Abstract
Aims
Sarcopenia is characterized by a gradual loss of skeletal muscle mass and strength with increased adverse outcomes. Recently, large-scale epidemiological studies have demonstrated a relationship between several chronic disorders and ocular pathological conditions using an oculomics approach. We hypothesized that sarcopenia can be predicted through eye examinations, without invasive tests or radiologic evaluations in the context of predictive, preventive, and personalized medicine (PPPM/3PM).
Methods
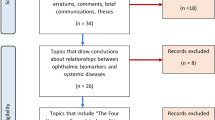
We analyzed data from the Korean National Health and Nutrition Examination Survey (KNHANES). The training set (80%, randomly selected from 2008 to 2010) data were used to construct the machine learning models. Internal (20%, randomly selected from 2008 to 2010) and external (from the KNHANES 2011) validation sets were used to assess the ability to predict sarcopenia. We included 8092 participants in the final dataset. Machine learning models (XGBoost) were trained on ophthalmological examinations and demographic factors to detect sarcopenia.
Results
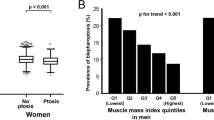
In the exploratory analysis, decreased levator function (odds ratio [OR], 1.41; P value <0.001), cataracts (OR, 1.31; P value = 0.013), and age-related macular degeneration (OR, 1.38; P value = 0.026) were associated with an increased risk of sarcopenia in men. In women, an increased risk of sarcopenia was associated with blepharoptosis (OR, 1.23; P value = 0.038) and cataracts (OR, 1.29; P value = 0.010). The XGBoost technique showed areas under the receiver operating characteristic curves (AUCs) of 0.746 and 0.762 in men and women, respectively. The external validation achieved AUCs of 0.751 and 0.785 for men and women, respectively. For practical and fast hands-on experience with the predictive model for practitioners who may be willing to test the whole idea of sarcopenia prediction based on oculomics data, we developed a simple web-based calculator application (https://knhanesoculomics.github.io/sarcopenia) to predict the risk of sarcopenia and facilitate screening, based on the model established in this study.
Conclusion
Sarcopenia is treatable before the vicious cycle of sarcopenia-related deterioration begins. Therefore, early identification of individuals at a high risk of sarcopenia is essential in the context of PPPM. Our oculomics-based approach provides an effective strategy for sarcopenia prediction. The proposed method shows promise in significantly increasing the number of patients diagnosed with sarcopenia, potentially facilitating earlier intervention. Through patient oculometric monitoring, various pathological factors related to sarcopenia can be simultaneously analyzed, and doctors can provide personalized medical services according to each cause. Further studies are needed to confirm whether such a prediction algorithm can be used in real-world clinical settings to improve the diagnosis of sarcopenia.








Similar content being viewed by others
Abbreviations
- ASM :
-
appendicular skeletal muscle mass
- AUC :
-
areas under the receiver operating characteristic curve
- BMI :
-
body mass index
- CT :
-
computed tomography
- DEXA :
-
dual-energy X-ray absorptiometry
- KNHANES :
-
Korean National Health and Nutrition Examination Survey
- KOS :
-
Korean Ophthalmological Society
- MRD1 :
-
marginal reflex distance 1
- MRI :
-
magnetic resonance imaging
- PPPM/3PM :
-
predictive, preventive, and personalized medicine
- SHAP :
-
SHapley Additive exPlanations
- TabNet :
-
deep learning network for tubular data
- XGBoost :
-
eXtreme Gradient Boosting
References
Cruz-Jentoft AJ, Sayer AA. Sarcopenia. The Lancet. 2019;393:2636–46.
Bruyère O, Beaudart C, Ethgen O, Reginster J-Y, Locquet M. The health economics burden of sarcopenia: a systematic review. Maturitas. 2019;119:61–9.
Biolo G, Cederholm T, Muscaritoli M. Muscle contractile and metabolic dysfunction is a common feature of sarcopenia of aging and chronic diseases: From sarcopenic obesity to cachexia. Clinical Nutrition. 2014;33:737–48.
Kim Y-S, Hong K-W, Han K, Park YC, Park J-M, Kim K, et al. Longitudinal observation of muscle mass over 10 years according to serum calcium levels and calcium intake among korean adults aged 50 and older: the Korean genome and epidemiology study. Nutrients. 2020;12(2856):e1–12.
