):S277–81.
Lippi SLP, Neely CLC, Amaya AL. Trace concentrations, heavy implications: influences of biometals on major brain pathologies of Alzheimer’s disease. Int J Biochem Cell Biol. 2022;143: 106136.
Cherny RA, Atwood CS, Xilinas ME, Gray DN, Jones WD, McLean CA, et al. Treatment with a copper-zinc chelator markedly and rapidly inhibits β-amyloid accumulation in Alzheimer’s disease transgenic mice. Neuron. 2001;30(3):665–76.
Zhang Y, He M-l. Deferoxamine enhances alternative activation of microglia and inhibits amyloid beta deposits in APP/PS1 mice. Brain Res. 2017;1677:86–92.
Benoit SL, Maier RJ. The nickel-chelator dimethylglyoxime inhibits human amyloid beta peptide in vitro aggregation. Sci Rep. 2021;11(1):1–11.
Bjørklund G, Mutter J, Aaseth J. Metal chelators and neurotoxicity: lead, mercury, and arsenic. Arch Toxicol. 2017;91(12):3787–97.
Roemhild K, von Maltzahn F, Weiskirchen R, Knüchel R, von Stillfried S, Lammers T. Iron metabolism: pathophysiology and pharmacology. Trends Pharmacol Sci. 2021;42(8):640–56.
Fasae KD, Abolaji AO, Faloye TR, Odunsi AY, Oyetayo BO, Enya JI, et al. Metallobiology and therapeutic chelation of biometals (copper, zinc and iron) in Alzheimer’s disease: limitations, and current and future perspectives. J Trace Elem Med Biol. 2021;67: 126779.
Yeo D, Choi TG, Kim SS. Metal ions-mediated oxidative stress in Alzheimer’s disease and chelation therapy. Reactive Oxygen Species: IntechOpen; 2021.
Amadi CN, Offor SJ, Frazzoli C, Orisakwe OE. Natural antidotes and management of metal toxicity. Environ Sci Pollut Res. 2019;26(18):18032–52.
Lima TG, Benevides FLN, Esmeraldo FL, Farias IS, Dourado DXC, Fontenele EGP, et al. Treatment of iron overload syndrome: a general review. Rev Assoc Med Bras. 2019;65:1216–22.
Hegde ML, Bharathi P, Suram A, Venugopal C, Jagannathan R, Poddar P, et al. Challenges associated with metal chelation therapy in Alzheimer’s disease. J Alzheimers Dis. 2009;17(3):457–68.
El-Shanshory M, Hablas NM, Aboonq MS, Fakhreldin AR, Attia M, Arafa W, et al. Nigella sativa improves anemia, enhances immunity and relieves iron overload-induced oxidative stress as a novel promising treatment in children having beta-thalassemia major. J Herbal Med. 2019;16: 100245.
Moayedi B, Gharagozloo M, Esmaeil N, Maracy MR, Hoorfar H, Jalaeikar M. A randomized double-blind, placebo-controlled study of therapeutic effects of silymarin in β-thalassemia major patients receiving desferrioxamine. Eur J Haematol. 2013;90(3):202–9.
Darvishi Khezri H, Salehifar E, Kosaryan M, Aliasgharian A, Jalali H, Hadian Amree A. Potential effects of silymarin and its flavonolignan components in patients with β-Thalassemia major: a comprehensive review in 2015. Adv Pharmacol Sci. 2016;2016.
Jetsrisuparb AJ, Komwilaisak P, Wiangnon S. Green tea consumption prevented iron overload: a case report of thalassemia intermedia. J Hematol Transfusion Med. 2014;24(4):389–94.
Sarkar R, Hazra B, Mandal N. Amelioration of iron overload-induced liver toxicity by a potent antioxidant and iron chelator, Emblica officinalis Gaertn. Toxicol Ind Health. 2015;31(7):656–69.
Tirgar P, Desai T. Investigation into iron chelating activity of Triticum aestivum (wheat grass) in iron-dextran induce iron overload model of thalassaemia. J Pharm Res. 2011;4(9):3066–9.
Lakey-Beitia J, Burillo AM, La Penna G, Hegde ML, Rao K. Polyphenols as potential metal chelation compounds against Alzheimer’s disease. J Alzheimers Dis. 2021;82(s1):S335–57.
Ashok A, Rai NK, Tripathi S, Bandyopadhyay S. Exposure to As-, Cd-, and Pb-mixture induces Aβ, amyloidogenic APP processing and cognitive impairments via oxidative stress-dependent neuroinflammation in young rats. Toxicol Sci. 2015;143(1):64–80.
