Abstract
Objective
To apply cumulative sum (CUSUM) to monitor a drug trial of nebulized hypertonic-saline in bronchiolitis. To test if monitoring with CUSUM control lines is practical and useful as a prompt to stop the drug trial early, if the study drug performs significantly worse than the comparator drug.
Design
Prospective, open label, controlled trial using standard therapy (epinephrine) and study drug (hypertonic-saline) sequentially in two groups of patients.
Setting
Hospital offering tertiary-level pediatric care.
Patients
Children, 2 months to 2 years, with first episode of bronchiolitis, excluding those with cardiac disease, immunodeficiency and critical illness at presentation.
Interventions
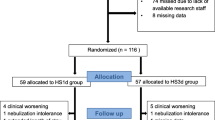
Nebulized epinephrine in first half of the bronchiolitis season (n = 35) and hypertonic saline subsequently (n = 29). Continuous monitoring of response to hypertonic-saline using CUSUM control-charts developed with epinephrine-response data.
Main outcome measures
Clinical score, tachycardia and total duration of hospital stay.
Results
In the epinephrine group, the maximum CUSUM was +2.25 (SD 1.34) and minimum CUSUM was −2.26 (SD 1.34). CUSUM score with hypertonic-saline group stayed above the zero line throughout the study.
There was no statistical difference in the post-treatment clinical score at 24 hours between the treatment groups {Mean (SD) 3.516 (2.816): 3.552 (2.686); 95% CI: −1.416 to + 1.356}, heart rate {Mean (SD) 136 (44): 137(12); 95% CI: −17.849 to +15.849) or duration of hospital stay (Mean (SD) 96.029 (111.41): 82.914 (65.940); 95% CI: −33.888 to +60.128}.
Conclusions
The software we developed allows for drawing of control lines to monitor study drug performance. Hypertonic-saline performed as well or better than nebulized epinephrine in bronchiolitis.
Similar content being viewed by others
References
Mandelberg A, Tal G, Witzling M, Someck E, Houri S, Balin A, et al. Nebulized 3% hypertonic saline solution treatment in hospitalized infants with viral bronchiolitis. Chest. 2003;123:481–487.
Tal G, Cesar K, Oron A, Houri S, Ballin A, Mandelberg A. Hypertonic saline/epinephrine treatment in hospitalized infants with viral bronchiolitis reduces hospitalization stay: 2 years experience. Isr Med Assoc J. 2006;8:169–173.
Wark PA, McDonald V. Nebulized hypertonic saline for cystic fibrosis. Cochrane Database Syst Rev. 2000;2:CD001506.
Mandelberg A, Amirav I. Hypertonic saline or high volume normal saline for viral bronchiolitis: mechanisms and rationale. Pediatr Pulmonol. 2010;451:36–40.
Zhang L, Mendoza-Sassi RA, Wainwright C, Klassen TP. Nebulized hypertonic saline solution for acute bronchiolitis in infants. Cochrane Database Syst Rev. 2008;4:CD006458.
Mathew JL. What works in bronchiolitis? Indian Pediatr. 2009;46:154–158.
McCulloch P, Taylor I, Sasako M, Lovett B, Griffin D. Randomised trials in surgery: problems and possible solutions. BMJ. 2002;324:1448–1451.
Yeung V. Clinical trials in children. In: Pediatric Drug Handling. Available from. http://www.pharmpress.com/shop/samples/paeditaric_sample_chapter.pdf. Accessed October 12, 2009.
Taylor WA. Change-Point Analysis: A Powerful New Tool for Detecting Changes. Available from: URL. http://www.variation.com/cpa/tech/changepoint.html. Accessed October 11, 2009.
Kinsey SE, Giles FJ, Holton J. Cusum plotting of temperature charts for assessing antimicrobial treatment in neutropenic patients. BMJ. 1989;299:775–776.
Ravn LI, Sprehn M, Pedersen CB. The Cusum score. A tool for evaluation of clinical competence. Ugeskr Laeger. 2001;163:3644–3648.
Watkins RE, Eagleson S, Veenendaal B, Wright G, Plant AJ. Applying cusum-based methods for the detection of outbreaks of Ross River virus disease in Western Australia. BMC Med Inform Decis Mak. 2008;8:37.
Uyan AP, Ozyurek H, Keskin M, Afsar Y, Yilmaz E. Comparison of two different bronchodilators in the treatment of acute bronchiolitis. Internet Journal of Pediatrics and Neonatology. 2003;3;1.
Beck R, Elias N, Shoval S, Tov N, Talmon G, Godfrey S, et al. Computerized acoustic assessment of treatment efficacy of nebulized epinephrine and albuterol in RSV bronchiolitis. BMC Pediatr. 2007;7:22.
Foresee: CUSUM Calculator for Clinical Control (4-C Software). Available from. http://jacob.puliyel.com/calculator/. Accessed August 7, 2011.
Confidence Interval Analysis (CIA) Software. Available from. http://www.som.soton.ac.uk/research/sites/cia/. Accessed August 7, 2011.
Puliyel A, Puliyel J. CUSUM for monitoring competency: computer software is useful for bootstrapping and real time CUSUM plotting. Br J Ophthalmol. 2011;95:295–296.
Kuzik BA, Al-Qadhi SA, Kent S, Flavin MP, Hopman W, Hotte S, et al. Nebulized hypertonic saline in the treatment of viral bronchiolitis in infants. J Pediatr. 2007;151:266–270.
Luo Z, Liu E, Luo J, Li S, Zeng F, Yang X, et al. Nebulized hypertonic saline/salbutamol solution treatment in hospitalized children with mild to moderate bronchiolitis. Pediatr Int. 2010;52:199–202.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gupta, N., Puliyel, A., Manchanda, A. et al. Nebulized hypertonic-saline vs epinephrine for bronchiolitis: Proof of concept study of cumulative sum (CUSUM) analysis. Indian Pediatr 49, 543–547 (2012). https://doi.org/10.1007/s13312-012-0122-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-012-0122-5