Abstract
Background
We investigated role of coronary microvascular disease (CMD) in maladaptive LV remodeling and prognosis in patients with aortic sclerosis or stenosis and no overt CAD.
Methods
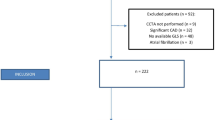
This was a retrospective cohort study of patients with aortic sclerosis or stenosis, normal myocardial perfusion and LV ejection fraction (EF) > 50% (n = 43) and matched controls without AS (n = 43). PET and echocardiograms were performed within 1 year of each other. Myocardial perfusion and myocardial flow reserve (MFR) were quantified using PET imaging. LV structure and function, including global longitudinal strain (GLS), were quantified by transthoracic echocardiography.
Results
Global MFR declined with increasing AS severity (P = 0.04). Probability of impaired MFR increased with severity of adverse LV remodeling (OR 1.88, CI 1.03 to 3.41, P =0.04). Reduced MFR associated with impaired GLS (r = − 0.29, P = 0.002) and associated with reduced MACE-free survival at 7.27 years median follow-up. Adjusted annualized rate of MACE was highest in those with impaired GLS and MFR and lowest in those with normal GLS and MFR (30.99% vs 1.86%, P =0.002).
Conclusion and Relevance
In patients with AS and no overt CAD, impaired MFR associates with adverse LV remodeling and subclinical LV mechanical dysfunction, and is a marker increased clinical risk.


Similar content being viewed by others
Abbreviations
- AS:
-
Aortic stenosis
- AVR:
-
Aortic valve replacement
- CMD:
-
Coronary microvascular dysfunction
- GLS:
-
Global longitudinal strain
- LVH:
-
Left ventricular hypertrophy
- MBF:
-
Myocardial blood flow
- MFR:
-
Myocardial flow reserve
- PET:
-
Positron emission tomography
- SSS:
-
Summed stress score
References
Nkomo VT, Gardin JM, Skelton TN, Gottdiener JS, Scott CG, Enriquez-Sarano M. Burden of valvular heart diseases: A population-based study. Lancet. 2006;368:1005-11.
Nishimura RA, Otto CM, Bonow RO, Carabello BA, Erwin JP 3rd, Fleisher LA, et al 2017 AHA/ACC focused update of the 2014 AHA/ACC Guideline for the Management of Patients With Valvular Heart Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2017;70:252-89.
Pellikka PA, Sarano ME, Nishimura RA, Malouf JF, Bailey KR, Scott CG, et al Outcome of 622 adults with asymptomatic, hemodynamically significant aortic stenosis during prolonged follow-up. Circulation. 2005;111:3290-5.
Kapadia SR, Tuzcu EM, Makkar RR, Svensson LG, Agarwal S, Kodali S, et al Long-term outcomes of inoperable patients with aortic stenosis randomly assigned to transcatheter aortic valve replacement or standard therapy. Circulation. 2014;130:1483-92.
Arnold SV, Spertus JA, Vemulapalli S, Li Z, Matsouaka RA, Baron SJ, et al Quality-of-life outcomes after transcatheter aortic valve replacement in an unselected population: A report From the STS/ACC transcatheter valve therapy registry. JAMA Cardiol. 2017;2:409-16.
Dweck MR, Boon NA, Newby DE. Calcific aortic stenosis: A disease of the valve and the myocardium. J Am Coll Cardiol. 2012;60:1854-63.
Azevedo CF, Nigri M, Higuchi ML, Pomerantzeff PM, Spina GS, Sampaio RO, et al Prognostic significance of myocardial fibrosis quantification by histopathology and magnetic resonance imaging in patients with severe aortic valve disease. J Am Coll Cardiol. 2010;56:278-87.
Galiuto L, Lotrionte M, Crea F, Anselmi A, Biondi-Zoccai GG, De Giorgio F, et al Impaired coronary and myocardial flow in severe aortic stenosis is associated with increased apoptosis: A transthoracic Doppler and myocardial contrast echocardiography study. Heart. 2006;92:208-12.