Wisessaowapak C, Visitnonthachai D, Watcharasit P, Satayavivad J. Prolonged arsenic exposure increases tau phosphorylation in differentiated SH-SY5Y cells: the contribution of GSK3 and ERK1/2. Environ Toxicol Pharmacol. 2021;84: 103626.
Kianoush S, Balali-Mood M, Mousavi SR, Moradi V, Sadeghi M, Dadpour B, et al. Comparison of therapeutic effects of garlic and d-Penicillamine in patients with chronic occupational lead poisoning. Basic Clin Pharmacol Toxicol. 2012;110(5):476–81.
Roy M, Sinha D, Mukherjee S, Biswas J. Curcumin prevents DNA damage and enhances the repair potential in a chronically arsenic-exposed human population in West Bengal, India. Eur J Cancer Prev. 2011;20(2):123–31.
Muthumani M, Prabu SM. Silibinin potentially protects arsenic-induced oxidative hepatic dysfunction in rats. Toxicol Mech Methods. 2012;22(4):277–88.
Desai V, Ganatra T, Joshi U, Desai T, Tirgar P. An investigation into the heavy metal chelating potential of ananas comosus fruit in arsenic intoxicated rats. J Pharm Res. 2012;5(8):4084–7.
Reddy YA, Chalamaiah M, Ramesh B, Balaji G, Indira P. Ameliorating activity of ginger (Zingiber officinale) extract against lead induced renal toxicity in male rats. J Food Sci Technol. 2014;51(5):908–14.
Velaga MK, Daughtry LK, Jones AC, Yallapragada PR, Rajanna S, Rajanna B. Attenuation of lead-induced oxidative stress in rat brain, liver, kidney and blood of male Wistar rats by Moringa oleifera seed powder. J Environ Pathol Toxicol Oncol. 2014;33(4):323.
El-Boshy M, Ashshi A, Gaith M, Qusty N, Bokhary T, AlTaweel N, et al. Studies on the protective effect of the artichoke (Cynara scolymus) leaf extract against cadmium toxicity-induced oxidative stress, hepatorenal damage, and immunosuppressive and hematological disorders in rats. Environ Sci Pollut Res. 2017;24(13):12372–83.
Singh T, Goel RK. Neuroprotective effect of Allium cepa L. in aluminium chloride induced neurotoxicity. Neurotoxicology. 2015;49:1–7.
Jakkala LK, Ali SA. Amelioration of the toxic effects of aluminium induced neurodegenerative changes in brain of albino rats by aloe vera. J Global Biosci. 2015;4(8):3171–7.
Tito A, Carola A, Bimonte M, Barbulova A, Arciello S, de Laurentiis F, et al. A tomato stem cell extract, containing antioxidant compounds and metal chelating factors, protects skin cells from heavy metal-induced damages. Int J Cosmet Sci. 2011;33(6):543–52.
Abib RT, Peres KC, Barbosa AM, Peres TV, Bernardes A, Zimmermann LM, Quincozes-Santos A, Fiedler HD, Leal RB, Farina M, Gottfried C. Epigallocatechin-3-gallate protects rat brain mitochondria against cadmium-induced damage. Food and chemical toxicology. 2011;49(10):2618–23.
Susan A, Rajendran K, Sathyasivam K, Krishnan UM. An overview of plant-based interventions to ameliorate arsenic toxicity. Biomed Pharmacother. 2019;109:838–52.
Brookmeyer R, Evans DA, Hebert L, Langa KM, Heeringa SG, Plassman BL, et al. National estimates of the prevalence of Alzheimer’s disease in the United States. Alzheimers Dement. 2011;7(1):61–73.
Kantarci K, Lowe VJ, Lesnick TG, Tosakulwong N, Bailey KR, Fields JA, et al. Early postmenopausal transdermal 17β-estradiol therapy and amyloid-β deposition. J Alzheimers Dis. 2016;53(2):547–56.
Rossetti MF, Cambiasso MJ, Holschbach MA, Cabrera R. Oestrogens and progestagens: synthesis and action in the brain. J Neuroendocrinol. 2016;28(7).
Uddin M, Rahman M, Jakaria M, Hossain M, Islam A, Ahmed M, et al. Estrogen signaling in Alzheimer’s disease: molecular insights and therapeutic targets for Alzheimer’s dementia. Mol Neurobiol. 2020;57(6):2654–70.
Henderson VW. Alzheimer’s disease: review of hormone therapy trials and implications for treatment and prevention after menopause. J Steroid Biochem Mol Biol. 2014;142:99–106.
Henderson VW, Ala T, Sainani KL, Bernstein AL, Stephenson BS, Rosen AC, et al. Raloxifene for women with Alzheimer disease: a randomized controlled pilot trial. Neurology. 2015;85(22):1937–44.
