Abstract
Background
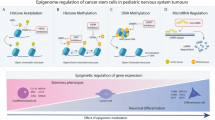
Epigenetic alterations are inherent to cancer cells, and epigenetic drugs are currently primarily used to treat hematological malignancies. Pediatric neuro-ectodermal tumors originate from neural crest cells and also exhibit epigenetic alterations involving e.g. apoptotic pathways, which suggests that these tumors may also be sensitive to epigenetic drugs. This notion prompted us to assess molecular and functional effects of low dosage epigenetic drugs in neuro-ectodermal tumor-derived cell lines of pediatric origin.
Results
In 17 neuroblastoma (NBL) and 5 peripheral primitive neuro-ectodermal tumor (PNET) cell lines a combination treatment of 5-aza-2′-deoxycytidine (DAC) and Trichostatin A (TSA) at nanomolar dosages was found to reduce proliferation and to induce wide-spread DNA demethylation, accompanied by major changes in gene expression profiles. Approximately half of the genes that were significantly up-regulated upon treatment exhibited a significant demethylation in their promoter regions. In the NBL cell lines, almost every cellular pathway (193/200) investigated showed expression alterations after treatment, especially a marked up-regulation of genes in the p53 pathway. The combination treatment also resulted in up-regulation of known epigenetically regulated genes such as X-chromosomal genes, tissue-specific genes and a limited number of imprinted genes, as well as known tumor suppressor genes and oncogenes.
Conclusions
Nanomolar dosages of epigenetic drugs have a dramatic impact on the genomes of neuro-ectodermal tumor-derived cell lines, including alterations in DNA methylation and concomitant alterations in gene expression.


Similar content being viewed by others
Abbreviations
- DAC:
-
5-aza-2′-deoxycytidine
- DMH:
-
differential methylation hybridization
- HDACi:
-
histone deacetylase inhibitor
- MDS:
-
myelodysplastic syndrome
- NBL:
-
neuroblastoma
- NMA:
-
MYCN amplified
- PNET:
-
primitive neuro-ectodermal tumor
- PRC2:
-
polycomb receptor complex 2
- TSA:
-
trichostatin A
- ZEB:
-
zebularine
References
S.B. Baylin, P.A. Jones, A decade of exploring the cancer epigenome - biological and translational implications. Nat Rev Cancer 11(10), 726–734 (2011)
A.P. Feinberg, B. Tycko, The history of cancer epigenetics. Nat Rev Cancer 4(2), 143–153 (2004)
J.P. Issa, H.M. Kantarjian, Targeting DNA methylation. Clin Cancer Res 15(12), 3938–3946 (2009)
R.L. Piekarz, S.E. Bates, Epigenetic modifiers: basic understanding and clinical development. Clin Cancer Res 15(12), 3918–3926 (2009)
H.M. Prince, M.J. Bishton, S.J. Harrison, Clinical studies of histone deacetylase inhibitors. Clin Cancer Res 15(12), 3958–3969 (2009)
G. Chai, L. Li, W. Zhou, L. Wu, Y. Zhao, D. Wang, S. Lu, Y. Yu, H. Wang, M.A. McNutt, Y.G. Hu, Y. Chen, Y. Yang, X. Wu, G.A. Otterson, W.G. Zhu, HDAC inhibitors act with 5-aza-2'-deoxycytidine to inhibit cell proliferation by suppressing removal of incorporated abases in lung cancer cells. PLoS One 3(6), e2445 (2008)
M. Dickinson, R.W. Johnstone, H.M. Prince, Histone deacetylase inhibitors: potential targets responsible for their anti-cancer effect. Invest New Drugs 28(Suppl 1), S3–20 (2010)
N. Steele, P. Finn, R. Brown, J.A. Plumb, Combined inhibition of DNA methylation and histone acetylation enhances gene re-expression and drug sensitivity in vivo. Br J Cancer 5, 758–763 (2009)
