Abstract
Purpose
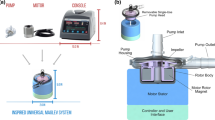
Pediatric heart failure patients remain in critical need of a dedicated mechanical circulatory support (MCS) solution as development efforts for specific pediatric devices continue to fall behind those for the adult population. The Inspired Pediatric VAD is being developed as a pediatric specific MCS solution to provide up to 30-days of circulatory or respiratory support in a compact modular package that could allow for patient ambulation during treatment.
Methods
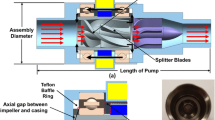
Hydrodynamic performance (flows, pressures), impeller/rotor mechanical properties (torques, forces), and flow shear stress and residence time distributions of the latest design version, Inspired Pediatric VAD V3, were numerically predicted and investigated using computational fluid dynamics (CFD) software (SolidWorks Flow Simulator).
Results
Hydrodynamic performance was numerically predicted, indicating no change in flow and pressure head compared to the previous device design (V2), while displaying increased impeller/rotor torques and translation forces enabled by improved geometry. Shear stress and flow residence time volumetric distributions are presented over a range of pump rotational speeds and flow rates. At the lowest pump operating point (3000 RPM, 0.50 L/min, 75 mmHg), 79% of the pump volume was in the shear stress range of 0–10 Pa with < 1% of the volume in the critical range of 150–1000 Pa for blood damage. At higher speed and flow (5000 RPM, 3.50 L/min, 176 mmHg), 65% of the volume resided in the 0–10 Pa range compared to 2.3% at 150–1000 Pa.
Conclusions
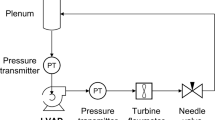
The initial computational characterization of the Inspired Pediatric VAD V3 is encouraging and future work will include device prototype testing in a mock circulatory loop and acute large animal model.









Similar content being viewed by others
References
Alemu, Y., and D. Bluestein. Flow-induced platelet activation and damage accumulation in a mechanical heart valve: numerical studies. Artif. Org. 31(9):677–688, 2007.
Berg, N., L. Fuchs, and L. Prahl Wittberg. Flow characteristics and coherent structures in a centrifugal blood pump. Flow Turbul. Combust. 102(2):469–483, 2019.
Burki, S., and I. Adachi. Pediatric ventricular assist devices: current challenges and future prospects. Vasc. Health Risk Manag. 13:177–185, 2017.
Caballero, A. D., and S. Laín. Numerical simulation of non-Newtonian blood flow dynamics in human thoracic aorta. Comput. Methods Biomech. Biomed. Eng. 18(11):1200–1216, 2015.
Carlos Álvarez, M., W. Vicente, F. Solorio, E. Mancilla, M. Salinas, and V. R. Zenit. A study of the Taylor-Couette flow with finned surface rotation. J. Appl. Fluid Mech. 12(5):1371–1382, 2019.
Colvin, M., et al. OPTN/SRTR 2015 annual data report. Heart Am. J. Transplant. 17:286–356, 2017.
Crow, S., et al. Acquired von Willebrand syndrome in continuous-flow ventricular assist device recipients. Ann. Thorac. Surg. 90(4):1263–1269, 2010.
Dipchand, A. I., et al. The registry of the international society for heart and lung transplantation: eighteenth official pediatric heart transplantation report - 2015; focus theme: early graft failure. J. Heart Lung Transplant. 34(10):1233–1243, 2015.
Eymard, R., T. Gallouët, and R. Herbin. Finite volume methods. Handb. Numer. Anal. 7(December):713–1018, 2000.
Fraser, K. H., et al. The effect of impeller position on CFD calculations of blood flow in magnetically levitated centrifugal blood pumps. In: ASME 2010 Summer Bioengineering Conference, SBC 2010, 2010, no. PARTS A AND B, pp. 119–120.
Fraser, K. H., M. E. Taskin, B. P. Griffith, and Z. J. Wu. The use of computational fluid dynamics in the development of ventricular assist devices. Med. Eng. Phys. 33(3):263–280, 2011.