Rocca WA, Grossardt BR, Shuster LT. Oophorectomy, menopause, estrogen treatment, and cognitive aging: clinical evidence for a window of opportunity. Brain Res. 2011;1379:188–98.
Rocca W, Bower J, Maraganore D, Ahlskog J, Grossardt B, De Andrade M, et al. Increased risk of cognitive impairment or dementia in women who underwent oophorectomy before menopause. Neurology. 2007;69(11):1074–83.
Hodis HN, Sarrel P. Menopausal hormone therapy and breast cancer: what is the evidence from randomized trials? Climacteric. 2018;21(6):521–8.
Deli T, Orosz M, Jakab A. Hormone replacement therapy in cancer survivors —review of the literature. Pathol Oncol Res. 2020;26(1):63–78.
de Villiers TJ, Hall JE, Pinkerton JV, Pérez SC, Rees M, Yang C, et al. Revised global consensus statement on menopausal hormone therapy. Maturitas. 2016;91:153–5.
Cassidy A. Committee on Toxicity draft report on phyto-oestrogens and health–review of proposed health effects of phyto-oestrogen exposure and recommendations for future research. Nutr Bull. 2003;28(2):205–13.
Kuhnle GG, Dell’Aquila C, Aspinall SM, Runswick SA, Joosen AM, Mulligan AA, et al. Phytoestrogen content of fruits and vegetables commonly consumed in the UK based on LC–MS and 13C-labelled standards. Food Chem. 2009;116(2):542–54.
Lima SMRR, Bernardo BFA, Yamada SS, Reis BF, da Silva GMD, Galvão MAL. Effects of Glycine max (L.) Merr. soy isoflavone vaginal gel on epithelium morphology and estrogen receptor expression in postmenopausal women: a 12-week, randomized, double-blind, placebo-controlled trial. Maturitas. 2014;78(3):205–11.
Soni M, Rahardjo TBW, Soekardi R, Sulistyowati Y, Yesufu-Udechuku A, Irsan A, et al. Phytoestrogens and cognitive function: a review. Maturitas. 2014;77(3):209–20.
Henderson VW, St John JA, Hodis HN, Kono N, McCleary CA, Franke AA, et al. Long-term soy isoflavone supplementation and cognition in women: a randomized, controlled trial. Neurology. 2012;78(23):1841–8.
Casini ML, Marelli G, Papaleo E, Ferrari A, D’Ambrosio F, Unfer V. Psychological assessment of the effects of treatment with phytoestrogens on postmenopausal women: a randomized, double-blind, crossover, placebo-controlled study. Fertil Steril. 2006;85(4):972–8.
Thorp AA, Sinn N, Buckley JD, Coates AM, Howe PR. Soya isoflavone supplementation enhances spatial working memory in men. Br J Nutr. 2009;102(9):1348–54.
Fournier L, Ryan-Borchers T, Robison L, Wiediger M, Park J, Chew B, et al. The effects of soy milk and isoflavone supplements on cognitive performance in healthy, postmenopausal women. J Nutr Health Aging. 2007;11(2):155.
Reinli K, Block G. Phytoestrogen content of foods–a compendium of literature values. Nutr Cancer. 1996;26(2):123–48.
Pan M, Li Z, Yeung V, Xu R-J. Dietary supplementation of soy germ phytoestrogens or estradiol improves spatial memory performance and increases gene expression of BDNF, TrkB receptor and synaptic factors in ovariectomized rats. Nutr Metab. 2010;7(1):1–11.
Lee M-R, Kim B, Lee Y, Park S-Y, Shim J-H, Chung B-H, et al. Ameliorative effects of Pueraria lobata extract on postmenopausal symptoms through promoting estrogenic activity and bone markers in ovariectomized rats. Evid-Based Complement Altern Med. 2021;2021:1.
Jdidi H, Ghorbel Koubaa F, Aoiadni N, Elleuch A, Makni-Ayadi F, El Feki A. Effect of Medicago sativa compared to 17β-oestradiol on osteoporosis in ovariectomized mice. Arch Physiol Biochem. 2020:1–8.
Bianchi VE, Bresciani E, Meanti R, Rizzi L, Omeljaniuk RJ, Torsello A. The role of androgens in women’s health and wellbeing. Pharmacol Res. 2021;171: 105758.
Raber J. Androgens, apoE, and Alzheimer’s disease. Sci Aging Knowl Environ. 2004;2004(11):re2.
Ajani EO, Usman LA. Tamarindus indica fruit pulp restores reproductive function in sodium fluoride administered rats. FASEB J. 2020;34(S1):1.
