Abstract
Background
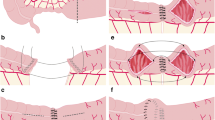
Kono-S anastomosis was described for the first time in 2011 and it showed a lower surgical recurrence rate in patients with Crohn’s disease when compared to the standard technique. The aim of this review is to assess the safety and effectiveness of this surgical procedure by analyzing the data existing in the literature.
Materials and methods
Pubmed, EMBASE and Scopus databases were used as data sources for a systematic comprehensive search of all studies where Kono-S anastomosis was performed in patients with Crohn’s disease. Perioperative data and clinical outcomes were measured.
Results
Five studies described the use of Kono technique to restore intestinal continuity. Postoperative complications rates seem to be acceptable, with the exception of one case regarding the surgical site infection and bowel obstruction rates of one of the studies compared to the others. Surgical recurrence rate ranges from 0 to 3.4% with significant differences between Kono-S anastomosis and other techniques in the only two existing comparative studies.
Conclusion
Kono’s anastomosis seems to be a safe procedure with encouraging results on the reduction of the need for reoperation due to relapse, but the few existing studies do not allow to draw final conclusions. Further comparative, randomized studies, with appropriate sample size, follow up and endoscopic evaluation are necessary to establish the real benefits in the use of this hand-sewn antimesenteric anastomosis compared to a stapled wide lumen side-to-side anastomosis.

Similar content being viewed by others
References
Pariente B, Cosnes J, Danese S et al (2011) Development of the Crohn’s disease digestive damage score, the Lémann score. Inflamm Bowel Dis 17:1415–1422
Bemelman WA, Warusavitarne J, Sampietro GM et al (2018) ECCO-ESCP consensus on surgery for Crohn’s disease. J Crohns Colitis 12:1–16
Bouguen G, Peyrin-biroulet L (2011) Surgery for adult Crohn’s disease: what is the actual risk? Gut 60:1178–1181
Peyrin-biroulet L, Loft EV Jr, Colombel JF, Sandborn WJ (2009) The natural history of adult Crohn’s disease in population-based cohorts. Am J Gastroenterol 105:289–297
Buisson A, Chevaux J, Allen PB, Bommelaer G, Peyrin-Biroulet L (2012) Review article: the natural history of postoperative Crohn’s disease recurrence. Aliment Pharmacol Ther 35:625–633
Cottone M, Rosselli M, Orlando A, Oliva L, Puleo A, Cappello M, Traina M, Tonelli F, Pagliaro L (1994) Smoking habits and recurrence in Crohn’s disease. Gastroenterology 106:643–648
Singh S, Nguyen GC (2017) Management of Crohn’s disease after surgical resection. Gastroenterol Clin N Am 46:563–575
Simillis C, Jacovides M, Reese GE, Yamamoto T, Tekkis PP (2010) Meta-analysis of the role of granulomas in the recurrence of Crohn disease. Dis Colon Rectum 53:177–185
Decousus S, Boucher AL, Joubert J, Pereira B, Dubois A, Goutorbe F, Déchelotte PJ, Bommelaer G, Buisson A (2016) Myenteric plexitis is a risk factor for endoscopic and clinical postoperative recurrence after ileocolonic resection in Crohn’s disease. Dig Liver Dis 48:753–758
Aguas M, Bastida G, Cerrillo E, Beltrán B, Iborra M, Sánchez-Montes C, Muñoz F, Barrio J, Riestra S, Nos P (2012) Adalimumab in prevention of postoperative recurrence of Crohn’s disease in high-risk patients. World J Gastroenterol 18:4391–4398
