Abstract
Introduction
Hypertension is a condition which in many cases is treated with more than one drug. Additionally, patients with hypertension often suffer from other concomitant diseases, such as diabetes mellitus or dyslipidemia, which adds to the number of pills that patients need to take (pill burden). The aim of this study was to investigate the impact of this pill burden on patients with hypertension in clinical practice in Germany.
Methods
This prospective, open-label, observational study enrolled adult patients for whom their physician considered treatment with a single-pill combination of amlodipine, valsartan, and hydrochlorothiazide as indicated. At the start of the observation period, physicians and patients filled in a respective questionnaire.
Results
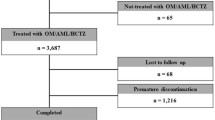
The questionnaires of 7,101 patients and 905 physicians were analyzed. The survey among the patients showed that the majority of patients felt burdened by the high number of pills to be taken. This was also seen as a potential reason for medication errors. Approximately half of the patients would be willing to make an out-of-pocket payment for reducing the number of pills to half. The results of the physician questionnaire indicate that the physicians were well aware of the set of problems that is generally associated with the high pill burden and that there is a clear willingness to use combination products in order to reduce the pill burden.
Conclusion
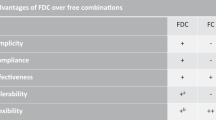
A high number of pills is considered a burden by the patients. This burden increases with the number of pills taken per day.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Kones R. Primary prevention of coronary heart disease: integration of new data, evolving views, revised goals, and role of rosuvastatin in management. A comprehensive survey. Drug Des Devel Ther. 2011;5:325–380.
Kearney P, Whelton M, Reynolds K, Muntner P, Whelton P, He J. Global burden of hypertension: Analysis of worldwide data. Lancet. 2005;365:217–223.
Wolf-Maier K, Cooper RS, Kramer H, et al. Hypertension treatment and control in five European countries, Canada, and the United States. Hypertension. 2004;43:10–17.
Law MR, Morris JK, Wald NJ. Use of blood pressure lowering drugs in the prevention of cardiovascular disease: meta-analysis of 147 randomised trials in the context of expectations from prospective epidemiological studies. BMJ. 2009;338:b1665.
Pepine CJ, Handberg EM, Cooper-DeHoff RM, et al; INVEST Investigators. A calcium antagonist vs a non-calcium antagonist hypertension treatment strategy for patients with coronary artery disease. The International Verapamil-Trandolapril Study (INVEST): a randomized controlled trial. JAMA. 2003;290:2805–2816.
Bakris GL. The importance of blood pressure control in the patient with diabetes. Am J Med. 2004;116(Suppl. 5A):30S–38S.
Dahlöf B, Sever PS, Poulter NR, et al; ASCOT Investigators. Prevention of cardiovascular events with an antihypertensive regimen of amlodipine adding perindopril as required versus atenolol adding bendroflumethiazide as required, in the Anglo-Scandinavian Cardiac Outcomes Trial-Blood Pressure Lowering Arm (ASCOT-BPLA): a multicentre randomised controlled trial. Lancet 2005;366:895–906.
Jamerson K, Bakris GL, Dahlöf B, et al; ACCOMPLISH Investigators. Exceptional early blood pressure control rates: the ACCOMPLISH trial. Blood Press. 2007;16:80–86.
Jamerson K, Weber MA, Bakris GL, et al; ACCOMPLISH Investigators. Benazepril plus amlodipine or hydrochlorothiazide for hypertension in high-risk patients. N Engl J Med. 2008;359:2417–2428.
DiMatteo MR, Giordani PJ, Lepper HS, Croghan TW. Patient adherence and medical treatment outcomes: a meta-analysis. Med Care. 2002;40:794–811.
Ho PM, Magid DJ, Shetterly SM, et al. Medication nonadherence is associated with a broad range of adverse outcomes in patients with coronary artery disease. Am Heart J. 2008;155:772–779.