Itzhaki RF, Lathe R, Balin BJ, Ball MJ, Bearer EL, Braak H, et al. Microbes and Alzheimer’s disease. J Alzheimers Dis. 2016;51(4):979–84.
Wozniak MA, Frost AL, Preston CM, Itzhaki RF. Antivirals reduce the formation of key Alzheimer’s disease molecules in cell cultures acutely infected with herpes simplex virus type 1. PLoS ONE. 2011;6(10): e25152.
Zhan X, Stamova B, Jin LW, DeCarli C, Phinney B, Sharp FR. Gram-negative bacterial molecules associate with Alzheimer disease pathology. Neurology. 2016;87(22):2324–32.
Zhao YL, Gou ZP, Shang JH, Li WY, Kuang Y, Li MY, et al. Anti-microbial effects in vitro and in vivo of Alstonia scholaris. Nat Prod Bioprospect. 2021;11(1):127–35.
Khan MR, Omoloso AD, Kihara M. Antibacterial activity of Alstonia scholaris and Leea tetramera. Fitoterapia. 2003;74(7–8):736–40.
Shoeib A, Zarouk A, El-Esnawy N. Screening of antiviral activity of some terrestrial leaf plants against acyclovir-resistant HSV type-1 in cell culture. Aust J Basic Appl Sci. 2011;5(10):75–92.
Xu HX, Wan M, Loh BN, Kon OL, Chow PW, Sim KY. Screening of traditional medicines for their inhibitory activity against HIV-1 protease. Phytother Res. 1996;10(3):207–10.
Ajibesin KK, Essien EE, Adesanya SA. Antibacterial constituents of the leaves of Dacryodes edulis. Afr J Pharm Pharmacol. 2011;5(15):1782–6.
Fakoya A, Owojuyigbe O, Fakoya S, Adeoye S. Possible antimicrobial activity of Morinda lucida stem bark, leaf and root extracts. Afr J Biotechnol. 2014;13(3):471.
Zhang H-J, Rumschlag-Booms E, Guan Y-F, Wang D-Y, Liu K-L, Li W-F, et al. Potent inhibitor of drug-resistant HIV-1 strains identified from the medicinal plant Justicia gendarussa. J Nat Prod. 2017;80(6):1798–807.
Adamson CS, Chibale K, Goss RJM, Jaspars M, Newman DJ, Dorrington RA. Antiviral drug discovery: preparing for the next pandemic. Chem Soc Rev. 2021;50(6):3647–55.
Notka F, Meier G, Wagner R. Concerted inhibitory activities of Phyllanthus amarus on HIV replication in vitro and ex vivo. Antiviral Res. 2004;64(2):93–102.
Yang Z, Wang Y, Zheng Z, Zhao S, Zhao J, Lin Q, et al. Antiviral activity of Isatis indigotica root-derived clemastanin B against human and avian influenza A and B viruses in vitro. Int J Mol Med. 2013;31(4):867–73.
Kumaki Y, Wandersee MK, Smith AJ, Zhou Y, Simmons G, Nelson NM, et al. Inhibition of severe acute respiratory syndrome coronavirus replication in a lethal SARS-CoV BALB/c mouse model by stinging nettle lectin, Urtica dioica agglutinin. Antiviral Res. 2011;90(1):22–32.
Abreu CM, Price SL, Shirk EN, Cunha RD, Pianowski LF, Clements JE, et al. Dual role of novel ingenol derivatives from Euphorbia tirucalli in HIV replication: inhibition of de novo infection and activation of viral LTR. PLoS ONE. 2014;9(5): e97257.
Itzhaki RF, Golde TE, Heneka MT, Readhead B. Do infections have a role in the pathogenesis of Alzheimer disease? Nat Rev Neurol. 2020;16(4):193–7.
Mouhajir F, Hudson J, Rejdali M, Towers G. Multiple antiviral activities of endemic medicinal plants used by Berber peoples of Morocco. Pharm Biol. 2001;39(5):364–74.
Haidari M, Ali M, Casscells SW III, Madjid M. Pomegranate (Punica granatum) purified polyphenol extract inhibits influenza virus and has a synergistic effect with oseltamivir. Phytomedicine. 2009;16(12):1127–36.
Neurath AR, Strick N, Li Y-Y, Debnath AK. Punica granatum (Pomegranate) juice provides an HIV-1 entry inhibitor and candidate topical microbicide. BMC Infect Dis. 2004;4(1):1–12.
Dominy SS, Lynch C, Ermini F, Benedyk M, Marczyk A, Konradi A, et al. Porphyromonas gingivalis in Alzheimer’s disease brains: evidence for disease causation and treatment with small-molecule inhibitors. Sci Adv. 2019;5(1):eaau3333.
