Abstract
Background
Cardiac resynchronization therapy (CRT) patients with different pathophysiology may influence mechanical dyssynchrony and get different ventricular resynchronization and clinical outcomes.
Methods
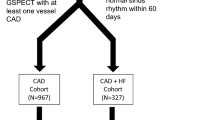
Ninety-two dilated cardiomyopathy (DCM) and fifty ischemic cardiomyopathy (ICM) patients with gated single-photon emission computed tomography (SPECT) myocardial perfusion imaging (MPI) were included in this retrospective study. Patients were classified based on the concordance between the left ventricular (LV) lead and the latest contraction or relaxation position. If the LV lead was located on or adjacent to both the latest contraction and relaxation position, the patient was categorized into the both match group; if the LV lead was located on or adjacent to the latest contraction or relaxation position, the patient was classified into the one match group; if the LV lead was located on or adjacent to neither the latest contraction nor relaxation position, the patient was categorized to the neither group. CRT response was defined as \(\ge 5\%\) improvement of LV ejection fraction at the 6-month follow-up. Variables with P < .05 in the univariate analysis were included in the stepwise multivariate model.
Results
During the follow-up period, 58.7% (54 of 92) for DCM patients and 54% (27 of 50) for ICM patients were CRT responders. The univariate analysis and stepwise multivariate analysis showed that QRS duration, systolic phase bandwidth (PBW), diastolic PBW, diastolic phase histogram standard deviation (PSD), and left ventricular mechanical dyssynchrony (LVMD) concordance were independent predictors of CRT response in DCM patients; diabetes mellitus and left ventricular end-systolic volume were significantly associated with CRT response in ICM patients. The intra-group comparison revealed that the CRT response rate was significantly different in the both match group of DCM (N = 18, 94%) and ICM (N = 24, 62%) patients (P = .016). However, there was no significant difference between DCM and ICM in the one match and neither group. For the inter-group comparison, Kruskal-Wallis H-test revealed that CRT response was significantly different in all the groups of DCM patients (P < .001), but not in ICM patients (P = .383).
Conclusions
Compared with ICM patients, systolic PBW, diastolic PBW and PSD have better predictive and prognostic values for the CRT response in DCM patients. Placing the LV lead in or adjacent to the latest contraction and relaxation position can improve the clinical outcomes of DCM patients, but it does not apply to ICM patients.





Similar content being viewed by others
Change history
19 October 2021
A Correction to this paper has been published: https://doi.org/10.1007/s12350-021-02834-0
Abbreviations
- CRT:
-
Cardiac resynchronization therapy
- DCM:
-
Dilated cardiomyopathy
- ICM:
-
Ischemic cardiomyopathy
- LV:
-
Left ventricular
- LVEDV:
-
Left ventricular end-diastolic volume
- LVEF:
-
Left ventricular ejection fraction
- LVESV:
-
Left ventricular end-systolic volume
- LVMD:
-
Left ventricular mechanical dyssynchrony
- MPI:
-
Myocardial perfusion imaging
- PBW:
-
Phase bandwidth
- PSD:
-
Phase histogram standard deviation
References
Fornwalt BK, Sprague WW, Bedell P, Suever JD, Gerritse B, Merlino JD, et al. Agreement is poor among current criteria used to define response to cardiac resynchronization therapy. Circulation 2010;121:1985-91.
Zhou W, Garcia EV. Nuclear image-guided approaches for cardiac resynchronization therapy (CRT). Curr Cardiol Rep 2016;18:7.
Trimble MA, Velazquez EJ, Adams GL, Honeycutt EF, Pagnanelli RA, Barnhart HX, et al. Repeatability and reproducibility of phase analysis of gated single-photon emission computed tomography myocardial perfusion imaging used to quantify cardiac dyssynchrony. Nucl Med Commun 2008;29:374-81.
Lin X, Xu H, Zhao X, Folks RD, Garcia EV, Soman P, et al. Repeatability of left ventricular dyssynchrony and function parameters in serial gated myocardial perfusion SPECT studies. J Nucl Cardiol 2010;17:811-6.
Henneman MM, Chen J, Dibbets-Schneider P, Stokkel MP, Bleeker GB, Ypenburg C, et al. Can LV dyssynchrony as assessed with phase analysis on gated myocardial perfusion SPECT preferably predict response to CRT? J Nucl Med 2007;48:1104-11.
