Abstract
Background
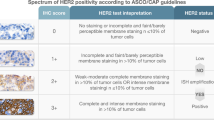
Diagnosis of triple-negative breast cancer (ER-negative, PgR-negative, HER2-negative; TNBC) is performed by means of immunohistological staining. HER2-negative includes HER2(0) and HER2(1+), based on differences in the staining intensity, but there have been no reports on comparison of these two types in TNBC. Accordingly, this study was designed to investigate the possible differences in the biological characteristics of HER2(0) breast cancer and HER2(1+) breast cancer in TNBC.
Methods
Tissue specimens from 89 TNBC patients were immunohistochemically stained for CK5/6, EGFR, p53, Ki67, E-cadherin, TOP2A and Bcl-2. The expressions of these markers and the clinicopathological findings were compared between the HER2(0) patient group and the HER2(1+) patient group. When either CK5/6 or EGFR was positive, the specimen was judged to be the basal-like phenotype of breast cancer.
Results
The percentages of CK5/6- and/or EGFR-positive specimens in the HER2(0) and HER2(1+) groups were 44.9 and 16.8%, respectively, showing that there was a significantly greater number of basal-like phenotype patients in the HER2(0) group (p < 0.01). The percentage of E-cadherin-positive specimens in the HER2(0) group was 66.6%, which was significantly greater than the 40.0% recorded in the HER2(1+) group (p < 0.05). The respective percentages of TOP2A-positive specimens in the HER2(0) and HER2(1+) groups were 55.0 and 30.0%, and the difference was statistically significant (p < 0.05).
Conclusion
In TNBC, HER2(0) breast cancer showed a strong tendency to include more of the basal-like phenotype compared with HER2(1+) breast cancer. The staining results indicated the possibility that HER2(0) breast cancer and HER2(1+) breast cancer have different characteristics.
Similar content being viewed by others
References
Sørlie T, Perou CM, Tibshirani R, Aas T, Geisler S, Johnsen H, et al. Gene expression patterns of breast carcinomas distinguish tumor subclasses with clinical implications. Proc Natl Acad Sci USA. 2001;98:10869–74.
Cleator S, Heller W, Coombers RC. Triple-negative breast cancer: therapeutic options. Lancet Oncol. 2007;8:235–44.
Prati R, Apple SK, Gornbein JA, Chang HR. Histopathologic characteristics predicting HER2/neu amplification in breast cancer. Breast J. 2005;11:433–9.
Gown AM. Current issues in ER and HER2 testing by IHC in breast cancer. Modern Pathol. 2008;21:S8–15.
Rakha EA, El-Sayed ME, Green AR, Lee AH, Robertson JF, Ellis IO. Prognostic markers in triple negative breast cancer. Cancer. 2006;109:25–32.
Sasa M, Bando Y, Takahashi M, Hirose T, Nagao T. Screening for basal marker expression is necessary for decision of therapeutic strategy for triple-negative breast cancer. J Surg Oncol. 2008;97:30–4.
Rakha EA, Putti TC, Abd El-Rehim DM, Paish C, Green AR, Powe DG, et al. Morphological and immunophenotypic analysis of breast carcinomas with basal and myoepithelial differentiation. J Pathol. 2006;208:495–506.
Ping T, Kristin AS, David GH. Molecular classification of breast carcinomas by immunohistochemical analysis. Are we ready? Diagn Mol Pathol. 2009;18:125–32.
Nielsen TO, Hsu FD, Jensen K, Cheang M, Karaca G, Hu Z, et al. Immunohistochemical and clinical characterization of the basal-like subtype of invasive breast carcinoma. Clin Cancer Res. 2004;10:5367–74.
Wolff AC, Hammond ME, Schwartz JN, Hagerty KL, Allred DC, Cote RJ, et al. American Society of Clinical Oncology/College of American Pathologists Guideline recommendations for human epidermal growth factor receptor 2 testing in breast cancer. Arch Pathol Lab Med. 2007;131:18.
Wolff AC, Hammond ME, Schwartz JN, Hagerty KL, Allred DC, Cote RJ, et al. American Society of Clinical Oncology/College of American Pathologists Guideline recommendations for human epidermal growth factor receptor 2 testing in breast cancer. J Clin Oncol. 2007;25:118–45.
