Abstract
Background
Studies in western clinical settings suggest that touch screen computer surveys are an acceptable mode of collecting information about cancer patients’ wellbeing
Purpose
We examined the acceptability of a touch screen tablet survey among cancer patients in Japan.
Methods
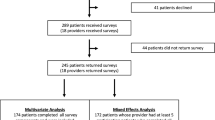
Eligible patients (n = 262) attending a university hospital radiation therapy (RT) department were invited to complete a touch screen tablet survey about psychosocial communication and care. Survey consent and completion rates, the proportion and characteristics of patients who completed the touch screen survey unassisted, and patient-reported acceptability were assessed.
Results
Of 158 consenting patients (consent rate 60 % [95 % CI 54, 66 %] of eligible patients), 152 completed the touch screen computer survey (completion rate 58 % [95 % CI 52, 64 %] of eligible patients). The survey was completed without assistance by 74 % (n = 113; 95 % CI 67, 81 %) of respondents. Older age was associated with higher odds of having assistance with survey completion (OR 1.09; 95 % CI 1.04, 1.14 %). Ninety-two percent of patients (95 % CI 86, 96 %) felt that the touch screen survey was easy to use and 95 % (95 % CI 90, 98 %) agreed or strongly agreed that they were comfortable answering the questions. Overall, 65 % (95 % CI 57, 73 %) of respondents would be willing to complete such a survey more than once while waiting for RT treatment.
Conclusions
Although patient self-reported acceptability of the touch screen survey was high, self-administered touch screen tablet surveys may not be entirely appropriate for older cancer patients or possibly for patients with lower educational attainment.

Similar content being viewed by others
References
Carter G, Britton B, Clover K, Rogers K, Adams C, McElduff P. Effectiveness of QUICATOUCH: a computerised touch screen evaluation for pain and distress in ambulatory oncology patients in Newcastle, Australia. Psychooncology. 2012;21(11):1149–57. doi:10.1002/pon.2020.
Cull A, Gould A, House A, et al. Validating automated screening for psychological distress by means of computer touchscreens for use in routine oncology practice. Br J Cancer. 2001;85(12):1842–9. doi:10.1054/bjoc.2001.2182.
Newell S, Girgis A, Sanson-Fisher R, Steward J. Are touchscreen computer surveys acceptable to medical oncology patients. J Psychosoc Oncol. 1997;15:37–46. doi:10.1300/J077v15n02_03.
DiRocco DN, Day SC. Obtaining patient feedback at point of service using electronic kiosks. Am J Manag Care. 2011;17(7):e270–e6.
Mackenzie LJ, Sanson-Fisher RW, Carey ML, D’Este CA. Radiation oncology outpatient perceptions of patient-centred care: a cross-sectional survey. BMJ open. 2013;3(2). doi:10.1136/bmjopen-2012-001265.
Mackenzie LJ, Carey ML, Sanson-Fisher RW, D’Este CA. Psychological distress in cancer patients undergoing radiation therapy treatment. Support Care Cancer : Off J Multinatl Assoc Support Care Cancer. 2013;21(4):1043–51. doi:10.1007/s00520-012-1624-3.
Aiello EJ, Taplin S, Reid R, et al. In a randomized controlled trial, patients preferred electronic data collection of breast cancer risk-factor information in a mammography setting. J Clin Epidemiol. 2006;59(1):77–81.
Allenby A, Matthews J, Beresford J, McLachlan SA. The application of computer touch-screen technology in screening for psychosocial distress in an ambulatory oncology setting. Eur J Cancer Care (Engl). 2002;11(4):245–53.
Velikova G, Wright EP, Smith AB, et al. Automated collection of quality-of-life data: a comparison of paper and computer touch-screen questionnaires. J Clin Oncol. 1999;17(3):998.
McCleary NJ, Wigler D, Berry D, et al. Feasibility of computer-based self-administered cancer-specific geriatric assessment in older patients with gastrointestinal malignancy. Oncologist. 2013;18(1):64–72. doi:10.1634/theoncologist.2012-0241.
Zarghom S, Di Fonzo D, Leung FH. Does socioeconomic status affect patients’ ease of use of a touch-screen (iPad) patient survey? Interact J Med Res. 2013;2(1):e1. doi:10.2196/ijmr.2314.
