Abstract
The effects of stem cell transplantation (SCT) in patients with peripheral T-cell lymphoma not otherwise specified (PTCL-NOS) and angioimmunoblastic T-cell lymphoma (AITL) remain controversial. We analyzed the feasibility of SCT and risk factors associated with outcomes of PTCL-NOS and AITL patients to identify the potential clinical efficacy of SCT. We retrospectively analyzed the data of PTCL-NOS (n = 83) and AITL (n = 112) patients who received autologous (n = 10 and 16, respectively) or allogeneic (n = 12 and 4, respectively) SCT, or no SCT (n = 61 and 92, respectively) between 2008 and 2018. All PTCL-NOS and AITL diagnoses were reconfirmed by an experienced hematopathologist. Median age at PTCL-NOS and AITL diagnoses in the SCT group was younger than that in the no SCT group. Significant risk factors for lower overall survival were intermediate–high and high-risk international prognostic indexes in PTCL-NOS patients (P = 0.0052), and a > 2 modified prognostic index for T-cell lymphoma (P = 0.0079) and no SCT (P = 0.028) in AITL patients. Autologous or allogeneic SCT compared with no SCT in AITL patients resulted in 3-year overall survival of 68.6% and 100% vs. 57.2% (P = 0.018). Strategies should be developed to improve selection of PTCL-NOS and AITL patients suitable for SCT and/or additional novel therapies.


Similar content being viewed by others
References
Swerdlow SH, Campo E, Harris NL, Jaffe ES, Pileri SA, Stein H, et al. WHO classification of tumours of haematopoietic and lymphoid tissues. Lyon: IARC Press; 2017.
Karlin L, Coiffier B. The changing landscape of peripheral T-cell lymphoma in the era of novel therapies. Semin Hematol. 2014;51:25–34.
Vose J, Armitage J, Weisenburger D. International peripheral T-cell and natural killer/T-cell lymphoma study:pathology findings and clinical outcomes. J Clin Oncol. 2018;26:4124–30.
Schmitz N, de Leval L. How I manage peripheral T-cell lymphoma, not otherwise specified and angioimmunoblastic T-cell lymphoma: current practice and a glimpse into the future. Br J Haematol. 2017;176:851–66.
Chihara D, Fanale MA, Miranda RN, Noorani M, Westin JR, Nastoupil LJ, et al. The survival outcome of patients with relapsed/refractory peripheral T-cell lymphoma-not otherwise specified and angioimmunoblastic T-cell lymphoma. Br J Haematol. 2017;176:750–8.
Cheson BD. Novel therapies for peripheral T-cell non-Hodgkin's lymphomas. Curr Opin Hematol. 2009;16:299–305.
Maruyama D, Tobinai K, Ogura M, Uchida T, Hatake K, Taniwaki M, et al. Romidepsin in Japanese patients with relapsed or refractory peripheral T-cell lymphoma: a phase I/II and pharmacokinetics study. Int J Hematol. 2017;106:655–65.
Gisselbrecht C, Sibon D. New perspectives in the therapeutic approach of peripheral T-cell lymphoma. Curr Opin Oncol. 2018;30:285–91.
Reimer P, Rüdiger T, Geissinger E, Weissinger F, Nerl C, Schmitz N, et al. Autologous stem-cell transplantation as first-line therapy in peripheral T-cell lymphomas: results of a prospective multicenter study. J Clin Oncol. 2009;27:106–13.
d'Amore F, Relander T, Lauritzsen GF, Jantunen E, Hagberg H, Anderson H, et al. Up-front autologous stem-cell transplantation in peripheral T-cell lymphoma:NLG-T-01. J Clin Oncol. 2012;30:3093–9.
Kharfan-Dabaja MA, Kumar A, Ayala E, Hamadani M, Reimer P, Gisselbrecht C, et al. Clinical practice recommendations on indication and timing of hematopoietic cell transplantation in mature T cell and NK/T cell lymphomas: an international collaborative effort on behalf of the Guidelines Committee of the American Society for Blood and Marrow Transplantation. Biol Blood Marrow Transplant. 2017;23:1826–38.
Rodríguez J, Conde E, Gutiérrez A, Arranz R, León A, Marín J, et al. The results of consolidation with autologous stem-cell transplantation in patients with peripheral T-cell lymphoma (PTCL) in first complete remission: the Spanish Lymphoma and Autologous Transplantation Group experience. Ann Oncol. 2007;18:627–52.
Kyriakou C, Canals C, Goldstone A, Caballero D, Metzner B, Kobbe G, et al. High-dose therapy and autologous stem-cell transplantation in angioimmunoblastic lymphoma: complete remission at transplantation is the major determinant of Outcome-Lymphoma Working Party of the European Group for Blood and Marrow Transplantation. J Clin Oncol. 2008;26:218–24.