Savarino E, Bodini G, Dulbecco P, Assandri L, Bruzzone L, Mazza F, Frigo AC, Fazio V, Marabotto E, Savarino V (2013) Adalimumab is more effective than azathioprine and mesalamine at preventing postoperative recurrence of Crohn’s disease: a randomized controlled trial. Am J Gastroenterol 108:1731–1742
Regueiro M, Schraut W, Baidoo L, Kip KE, Sepulveda AR, Pesci M, Harrison J, Plevy SE (2009) Infliximab prevents Crohn’s disease recurrence after ileal resection. Gastroenterology 136:441–450
Rutgeerts P, Geboes K, Vantrappen G, Kerremans R, Coenegrachts JL, Coremans G (1984) Natural history of recurrent Crohn’s disease at the ileocolonic anastomosis after curative surgery. Gut 25:665–672
Gionchetti P, Dignass A, Danese S et al (2017) 3rd European evidence-based consensus on the diagnosis and management of Crohn’s disease 2016: part 2: surgical management and special situations. J Crohn’s Colitis 11:135–149
Kono T, Ashida T, Ebisawa Y, Chisato N, Okamoto K, Katsuno H, Maeda K, Fujiya M, Kohgo Y, Furukawa H (2011) A new antimesenteric functional end-to-end handsewn anastomosis: surgical prevention of anastomotic recurrence in Crohn’s disease. Dis Colon Rectum 54:586–592
Slim K, Nini E, Forestier D et al (2003) Methodological index for non-randomized studies (Minors): development and validation of a new instrument. ANZ J Surg 73:712–716
Murad MH, Sultan S, Haffar S, Bazerbachi F (2018) Methodological quality and synthesis of case series and case reports. BMJ Evid Based Med 23:60–63
Fichera A, Zoccali M, Kono T (2012) Antimesenteric functional end-to-end handsewn (Kono-S) anastomosis. J Gastrointest Surg 16:1412–1416
Kono T, Fichera A, Maeda K, Sakai Y, Ohge H, Krane M, Katsuno H, Fujiya M (2016) Kono-S anastomosis for surgical prophylaxis of anastomotic recurrence in Crohn’s disease: an international multicenter study. J Gastrointest Surg 20:783–790
Katsuno H, Maeda K, Hanai T, Masumori K, Koide Y, Kono T (2015) Novel antimesenteric functional end-to-end handsewn (Kono-s) anastomoses for Crohn’s disease: a report of surgical procedure and short-term outcomes. Dig Surg 32:39–44
Seyfried S, Post S, Kienle P, Galata CL (2019) The Kono-S anastomosis in surgery for Crohn’s disease: first results of a new functional end-to-end anastomotic technique after intestinal resection in patients with Crohn’s disease in Germany. Chirurg 90:131–136
Shimada N, Ohge H, Kono T, Sugitani A, Yano R, Watadani Y, Uemura K, Murakami Y, Sueda T (2018) Surgical recurrence at anastomotic site after bowel resection in Crohn’s disease: comparison of Kono-S and end-to-end anastomosis. J Gastrointest Surg 23:312–319
De Cruz P, Kamm MA, Prideaux L, Allen PB, Desmond PV (2012) Postoperative recurrent luminal Crohn’s disease: a systematic review. Inflamm Bowel Dis 18:758–777
Wolters FL, Russel MG, Sijbrandij J et al (2006) Phenotype at diagnosis predicts recurrence rates in Crohn’s disease. Gut 55:1124–1130
Vester-Andersen MK, Vind I, Prosberg MV, Bengtsson BG, Blixt T, Munkholm P, Andersson M, Jess T, Bendtsen F (2014) Hospitalisation, surgical and medical recurrence rates in inflammatory bowel disease 2003–2011—a Danish population-based cohort study. J Crohn’s Colitis 8:1675–1683
Watanabe T, Sasaki I, Sugita A, Fukushima K, Futami K, Hibi T, Watanabe M (2012) Interval of less than 5 years between the first and second operation is a risk factor for a third operation for Crohn’s disease. Inflamm Bowel Dis 18:17–24
Cameron JL, Hamilton SR, Coleman J, Sitzmann JV, Bayless TM (1992) Patterns of ileal recurrence in Crohn’s disease. A prospective randomized study. Ann Surg 215:546–551