Umemuro H. Computer attitudes, cognitive abilities, and technology usage among older Japanese adults. Gerontechnology. 2004;3(2):64–76.
Umemuro H. Lowering elderly Japanese users’ resistance towards computers by using touchscreen technology. Univ Access Inf Soc. 2004;3(3-4):276–88. doi:10.1007/s10209-004-0098-6.
Ramers-Verhoeven CW, Geipel GL, Howie M. New insights into public perceptions of cancer. ecancer. 2013. doi:10.3332/ecancer.2013.349.
Nakanotani T, Akechi T, Takayama T, et al. Characteristics of elderly cancer patients’ concerns and their quality of life in Japan: a web-based survey. Jpn J Clin Oncol. 2014;44(5):448–55. doi:10.1093/jjco/hyu029.
Umezawa S, Fujisawa D, Fujimori M, Ogawa A, Matsushima E, Miyashita M. Prevalence, associated factors and source of support concerning supportive care needs among Japanese cancer survivors. Psycho-Oncol. 2014:n/a-n/a. doi:10.1002/pon.3702.
Bullinger M, Alonso J, Apolone G, et al. Translating health status questionnaires and evaluating their quality: the IQOLA Project approach. International Quality of Life Assessment. J Clin Epidemiol. 1998;51(11):913–23. doi:S0895435698000821 [pii].
Mackenzie LJ, Carey ML, Sanson-Fisher RW, D’Este CA, Hall AE. Cancer patients’ willingness to answer survey questions about life expectancy. Support Care Cancer : Off J Multinatl Assoc Support Care Cancer. 2012;20(12):3335–41. doi:10.1007/s00520-012-1477-9.
Zigmond AS, Snaith RP. The hospital anxiety and depression scale with the irritability depression-anxiety scale and the leeds situational anxiety scale manual. London: GL Assessment Ltd; 1994.
Kugaya A, Akechi T, Okuyama T, Okamura H, Uchitomi Y. Screening for psychological distress in Japanese cancer patients. Jpn J Clin Oncol. 1998;28(5):333–8.
Akechi T, Okuyama T, Endo C, et al. Patient’s perceived need and psychological distress and/or quality of life in ambulatory breast cancer patients in Japan. Psycho-Oncology. 2011;20(5):497–505. doi:10.1002/pon.1757.
Miura K, Ando S, Imai T. The association of cognitive fatigue with menopause, depressive symptoms, and quality of life in ambulatory breast cancer patients. Breast Cancer. 2014:1-8. doi:10.1007/s12282-014-0578-3.
Kendall J, Glaze K, Oakland S, Hansen J, Parry C. What do 1281 distress screeners tell us about cancer patients in a community cancer center? Psycho-Oncology. 2011;20(6):594–600. doi:10.1002/pon.1907.
Pirl WF, Fann JR, Greer JA, et al. Recommendations for the implementation of distress screening programs in cancer centers: report from the American Psychosocial Oncology Society (APOS), Association of Oncology Social Work (AOSW), and Oncology Nursing Society (ONS) joint task force. Cancer. 2014;120(19):2946–54. doi:10.1002/cncr.28750.
Wilcox AB, Gallagher KD, Boden-Albala B, Bakken SR. Research data collection methods: from paper to tablet computers. Med Care. 2012;50(Suppl):S68–73. doi:10.1097/MLR.0b013e318259c1e7.
Acknowledgments
The data presented in this manuscript were presented in part at the IPOS 14th World Congress of Psycho-Oncology. The authors would like to acknowledge Dr. Masakazu Ogura, Prof. Masahiro Hiraoka, and Ms. Ayako Fujii for their support and assistance with project management and patient recruitment. We would also like to thank the radiation oncology department patients and staff for participating in this research study. This research was funded by Dr. Lisa Mackenzie’s Endeavour Scholarship, and Lisa is currently supported by a HMRI Early Career Support Grant.
Conflict of Interest
The authors declare that they have no competing interests.
Informed Consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000. Informed consent was obtained from all patients for being included in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Suzuki, E., Mackenzie, L., Sanson-Fisher, R. et al. Acceptability of a Touch Screen Tablet Psychosocial Survey Administered to Radiation Therapy Patients in Japan. Int.J. Behav. Med. 23, 485–491 (2016). https://doi.org/10.1007/s12529-015-9502-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12529-015-9502-2