Abstract
Background
Infertility is a source of stress, particularly in pronatalist societies in which a lifestyle without children is viewed as an unacceptable option. The present study examined the relationship between the use of culturally adapted religious coping strategies and emotional adjustment among women coping with fertility problems.
Methods
This is a cross-sectional correlational study. One hundred and eighty-six religious Israeli women undergoing fertility treatment filled out questionnaires assessing their use of culturally adapted religious coping strategies and emotional adjustment (distress/well-being).
Results
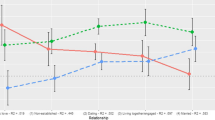
A path analysis showed that the culturally adapted religious coping strategies of seeking the support of Rabbis and seeking the support of God had a strong correlation with reduced psychological distress, but not with enhanced psychological well-being. Seeking approval and recognition from the community was correlated with reduced distress and enhanced well-being. However, seeking ties and belonging to the community was correlated with increased psychological distress and reduced psychological well-being. Finally, women without children experienced greater psychological distress than women with children and sought more support of Rabbis and fewer ties with the community.
Conclusions
In a pronatalist culture that sanctifies childbirth, infertility is a source of significant distress. Professionals’ awareness of the culturally adapted religious coping strategies utilized by their clients may help them conduct culturally sensitive intervention, which may greatly help to enhance emotional adjustment. Future research is recommended to develop instruments that measure culturally adapted strategies and their influence on emotional adjustment over time, in different states of health while comparing different cultures.

Similar content being viewed by others
Notes
1Since the counseling institute is equal to high seeking of support of Rabbis, and these women did not differ from other participants in any other respect, controlling for recruitment source may have removed valid variance in the variable Seeking the Support of Rabbis and artificially diminished the contribution of this variable.
References
Gana K, Jakubowska S. Relationship between infertility-related stress and emotional distress and marital satisfaction. J Health Psychol. 2016;21(6):1043–54.
Sexton MB, Byrd MR, Von Kluge S. Measuring resilience in women experiencing infertility using the CD-RISC: examining infertility-related stress, general distress, and coping styles. J Psychiatr Res. 2010;44(4):236–41.
Greil AL, McQuillan J, Sanchez D. Does fertility specific distress vary by race/ethnicity among a probability sample of women in the United States? J Health Psychol. 2014;21(2):183–92.
Hampshire KR, Blell MT, Simpson B. ‘Everybody is moving on’: infertility, relationality and the aesthetics of family among British-Pakistani Muslims. Soc Sci Med. 2012;74(7):1045–52.
Benyamini Y, Gozlan M, Weissman A. Normalization as a strategy for maintaining quality of life while coping with infertility in a pronatalist culture. Int J Behav Med. 2017;24(6):871–9.
Holter H, Anderheim L, Bergh C, Möller A. First IVF treatment—short-term impact on psychological well-being and the marital relationship. Hum Reprod. 2006;21(12):3295–302.
Neter E, Goren S. Infertility centrality in the woman’s identity and goal adjustment predict psychological adjustment among women in ongoing fertility treatments. Int J Behav Med. 2017;24(6):880–92.
Bergart AM. The experience of women in unsuccessful infertility treatment: what do patients need when medical intervention fails? Soc Work Health Care. 2000;30(4):45–69.
Benyamini Y, Gozlan M, Kokia E. Variability in the difficulties experienced by women undergoing infertility treatments. Fertil Steril. 2005;83(2):275–83.
Leon IG. Understanding and treating infertility: psychoanalytic considerations. J Am Acad Psychoanal Dyn Psychiatry. 2010;38(1):47–75.
Remennick L. Childless in the land of imperative motherhood: stigma and coping among infertile Israeli women. Sex Roles. 2000;43(11):821–41.
Cousineau TM, Domar AD. Psychological impact of infertility. Best Pract Res Clin Obstet Gynaecol. 2007;21(2):293–308.
Greil AL, Slauson-Blevins K, McQuillan J. The experience of infertility: a review of recent literature. Sociol Health Illn. 2010;32(1):140–62.
Israel Ministry of Health. 2017. https://www.health.gov.il/Subjects/fertility/ovum_donation. Accessed Apr 09, 2018.
