Abstract
Progress in surgical practice has paralleled the civilizational evolution. Surgery has progressed from being the last resort in saving life to being form and function preserver. Post-renaissance Industrial age gave an impetus to this march of surgery. The currently on going digital technological revolution has further catalysed this march. Having achieved the stabilized and acceptable clinical outcomes, the surgeon has embarked on a journey of improving patient reported outcomes (PRO). Improvement in PROs with the advent of laparoscopic surgery with the attendant emphasis on minimising invasion has led to debates about invasion being just parietal or holistic in physiological sense. There is a concern that parietal invasiveness shouldn’t be a trade-off for compromised clinical outcomes. Single Incision Laparoscopic Surgery (SILS) in its current avatar with current instrumentation seems to be an enthusiastic bandwagon rolling on with the cosmetic benefits acting as veil to hide the potential clinical concerns. History of surgical innovations is riddled with tales of vindictiveness and vicissitude. Lest the same fate befalls SILS we would do better to examine the SILS bandwagon in its current form till the emerging technologies address the current concerns.




Similar content being viewed by others
References
Agarwal BB (2008) Journey of the carbon-literate and climate-conscious endosurgeon having a head, heart, hands, and holistic sense of responsibility. Surg Endosc 22:2539–2540
Agarwal BB (2009) Informed consent—‘da Vinci code’ for our safety in empowered patient’s safety. Surg Endosc 23:1158–1160
Agarwal BB, Sarangi R, Mahajan KC (2010) Outcomes with thyroidectomy: what are they?—patient reported voice quality, not merely nerve preservation. Surg Endosc 24:735–737
Agarwal BB, Agarwal S (2009) Recurrent laryngeal nerve, phonation and voice preservation—energy devices in thyroid surgery—a note of caution. Langenbecks Arch Surg 394:911–912
Riskin DJ, Longaker MT, Gertner M, Krummel TM (2006) Innovation in surgery: a historical perspective. Ann Surg 244:686–693
Beger HG, Arbogast R (2006) The art of surgery in the 21st century: based on natural sciences and new ethical dimensions. Langebecks Arch Surg 391:143–148
Wexner SD (2009) Trials and tribulations in the history of surgical innovation: SAGES 2007 presidential address. Surg Endosc 23(6):1171–1179
Litynski GS (1998) Kurt Semm and the fight against scepticism: endoscopic hemostasis, laparoscopic appendectomy, and Semm’s impact on the “laparoscopic revolution”. JSLS 2:309–313
Dumas A (1932) The History of Anaesthesia. J Natl Med Assoc 24:6–9
Kandela P (1998) 175 years at The Lancet. The editors. Lancet 352(9134):1141–1143
Satava RM (2008) Advanced technologies and the future of medicine and surgery. Yonsei Med J 49:873–878
Agarwal BB (2010) Umbilicus, navel, belly button—vitruvian guide for esthetic cosmetics: a Da Vinci code for beautiful informed consent. Surg Endosc 24:236–238
Beger HG, Rau BM (2006) Randomized controlled clinical trials support but not substitute of decision making in surgery. Langebecks Arch Surg 391:301–303
Agarwal BB (2009) Letter 3: randomized clinical trial of antibiotic therapy versus appendicectomy as primary treatment of acute appendicitis in unselected patients. Br J Surg 96:473–481
Agarwal BB, Mahajan KC (2010) Nomenclature of abbreviated acronyms (Naa…)—caveamus surgeones. Surg Endosc 24:724–725
Gruen RL, Watters DA, Hollands MJ (2012) Surgical wisdom. Br J Surg 99:3–5