M. Bishton, M. Kenealy, R. Johnstone, W. Rasheed, H.M. Prince, Epigenetic targets in hematological malignancies: combination therapies with HDACis and demethylating agents. Expert Rev Anticancer Ther 7(10), 1439–1449 (2007)
W. Blum, R.B. Klisovic, B. Hackanson, Z. Liu, S. Liu, H. Devine, T. Vukosavljevic, L. Huynh, G. Lozanski, C. Kefauver, C. Plass, S.M. Devine, N.A. Heerema, A. Murgo, K.K. Chan, M.R. Grever, J.C. Byrd, G. Marcucci, Phase I study of decitabine alone or in combination with valproic acid in acute myeloid leukemia. J Clin Oncol 25(25), 3884–3891 (2007)
M. Bots, R.W. Johnstone, Rational combinations using HDAC inhibitors. Clin Cancer Res 15(12), 3970–3977 (2009)
G. Garcia-Manero, H.M. Kantarjian, B. Sanchez-Gonzalez, H. Yang, G. Rosner, S. Verstovsek, M. Rytting, W.G. Wierda, F. Ravandi, C. Koller, L. Xiao, S. Faderl, Z. Estrov, J. Cortes, S. O'Brien, E. Estey, C. Bueso-Ramos, J. Fiorentino, E. Jabbou, J.P. Issa, Phase 1/2 study of the combination of 5-aza-2'-deoxycytidine with valproic acid in patients with leukemia. Blood 108(10), 3271–3279 (2006)
R.W. Johnstone, Histone-deacetylase inhibitors: novel drugs for the treatment of cancer. Nat Rev Drug Discov 1(4), 287–299 (2002)
A. Insinga, S. Minucci, P.G. Pelicci, Mechanisms of selective anticancer action of histone deacetylase inhibitors. Cell Cycle 4(6), 741–743 (2005)
A. Insinga, S. Monestiroli, S. Ronzoni, V. Gelmetti, F. Marchesi, A. Viale, L. Altucci, C. Nervi, S. Minucci, P.G. Pelicci, Inhibitors of histone deacetylases induce tumor-selective apoptosis through activation of the death receptor pathway. Nat Med 11(1), 71–76 (2005)
P. Marks, R.A. Rifkind, V.M. Richon, R. Breslow, T. Miller, W.K. Kelly, Histone deacetylases and cancer: causes and therapies. Nat Rev Cancer 1(3), 194–202 (2001)
J. E. Fraczek, M. Vinken, D. Tourwe, T. Vanhaecke,V. Rogiers, Synergetic effects of DNA demethylation and histone deacetylase inhibition in primary rat hepatocytes. Invest New Drugs (2011)
F. Lyko, R. Brown, DNA methyltransferase inhibitors and the development of epigenetic cancer therapies. J Natl Cancer Inst 97(20), 1498–1506 (2005)
H.C. Tsai, H. Li, L. Van Neste, Y. Cai, C. Robert, F.V. Rassool, J.J. Shin, K.M. Harbom, R. Beaty, E. Pappou, J. Harris, R.W. Yen, N. Ahuja, M.V. Brock, V. Stearns, D. Feller-Kopman, L.B. Yarmus, D. Feller-Kopman, L.B. Yarmus, Y.C. Lin, A.L. Welm, J.P. Issa, I. Minn, W. Matsui, Y.Y. Jang, S.J. Sharkis, S.B. Baylin, C.A. Zahnow, Transient low doses of DNA-demethylating agents exert durable antitumor effects on hematological and epithelial tumor cells. Cancer Cell 21(3), 430–446 (2012)
J. Lopez, M. Percharde, H.M. Coley, A. Webb, T. Crook, The context and potential of epigenetics in oncology. Br J Cancer 4, 571–577 (2009)
T. Qin, J. Jelinek, J. Si, J. Shu, J.P. Issa, Mechanisms of resistance to 5-aza-2'-deoxycytidine in human cancer cell lines. Blood 113(3), 659–667 (2009)
T. Qin, E.M. Youssef, J. Jelinek, R. Chen, A.S. Yang, G. Garcia-Manero, J.P. Issa, Effect of cytarabine and decitabine in combination in human leukemic cell lines. Clin Cancer Res 13(14), 4225–4232 (2007)
E.E. Cameron, K.E. Bachman, S. Myohanen, J.G. Herman, S.B. Baylin, Synergy of demethylation and histone deacetylase inhibition in the re-expression of genes silenced in cancer. Nat Genet 21(1), 103–107 (1999)
O. Galm, J.G. Herman, S.B. Baylin, The fundamental role of epigenetics in hematopoietic malignancies. Blood Rev 20(1), 1–13 (2006)