Barone-Rochette G, Pierard S, De Meester de Ravenstein C, Seldrum S, Melchior J, Maes F, et al Prognostic significance of LGE by CMR in aortic stenosis patients undergoing valve replacement. J Am Coll Cardiol. 2014;64:144-54.
Weidemann F, Herrmann S, Stork S, Niemann M, Frantz S, Lange V, et al Impact of myocardial fibrosis in patients with symptomatic severe aortic stenosis. Circulation. 2009;120:577-84.
Treibel TA, Kozor R, Schofield R, Benedetti G, Fontana M, Bhuva AN, et al Reverse myocardial remodeling following valve replacement in patients with aortic stenosis. J Am Coll Cardiol. 2018;71:860-71.
Meimoun P, Germain AL, Elmkies F, Benali T, Boulanger J, Espanel C, et al Factors associated with noninvasive coronary flow reserve in severe aortic stenosis. J Am Soc Echocardiogr. 2012;25:835-41.
Nemes A, Forster T, Varga A, Vass A, Borthaiser A, Pálinkás A, et al How can coronary flow reserve be altered by severe aortic stenosis? Echocardiography. 2002;19:655-9.
Rajappan K, Rimoldi OE, Dutka DP, Ariff B, Pennell DJ, Sheridan DJ, et al Mechanisms of coronary microcirculatory dysfunction in patients with aortic stenosis and angiographically normal coronary arteries. Circulation. 2002;105:470.
Marcus ML. Importance of abnormalities in coronary flow reserve to the pathophysiology of left ventricular hypertrophy secondary to hypertension. (0160-9289 (Print)). eng.
Kearney LG, Lu K, Fau-Ord M, Ord M, Fau-Patel SK, Patel Sk, Fau-Profitis K, Profitis K, Fau-Matalanis G, Matalanis G, Fau-Burrell LM, et al Global longitudinal strain is a strong independent predictor of all-cause mortality in patients with aortic stenosis. (2047-2412 (Electronic)). eng.
Kusunose K, Goodman A, Parikh R, Barr T, Agarwal S, Popovic ZB, et al Incremental prognostic value of left ventricular global longitudinal strain in patients with aortic stenosis and preserved ejection fraction. (1942-0080 (Electronic)). eng.
Vollema E, Sugimoto T, Shen M, et al Association of left ventricular global longitudinal strain with asymptomatic severe aortic stenosis: Natural course and prognostic value. JAMA Cardiol. 2018;3:839-47.
Otto CM, Lind Bk, Fau-Kitzman DW, Kitzman Dw, Fau-Gersh BJ, Gersh Bj, Fau-Siscovick DS, Siscovick DS. Association of aortic-valve sclerosis with cardiovascular mortality and morbidity in the elderly. (0028-4793 (Print)). eng.
El Fakhri G, Kardan A, Sitek A, Dorbala S, Abi-Hatem N, Lahoud Y, et al Reproducibility and accuracy of quantitative myocardial blood flow assessment with (82)Rb PET: comparison with (13)N-ammonia PET. J Nucl Med. 2009;50:1062-71.
Lortie M, Beanlands RS, Yoshinaga K, Klein R, Dasilva JN, DeKemp RA. Quantification of myocardial blood flow with 82Rb dynamic PET imaging. Eur J Nucl Med Mol Imaging. 2007;34:1765-74.
Camici PG, d’Amati G, Rimoldi O. Coronary microvascular dysfunction: mechanisms and functional assessment. Nat Rev Cardiol. 2015;12:48-62.
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, et al Recommendations for cardiac chamber quantification by echocardiography in adults: An update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2015;28:1-39.
Baumgartner H, Hung J, Bermejo J, Chambers JB, Edvardsen T, Goldstein S, et al Recommendations on the Echocardiographic assessment of aortic valve stenosis: A focused update from the european association of cardiovascular imaging and the American Society of Echocardiography. J Am Soc Echocardiogr. 2047;30:372-92.
Nagueh SF, Smiseth OA, Appleton CP, Byrd BF 3rd, Dokainish H, Edvardsen T, et al Recommendations for the evaluation of left ventricular diastolic function by echocardiography: An update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2016;29:277-314.