The Japanese Breast Cancer Society. General rules for clinical and pathological recording for breast cancer. 16th ed. Japan: KANEHARA & CO., LTD; 2005.
Owens MA, Horten BC, Da Silva MM. HER2 amplification ratios by fluorescence in situ hybridization and correlation with immunohistochemistry in a cohort of 6556 breast cancer tissues. Clin Breast Cancer. 2004;5:63–9.
Turashvili G, Leung S, Turbin D, Montgomery K, Gilks B, West R, et al. Inter-observer reproducibility of HER2 immunohistochemical assessment and concordance with fluorescent in situ hybridization (FISH): pathologist assessment compared to quantitative image analysis. BMC Cancer. 2009;9:165.
McCormick SR, Lillemoe TJ, Beneke J, Schrauth J, Reinartz J. HER2 assessment by immunohistochemical analysis and fluorescence in situ hybridization: comparison of HercepTest and PathVysion commercial assays. Am J Clin Pathol. 2002;117:935–43.
Viale G, Bottiglieri L. Pathological definition of triple negative breast cancer. Eur J Cancer. 2009;45:5–10.
Rakha EA, Abd Ei Rehim D, Pinder SE, Lewis SA, Ellis IO. E-cadherin expression in invasive non-lobular carcinoma of the breast and its prognostic significance. Histopathology. 2005;46:685–93.
Mahler-Araujo B, Savage K, Parry S, Reis-Filho JS. Reduction of E-cadherin expression is associated with non-lobular breast carcinomas of basal-like and triple negative phenotype. J Clin Pathol. 2008;61:615–20.
Mohammadizadeh F, Ghasemibasir H, Rajabi P, Naimi A, Eftekhari A, Mesbah A. Correlation of E-cadherin expression and routine immunohistochemistry panel in breast invasive ductal carcinoma. Cancer Biomarkers. 2009;5:1–8.
Tan DS, Potts HW, Leong AC, Gillett CE, Skilton D, Harris WH, et al. The biological and prognostic significance of cell polarity and E-cadherin in grade 1 infiltrating ductal carcinoma of the breast. J Pathol. 1999;189:20–7.
Tan DS, Marchió C, Jones RL, Savage K, Smith IE, Dowsett M, et al. Triple negative breast cancer: molecular profiling and prognostic impact in adjuvant anthracycline-treated patients. Breast Cancer Res Treat. 2008;111:27–44.
Carey LA, Dees EC, Sawyer L, Gatti L, Moore DT, Collichio F, et al. The triple negative paradox: primary tumor chemosensitivity of breast cancer subtype. Clin Cancer Res. 2007;13:2329–34.
Tsutsui S, Yasuda K, Suzuki K, Takeuchi H, Nishizaki T, Higashi H, et al. Bcl-2 protein expression is associated with p27 and p53 protein expressions and MIB-1 counts in breast cancer. BMC Cancer. 2006;6:187–93.
Poincloux L, Durando X, Seitz JF, Thivat E, Bardou VJ, Giovannini MH, et al. Loss of Bcl-2 expression in colon cancer: a prognostic factor for recurrence in stage II colon cancer. Surg Oncol. 2009;18:357–65.
Liu H, Fan Q, Zhang Z, Li X, Yu H, Meng F. Basal-HER2 phenotype shows poorer survival than basal-like phenotype in hormone receptor-negative invasive breast cancers. Hum Pathol. 2008;39:167–74.
Potemski P, Kusinska R, Watala C, Pluciennik E, Bednarek AK, Kordek R. Prognostic relevance of basal cytokeratin expression in operable breast cancer. Oncology. 2005;69:478–85.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Nakagawa, M., Bando, Y., Nagao, T. et al. Among triple-negative breast cancers, HER2(0) breast cancer shows a strong tendency to be basal-like compared with HER2(1+) breast cancer: preliminary results. Breast Cancer 19, 54–59 (2012). https://doi.org/10.1007/s12282-011-0265-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12282-011-0265-6