T.J. Walton, G. Li, R. Seth, S.E. McArdle, M.C. Bishop, R.C. Rees, DNA demethylation and histone deacetylation inhibition co-operate to re-express estrogen receptor beta and induce apoptosis in prostate cancer cell-lines. Prostate 68(2), 210–222 (2008)
H.C. Tsai, S.B. Baylin, Cancer epigenetics: linking basic biology to clinical medicine. Cell Res 21(3), 502–517 (2011)
C.D. Margetts, M. Morris, D. Astuti, D.C. Gentle, A. Cascon, F.E. McRonald, D. Catchpoole, M. Robledo, H.P. Neumann, F. Latif, E.R. Maher, Evaluation of a functional epigenetic approach to identify promoter region methylation in phaeochromocytoma and neuroblastoma. Endocr Relat Cancer 15(3), 777–786 (2008)
B. Banelli, I. Gelvi, A. Di Vinci, P. Scaruffi, I. Casciano, G. Allemanni, S. Bonassi, G.P. Tonini, M. Romani, Distinct CpG methylation profiles characterize different clinical groups of neuroblastic tumors. Oncogene 24(36), 5619–5628 (2005)
J. Hoebeeck, E. Michels, F. Pattyn, V. Combaret, J. Vermeulen, N. Yigit, C. Hoyoux, G. Laureys, A. De Paepe, F. Speleman, J. Vandesompele, Aberrant methylation of candidate tumor suppressor genes in neuroblastoma. Cancer Lett 273(2), 336–346 (2009)
K. Harada, S. Toyooka, A. Maitra, R. Maruyama, K.O. Toyooka, C.F. Timmons, G.E. Tomlinson, D. Mastrangelo, R.J. Hay, J.D. Minna, A.F. Gazdar, Aberrant promoter methylation and silencing of the RASSF1A gene in pediatric tumors and cell lines. Oncogene 21(27), 4345–4349 (2002)
M. Abe, M. Ohira, A. Kaneda, Y. Yagi, S. Yamamoto, Y. Kitano, T. Takato, A. Nakagawara, T. Ushijima, CpG island methylator phenotype is a strong determinant of poor prognosis in neuroblastomas. Cancer Res 65(3), 828–834 (2005)
T. Teitz, T. Wei, M.B. Valentine, E.F. Vanin, J. Grenet, V.A. Valentine, F.G. Behm, A.T. Look, J.M. Lahti, V.J. Kidd, Caspase 8 is deleted or silenced preferentially in childhood neuroblastomas with amplification of MYCN. Nat Med 6(5), 529–535 (2000)
P. Gonzalez-Gomez, M.J. Bello, J. Lomas, D. Arjona, M.E. Alonso, C. Aminoso, I. Lopez-Marin, N.P. Anselmo, J.L. Sarasa, M. Gutierrez, C. Casartelli, J.A. Rey, Aberrant methylation of multiple genes in neuroblastic tumours. relationship with MYCN amplification and allelic status at 1p. Eur J Cancer 39(10), 1478–1485 (2003)
A. Decock, M. Ongenaert, J. Vandesompele, F. Speleman, Neuroblastoma epigenetics: From candidate gene approaches to genome-wide screenings. Epigenetics 6(8), 962–970 (2011)
M.M. van Noesel, S. van Bezouw, G.S. Salomons, P.A. Voute, R. Pieters, S.B. Baylin, J.G. Herman, R. Versteeg, Tumor-specific down-regulation of the tumor necrosis factor-related apoptosis-inducing ligand decoy receptors DcR1 and DcR2 is associated with dense promoter hypermethylation. Cancer Res 62(7), 2157–2161 (2002)
M.M. van Noesel, S. van Bezouw, P.A. Voute, J.G. Herman, R. Pieters, R. Versteeg, Clustering of hypermethylated genes in neuroblastoma. Genes Chromosomes Cancer 38(3), 226–233 (2003)
H. Caren, A. Djos, M. Nethander, R. M. Sjoberg, P. Kogner, C. Enstrom, S. Nilsson,T. Martinsson, Identification of epigenetically regulated genes that predict patient outcome in neuroblastoma. BMC Cancer. 11:(1): p. 66 (
P. G. Buckley, S. Das, K. Bryan, K. M. Watters, L. Alcock, J. Koster, R. Versteeg,R. L. Stallings, Genome-wide DNA methylation analysis of neuroblastic tumors reveals clinically relevant epigenetic events and large-scale epigenomic alterations localized to telomeric regions. Int J Cancer (