White JJ (2008) Surgical precision. Arch Surg 143:1040
Weizman D, Cyriac J, Urbach DR (2007) What is meant when a laparoscopic surgical procedure is described as “safe”? Surg Endosc 21:1369–1372
Hoover EL (2007) Patient Safety and Surgeons: why the resistance? Arch Surg 142:1127–1128
Pescatori M (2011) STARR and the older surgeon: what makes the difference? Int J Colorectal Dis 26:1497–1498
Angelos P (2009) Complications, errors, and surgical ethics. World Journal of Surgery 33:609–611
Rikkers LF (2022) The bandwagon effect. J Gastrointest Surg 6:787–94
Cuschieri A (2006) Nature of human error: implications for surgical practice. Ann Surg 244:642–648
Karl RC (2007) The origins of malpractice claims. Ann Surg 246:712–713
Regenbogen SE, Greenberg CC, Studdert DM, Lipsitz SR, Zinner MJ, Gawande AA (2007) Patterns of technical error among surgical malpractice claims: an analysis of strategies to prevent injury to surgical patients. Ann Surg 246:705–711
Cuschieri A (2002) Myths surrounding bile duct injury. ANZ J Surg 72:79–80
Agarwal BB (2009) Patient safety in laparoscopic cholecystectomy. Arch Surg 144:979
Millat B, Fingerhut A, Cuschieri A (2006) Live surgery and video presentations: seeing is believing … but no more: a plea for structured rigor and ethical considerations. Surg Endosc 20:845–847
Eypasch E, Lefering R, Kum CK, Troidl H (1995) Probability of adverse events that have not yet occurred: a statistical reminder. BMJ 311:619–620
Agarwal BB (2010) Energized dissection, energized hemostasis. Arch Surg 145:1021
Agarwal BB, Gupta M, Agarwal S, Mahajan KC (2007) Laparoscopic cholecystectomy without using any energy source. J Laparoendosc Adv Surg Tech A 17:296–301
Agarwal BB, Gupta M, Agarwal S, Mahajan KC (2007) Anatomical footprint for safe laparoscopic cholecystectomy without using any energy source: a modified technique. Surg Endosc 21:2154–2158
Cook RI (2003) Seeing is believing. Ann Surg 237:472–473
Patrick R (2008) Avoiding mediocrity. Surg Endosc 22:1736–1737
Ubel PA, Jepson C, Silver-Isenstadt A (2003) Don’t ask, don’t tell: a change in medical student attitudes after obstetrics/gynecology clerkships toward seeking consent for pelvic examinations on an anesthetized patient. Am J Obstet Gynecol 188:575–579
Satava RM (2002) The bio-intelligence age: surgery after the information age. Journal of Gastrointestinal Surgery 6:795–799
Sugimoto M (2010) Recent advances in visualization, imaging, and navigation in hepatobiliary and pancreatic sciences. J Hepatobiliary Pancreat Sci 17:574–576
Curet MJ (2010) Shame on them. Single-incision laparoscopic surgery: are we doomed to repeat the mistakes of the past?: comment on “Single-incision laparoscopic surgery for cholecystectomy”. Arch Surg 145:1191–1192
Boni L, Dionigi G, Rovera F (2009) Natural orifices transluminal endoscopic surgery (NOTES) and other allied “ultra” minimally invasive procedures: are we loosing the plot? Surg Endosc 23:927–929
Agarwal BB, Agarwal S (2008) Surgical pilgrimage—the need to avoid navigation through drains, medicine or ‘medisin’: our notes on NOTES. Surg Endosc 22:271–272
Bencsath KP, Falk G, Morris-Stiff G, Kroh M, Walsh RM, Chalikonda S (2011) Single-incision laparoscopic cholecystectomy: do patients care? J Gastrointest Surg 29
Agarwal BB, Agarwal S (2007) The man–machine interface, a paradox of technology. Is the black box (BB) concept an angel or a demon? Surg Endosc 21:1680
Cheerleader or watchdog? [No authors listed] Nature 2009 25;459:1033
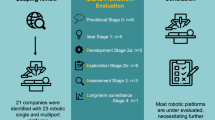