Kapadia SP, Pudakalkatti PS, Shivanaikar S. Detection of antimicrobial activity of banana peel (Musa paradisiaca L.) on Porphyromonas gingivalis and Aggregatibacter actinomycetemcomitans: an in vitro study. Contemp Clin Dent. 2015;6(4):496.
Carrol DH, Chassagne F, Dettweiler M, Quave CL. Antibacterial activity of plant species used for oral health against Porphyromonas gingivalis. PLoS ONE. 2020;15(10): e0239316.
Bairamian D, Sha S, Rolhion N, Sokol H, Dorothée G, Lemere CA, et al. Microbiota in neuroinflammation and synaptic dysfunction: a focus on Alzheimer’s disease. Mol Neurodegener. 2022;17(1):19.
Vogt NM, Kerby RL, Dill-McFarland KA, Harding SJ, Merluzzi AP, Johnson SC, et al. Gut microbiome alterations in Alzheimer’s disease. Sci Rep. 2017;7(1):13537.
Cattaneo A, Cattane N, Galluzzi S, Provasi S, Lopizzo N, Festari C, et al. Association of brain amyloidosis with pro-inflammatory gut bacterial taxa and peripheral inflammation markers in cognitively impaired elderly. Neurobiol Aging. 2017;49:60–8.
Harach T, Marungruang N, Duthilleul N, Cheatham V, Mc Coy K, Frisoni G, et al. Reduction of Abeta amyloid pathology in APPPS1 transgenic mice in the absence of gut microbiota. Sci Rep. 2017;7(1):1–15.
Kowalski K, Mulak A. Brain-gut-microbiota axis in Alzheimer’s disease. J Neurogastroenterol Motil. 2019;25(1):48–60.
Kim CS, Cha L, Sim M, Jung S, Chun WY, Baik HW, et al. Probiotic supplementation improves cognitive function and mood with changes in gut microbiota in community-dwelling older adults: a randomized, double-blind, placebo-controlled, multicenter trial. J Gerontol A Biol Sci Med Sci. 2021;76(1):32–40.
Bonfili L, Cecarini V, Berardi S, Scarpona S, Suchodolski JS, Nasuti C, et al. Microbiota modulation counteracts Alzheimer’s disease progression influencing neuronal proteolysis and gut hormones plasma levels. Sci Rep. 2017;7(1):2426.
Bonfili L, Cuccioloni M, Gong C, Cecarini V, Spina M, Zheng Y, et al. Gut microbiota modulation in Alzheimer’s disease: focus on lipid metabolism. Clin Nutr. 2022;41(3):698–708.
Singh A, D’Amico D, Andreux PA, Dunngalvin G, Kern T, Blanco-Bose W, et al. Direct supplementation with Urolithin A overcomes limitations of dietary exposure and gut microbiome variability in healthy adults to achieve consistent levels across the population. Eur J Clin Nutr. 2021;76:297.
Eid HM, Wright ML, Anil Kumar NV, Qawasmeh A, Hassan STS, Mocan A, et al. Significance of microbiota in obesity and metabolic diseases and the modulatory potential by medicinal plant and food ingredients. Front Pharmacol. 2017;8:387.
Ghosh TS, Rampelli S, Jeffery IB, Santoro A, Neto M, Capri M, et al. Mediterranean diet intervention alters the gut microbiome in older people reducing frailty and improving health status: the NU-AGE 1-year dietary intervention across five European countries. Gut. 2020;69(7):1218–28.
Izadi M, Ali TA, Pourkarimi E. Over fifty years of life, death, and cannibalism: a historical recollection of apoptosis and autophagy. Int J Mol Sci. 2021;22(22):12366.
Su JH, Anderson AJ, Cummings BJ, Cotman CW. Immunohistochemical evidence for apoptosis in Alzheimer’s disease. NeuroReport. 1994;5(18):2529–33.
Fricker M, Tolkovsky AM, Borutaite V, Coleman M, Brown GC. Neuronal cell death. Physiol Rev. 2018;98(2):813–80.
Mattson MP, Arumugam TV. Hallmarks of brain aging: adaptive and pathological modification by metabolic states. Cell Metab. 2018;27(6):1176–99.
Liu RM. Aging, cellular senescence, and Alzheimer’s disease. Int J Mol Sci. 2022;23(4):1989.
Gómez-Estrada H, Díaz-Castillo F, Franco-Ospina L, Mercado-Camargo J, Guzmán-Ledezma J, Medina JD, et al. Folk medicine in the northern coast of Colombia: an overview. J Ethnobiol Ethnomed. 2011;7:27.