Chapman RH, Benner JS, Petrilla AA, et al. Predictors of adherence with antihypertensive and lipid-lowering therapy. Arch Intern Med. 2005;165:1147–1152.
Rottlaender D, Scherner M, Schneider T, Erdmann E. [Multimedikation, compliance und zusatzmedikation bei patienten mit kardiovaskulären erkrankungen]. Dtsch Med Wochenschr. 2007;132:139–144. In German.
Mancia G, De BG, Dominiczak A, et al; the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension; the Task Force for the Management of Arterial Hypertension of the European Society of Cardiology. Guidelines for the Management of Arterial Hypertension: The Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur Heart J. 2007;28:1462–1536.
Volpe M, Chin D, Paneni F. The challenge of polypharmacy in cardiovascular medicine. Fundam Clin Pharmacol. 2010;24:9–17.
Theobald K, Capan M, Herbold M, Schinzel S, Hundt F. Quality assurance in non-interventional studies. GMS Ger Med Sci. 2009;7:Doc 29.
Lüders S, Schrader J, Schmieder RE, Smolka W, Wegscheider K, Bestehorn K. Improvement of hypertension management by structured physician education and feedback system: cluster randomized trial. Eur J Cardiovasc Prev Rehabil. 2010;17:271–279.
Qureshi NN, Hatcher J, Chaturvedi N, Jafar TH. Effect of general practitioner education on adherence to antihypertensive drugs: cluster randomized controlled trial. BMJ. 2007;335:1030.
Adherence to long-term therapies. Evidence for action. 2003. World Health Organization website. Available at: http://whqlibdoc.who.int/publications/2003/9241545992.pdf. Accessed Mar 12 2013.
Neutel JM, Smith DHG. Improving patient compliance: a major goal in the management of hypertension. J Clin Hypertens. 2003;5:127–132.
Cadieux RJ. Drug interactions in the elderly. How multiple drug use increases risk exponentially. Postgrad Med. 1989;86:179–186.
Fux R, Greiner D, Geldmacher M, Mörike K, Gleiter CH. Multiple drug prescribing by general practitioners in a German region: Implications for drug interactions and patient safety. Int J Clin Pharmacol Ther. 2006;44:539–547.
Nguyen JK, Fouts MM, Kotabe SE, Lo E. Polypharmacy as a risk factor for adverse drug reactions in geriatric nursing home residents. Am J Geriatr Pharmacother. 2006;4:36–41.
Jesson B. Minimising the risk of polypharmacy. Nurs Older People. 2011;23:14–20.
Wehling M. Guideline-driven polypharmacy in elderly, multimorbid patients is basically flawed: there are almost no guidelines for these patients. J Am Geriatr Soc. 2011;59:376–377.
Patterson SM, Hughes C, Kerse N, Cardwell CR, Bradley MC. Interventions to improve the appropriate use of polypharmacy for older people. Cochrane Database Syst Rev. 2012;5:CD008165.
Garfinkel D, Mangin D. Feasibility study of a systematic approach for discontinuation of multiple medications in older adults: addressing polypharmacy. Arch Intern Med. 2010;170:1648–1654.
Gokula M, Holmes HM. Tools to reduce polypharmacy. Clin Geriatr Med. 2012;28:323–341.
Black N. Why we need observational studies to evaluate the effectiveness of health care. BMJ. 1996;312:1215–1218.
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP; STROBE Initiative. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol. 2008;61:344–349.
Silverman SL. From randomized controlled trials to observational studies. Am J Med. 2009;122:114–120.
Author information
Authors and Affiliations
Corresponding author
Additional information
To view enhanced content go to www.advancesintherapy.com
This article is published with open access at Springerlink.com
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 2.0 International License (https://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Hagendorff, A., Freytag, S., Müller, A. et al. Pill Burden in Hypertensive Patients Treated with Single-Pill Combination Therapy — An Observational Study. Adv Therapy 30, 406–419 (2013). https://doi.org/10.1007/s12325-013-0018-3
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-013-0018-3