Abstract
Background and Aims
To determine the time to normalization of common bile duct (CBD) diameter after endoscopic sphincterotomy and stone extraction in patients with choledocholithiasis.
Methods
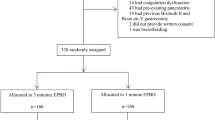
Patients with CBD dilation due to choledocholithiasis were enrolled. CBD diameter was measured by transabdominal ultrasonography before, and repeated after one, three, six and twelve months after endoscopic sphincterotomy and stone extraction, until normalization of CBD diameter.
Results
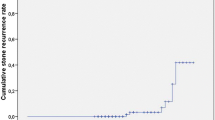
Of 115 cases enrolled over a 36-month period, CBD diameter reversed to normal in 71 (61.7%) patients after one month. Of the remaining 44 patients, CBD diameter reversed to normal in 36 patients (including 3 in whom repeat ERCP revealed choledocholithiasis) at the end of three months. CBD diameter had not reversed to normal diameter in 8 (18.2%) patients; none of these patients had symptoms. Two of them had asymptomatic dilated CBD after 6 months with no abnormal liver function tests (LFT); the duct reversed to normal at the last follow-up (month 12).
Conclusions
Asymptomatic CBD dilation may persist in a minority of patients (18% at the end of 3 months) after removal of CBD stones. A dilated CBD can be attributed to retained choledocholithiasis within the first month, if it is associated with symptoms and abnormal LFT.
Similar content being viewed by others
References
Karincaoglu M, Yildirim B, Seckin Y, Kantarceken B, Aladag M, Hilmioglu F. Common bile duct diameters after endoscopic sphincterotomy in patients with common bile duct stones: ultrasonographic evaluation. Abdom Imaging 2003;28:531–535.
Persson B, Olsson J. Variations of common bile duct diameter after endoscopic sphincterotomy. Gastrointest Radiol 1991;16:45–48.
Lacaine F, Corlette MB, Bismuth H. Preoperative evaluation of the risk of common bile duct stones. Arch Surg 1980;115:1114–1116.
Saltzstein EC, Peacock JB, Thomas MD. Preoperative bilirubin, alkaline phosphatase and amylase levels as predictors of common duct stones. Surg Gynecol Obstet 1982;154:381–384.
Abboud PA, Malet PF, Berlin JA, et al. Predictors of common bile duct stones prior to cholecystectomy: a metaanalysis. Gastrointest Endosc 1996;44:450–455.
Sgourakis G, Dedemadi G, Stamatelopoulos A, Leandros E, Voros D, Karaliotas K. Predictors of common bile duct lithiasis in laparoscopic era. World J Gastroenterol 2005;11:3267–3272.
Pasanen PA, Partanen KP, Pikkarainen PH, Alhava E.M, Janatuinen EK, Pirinen AE. A comparison of ultrasound, computed tomography and endoscopic retrograde cholangiopancreatography in the differential diagnosis of benign and malignant jaundice and cholestasis. Eur J Surg 1993;159:23–29.
Pedersen OM, Nordgard K, Kvinnsland S. Value of sonography in obstructive jaundice. Limitations of bile duct caliber as an index of obstruction. Scand J Gastroenterol 1987;22:975–981.
Freise J, Kleine P, Gebel M. Width of the lumen of the common bile duct: sonography compared with ERCP. Rontgenblatter 1985;38:241–243.
Mueller PR, Ferrucci JT Jr., Simeone JF, vanSonnenberg E, Hall DA, Wittenberg J. Observations on the distensibility of the common bile duct. Radiology 1982;142:467–472.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kolahdoozan, S., Sotoudehmanesh, R., Khatibian, M. et al. Long-term follow-up of common bile duct diameter after endoscopic sphincterotomy in patients with common bile duct stones. Indian J Gastroenterol 29, 28–31 (2010). https://doi.org/10.1007/s12664-010-0004-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12664-010-0004-5