D.M. Murphy, P.G. Buckley, K. Bryan, S. Das, L. Alcock, N.H. Foley, S. Prenter, I. Bray, K.M. Watters, D. Higgins, R.L. Stallings, Global MYCN transcription factor binding analysis in neuroblastoma reveals association with distinct E-box motifs and regions of DNA hypermethylation. PLoS One 4(12), e8154 (2009)
M. Berdasco, S. Ropero, F. Setien, M.F. Fraga, P. Lapunzina, R. Losson, M. Alaminos, N.K. Cheung, N. Rahman, M. Esteller, Epigenetic inactivation of the Sotos overgrowth syndrome gene histone methyltransferase NSD1 in human neuroblastoma and glioma. Proc Natl Acad Sci USA 106(51), 21830–21835 (2009)
Y. Sugino, A. Misawa, J. Inoue, M. Kitagawa, H. Hosoi, T. Sugimoto, I. Imoto, J. Inazawa, Epigenetic silencing of prostaglandin E receptor 2 (PTGER2) is associated with progression of neuroblastomas. Oncogene 26(53), 7401–7413 (2007)
R.E. George, J.M. Lahti, P.C. Adamson, K. Zhu, D. Finkelstein, A.M. Ingle, J.M. Reid, M. Krailo, D. Neuberg, S.M. Blaney, L. Diller, Phase I study of decitabine with doxorubicin and cyclophosphamide in children with neuroblastoma and other solid tumors: a Children's Oncology Group study. Pediatr Blood Cancer 55(4), 629–638 (2010)
A. Aparicio, C.A. Eads, L.A. Leong, P.W. Laird, E.M. Newman, T.W. Synold, S.D. Baker, M. Zhao, J.S. Weber, Phase I trial of continuous infusion 5-aza-2'-deoxycytidine. Cancer Chemother Pharmacol 51(3), 231–239 (2003)
H. Kantarjian, Y. Oki, G. Garcia-Manero, X. Huang, S. O'Brien, J. Cortes, S. Faderl, C. Bueso-Ramos, F. Ravandi, Z. Estrov, A. Ferrajoli, W. Wierda, J. Shan, J. Davis, F. Giles, H.I. Saba, J.P. Issa, Results of a randomized study of 3 schedules of low-dose decitabine in higher-risk myelodysplastic syndrome and chronic myelomonocytic leukemia. Blood 109(1), 52–57 (2007)
A. Thibault, W.D. Figg, R.C. Bergan, R.M. Lush, C.E. Myers, A. Tompkins, E. Reed, D. Samid, A phase II study of 5-aza-2'deoxycytidine (decitabine) in hormone independent metastatic (D2) prostate cancer. Tumori 84(1), 87–89 (1998)
W. D. Johnson, A pharmacokinetic/pharmacodynamic approach to evaluating the safety of zebularine in non-human primates Proc Amer Assoc Cancer Res. 47: (2006)
J.L. Holleran, R.A. Parise, E. Joseph, J.L. Eiseman, J.M. Covey, E.R. Glaze, A.V. Lyubimov, Y.F. Chen, D.Z. D'Argenio, M.J. Egorin, Plasma pharmacokinetics, oral bioavailability, and interspecies scaling of the DNA methyltransferase inhibitor, zebularine. Clin Cancer Res 11(10), 3862–3868 (2005)
S. Shichijo, A. Yamada, K. Sagawa, O. Iwamoto, M. Sakata, K. Nagai, K. Itoh, Induction of MAGE genes in lymphoid cells by the demethylating agent 5-aza-2'-deoxycytidine. Jpn J Cancer Res 87(7), 751–756 (1996)
F. Condorelli, I. Gnemmi, A. Vallario, A.A. Genazzani, P.L. Canonico, Inhibitors of histone deacetylase (HDAC) restore the p53 pathway in neuroblastoma cells. Br J Pharmacol 153(4), 657–668 (2008)
C. De Smet, C. Lurquin, B. Lethe, V. Martelange, T. Boon, DNA methylation is the primary silencing mechanism for a set of germ line- and tumor-specific genes with a CpG-rich promoter. Mol Cell Biol 19(11), 7327–7335 (1999)
P.G. Buckley, S. Das, K. Bryan, K.M. Watters, L. Alcock, J. Koster, R. Versteeg, R.L. Stallings, Genome-wide DNA methylation analysis of neuroblastic tumors reveals clinically relevant epigenetic events and large-scale epigenomic alterations localized to telomeric regions. Int J Cancer 128(10), 2296–2305 (2011)