Golubnitschaja O, Liskova A, Koklesova L, Samec M, Biringer K, Büsselberg D, et al. Caution, “normal” BMI: health risks associated with potentially masked individual underweight—EPMA Position Paper 2021. EPMA Journal. 2021;12:243–64.
Tournadre A, Vial G, Capel F, Soubrier M, Boirie Y. Sarcopenia. Joint Bone Spine. 2019;86:309–14.
Bian A-L, Hu H-Y, Rong Y-D, Wang J, Wang J-X, Zhou X-Z. A study on relationship between elderly sarcopenia and inflammatory factors IL-6 and TNF-α. European Journal of Medical Research. 2017;22:25.
Cesari M, Fielding RA, Pahor M, Goodpaster B, Hellerstein M, van Kan GA, et al. Biomarkers of sarcopenia in clinical trials-recommendations from the International Working Group on Sarcopenia. J Cachexia Sarcopenia Muscle. 2012;3:181–90.
Lee K, Shin Y, Huh J, Sung YS, Lee I-S, Yoon K-H, et al. Recent issues on body composition imaging for sarcopenia evaluation. Korean J Radiol. 2018;20:205–17.
Wagner SK, Fu DJ, Faes L, Liu X, Huemer J, Khalid H, et al. Insights into systemic disease through retinal imaging-based oculomics. Trans Vis Sci Tech. 2020;9:6–6.
Yadav S, Tandon R. Comprehensive eye examination: what does it mean? Community Eye Health. 2019;32:S1–4.
Abràmoff MD, Niemeijer M, Suttorp-Schulten MSA, Viergever MA, Russell SR, van Ginneken B. Evaluation of a system for automatic detection of diabetic retinopathy from color fundus photographs in a large population of patients with diabetes. Diabetes Care. 2008;31:193–8.
Shin J, Kang MS, Park K, Lee JS. Association between metabolic risk factors and optic disc cupping identified by deep learning method. Plos One. 2020;15(e0239071):e1–11.
Rim TH, Lee CJ, Tham Y-C, Cheung N, Yu M, Lee G, et al. Deep-learning-based cardiovascular risk stratification using coronary artery calcium scores predicted from retinal photographs. The Lancet Digital Health. 2021;3:e306–16.
Zhan X, Li J, Guo Y, Golubnitschaja O. Mass spectrometry analysis of human tear fluid biomarkers specific for ocular and systemic diseases in the context of 3P medicine. EPMA Journal. 2021;12:449–75.
Yoo TK, Kim SW, Seo KY. Association between Serum Immnunoglobulin E and pterygium: a population-based study from South Korea. Current Eye Research. 2018;43:1090–6.
Cohen LM, Campbell BC, Esfandiari M, Goldberg RA, Rootman DB. Ophthalmic surgeries and systemic medical conditions associated with the development of involutional ptosis. Ophthalmic Plastic & Reconstructive Surgery. 2021;37:133–7.
Yoo TK, Kim SH, Kwak J, Kim HK, Rim TH (2018) Association between osteoporosis and age-related macular degeneration: the Korea National Health and Nutrition Examination Survey. Invest Ophthalmol Vis Sci. 59:AMD132–42.
Bertele N, Karabatsiakis A, Buss C, Talmon A. How biomarker patterns can be utilized to identify individuals with a high disease burden: a bioinformatics approach towards predictive, preventive, and personalized (3P) medicine. EPMA Journal. 2021;12:507–16.
Wang W, Yan Y, Guo Z, Hou H, Garcia M, Tan X, et al. All around suboptimal health — a joint position paper of the Suboptimal Health Study Consortium and European Association for Predictive. Preventive and Personalised Medicine. EPMA Journal. 2021;12:403–33.
Poplin R, Varadarajan AV, Blumer K, Liu Y, McConnell MV, Corrado GS, et al. Prediction of cardiovascular risk factors from retinal fundus photographs via deep learning. Nature Biomedical Engineering. 2018;2:158.
Zheng Y, Guo Z, Zhang Y, Shang J, Yu L, Fu P, et al. Rapid triage for ischemic stroke: a machine learning-driven approach in the context of predictive, preventive and personalised medicine. EPMA Journal. 2022;13:285–98.
Kweon S, Kim Y, Jang M, Kim Y, Kim K, Choi S, et al. Data resource profile: the Korea National Health and Nutrition Examination Survey (KNHANES). Int J Epidemiol. 2014;43:69–77.
Yoo TK, Oh E. Association between dry eye syndrome and osteoarthritis severity: a nationwide cross-sectional study (KNHANES V). Pain Medicine. 2021;22:2525–32.