Shah AM, Cheng S, Fau-Skali H, Skali H, Fau-Wu J, Wu J, Fau-Mangion JR, Mangion Jr Fau-Kitzman D, Kitzman D, Fau-Matsushita K, et al Rationale and design of a multicenter echocardiographic study to assess the relationship between cardiac structure and function and heart failure risk in a biracial cohort of community-dwelling elderly persons: the Atherosclerosis Risk in Communities study. (1942-0080 (Electronic)). eng.
Thygesen K, Alpert JS, Jaffe AS, Simoons ML, Chaitman BR, White HD, et al Third universal definition of myocardial infarction. Circulation. 2012;126:2020-35.
Herzog BA, Husmann L, Valenta I, Gaemperli O, Siegrist PT, Tay FM, et al Long-term prognostic value of 13 N-ammonia myocardial perfusion positron emission tomography added value of coronary flow reserve. J Am Coll Cardiol. 2009;54:150-6.
Murthy VL, Naya M, Foster CR, Hainer J, Gaber M, Di Carli G, et al Improved cardiac risk assessment with noninvasive measures of coronary flow reserve. Circulation. 2011;124:2215-24.
Crea F, Camici PG, Bairey Merz CN. Coronary microvascular dysfunction: an update. Eur Heart J. 2014;35:1101-11.
Garcia D, Camici PG, Durand LG, Rajappan K, Gaillard E, Rimoldi OE, et al Impairment of coronary flow reserve in aortic stenosis. J Appl Physiol. 2009;106:113-21.
Camici PG, Crea F. Coronary microvascular dysfunction. N Engl J Med. 2007;356:830-40.
Schindler TH, Schelbert HR, Quercioli A, Dilsizian V. Cardiac PET imaging for the detection and monitoring of coronary artery disease and microvascular health. JACC Cardiovasc Imaging. 2010;3:623-40.
Cohn JN, Ferrari R, Sharpe N. Cardiac remodeling—concepts and clinical implications: a consensus paper from an international forum on cardiac remodeling. J Am Coll Cardiol. 2000;35:569-82.
Cioffi G, Faggiano P, Vizzardi E, Tarantini L, Cramariuc D, Gerdts E, et al Prognostic effect of inappropriately high left ventricular mass in asymptomatic severe aortic stenosis. Heart. 2011;97:301-7.
Smiseth OA, Torp H, Opdahl A, Haugaa KH, Urheim S. Myocardial strain imaging: how useful is it in clinical decision making? (1522-9645 (Electronic)). eng.
Ng ACT, Prihadi EA, Antoni ML, Bertini M, Ewe SH, Ajmone Marsan N, et al Left ventricular global longitudinal strain is predictive of all-cause mortality independent of aortic stenosis severity and ejection fraction. Eur Heart J Cardiovasc Imaging. 2018;19:859-67.
Kearney LG, Lu K, Ord M, Patel SK, Profitis K, Matalanis G, et al Global longitudinal strain is a strong independent predictor of all-cause mortality in patients with aortic stenosis. Eur Heart J Cardiovasc Imaging. 2012;13:827-33.
Disclosures
Dr. Dorbala is a member of an advisory board for General Electric Health Care. Dr. Di Carli has received consulting fees from Sanofi and General Electric. Dr. Kaneko has served as a proctor and speaker for Edwards Lifesciences, Abbot and Medtronic. Dr. Shah has served as a proctor and educator for Edwards Lifesciences and educator for St. Jude Medical. All other authors have no disclosures to report.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The authors of this article have provided a PowerPoint file, available for download at SpringerLink, which summarises the contents of the paper and is free for re-use at meetings and presentations. Search for the article DOI on SpringerLink.com.
Funding
This was supported by National Institutes of Health Grant Numbers 5T32HL094301 to Drs. Zhou, Bajaj, Gupta, Divakaran; K23HL135438 to Dr. Taqueti; and R01HL132021 to Dr. Di Carli.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhou, W., Bajaj, N., Gupta, A. et al. Coronary microvascular dysfunction, left ventricular remodeling, and clinical outcomes in aortic stenosis. J. Nucl. Cardiol. 28, 579–588 (2021). https://doi.org/10.1007/s12350-019-01706-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12350-019-01706-y