Abstract
Background
The role of dietary habits in the etiology of pancreatic cancer (PC) has not yet been well elucidated.
Aim
The aim of the present study was to examine the association of the frequency of different food groups’ intake and their cooking methods with PC risk based on a well-designed case–control study.
Methods
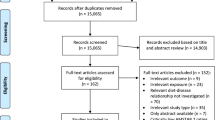
A case–control study including 307 PC patients and 322 controls referred to four tertiary endosonography centers was conducted from January 2011 to January 2014 to compare the frequency intake of different food items and their cooking methods between cases and controls.
Results
After adjustment for gender, age, body mass index, years of education, diabetes and alcohol history, smoking status, and opium use, a significant direct relationship was observed between PC risk and intake frequency (time/week) of bread (OR = 1.50; 95 % CI 1.05–2.13; p-value 0.024), rice (OR = 2.10; 95 % CI 1.15–3.82; p for trend 0.034), and red meat (OR = 2.25; 95 % CI 1.22–4.14; p for trend 0.033) (time/day), when comparing the highest category of intake frequency with the lowest, while increasing frequency of fish consumption was associated with a lower risk of PC (OR = 0.93; 95 % CI0.59–1.47; p for trend 0.009). Increasing consumption of barbecuing red meat and deep fried vegetables was associated with 67 % and 70 % increased risk of PC (p-value 0.025 and 0.006, respectively).
Conclusion
Our results indicate that increased frequency of intake of bread, rice, and red meat (especially barbecued) and deep fried vegetables can aggregate PC risk, while increased frequency of fish consumption can protect against PC. However, more studies are still needed.
Similar content being viewed by others
References
Yadav D, Lowenfels AB. The epidemiology of pancreatitis and pancreatic cancer. Gastroenterology. 2013;144:1252–61.
Ferlay J, Shin HR, Bray F, Forman D, Mathers C, Parkin DM. Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008. Int J Cancer. 2010;127:2893–917.
Greer JB, Brand RE. New developments in pancreatic cancer. Curr Gastroenterol Rep. 2011;13:131–9.
Cappellani A, Cavallaro A, Di Vita M, et al. Diet and pancreatic cancer: many questions with few certainties. Eur Rev Med Pharmacol Sci. 2012;16:192–206.
Pandol S, Gukovskaya A, Edderkaoui M, Dawson D, Eibl G, Lugea A. Epidemiology, risk factors, and the promotion of pancreatic cancer: role of the stellate cell. J Gastroenterol Hepatol. 2012;27 Suppl 2:127–34.
Siegel R, Ma J, Zou Z, Jemal A. Cancer statistics, 2014. CA Cancer J Clin. 2014;64:9–29.
Bao Y, Hu FB, Giovannucci EL, et al. Nut consumption and risk of pancreatic cancer in women. Br J Cancer. 2013;109:2911–6.
Hart AR, Kennedy H, Harvey I. Pancreatic cancer: a review of the evidence on causation. Clin Gastroenterol Hepatol. 2008;6:275–82.
Anderson LN, Cotterchio M, Gallinger S. Lifestyle, dietary, and medical history factors associated with pancreatic cancer risk in Ontario, Canada. Cancer Causes Control. 2009;20:825–34.
Stolzenberg-Solomon RZ, Adams K, Leitzmann M, et al. Adiposity, physical activity, and pancreatic cancer in the National Institutes of Health-AARP Diet and Health Cohort. Am J Epidemiol. 2008;167:586–97.
Grote VA, Rohrmann S, Nieters A, et al. Diabetes mellitus, glycated haemoglobin and C-peptide levels in relation to pancreatic cancer risk: a study within the European Prospective Investigation into Cancer and Nutrition (EPIC) cohort. Diabetologia. 2011;54:3037–46.
Silverman DT, Schiffman M, Everhart J, et al. Diabetes mellitus, other medical conditions and familial history of cancer as risk factors for pancreatic cancer. Br J Cancer. 1999;80:1830–7.
Chang MC, Wong JM, Chang YT. Screening and early detection of pancreatic cancer in high risk population. World J Gastroenterol. 2014;20:2358–64.
Zhang J, Dhakal IB, Gross MD, et al. Physical activity, diet, and pancreatic cancer: a population-based, case–control study in Minnesota. Nutr Cancer. 2009;61:457–65.
Rubin MS, Clouston S, Link BG. A fundamental cause approach to the study of disparities in lung cancer and pancreatic cancer mortality in the United States. Soc Sci Med. 2014;100:54–61.
Farrokhzad S, Nedjat S, Kamangar F, Kamali M, Malekzadeh R, Pourshams A. Validity and reliability of a questionnaire designed to assess risk factors of pancreatic cancer in iran. Arch Iran Med. 2014;17:102–5.
Azar M, Sarkisian E. Food Composition Table of Iran. Tehran: National Nutrition and Food Research Institute: Shahid Beheshti University Press. 1980.
Yener Y, Kalipci E, Oztas H, Aydin AD, Yildiz H. Possible neoplastic effects of acrylamide on rat exocrine pancreas. Biotech Histochem. 2013;88:47–53.
Abedi-Ardekani B, Kamangar F, Hewitt SM, et al. Polycyclic aromatic hydrocarbon exposure in oesophageal tissue and risk of oesophageal squamous cell carcinoma in north-eastern Iran. Gut. 2010;59:1178–83.
Etemadi A, Islami F, Phillips DH, et al. Variation in PAH-related DNA adduct levels among non-smokers: the role of multiple genetic polymorphisms and nucleotide excision repair phenotype. Int J Cancer. 2013;132:2738–47.