Park S-J, Ryu S-Y, Park J, Choi S-W. Association of sarcopenia with metabolic syndrome in Korean population using 2009–2010 Korea National Health and Nutrition Examination Survey. Metabolic Syndrome and Related Disorders. 2019;17:494.
Studenski SA, Peters KW, Alley DE, Cawthon PM, McLean RR, Harris TB, et al. The FNIH Sarcopenia Project: Rationale, Study Description, Conference Recommendations, and Final Estimates. J Gerontol A Biol Sci Med Sci. 2014;69:547–58.
Lee Y, Jung KS, Kim SU, Yoon H, Yun YJ, Lee B-W, et al. Sarcopaenia is associated with NAFLD independently of obesity and insulin resistance: Nationwide surveys (KNHANES 2008–2011). Journal of Hepatology. 2015;63:486–93.
Paik J-S, Han K, Yang S-W, Park Y, Na K, Cho W, et al. Blepharoptosis among Korean adults: age-related prevalence and threshold age for evaluation. BMC Ophthalmology. 2020;20:99.
Oh E, Yoo TK, Hong S. Artificial neural network approach for differentiating open-angle glaucoma from glaucoma suspect without a visual field test. Invest Ophthalmol Vis Sci. 2015;56:3957–66.
Chen T, Guestrin C. Xgboost: A scalable tree boosting system. Proceedings of the 22nd acm sigkdd international conference on knowledge discovery and data mining. 2016;85–94.
Arik SÖ, Pfister T. TabNet: attentive interpretable tabular learning. Proceedings of the AAAI Conference on Artificial Intelligence. 2021;35:6679–87.
Asadi-Pooya AA, Kashkooli M, Asadi-Pooya A, Malekpour M, Jafari A. Machine learning applications to differentiate comorbid functional seizures and epilepsy from pure functional seizures. Journal of Psychosomatic Research. 2022;153:110703.
Shwartz-Ziv R, Armon A. Tabular data: Deep learning is not all you need. Information Fusion. 2022;81:84–90.
Lundberg SM, Nair B, Vavilala MS, Horibe M, Eisses MJ, Adams T, et al. Explainable machine-learning predictions for the prevention of hypoxaemia during surgery. Nature Biomedical Engineering. 2018;2:749.
Rim TH, Lee G, Kim Y, Tham Y-C, Lee CJ, Baik SJ, et al. Prediction of systemic biomarkers from retinal photographs: development and validation of deep-learning algorithms. The Lancet Digital Health. 2020;2:e526–36.
Scharf G, Heineke J. Finding good biomarkers for sarcopenia. J Cachexia Sarcopenia Muscle. 2012;3:145–8.
Rossi AP, Micciolo R, Rubele S, Fantin F, Caliari C, Zoico E, et al. Assessing the risk of sarcopenia in the elderly: the Mini Sarcopenia Risk Assessment (MSRA) questionnaire. J Nutr Health Aging. 2017;21:743–9.
Bahat G, İlhan B. Sarcopenia and the cardiometabolic syndrome: A narrative review. European Geriatric Medicine. 2016;7:220–3.
Kim MH, Cho J, Zhao D, Woo KI, Kim Y-D, Kim S, et al. Prevalence and associated factors of blepharoptosis in Korean adult population: the Korea National Health and Nutrition Examination Survey 2008–2011. Eye. 2017;31:940–6.
Wouters RJ, van den Bosch WA, Mulder PGH, Lemij HG. Upper eyelid motility in blepharoptosis and in the aging eyelid. Investigative Ophthalmology & Visual Science. 2001;42:620–5.
Beebe DC, Holekamp NM, Shui Y-B. Oxidative damage and the prevention of age-related cataracts. Ophthalmic Res. 2010;44:155–65.
Babenko B, Mitani A, Traynis I, Kitade N, Singh P, Maa AY, et al. Detection of signs of disease in external photographs of the eyes via deep learning. Nat Biomed Eng. 2022;1–14.
Xiao W, Huang X, Wang JH, Lin DR, Zhu Y, Chen C, et al. Screening and identifying hepatobiliary diseases through deep learning using ocular images: a prospective, multicentre study. Lancet Digit Health. 2021;3:e88–97.
Darvishi A, Hemami MR, Shafiee G, Daroudi R, Mohseni M, Shekarabi FH, et al. Sarcopenia screening strategies in older people: a cost effectiveness analysis in Iran. BMC Public Health. 2021;21:926.