V. M. Komashko,P. J. Farnham, 5-azacytidine treatment reorganizes genomic histone modification patterns. Epigenetics. 5:(3): (2010)
Y. Gomyo, J. Sasaki, C. Branch, J.A. Roth, T. Mukhopadhyay, 5-aza-2'-deoxycytidine upregulates caspase-9 expression cooperating with p53-induced apoptosis in human lung cancer cells. Oncogene 23(40), 6779–6787 (2004)
M.S. Soengas, P. Capodieci, D. Polsky, J. Mora, M. Esteller, X. Opitz-Araya, R. McCombie, J.G. Herman, W.L. Gerald, Y.A. Lazebnik, C. Cordon-Cardo, S.W. Lowe, Inactivation of the apoptosis effector Apaf-1 in malignant melanoma. Nature 409(6817), 207–211 (2001)
W.G. Zhu, Z. Dai, H. Ding, K. Srinivasan, J. Hall, W. Duan, M.A. Villalona-Calero, C. Plass, G.A. Otterson, Increased expression of unmethylated CDKN2D by 5-aza-2'-deoxycytidine in human lung cancer cells. Oncogene 20(53), 7787–7796 (2001)
A. Doi, I.H. Park, B. Wen, P. Murakami, M.J. Aryee, R. Irizarry, B. Herb, C. Ladd-Acosta, J. Rho, S. Loewer, J. Miller, T. Schlaeger, G.Q. Daley, A.P. Feinberg, Differential methylation of tissue- and cancer-specific CpG island shores distinguishes human induced pluripotent stem cells, embryonic stem cells and fibroblasts. Nat Genet 41(12), 1350–1353 (2009)
A. Meissner, T.S. Mikkelsen, H. Gu, M. Wernig, J. Hanna, A. Sivachenko, X. Zhang, B.E. Bernstein, C. Nusbaum, D.B. Jaffe, A. Gnirke, R. Jaenisch, E.S. Lander, Genome-scale DNA methylation maps of pluripotent and differentiated cells. Nature 454(7205), 766–770 (2008)
R. Lister, M. Pelizzola, R.H. Dowen, R.D. Hawkins, G. Hon, J. Tonti-Filippini, J.R. Nery, L. Lee, Z. Ye, Q.M. Ngo, L. Edsall, J. Antosiewicz-Bourget, R. Stewart, V. Ruotti, A.H. Millar, J.A. Thomson, B. Ren, J.R. Ecker, Human DNA methylomes at base resolution show widespread epigenomic differences. Nature 462(7271), 315–322 (2009)
E.M. Klenova, H.C. Morse 3rd, R. Ohlsson, V.V. Lobanenkov, The novel BORIS + CTCF gene family is uniquely involved in the epigenetics of normal biology and cancer. Semin Cancer Biol 12(5), 399–414 (2002)
S. Vatolin, Z. Abdullaev, S.D. Pack, P.T. Flanagan, M. Custer, D.I. Loukinov, E. Pugacheva, J.A. Hong, H. Morse 3rd, D.S. Schrump, J.I. Risinger, J.C. Barrett, V.V. Lobanenkov, Conditional expression of the CTCF-paralogous transcriptional factor BORIS in normal cells results in demethylation and derepression of MAGE-A1 and reactivation of other cancer-testis genes. Cancer Res 65(17), 7751–7762 (2005)
R. Ohlsson, R. Renkawitz, V. Lobanenkov, CTCF is a uniquely versatile transcription regulator linked to epigenetics and disease. Trends Genet 17(9), 520–527 (2001)
A. Woloszynska-Read, S.R. James, C. Song, B. Jin, K. Odunsi, A.R. Karpf, BORIS/CTCFL expression is insufficient for cancer-germline antigen gene expression and DNA hypomethylation in ovarian cell lines. Cancer Immun 10(6) (2010)
J.P. Issa, G. Garcia-Manero, F.J. Giles, R. Mannari, D. Thomas, S. Faderl, E. Bayar, J. Lyons, C.S. Rosenfeld, J. Cortes, H.M. Kantarjian, Phase 1 study of low-dose prolonged exposure schedules of the hypomethylating agent 5-aza-2'-deoxycytidine (decitabine) in hematopoietic malignancies. Blood 103(5), 1635–1640 (2004)
Acknowledgments
We would like to thank Judith Boer and Maarten van Iterson for their help in normalization of the CpG island methylation array data and their input in discussions on data analysis. This work was funded by the Dutch Neuroblastoma Foundation Villa Joep, the Dutch Cancer Society and the ODAS foundation (The Netherlands).