Tsai SC, Chang YC, Chiang KF, Lin WY, Huang JL, Hung GU, et al. LV dyssynchrony is helpful in predicting ventricular arrhythmia in ischemic cardiomyopathy after cardiac resynchronization therapy a preliminary study. Medicine (United States) 2016;95:e2840.
Pazhenkottil AP, Buechel RR, Husmann L, Nkoulou RN, Wolfrum M, Ghadri JR, et al. Long-term prognostic value of left ventricular dyssynchrony assessment by phase analysis from myocardial perfusion imaging. Heart 2011;97:33-7.
Wang L, Yang MF, Cai M, Zhao SH, He ZX, Wang YT. Prognostic significance of left ventricular dyssynchrony by phase analysis of gated spect in medically treated patients with dilated cardiomyopathy. Clin Nucl Med 2013;38:510-5.
Zhang X, Qian Z, Tang H, Hua W, Su Y, Xu G, et al. A new method to recommend left ventricular lead positions for improved CRT volumetric response and long-term prognosis. J Nucl Cardiol 2019;28:672-84.
Wang C, Shi J, Ge J, Tang H, He Z, Liu Y, et al. Left ventricular systolic and diastolic dyssynchrony to improve cardiac resynchronization therapy response in heart failure patients with dilated cardiomyopathy. J Nucl Cardiol 2020. https://doi.org/10.1007/s12350-020-02132-1.
Elliott P, Andersson B, Arbustini E, Bilinska Z, Cecchi F, Charron P, et al. Classification of the cardiomyopathies: A position statement from the european society of cardiology working group on myocardial and pericardial diseases. Eur Heart J 2008;29:270-6.
Bose A, Kandala J, Upadhyay GA, Riedl L, Ahmado I, Padmanabhan R, et al. Impact of myocardial viability and left ventricular lead location on clinical outcome in cardiac resynchronization therapy recipients with ischemic cardiomyopathy. J Cardiovasc Electrophysiol 2014;25:507-13.
Chen J, Kalogeropoulos AP, Verdes L, Butler J, Garcia EV. Left-ventricular systolic and diastolic dyssynchrony as assessed by multi-harmonic phase analysis of gated SPECT myocardial perfusion imaging in patients with end-stage renal disease and normal LVEF. J Nucl Cardiol 2011;18:299-308.
Chen J, Garcia EV, Folks RD, Cooke CD, Faber TL, Tauxe EL, et al. Onset of left ventricular mechanical contraction as determined by phase analysis of ECG-gated myocardial perfusion SPECT imaging: Development of a diagnostic tool for assessment of cardiac mechanical dyssynchrony. J Nucl Cardiol 2005;12:687-95.
Singh JP, Klein HU, Huang DT, Reek S, Kuniss M, Quesada A, et al. Left ventricular lead position and clinical outcome in the multicenter automatic defibrillator implantation trial–cardiac resynchronization therapy (MADIT-CRT) trial. Circulation 2011. https://doi.org/10.1161/CIRCULATIONAHA.110.000646.
Seabold S, Perktold J. Statsmodels: Econometric and statistical modeling with Python. In: Proceedings of the 9th Python in Science Conference; 2010. p. 92-96.
Goldberg AS, Alraies MC, Cerqueira MD, Jaber WA, Aljaroudi WA. Prognostic value of left ventricular mechanical dyssynchrony by phase analysis in patients with non-ischemic cardiomyopathy with ejection fraction 35-50% and QRS < 150 ms. J Nucl Cardiol 2014;21:57-66.
Peix A, Karthikeyan G, Massardo T, Kalaivani M, Patel C, Pabon LM, et al. Value of intraventricular dyssynchrony assessment by gated-SPECT myocardial perfusion imaging in the management of heart failure patients undergoing cardiac resynchronization therapy (VISION-CRT). J Nucl Cardiol 2019. https://doi.org/10.1007/s12350-018-01589-5.
Peix A, Padrón K, Cabrera L, Castañeda O, Milán D, Castro J, et al. Intraventricular synchronism assessment by gated - SPECT myocardial perfusion imaging in cardiac resynchronization therapy. Does cardiomyopathy type influence results? EJNMMI Res 2020. https://doi.org/10.1186/s13550-020-00703-4.