Smith SM, Burns LJ, van Besien K, Lerademacher J, He W, Fenske TS, et al. Hematopoietic cell transplantation for systemic mature T-cell non-Hodgkin lymphoma. J Clin Oncol. 2013;31:3100–9.
Yin J, Wei J, Xu JH, Xiao Y, Zhang YC. Autologous stem cell transplantation as the first-line treatment for peripheral T cell lymphoma: results of a comprehensive meta-analysis. Acta Haematol. 2014;131:114–25.
Corradini P, Tarella C, Zallio F, Dodero A, Zanni M, Valagussa P, et al. Long-term follow-up of patients with peripheral T-cell lymphomas treated up-front with high-dose chemotherapy followed by autologous stem cell transplantation. Leukemia. 2006;20:1533–8.
Mercadal S, Briones J, Xicoy B, Pedro C, Escoda L, Estany C, et al. Intensive chemotherapy (high-dose CHOP/ESHAP regimen) followed by autologous stem-cell transplantation in previously untreated patients with peripheral T-cell lymphoma. Ann Oncol. 2008;19:958–63.
Yam C, Landsburg DJ, Nead KT, Lin X, Mato AR, Svoboda J, et al. Autologous stem cell transplantation in first complete remission may not extend progression-free survival in patients with peripheral T cell lymphomas. Am J Hematol. 2016;91:672–6.
Fossard G, Broussais F, Coelho I, Bailly S, Nicolas-Virelizier E, Toussaint E, et al. Role of up-front autologous stem-cell transplantation in peripheral T-cell lymphoma for patients in response after induction: an analysis of patients from LYSA centers. Ann Oncol. 2018;29:715–23.
Fossard G, Broussais F, Coelho I, Bailly S, Nicolas-Virelizier E, Toussaint E, et al. he impact of stem cell transplantation on the natural course of peripheral T-cell lymphoma: a real-world experience. Ann Hematol. 2018;97:1241–50.
Loirat M, Chevallier P, Leux C, Moreau A, Bossard C, Guillaume T, et al. Upfront allogeneic stem-cell transplantation for patients with nonlocalized untreated peripheral T-cell lymphoma: an intention-to-treat analysis from a single center. Ann Oncol. 2015;26:386–92.
Kyriakou C, Canals C, Finke J, Kobbe G, Harousseau JL, Kolb HJ, et al. Allogeneic stem cell transplantation is able to induce long-term remissions in angioimmunoblastic T-cell lymphoma: a retrospective study from the lymphoma working party of the European group for blood and marrow transplantation. J Clin Oncol. 2009;27:3951–8.
Wulf G, Hasenkamp J, Jung W, Wilhelm C, Held G, Nickelsen M, et al. Allogeneic stem cell transplantation for patients with relapsed or refractory T-cell lymphoma:efficacy of lymphoma-directed conditioning against advanced disease. Bone Marrow Transplant. 2019;54:877–84.
Gu Z, Wang L, Wang Q, Li H, Bo J, Wang S, et al. Outcomes of myeloablative peripheral blood stem cell transplantation for non-complete remission patients with relapsed/refractory peripheral T cell lymphomas. Ann Hematol. 2019;98:1237–47.
Gallamini A, Stelitano C, Calvi R, Bellei M, Mattei D, Vitolo U, et al. Peripheral T-cell lymphoma unspecified (PTCL-U): a new prognostic model from a retrospective multicentric clinical study. Blood. 2004;103:2474–9.
Went P, Agostinelli C, Gallamini A, Piccaluga PP, Ascani S, Sabattini E, et al. Marker expression in peripheral T-cell lymphoma: a proposed clinical-pathologic prognostic score. J Clin Oncol. 2006;24:2472–9.
Weisenburger DD, Savage KJ, Harris NL, Gascoyne RD, Jaffe ES, MacLennan KA, et al. Peripheral T-cell lymphoma, not otherwise specified: a report of 340 cases from the International Peripheral T-cell Lymphoma Project. Blood. 2011;117:3402–8.
Fine JP, Gray RJ. A proportional hazards model for the subdistribution of a competing risk. J Am Stat Assoc. 1999;94:496–509.
Kanda Y. Investigation of the freely available easy-to-use software 'EZR' for medical statistics. Bone Marrow Transplant. 2013;48:452–8.
Numata A, Miyamoto T, Ohno Y, Kamimura T, Kamezaki K, Tanimoto T, et al. Long-term outcomes of autologous PBSCT for peripheral T-cell lymphoma: retrospective analysis of the experience of the Fukuoka BMT group. Bone Marrow Transplant. 2010;45:311–6.
Sugimoto M, Ito S, Mashima K, Umino K, Minakata D, Nakano H, et al. Retrospective evaluation of the MEAM regimen as a conditioning regimen before autologous peripheral blood stem cell transplantation for lymphoma in two centers with different dosing schedules of melphalan. Ann Hematol. 2016;95:1513–9.
