Abstract
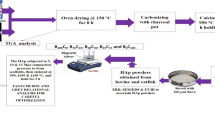
The use of multi-porous scaffolds for bone tissue engineering has been shown to improve osteogenesis. Although the exact mechanisms by which these scaffolds promote new bone formation have not yet been recognized well, related hypotheses can be found in many previous studies. The aim of this study was to examine the influence of the modulation of the pore size of beta- TCP ceramics on osteogenic differentiation in rats with calvarial defects. Treatments with macro- and meso-sized particles of NaCl, which was used as a porogen, were carried out during scaffold manufacturing, and the pore sizes of the beta-TCP scaffolds were measured by SEM. New bone formation was evaluated by Micro-CT, H&E staining, and immuno-histochemical analysis at week 4 after the operation. It was observed that the multi porosity of beta-TCP ceramics was controlled by treating the scaffolds with NaCl particles of two sizes (500–800 μm and 10–50 μm) during the firing process. Histological and immunohistochemical analysis of type 1 collagen and osteocalcin protein expression showed that the new bone formation and mineralization in case of the multi-porous beta-TCP ceramics comprising macro-and meso-sized pores were significantly higher than those in case of single porous macro- or meso-sized scaffolds. In conclusion, the distribution and size of the pores, as well as the surface structure of the scaffolds, may play an important role for osteogenic differentiation in vivo.
Similar content being viewed by others
Abbreviations
- Beta-TCP:
-
eta-tricalcium phosphate
- SEM:
-
scanning electron microscopy
- Micro-CT:
-
micro-computerized tomography
- H&E:
-
hematoxylin and eosin
- HA:
-
hydroxyapatite
- ANOVA:
-
analysis of variance
References
Wang, W. and K. W. K. Yeung (2017) Bone grafts and biomaterials substitutes for bone defect repair: A review. Bioact Mater. 2: 224–247.
Campana, V., G. Milano, E. Pagano, M. Barba, C. Cicione, G. Salonna, W. Lattanzi, and G. Logroscino (2014) Bone substitutes in orthopaedic surgery: from basic science to clinical practice. J. Mater. Sci. Mater. Med. 25: 2445–2461.
Polo-Corrales, L., M. Latorre-Esteves, and J. E. Ramirez-Vick (2014) Scaffold design for bone regeneration. J. Nanosci. Nanotechnol. 14: 15–56.
Bauer, T. W. and G. F. Muschler (2000) Bone graft materials. An overview of the basic science. Clin. Orthop. Relat. Res. 371: 10–27.
Sheikh, Z., S. Najeeb, Z. Khurshid, V. Verma, H. Rashid, and M. Glogauer (2015) Biodegradable materials for bone repair and tissue engineering applications. Materials (Basel). 8: 5744–5794.
Kasten, P., I. Beyen, P. Niemeyer, R. Luginbuhl, M. Bohner, and W. Richter (2008) Porosity and pore size of beta-tricalcium phosphate scaffold can influence protein production and osteogenic differentiation of human mesenchymal stem cells: an in vitro and in vivo study. Acta Biomater. 4: 1904–1915.
Kasten, P., R. Luginbuhl, M. van Griensven, T. Barkhausen, C. Krettek, M. Bohner, and U. Bosch (2003) Comparison of human bone marrow stromal cells seeded on calcium-deficient hydroxyapatite, beta-tricalcium phosphate and demineralized bone matrix. Biomaterials. 24: 2593–2603.
Li, X., C. A. van Blitterswijk, Q. Feng, F. Cui, and F. Watari (2008) The effect of calcium phosphate microstructure on bone-related cells in vitro. Biomaterials. 29: 3306–3316.
Li, X., H. Liu, X. Niu, Y. Fan, Q. Feng, F. Z. Cui, and F. Watari (2011) Osteogenic differentiation of human adipose-derived stem cells induced by osteoinductive calcium phosphate ceramics. J. Biomed. Mater. Res. B Appl. Biomater. 97: 10–19.
Zhang, K., Y. Fan, N. Dunne, and X. Li (2018) Effect of microporosity on scaffolds for bone tissue engineering. Regen. Biomater. 5: 115–124.
Soler-Illia, G. J., C. Sanchez, B. Lebeau, and J. Patarin (2002) Chemical strategies to design textured materials: from microporous and mesoporous oxides to nanonetworks and hierarchical structures. Chem. Rev. 102: 4093–4138.