Conflict of interest
We have no conflict of interest or financial conflict to disclose.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary materials
Below is the link to the electronic supplementary material.
Supplementary Figure 1
(Figure made available from previously published paper; Iterson et al. 2012 SAGMB, publisher De Gruyter) Schematic Differential methylation and Hybridization (DMH) protocol Protocol for enrichment of methylated DNA fragments, which also enriches for fragments without methylation sensitive restriction sites. (DOCX 1061 kb)
Supplementary Figure 2
(Figures made available from previously published paper; Iterson et al. 2012 SAGMB, publisher De Gruyter) MA-plots for six cell lines with weighted P-spline curves using different weights (invariant probes in black). The blue curve is a normal normalization obtained without any weights, the red curve is mainly based on the invariant probes with a high weight for the invariant probes (weight=10.000) versus all the other probes (w=1), and the yellow curve is an intermediate with an equal total weight of all the invariant probes (weight=250) versus all the other probes (weight =1). The yellow curve was chosen for normalization purposes because it also covers the high intensity range where no or little invariant probes are present. (DOCX 128 kb)
Supplementary Figure 3
(Figure made available from previously published paper; Iterson et al. 2012 SAGMB, publisher De Gruyter): MA-plots before and after normalization for a single cell line (treated and untreated, invariant probes in black). The upper panel shows raw data with normal P-spline and equally weighted P-spline curves respectively in green and red. The middle panels shows normal P-spline normalized data and the lower panels the weighted P-spline normalization data. The chosen equally weighted p-spline normalization method creates quite similarly-shaped curves compared with normal normalization methods. (DOCX 72 kb)
Supplementary Figure 4
Methylation ratios all cell lines before and after normalization. Box and whisker plots displaying the distribution of methylation levels (2log ratios) of all neuro-ectodermal cell line pairs. On the x-axis, untreated (U) and treated (T) cell line pairs are displayed. Panel A and B show the unnormalized data in which a clear shift towards lower methylation levels for treated cell lines is observed in each treatment pair. Panel C and D show the lowess normalized data that results in the loss of demethylating effects due to signal scaling. Panel E and F show normalized data using the weighed P-spline normalization method that is based on methylation independent control probes as used throughout the further article (Iterson 2012, SAGMB). This method removed the technical noise, while retaining the demethylating treatment effect. X-axis: cell line pairs from left to right NMB, SK-N-MC, CHP-100, SH-SY5Y, LAN-5, KCNR, TR-14, IMR-32, SK-N-DW, SJNB-8, AMC-106c, TC-32, SK-N-SH, SJNB-1, SH-EP-21N/tet2/N, SK-N-BE, SK-N-AS, NGP-C4, SH-EP-2/tet2, GI-M-EN, SJNB-10, CB-AGPN. (DOCX 623 kb)
Supplementary Figure 5
Upregulation of TNFRSF25 mRNA expression after epigenetic treatment. Light grey: non-MYCN amplified (NMA-) cell line SK-N-AS. Dark grey: NMA+ cell line IMR-32. On theX-axis it is indicated which single or combination drug treatment was used. The Y-axis shows the fold of expression change of TNFRSF25 compared with the untreated control. Mi = methylation inhibitor; HDACi = histone deacetylase inhibitor. Concentrations drugs used: Decitabine 7.5 μM in SK-N-AS (+/- IC50) and 50nM in IMR-32 (+/- IC50). Zebularine 60 μM (+/- IC50), FK228 1.5nM (+/- IC50), TSA 100 nM (+/- IC50). (DOCX 64 kb)
Supplementary Figure 6
