Abstract
Objective
To evaluate the short term clinical effects of delayed cord clamping in preterm neonates.
Design
Randomized controlled trial.
Setting
A tertiary care neonatal unit from October 2013 to September 2014.
Participants
78 mothers with preterm labor between 27 to 316/7 weeks gestation.
Intervention
Early cord clamping (10 s), delayed cord clamping (60 s) or delayed cord clamping (60 s) along with intramuscular ergometrine (500 μg) administered to the mother.
Main outcome measures
Primary: hematocrit at 4 h after birth; Secondary: temperature on admission in neonatal intensive care unit, blood pressure (non-invasive) at 12 h, and urinary output for initial 72 h.
Results
Mean (SD) hematocrit at 4 h of birth was 58.9 (2.4)% in delayed cord clamping group, and 58.7 (2.1)% in delayed cord clamping with ergometrine group as compared to 47.6 (1.3)% in early cord clamping group. Mean (SD) temperature on admission in NICU was 35.8 (0.2)ºC, 35.8 (0.3)ºC, and 35.5 (0.3)ºC, respectively in these three groups. The mean (SD) non-invasive blood pressure at 12 h of birth was 45.8 (7.0) mmHg, 45.8 (9.0) mmHg, and 35.5 (8.6) mmHg, respectively in these three groups. Mean (SD) urinary output on day 1 of life was 1.1 (0.2) mL/kg/h, 1.1 (0.2) mL/kg/hr and 0.9 (0.2) ml/kg/h, respectively.
Conclusion
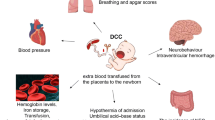
In preterm neonates delayed cord clamping along with lowering the infant below perineum or incision site and administration of ergometrine to mother has significant benefits in terms of increase in hematocrit, higher temperature on admission, and higher blood pressure and urinary output during perinatal transition.
Similar content being viewed by others
References
Van Rheenen P, De Moor L, Eschbach S, De Grooth H, Brabin B. Delayed cord clamping and haemoglobin levels in infancy: A randomised controlled trial in term babies. Trop Med Int Health. 2007;12:603–16.
Farrar D, Tuffnell D, Airey R, Duley L. Care during the third stage of labour: A postal survey of UK midwives and obstetricians. BMC Pregnancy Childbirth. 2010;10:23.
Tarnow-Mordi WO, Duley L, Field D, Marlow N, Morris J, Newnham J, et al. Timing of cord clamping in very preterm infants: More evidence is needed. Am J Obstet Gynecol. 2014;211:118–23.
Yao AC, Moinian M, Lind J. Distribution of blood between the infant and the placenta after birth. Lancet. 1969;7626:871–3.
Lindercamp O, Nelle KM, Zilow EP. The effect of early and late cord clamping on blood viscosity and other hemorheological parameters in full term neonates. Acta Paediatrica. 1992;81:45–750.
Obladen M, Diepold K, Maier RF. The European Multicentre rhEPO study group: Venous and arterial haematological profiles of very low birth weight infants. Pediatrics. 2000;106:707–9.
Rabe H, Diaz-Rossello JL, Duley L, Dowswell T. Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. Cochrane Database Syst Rev. 2012:8:CD003248.
Ibrahim HM, Krouskop RW, Lewis DF, Dhanireddy R. Placental transfusion: Umbilical cord clamping and preterm infants. J Perinatol. 2000;20:351–4.
Oh W, Fanaroff AA, Carlo WA, Donovan EF, McDonald SA, Poole WK. Effects of delayed cord clamping in very low birth weight infants. J Perinatol. 2011;31:568–71.
McDonnell M, Henderson-Smart DJ. Delayed umbilical cord clamping in preterm infants: a feasibility study. J Paediatr Child Health. 1997;33:308–10.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dipak, N.K., Nanavati, R.N., Kabra, N.K. et al. Effect of delayed cord clamping on hematocrit, and thermal and hemodynamic stability in preterm neonates: A randomized controlled trial . Indian Pediatr 54, 112–115 (2017). https://doi.org/10.1007/s13312-017-1011-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-017-1011-8