Domar AD, Clapp D, Slawsby E, Kessel B, Orav J, Freizinger M. The impact of group psychological interventions on distress in infertile women. Health Psychol. 2000;19(6):568–75.
Haelyon H. “Longing for a child”: perceptions of motherhood among Israeli-Jewish women undergoing in vitro fertilization treatments. A J Of Jewish. 2006;12:177–202.
Granek L, Nakash O. The impact of militarism, patriarchy, and culture on Israeli women’s reproductive health and well-being. Int J Behav Med. 2017;24(6):893–900.
Kahn SM. Reproducing Jews: a cultural account of assisted conception in Israel. Durham: Duke University Press; 2000.
Israel Ministry of Health. 2010. https://www.health.gov.il/UnitsOffice/HD/MTI/info/Pages. Accessed Apr 09, 2018.
Chandra A, Martinez GM, Mosher WD, Abma JC, Jones J. Fertility, family planning, and reproductive health of US women; data from the 2002 National Survey of Family Growth. Vital Health Stat. 2005;23(25):1–174.
Knesset Research and Information Center. 2012. http://main.knesset.gov.il/Activity/Info/MMM/Pages/search.aspx?mode=advancedPlusText&searchValue. Accessed Apr 05, 2018.
Sullivan EA, Zegers-Hochschild F, Mansour R, Ishihara O, de Mouzon J, Nygren KG, et al. International Committee for Monitoring Assisted Reproductive Technologies (ICMART) world report: assisted reproductive technology 2004. Hum Reprod. 2013;28(5):1375–90.
Nachtigall RD. International disparities in access to infertility services. Fertil Steril. 2006;85(4):871–5.
Simonstein F. A rational cure for prereproductive stress syndrome—a perspective from Israel: a rejoinder to Häyry, Bennet, Holm, and Aksoy. J Med Ethics. 2005;31(9):557.
Sheleg Y. The new religious: a contemporary look at religious society in Israel. Jerusalem: Keter Press; 2000.
Rapoport T, Garb Y, Penso A. Religious socialization and female subjectivity: religious-Zionist adolescent girls in Israel. Sociol Educ. 1995;68(1):48–61.
Kulik L. The sense of empowerment, life values, and the centrality of working life among ultra-Orthodox Jewish women in the labor market. Ramat Gan: University Press; 2012.
Weizmann G. “Give me children or else I dead”: orthodox Jewish perspectives on fertility. In: Blyth E, Landau R, editors. Faith and fertility: attitudes towards reproductive practices in different religions from ancient to modern times. London: Jessica Kingsley Publishers; 2009. p. 205–24.
Benyamini Y, Gefen-Bardarian Y, Gozlan M, Tabiv G, Shiloh S, Kokia E. Coping specificity: the case of women coping with infertility treatments. Psychol Health. 2008;23(2):221–41.
Terry DJ, Hynes GJ. Adjustment to a low-control situation: reexamining the role of coping responses. J Pers Soc Psychol. 1998;74(4):1078–92.
Lansakara N, Wickramasinghe AR, Seneviratne HR. Feeling the blues of infertility in a South Asian context: psychological well-being and associated factors among Sri Lankan women with primary infertility. Women Health. 2011;51(4):383–99.
Koenig HG, King DE, Carson VB. Handbook of religion and health. 2nd ed. New York: Oxford University Press; 2012.
Pargament KI. The psychology of religion and coping: theory, research, practice. New York: Guilford Press; 1997.
Pargament KI. Spiritually integrated psychotherapy. New York: Guilford Press; 2007.
Pargament KI, Koenig HG, Perez LM. The many methods of religious coping: development and initial validation of the RCOPE. J Clin Psychol. 2000;56(4):519–43.
Rosmarin DH, Pirutinsky S, Pargament KI, Krumrei EJ. Are religious beliefs relevant to mental health among Jews? Psychol Relig Spiritual. 2009;1(3):180–90.
Nouman H, Benyamini Y. Religious coping in stressful situations: developing the JRP-COPE measurement tool for religious Jewish population. Arch Psychol Relig. 2016;38(2):184–209.
