Abstract
Purpose
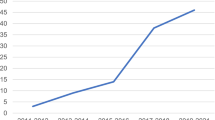
Over the years, the number of total hip replacements has been steadily increasing. Despite the improvement in surgical results, the number of claims for malpractice is higher. The primary endpoint of this work is to provide an analysis of litigation after hip replacement, to outline what are the instigating causes and costs. The secondary endpoint is to propose a possible preventive strategy for an improved care and a reduction in legal proceedings.
Materials and methods
The data of this study were collected from medical and legal files and from professional liability insurance of our institution from January 2005 to December 2016.
Results
Out of a total of 4770 THA, 40 claims were received. Peripheral nerve injuries represent the first cause of litigation (37%), followed by infectious complications, leg length discrepancy, metallosis, dislocations of the implant and a case of deep vein thrombosis. From the analysis of the past trial judgment, complications such as nerve lesions and infections are almost always recognized, as a medical error, with a high percentage of claims settled.
Conclusion
This study shows the necessity of preventive strategies to reduce the higher number of claims for malpractice in total hip arthroplasty. Some complications such as nerve injuries and infection are frequently considered directly dependent on physician’s errors. Litigations can be reduced providing evidence of a diligent execution of the surgical procedure and of a proper postoperative management: the correct compilation of a specific informed consent and adequate doctor–patient communication.

Similar content being viewed by others
References
Learmonth ID, Young C, Rorabeck C (2007) The operation of the century: total hip replacement. Lancet 370:1508–1519
Berry DJ, Berger RA, Callaghan JJ et al (2003) Minimally invasive total hip arthroplasty. Development, early results, and a critical analysis. J Bone Joint Surg Am 85-A(11):2235–2246
Berry DJ (2005) “Minimally invasive” total hip arthroplasty. J Bone Joint Surg 87(4):699–700
Jones CA, Voaklander DC, Johnston DW, Suarez-Almazor ME (2000) Health related quality of life outcomes after total hip and knee arthroplasties in a community based population. J Rheumatol 27(7):1745–1752
Saleh KJ, Kassim R, Yoon P, Vorlicky LN (2002) Complications of total hip arthroplasty. Am J Orthop 31(8):485–488
Coventry MB, Beckenbaugh RD, Nolan DR, Ilstrup DM (1974) 2,012 Total hip arthroplasties. A study of postoperative course and early complications. J Bone Joint Surg Am 56(2):273–284
Gould MT, Langworthy MJ, Santore R, Provencher MT (2003) An analysis of orthopaedic liability in the acute care setting. Clin Orthop Relat Res 407:59–66
Italian Cassation Court On-line Archives. www.italgiure.giustizia.it/sncass. Accessed Sept 2017
Scott CEH, Bugler KE, Clement ND, MacDonald D, Howie CR, Biant LC (2012) Patient expectations of arthroplasty of the hip and knee. Bone Joint J 94-B(7):974–981
Patterson DC, Grelsamer R, Bronson MJ, Moucha CS (2017) Lawsuits after primary and revision total knee arthroplasty: a malpractice claims analysis. J Am Acad Orthop Surg 25(10):e235–e242
Bhutta MA, Arshad MS, Hassan S, Henderson JJ (2011) Trends in joint arthroplasty litigation over five years: the British experience. Ann R Coll Surg Engl 93(6):460–464
Zengerink I, Reijman M, Mathijssen NMC, Eikens-Jansen MP, Bos PK (2016) Hip arthroplasty malpractice claims in the Netherlands: closed claim study 2000–2012. J Arthroplasty 31(9):1890–1893.e4
McWilliams AB, Douglas SL, Redmond AC et al (2013) Litigation after hip and knee replacement in the National Health Service. Bone Joint J 95-B(1):122–126
Chen A, Patel NK, Khan Y, Cobb JP, Gupte CM (2015) The cost of adverse events from knee surgery in the United Kingdom: an in-depth review of the National Health Service Litigation Authority database. Knee 22(4):286–291
Beresford-Cleary N, Halliday J, Biant J, Breusch J (2011) Consent process for elective total hip and knee arthroplasty. J Orthop Surg (Hong Kong) 19(3):274–278
Prous J (2009) The changing face of healthcare. Eur Biopharm Rev 35:66–67
Bajada S, Dwamena S, Abdul Z, Williams R, Ennis O (2017) Improving consent form documentation and introduction of procedure-specific labels in a district general hospital. BMJ Qual Improv Rep 6(1):u211571.w4730
Barritt AW, Clark L, Teoh V, Cohen AMM, Gibb PA (2010) Assessing the adequacy of procedure-specific consent forms in orthopaedic surgery against current methods of operative consent. Ann R Coll Surg Engl 92(3):246–249
McDonald S, Page MJ, Beringer K, Wasiak J, Sprowson A (2014) Preoperative education for hip or knee replacement. Cochrane Database Syst Rev 5:CD003526
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Novi, M., Vanni, C., Parchi, P.D. et al. Claims in total hip arthroplasty: analysis of the instigating factors, costs and possible solution. Musculoskelet Surg 104, 43–48 (2020). https://doi.org/10.1007/s12306-019-00590-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-019-00590-6