Abstract
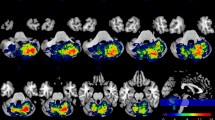
To date, few studies focused on prediction of functional recovery after cerebellar stroke. The main aim of this prospective pilot study was to determine the association between cerebellar lesion location and functional outcome in adults with acute cerebellar infarction. We examined 14 patients with first-ever unilateral cerebellar ischemic stroke within 7 days and at 90 days from the onset of stroke by means of the International Cooperative Ataxia Rating Scale. Cerebellar lesions were traced from magnetic resonance imaging performed within 72 h since stroke and region of interest were generated. The association between the International Cooperative Ataxia Rating Scale score and lesion location was determined with the voxel-based lesion-symptom mapping methods implemented in the MRIcro software. Colored lesion-symptom maps representing the z statistics were generated and overlaid onto the MNI-ICBM 152 linear probabilistic atlas of the human brain and the Johns Hopkins University white matter templates. Our results documented that injuries to the V, VI, VIIA Crus I, VIIA Crus II, VIIB, VIIIA, and VIIIB lobules and the middle cerebellar peduncle are significantly associated with the International Cooperative Ataxia Rating Scale (ICARS) score at 1 week after the onset of stroke. Furthermore, we found that injuries to the VI, VIIA Crus I, VIIA Crus II, VIIB, VIIIA, and VIIIB lobules, the dentate nucleus, and the middle cerebellar peduncle are significantly associated with the ICARS score at 3 months since the cerebellar stroke onset. The findings of this pilot study might improve prognostic accuracy of functional outcome in patients with acute cerebellar infarction.


Similar content being viewed by others
References
Datar S, Rabinstein AA. Cerebellar infarction. Neurol Clin. 2014;32:979–91.
Dziadkowiak E, Chojdak-Łukasiewicz J, Guziński M, Noga L, Paradowski B. The usefulness of the TOAST classification and prognostic significance of pyramidal symptoms during the acute phase of cerebellar ischemic stroke. Cerebellum. 2015. doi:10.1007/s12311-015-0676-6.
Kase CS, Norrving B, Levine SR, Babikian VL, Chodosh EH, Wolf PA, et al. Cerebellar infarction. Clinical and anatomic observations in 66 patients. Stroke. 1993;24:76–83.
Deluca C, Moretto G, Di Matteo A, Cappellari M, Basile A, Bonifati DM, et al. Ataxia in posterior circulation stroke: clinical-MRI correlations. J Neurol Sci. 2011;300:39–46.
Stinear C. Prediction of recovery of motor function after stroke. Lancet Neurol. 2010;9:1228–32.
Picelli A, Tamburin S, Dambruoso F, Midiri A, Girardi P, Santamato A, et al. Topical distribution of initial paresis of the limbs to predict clinically relevant spasticity after ischemic stroke: a retrospective cohort study. Eur J Phys Rehab Med. 2014;50:489–94.
Konczak J, Pierscianek D, Hirsiger S, Bultmann U, Schoch B, Gizewski ER, et al. Recovery of upper limb function after cerebellar stroke: lesion symptom mapping and arm kinematics. Stroke 2010;2191–200.
Kelly PJ, Stein J, Shafqat S, Eskey C, Doherty D, Chang Y, et al. Functional recovery after rehabilitation for cerebellar stroke. Stroke. 2001;32:530–4.
Grips E, Sedlaczek O, Bäzner H, Fritzinger M, Daffertshofer M, Hennerici M. Supratentorial age-related white matter changes predict outcome in cerebellar stroke. Stroke. 2005;36:1988–93.
Schoch B, Dimitrova A, Gizewski ER, Timmann D. Functional localization in the human cerebellum based on voxelwise statistical analysis: a study of 90 patients. Neuroimage. 2006;30:36–51.
Duncan PW, Zorowitz R, Bates B, Choi JY, Glasberg JJ, Graham GD, et al. Management of adult stroke rehabilitation care: a clinical practice guideline. Stroke. 2005;36:e100–43.
Schoch B, Regel JP, Frings M, Gerwig M, Maschke M, Neuhäuser M, et al. Reliability and validity of ICARS in focal cerebellar lesions. Mov Disord. 2007;22:2162–9.
Bultmann U, Pierscianek D, Gizewski ER, Schoch B, Fritsche N, Timmann D, et al. Functional recovery and rehabilitation of postural impairment and gait ataxia in patients with acute cerebellar stroke. Gait Posture. 2014;39:563–9.
Lim JH, Cheon SH. Analysis of variation of length of stay (LOS) after ischemic and hemorrhagic stroke using the Charlson Comorbidity Index (CCI). J Phys Ther Sci. 2015;27:799–803.
Picelli A, Tamburin S, Gajofatto F, Zanette G, Praitano M, Saltuari L, et al. Association between severe upper limb spasticity and brain lesion location in stroke patients. Biomed Res Int. 2014;2014:162754.
Acknowledgments
We would like to recognize the contribution of Marco Veronese in helping us with the preparation of various figures in the paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Compliance with Ethical Standards
All patients gave their informed consent for participation in the current study, which was carried out according to the Declaration of Helsinki and approved by the local Ethics Committee.
Conflict of Interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Picelli, A., Zuccher, P., Tomelleri, G. et al. Prognostic Importance of Lesion Location on Functional Outcome in Patients with Cerebellar Ischemic Stroke: a Prospective Pilot Study. Cerebellum 16, 257–261 (2017). https://doi.org/10.1007/s12311-015-0757-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12311-015-0757-6