Rosmarin DH, Pargament KI, Krumrei EJ, Flannelly KJ. Religious coping among Jews: development and initial validation of the JCOPE. J Clin Psychol. 2009;65(7):670–83.
Coleman-Brueckheimer K, Spitzer J, Koffman J. Involvement of Rabbinic and communal authorities in decision-making by Haredi Jews in the UK with breast cancer: an interpretative phenomenological analysis. Soc Sci Med. 2009;68(2):323–33.
Firer M. Seeking professional psychological help in the ultra-Orthodox population. Ramat Gan: University Press; 2001.
Greenfield EA, Marks NF. Religious social identity as an explanatory factor for associations between more frequent formal religious participation and psychological well-being. Int J Psychol Relig. 2007;17(3):245–59.
Beit-Hallahmi B, Argyle M. The psychology of religious behavior belief and experience. London: Routledge Press; 1997.
Fiala WE, Bjorck JP, Gorsuch R. The religious support scale: construction, validation, and cross-validation. Am J Community Psychol. 2002;30(6):761–86.
Ben-Meir Y, Kedem PA. Measure of religiosity for the Jewish population of Israel. Megamot. 1979;24(3):353–62.
Stanton AL. Cognitive appraisals, coping processes, and adjustment to infertility. In: Stanton AL, Dunkel-Schetter C, editors. Infertility: perspective from stress and coping research. New-York: Plenum Press; 1991. p. 87–108.
Benyamini Y, Gozlan M, Kokia E. On the self-regulation of a health for threat: cognitions, coping, and emotions among women undergoing treatment infertility. Cogn Ther Res. 2004;28(5):577–92.
Faul F, Erdfelder E, Buchner A, Lang AG. Statistical power analyses using G* power 3.1: tests for correlation and regression analyses. Behav Res Methods. 2009;41(4):1149–60.
Kline RB. Principles and practice of structural equation modeling. New York: The Guilford Press; 2005.
Leventhal H, Meyer D, Nerenz DR. The common sense representation of illness danger. In: Rachman S, editor. Contributions to medical psychology. New York: Pargamon Press; 1980. p. 17–30.
Hollos M, Larsen U, Obono O, Whitehouse B. The problem of infertility in high fertility populations: meanings, consequences and coping mechanisms in two Nigerian communities. Soc Sci Med. 2009;68(11):2061–8.
Nahar P. Health seeking behaviour of childless women in Bangladesh: an ethnographic exploration for the special issue on: loss in child bearing. Soc Sci Med. 2010;71(10):1780–7.
Benyamini Y. Stress and coping with women’s health issues: a review from a self-regulation perspective. Eur Psychol. 2009;14(1):63–71.
Rosmarin DH, Pargament KI, Pirutinsky S, Mahoney A. A randomized controlled evaluation of a spiritually integrated treatment for subclinical anxiety in the Jewish community, delivered via the Internet. J Anxiety Disord. 2010;24(7):799–808.
Hobfoll SE. Conservation of resources: a new attempt at conceptualizing stress. Am Psychol. 1989;44(3):513–24.
Lazar A, Bjorck JP. Religious support and psychosocial well-being among a religious Jewish population. Ment Health Relig Cult. 2008;11(4):403–21.
Hill PC, Pargament KI. Advances in the conceptualization and measurement of religion and spirituality: implications for physical and mental health research. Am Psychol. 2008;S(1):3–17.
Greil A, McQuillan J, Slauson-Blevins K. The social construction of infertility. Sociol Compass. 2011;5(8):736–46.
Mindes EJ, Ingram KM, Kliewer W, James CA. Longitudinal analyses of the relationship between unsupportive social interactions and psychological adjustment among women with fertility problem. Soc Sci Med. 2003;56(10):2165–80.
Slade P, O'Neill C, Simpson AJ, Lashen H. The relationship between perceived stigma, disclosure patterns, support and distress in new attendees at an infertility clinic. Hum Reprod. 2007;22(8):2309–17.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nouman, H., Benyamini, Y. Religious Women’s Coping with Infertility: Do Culturally Adapted Religious Coping Strategies Contribute to Well-Being and Health?. Int.J. Behav. Med. 26, 154–164 (2019). https://doi.org/10.1007/s12529-018-9757-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12529-018-9757-5