Bao W, Sun Y, Zhang T, Zou L, Wu X, Wang D, et al. Exercise programs for muscle mass, muscle strength and physical performance in older adults with sarcopenia: a systematic review and meta-analysis. Aging Dis. 2020;11:863–73.
Jeong S, Lemke BN, Dortzbach RK, Park YG, Kang HK. The Asian upper eyelid: an anatomical study with comparison to the Caucasian eyelid. Archives of Ophthalmology. 1999;117:907–12.
Woo J, Arai H, Ng TP, Sayer AA, Wong M, Syddall H, et al. Ethnic and geographic variations in muscle mass, muscle strength and physical performance measures. European Geriatric Medicine. 2014;5:155–64.
Sabel BA, Wang J, Fähse S, Cárdenas-Morales L, Antal A. Personality and stress influence vision restoration and recovery in glaucoma and optic neuropathy following alternating current stimulation: implications for personalized neuromodulation and rehabilitation. EPMA Journal. 2020;11:177–96.
McManus JR, Netland PA. Screening for glaucoma: rationale and strategies. Current Opinion in Ophthalmology. 2013;24:144–9.
Rodriguez-Acuña R, Mayoral E, Aguilar-Diosdado M, Rave R, Oyarzabal B, Lama C, et al. Andalusian program for early detection of diabetic retinopathy: implementation and 15-year follow-up of a population-based screening program in Andalusia, Southern Spain. BMJ Open Diabetes Research and Care. 2020;8(e001622):e1–8.
Beaudart C, Dawson A, Shaw SC, Harvey NC, Kanis JA, Binkley N, et al. Nutrition and physical activity in the prevention and treatment of sarcopenia: systematic review. Osteoporos Int. 2017;28:1817–33.
Garnica O, Gómez D, Ramos V, Hidalgo JI, Ruiz-Giardín JM. Diagnosing hospital bacteraemia in the framework of predictive, preventive and personalised medicine using electronic health records and machine learning classifiers. EPMA Journal. 2021;12:365–81.
Mun S, Park K, Lee S. Evaluation of thermal sensitivity is of potential clinical utility for the predictive, preventive, and personalized approach advancing metabolic syndrome management. EPMA J. 2022;13:125–35.
Acknowledgements
We would like to thank the Editage for English language editing.
Data availability
The raw data used for model training, validation, and testing are publicly available at https://knhanes.kdca.go.kr/knhanes/eng. The development data for this study is available at http://data.mendeley.com/datasets/h547645876. The sarcopenia risk calculator is accessible at https://knhanesoculomics.github.io/sarcopenia.
Code availability
The XGBoost and TabNet codes used as the backbone of our architecture are available at http://data.mendeley.com/datasets/h547645876. The codes that support the findings of this study are available from the corresponding authors, upon reasonable request.
Author information
Authors and Affiliations
Contributions
Bo Ram Kim, Tae Keun Yoo, and Bom Taeck Kim had full access to all the data in the study and take responsibility for the integrity and accuracy of its analysis. All authors met the following criteria: (1) substantial contributions to the conception or design of the work or the acquisition, analysis, or interpretation of the data; (2) drafting the work or revising it critically for important intellectual content; (3) approval of the final version; and (4) accountability for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The study protocol was approved by the Institutional Review Board of the Korean Center for Disease Control and Prevention (No. 2008–04EXP-01-C, 2009–01CON-03-C, 2010–02CON-21-C, and 2011–02CON-06-C). The raw data sets are publicly available through the KNHANES website, and data collection from the KNHANES dataset was approved by the Institutional Review Board of the Korean National Institute for Bioethics Policy, which waived the requirement for informed consent for this study. The study adhered to the tenets of the Declaration of Helsinki.
Consent for publication
Not applicable.
Competing interests
Jin Kuk Kim, Ik Hee Ryu, and Tae Keun Yoo are executives of VISUWORKS, Inc., a Korean artificial intelligence company providing medical machine learning solutions. Jin Kuk Kim is an executive of the Korea Intelligent Medical Industry Association. They received salaries or stocks as part of their standard compensation packages. The remaining authors declare no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(PDF 339 kb)
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kim, B.R., Yoo, T.K., Kim, H.K. et al. Oculomics for sarcopenia prediction: a machine learning approach toward predictive, preventive, and personalized medicine. EPMA Journal 13, 367–382 (2022). https://doi.org/10.1007/s13167-022-00292-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13167-022-00292-3