Limiting dilution approach for identification of the optimal concentration of DAC and TSA. TAQMAN analysis for the TNFRSF25 gene was performed in 7 NBL and 1 PNET line with increasing concentrations of DAC and TSA. For each drug combination, numbers refer to the fold upregulation of TNFRSF25 gene expression compared with the untreated cell line or lowest treatment concentration if the value of the untreated sample is missing. Whereas colors refer to an estimation of cell viability as deduced from absolute GAPDH levels. (DOCX 660 kb)
Supplementary Figure 7
Upregulation of TNFRSF10C (A), TNFRSF10D (B) and RASSF1A (C) mRNA expression after epigenetic treatment. On the x-axis the different cell lines with in white, the MYCN amplified (NMA) NBL cell lines, in dark grey the non-NMA cell lines and in light grey the PNET cell lines. On the y-axis the fold change of mRNA expression after treatment with DAC and TSA. Most consistently upregulated cell lines across the different genes: SH-EP-21N, SH-SY5Y, NMB, SK-N-AS. (DOCX 65 kb)
Supplementary Figure 8
Cell cycle distribution in four cell lines. A. IMR-32, B. NMB, C. GI-M-EN, D. CHP-100)) with and without DAC 30nM and TSA 25nM pre-treatment. The PI signal is shown on the x-axis and the cell count on the y-axis. In CHP-100 a small shift from G2 to G0-G1 stage has been shown without changes in the other cell lines. Cell line SK-N-MC missing due to a lack of material. (DOCX 183 kb)
Supplementary Figure 9
PI-Annexin measurement of apoptosis in all cell lines. On the Y-axis the signal for annexin IV (apoptosis marker), on the Y-axis PI staining (marker necrosis/membrane permeability). No large shifts noted. (DOCX 376 kb)
Supplementary Figure 10
Cell viability (triplicate measurements) in response to Vincristin and Doxorubicin with and without DAC 30nM and TSA 25nM pre-treatment. On the X- axis accumulating dosages of drugs (10log scale), on the y-axis cell viability. Vincristin sensitivity seems to be enhanced at low concentrations after DAC and TSA pre-treatment in NMB, no other effects noted. (DOCX 106 kb)
Supplementary Figure 11
Principle component analysis based on expression array probesets. Unsupervised principal component analyses of expression array data using all probe sets (left panel) and most variant probe sets (right panel, n=236 with variance >3). Green, PNETs; Blue, NBL non-NMA; Red, NBL NMA; Purple, SHEP-21N (MYCN transvectant). (DOCX 81 kb)
Supplementary Figure 12
Validation of upregulation of epigenetically regulated genes after DAC and TSA. Confirmation array expression changes tissue specific genes (DDR1 and DAZL) and X-chromosomal genes (XIST and ACRC) by RT-QPCR. The cell lines that did not show upregulation of XIST (within oval) were all female cell lines. These cell lines already had high XIST expression before treatment. Cluster 2 consists of non-MYCN amplified NBL cell lines GI-M-EN, SK-N-AS, SH-EP-2, and SH-EP-21N, while cluster 3 consists of all other NBL cell lines, which are mostly MYCN amplified. (DOCX 61 kb)
Supplementary Figure 13
Upregulation TP53 after DAC and TSA treatment. Western blot p53 protein expression, showing upregulated expression of p53 after DAC and TSA treatment for NMB, SJNB8 (in short SJ8) and AMC106c (in short AMC). U, untreated; T, treated. (DOCX 36 kb)
Supplementary Methods
(DOCX 15 kb)
Supplementary Tables
(DOCX 105 kb)
Rights and permissions
About this article
Cite this article
Duijkers, F.A., de Menezes, R.X., Goossens-Beumer, I.J. et al. Epigenetic drug combination induces genome-wide demethylation and altered gene expression in neuro-ectodermal tumor-derived cell lines. Cell Oncol. 36, 351–362 (2013). https://doi.org/10.1007/s13402-013-0140-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13402-013-0140-x