Fraser, K. H., T. Zhang, M. E. Taskin, B. P. Griffith, and Z. J. Wu. A quantitative comparison of mechanical blood damage parameters in rotary ventricular assist devices: shear stress, exposure time and hemolysis index. J. Biomech. Eng. 134(8):1–11, 2012.
Frêne, J., D. Nicolas, B. Degueurce, D. Berthe, and M. B. T.-T. S. Godet, eds. Chapter 11—Superlaminar flow regimes. In: Hydrodynamic Lubrication, vol. 33, Elsevier, 1990, pp. 347–386.
Garon, A., and M. I. Farinas. Fast three-dimensional numerical hemolysis approximation. Artif. Org. 28(11):1016–1025, 2004.
Hochareon, P., K. B. Manning, A. A. Fontaine, J. M. Tarbell, and S. Deutsch. Correlation of in vivo clot deposition with the flow characteristics in the 50 cc Penn State Artificial Heart: a preliminary study. ASAIO J. 50(6):537–542, 2004.
Körfer, S., S. Klaus, and K. Mottaghy. Application of Taylor vortices in hemocompatibility investigations. Int. J. Artif. Org. 26(4):331–338, 2003.
Ng, J. H., R. K. Jaiman, and T. T. Lim. Interaction dynamics of longitudinal corrugations in Taylor-Couette flows. Phys. Fluids. 30(9):093601, 2018.
Nishida, M., T. Yamane, and B. Asztalos. Washout hole flow measurement for the development of a centrifugal blood pump. Artif. Org. 22(5):386–392, 1998.
Reay, D., C. Ramshaw, and A. B. T.-P. I. Harvey, eds. Chapter 5—Reactors. In: Isotopes in Organic Chemistry. Oxford: Butterworth-Heinemann, 2008, pp. 103–186.
Rezaienia, M. A., G. Paul, E. Avital, M. Rothman, and T. Korakianitis. Computational parametric study of the axial and radial clearances in a centrifugal rotary blood pump. ASAIO J. 64(5):643–650, 2018.
Rossano, J. W., et al. Prevalence, morbidity, and mortality of heart failure-related hospitalizations in children in the United States: a population-based study. J. Card. Fail. 18(6):459–470, 2012.
Shibeshi, S. S., and W. E. Collins. The rheology of blood flow in a branched arterial system. Appl. Rheol. 15(6):398–405, 2005.
Shu, F., R. Tian, S. Vandenberghe, and J. F. Antaki. Experimental study of micro-scale Taylor vortices within a co-axial mixed-flow blood pump. Artif. Org. 40(11):1071–1078, 2016.
Sobachkin, A., and G. Dumnov. Numerical basis of CAD-embedded CFD. In: NAFEMS World Congress 2013, 2013, no. February, pp. 1–20.
SOLIDWORKS Flow Simulation: Sliding Mesh. [Online]. https://files.goengineer.com/docs/support/SOLIDWORKS_Flow_Simulation_Sliding_Mesh.pdf. Accessed 16 Mar 2020.
Song, X., A. L. Throckmorton, H. G. Wood, J. F. Antaki, and D. B. Olsen. Computational fluid dynamics prediction of blood damage in a centrifugal pump. Artif. Org. 27(10):938–941, 2003.
Thamsen, B., et al. Numerical analysis of blood damage potential of the HeartMate II and HeartWare HVAD rotary blood pumps. Artif. Org. 39(8):651–659, 2015.
Thamsen, B., et al. A two-stage rotary blood pump design with potentially lower blood trauma: a computational study. Int. J. Artif. Org. 39(4):178–183, 2016.
Ting, D. S.-K. Chapter 1—Introducing flow turbulence. In: Basics of Engineering Turbulence, edited by D. S.-K. B. T.-B. of E. T. Ting. Academic Press, 2016, pp. 3–18.
Tompkins, L. H., et al. Design and initial computational evaluation of a pediatric MagLev rotary blood pump. ASAIO J. 67:1026, 2020.