Ergina PL, Cook JA, Blazeby JM et al (2009) Challenges in evaluating surgical innovation. J Lancet 374:1097–1104
Agarwal BB, Chintamani C (2011) Reminder of the metrics of endosurgical innovation. Arch Surg 146:1108
Blazeby JM, Avery K, Sprangers M, Pikhart H, Fayers P, Donovan J (2006) Health-related quality of life measurement in randomized clinical trials in surgical oncology. J Clin Oncol 24:3178–3186
(1991) A prospective analysis of 1518 laparoscopic cholecystectomies. The Southern Surgeons Club. [No authors listed]. N Engl J Med 324:1073–1078
Barone JE, Lincer RM (1991) Correction: a prospective analysis of 1518 laparoscopic cholecystectomies. N Engl J Med 325:1517–1518
Levine DW (1991) An analysis of laparoscopic cholecystectomy. N Engl J Med 325:967–968
Slater K, Strong RW, Wall DR, Lynch SV (2002) Iatrogenic bile duct injury: the scourge of laparoscopic cholecystectomy. ANZ J Surg 72:83–88
Walker T (2008) Biliary injury after laparoscopic cholecystectomy: why still a problem? Gastroentrology 134:894–895
Maschuw K, Osei-Agyemang T, Weyers P et al (2008) The impact of self-belief on laparoscopic performance of novices and experienced surgeons. World J Surg 32:1911–1916
Strasberg SM, Gouma DJ (2012) ‘Extreme’ vasculobiliary injuries: association with fundus-down cholecystectomy in severely inflamed gallbladders. HPB (Oxford) 14:1–8
Buell JF, Cronin DC, Funaki B et al (2002) Devastating and fatal complications associated with combined vascular and bile duct injuries during cholecystectomy. Arch Surg 137:703–8, discussion 708–10
Dekker SW, Hugh TB (2008) Laparoscopic bile duct injury: understanding the psychology and heuristics of the error. ANZ J Surg 78:1109–1114
Lau KN, Sindram D, Agee N, Martinie JB, Iannitti DA (2010) Bile duct injury after single incision laparoscopic cholecystectomy. JSLS 14:587–591
Vollmer CM Jr, Callery MP (2007) Biliary injury following laparoscopic cholecystectomy: why still a problem? Gastroenterology 133:1039–1041
Flum DR, Koepsell T, Heagerty P, Sinanan M, Dellinger EP (2001) Common bile duct injury during laparoscopic cholecystectomy and the use of intraoperative cholangiography: adverse outcome or preventable error? Arch Surg 136:1287–1292
Agarwal BB, Mahajan KC (2010) Laparoscopic biliary tract injury prevention: zero tolerance, error free performance. Surg Endosc 24:728–729
Fry DE, Pine M, Jones BL, Meimban RJ (2010) Patient characteristics and the occurrence of never events. Arch Surg 145:148–151
Thompson KM, Oldenburg WA, Deschamps WA, Rupp WC, Smitth CD (2011) Chasing zero: the drive to eliminate surgical site infections. Ann Surg 254:430–7
Cuschieri A (2004) Surgical errors and their prevention. Surg Endosc 19:1013
Agarwal BB, Agarwal S, Gupta M, Mahajan K (2008) Transaxillary endoscopic excision of benign breast lumps: a new technique. Surg Endosc 22:407–410
Lee PC, Lo C, Lai PS, Chang JJ, Huang SJ, Lin MT et al (2010) Randomized clinical trial of single-incision laparoscopic cholecystectomy versus mini laparoscopic cholecystectomy. Br J Surg 97:1007–1012
Tsimoyiannis EC, Tsimogiannis KE, Pappas-Gogos G, Farantos C, Benetatos N, Mavridou P et al (2010) Different pain scores in single transumbilical incision laparoscopic cholecystectomy versus classic laparoscopic cholecystectomy: a randomized controlled trial. Surg Endosc 24:1842–1848
Marks J, Tacchino R, Roberts K, Onders R, Denoto G, Paraskeva P et al (2011) Prospective randomized controlled trial of traditional laparoscopic cholecystectomy versus single-incision laparoscopic cholecystectomy: report of preliminary data. Am J Surg 201:369–373
