Abstract
Objective
To compare the effects of cilostazol on cerebral arteries and cerebrovascular blood flow in secondary prevention of ischemic stroke, with those of aspirin.
Methods
Sixty-eight patients who had ischemic stroke during the recent 1–6 months were recruited and randomized into cilostazol or aspirin group. Cerebrovascular condition was assessed by magnetic resonance angiography (MRA) and transcranial doppler ultrasonography (TCD) at the beginning of the study and after 12-month medication.
Results
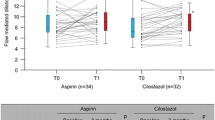
During the clinical follow-up, ischemic stroke recurred in 2 patients in cilostazol group, while in aspirin group, one case of ischemic stroke recurrence and one case of acute myocardial infarction were found. MRA revealed that in aspirin group, the percentages of patients experiencing aggravation and attenuation of cerebrovascular condition were 3.3% and 6.7%, respectively, while in aspirin group, they were 3.3% and 10%, respectively. Moreover, TCD revealed that 26.9% of the patients in aspirin group and 14.3% of the patients in cilostazol group experienced aggravation of cerebrovascular condition. However, the systolic peak flow velocity of the previously abnormal arteries increased by 42.9% after 12-month medication of cilostazol, which was significantly higher than that after aspirin medication (27.5%) (P = 0.04). Furthermore, as a major side effect of antiplatelet therapy, the frequrency of bleeding was much less in cilostazol group (0 case in cilostazol group vs 5 in aspirin, P < 0.05).
Conclusion
Cilostazol is as effective as aspirin in preventing the aggravation of cerebral arteries in secondary prevention of ischemic stroke. Besides, it is more safe. Cilostazol can increase the systolic peak flow velocity of cerebral arteries, which may improve the blood supply of focal ischemia.
摘要
目的
观察西乐他唑与阿司匹林在脑梗死二级预防中对脑血맜状况和脑血流的影响, 并作比较。
方法
选取在近1–6 个月内有脑梗死病史患者68 例, 随机分配入西乐他唑和阿司匹林组。 在入组时及用药12 个月后, 应用核磁共振血맜成像(MRA)和经颅多普勒超声(TCD)方法评价患者脑血맜状况。
结果
随访期间, 西乐他唑组有2例患者再发脑梗死, 而阿司匹林组有1 例再发脑梗死, 1 例发生急性心肌梗死。 MRA 检测发现, 西乐他唑组患者血맜状况恶化和好转的比例分别为3.3%和6.7%, 阿司匹林组分别为3.3%和10.0%。 TCD检测显示西乐他唑和阿司匹林组患者血맜状况恶化发生的比例分别为14.3%和26.9%。 以上结果两组间均无统计学差异。 服用西乐他唑12个月后, 血流异常的血맜中其收缩期血流峰值升高的比例高于阿司匹林组, 分别为42.9%和27.5%。 作为抗血小板治疗的主要副作用, 出血事件在西乐他唑组发生0 例, 在阿司匹林组发生5 例(P < 0.05)。
结论
西乐他唑在脑梗死二级预防中同阿司匹林一样有效且比阿司匹林更为安全。 西乐他唑能升高脑血맜峰值血流速度, 改善缺血灶血供。
Similar content being viewed by others
References
Szczeklik A, Musial J, Undas A, Sanak M, Nizankowski R. Aspirin resistance. Pharmacol Rep 2005, 57Suppl: 33–41.
He J, Whelton PK, Vu B, Klag MJ. Aspirin and risk of hemorrhage stroke: a meta-analysis of randomized controlled trials. JAMA 1998, 280(22): 1930–1935.
Gotoh F, Tohgi H, Hirai S. Cilostazol Stroke Prevention Study: a placebo-controlled double-blind trial for secondary prevention of ischemic stroke. Cerebrovasc Dis 2000, 9(4): 147–157.
Matsumoto M. Cilostazol in secondary prevention of stroke: impact of the Cilostazol Stroke Prevention Study. Atheroscler Suppl 2005, 6(4): 33–40.
Kwon SU, Cho YJ, Koo JS, Bae HJ, Lee YS, Hong KS, et al. Cilostazol prevents the progression of the symptomatic intracranial arterial stenosis: the multicenter double-blind placebo-controlled trial of cilostazol in symptomatic intracranial arterial stenosis. Stroke 2005, 36(4): 782–786.
Becker RW, Lusis E, Sohn RL, Kline RA. Effects of cilostazol on human venous smooth muscle. Ann Vasc Surg 2005, 19(3): 393–397.
Wang T, Elam MB, Forbes WP, Zhong J, Nakajima K. Reduction of remnant lipoprotein cholesterol concentrations by cilostazol in patients with intermittent claudication. Atherosclerosis 2003, 171(2): 337–342.
Lee JH, Park SY, Shin YW, Hong KW, Kim CD, Sung SM, et al. Neuroprotection by cilostazol, a phosphodiesterase type 3 inhibitor, against apoptotic white matter changes in rat after chronic cerebral hypoperfusion. Brain Res 2006, 1082(1): 182–191.
Schror K. The pharmacology of cilostazol. Diabetes Obes Metab 2002, 4Suppl 2: S14–S19.
Sliwka U, Klotzsch C, Popescu O, Brandt K, Schmidt P, Berlit P, et al. Do chronic middle cerebral artery stenoses represent an embolic focus? A multirange transcranial Doppler study. Stroke 1997, 28(7): 1324–1327.
He J, Gu D, Wu X, Reynolds K, Duan X, Yao C, et al. Major causes of death among men and women in China. N Engl J Med 2005, 353: 1124–1134.
Huang Y, Cheng Y, Wu J, Li Y, Xu E, Hong Z, et al. Cilostazol as an alternative to aspirin after ischaemic stroke: a randomized, double-blind, pilot study. Lancet Neurol 2008, 7(6): 494–499.
Yashiro Y, Ohhashi T. Effects of cilostazol, a selective cyclic AMP phosphodiesterase inhibitor on isolated rabbit spinal arterioles. Jpn J Physiol 2002, 52(5): 471–477.
Tanaka K, Gotoh F, Fukuuchi Y, Amano T, Uematsu D, Kawamura J, et al. Effects of a selective inhibitor of cyclic AMP phosphodiesterase on the pial microcirculation in feline cerebral ischemia. Stroke 1989, 20(5): 668–673.
Honda F, Imai H, Ishikawa M, Kubota C, Shimizu T, Fukunaga M, et al. Cilostazol attenuates gray and white matter damage in a rodent model of focal cerebral ischemia. Stroke 2006, 37(1): 223–228.
Shinoda-Tagawa T, Yamasaki Y, Yoshida S, Kajimoto Y, Tsujino T, Hakui N, et al. A phosphodiesterase inhibitor, cilostazol, prevents the onset of silent brain infarction in Japanese subjects with Type II diabetes. Diabetologia 2002, 45(2): 188–194.
Komas N, Lugnier C, Andriantsitohaina R, Stoclet JC. Characterisation of cyclic nucleotide phosphodiesterases from rat mesenteric artery. Eur J Pharmacol 1991, 208(1): 85–87.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Guo, JJ., Xu, E., Lin, QY. et al. Effect of cilostazol on cerebral arteries in secondary prevention of ischemic stroke. Neurosci. Bull. 25, 383–390 (2009). https://doi.org/10.1007/s12264-009-6192-2
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12264-009-6192-2