Tonks, L. Note on earnshaw’s theorem. Electr. Eng. 59(3):118–119, 1940.
Turitto, V. T., and C. L. Hall. Mechanical factors affecting hemostasis and thrombosis. Thromb. Res. 92(6 SUPPL. 2):25–31, 1998.
White, F. M. Fluid Mechanics. New York: McGraw-Hill, 1999.
Wiegmann, L., et al. Blood pump design variations and their influence on hydraulic performance and indicators of hemocompatibility. Ann. Biomed. Eng. 46(3):417–428, 2018.
Wootton, D. M., and D. N. Ku. Fluid mechanics of vascular systems, diseases, and thrombosis. Annu. Rev. Biomed. Eng. 1:299–329, 1999.
Wu, J., B. E. Paden, H. S. Borovetz, and J. F. Antaki. Computational fluid dynamics analysis of blade tip clearances on hemodynamic performance and blood damage in a centrifugal ventricular assist device. Artif. Org. 34(5):402–411, 2010.
Zhang, J., et al. Computational and experimental evaluation of the fluid dynamics and hemocompatibility of the centrimag blood pump. Artif. Org. 30(3):168–177, 2006.
Zhang, J., et al. Optimization of a miniature Maglev ventricular assist device for pediatric circulatory support. ASAIO J. 53(1):23–31, 2007.
Author Contributions
All authors contributed equally to this manuscript.
Funding
This development effort and study was supported by National Institutes of Health (NIH) Small Business Innovation Research (SBIR) Grant No. 1R43HL144214-01.
Data Availability
Additional data from this study is made available as a Supplementary Materials document.
Conflict of interest
LHT is a consultant for Inspired Therapeutics LLC. BNG is the CTO and a co-Founder of Inspired Therapeutics LLC, and served as Co-Investigator on grant R43HL144214-01. SRP was a sub-contract consultant with Veritium Research LLC for NIH SBIR phase I grant R43HL144214-01. GFM was a sub-contract consultant with Veritium Research on grant R43HL144214-01. TR, JAK, and SJW are faculty at the University of Louisville. PCP is an employee of Inspired Therapeutics LLC. SCK and MSS were Co-Investigators with sub-contract University of Louisville on grant R43HL144214-01. KAD is the CEO and co-Founder of Inspired Therapeutics LLC, and served as Principal Investigator on grant R43HL144214-01. Additional Affiliations Unrelated to the Presented Work LHT is a co-owner of MAST LLC, engineer with Cor Habere Corp., and consultant with VADovations Inc. BNG is a consultant to Paragonix Technologies, Inc., Vivante Health, Inc., and Cardiac Assist Holdings. SCK and MSS are co-founders of Cor Habere Corp. and MAST LLC developing medical devices supported by NIH SBIR phase I grants R43HL142337-01, R43HL142385-01, R43HL152894-01. MSS is also a consultant with Magenta Medical. KAD is a Co-Investigator on NIH SBIR phase I grant R43HL142385-01 and consultant on NIH SBIR grant R43HL158430-01. KAD is also President and COO of VADovations Inc, and serves as a consultant to BiVACOR Inc, CH-Biomedical USA Inc, Jarvik Heart International, Vortronix Medical LLC, Teal Health Inc., CAH Holdings LLC, and “The Kidney Project” affiliated with the University of California San Francisco and Vanderbilt University. KAD serves on the Board of Directors for Makana Therapeutics and Artio Medical. All of these additional author affiliations are unrelated to the work presented in this manuscript.
Ethical Approval
No human studies were carried out by the authors for this article. No animal studies were carried out by the authors for this article.
Consent to Participate
Not Applicable
Consent for Publication
Not Applicable
Author information
Authors and Affiliations
Corresponding authors
Additional information
Associate Editor Ajit P. Yoganathan oversaw the review of this article
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tompkins, L.H., Gellman, B.N., Prina, S.R. et al. Development of Inspired Therapeutics Pediatric VAD: Computational Analysis and Characterization of VAD V3. Cardiovasc Eng Tech 13, 624–637 (2022). https://doi.org/10.1007/s13239-021-00602-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13239-021-00602-2