Guo Z, Li Y, Zhu W, Gong J, Li N, Li J (2013) Comparing outcomes between side-to-side anastomosis and other anastomotic configurations after intestinal resection for patients with Crohn’s disease: a meta-analysis. World J Surg 37:893–901
He X, Chen Z, Huang J, Lian L, Rouniyar S, Wu X, Lan P (2014) Stapled side-to-side anastomosis might be better than handsewn end-to-end anastomosis in ileocolic resection for Crohn’s disease: a meta-analysis. Dig Dis Sci 59:1544–1551
Zurbuchen U, Kroesen AJ, Knebel P, Betzler MH, Becker H, Bruch HP, Senninger N, Post S, Buhr HJ, Ritz JP, German Advanced Surgical Treatment Study Group (2013) Complications after end-to-end vs. side-to-side anastomosis in ileocecal Crohn’s disease—early postoperative results from a randomized controlled multi-center trial (ISRCTN-45665492). Langenbeck’s Arch Surg 398:467–474
McLeod RS, Wolff BG, Ross S, Parkes R, McKenzie M, Investigators of the CAST Trial (2009) Recurrence of Crohn’s disease after ileocolic resection is not affected by anastomotic type: results of a multicenter, randomized, controlled trial. Dis Colon Rectum 52:919–927
Hashemi M, Novell JR, Lewis AA (1998) Side-to side stapled anastomosis may delay recurrence in Crohn’s disease. Dis Colon Rectum 41:1293–1296
Yamamoto T, Bain IM, Mylonakis E, Allan RN, Keighley MR (1999) Stapled functional end-to-end anastomosis versus sutured end-to-end anastomosis after ileocolonic resection in Crohn disease. Scand J Gastroenterol 34:708–713
Muñoz-Juárez M, Yamamoto T, Wolff BG, Keighley MR (2001) Wide-lumen stapled anastomosis vs. conventional end-to-end anastomosis in the treatment of Crohn’s disease. Dis Colon Rectum 44:20–26
Coffey JC, O’Leary DP (2016) The mesentery: structure, function, and role in disease. Lancet Gastroenterol Hepatol 1:238–247
Coffey JC, O’Leary DP, Kiernan MG, Faul P (2016) The mesentery in Crohn’s disease: friend or foe? Curr Opin Gastroenterol 32:267–273
Coffey CJ, Kiernan MG, Sahebally SM (2018) Inclusion of the mesentery in ileocolic resection for Crohn’s disease is associated with reduced surgical recurrence. J Crohn’s Colitis 12:1139–1150
Peltrini R, Bucci L (2019) “Mesentery-based surgery” to prevent surgical recurrence in Crohn’s disease: from basics to surgical practice. Int J Colorectal Dis 34:353–354
Ojima H, Sohda M, Ando H, Sano A, Fukai Y, Ogawa A, Mochida Y, Kuwano H (2015) Relationship between functional end-to-end anastomosis for colon cancer and surgical site infections. Surg Today 45:1489–1492
Luglio G, Rispo A, Castiglione F, Imperatore N, Giglio MC, De Palma GD, Bucci L (2016) Kono-type anastomosis in a patient with severe multi-recurrent Crohn’s disease. Int J Colorectal Dis 31:1565–1566
Luglio G, Giglio MC, Rispo A, Peltrini R, Sacco M, Sollazzo V, Bucci C, Spadarella E, Terracciano F, De Palma GD, Bucci L (2016) SuPREMe-CD study: surgical prevention of anastomotic recurrence by excluding mesentery in Crohn’s disease-preliminary results and trial protocol. J Crohn’s Colitis 10(Suppl 1):S398
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human participants and/or animals
This article does not contain any studies with animals performed by any of the authors.
Informed consent
The informed consent does not apply since this is a review study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Peltrini, R., Greco, P.A., Manfreda, A. et al. Kono-S anastomosis after intestinal resection for Crohn’s disease. Updates Surg 72, 335–340 (2020). https://doi.org/10.1007/s13304-019-00700-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13304-019-00700-w