Bucher P, Pugin F, Buchs NC, Ostermann S, Morel P (2011) Randomized clinical trial of laparoendoscopic single site versus conventional laparoscopic cholecystectomy. Br J Surg 98:1695–1702
Connor S (2009) Single-port-access cholecystectomy: history should not be allowed to repeat. World J Surg 33:1020–1021
Ma J, Cassera MA, Spaun GO, Hammill CW, Hansen PD, Aliabadi-Wahle S (2011) Randomized controlled trial comparing single-port laparoscopic cholecystectomy and four-port laparoscopic cholecystectomy. Ann Surg 254:22–27
Bignell M, Hindmarsh A, Nageswaran H, Mothe B, Jenkinson A, Mahon D, Rhodes M (2011) Assessment of cosmetic outcome after laparoscopic cholecystectomy among women 4 years after laparoscopic cholecystectomy: is there a problem? Surg Endosc 25:2574–2577
Bencsath KP, Falk G, Morris-Stiff G, Kroh M, Walsh RM, Chalikonda S (2012) Single-incision laparoscopic cholecystectomy: do patients care? J Gastrointest Surg 16(3):535–539
Fischer L, Deckert A, Diener MK, Zimmermann JB, Büchler MW, Seiler CM (2011) Ranking of patient and surgeons’ perspectives for endpoints in randomized controlled trials—lessons learned from the POVATI trial [ISRCTN 60734227]. Langenbecks Arch Surg 396:1061–1066
Lamadé W, Friedrich C, Ulmer C, Basar T, Weiss H, Thon KP (2011) Impact of body image on patients’ attitude towards conventional, minimal invasive, and natural orifice surgery. Langenbecks Arch Surg 396:331–336
Iranmanesh P, Morel P, Inan I, Hagen M (2011) Choosing the cosmetically superior laparoscopic access to the abdomen: the importance of the umbilicus. Surg Endosc 25:2578–2585
Ioannidis JP (2010) Lies, damned lies, and medical science. The Atlantic November, 2010. Available from: http://www.theatlantic.com/magazine/archive/2010/11/lies-damned-lies-and-medical-cience/8269/ [Last accessed on 19 December 2011]
Ioannidis JP (2005) Contradicted and initially stronger effects in highly cited clinical research. JAMA 294:218–228
Jackson R, Feder G (1998) Guidelines for clinical guidelines. BMJ 317:427–428
Colhoun HM, McKeigue PM, Davey Smith G (2003) Problems of reporting genetic associations with complex outcomes. Lancet 361:865–867
Krugman P (2011) Patients are not consumers. The New York Times, April 21, 2011. Available from http://www.nytimes.com/2011/04/22/opinion/22krugman.html [Last accessed on 19 December 2011]
Hey J, Roberts KJ, Morris-Stiff GJ, Toogood GJ (2012) Patient views through the keyhole: new perspectives on single-incision vs.multiport laparoscopic cholecystectomy. HPB (Oxford) 14:242–246
Acknowledgement
We are grateful to Ms Ramneek Kaur, Krishna Adit and Nayan Agarwal for their valuable help in documentation and preparation of manuscript.
Disclosures
The authors have taken SILS as representing a truly single Incision Laparoscopic Surgery and not the usually practiced ‘Reduced Port Surgery’ (RPS) that is erroneously confused with SILS by some. Scientifically even a single trans-parietal suture puncture negates the concept of SILS. The authors practice RPS by routinely using a single 10 mm umbilical port supported by two or three 2.7 mm to 3.5 mm working ports for laparoscopic cholecystectomies etc.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Agarwal, B.B., Chintamani, Ali, K. et al. Innovations in Endosurgery—Journey into the Past of the Future. Indian J Surg 74, 234–241 (2012). https://doi.org/10.1007/s12262-012-0583-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-012-0583-8