Giralt S, Ballen K, Rizzo D, Bacigalupo A, Horowitz M, Pasquini M, et al. Reduced-intensity conditioning regimen workshop: defining the dose spectrum-report of a workshop convened by the Center for International Blood and Marrow Transplant Research. Biol Blood Marrow Transplant. 2009;15:367–9.
Yamasaki S, Chihara D, Kim SW, Kawata T, Mizuta S, Ago H, et al. Risk factors and timing of autologous stem cell transplantation for patients with peripheral T-cell lymphoma. Int J Hematol. 2019;109:175–86.
Cheson BD, Pfistner B, Juweid ME, Gascoyne RD, Specht L, Horning SJ, et al. Revised response criteria for malignant lymphoma. J Clin Oncol. 2007;25:579–86.
Barrington SF, Mikhaeel NG, Kostakoglu L, Meignan M, Hutchings M, Müeller SP, et al. Role of imaging in the staging and response assessment of lymphoma: consensus of the International Conference on Malignant Lymphomas Imaging Working Group. J Clin Oncol. 2014;32:3048–58.
Cottereau AS, Becker S, Broussais F, Casasnovas O, Kanoun S, Roques M, et al. Prognostic value of baseline total metabolic tumor volume (TMTV0) measured on FDG-PET/CT in patients with peripheral T-cell lymphoma (PTCL). Ann Oncol. 2016;27:719–24.
Mak V, Hamm J, Chhanabhai M, Shenkier T, Klasa R, Sehn LH, et al. Survival of patients with peripheral T-cell lymphoma after first relapse or progression: spectrum of disease and rare long-term survivors. J Clin Oncol. 2013;31:1970–6.
Le Gouill S, Milpied N, Buzyn A, De Latour RP, Vernant JP, Mohty M, et al. Graft-versus-lymphoma effect for aggressive T-cell lymphomas in adults: a study by the Société Francaise de Greffe de Moëlle et de Thérapie Cellulaire. J Clin Oncol. 2008;26:2264–71.
Kanate AS, Mussetti A, Kharfan-Dabaja MA, Ahn KW, DiGilio A, Beitinjaneh A, et al. Reduced-intensity transplantation for lymphomas using haploidentical related donors vs HLA-matched unrelated donors. Blood. 2016;127:938–47.
Acknowledgments
We thank the patients and clinical staff for their participation in the study. We appreciate Akishiko Numata, Goichi Yoshimoto, Yasuo Mori (Kyushu University Hospital), Takuro Kuriyama, Yayoi Matsuo, Masayasu Hayashi, and Tomonori Shimokawa (Hamanomachi Hospital) for checking the medical records. The authors also acknowledge the Clinical Research Institute, Kyushu Medical Hospital for editorial support. We thank Edanz Group (www.edanzediting.com/ac) for editing a draft of this manuscript. All named authors meet the International Committee of Medical Journal Editors criteria for authorship of this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Funding
No funding or sponsorship was received for this study or publication of this article. The article processing charges were funded by the authors.
Author information
Authors and Affiliations
Consortia
Contributions
SY designed the study, analyzed the data, and prepared the manuscript., SY, KK, IC, YI, K/K, HH., KT., RO., YS., TM, TE, KO, KA, and HI prepared and reviewed the manuscript. All authors approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Koji Kato: Consulting or advisory role with AbbVie, AstraZeneca, Celgene, Chugai, Eisai, Janssen, and Novartis. Honoraria from Chugai, Takeda, MSD, Kyowa-Kirin, Janssen, Celgene, Ono, Dainippon-Sumitomo, AbbVie, Novartis. Research funding from Chugai, Takeda, Kyowa-Kirin, Abbvie, Eisai, Janssen, Novartis, Mundi, AstraZeneca, Celgene, Ono, MSD, and Otsuka. The other authors declare that there are no competing financial interests regarding this article.
Ethical approval
The present study was retrospective and did not involve any experimental intervention, which was approved by the Institutional Review Board of Kyushu Medical Center.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
12185_2020_2879_MOESM1_ESM.pptx
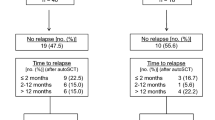
Supplemental Figure 1. Flow chart of patients included in this analysis. Supplemental Figure 2. Kaplan-Meier estimates of OS of PTCL-NOS patients after the landmark time (A, 2 months from diagnosis; B, 4 months from diagnosis; C, 6 months from diagnosis). Supplemental Figure 3. Kaplan-Meier estimates of OS of AITL patients after the landmark time (A, 2 months from diagnosis; B, 4 months from diagnosis; C, 6 months from diagnosis).1 (PPTX 172 kb)
About this article
Cite this article
Yamasaki, S., Yoshida, S., Kato, K. et al. Effects of stem cell transplantation in patients with peripheral T-cell lymphoma not otherwise specified and angioimmunoblastic T-cell lymphoma. Int J Hematol 112, 74–83 (2020). https://doi.org/10.1007/s12185-020-02879-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12185-020-02879-w