Upasani MS, Upasani SV, Beldar VG, Beldar CG, Gujarathi PP. Infrequent use of medicinal plants from India in snakebite treatment. Integr Med Res. 2018;7(1):9–26.
Mehta P, Bisht K, Sekar KC. Diversity of threatened medicinal plants of Indian Himalayan Region. Plant Biosyst Int J Dealing Aspects Plant Biol. 2021;155(6):1121–32.
Pedrollo CT, Kinupp VF, Shepard G, Heinrich M. Medicinal plants at Rio Jauaperi, Brazilian Amazon: ethnobotanical survey and environmental conservation. J Ethnopharmacol. 2016;186:111–24.
Rai PK, Lalramnghinglova H. Ethnomedicinal plant resources of Mizoram, India: implication of traditional knowledge in health care system. Ethnobotanical Leaflets. 2010;2010(3):6.
Pieroni A, Sõukand R. The disappearing wild food and medicinal plant knowledge in a few mountain villages of North-Eastern Albania. J Appl Botany Food Qual. 2017;90.
Bhattarai S, Chaudhary RP, Taylor RS. Ethnomedicinal plants used by the people of Manang district, central Nepal. J Ethnobiol Ethnomed. 2006;2:41.
Sharma J, Gairola S, Gaur RD, Painuli RM, Siddiqi TO. Ethnomedicinal plants used for treating epilepsy by indigenous communities of sub-Himalayan region of Uttarakhand, India. J Ethnopharmacol. 2013;150(1):353–70.
Getaneh S, Girma Z. An ethnobotanical study of medicinal plants in Debre Libanos Wereda, Central Ethiopia. Afr J Plant Sci. 2014;8(7):366–79.
Singh YN. Traditional medicine in Fiji: some herbal folk cures used by Fiji Indians. J Ethnopharmacol. 1986;15(1):57–88.
Longuefosse JL, Nossin E. Medical ethnobotany survey in Martinique. J Ethnopharmacol. 1996;53(3):117–42.
Malawani A, Nuneza O, Uy M, Senarath W. Ethnobotanical survey of the medicinal plants used by the Maranois in Pualas, Lanao del Sur. Philippines BEPLS. 2017;6(6):45–53.
Motti R, Motti P. An ethnobotanical survey of useful plants in the agro Nocerino Sarnese (Campania, southern Italy). Hum Ecol. 2017;45(6):865–78.
Gazzaneo LRS, De Lucena RFP, de Albuquerque UP. Knowledge and use of medicinal plants by local specialists in a region of Atlantic Forest in the state of Pernambuco (Northeastern Brazil). J Ethnobiol Ethnomed. 2005;1(1):1–8.
Lulekal E, Kelbessa E, Bekele T, Yineger H. An ethnobotanical study of medicinal plants in Mana Angetu district, southeastern Ethiopia. J Ethnobiol Ethnomed. 2008;4:10.
Polat R, Satıl F. An ethnobotanical survey of medicinal plants in Edremit Gulf (Balıkesir-Turkey). J Ethnopharmacol. 2012;139(2):626–41.
Bussmann RW, Sharon D. Traditional medicinal plant use in Northern Peru: tracking two thousand years of healing culture. J Ethnobiol Ethnomed. 2006;2:47.
Lee C, Kim S-Y, Eum S, Paik J-H, Bach TT, Darshetkar AM, et al. Ethnobotanical study on medicinal plants used by local Van Kieu ethnic people of Bac Huong Hoa nature reserve, Vietnam. J Ethnopharmacol. 2019;231:283–94.
Ji H, Shengji P, Chunlin L. An ethnobotanical study of medicinal plants used by the Lisu people in Nujiang, northwest Yunnan, China. Econ Bot. 2004;58(1):S253–64.
Malan DF, Neuba DF, Kouakou KL. Medicinal plants and traditional healing practices in Ehotile people, around the Aby Lagoon (eastern littoral of Côte d’Ivoire). J Ethnobiol Ethnomed. 2015;11:21.
Voeks RA, Leony A. Forgetting the forest: assessing medicinal plant erosion in eastern Brazil. Econ Bot. 2004;58(1):S294–306.
Nankaya J, Gichuki N, Lukhoba C, Balslev H. Sustainability of the loita Maasai childrens’ ethnomedicinal knowledge. Sustainability. 2019;11(19):5530.
Begossi A, Hanazaki N, Tamashiro JY. Medicinal plants in the Atlantic Forest (Brazil): knowledge, use, and conservation. Hum Ecol. 2002;30(3):281–99.
Joly LG, Guerra S, Séptimo R, Solís PN, Correa M, Gupta M, et al. Ethnobotanical inventory of medicinal plants used by the Guaymi Indians in western Panama. Part I. J Ethnopharmacol. 1987;20(2):145–71.