Ludwig DR, Friehling M, Schelbert EB, Schwartzman D. Impact of scar on SPECT assay of left ventricular contraction dyssynchrony. Eur J Nucl Med Mol Imaging 2014;41:529-35.
Yokoshiki H, Mitsuyama H, Watanabe M, Mitsuhashi T, Shimizu A. Cardiac resynchronization therapy in ischemic and non-ischemic cardiomyopathy. J Arrhythmia 2017;33:410-6.
Aljaroudi W, Alraies MC, Menon V, Jaber WA. Predictors and incremental prognostic value of left ventricular mechanical dyssynchrony response during stress-gated positron emission tomography in patients with ischemic cardiomyopathy. J Nucl Cardiol 2012. https://doi.org/10.1007/s12350-012-9592-z.
Boogers MJ, Chen J, Van Bommel RJ, Borleffs CJW, Dibbets-Schneider P, Van Der Hiel B, et al. Optimal left ventricular lead position assessed with phase analysis on gated myocardial perfusion SPECT. Eur J Nucl Med Mol Imaging 2011;38:230-8.
Lin X, Xu H, Zhao X, Chen J. Sites of latest mechanical activation as assessed by SPECT myocardial perfusion imaging in ischemic and dilated cardiomyopathy patients with LBBB. Eur J Nucl Med Mol Imaging 2014;41:1232-9.
Ypenburg C, Schalij MJ, Bleeker GB, Steendijk P, Boersma E, Dibbets-Schneider P, et al. Impact of viability and scar tissue on response to cardiac resynchronization therapy in ischaemic heart failure patients. Eur Heart J 2007;28:33-41.
Adelstein EC, Tanaka H, Soman P, Miske G, Haberman SC, Saba SF, et al. Impact of scar burden by single-photon emission computed tomography myocardial perfusion imaging on patient outcomes following cardiac resynchronization therapy. Eur Heart J 2011;32:93-103.
Disclosure
All authors declare that there are no conflicts of interest.
Author information
Authors and Affiliations
Contributions
ZH—Contribution: Conception and design; analysis and interpretation of data; drafting of the manuscript and revising it critically for important intellectual content. DL—Contribution: Revising it critically for important intellectual content. CC—Contribution: Revising it critically for important intellectual content. H-YQ—Contribution: Revising it critically for important intellectual content. ZZ—Contribution: Revising it critically for important intellectual content. XH—Contribution: Revising it critically for important intellectual content. JZ—Contribution: Revising it critically for important intellectual content. M-LC—Contribution: Revising it critically for important intellectual content. CW—Contribution: Acquisition, analysis, and interpretation of data; revising the manuscript critically for important intellectual content. WZ—Contribution: Conception and design; analysis and interpretation of data; revising the manuscript critically for important intellectual content; and final approval of the manuscript submitted.
Corresponding authors
Ethics declarations
Ethical approval
The study was approved by the scientific councils of the participating county scientific councils and complied with the Declaration of Helsinki. Written informed consent was obtained from all participants, and patient anonymity was maintained during data analysis.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The authors of this article have provided a PowerPoint file, available for download at SpringerLink, which summarises the contents of the paper and is free for re-use at meetings and presentations. Search for the article DOI on SpringerLink.com.
The authors have also provided an audio summary of the article, which is available to download as ESM, or to listen to via the JNC/ASNC Podcast.
All editorial decisions for this article, including selection of reviewers and the final decision, were made by guest editor Saurabh Malhotra, MD, MPH.
Funding
This research was supported by a grant from the American Heart Association (Project Number: 17AIREA33700016, PI: Weihua Zhou) and a new faculty grant from Michigan Technological University Institute of Computing and Cybersystems (PI: Weihua Zhou), and grants from the National Nature Science Foundation of China (81900295) and the Natural Science Foundation of Jiangsu Province (BK 20191071).
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
He, Z., Li, D., Cui, C. et al. Predictive values of left ventricular mechanical dyssynchrony for CRT response in heart failure patients with different pathophysiology. J. Nucl. Cardiol. 29, 2637–2648 (2022). https://doi.org/10.1007/s12350-021-02796-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12350-021-02796-3