Murphy, C. M., M. G. Haugh, and F. J. O’Brien (2010) The effect of mean pore size on cell attachment, proliferation and migration in collagen-glycosaminoglycan scaffolds for bone tissue engineering. Biomaterials. 31: 461–466.
Reinwald, Y., R. K. Johal, A. M. Ghaemmaghami, F. R. A. J. Rose, S. M. Howdle, and K. M. Shakesheff (2014) Interconnectivity and permeability of supercritical fluid-foamed scaffolds and the effect of their structural properties on cell distribution. Polymer. 55: 435–444.
Murphy, C. M. and F. J. O’Brien (2010) Understanding the effect of mean pore size on cell activity in collagen-glycosaminoglycan scaffolds. Cell Adh. Migr. 4: 377–381.
Wei, J., J. Jia, F. Wu, S. Wei, H. Zhou, H. Zhang, J. W. Shin, and C. Liu (2010) Hierarchically microporous/macroporous scaffold of magnesium-calcium phosphate for bone tissue regeneration. Biomaterials. 31: 1260–1269.
Diao, J., J. OuYang, T. Deng, X. Liu, Y. Feng, N. Zhao, C. Mao, and Y. Wang (2018) 3D-plotted beta-tricalcium phosphate scaffolds with smaller pore sizes improve in vivo bone regeneration and biomechanical properties in a critical-sized calvarial defect rat model. Adv. Healthc Mater. 7: e1800441.
Dai, W., N. Kawazoe, X. Lin, J. Dong, and G. Chen (2010) The influence of structural design of PLGA/collagen hybrid scaffolds in cartilage tissue engineering. Biomaterials. 31: 2141–2152.
Bose, S., M. Roy, and A. Bandyopadhyay (2012) Recent advances in bone tissue engineering scaffolds. Trends Biotechnol. 30: 546–554.
Karageorgiou, V. and D. Kaplan (2005) Porosity of 3D biomaterial scaffolds and osteogenesis. Biomaterials. 26: 5474–5491.
Woodard, J. R., A. J. Hilldore, S. K. Lan, C. J. Park, A. W. Morgan, J. A. Eurell, S. G. Clark, M. B. Wheeler, R. D. Jamison, and A. J. Wagoner Johnson (2007) The mechanical properties and osteoconductivity of hydroxyapatite bone scaffolds with multi-scale porosity. Biomaterials. 28: 45–54.
Sopyan, I., A. Fadli, and M. Mel (2012) Porous alumina-hydroxyapatite composites through protein foaming-consolidation method. J. Mech. Behav. Biomed. Mater. 8: 86–98.
Yoshikawa, H., N. Tamai, T. Murase, and A. Myoui (2009) Interconnected porous hydroxyapatite ceramics for bone tissue engineering. J. R Soc. Interface. 6: S341–S348.
Guda, T., A. Darr, D. T. Silliman, M. H. Magno, J. C. Wenke, J. Kohn, and P. R. Brown Baer (2014) Methods to analyze bone regenerative response to different rhBMP-2 doses in rabbit craniofacial defects. Tissue Eng. Part C Methods. 20: 749–760.
Sawyer, A. A., S. J. Song, E. Susanto, P. Chuan, C. X. Lam, M. A. Woodruff, D. W. Hutmacher, and S. M. Cool (2009) The stimulation of healing within a rat calvarial defect by mPCL-TCP/collagen scaffolds loaded with rhBMP-2. Biomaterials. 30: 2479–2488.
Sun, L., D. Pereira, Q. Wang, D. B. Barata, R. Truckenmuller, Z. Li, X. Xu, and P. Habibovic (2016) Controlling growth and osteogenic differentiation of osteoblasts on microgrooved polystyrene surfaces. PLoS One. 11: e0161466.
Tsao, Y. T., Y. J. Huang, H. H. Wu, Y. A. Liu, Y. S. Liu, and O. K. Lee (2017) Osteocalcin mediates biomineralization during osteogenic maturation in human mesenchymal stromal cells. Int. J. Mol. Sci. 18: 159.
Acknowledgements
This research was supported by a grant (17172MFDS394) from the Ministry of Food and Drug Safety in 2017, the Clinical Medicine Research Institute of the Chosun University Hospital(2016) and Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education (2017R1D1A3B03031764).
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Park, M., Lee, G., Ryu, K. et al. Improvement of Bone Formation in Rats with Calvarial Defects by Modulating the Pore Size of Tricalcium Phosphate Scaffolds. Biotechnol Bioproc E 24, 885–892 (2019). https://doi.org/10.1007/s12257-019-0248-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12257-019-0248-6