Islami F, Boffetta P, van Schooten FJ, et al. Exposure to polycyclic aromatic hydrocarbons among never smokers in Golestan Province, Iran, an area of high incidence of esophageal cancer—a cross-sectional study with repeated measurement of urinary 1-OHPG in two seasons. Front Oncol. 2012;2:14.
Kamangar F, Strickland PT, Pourshams A, et al. High exposure to polycyclic aromatic hydrocarbons may contribute to high risk of esophageal cancer in northeastern Iran. Anticancer Res. 2005;25:425–8.
Marjani HA, Biramijamal F, Rakhshani N, Hossein-Nezhad A, Malekzadeh R. Investigation of NQO1 genetic polymorphism, NQO1 gene expression and PAH-DNA adducts in ESCC. A case–control study from Iran. Genet Mol Res. 2010;9:239–49.
Roshandel G, Semnani S, Malekzadeh R, Dawsey SM. Polycyclic aromatic hydrocarbons and esophageal squamous cell carcinoma. Arch Iran Med. 2012;15:713–22.
Anderson KE, Sinha R, Kulldorff M, et al. Meat intake and cooking techniques: associations with pancreatic cancer. Mutat Res. 2002;506–507:225–31.
Larsson SC, Wolk A. Red and processed meat consumption and risk of pancreatic cancer: meta-analysis of prospective studies. Br J Cancer. 2012;106:603–7.
Heinen MM, Verhage BA, Goldbohm RA, van den Brandt PA. Meat and fat intake and pancreatic cancer risk in the Netherlands Cohort study. Int J Cancer. 2009;125:1118–26.
Anderson KE, Mongin SJ, Sinha R, et al. Pancreatic cancer risk: associations with meat-derived carcinogen intake in the prostate, lung, colorectal, and ovarian cancer screening trial (PLCO) cohort. Mol Carcinog. 2012;51:128–37.
Michaud DS. Dietary meat, dairy products, fat, and cholesterol and pancreatic cancer risk in a prospective study. Am J Epidemiol. 2003;157:1115–25.
Stolzenberg-Solomon RZ, Cross AJ, Silverman DT, et al. Meat and meat-mutagen intake and pancreatic cancer risk in the NIH-AARP cohort. Cancer Epidemiol Biomarkers Prev. 2007;16:2664–75.
Larsson SC, Hakanson N, Permert J, Wolk A. Meat, fish, poultry and egg consumption in relation to risk of pancreatic cancer: a prospective study. Int J Cancer. 2006;118:2866–70.
Qin B, Xun P, He K. Fish or long-chain (n-3) PUFA intake is not associated with pancreatic cancer risk in a meta-analysis and systematic review. J Nutr. 2012;142:1067–73.
He K, Xun P, Brasky TM, Gammon MD, Stevens J, White E. Types of fish consumed and fish preparation methods in relation to pancreatic cancer incidence: the VITAL Cohort Study. Am J Epidemiol. 2013;177:152–60.
Rohrmann S, Linseisen J, Nothlings U, et al. Meat and fish consumption and risk of pancreatic cancer: results from the European prospective investigation into cancer and nutrition. Int J Cancer. 2013;132:617–24.
Larsson SC, Hakansson N, Naslund I, Bergkvist L, Wolk A. Fruit and vegetable consumption in relation to pancreatic cancer risk: a prospective study. Cancer Epidemiol Biomarkers Prev. 2006;15:301–5.
Ghadirian P, Nkondjock A. Consumption of food groups and the risk of pancreatic cancer: a case–control study. J Gastrointest Cancer. 2010;41:121–9.
Chan JM, Wang F, Holly EA. Vegetable and fruit intake and pancreatic cancer in a population-based case–control study in the San Francisco bay area. Cancer Epidemiol Biomarkers Prev. 2005;14:2093–7.
Nothlings U, Wilkens LR, Murphy SP, Hankin JH, Henderson BE, Kolonel LN. Vegetable intake and pancreatic cancer risk: the multiethnic cohort study. Am J Epidemiol. 2007;165:138–47.
Vrieling A, Verhage BA, van Duijnhoven FJ, et al. Fruit and vegetable consumption and pancreatic cancer risk in the European Prospective Investigation into Cancer and Nutrition. Int J Cancer. 2009;124:1926–34.
Jansen RJ, Robinson DP, Stolzenberg-Solomon RZ, et al. Fruit and vegetable consumption is inversely associated with having pancreatic cancer. Cancer Causes Control. 2011;22:1613–25.
Koushik A, Spiegelman D, Albanes D, et al. Intake of fruits and vegetables and risk of pancreatic cancer in a pooled analysis of 14 cohort studies. Am J Epidemiol. 2012;176:373–86.
Genkinger JM, Wang M, Li R, et al. Dairy products and pancreatic cancer risk: a pooled analysis of 14 cohort studies. Ann Oncol. 2014;25:1106–15.
Jansen RJ, Robinson DP, Frank RD, et al. Fatty acids found in dairy, protein and unsaturated fatty acids are associated with risk of pancreatic cancer in a case–control study. Int J Cancer. 2014;134:1935–46.
Conflict of interest
ZGh, AH, HEZ, SF, RR, RM, and AP declare no conflict of interest related to this work.
Ethics statement
The authors declare that the survey was performed in a manner that conforms to the Declaration of Helsinki of 1975, as revised in 2000 and 2008, concerning human and animal rights and that the authors followed the policy concerning informed consent wherever applicable as shown in www.Springer.com.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ghorbani, Z., Hekmatdoost, A., Zinab, H.E. et al. Dietary food groups intake and cooking methods associations with pancreatic cancer: A case–control study. Indian J Gastroenterol 34, 225–232 (2015). https://doi.org/10.1007/s12664-015-0573-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12664-015-0573-4