Au DT, Wu J, Jiang Z, Chen H, Lu G, Zhao Z. Ethnobotanical study of medicinal plants used by Hakka in Guangdong, China. J Ethnopharmacol. 2008;117(1):41–50.
Chander MP, Kartick C, Gangadhar J, Vijayachari P. Ethno medicine and healthcare practices among Nicobarese of Car Nicobar—an indigenous tribe of Andaman and Nicobar Islands. J Ethnopharmacol. 2014;158:18–24.
Kassam K-A. Viewing change through the prism of indigenous human ecology: findings from the Afghan and Tajik Pamirs. Hum Ecol. 2009;37(6):677–90.
Pawera L, Verner V, Termote C, Sodombekov I, Kandakov A, Karabaev N, et al. Medical ethnobotany of herbal practitioners in the Turkestan Range, southwestern Kyrgyzstan. Acta Societatis Botanicorum Poloniae. 2016;85(1).
Chakraborty P. Herbal genomics as tools for dissecting new metabolic pathways of unexplored medicinal plants and drug discovery. Biochimie open. 2018;6:9–16.
Roychoudhury A, Bhowmik R. State-of-the-art technologies for improving the quality of medicinal and aromatic plants. In: Aftab T, Hakeem KR, editors. Medicinal and aromatic plants. Cham: Springer; 2021. p. 593–627.
Espinosa-Leal CA, Puente-Garza CA, García-Lara S. In vitro plant tissue culture: means for production of biological active compounds. Planta. 2018;248(1):1–18.
Hanafy AS, Dietrich D, Fricker G, Lamprecht A. Blood-brain barrier models: rationale for selection. Adv Drug Deliv Rev. 2021;176: 113859.
Hajal C, Le Roi B, Kamm RD, Maoz BM. Biology and models of the blood–brain barrier. Annu Rev Biomed Eng. 2021;23:359–84.
Kim HN. Engineered models for studying blood-brain-barrier-associated brain physiology and pathology. 2021.
Adriani G, Ma D, Pavesi A, Kamm RD, Goh EL. A 3D neurovascular microfluidic model consisting of neurons, astrocytes and cerebral endothelial cells as a blood–brain barrier. Lab Chip. 2017;17(3):448–59.
Fernandes DC, Reis RL, Oliveira JM. Advances in 3D neural, vascular and neurovascular models for drug testing and regenerative medicine. Drug Discovery Today. 2021;26(3):754–68.
Mattson MP, Cheng B, Davis D, Bryant K, Lieberburg I, Rydel RE. beta-Amyloid peptides destabilize calcium homeostasis and render human cortical neurons vulnerable to excitotoxicity. J Neurosci. 1992;12(2):376–89.
Abdul HM, Sama MA, Furman JL, Mathis DM, Beckett TL, Weidner AM, et al. Cognitive decline in Alzheimer’s disease is associated with selective changes in calcineurin/NFAT signaling. J Neurosci. 2009;29(41):12957–69.
Berridge MJ. Dysregulation of neural calcium signaling in Alzheimer disease, bipolar disorder and schizophrenia. Prion. 2013;7(1):2–13.
Tong BC, Wu AJ, Li M, Cheung KH. Calcium signaling in Alzheimer’s disease & therapies. Biochim Biophys Acta Mol Cell Res. 2018;1865(11 Pt B):1745–60.
Karpurapu M, Lee YG, Qian Z, Wen J, Ballinger MN, Rusu L, et al. Inhibition of nuclear factor of activated T cells (NFAT) c3 activation attenuates acute lung injury and pulmonary edema in murine models of sepsis. Oncotarget. 2018;9(12):10606.
Da Mesquita S, Louveau A, Vaccari A, Smirnov I, Cornelison RC, Kingsmore KM, et al. Functional aspects of meningeal lymphatics in ageing and Alzheimer’s disease. Nature. 2018;560(7717):185–91.
Bacyinski A, Xu M, Wang W, Hu J. The paravascular pathway for brain waste clearance: current understanding, significance and controversy. Front Neuroanat. 2017;11:101.
Iliff JJ, Wang M, Liao Y, Plogg BA, Peng W, Gundersen GA, et al. A paravascular pathway facilitates CSF flow through the brain parenchyma and the clearance of interstitial solutes, including amyloid β. Sci Transl Med. 2012;4(147):147.
Ishida K, Yamada K, Nishiyama R, Hashimoto T, Nishida I, Abe Y, et al. Glymphatic system clears extracellular tau and protects from tau aggregation and neurodegeneration. J Exp Med. 2022;219(3): e20211275.
