Abstract
Purpose
Evaluate the efficacy and safety of MESNA (sodium 2-mercaptoethanesulfonate) injection into the epidural space in the FBSS.
Methods
We designed a prospective phase II longitudinal study. Six consecutive patients were enrolled. Patients underwent one peridural injection per week for 3 weeks. NRS and ODI were investigated before and 48 h after injections, and at 1 week, 1 month and 2 months after the last procedures. Opioids intake is investigated before procedures and 1 week, 1 month and 3 months after the last procedures. Lumbosacral MRI is performed before the first procedure, at the end and 3 months after the last procedures.
Results
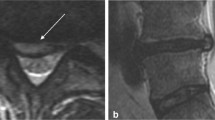
From baseline, at 3 months, NRS in standing, sitting and lying position improved, respectively, of 34.29, 30.56 and 26.47%; ODI improved of 20.3%; the average decrease in morphine intake was 20.54%. No difference in MR images was found. Conclusions Our preliminary results suggest that MESNA might be an efficacy alternative to common practice.
Similar content being viewed by others
References
Di Martino A, Merlini L, Faldini C (2013) Autoimmunity in intervertebral disc herniation: from bench to bedside. Expert Opin Ther Targets 17:1461–1470
Onesti ST (2004) Failed back syndrome. Neurologist 10:259–264
Katz JN (1995) Lumbar spinal fusion. Surgical rates, costs, and complications. Spine 20:78S–83S
Chan CW, Peng P (2011) Failed back surgery syndrome. Pain Med 12:577–606
Goren MP (1992) Oral mesna: a review. Semin Oncol 19:65–71
Lewis LD, Burton LC, Harper PG et al (1992) Uroepithelial and nephrotubula toxicity in patients receiving ifosfamide/mesna: measurement of urinary N-acetyl-beta-d-glucosaminidase and beta-2-microglobulin. Eur J Cancer 28A:1976–1981
Zini CBS, Gandolfi A, Piazza F et al. (1998) Use of sodium 2-mercaptoethanesulfonate in surgery. WO016213
Casale M, Di Martino A, Salvinelli F et al (2010) MESNA for chemically assisted tissue dissection. Expert Opin Investig Drugs 19:699–707
Vincenti V, Mondain M, Pasanisi E et al (1999) Cochlear effects of mesna application into the middle ear. Ann N Y Acad Sci 884:425–432
Denaro VFF, Di Martino A, Denaro L et al (2001) Effect of a mucolytic agent on collagen fibres: an optical and polarized light histological study. Eur J Orthop Surg Traumatol 11:209–212
Ajmal N, Riordan CL, Cardwell N et al (2003) Chemically assisted capsulectomy in the rabbit model: a new approach. Plast Reconstr Surg 112:1449–1454 (discussion 62–63)
Denaro V, Di Martino A, Longo UG et al (2008) Effectiveness of a mucolythic agent as a local adjuvant in revision lumbar spine surgery. Eur Spine J 17:1752–1756
Fairbank JC, Pynsent PB (2000) The oswestry disability index. Spine 25:2940–2952 (discussion 52)
Parr AT, Diwan S, Abdi S (2009) Lumbar interlaminar epidural injections in managing chronic low back and lower extremity pain: a systematic review. Pain Physician 12:163–188
Ross JS, Obuchowski N, Zepp R (1998) The postoperative lumbar spine: evaluation of epidural scar over a 1-year period. Am J Neuroradiol 19:183–186
Ross JS, Obuchowski N, Modic MT (1999) MR evaluation of epidural fibrosis: proposed grading system with intra- and inter-observer variability. Neurol Res 21(Suppl 1):S23–S26
Abdi S, Datta S, Trescot AM et al (2007) Epidural steroids in the management of chronic spinal pain: a systematic review. Pain Physician 10:185–212
Manchikanti L (2002) Role of neuraxial steroids in interventional pain management. Pain Physician 5:182–199
Byrod G, Otani K, Brisby H et al (2000) Methylprednisolone reduces the early vascular permeability increase in spinal nerve roots induced by epidural nucleus pulposus application. J Orthop Res 18:983–987
Revel M, Auleley GR, Alaoui S et al (1996) Forceful epidural injections for the treatment of lumbosciatic pain with post-operative lumbar spinal fibrosis. Rev Rhum Engl Ed 63:270–277
Hesla EBH (1979) Epidural analgesia and epidural steroid injection for treatment of chronic low back pain and sciatica. Tidsskr Nor Laegeforen 99:936–939
Manchikanti L, Singh V, Cash KA et al (2008) Preliminary results of a randomized, equivalence trial of fluoroscopic caudal epidural injections in managing chronic low back pain: part 3—post surgery syndrome. Pain Physician 11:817–831
Parr AT, Manchikanti L, Hameed H et al (2012) Caudal epidural injections in the management of chronic low back pain: a systematic appraisal of the literature. Pain Physician 15:E159–E198
Cohen SP, Bicket MC, Jamison D et al (2013) Epidural steroids: a comprehensive, evidence-based review. Reg Anesth Pain Med 38:175–200
Helm Ii S, Benyamin RM, Chopra P et al (2012) Percutaneous adhesiolysis in the management of chronic low back pain in post lumbar surgery syndrome and spinal stenosis: a systematic review. Pain Physician 15:E435–E462
Racz GBSM, Gintautas J, Kline WM (1982) Intractable pain therapy using a new epidural catheter. JAMA 248:579–581
Epter RS, Helm S, Hayek SM et al (2009) Systematic review of percutaneous adhesiolysis and management of chronic low back pain in post lumbar surgery syndrome. Pain Physician 12:361–378
Manchikanti L, Rivera JJ, Pampati V et al (2004) One day lumbar epidural adhesiolysis and hypertonic saline neurolysis in treatment of chronic low back pain: a randomized, double-blind trial. Pain Physician 7:177–186
Menzel EJ, Farr C (1998) Hyaluronidase and its substrate hyaluronan: biochemistry, biological activities and therapeutic uses. Cancer Lett 131:3–11
Kim SB, Lee KW, Lee JH et al (2012) The effect of hyaluronidase in interlaminar lumbar epidural injection for failed back surgery syndrome. Ann Rehabil Med 36:466–473
Yousef AA, El-Deen AS, Al-Deeb AE (2010) The role of adding hyaluronidase to fluoroscopically guided caudal steroid and hypertonic saline injection in patients with failed back surgery syndrome: a prospective, double-blinded, randomized study. Pain Pract 10:548–553
Devulder J (1998) Transforaminal nerve root sleeve injection with corticosteroids, hyaluronidase, and local anesthetic in the failed back surgery syndrome. J Spinal Disord 11:151–154
Devulder J, Deene P, De Laat M et al (1999) Nerve root sleeve injections in patients with failed back surgery syndrome: a comparison of three solutions. Clin J Pain 15:132–135
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We have patented the peridural use of MESNA (IPN WO2012/052888 A1 and Italian Patent #0001402161): property of the patent is the Institution University Campus Bio-Medico of Rome; royalties are not personal to the authors, but devolved to the Institutional Research of the Respective Departments of the Authors.
Rights and permissions
About this article
Cite this article
Carassiti, M., Di Martino, A., Centonze, A. et al. Failed back surgery syndrome: a new strategy by the epidural injection of MESNA. Musculoskelet Surg 102, 179–184 (2018). https://doi.org/10.1007/s12306-017-0520-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12306-017-0520-x