Wheat J, Currie G, Kiat H, Bone K. Improving lymphatic drainage with herbal preparations: a potentially novel approach to management of lymphedema. Aust J Med Herbalism. 2009;21(3):66–70.
Ruggiero MA, Gordon DP, Orrell TM, Bailly N, Bourgoin T, Brusca RC, et al. A higher level classification of all living organisms. PLoS ONE. 2015;10(4): e0119248.
Xiang S, Liu F, Lin J, Chen H, Huang C, Chen L, et al. Fucoxanthin inhibits β-amyloid assembly and attenuates β-amyloid oligomer-induced cognitive impairments. J Agric Food Chem. 2017;65(20):4092–102.
Olasehinde TA, Olaniran AO, Okoh AI. Macroalgae as a valuable source of naturally occurring bioactive compounds for the treatment of Alzheimer’s disease. Mar Drugs. 2019;17(11):609.
Ogawa Y, Kaneko Y, Sato T, Shimizu S, Kanetaka H, Hanyu H. Sarcopenia and muscle functions at various stages of Alzheimer disease. Front Neurol. 2018;9:710.
Salvadori L, Mandrone M, Manenti T, Ercolani C, Cornioli L, Lianza M, et al. Identification of Withania somnifera-Silybum marianum-Trigonella foenum-graecum Formulation as a Nutritional Supplement to Contrast Muscle Atrophy and Sarcopenia. Nutrients. 2021;13(1):49.
Sethy R, Kullu B. Micropropagation of ethnomedicinal plant Calotropis sp. and enhanced production of stigmasterol. Plant Cell Tissue Organ Cult (PCTOC). 2022;149:147.
Sharma N, Acharya S, Kumar K, Singh N, Chaurasia O. Hydroponics as an advanced technique for vegetable production: an overview. J Soil Water Conserv. 2018;17(4):364–71.
Maggini R, Kiferle C, Pardossi A. Hydroponic production of medicinal plants. Medicinal plants: antioxidant properties, traditional uses and conservation strategies. Hauppauge: Nova Science Publishers Inc; 2014. p. 91–116.
Nwafor I, Nwafor C, Manduna I. Constraints to cultivation of medicinal plants by smallholder farmers in South Africa. Horticulturae. 2021;7(12):531.
Sambo P, Nicoletto C, Giro A, Pii Y, Valentinuzzi F, Mimmo T, et al. Hydroponic solutions for soilless production systems: issues and opportunities in a smart agriculture perspective. Front Plant Sci. 2019;10:923.
Izquierdo J. editor Simplified hydroponics: a tool for food security in Latin America and the Caribbean. Int Conf Exhib Soil Cult: ICESC. 2005;2005:742.
Carrasco G, Manríquez P, Galleguillos F, Fuentes-Peñailillo F, Urrestarazu M, editors. Evolution of soilless culture in Chile. III International Symposium on Soilless Culture and Hydroponics: Innovation and Advanced Technology for Circular Horticulture 1321; 2021.
Noe N, Lehmann J. Prelude medicinal plants. Belgian Biodiversity Platform. Database. 2012.
Hoffman M, Koenig K, Bunting G, Costanza WJ. Biodiversity Hotspots (version 2016.1). 2016.
Acknowledgements
We would like to thank David Tyler for helpful comments on the manuscript, and Jason Tyler and Renee Tyler for assistance with preparation of the manuscript. We also thank Elaine Dodsworth for technical advice.
Author information
Authors and Affiliations
Contributions
ST designed the study and wrote the manuscript. LT performed the RStudio graphics mapping and contributed to the writing of the manuscript. Both the authors have read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1.
Table S1. An ethnomedical toolkit.
Additional file 2.
Table S2. List of species with ethnomedical use of neurodegenerative disease therapeutic potential.
Additional file 3.
Table S3. Bioactivities listed by species.
Additional file 4.
Table S4. Bioactivities listed by category.
Additional file 5.
Table S5. Phytochemicals with anti-amyloid and tau activity.
Additional file 6.
Table S6. Examples of plants with activity against infectious agents implicated in Alzheimer’s disease.
Additional file 7.
Table S7. Plants with ethnological reports of memory improvement demonstrating bioactivities of therapeutic relevance to 15 causal hypotheses for AD.
Additional file 8.
Table S1–S7. References.
Additional file 9.
File S1. Materials and Methods further details.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tyler, S.E.B., Tyler, L.D.K. Therapeutic roles of plants for 15 hypothesised causal bases of Alzheimer’s disease. Nat. Prod. Bioprospect. 12, 34 (2022). https://doi.org/10.1007/s13659-022-00354-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s13659-022-00354-z